Biomechanics exam 2 (sadge but happy)
1/161
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
162 Terms
What is the Load-Deformation curve?
A graph that shows the relationship between the load applied to a material and the resulting deformation.

Define stress in biomechanics.
Stress (σ) is the force applied to deform a structure per unit area (N/m², Pa), calculated as σ = F/A.
Define strain in biomechanics.
Strain (ε) is the resulting deformation of tissues caused by applied stress, expressed as a percentage (ε = ΔL/L).
What is the Elastic Region on the Stress-Strain Curve?
The linear portion of the curve where, if stress is removed, the material returns to its original state.
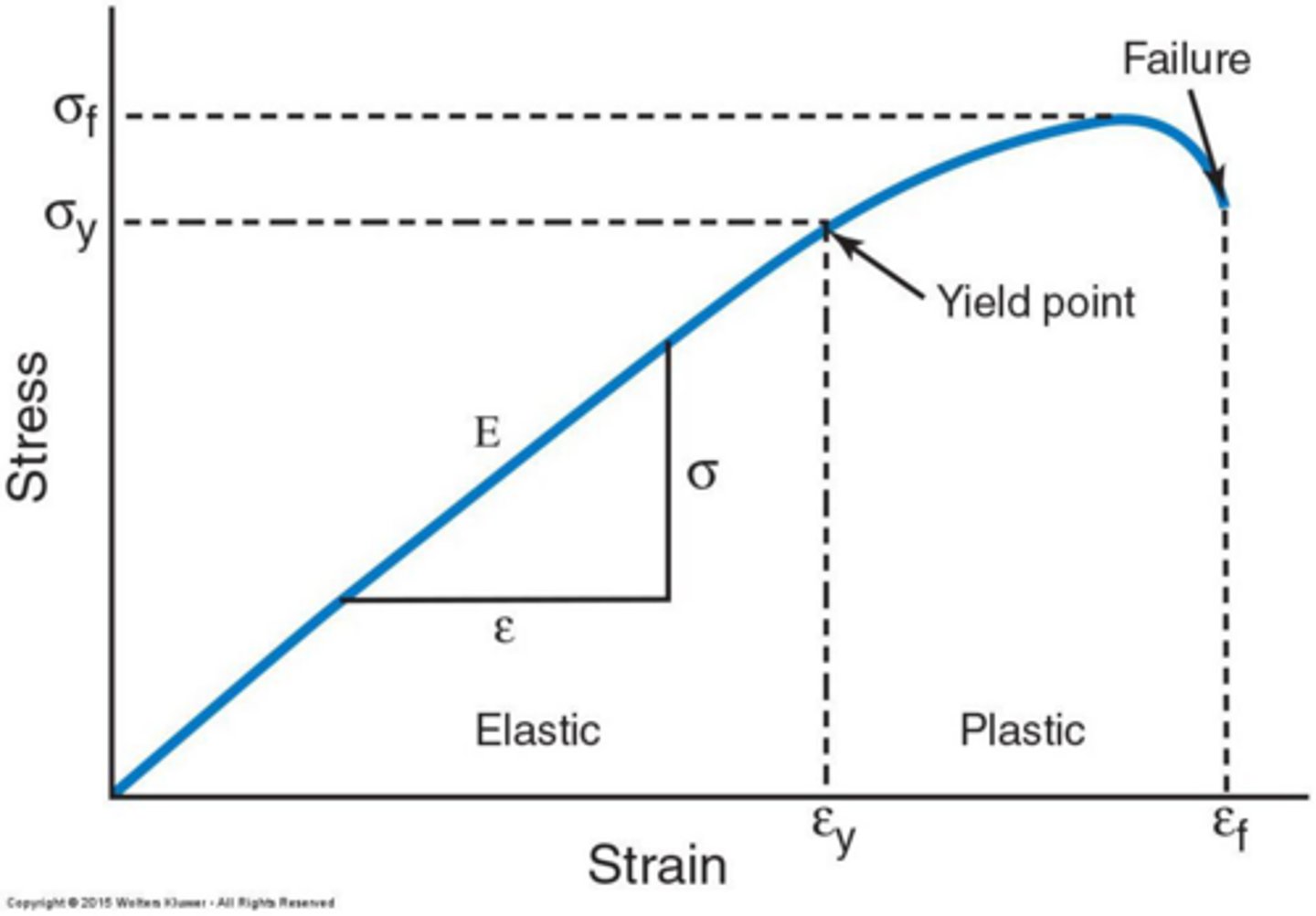
What is the Yield Point on the Stress-Strain Curve?
The point where the slope of the curve decreases as greater force is applied, indicating the transition to permanent deformation.
What occurs in the Plastic Region of the Stress-Strain Curve?
The material is permanently deformed, and if stress is removed, it does not return to its original state.
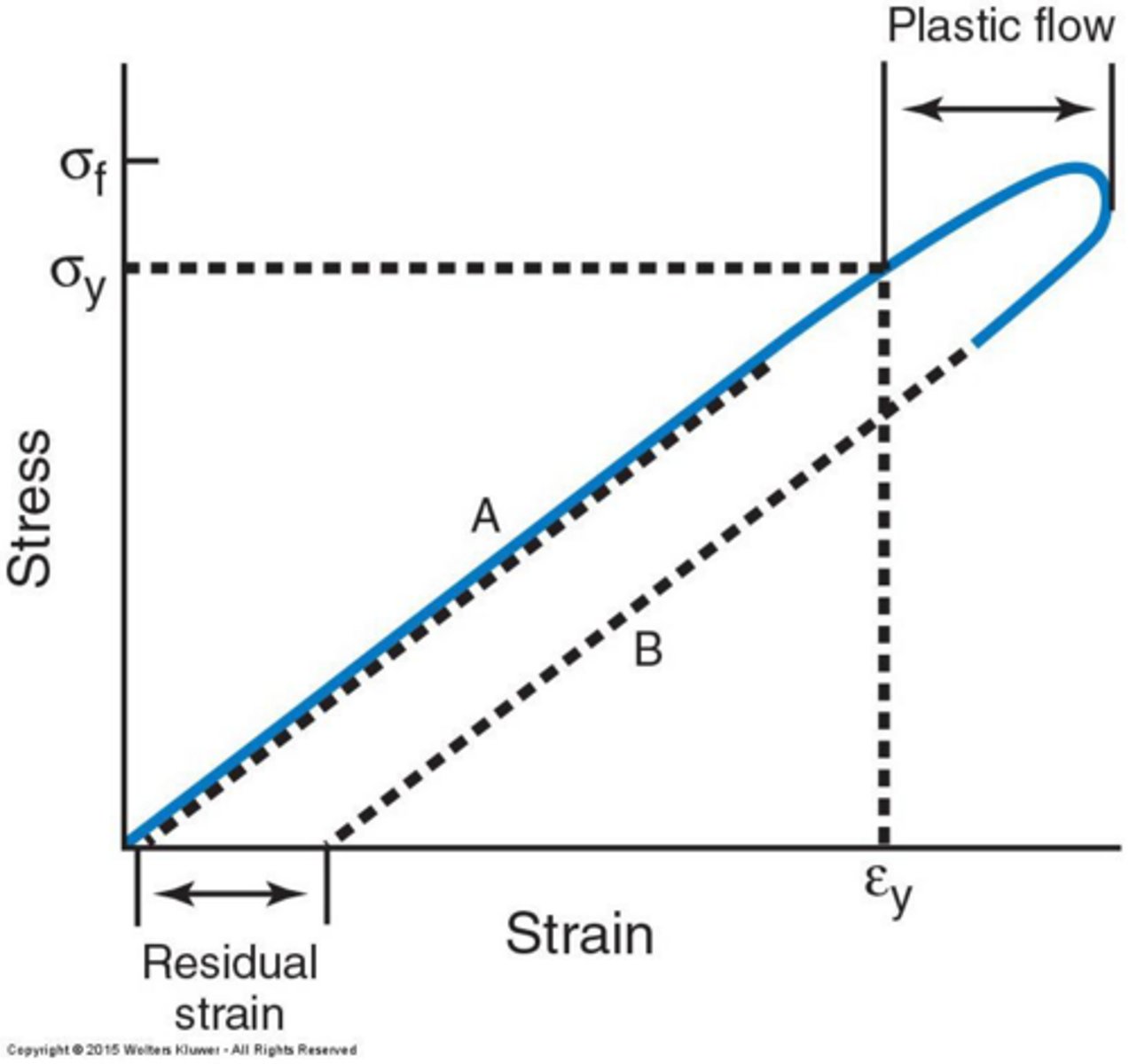
What is Toughness in biomechanics?
The combination of stress and strain that indicates a material's ability to absorb energy before failing.
Define Resilience in the context of materials.
The ability of a material to absorb forces in the elastic range and return to its original shape.
What is Residual Strain?
The difference between the original length and the length resulting from stress in the plastic region.
What are viscoelastic properties?
Time-dependent responses of materials to stress, including creep and stress relaxation.
