BSCI202: Reproductive System
1/234
Earn XP
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
235 Terms
A male who produces male gametes, which are called what?
Spermatozoa (sperm)
A female who produces female gametes, which are called what? They also provide what?
ova (eggs); site for fertilization and implantation
What are characteristics of gametes in sexual reproduction?
Haploid, n (contains 23 chromosomes)
What is formed when male gamete and female gamete combine?
Zygote
What are the characteristics of a zygote?
diploid, 2n (46 chromosomes)
The gametes in sexual reproduction are produced by what process?
Meiosis
What is the type of cell division that occurs in primary sex organs also known as gonads?
Meiosis
What is the process of meiosis of the sex chromosomes called?
Gametogenesis
This process is defined as the cellular and nuclear processes that reduce the chromosomal content per nucleus from two sets to one set
Meiosis
This type of reproduction results in genetic diversity which is the basis of Natural Selection
Sexual reproduction
Children of a couple are ____________ due to genotypic variation among offspring
not genetically identical
What type of reproduction results in a “population control” and less intraspecific competition which prevents competition for resources among offspring?
Sexual reproduction
What are the disadvantages of sexual reproduction?
Tedious/time-consuming, couple must be reproductively compatible, and it is not an efficient process
The Male Reproductive System is divided into 2 major parts which are?
Male primary sex organs/gonads (Testes) and male accessory reproductive structures
What is the male primary sexual organs called? Where is it located?
Testes; in the scrotum hanging outside the body, from the perineum
What is the male sex steroid hormones called?
Androgens
What are the three types of androgens?
DHEA, Androstenedione, and Testosterone
How many male accessory reproductive structures are there?
4 ducts and 3 glands
What are the 4 male accessory reproductive ducts called?
Epididymides; Vasa deferentia; Ejaculatory ducts; Urethra
What are the 3 male accessory reproductive glands called?
Seminal vesicles; Prostate gland; Bulbourethral glands
Each testis is surrounded by 2 membranes, what are those membranes called?
Outer Tunica Vaginalis; Inner Tunica Albuginea
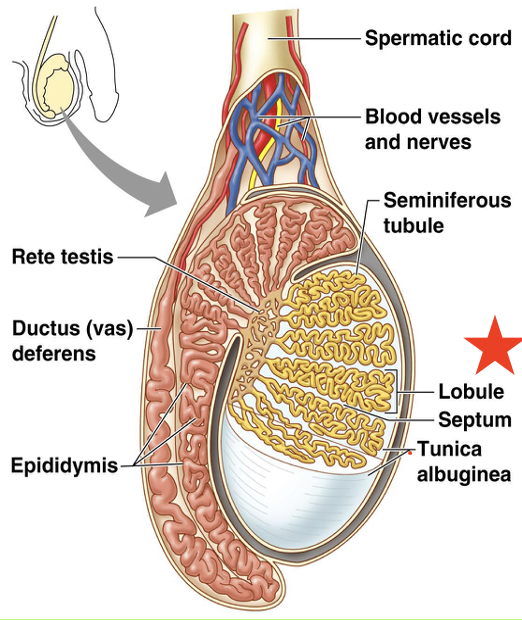
Tunica albuginea partitions the testis into wedge-like LOBULES - each lobule contains highly coiled tubules called what?
Seminiferous tubules
What is the structural units of testis called?
Tubules
“Sperm factories", spermatogenesis occurs here
Seminiferous tubules
What are the three types of cells in the testes?
Spermatogenic cells, Leydig cells (interstitial cells), Sustentacular cells (Sertoli cells)
What cells are located in between the seminiferous tubules and are endocrine cells that are stimulated by luteinizing hormone (LH) to synthesize the Androgens?
Leydig cells
These cells are located at the periphery of the seminiferous tubules – stimulated by FSH to produce androgen binding protein (ABP) + other functions
Sustentacular cells
What is the optimum temperature for spermatogensis?
