Fluid balance
1/44
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
45 Terms
What is a sensible water loss
Urine, faeces, blood loss
What is an insensible fluid loss
Skin
Lungs
How can water exit the body and roughly how much is lost from each source?
Skin—450 mL daily in temperate climates
Kidneys—1 to 2 L of urine daily.
Respiratory mucous membranes—breath (250–350 mL daily).
Digestive system, including faeces (200 mL daily).
What causes increased water loss from the skin
Higher temperature
What causes increased water loss from the kidneys
Water loss via urine increases during hyperglycemia (diabetes mellitus) as well as in disorders involving antidiuretic hormone (vasopressin).
What causes increased water loss from respiratory mucous membranes?
Respiratory infections trigger increased mucous secretions, resulting in increased water loss
What causes increased water loss from the digestive system?
Vomiting and diarrhoea
What are the uses of water in the body
Regulating Body Temperature
Moistening Tissues
Protecting Organs and Tissues
Delivering Nutrients and Oxygen
Lubricating Joints
Supporting Digestion
Flushing Out Waste
Define fluid balance
Fluid balance is the regulation of the body’s fluid compartments to maintain a stable internal environment.
What are the complications of inadequate fluid intake?
Dehydration can leave you feeling tired, nauseous, and often results in frequent headaches, constipation, and, in some cases, urinary tract infections.
What are the main fluid compartments
Intracellular
Extracellular
Plasma (inside blood vessels)
Interstitial (between cells)
Transcellular (pericardial, CSF, synovial fluid—i.e., within an epithelial-lined space)
Describe the percentage of body composition that is water and how is this then divided between intracellular and extracellular fluid
Total body water is about 60% of their body weight
Roughly 2/3 of that is intracellular fluid, and the other 1/3 is extracellular fluid.
What ions does intracellular fluid dissolve?
The major intracellular cations are potassium (K+) and magnesium (Mg2+), whereas the major anions are proteins and organic phosphates like ATP.
What ions does extracellular fluids dissolve?
The major cation in extracellular fluid, both in the interstitial fluid and in the plasma, is sodium (Na+), and the major anions are chloride (Cl-) and bicarbonate (HCO3-).
How does plasma and interstitial fluid differ in composition
So compared to the plasma, interstitial fluid tends to have higher concentrations of small anions like Cl- and lower concentrations of small cations like Na+.
Describe plasma
Plasma is the only major fluid compartment that exists as a real fluid collection all in one location.
How does plasma differ from interstitial fluid
It differs from ISF in its much higher protein content and its high bulk flow (transport function)
What is the function of plasma
Transports nutrients, hormones and proteins
Removes waste
What is the function of the interstitial fluid
Provide the cells of the body with nutrients and a means of waste removal.
The interstitial ECM contains a great deal of connective tissue and proteins (such as collagen) that are involved in blood clotting and wound healing.
What is Transcellular fluid
Transcellular fluid is the portion of total body water contained within the epithelial-lined spaces
What is the function of transcellular fluid
lubrication of epithealial lined cavities, and sometimes electrolyte transport.
Describe the composition of ICF
ICF is the fluid within cells. It contains high levels of potassium (K⁺) and negatively charged proteins.
What is the function of ICF (Intracellular fluid)
Supports cell metabolism, nutrient transport, and waste removal.
What separates intracellular and intrastitial fluid
Plasma membranes separate IF from ICF
What factors affect fluid balance
Osmosis:
Hydrostatic Pressure: .
Solute Concentration:
Protein Channels:
Describe osmosis
Water moves across semi-permeable membranes based on solute concentration gradients.
Describe hydrostatic pressure
Differences in pressure drive fluid movement.
Describe solute concentration as a part of fluid balance
Maintaining proper solute balance ensures normal cell function.
Describe Protein Channels role in fluid balance
These regulate solute movement
What is oral rehydration therapy
Oral rehydration therapy (ORT) is a simple, cost-effective treatment for dehydration, especially due to diarrhoea.
What are the key mechanisms involved in oral rehydration therapy?
Sodium-Glucose Co-Transport
Water Absorption
Describe Sodium-Glucose Co-Transport
In the small intestine, sodium (Na⁺) and glucose are absorbed together through a co-transport mechanism.
This process is facilitated by a specific protein called the sodium-glucose linked transporter 1 (SGLT1).
When glucose is absorbed, it pulls sodium along with it into the intestinal cells.
Describe water absorption as a part of ORT
The absorption of sodium and glucose creates an osmotic gradient.
Water follows this gradient and moves from the intestinal lumen into the cells and then into the bloodstream.
This helps to rehydrate the body by replenishing lost fluids.
Describe the practical applications of oral rehydration therapy
ORT solutions typically contain a precise balance of salts (sodium chloride), glucose, and water.
The presence of glucose in the solution enhances the absorption of sodium and, consequently, water.
This method is effective even in severe cases of dehydration and can be administered easily without the need for intravenous fluids.
What are the benefits of ORT
Accessibility: ORT can be administered at home, making it accessible in low-resource settings.
Effectiveness: It quickly restores hydration and electrolyte balance.
Safety: It has a low risk of complications compared to intravenous rehydration.