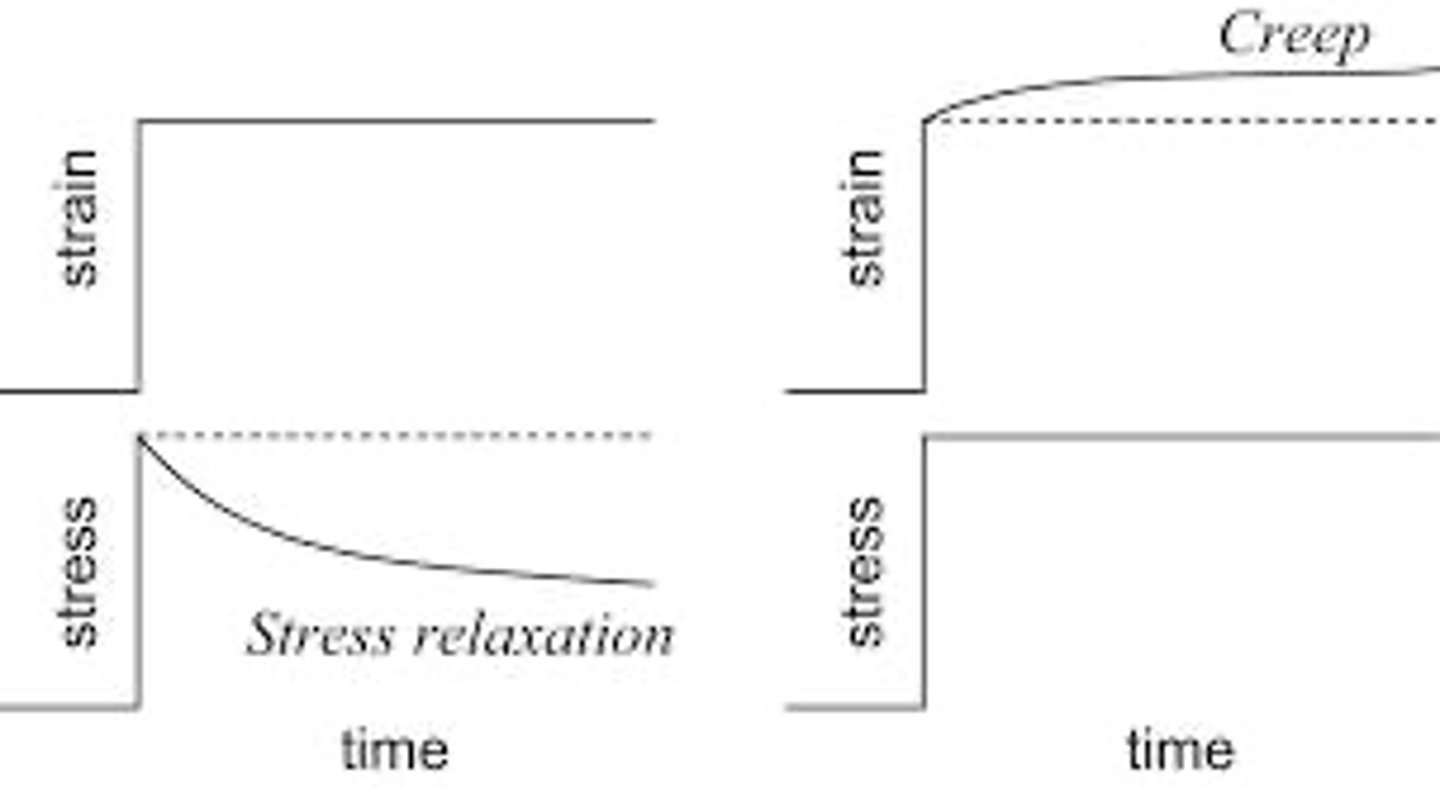
What is Creep in biomechanics?
The permanent deformation that occurs when constant stress is applied over a long period.
What is Stress Relaxation?
The decrease in internal resistance or stress over time when a tissue is held at a constant strain.
What does Isotropic Behavior mean?
Material exhibits the same properties regardless of the direction of the applied force.
What does Anisotropic Behavior mean?
Material has differing mechanical properties depending on how it is loaded.
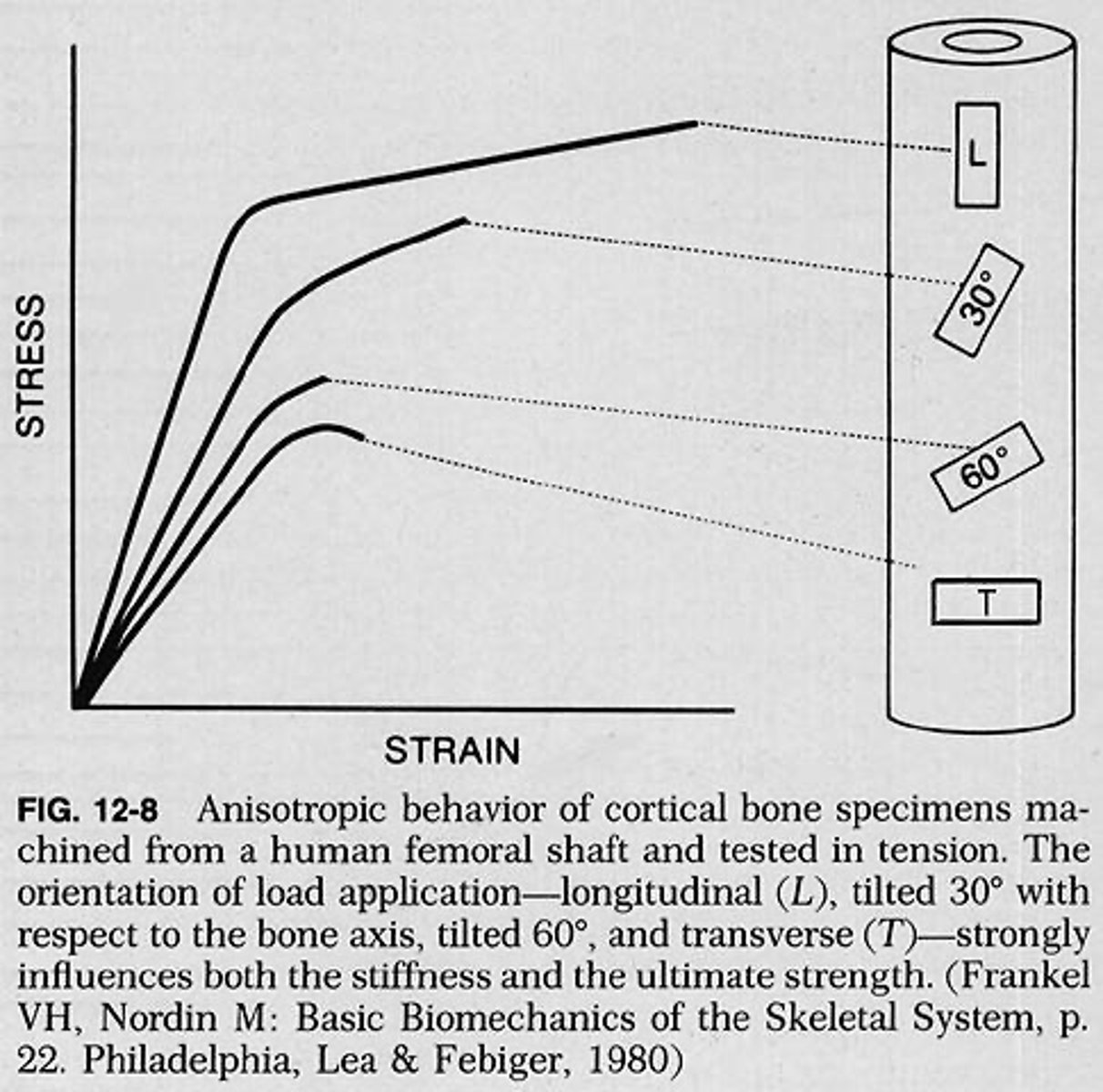
How does temperature affect collagenous tissue?
Warmed collagenous tissue exhibits greater ultimate strength and strain at failure, shifting the stress/strain curve to the right.
What happens to tissue with decreased use?
Strength decreases due to lack of mechanical loading.
What happens to tissue with increased use?
Strength increases due to mechanical loading.
What are the main components of connective tissue?
Fibrous components include collagen and elastin; non-fibrous components include ground substance, glycoproteins, water, and proteoglycans.
What is the composition of bone?
Bone is composed of 60-70% inorganic salts and collagen, with 25-30% water content.
What role do osteoblasts play in bone?
Osteoblasts produce new bone by forming osteoid.
What role do osteoclasts play in bone?
Osteoclasts resorb bone tissue, aiding in growth and healing.
What is the recycling rate of bone mass in humans?
Humans recycle 5-7% of bone mass each week.
What are the primary functions of bone?
Structure/support, leverage, protection, storage, and blood cell formation.
What type of bone tissue is dense and forms the outer shell?
Cortical (Compact) bone.
