Lecture 24: GI Physiology
1/185
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
186 Terms
What organs make up the alimentary canal?
Mouth, esophagus, stomach, small intestine, large intestine, rectum, and the anus
What are the accessory digestive organs?
Salivary glands, liver, gallbladder, pancreas.
The alimentary canal is approximately ______ feet long
30
The GI tract is divided by ______ and ______ that regulate flow.
Sphincters; valves.
T/F: The pyloric valve separates the ileum from the cecum.
False: the ileocecal valve separates the ileum from the cecum; the pyloric valve separates the stomach from the duodenum.
Which three accessory organs are shown connected to the duodenum?
Liver, gallbladder, and pancreas.
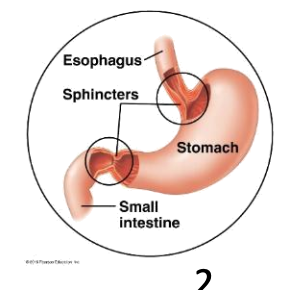
Which structure is shown between the stomach and small intestine?
The pyloric sphincter
Which organ is shown inferior to the liver and stores bile?
Gallbladder
How many liters of fluid enter the GI tract daily?
9
How many liters are absorbed by the small intestine?
7.5
Daily ingestion contributes ______ liters of fluid to the GI tract.
2
Daily secretions contribute ______ liters of fluid to the GI tract.
7
T/F: Most GI secretions are reabsorbed.
True: 9L enter and 9L are reabsorbed
Which secretion contributes the largest volume to GI fluid?
Gastric secretions (2.0 L/day).
What is the definition of secretion?
Movement of substances from cells into the lumen or ECF
What is the definition of digestion?
Chemical and mechanical breakdown of food into absorbable units.
What is the definition of absorption?
Movement of substances from lumen to ECF.
Motility is the movement of ______ through the GI tract.
Chyme
T/F: Excretion removes large amounts of metabolic waste.
False: fecal matter contains very little metabolic waste; most is undigested material and bacteria.
Which macromolecule is broken down into amino acids?
Proteins
Which macromolecule is broken down into monosaccharides?
Carbohydrates
Which macromolecule is broken down into nucleotides?
Nucleic acids
What do lipids break down into?
Monoglycerides and free fatty acids
Which enzymes break down polysaccharides?
Carbohydrate‑digesting enzymes.
Which products of fat digestion enter absorption?
Glycerol and fatty acids
Which digestive enzymes are bound to apical membranes?
Brush‑border enzymes
Which nutrient type is absorbed into lacteals?
Fats
What are the four layers of the GI tract wall?
Mucosa, submucosa, muscularis externa, serosa
What are the three components of the mucosa?
Epithelium, lamina propria, and muscularis mucosae.
The submucosa contains the ______ plexus.
submucosal
The muscularis externa contains the ______ plexus.
Myenteric
T/F: The serosa is continuous with the mesentery
True
Which structures increase surface area by 600×?
Villi, crypts, and microvilli
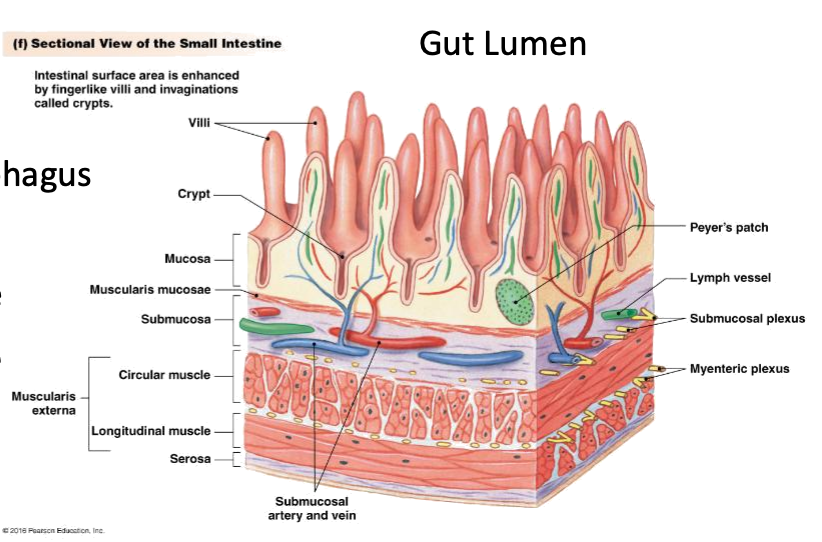
Which immune structure is shown in the mucosa?
Peyer’s Patch
Which vessel type absorbs fats?
Lacteals
Which cells secrete mucus?
Goblet cells
Which cells secrete hormones?
Enteroendocrine cells
What type of epithelium lines the small intestine?
Simple columnar epithelium with microvilli.
What is the function of enteroendocrine cells?
Secrete hormones.
Stem cells in the crypts replace ______ cells.
damaged
The brush border is formed by ______.