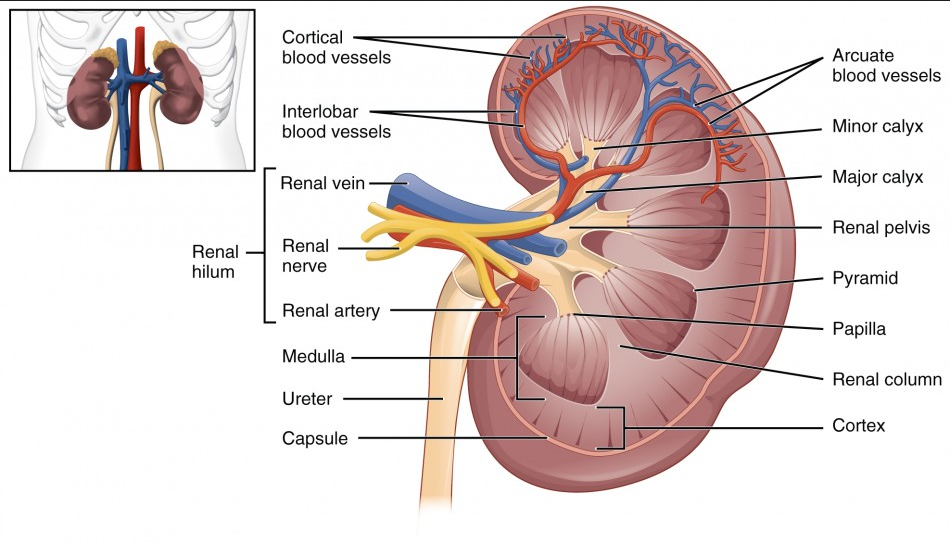
Draw the kidney structure
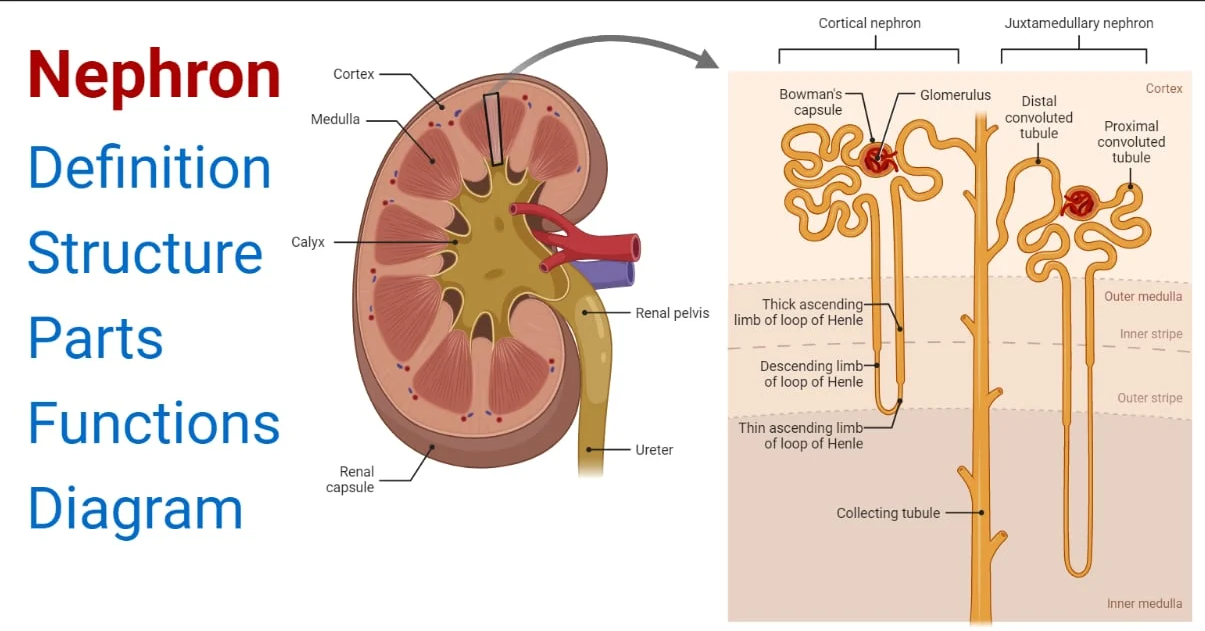
Draw the structure of the nephron
Describe the roles of the kidney
Filtration
Reabsorption
Excretion
Regulation of electrolytes
Acid-Base balance
Hormone production
Describe filtration in the kidney
The kidneys filter blood to remove waste products and excess substances, including water.
Each kidney contains about a million nephrons, which are the functional units responsible for this filtration process.
Describe reabsorption in the kidney
After filtration, the kidneys reabsorb necessary substances like water, glucose, and electrolytes (sodium, potassium, calcium) back into the bloodstream.
This process ensures that essential nutrients and fluids are retained while waste products are excreted.
Describe Excretion in the kidney
The kidneys excrete waste products and excess substances in the form of urine.
This helps to regulate the volume and composition of body fluids.
Describe regulation of electrolytes in the kidney
The kidneys maintain the balance of electrolytes in the body by adjusting the reabsorption and excretion of ions like sodium, potassium, and calcium.
This balance is vital for proper nerve and muscle function.
Describe acid-base balance in the kidney
The kidneys help maintain the body’s pH balance by excreting hydrogen ions and reabsorbing bicarbonate from urine.
This process is essential for preventing acidosis or alkalosis, which can disrupt normal bodily functions.
Describe hormone production in the kidney
The kidneys produce hormones like renin, which regulates blood pressure, and erythropoietin, which stimulates red blood cell production.
They also convert vitamin D into its active form, which is important for calcium absorption and bone health.