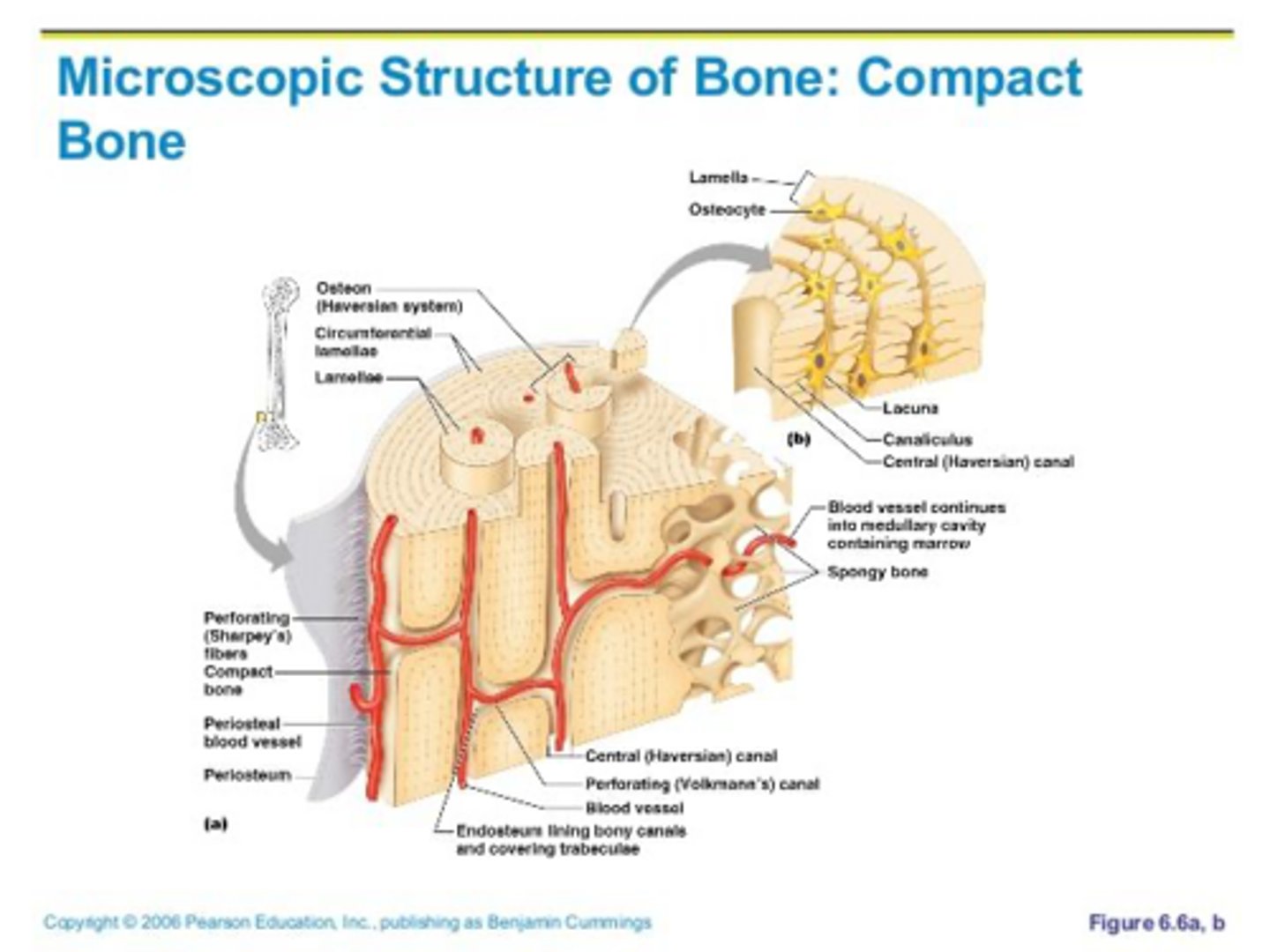
What type of bone tissue is less dense and contains trabeculae?
Cancellous (Spongy) bone.
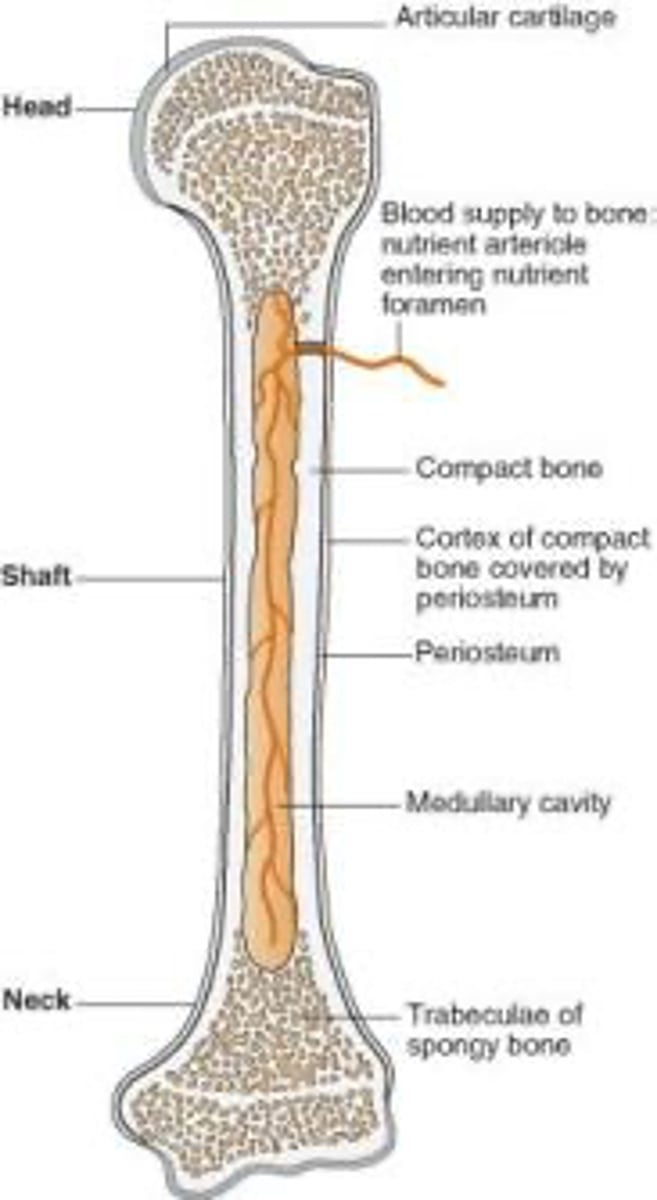
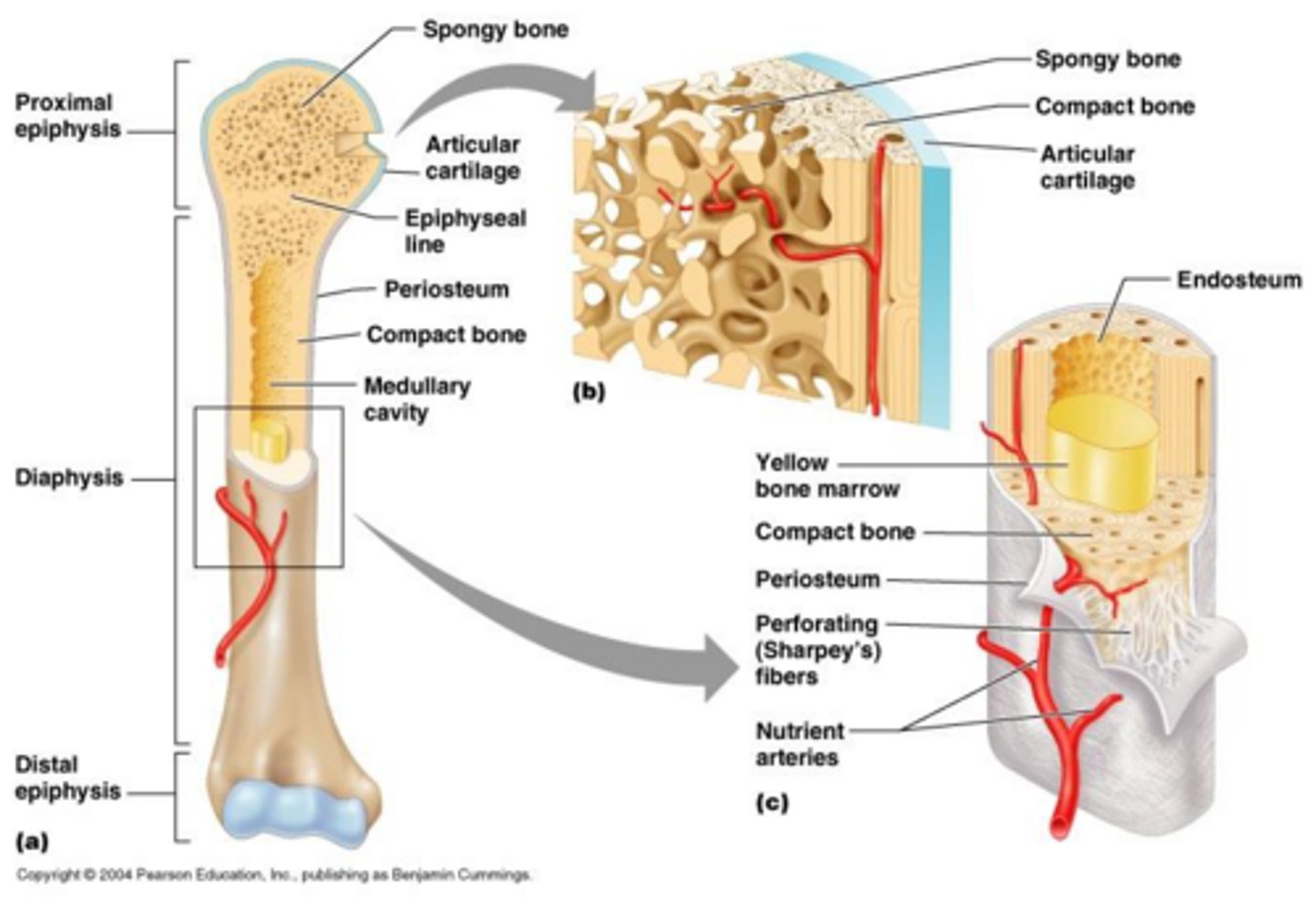
What is the significance of the Haversian Canal System in bone?
