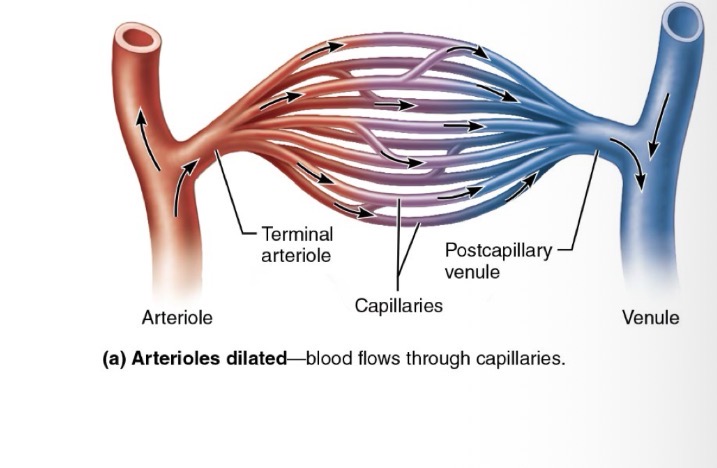
chapter 19: blood vessels
1/60
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
61 Terms
Lumen
The inside space, cavity, or channel within a tubular structure like blood vessels or organs
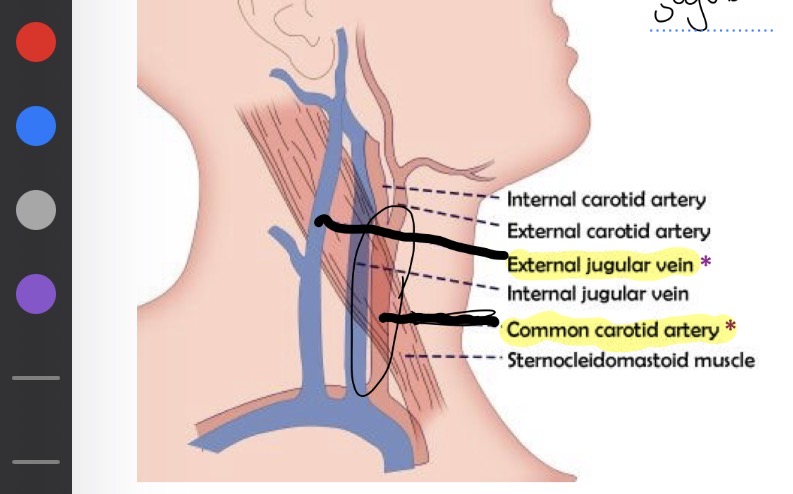
Vein and artery in neck
External jugular : vein
Common carotid : artery
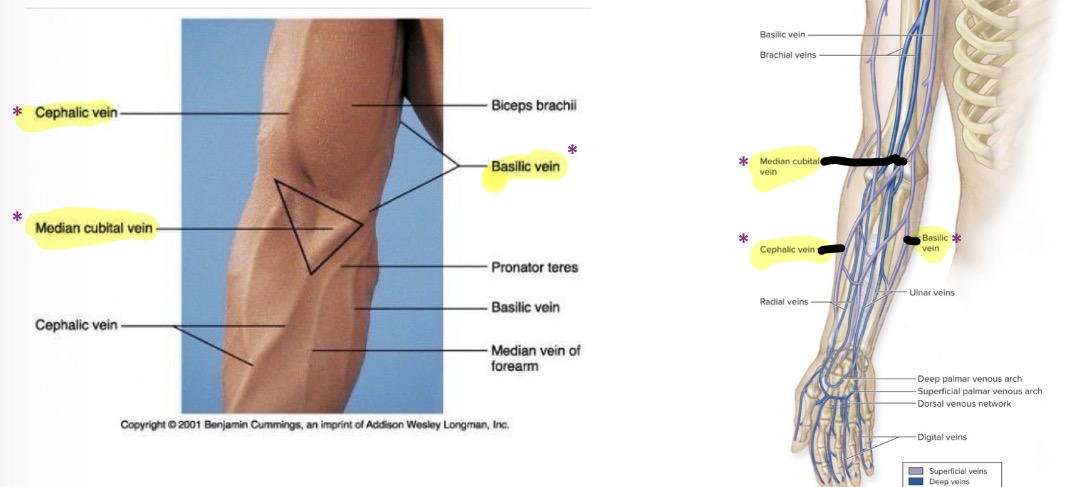
Veins in arms
Cephalon vein
Basilic vein
Median cubital vein
