IMPLANTS FINAL
1/203
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
204 Terms
subperiosteal
implant that sits below the periosteum
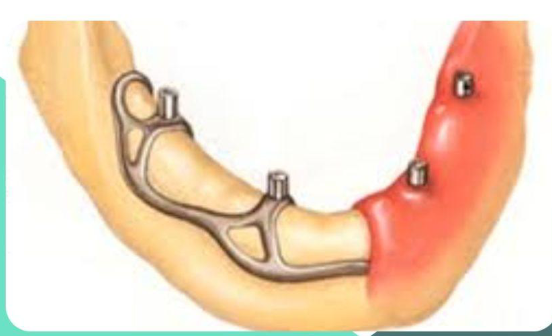
transosseous
implant that goes through the bone, ONLY for MANDIBULAR edentulous arches
endosseous
implants that sitts within living bone
subperiosteal
which type of implant rests on the alveolar bone WITHOUT any mechanical anchoring components
false
T/F transosseous implants are used for patients with edentulous maxillary arch
true
T/F moderately rough surface characteristic of endosseous implants has shown improved healing ability and stability
internal threads
used to secure a restoration/component (abutment) to the implant body
8-12 weeks
how long is the healing phase after implant placement
abutment supported/cement retained
implant that has TWO parts, separate CUSTOM ABUTMENT
to support a CEMENT RETAINED CROWN
screw retained
abutment part incorporated into the crown making it a ONE-
PIECE restoration, crown with screw access hole
abutment
device which serves to support and attach thee prosthesis to the implant
screw
how is the abutment secured to the implant
osseointegration
anchorage mechanism for endosseous implants, allows for the support of prosthetic with bone tissue
careful planning, surgical technique, prosthetic management
requirements of succssful OSSEOINTEGRATION
inflammatory process
what drives SUCCESSFUL OSSEOINTEGRATION
protein adsorption
key for TISSUE INEGRATION with biomaterial
osseointegration
immune‐modulated,multifactorial, and complex healing process where a number of cells and mediators are involved
lack of PDL and circular gingival fibers (instead of perpendicular)
how are implants diffferent than teeth?
overload, receptors
dental implants are at an increased risk of _____ due to few ______ in the surrounding bone
irrigation and 600-800 rpm
when drilling an osteotomy how is frictional heat reduced?
25-35 rpm
speed for implant placement
false
T/F implant should be placed with irrigation
true
T/F FLAPLESS surgery requires a precision surgical guide
friction heat
tisue damaged by _____ provides an ideal habitat for microorganisms
true
T/F there should be irrigation during osteotomy
necrotic zone
Mix of healthy cells-osteoblasts, osteocytes, osteoclasts, and mesenchymal
stem cells between the bone and implant after implant placement
osteoblasts
grow new bone
mesenchymal stem cells
undifferentiated cells that may be stimulated to transform into osteoblasts
osteoclasts
dissolve bone
osteocytes
cells within living bone that participate in remodeling process
vascular invasion
__________ of the necrotic cortex will depend on the ability of
osteoclasts to resorb the necrotic bone and osteoblasts to produce new bone
blood supply
Poor ______ stimulates proliferation of fibrous tissue
10
The bone remodeling of the region at the implant surface will start ~ ___ days after
implant placement
true
T/F with OSSEOSHAPER drill the osteotomy should be widened and fianalized at slow speed (<50 rpm) with NO IRRIGATION
0.2mm
marginal bone loss should NOT exceed ____ after the first year
titanium
low corosion duue to ttenacoius surface oxide layer
stable oxide layer
KEY factor for creating a strong bone-implant interface on which mineralized
bone can be deposited
100 Å
how close is the intimate contact betweeen extra cellular matrix produced by osteroblasts and the titanium surface
primary implant stability
how well the implant is mechanically anchored to the bone
threaded shape
provide superior initial implant stability with imporved and fasted osseointegration
threaded
which implants has seeen less bone loss over time
true
T/F there is NO DIFFERENCE between straight and taperped implants in initial implant stability in well mineralized bone
tapered
developed for sites with “soft” bone quality to provide better initial implant stability by “condensing” the surrounding bone
50-100
after placement implant micromovement should NOT exceed ____µm
secondary integration
replacing the initial bone matrix with mature, mineralized bone around the implant
moderately rough implant surface
Improves initial bone-implant stability and stimulates osteoblast activity and promotes
formation of new bone
30-70%
percentage of surface of successful implant that will have “intimate” bone contact
dull
a ____ sound upon tapping usually indicates lack of osteointegration
chemotherapy
can adversely affect wound healing by preventing cell division and protein synthesis
1-2
A dental implant requires about ___mm of bone around the entire implant body
1.5 mm
Minimum space between TEETH and IMPLANT