It contains blood vessels and nerves, providing a rich blood and nerve supply.
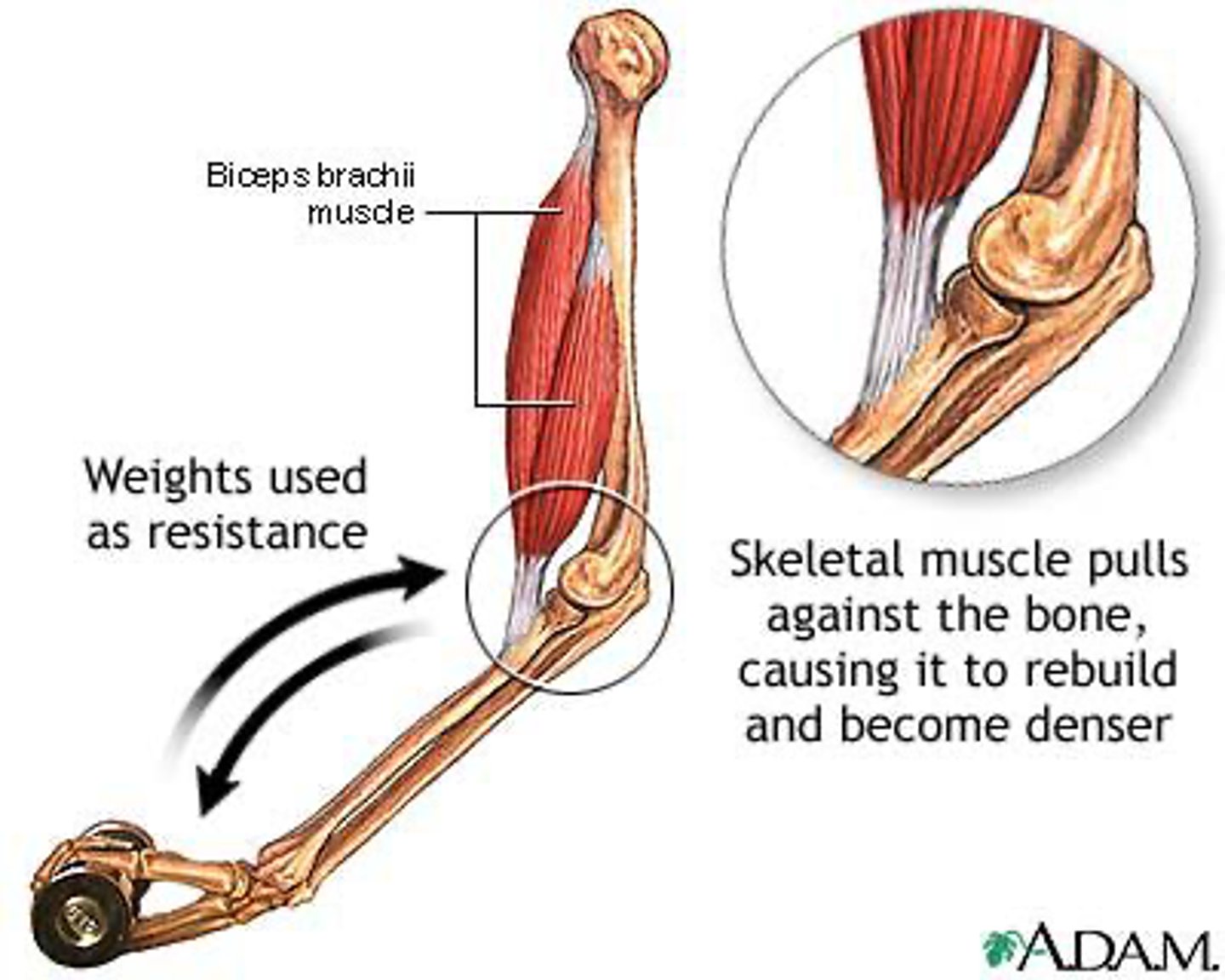
What is Wolf's Law?
Bones grow according to the stresses placed upon them.
What happens to bone when load increases?
Osteoblast activity increases, leading to bone formation.
What is the Area Moment of Inertia?
It measures resistance to bending load in a bone.
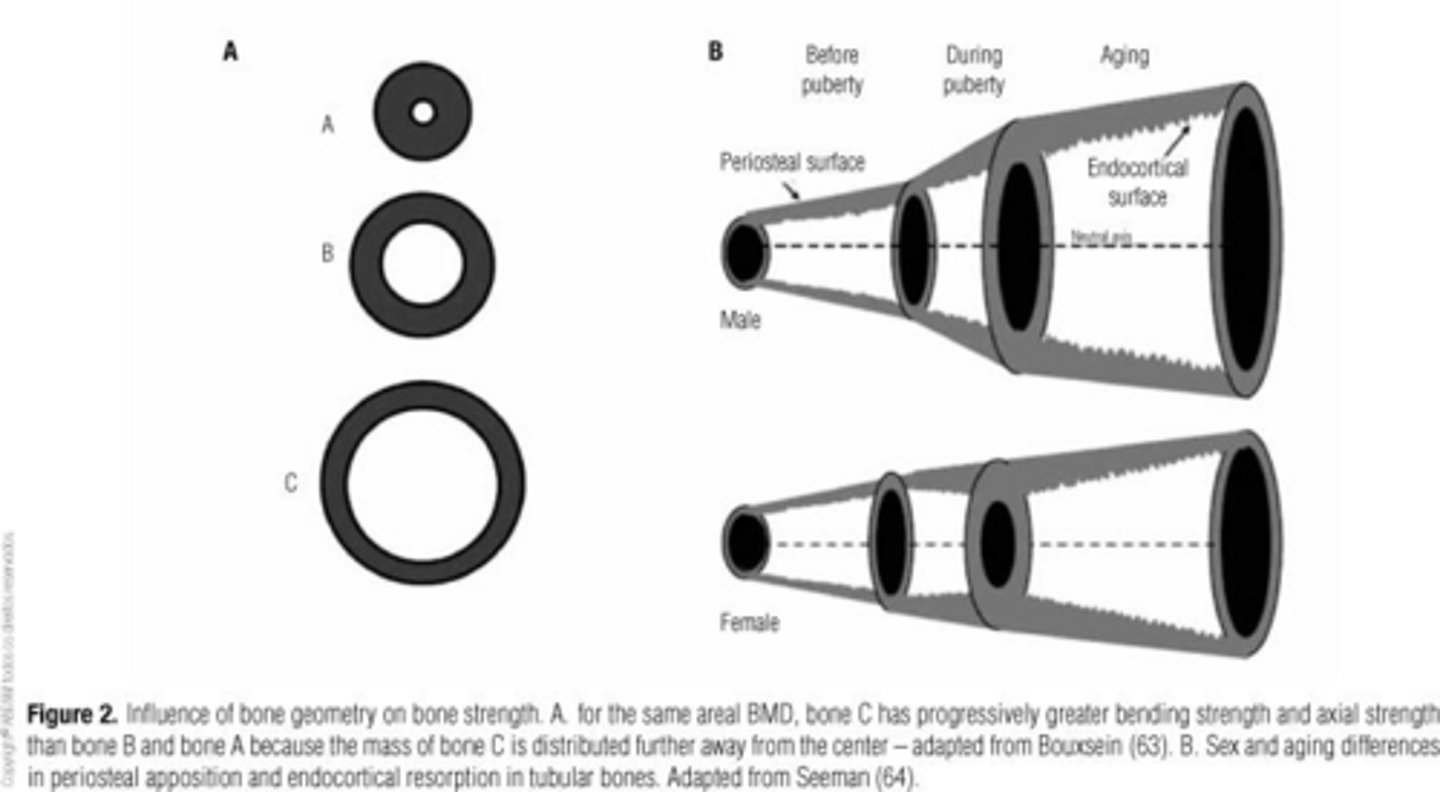
What is the Polar Moment of Inertia?
It measures resistance to torsional loading in a bone.
How does the shape of a bone influence its mechanical behavior?
A larger cross-sectional area makes the bone stronger and stiffer.