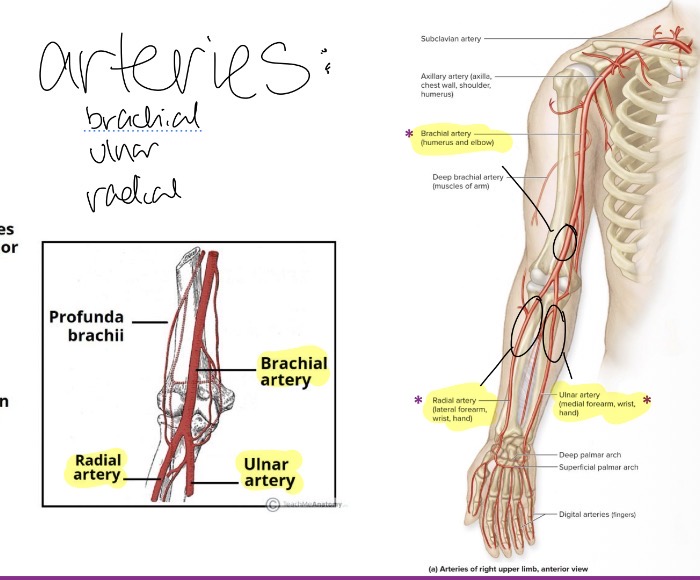
Arteries in arms
Brachial
Radial
Ulnar
Arteries in the abdomen
Mesentric arteries
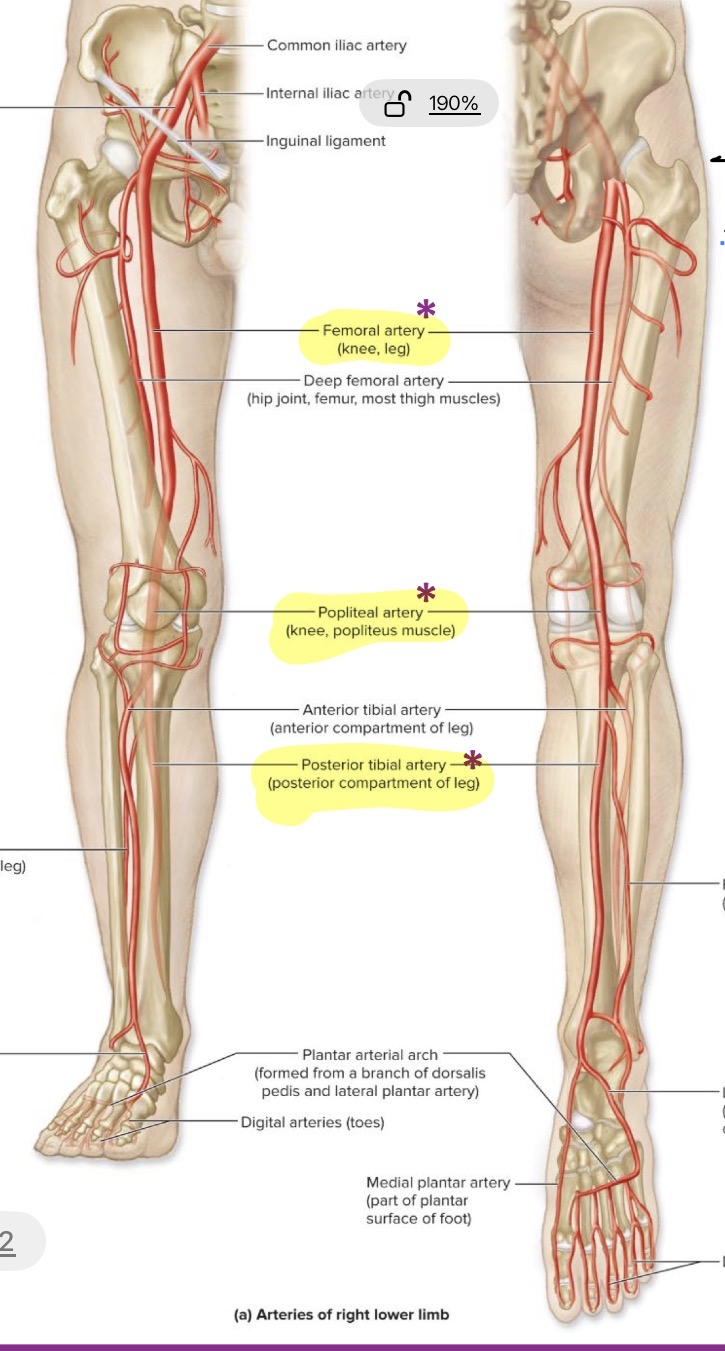
Arteries in the leg
Femoral
Poplitel
Posterior tibial
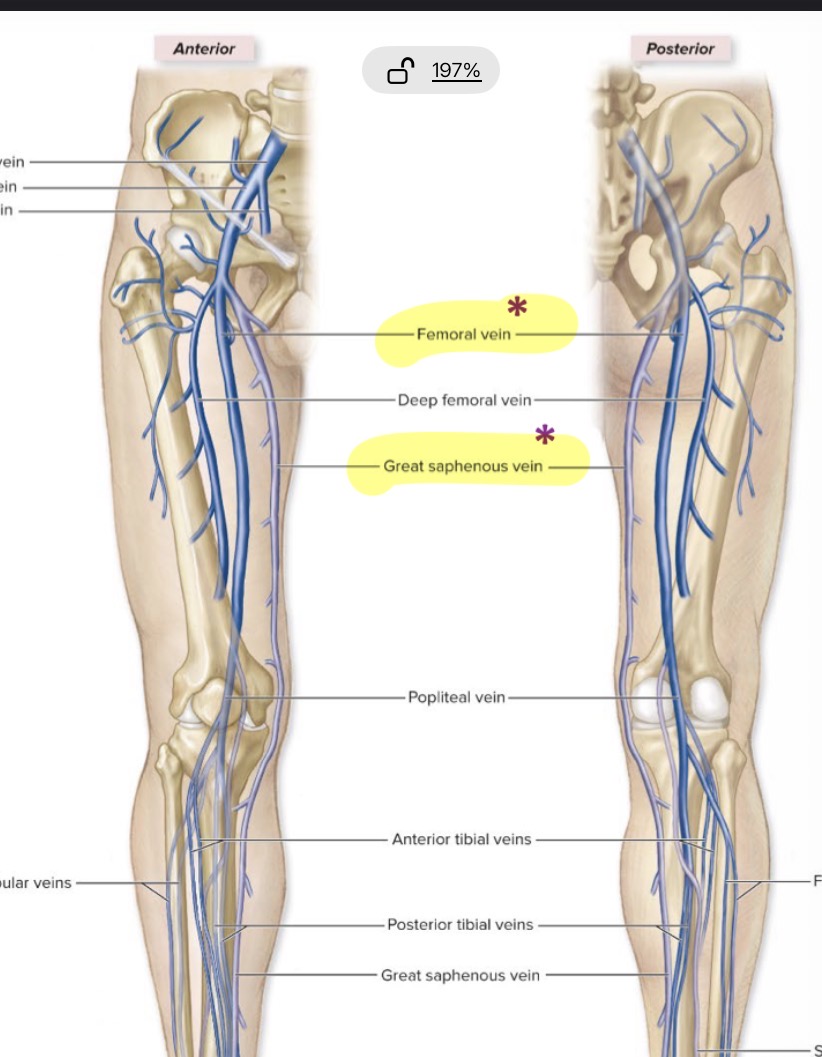
Veins in the leg
Femoral
Great saphenous
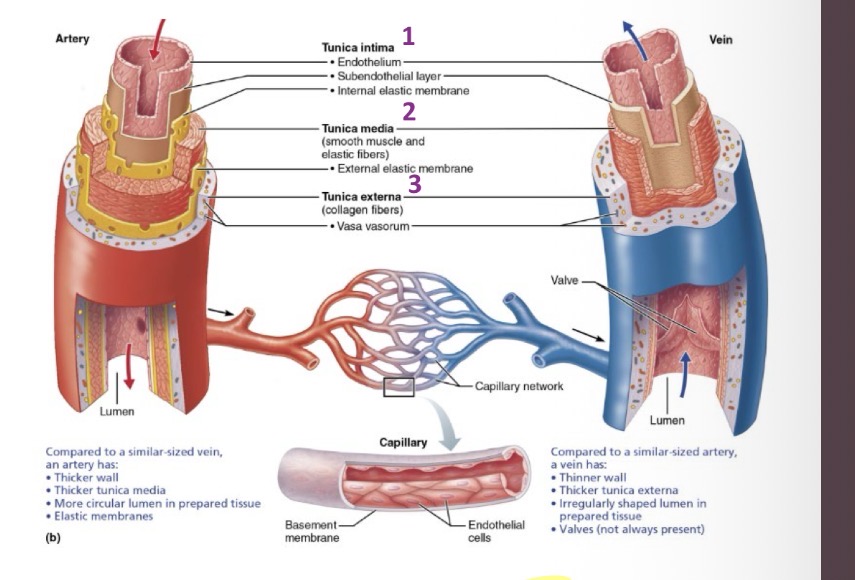
Layers of blood vessels
Intima
Media
3.Externa
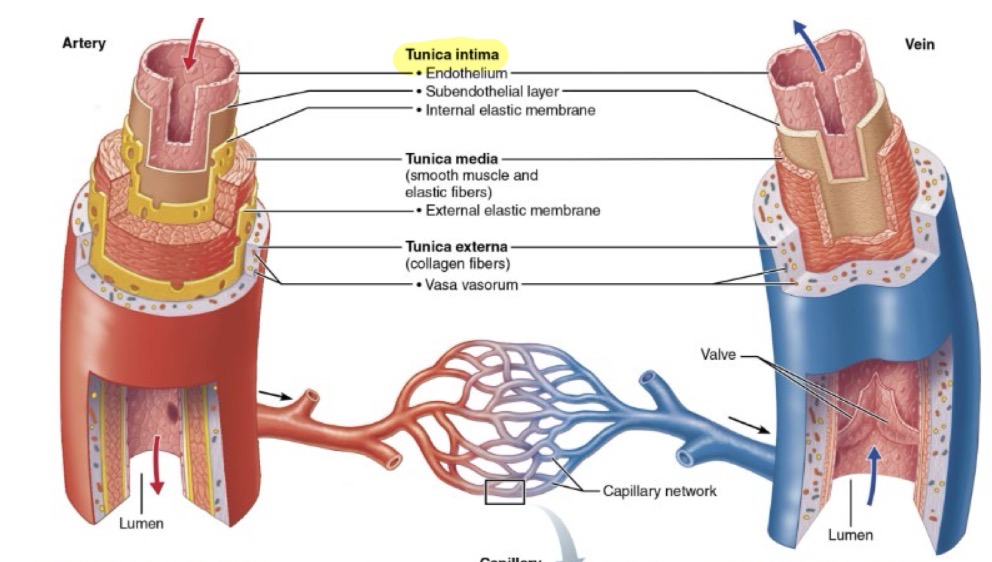
Tunica Intima
The innermost layer of a vessel wall
