Female reproductive system - slides
1/23
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
24 Terms
Gonads
Ovaries
oogenesis
hormones
Organs
Uterine(fallopian) tubes/oviducts
Uterus
Vagina
External organs- vulva/pudenum
Mammary glands
Ovaries
produce games and hormones
held by ovarian, broad and suspensory ligament
consist of : germinal epithelium, tunica albuginea, ovarian cortex, ovarian medulla
Primordial follicle
baby follicles that develop into primary follicles during ovarian development. They consist of an oocyte surrounded by a single layer of follicular cells.
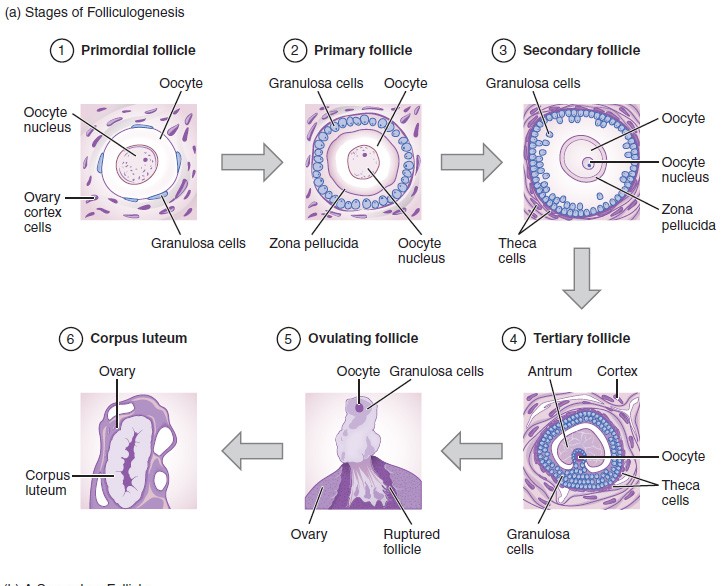
Follicles
ovarian follicles contain oocytes in various stages of development, and their supporting cells (follicular cells/granulosal cells)
6 types'
Primordial follicle
Primary follicle
Secondary follicle
Tertiary (Mature/Vesicular/Graafian) follicle
Corpus luteum
Corpus albicans
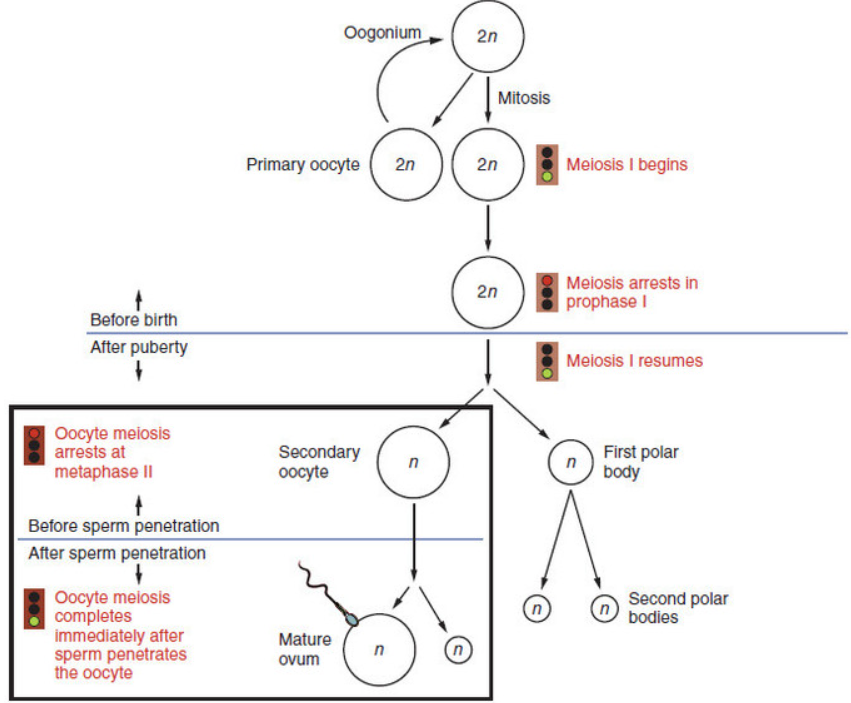
Oogenesis
Formation of gametes in the ovaries
begins before birth
primordial germ cells migrate from the yolk sac
Uterine tubes (fallopian tubes)
Histology
mucosa- simple ciliated columnar epithelium
muscularis
serosa
Anatomical parts
infundibulum
ampulla
isthmus
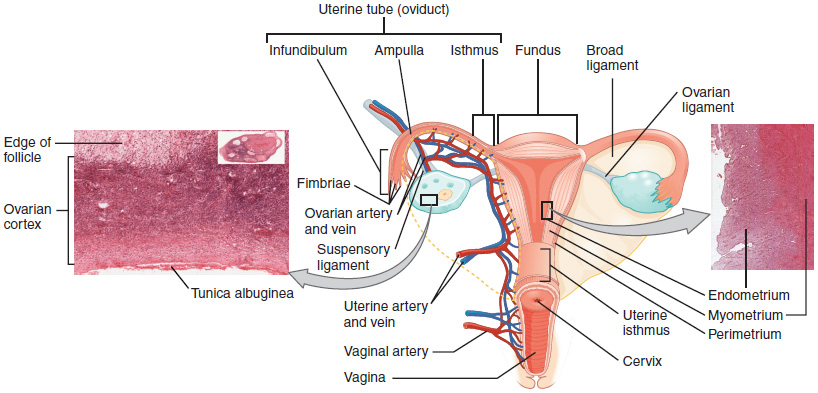
Uterus major areas
body
fundus
isthmus
cervix
cervical canal
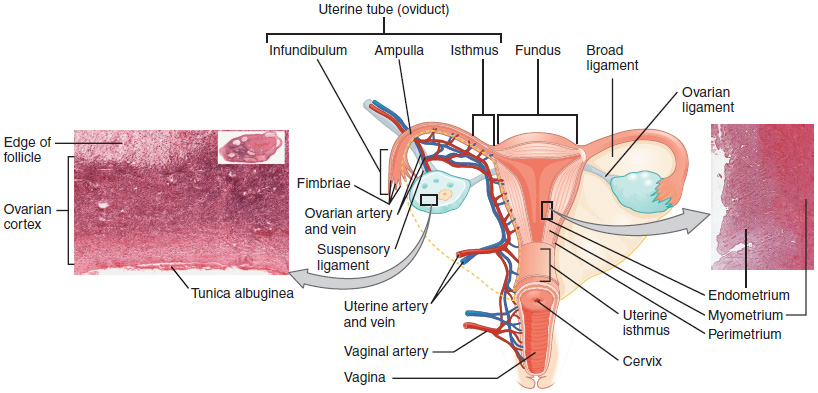
Uterus interior parts
uterine cavity
cervical canal
internal os
external os
Uterus Histology
3 layers
perimetrium(serosa): visceral peritoneum
myometrium: 3 layers of smooth muscle
endometrium: mucosal lining of uterine cavity - stratum functionalis and stratum basalis
Endometriosis
Growth of endometrial tissue outside of uterus
causes pain, scarring and infertility
exact cause: unknown
Vagina function
Passageway for birth, menstrual flow and intercourse
Vagina layers
3 layers (outer to inner)
mucosa
muscularis (smooth muscle layer)
Adventitia
External genitalia (vulva)
Mons pubis
rounded mass of fatty tissue, overlying pubic symphysis
Labia majora (like scrotum)
Labia minora (like spongy penile urethra)
Clitoris (like glans penis)
Vestibule
external urethral orifice, openings of several ducted glands and vaginal orifice
Bulb of vesibule
elongated masses of erectile tissue on either side of vaginal orifice
homologous to erectile tissue of penis
Paraurethral(skene’s) glands
like erectile tissue of penis
secrete mucus
homologous to prostate gland
Mammary glands
Modified sweat glands that produce milk (lactation)
lobes (15-20) → lobules → alveoli
lactiferous ducts
areola
suspensory ligaments
Ovarian cycle hormones FSH
hypothalamus releases gonadotropin-releasing hormone (GnRH) that stimulates the anterior pituitary to secrete follicle-stimulating hormone (FSH), promoting ovarian follicle development.
stimulates growing follicles (initial development of ovarian follicles)
stimulates further development of ovarian follicles and their secretion of estrogen and inhibin
