Microbio Exam 3
1/38
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
39 Terms
D
Which of the following is an example of passive immunization?
A. natural infection
B. live, attenuated vaccine
C. mRNA vaccine
D. breast milk
D
The best protection against a second infection by a pathogen is which of the following?
A. IV immunoglobulin
B. subunit vaccine
C. live, attenuated vaccine
D. natural infection
B
The concept whereby unvaccinated people are protected from infection by those in the community who are vaccinated is called _____.
A. passive immunity
B. herd immunity
C. altruistic immunity
D. active immunity
B
An ELISA was performed on the sera of three patients to detect antibody against hepatitis B virus. Given the titer results shown here, which patient’s serum had the most anti–hepatitis B antibody?
A. Patient 1: dilution, 1:30
B. Patient 2: dilution, 1:1,350
C. Patient 3: dilution, 1:640
D. not enough information given
C
Which of the following is the best method for differentiating a patient’s various T-cell populations and counting the cells in each?
A. Agglutination
B. Immunofluorescence microscopy
C. FACS
D. ELISA
B
Indirect immunofluorescence microscopy was used to diagnose a patient with syphilis. Which of the following descriptions best represents the process?
A. Tissue from the patient was smeared on a glass slide, and fluorescently labeled anti–syphilis IgG antibody was added.
B. Known syphilis organisms were smeared on a glass slide, patient blood serum was added, and then fluorescently labeled anti–human IgG antibody was added.
C. Tissue from the patient was smeared on a glass slide, patient blood serum was added, and then fluorescently labeled anti–syphilis IgG antibody was added.
D. Known syphilis organisms were smeared on a glass slide, fluorescently labeled patient blood serum was added, and then anti–syphilis IgG antibody was added.
D
Which of the following hypersensitivity reactions is antibody-independent?
A. Type I
B. Type II
C. Type III
D. Type IV
C
Omalizumab prevents anaphylaxis by which of the following means?
A. Increasing epinephrine production to stop mast cell degranulation
B. Killing sensitized mast cells
C. Blocking IgE from binding to mast cells
D. Contracting smooth muscle around bronchioles
C
In Case History 17.2, Richard, blood type B, needed a blood transfusion. Assume that the blood bank ran out of type B RBCs. What blood type could be substituted?
A. A
B. B
C. O
D. AB
D
The most common form of severe combined immunodeficiency is due to _____.
A. adenosine deaminase deficiency
B. diminished production of IL-2
C. decreased surface CD40 ligand (CD40L; or CD154)
D. a lack of IL-2 receptor
C
A 1-month-old child with a low WBC count, low-set ears, a cleft palate, and an underdeveloped thymus most likely has which one of the following?
A. IgA deficiency
B. X-linked agammaglobulinemia
C. DiGeorge syndrome
D. Bare lymphocyte syndrome
A
Treatment of patients who have X-linked agammaglobulinemia includes which one of the following?
A. IV administration of immunoglobulin
B. Thymus transplant
C.T-cell transfusion
D. B-cell transfusion
A
Autoantibodies are formed when _____.
A. an autoantibody-producing B cell presents a nonself epitope to a TFH cell.
B. T and B cells that are autoreactive to the same self-antigen escape negative selection
C. a B cell undergoes isotype switching
D. a superantigen activates an autoantibody-producing B cell
D
The pathophysiology of Graves’ disease involves _____.
A. autoantibody that targets acetylcholine receptor
B. cytotoxic T cells that destroy thyroid follicle cells
C. autoantibody that targets myelin protein
D. autoantibody that targets thyroid-stimulating hormone receptor
B
Why can type A RBCs be transplanted (transfused) to type A individuals with mismatched MHC complexes?
A. RBCs are not antigen-presenting cells.
B. MHC type I complexes are absent on RBCs.
C. Type A antibodies in the recipient do not recognize the donor’s red blood cells.
D. The recipient’s T cells recognize the donor’s blood cells as self.
A
The accompanying graph plots guanine plus cytosine content across the genome of a bacterial pathogen whose overall GC content is 50%. Which of the following chromosome segments could represent a pathogenicity island?