Composition: Endothelium (simple squamous epithelium)
Functions: selectively permeable barrier, secretes chemicals, repels blood cells and platelets, and inflammation
only layer containing capillaries
Tunica Media
The middle layer of a vessel wall
Composition: Smooth muscle, elastic tissue, and collagen (amount varies)
Functions: Strengthens vessels to prevent rupture and facilitates vasomotion (vasoconstriction and vasodilation)
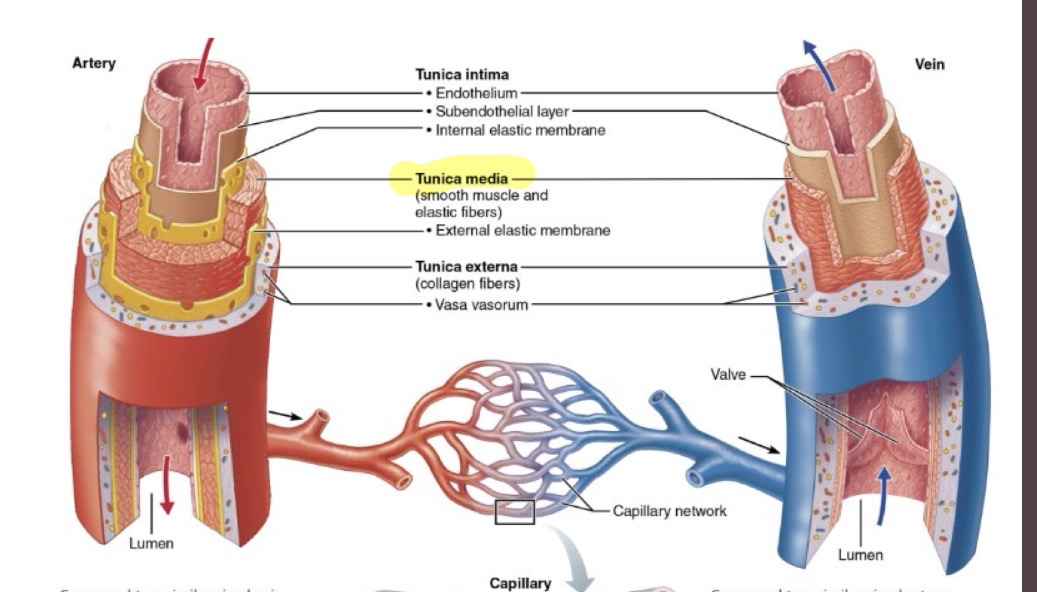