34 degrees Celcius
What are the functions of the scrotum?
Maintains testes at lower temperature to prepare for spermatogenesis
What are the 2 muscles that maintain the optimum intrascrotal temperature?
Cremaster muscle and Dartos muscle
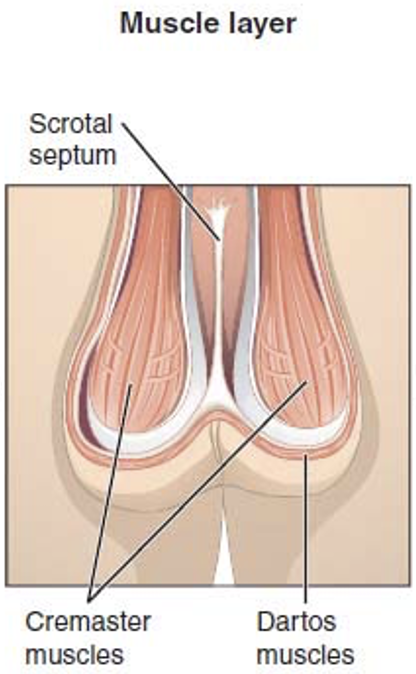
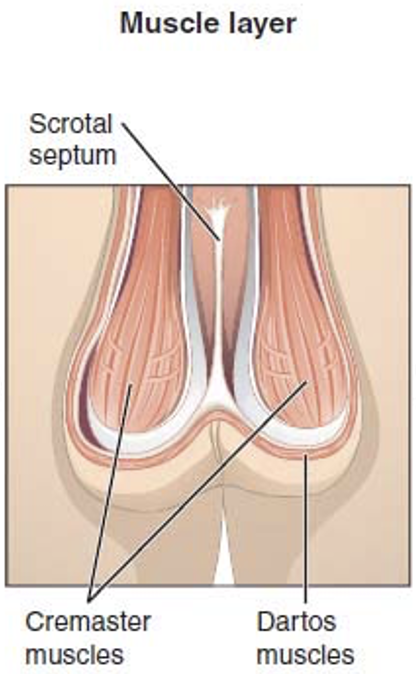
What are the actions of the 2 muscles that maintain the optimum intrascrotal temperature in cold weather?
The CREMASTER muscle contracts pulling the scrotum closer to the body for some warmth; the DARTOS muscle contracts to cause the surface of the scrotum to wrinkle , reducing heat loss
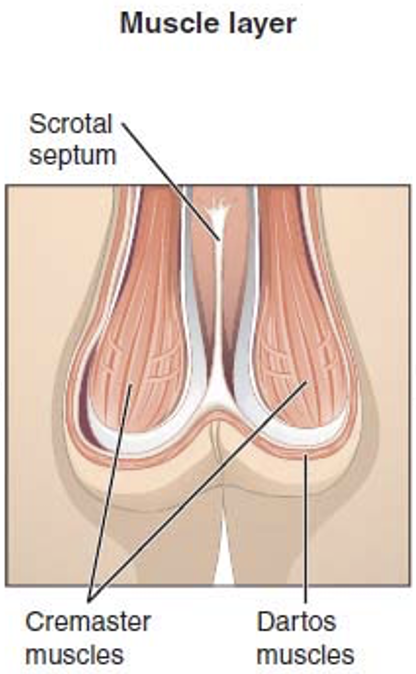
What are the actions of the 2 muscles that maintain the optimum intrascrotal temperature in hot weather?
The CREMASTER muscle relaxes causing the scrotum hangs lower away from the body; the DARTOS muscle relaxes and the skin becomes flaccid and the surface area of the scrotum increases - this increases heat loss.
What are the functions of the testes?
Production of the male sex steroid hormones known as the ANDROGENS; Spermatogenesis
What cells inside the testes (but external to the seminiferous tubules) are the endocrine cells stimulated by LH (luteinizing hormone) to produce the androgens = Androstenedione, DHEA, Testosterone?