-Inhibin: inhibits release of FSH and to a lesser extent LH
-Estrogen: promotes development of secondary sexual characteristics, moderate levels inhibit release of GnRH, FSH, and LH
Ovarian cycle hormones LH
hypothalamus releases gonadotropin-releasing hormone (GnRH) that stimulates the anterior pituitary to secrete luteinizing hormone (LH), which triggers ovulation and promotes the formation of the corpus luteum.
stimulates OVULATION(further development of ovarian follicles and their secretion of estrogen and inhibin)
stimulates CORPUS LUTEUM (stays until the cycle ends, if fertilized it can stay up to 3 months for fetus growth and nourishment)- secretion of progesterone, estrogens, relaxin, and inhibin
Ovarian cycle
follicular phase
ovulation
luteal phase
The ovarian cycle encompasses the series of hormone-controlled events during which ovarian follicles mature and ovulation occurs, followed by the luteal phase where the corpus luteum develops.
Uterine cycle
menstruation
proliferate phase
secretory phase
The uterine cycle consists of three main phases: the menstruation phase, where the uterine lining is shed; the proliferative phase, during which the lining thickens and regenerates; and the secretory phase, where the lining prepares for potential implantation of an embryo.
Follicular phase
pituitary hormone effect: LH and FSH stimulate several follicles to grow
Ovarian hormone effect: dominant follicle produces estradiol → Inhibits GnRH, FSH, and LH production causes endometrium thickening
Ovulation
Pituitary hormone effect: LH and FSH stimulate maturation of one of the growing follicles
Ovarian hormone effects: Growing follicle continues to produce estradiol→ stimulates GnRH, FSH, LH production and LH surge triggers ovulation
The process in which a mature ovarian follicle releases an egg, typically around the midpoint of the menstrual cycle, influenced by a surge of luteinizing hormone (LH).
Luteal phase
Pituitary hormone effect: LH stimulates formation of a corpus luteum from follicular tissue left behind after ovulation
Ovarian hormone effects: the corpus luteum secretes progesterone which
inhibits GnRH, FSH, and LH production
Maintains the endometrium: as the corpus luteum degrades, progesterone declines, initiating sloughing of the stratum functionalis
Perimenopause
time near menopause
may have irregular or skipped periods
Menopause
stopped having monthly menstrual cycles for one year
typically between 45-55 years
some atrophy of reproductive organ and breasts (no remaining follicles to stimulate estrogen secretion
Decrease in vaginal wall thickness and uterus shrinking
hot flashes with periodic elevation in body temperature (skin blood vessels undergo intense vasodilation)
possibly thinning scalp hair and increased facial hair- coarse (due to relatively high testosterone levels)
Increased risk of osteoporosis and heart disease
sx are sometimes treated with hormone replacement therapy