Tunica Externa
The outermost layer of a vessel wall
Composition: Loose connective tissue
Functions: Protects and anchors the vessel; provides a passage for nerves and lymphatic vessels
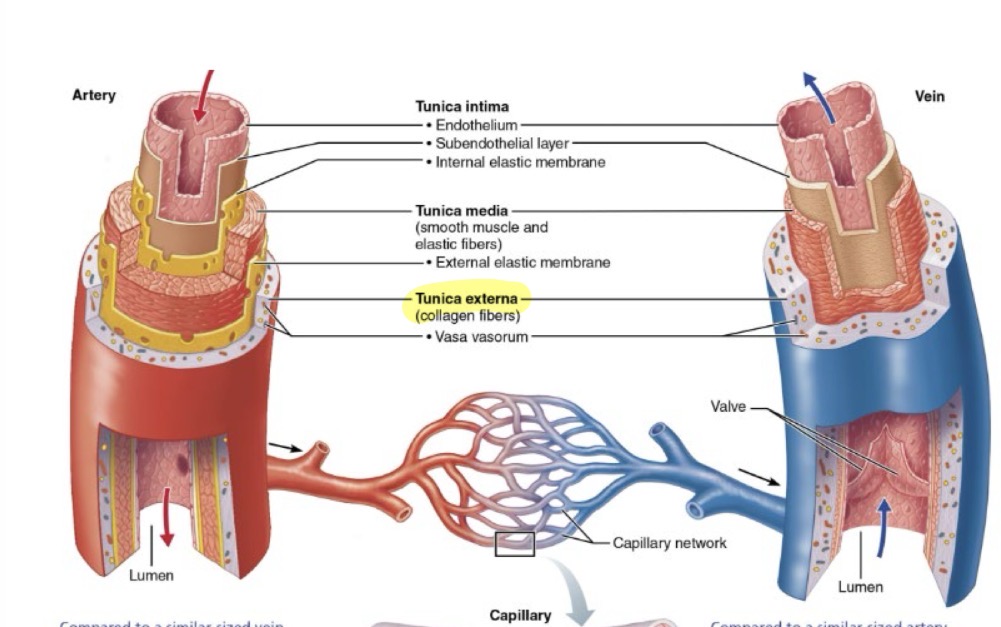
Vaso Vasorum
"blood vessel of blood vessels"; small vessels found in the tunica externa that supply larger blood vessels
Arteries
Vessels designed to withstand surges of pressure that carry blood away from the heart.