Leydig cells
What hormone is required for the initiation and maintenance of spermatogenesis?
Testosterone
Spermatogenesis produces how much sperm a day?
100-400 million sperm/day
When one ages, testosterone levels drop; what happens to the number of sperm produced?
Decreases
What are all the major events of the life of a sperm?
Spermatogenesis, Mitosis, Meiosis, Spermiogenesis, Capacitation
Spermatogenesis consist of 3 main (sequential) phases which are?
1. Mitosis, 2. Meiosis, 3. Spermiogenesis
What phase of Spermatogenesis is this?
Spermatogonium (2n) undergoes ______ to yield 2 identical daughter cells called type “A” cell and type “B” cell.
The type “A” cell replenishes the spermatogonial stock
The type “B” cell moves toward the lumen of seminiferous tubule and it’s referred to as the PRIMARY SPERMATOCYTE (2n= diploid)
1. Mitosis
What phase of Spermatogenesis is this?
1st ______ division (Reduction division) – Primary spermatocyte completes the first ______ division to yield 2 HAPLOID cells of equal size called SECONDARY SPERMATOCYTES (n = 23)
2nd ______ division (Equational division) – 2 secondary spermatocytes complete the second ______ division to yield 4 HAPLOID cells of equal size called SPERMATIDS (n) – round with superfluous cytoplasm and non-motile
2. Meiosis
What phase of Spermatogenesis is this?
First maturation process that converts the round into the spermatids into the stream-lined spermatozoa (sperm) - capable of locomotion = “swimming”
3. Spermiogenesis
What are the 3 regions of a Sperm?
Head, Midpiece, Tail (=Flagellum)
What region is this of the sperm?
Contains the haploid nucleus with an ACROSOME = helmet-like structure and contains hydrolytic enzymes
Head
What region is this of the sperm?
Contains mitochondria – for aerobic respiration to produce ATP to support “swimming”
Midpiece
What region is this of the sperm?
Composed of microtubules and contains disulfide linkages required for whiplashing movements during “swimming”.
Tail (Flagellum)
What are the target cells for Follicle-stimulating hormone (FSH)?
Sustentacular (Sertoli) cells
Why are sustentacular (Sertoli) cells the target cells for FSH?
They form the blood-testis barrier that surrounds the developing spermatogenic cells in the seminiferous tubules
What is the significance of the blood-testis barrier?
Prevents contact between cells of the specific immune system and the developing spermatogenic cells in the seminiferous tubules; these spermatogenic cells are developing after the specific immune cells have been programmed to differentiate between “self” and “non self” antigens. Hence, the cells of the specific immune system will attack and destroy the spermatogenic cells if they come into direct contact
What type of proteins can Sustentacular cells produce?
Androgen Binding Proteins (ABPs)
These bind and concentrate testosterone around the spermatogenic cells in the seminiferous tubules
Androgen Binding Proteins (ABPs)
What type of fluid can Sustentacular cells produce?
Testicular fluid
What acts as a transport medium for sperm transport in spermiation – the release of sperm in _________ into the lumen of seminiferous tubules.
Testicular fluid
Testosterone is converted in the bloodstream to be a more potent form called what?
Dihydrotestosterone (DHT)
What enzyme converted Testosterone into Dihydrotestosterone?
5 alpha reductase
What is the prenatal effect of Testosterone (DHT)?
Stimulates the differentiation of the male internal and external genitalia
5 alpha reductase deficiency in the male fetus (XY) will result in what?
Differentiation of the female external genitalia
The female fetus (XX) with high levels of androgens as in Congenital Adrenal Hyperplasia (CAH), will result in what?
Differentiation of the male external genitalia
What is the postnatal actions of Testosterone (DHT)?
Stimulates the male secondary sex characteristics

Maleness is an active process dependent on the continuous release of what hormone?
Testosterone
Low levels of testosterone is called what? It results in what of the external genitalia?