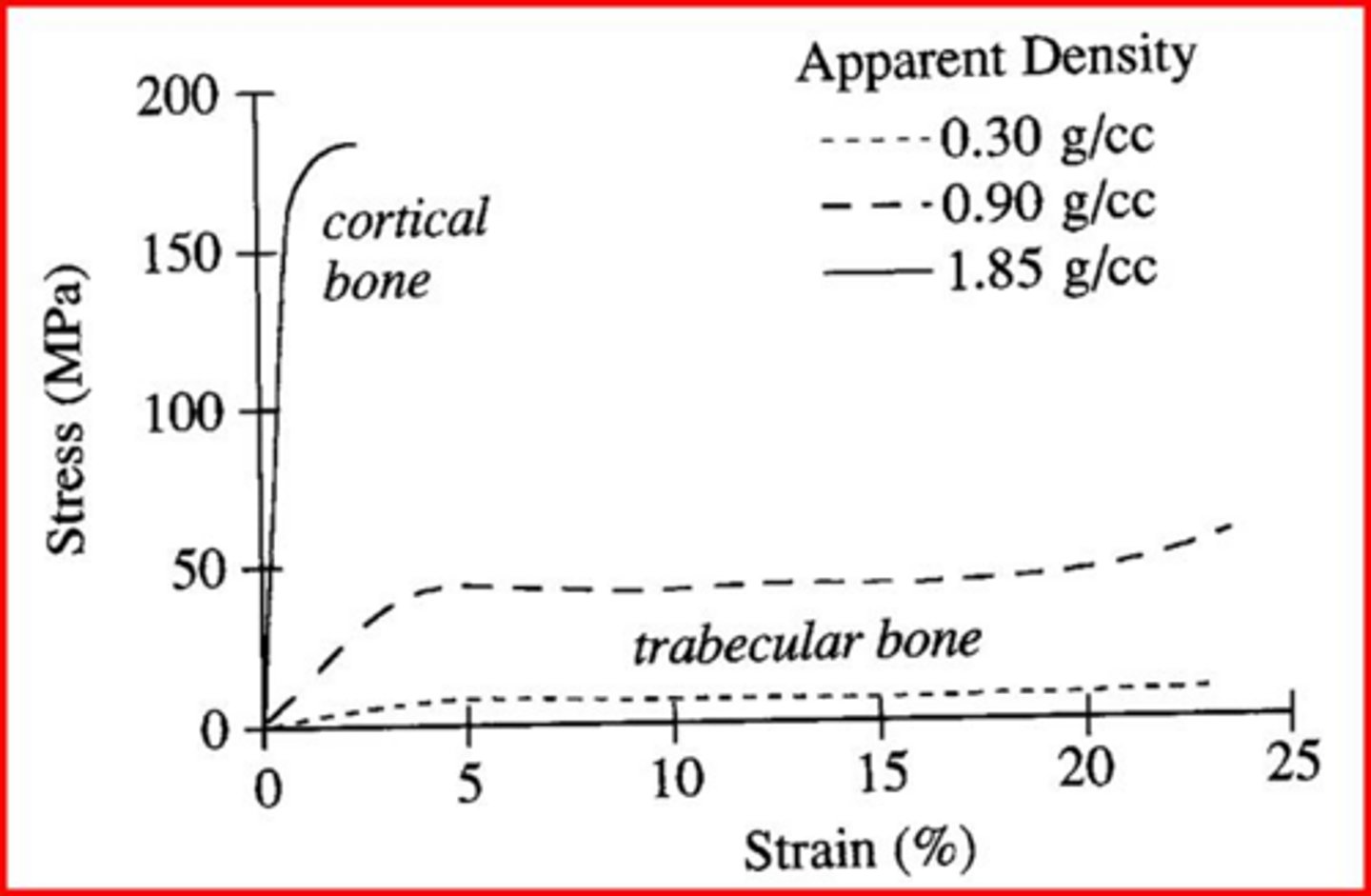
What is the strain at which cortical bone typically fractures?
Cortical bone fractures at approximately 2% strain.
What is the strain at which cancellous bone typically fractures?
Cancellous bone fractures at approximately 7% strain.
What is anisotropic behavior in bone?
Bone exhibits different mechanical properties in different directions.
What factors influence the behavior of bone?
Orientation, size, and density of trabeculae.
How does muscle force influence bone loading?
Soft tissue forces generate the highest force on bone during movement.
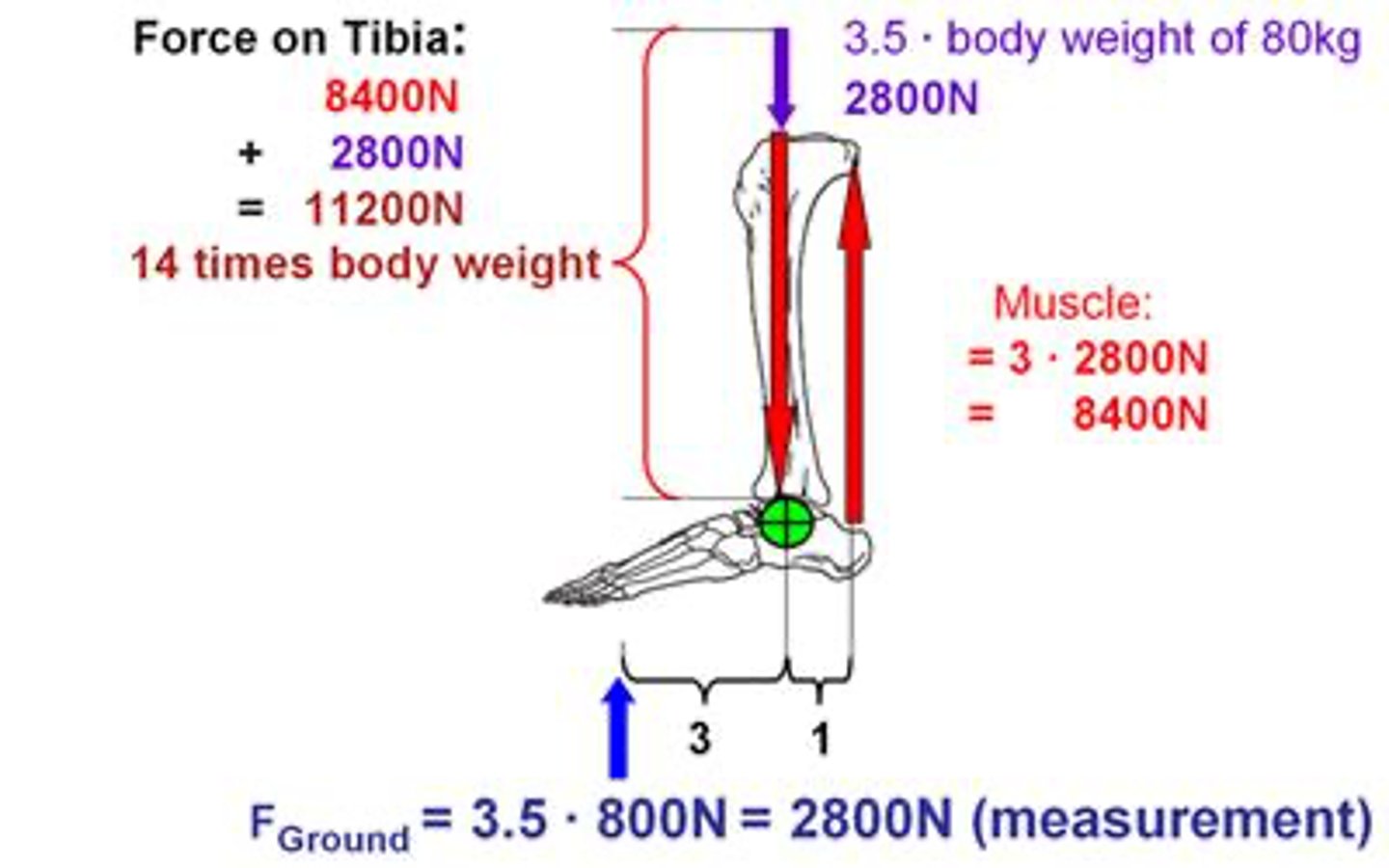
What is the effect of repetitive loading on bones?
Stress fractures can occur with low load applied at high frequency.
What long-term effects does exercise have on bones?
It increases bone mass, cortical thickness, and bone mineral content.
How does aging affect bone density?
Aging results in decreased osteoblast activity and increased osteoclast activity, leading to weaker bones.
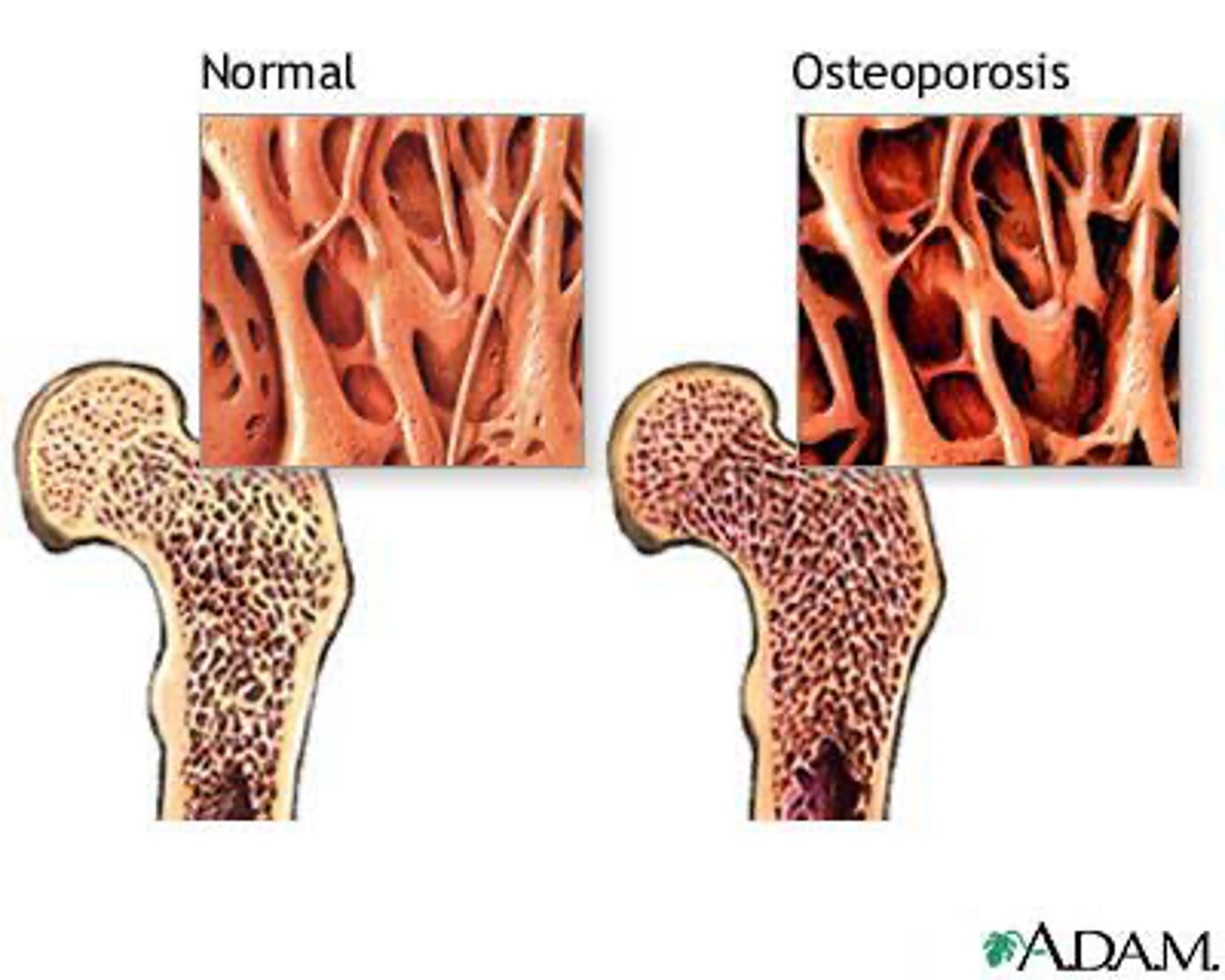
What is the role of compression in bone growth?