- thicker walls and more smooth muscle than veins
Elastic Arteries
largest diameter arteries (e.g., aorta, pulmonary trunk)
Composition: Elastic tunica media
Functions: Reduce the effects of blood pressure surges by expanding during systole and recoiling during diastole
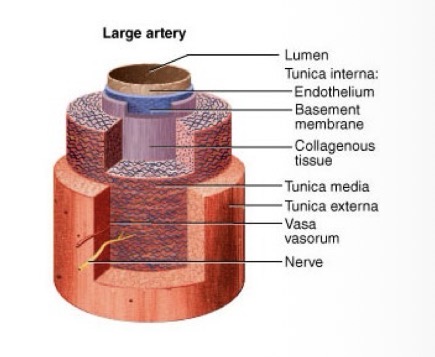
Muscular Arteries
Thick-walled arteries (e.g., brachial artery, femoral artery).
Composition: Thick smooth muscle
Functions: Deliver blood to specific organs and adjust flow based on demand
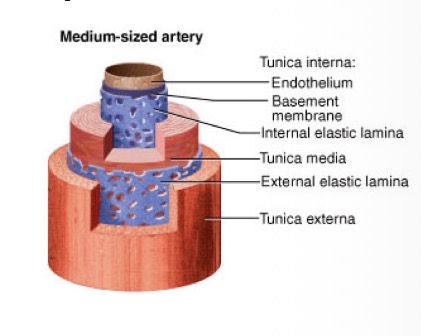
Arterioles (arteries)
Small vessels that lead into capillary beds
Composition: Variable smooth muscle layers and little elastic tissue
Functions: Primary controllers of blood flow; most responsible for peripheral resistance (PR) and significantly affecting blood pressure
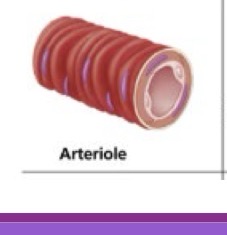
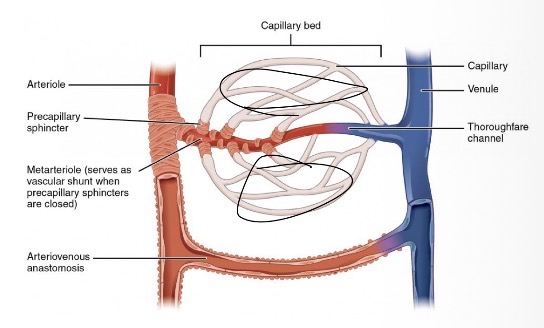
Capillaries (Exchange Vessels)
Microscopic connections between arteries and veins
consisting of a single layer of endothelial cells and a sparse basal lamina
Their diameter allows only a single RBC to pass at a time to slow velocity for exchange
Veins (Capacitance Vessels)
Vessels that carry blood towards the heart
They have thinner walls, larger lumens, and often contain valves to prevent backflow
At rest, they act as blood reservoirs, containing about 60% of the body's blood volume
Anastomoses
Branching of vessels that provide collateral (alternative) pathways for blood flow
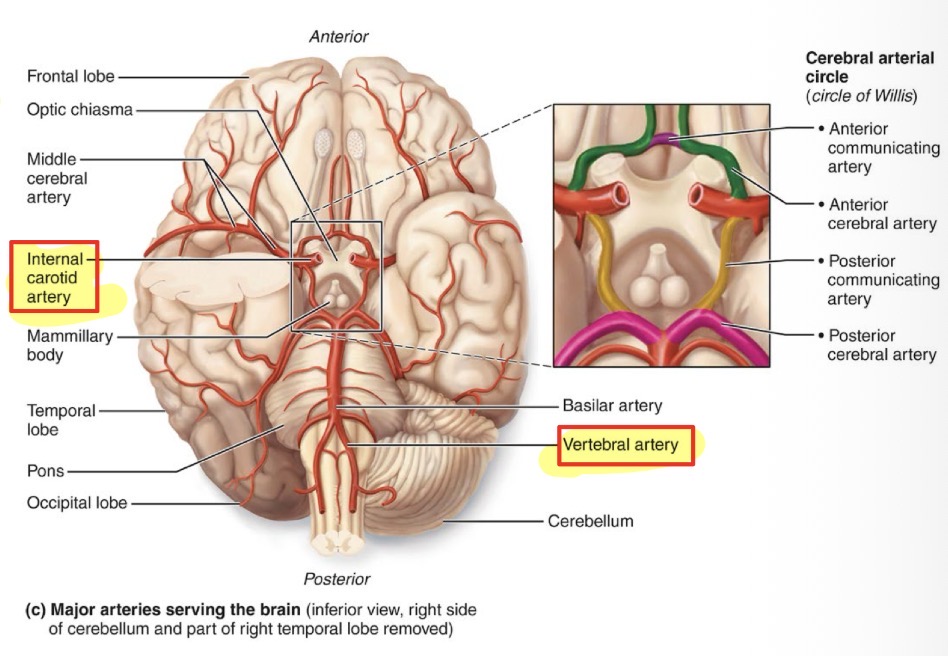
Cerebral Arterial Circle (Circle of Willis)
A ring or pentagon-shaped structure of arteries at the base of the brain where the internal carotid and vertebral artery pathways connect
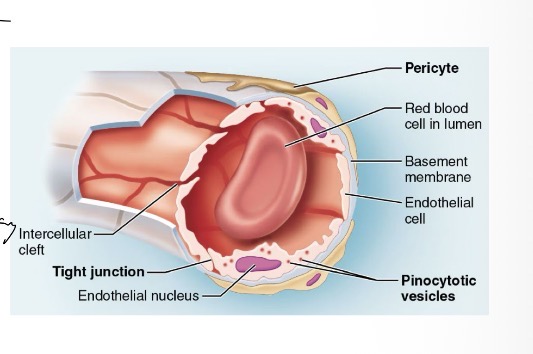
Continuous Capillaries