Hypogonadism; shrinking of external genitalia
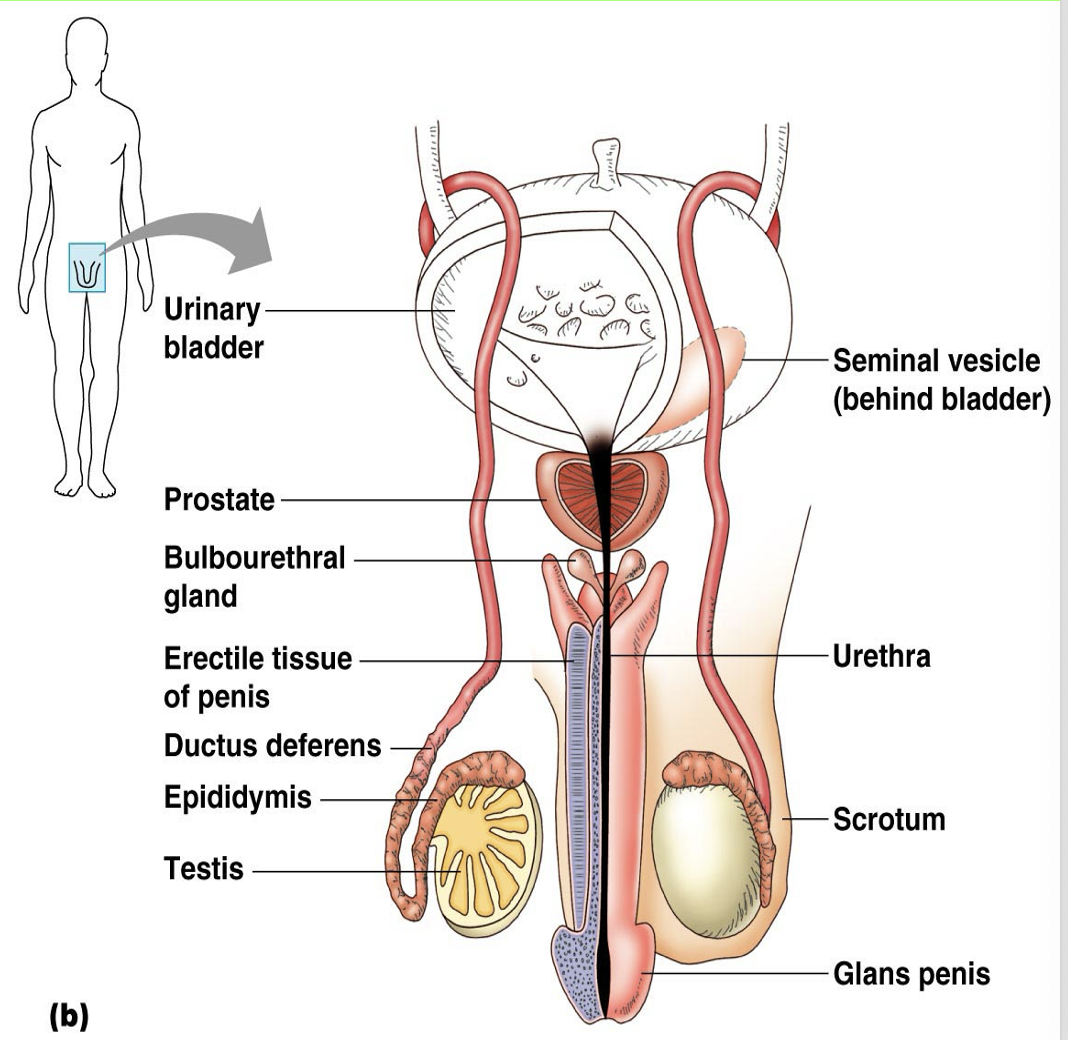
For the four male reproductive accessory ducts, how many of them are in one healthy male?