Compression stimulates the conversion of cartilaginous tissue into bone.
What can excessive compression or tension lead to in bone growth?
It can halt bone growth or deformities.
What is the impact of dynamic loading compared to static loading on bone?
Dynamic loading is more effective for stimulating bone remodeling.
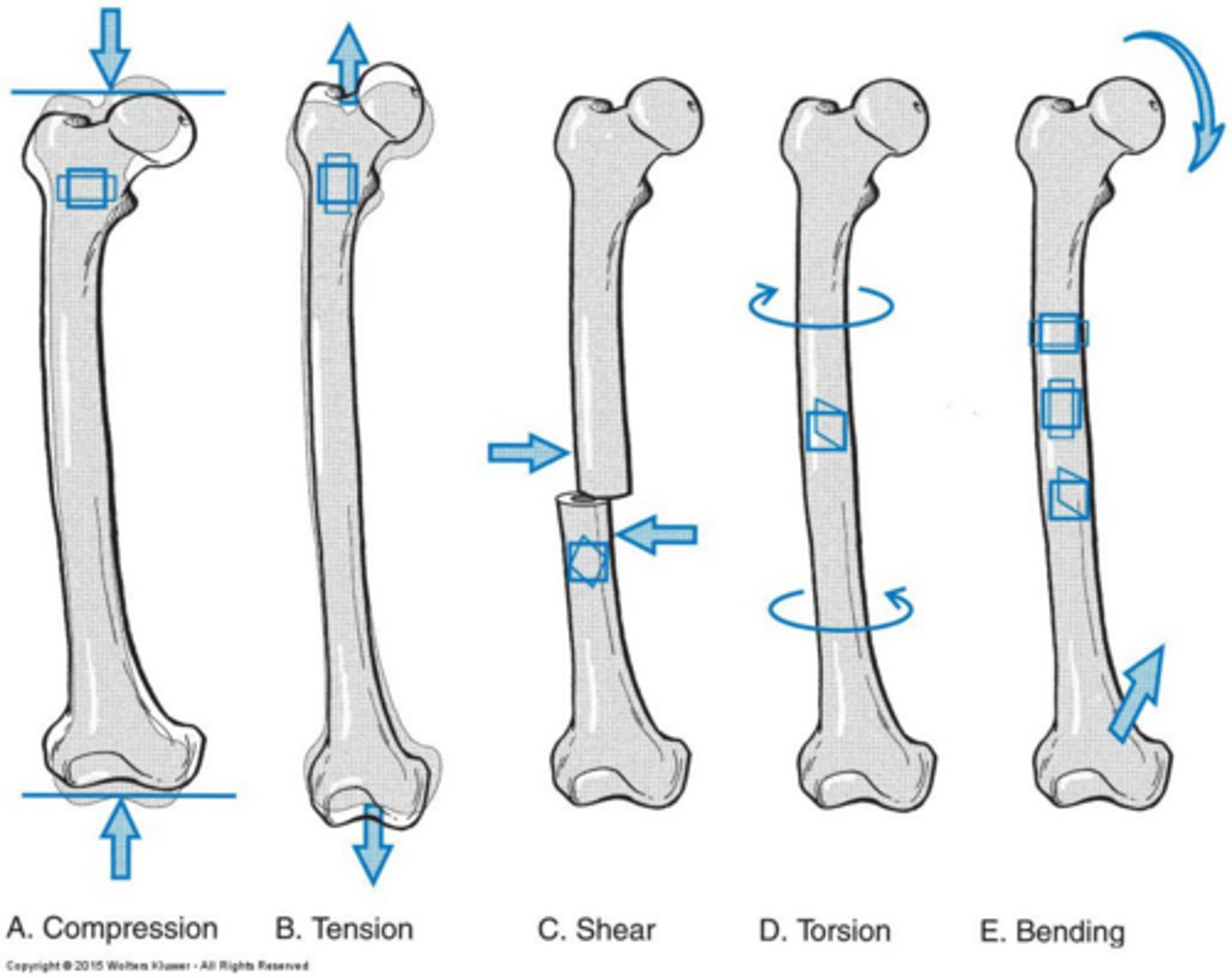
What causes the forces acting on bones?
Gravity and muscle force are primary contributors.
What are the two types of fibrocartilage?
White fibrocartilage (more collagen than elastin, found in intervertebral discs) and yellow fibrocartilage (more elastin than collagen, found in ears).
What is the primary type of cartilage found in joint surfaces?
Hyaline cartilage, also known as articular cartilage.
What is the thickness range of articular cartilage?
From 1 to 7 mm, depending on the joint.
How does the thickness of articular cartilage vary in the elbow and patella?
In the elbow, cartilage is thin due to surface area and forces; in the patella, the under surface is 5-7 mm thick due to small surface area.
What is the vascularity of articular cartilage?
Articular cartilage is avascular, receiving nutrition from synovial fluid.
What is the composition of articular cartilage?
60-80% water, 2-10% chondrocytes, type II collagen, and proteoglycans.
What is the role of chondrocytes in articular cartilage?
Chondrocytes are responsible for the development and repair of the extracellular matrix (ECM).
What is the structure of a proteoglycan molecule?
It has a bottle brush design with hyaluronan as the spine and GAG chains like keratin sulfate and chondroitin sulfate attached.
How does articular cartilage receive nutrients?
Nutrients diffuse through synovial fluid, with fluid exuded through pores in Zone 1.
What are the four main roles of articular cartilage?
Load redistribution, lubrication, compressive force transmission, and protection of bone.
How does articular cartilage reduce contact stresses?
It reduces contact stresses by 50% through fluid pressure and collagen resistance to tension.
What is the coefficient of friction for articular cartilage?
It has a very low coefficient of friction, ranging from 0.001 to 0.05.
What happens to fluid pressure in healthy vs. pathological articular cartilage?
In healthy cartilage, low permeability prolongs fluid retention, while pathological conditions lead to increased fluid loss and deformation.
What mechanical behaviors characterize articular cartilage?
Articular cartilage is anisotropic and viscoelastic.
What occurs during constant low-level loading of articular cartilage?
It leads to creep, where there is a gradual increase in strain/deformation.
What is the effect of high-speed loading on articular cartilage?
High-speed loading results in stiffer cartilage, affecting deformation and load distribution.
What is the impact of immobilization on articular cartilage?
It decreases fluid flow and nutrition, leading to degeneration of articular cartilage.
What are the effects of aging on articular cartilage?
Aging leads to decreased water content, increased stiffness, and smaller proteoglycan size, reducing load distribution.
What factors influence contact pressure in joints?
Contact pressure is influenced by contact force, contact area, and alignment.
What are the ways to change contact pressure?
Decrease contact force, increase contact area, decrease body weight, increase shock absorption, stretch tight structures, and decrease speed of application.
Why is healing of articular cartilage poor?
Chondrocytes are slow to produce cartilage, and there is very little blood supply, leading to ineffective healing.
What are the consequences of osteoarthritis on articular cartilage?
Osteoarthritis leads to damage, inflammation, and destruction of articular cartilage.
What is the role of hyaluronic acid in articular cartilage?
Hyaluronic acid is important for lubrication and maintaining low friction in joints.
What happens to articular cartilage under compression?
Articular cartilage develops creep and stress relaxation with constant compression.
What is the significance of intermittent joint loading?
Intermittent joint loading is essential for maintaining the structure and function of articular cartilage.
What are the main objectives of the study of Tendons and Ligaments?
Understand their anatomy, mechanisms of injury, mechanical behavior, viscoelastic properties, and effects of pregnancy, diabetes, immobilization, and aging.