cells are tightly held together with intercellular clefts that allow small molecules to pass while holding back large molecules
Found in most tissues
May contain pericytes
Fenestrated Capillaries
Contain fenestrations (pores) for greater permeability of water-soluble substances (no formed elements)
kidneys and endocrine glands
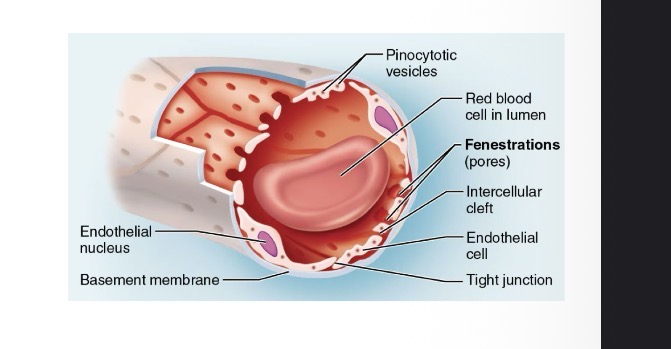
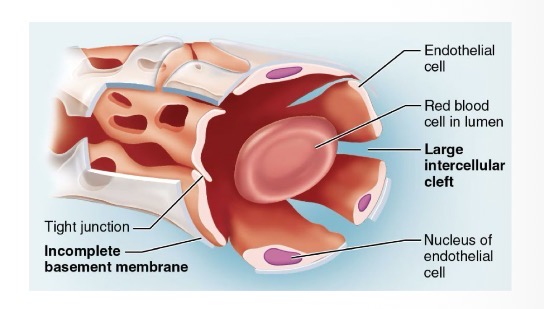
Sinusoids
Irregular, blood-filled spaces with large fenestrations and an incomplete basement membrane, allowing formed elements (like blood cells) to pass
Found in the liver, bone marrow, and spleen
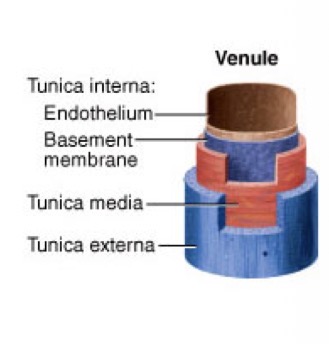
Venules
Include post-capillary venules (extremely porous) and muscular venules (thin tunica media and externa)
Post-capillary venules
Smallest venous vessels that collect blood directly from capillary beds
endothelial layer and basement membrane with scattered pericytes, lacking smooth muscle
Extremely porous (high permeability)
Muscular Venules
Small blood vessels that collect blood from capillaries and transition into larger veins
thin tunic media and externa, endothelium of simple squamous cells
Follow postcapillary venules
Medium veins
All three tunics, thick media, large lumen, valves
Venous Sinuses
Veins with thin walls, large lumens, and no smooth muscle, meaning they cannot perform vasoconstriction (e.g., coronary sinus)
Large Veins
Vessels with all three layers and a thick tunica externa, but no valves
Blood Flow (ml/min)
The volume of blood moving through a tissue in a given time; equivalent to cardiac output
Blood Pressure (mmHg)
The force blood exerts against a vessel wall. Clinically, this refers to systemic arterial pressure (e.g., 120/80)
Blood Perfusion (ml/min/g)
The specific flow of blood through the capillary beds
acts as an "on/off switch" for nutrient exchange
Resistance
Friction encountered by blood through vessels