Epididymides (2), Vasa deferentia (2), Ejaculatory ducts (2), Urethra (1)
What is the order of sperm transport through the male accessory reproductive ducts?
Epididymides → Vasa deferentia → Ejaculatory ducts → Urethra
What male accessory reproductive duct is this?
First ducts to receive sperm; highly coiled connect testes to the vasa deferentia
Sperm spend 20 days to mature with a more rigid tail
Sperm gain the ability to “swim” however, sperm swim only in the female reproductive tract
Epididymides
What male accessory reproductive duct is this?
Sperm storage sites
Enclosed in spermatic cord (with testicular arteries, pampiniform plexus, and nerves)
Vasectomy = surgical cut and ligation of both vasa deferentia (next time) “Permanent male birth control”
Vasa deferentia
What male accessory reproductive duct is this?
During ejaculation, receive sperm from vasa deferentia and secretions from the seminal vesicles and the prostate gland forming SEMEN
Ejaculatory ducts
What male accessory reproductive duct is this?
Has a dual function of transporting urine and semen – semen always has the right of way during ejaculation
Urethra
What does the male urethra consist of?
Prostatic urethra, Membranous urethra, and Penile urethra
What region of the male urethra is this?
Passes through the prostate
Prostatic urethra
What region of the male urethra is this?
Passes through the urogenital diaphragm
Membranous urethra
What region of the male urethra is this?
Passes through the penis – 15cm (6in) long
Penile (spongy) urethra
Why are females more prone to developing urinary tract infection (UTI) than males?
Easier access because of the shorter urethra (4cm vs. 20cm)
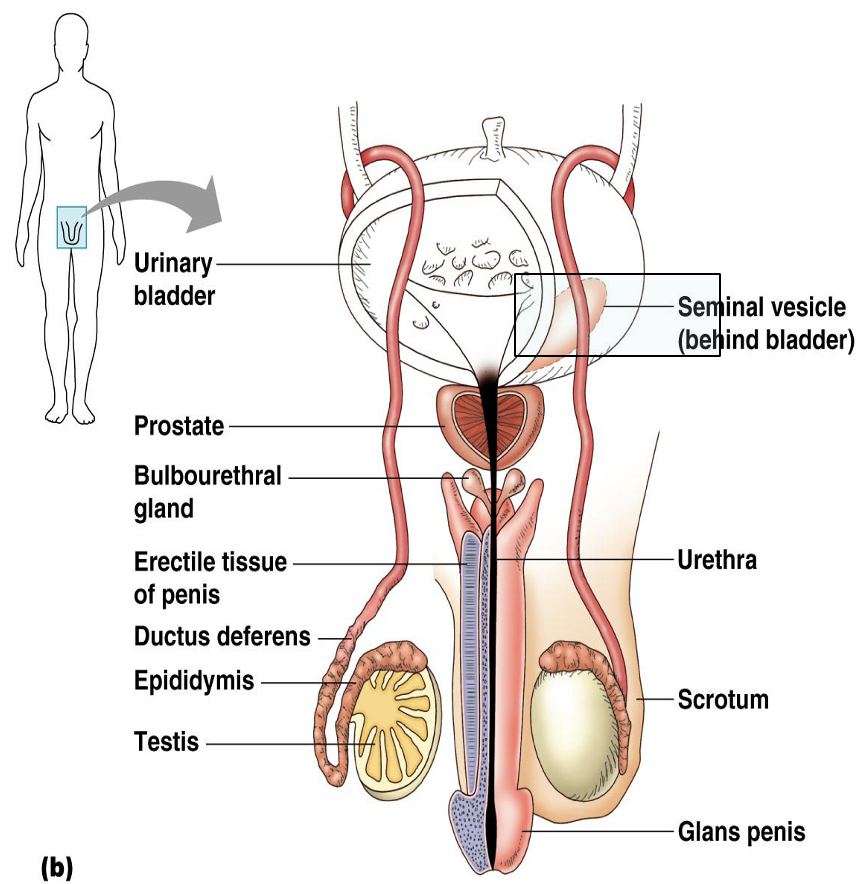
For the four male reproductive accessory glands, how many of them are in one healthy male?