What model describes muscle-tendon interaction?
Hill Model of Muscle-Tendon Interaction, which includes Series Elastic Components (SEC), Parallel Elastic Components (PEC), and Contractile Components (CC).
What is the function of Muscle Spindles?
They detect stretch of the muscle and send afferent information to the spinal cord, leading to an immediate efferent impulse to activate the muscle.
What do Golgi Tendon Organs (GTO) monitor?
They monitor force or tension in the muscle and provide reflexive inhibition to prevent injury.
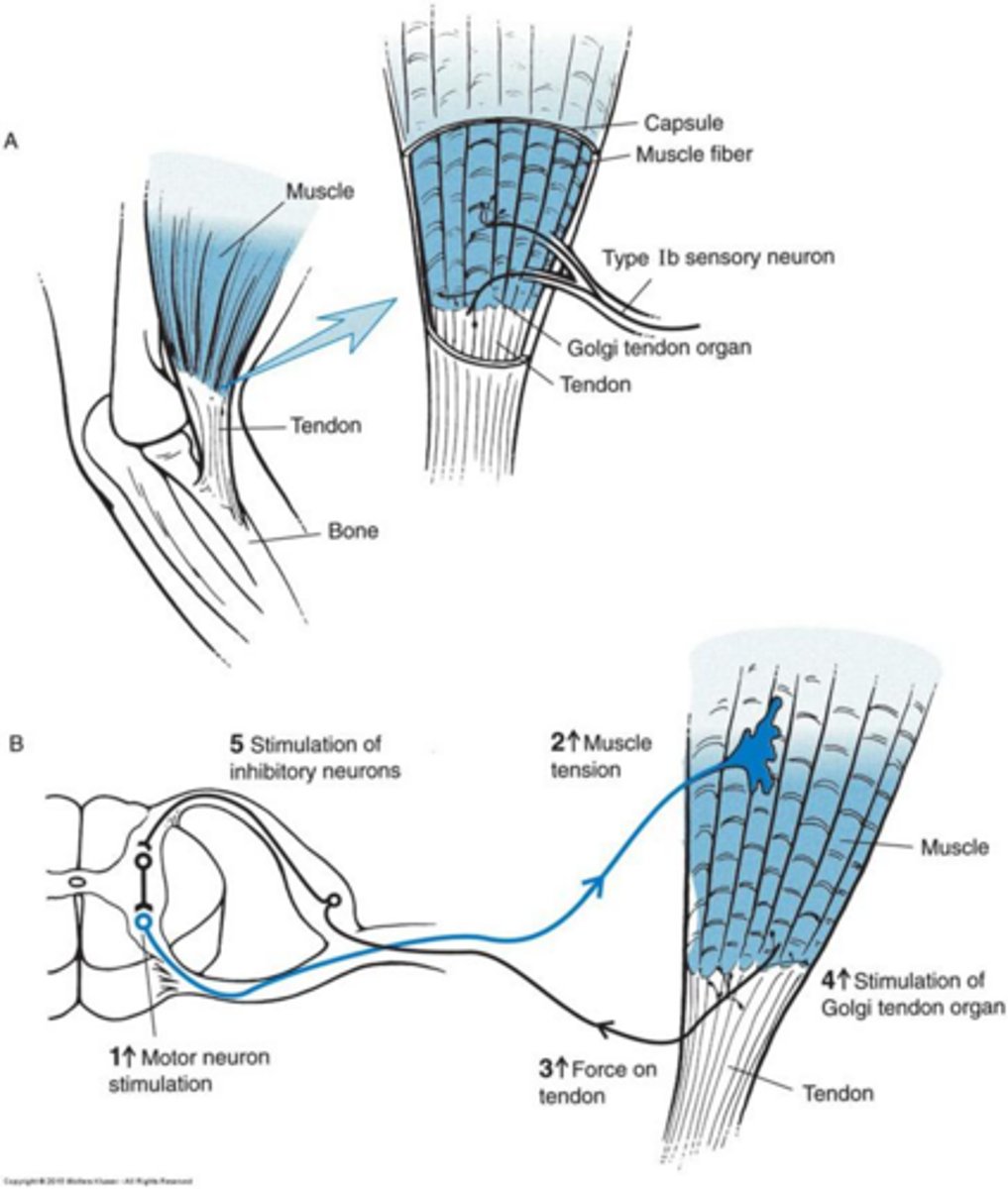
How are Tendons and Ligaments anatomically arranged?
Tendons are arranged in parallel bundles, while ligaments are arranged in a haphazard fashion along stress lines.
What type of collagen do tendons primarily contain?
Type I collagen fibrils.
What is the primary difference between elastin and collagen?
Elastin allows more extensibility, while collagen provides tensile strength.
What is the blood supply difference between tendons and ligaments?
Tendons are better vascularized than ligaments, which are hypovascular and have a slower healing process.
What happens to tendons and ligaments after immobilization?
They lose strength rapidly, with a 50% loss of strength after 6 weeks.
What is the effect of aging on tendons and ligaments?
Collagen fibrils decrease in size, water content decreases, and collagen concentration decreases, leading to reduced stiffness.
What is the typical structure of a neuron?
A neuron consists of a cell body, dendrites, and an axon.
What is the relationship between axon size and conduction velocity?
Conduction velocity is proportional to the size of the axon.
What are the connective tissue layers of peripheral nerves?
Epineurium (outermost layer), Perineurium (covers each fascicle), and Endoneurium (covers axons).
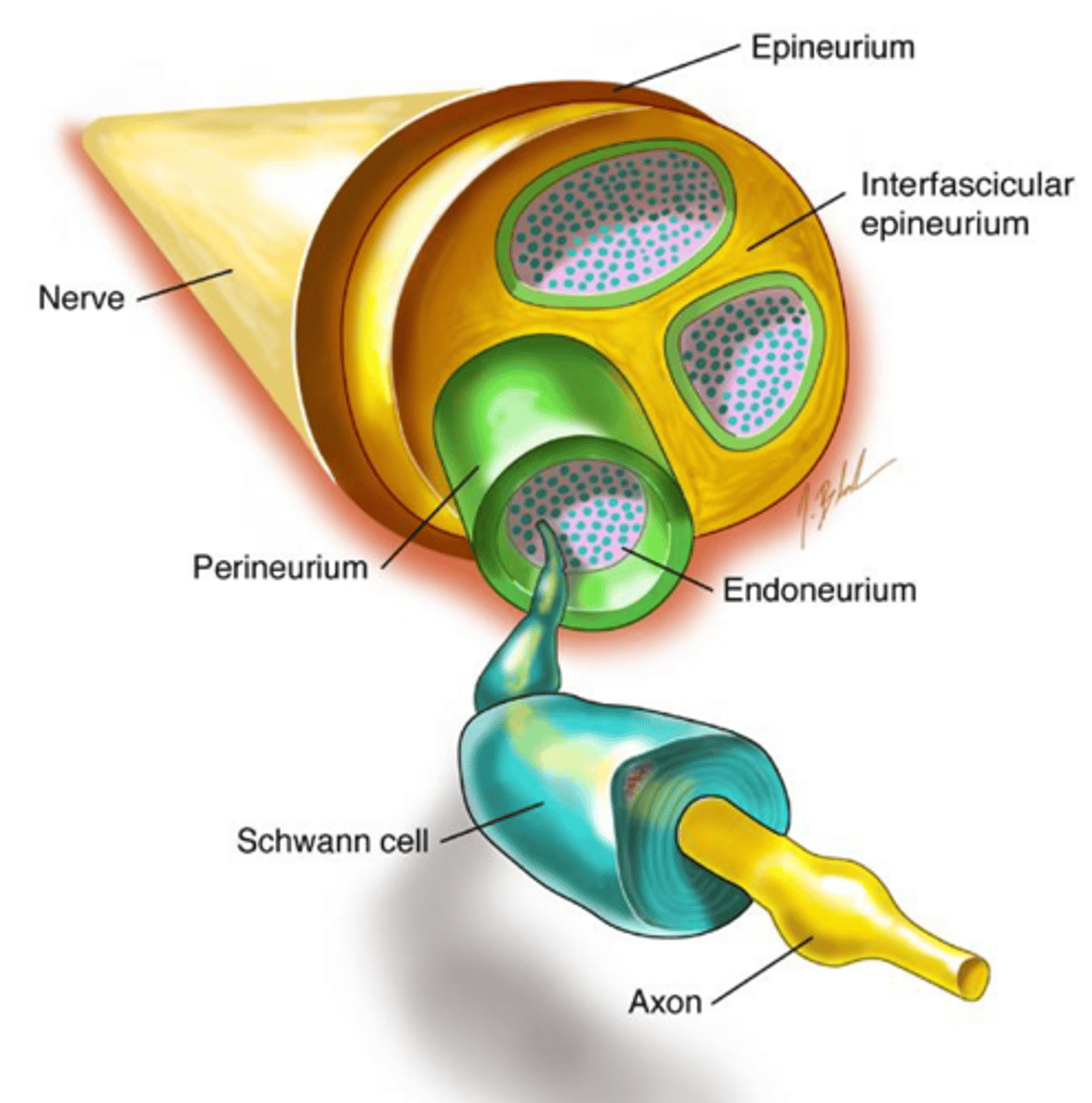
What happens to peripheral nerves under stretching?
8% strain decreases microcirculation, 15% strain disrupts axons, and complete failure occurs at 25-30% strain.