A. A and C
B. A and D
C. B and C
D. B and D
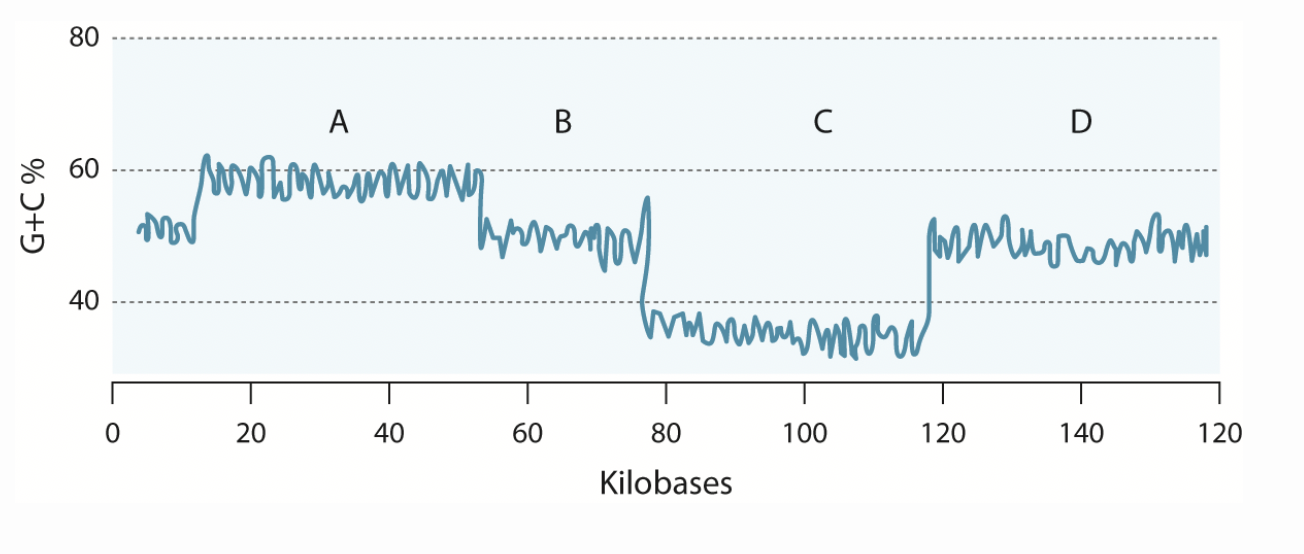
A
Which of the following mechanisms contributes directly to pathogen evolution?
A. conjugation
B. type III secretion
C. exocytosis
D. phagocytosis
C
Which of the following statements is true?
A. All virulence genes are located within pathogenicity islands.
B. Bacterial housekeeping genes are virulence factors.
C. DNA sequences flanking pathogenicity islands are often remnants of HGT mechanisms.
D. All pathogens have pathogenicity islands.
B
Chronic infections are usually associated with _____.
A. antibiotic-resistant bacteria
B. biofilm-producing bacteria
C. capsule-forming bacteria
D. exotoxin-producing bacteria
C
Bordetella pertactin is an example of a(n) _____.
A. pilus
B. capsule
C. nonpilus adhesin
D. endotoxin
D
Pilus contact between a pathogen and a host cell _____.
A. delivers exotoxins into cells via the pilus
B. enables the pathogen to avoid the immune system
C. extracts nutrients from the host cell
D. prevents evacuation of the pathogen
B
Salmonella enterica serovar Typhimurium, while causing an infection, _____.
A. moves intracellularly via actin tails
B. remains in a Salmonella-containing host cell vacuole
C. prefers growth within a host cell phagolysosome
D. makes protein A that binds antibody Fc regions
D
Which one of the following bacteria is an obligate intracellular pathogen?
A. Salmonella
B. Listeria
C. Shigella
D. Rickettsia
A
During infection, Listeria monocytogenes _____.
A. moves intracellularly via actin tails
B. remains in the host cell phagosome
C. prefers growth within a phagolysosome
D. uses a polysaccharide capsule to avoid phagocytosis
B
Which of the following toxins ADP-ribosylates a G-factor?