Seminal Vesicles (2), Prostate gland (1), Bulbourethral glands (2)
What male accessory reproductive gland is this?
What male accessory reproductive gland is this?
Secrete 60% of seminal fluid; secretion contains Fructose, Coagulating enzymes, Ascorbic acid (vit. C), and Prostaglandins
Seminal vesicles
What in the secretion of Seminal vesicles is this?
Used by sperm to produce energy for locomotion
Fructose
What in the secretion of Seminal vesicles is this?
For the temporary coagulation of ejaculated semen to protect sperm and to begin the process of capacitation
Coagulating enzymes (ie. vesiculase) acts as a reducing agent to protect sperm against oxidation; acts as an antioxidant
What in the secretion of Seminal vesicles is this?
Acts as a reducing agent to protect sperm against oxidation; acts as an antioxidant
Ascorbic acid (vitamin C)
What in the secretion of Seminal vesicles is this?
Facilitates sperm movement in the female reproductive tract
Prostaglandins
What male accessory reproductive gland is this?
Secrete 33% of seminal fluid; secretion contains Citrate, Fibrinolysin, Acid phosphatase
Prostate gland
What in the secretion of Prostate gland is this?
Acts as calcium chelator to end semen coagulation
Citrate
What in the secretion of Prostate gland is this?
Liquefaction agent that liquefies the coagulated semen
Fibrinolysin
What in the secretion of Prostate gland is this?
Unique enzyme that activates phospholipid metabolism
Acid phosphatase
Increase in acid phosphatase levels are indicative of the growth of what gland? What is this condition called?
Prostate gland; Benign Prostatic Hyperplasia (BPH)
Increase in the levels of the tumor marker, prostate specific antigen (PSA), is indicative of what condition?
Prostate cancer (malignant)
What male accessory reproductive gland is this?
Secrete a thick alkaline fluid (the pre-ejaculate) which neutralizes any acidic urine residue in the urethra prior to ejaculation; sperm are immobilized/destroyed in an acidic environment.
Bulbourethral (Cowper’s) glands
What are the 3 erectile tissues of the Penis?
2 dorsal erectile tissues (corpora cavernosa) and 1 ventral erectile tissue (corpus spongiosum)
What are the two regions of the penis?
Root and Shaft
What is this region of the penis?
Attaches penis to the perineum
Root
What is this region of the penis?
The body that ends in an expanded tip called the glans penis; cuff of skin surrounding the glans is called the prepuce or the foreskin
Shaft
What is the surgical removal of the prepuce/foreskin called?
Circumcision
What health condition is this?
Penis becomes engorged as blood fills the vascular spaces in the erectile tissues and the penis is erected
Penile erection
What health condition is this?
The inability to initiate/maintain a penile erection
Erectile dysfunction
Does uncircumcised penis harbor more pathogens and hence, exhibit more incidence of infections compared to circumcised penis?
No, so far as the prepuce (foreskin) in the uncircumcised penis is retracted and properly cleaned, there is no increased incidence of infection; if not properly cleaned, then there is an increased incidence of infections.
What are the female primary sex organs (gonads)? Where is it located?
Ovaries; located in pelvic cavity
What are the functions of the ovaries?
Oogenesis and Production of female sex steroid hormones (estrogen, progesterone)
What are the female accessory reproductive structures?
3 ducts and vulva
What is the female external genitalia called?
Vulva
In the Female Accessory Reproductive structures, what are the three ducts called?
Fallopian tubes, uterus, and vagina
During the undifferentiated stage at 6 weeks gestation, what happens if there is no testosterone towards 10 weeks gestation? What sex is determined at 14 weeks gestation?
No Y chromosome; development of reproductive structures does not require hormones; Female