which opposes flow
Blood Viscosity
The "thickness" of blood
directly proportional to resistance and oppositely proportional to flow
decreases with anemia
increases with blood doping or dehydration
Blood Vessel Length
The distance blood must travel
directly proportional to resistance and oppositely proportional to flow
Blood Vessel Diameter
The most influential factor for resistance and friction
controlled by the Sympathetic Nervous System (SNS)
Laminar Flow
Normal, smooth, silent, and efficient blood flow
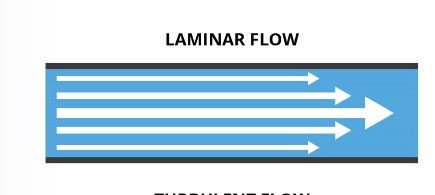
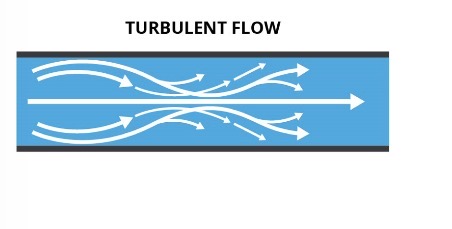
Turbulent Flow
Non-smooth flow caused by obstructions like plaques, heart murmurs, or valve stenosis
Pulse Pressure (PP)
Calculated as SBP – DBP
measures pressure surges and indicates the force of each heartbeat and artery health (average is 40)
Mean Arterial Pressure (MAP)
average of pressures throughout the cardiac cycle: calculated as DBP + 1/3 (PP). It is the most important index of perfusion; it must be 60 or higher for organs to receive enough blood
Skeletal Muscle Pump
mechanical venous return mechanism where contracting muscles (like the calves/gastrocnemius, the "second heart") press against veins to propel blood toward the heart
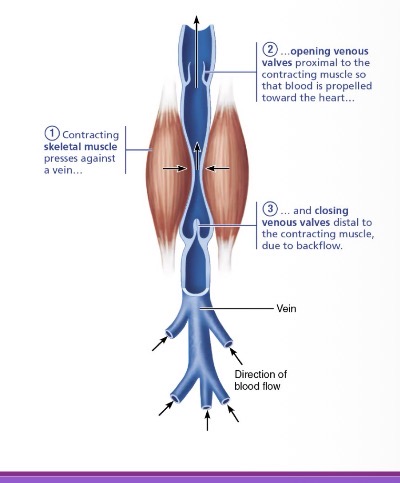
Respiratory Pump
mechanical venous return mechanism where deep breathing changes pressure in the abdomen and thorax to squeeze blood toward the heart
Sympathetic Vasoconstriction
neural (involuntary) mechanism where the sympathetic nervous system signals smooth muscle in veins to constrict to help return blood to the heart
Medulla Oblongata
brainstem's "autopilot" for the cardiovascular system
containing the Vasomotor Center (controls diameter) and the Cardioacceleratory/inhibitory centers (regulate heart rate)