What are the critical pressure levels for nerve compression injuries?
30 mmHg for 4-6 hours causes functional changes; 80 mmHg leads to complete breakdown of circulation.
What types of compression can affect nerves?
Direct compression (between two structures) and indirect compression (overall pressure increase).
What is the effect of corticosteroid injections on tendons?
They weaken the tensile strength of injected tendons and can lead to loss of fatty tissue.
What is the impact of pregnancy on ligaments and tendons?
Tensile strength decreases during the third trimester and postpartum due to increased hormone Relaxin.
What are the effects of diabetes on tendons?
Higher rates of tendon contractures, tendinopathies, joint stiffness, capsulitis, and osteoporosis.
What is the role of ligaments in joint stability?
They maintain the relationship of articular surfaces, resist non-physiologic joint movements, and assist in physiologic movements.
What is the significance of the Sharpey's fibers?
They are formed from the endotenon and help anchor tendons to bone.
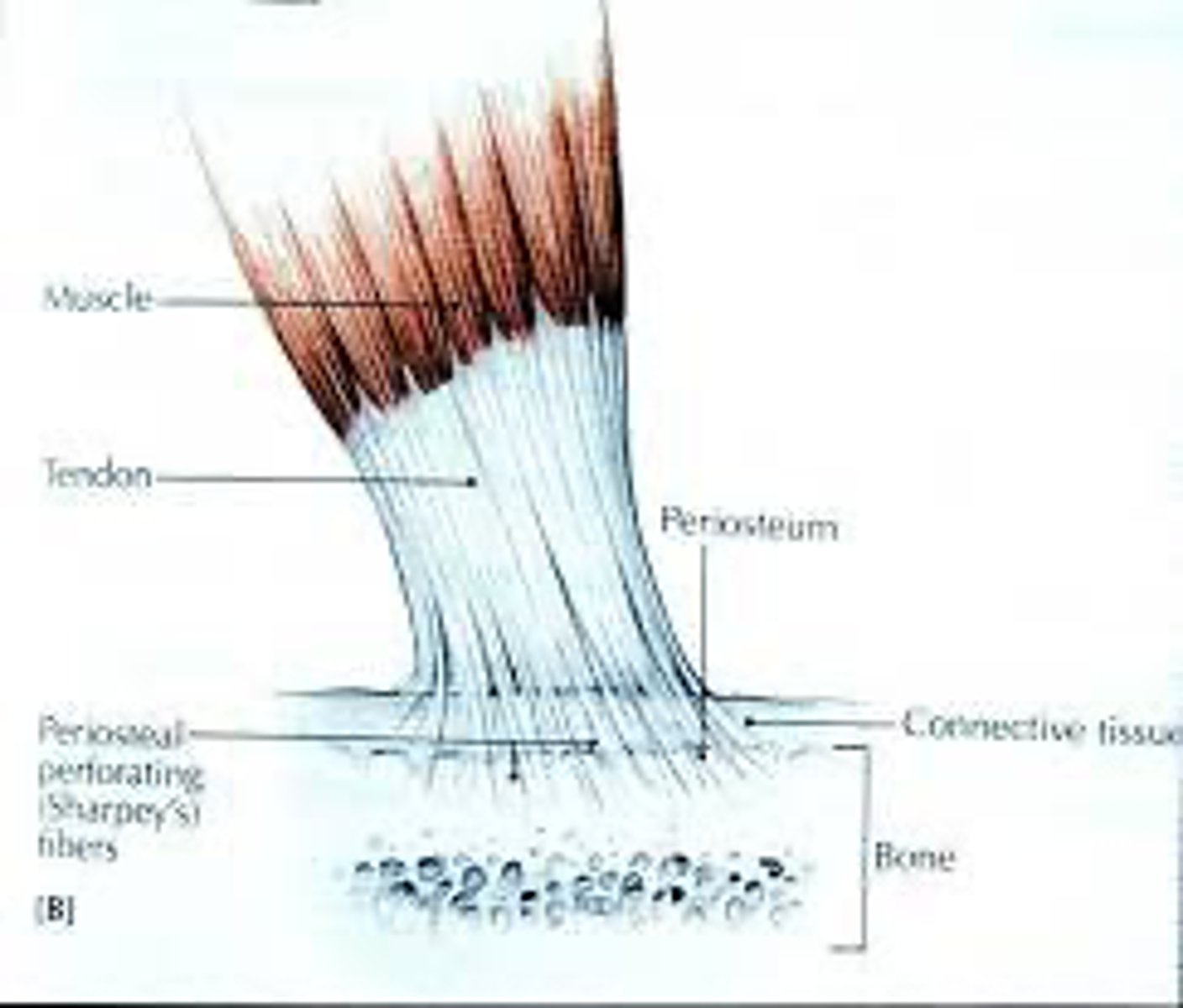
What is the primary function of the Golgi ligament endings?
They contribute to position sense in the joint.
What is the consequence of fast strain rates on ligaments?
They increase ultimate strength but can lead to mid-substance tears if strain exceeds yield.
What are the symptoms of peripheral nerve stretching injuries?
Severe burning, tingling, and numbness that may resolve in minutes, days, or months.
What is the typical recovery timeline for ACL strength after immobilization?
Strength properties decrease after immobilization, with recovery resembling baseline after 12 months of rehabilitation.
What is the role of fibroblasts in tendon structure?
Fibroblasts are involved in the maintenance and repair of tendon tissue.
What is the primary function of the sarcoplasmic reticulum in muscle cells?
Responsible for release and uptake of calcium ions.
What are the two types of myofilaments in muscle tissue?
Actin (thin filament) and Myosin (thick filament).
What is the role of tropomyosin in muscle contraction?
Covers actin binding sites until calcium binds to troponin.
What mechanism describes muscle shortening during contraction?
Sliding Filament Mechanism.
What are the components of the Hill Model of Muscle-Tendon Interaction?
Series elastic components (SEC), parallel elastic components (PEC), and contractile component (CC).
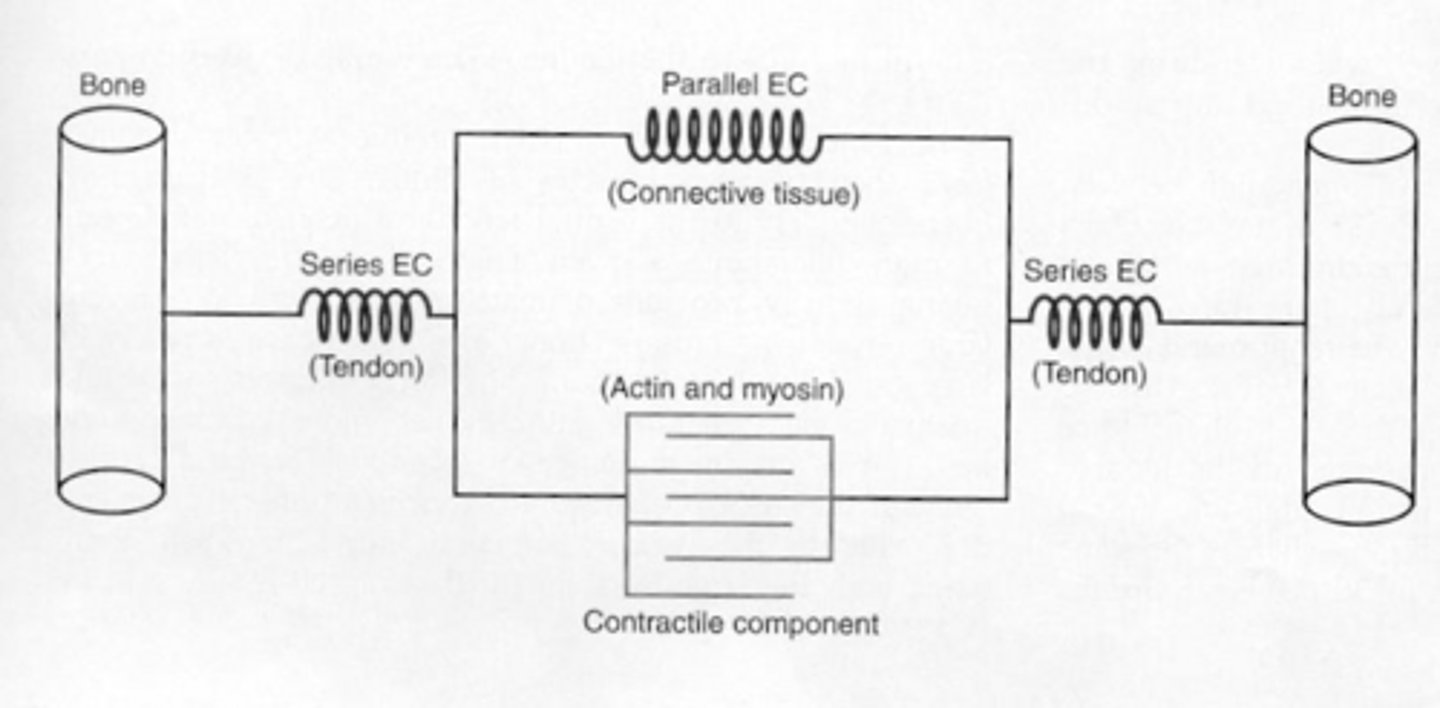
What are the two primary functions of muscles?
Mobility (produce motion) and Stability (maintain posture and stabilize joints).