3 mm
Minimum space between IMPLANT and IMPLANT
1
Buccal/lingual bone layer must beat least ___mm thick
bone graft
Should always be recommended after extraction if the site is planned for an implant
true
T/F Never touch the graft materials or membrane with gloves or non-sterile instrument
Osteoconduction
ability of bone-forming cells in the grafting area to move across a scaffold and slowly replace it with new bone over time
Osteoinduction
process by which osteogenesis (i.e., new bone formation from osteo-competent cells) is induced
autografts, allograft, and bone morphogenic proteins (BMPs)
Osteoinductive graft materials
hydroxyapatite, xenograft, tricalcium phosphate, calcium sulphates, glass ceramics
osteoconductive graft materials
8-12mm
Recommended minimum inter occlusal height for fixed CEMENT retained prostheses/crowns
6-8mm
Recommended minimum inter occlusal height for fixed SCREW reetaineed prostheses/crowns
SLA or SLAactive (sanblasted large grit acid etched)
implant surface of STRAUMANN is:
sodium chloride (saline)
SLActive are stored in isotonic ____ solution to prevent contamination and promote surface eneregy
one connection for all implant sizes
benefit of STRAUMANN BLX implant
guide pin
used to secure IMPRESSION COPING to the IMPLANT
SC
Straumann implant for Upper lateral incisors/lower incisors
NC
Straumann implant for Upper & lower anterior teeth, bicuspids (lack of alveolar
bone/space)
RC (4.1 mm)
Straumann implant for Single upper anterior teeth, bicuspid-, and molar area, multi-unit FPDs, complete arch fixed prostheses, overdentures, RPD (distal extension support)
RC (4.8 mm)
Straumann implant for Single molars, posterior multi-unit FPDs
35 Ncm
all STRAUMANN abutement screws are tightened to _____
TI-unite
surface of NOBEL biocare systems are
anodic oxidation
the TI-UNITE surface of NOBEL biocare systems are characterized by
NP (narrow platform)
NOBEL biocare implant for Lower incisors, upper lateral incisors, and single rooted anterior teeth if there is a lack of alveolar bone/space
RP (regular platform)
NOBEL biocare implant for Single anterior teeth, bicuspids, multi-unit FPDs, complete arch fixed prostheses, overdentures/ RPD (distal extension support)
WP (wide platform)
NOBEL biocare implant for Single molars
abutment screw
Should only be used in patient’s mouth- not be sent to lab
35 Ncm
ALL abutments/restorations on Nobel Parallel implants require ____ insertion torque
torque wrench
Use the ______ only to do the final tightening of the abutment screw
engaging
single units require _____ abutment design
non-engaging
when splinting 2+ units in a multi-unit restoration a _____ abutement design is required
non-engaging
for SCREW retained MULTI-UNIT restorations ALWAYS use a ____ abutment
engaging
for CEMENT-retained MULTI-UNIT restorations ALWAYS use ____ abutments (separate)
true
T/F prescribe prophylactic Antibiotics dose to take 1 h before surgery if patient has artificial heart valves, joint prostheses, other health concerns
direction indicator
Provides valuable information about depth, position, and angulation of the osteotomy
0.5 mm
The final osteotomy is normally about ____ narrower than the diameter of the implant to allow for good initial stability
true
T/F the implant surface should NEVER be touched with gloves or instrruments
true
T/F no post op antibiotics are necessary for healthy patients
only RB/HB
For IMPLANTS what is the impression material needed
5 min
impression coping must be placed immediately as tisssue will begin to colapse after ____
true
T/F NEVER use hand wrench to tighten guide pin onto impression coping
true
T/F a full arch tray should always be used from implants (single or multiple)
open tray
Guide Pin is unscrewed BEFORE removing the tray
open tray
the IMPRESSION COPINg will ALWAYS be removed WITH the impression
open tray
impression technique recommended for ANTERIOR implants and MULTI-UNIT restorations
35-40 mm
vertical clearance needed for open tray technique
closed tray
coping/plastic cap is removed with impression and metal coping stays connected to the implant. coping is theen unscrewed and repositioned into impression after tray is removed
plastic cap
what helps reposition the metal coping into the impression in the CLOSED teechnique
closed tray
impression technique that can be useed anywhere in the mouth and for single or multi-unit restorations
analog/implant replica
embedded in the master cast and used for the fabrication of the restoration has internal geometry identical to that of the implant
before
The analog is connected to the impression coping _____ the impression is poured