Vasomotor Center
Controls vessel diameter vis sympathetic NS
Cardioacceleratory/inhibitory Center
Regulates heart rate using sympathies NS
Baroreflex
negative feedback mechanism using pressure-sensitive mechanoreceptors in the carotid sinuses and aortic arch to reduce HR, CO, and BP during acute surges (e.g., standing up quickly)
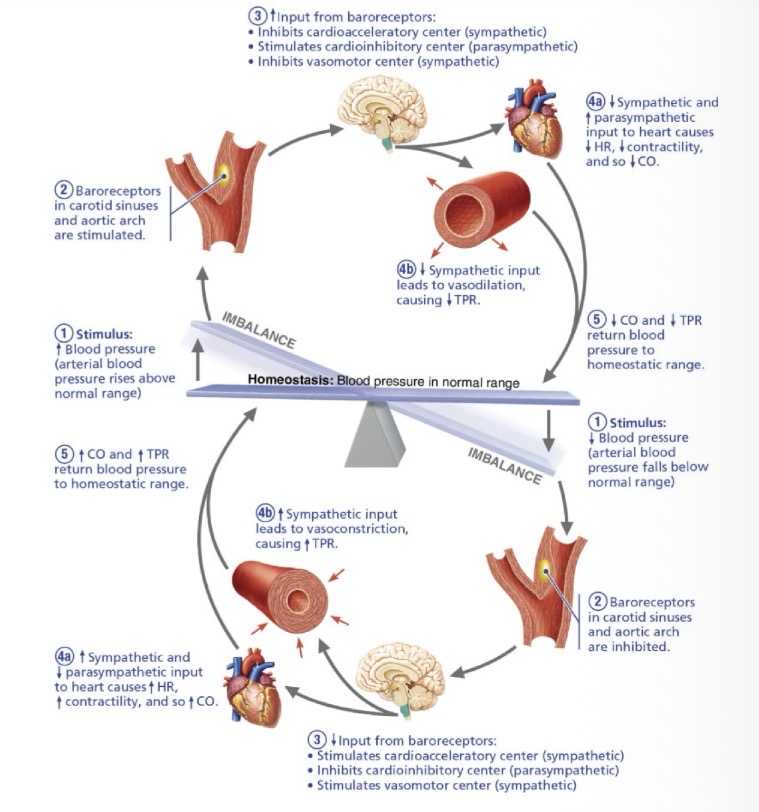
Chemoreflex
response to chemical changes sensed by receptors (↓pH, ↓O2, ↑CO2)
primary role is adjusting respiration
secondary role is using vasomotor changes to increase perfusion
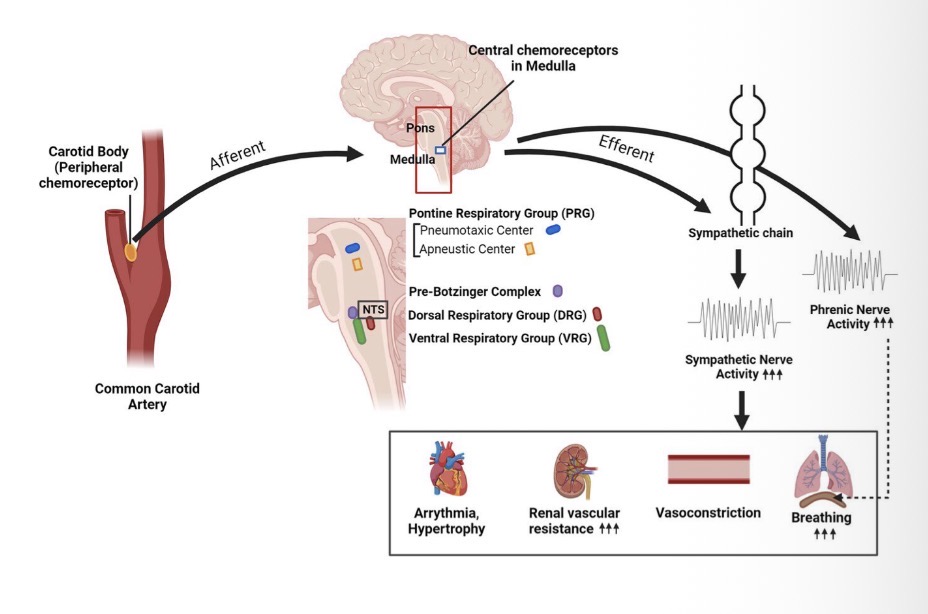
Vasoconstriction
Vessels diameter narrows
Vasodilation
Vessels diameter widen
Vasomotor changes
Changes in diameter of blood vessels
Diffusion
primary mode of exchange where substances move from high to low concentration
Small solutes (O2) diffuse through endothelial cells
large solutes (proteins) pass through fenestrations or gaps
Transcytosis
form of vesicular transport used to move specific macromolecules across the endothelial cell
Pinocytosis
non-specific form of transcytosis for "in-between" sized molecules
Exocytosis
final step of vesicular transport where a vesicle fuses with the cell membrane to release contents into the interstitial fluid or bloodstream
Modes of capillary exchange
Diffusion
Vesicular transport
transcytosis
Pinocytosis
exocytosis
Mechanisms of venous return
Skeletal muscle pump
Respiratory pump
Sympathetic vasoconstriction
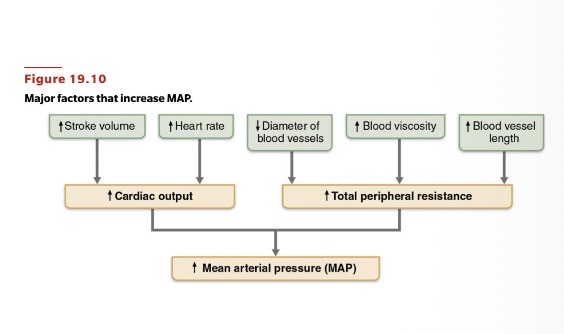
Determinants of Blood Pressure
1 total peripheral resistance
2 cardiac output
3 blood volume
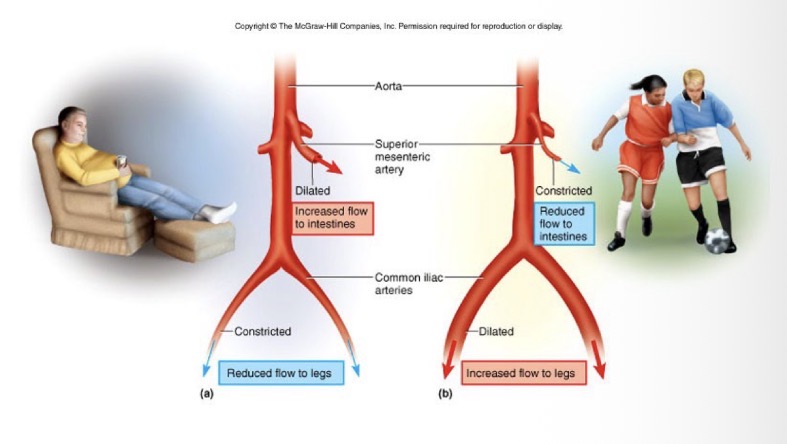
Redirection of Blood Flow
Pressure downstream decreases
Pressure upstream increase
Blood takes the path of least resistance
Capillary exchange of nutrients
Blood to capillary to interstitial space to tissue