Microvilli
T/F: Crypt cells secrete digestive enzymes.
False: they secrete ions and water; enzymes come from enterocytes or pancreas.
Which vessels run inside each villus?
Capillaries and lacteals
Which cells are shown transporting nutrients?
Enterocytes
Which cells divide to replace the epithelium?
Stem cells in crypts
What type of muscle makes up the muscularis externa?
Smooth muscle
Which nervous system provides input to the myenteric plexus?
ANS
The myenteric plexus primarily regulates ______.
Motility
The submucosal plexus primarily regulates ______.
secretion
T/F: The serosa is a thick muscular layer.
False: it is a thin connective tissue layer continuous with the peritoneum.
Which layer of the stomach contains the oblique muscle?
Muscularis externa.
Which layer of the stomach contains the gastric glands?
Mucosa
Which layer of the stomach contains the submucosal blood vessels?
Submucosa
Which stomach layer is the outermost?
Serosa
Which muscle layer in the stomach is responsible for peristalsis?
Circular and longitudinal layers of the muscularis externa.
What are the three modes of GI communication?
Endocrine, paracrine, and neurocrine.
What do endocrine cells in the gut “taste”?
Luminal contents
Histamine is released from ______ cells.
Enterochromaffin‑like (ECL) cells.
Somatostatin is released from ______ cells.
D
T/F: Paracrine signals enter the bloodstream before reaching their target.
False; they act locally in the interstitial fluid.
Where do endocrine hormones travel to reach their targets?
Through the bloodstream
What is the immediate environment where paracrine signals act?
Interstitial fluid
Which structure releases neurocrine transmitters?
Neurons
Which type of cell receives neurocrine signals?
Smooth muscle of gland cells
What are the two major plexuses of the ENS?
Myenteric and submucosal plexus
What type of neurons are found in the ENS?
Sensory, interneurons, and motor neurons.
The ENS can function independently of the ______.
CNS
The ENS increases the ______ of rhythmic contractions.
Intensity.
T/F: The ENS inhibits sphincter contraction.
True
Which plexus lies between the circular and longitudinal muscle layers?
Myenteric plexus
Which neurotransmitter is know to be inhibitory?
Norepinephrine
Which neurotransmitter is known to be excitatory?
Acetylcholine
Which cells detect luminal stimuli
Sensory neurons in the mucosa
What are slow‑wave potentials?
Cyclical depolarizations in GI smooth muscle.
What cells generate slow waves?
Interstitial cells of Cajal
Action potentials occur when slow waves exceed ______.
Threshold
The force of contraction depends on the number of ______.
Action potentials
T/F: Slow waves always cause contractions.
False: only slow waves that reach threshold trigger action potentials and contractions.
What happens when slow waves do not reach threshold?
No action potentials; no contraction.
What increases the amplitude of slow waves?
Parasympathetic stimulation (ACh).
What decreases the amplitude of slow waves?
Sympathetic stimulation (NE).
Which type of contraction lasts minutes to hours?
Tonic contractions
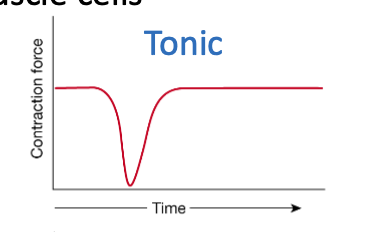
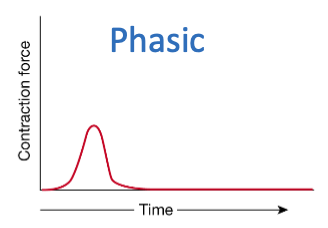
Which type of contraction lasts only seconds?
Phasic contractions.
What is a short reflex?
A reflex contained entirely within the ENS.
What is a long reflex?
A reflex involving the CNS.
The gastrocolic reflex increases ______ after eating.
Colon motility
The enterogastric reflex inhibits ______ activity.
Gastric
T/F: The vagovagal reflex involves both afferent and efferent vagus fibers.
True
Which organ signals the colon to contract after eating?
Stomach
Which phase of digestion begins with sight, smell, or thought of food?
Cephalic phase
Which system mediates the cephalic phase?
Parasympathetic nervous system.
What cells release gastrin?
G cells in the antrum and duodenum
What stimulates gastrin release?
Peptides, amino acids, stomach distention, GRP, ACh
Gastrin is inhibited by ______.
Somatostatin
Gastrin’s primary target cells are ______ and ______.
ECL cells; parietal cells
T/F: Gastrin is less potent than histamine at stimulating acid secretion.
False: gastrin is ~1500× more potent than histamine
Which neurotransmitter stimulates G cells?
GRP (gastrin‑releasing peptide)
Which cell releases histamine in response to gastrin?
ECL cell
Which receptor on parietal cells binds histamine?
H₂ receptor
Which cell releases somatostatin to inhibit gastrin?
D cell