A. Diphtheria toxin
B. Escherichia coli LT
C. Shiga toxin
D. Anthrax EF toxin
C
Which of the following toxins stimulates cytokine production through a superantigen mechanism?
A. Diphtheria toxin
B. Shiga toxin
C. Toxic shock syndrome toxin
D. Staphylococcal alpha toxin
C
Type III secretion systems are paralogous to _____.
A. conjugation systems
B. transduction systems
C. flagellum synthesis systems
D. type IV pili
B
Which of the following best explains why one person can develop multiple colds over a lifetime?
A. Ineffective B-cell memory for the rhinovirus
B. Multiple rhinovirus strains that possess different VP1 structures
C. A constantly changing ICAM-1 structure in hosts
D. Different strains of rhinovirus that attach to different host cell receptors
C
Cytomegalovirus, which can cause a mononucleosis-type disease, prevents the immune system from destroying infected cells by _____.
A. down-regulating MHC II on infected cells
B. inhibiting production of anti-inflammatory cytokines
C. placing a molecular mimic of MHC I on an infected cell’s surface
D. placing a molecular mimic of MHC II on an infected cell’s surface
B
Which of the following virulence mechanisms does influenza virus use?
A. E7 protein to control host cell division
B. NS1 protein to inhibit production of interferon
C. miRNAs to inhibit apoptosis
D. Nef protein to down-regulate MHC I
C
What percentage of the world’s population is thought to be infected with Toxoplasma gondii?
A. 5%
B. 25%
C. 50%
D. 90%
D
By which of the following actions do Leishmania protozoa avoid the immune system?
A. Up-regulate TNF-α in infected macrophages
B. Vary their surface antigens
C. Inhibit plasma cell formation
D. Down-regulate IL-12 production in infected macrophages
A
Which of the following organisms is a nondimorphic pathogenic fungus?
A. Aspergillus fumigatus
B. Blastomyces dermatitidis
C. Histoplasma capsulatum
D. Cryptococcus neoformans
B
Of the following, which is the best clinical reason to identify the etiologic agent causing an infection?
A. To accurately predict disease severity
B. To alert the clinician about possible disease sequelae
C. To pinpoint the source of the infection
D. To indicate whether gloves should be worn when examining the patient
C
Twenty-five students from two schools were stricken with bacterial diarrhea. All the patients went to a countywide fair 3 days ago that 400 students attended. Which of the following would best confirm that the county picnic was the source of infection?
A. Different bacterial species were isolated from the sick students but all had the same antibiotic resistance pattern.
B. The same bacterial species was found in each of the 400 students and all specimens had the same antibiotic resistance pattern.
C. The same bacterial species with the same antibiotic resistance pattern was found in all the sick students and in a vendor at the picnic.
D. The same bacterial species but with different antibiotic resistance patterns was found in all the sick students and in a vendor at the picnic.
B
A 13-year-old boy has a high fever and is disoriented, but his blood pressure is normal. Blood cultures are obtained and are incubated aerobically and anaerobically. After overnight incubation, growth is observed in all blood culture bottles. Which of the following is the most defensible conclusion?
A. The sample was contaminated because an aerobe and an anaerobe are unlikely to both be present in the patient’s blood.
B. The patient has septicemia caused by an organism that is facultative with respect to oxygen.
C. The patient has septicemia and the organism is aerobic.
D. The patient has septicemia caused by a Gram-negative rod.
A
A urine specimen from a patient who experienced burning pain upon urination contained Gram-negative, lactose-positive, indole-positive rods that were urease negative. Which of the following bacterial species has these characteristics?
A. Escherichia coli
B. Proteus mirabilis
C. Staphylococcus aureus
D. Streptococcus pneumoniae
D
A fecal sample from a patient with diarrhea contained a bacterium that produced white colonies on MacConkey medium, produced colonies with black centers on Hektoen agar, and was catalase-positive but did not grow on CNA blood agar. Which of the following bacterial species has this biochemical profile?
A. Shigella flexneri
B. Escherichia coli
C. Staphylococcus aureus
D. Salmonella enterica
B
_____ prevents the Gram staining of Mycobacterium tuberculosis.
A. peptidoglycan
B. mycolic acid
C. lipopolysaccharide
D. teichoic acid