Non-Salivary Secretions of the GI Tract
1/40
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
41 Terms
What are the FUNCTIONS of the SMALL INTESTINE?
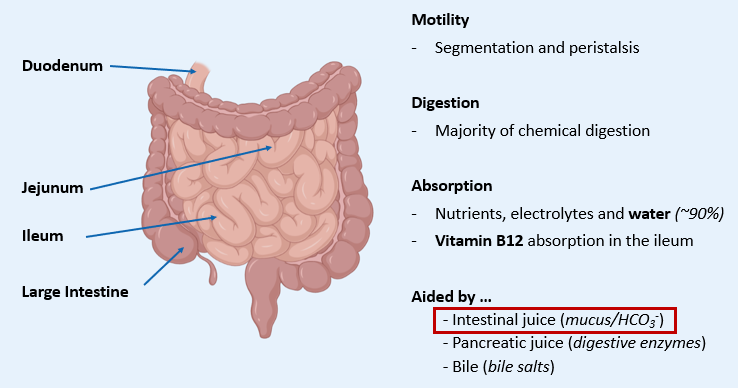
Specialisation of the INTESTINE WALL
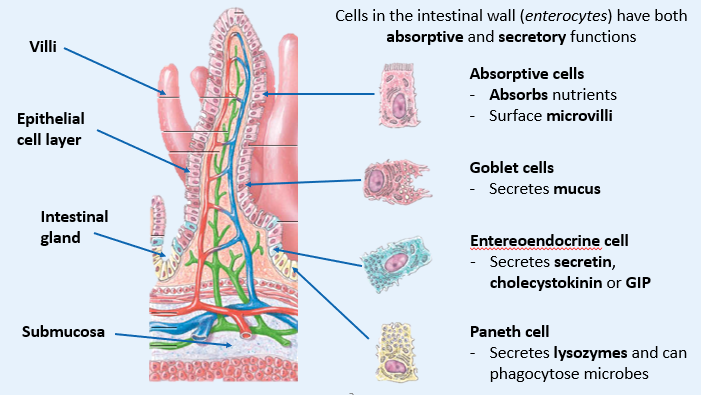
What is the BRUNNER’S GLAND?
1) Compound tubular submucosal glands found in the duodenum
2) Main function is to secrete mucus and HCO3-
3) Progressive neutralisation of low pH (acidic) chyme from stomach
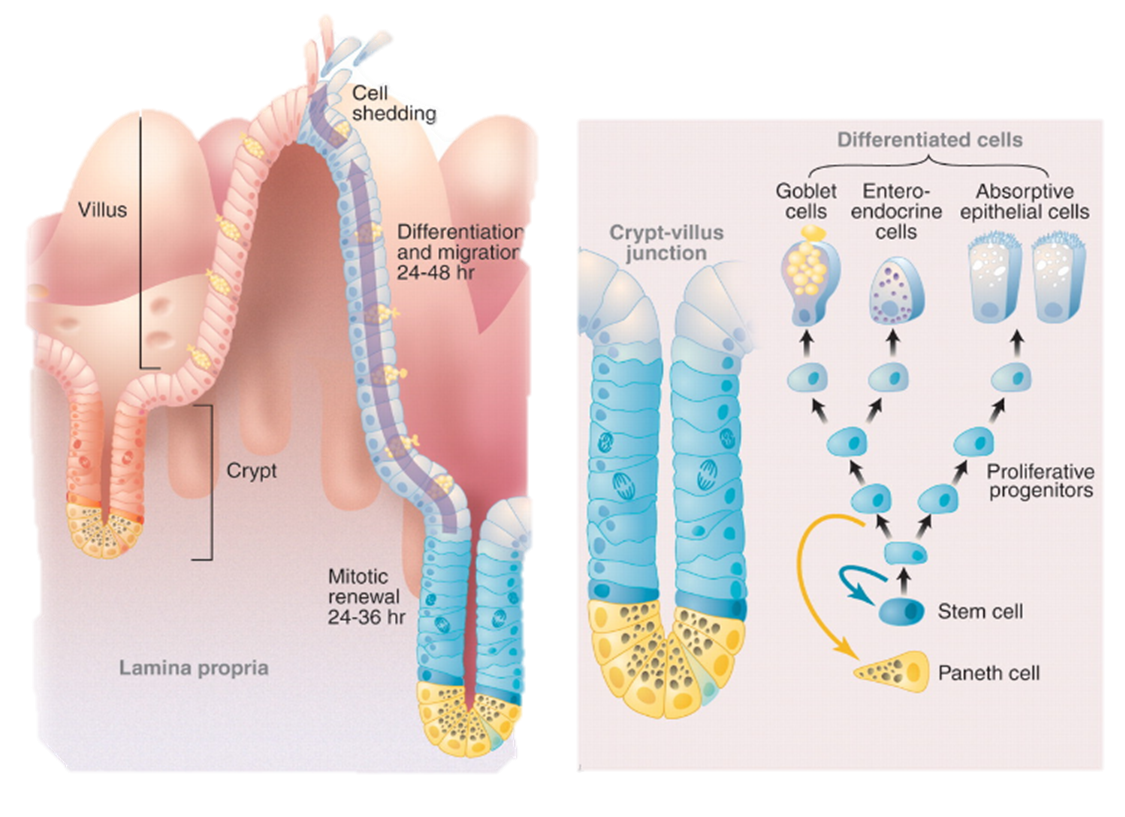
How does STEM CELL RENEWAL replace Epithelial Cells?
1) Intestinal stem cells proliferate (mitosis) in the crypt region
2) Intestinal stem cells then differentiate into the other enterocyte cells
3) Harsh environment requires a rapid turnover of epithelial cells every 5-7 days
4) Vulnerable to radiation, chemotherapy
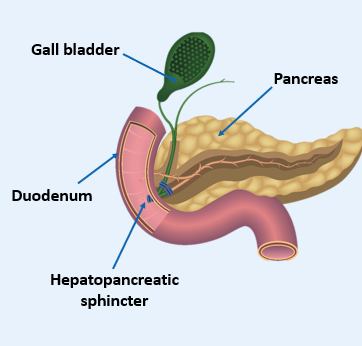
What is the HEPATOPANCREATIC SPINCHTER?
Secretions from the duodenal wall mix with pancreatic and biliary secretions regulated by the hepatopancreatic sphincter (sphincter of Oddi)
Hepatopancreatic Spinchter - ENDOCRINE SECRETIONS
Endocrine Secretions
1) CCK (I cells) – stimulates pancreatic and gallbladder secretion
2) Secretin (S cells ) – stimulates pancreatic and biliary bicarbonate secretion
3) GIP (K cells) – may inhibit acid secretion / stimulate insulin release
Hepatopancreatic Spinchter - EXOCRINE PANCREATIC JUICE
Exocrine pancreatic juice (1.5 L): bicarbonate / digestive enzymes
Hepatopancreatic Spinchter - BILE
Bile (0.5-1 L) : bile salts for lipid emulsification (liver hepatocyte synthesis, gall bladder storage)
What are INTESTINAL BACTERIA?
1) Bacteria secrete vitamins B and K for subsequent absorption
2) Bacteria act on chyme and produce hydrogen, CO2 and methane gas
3) Bacteria produce stercobilin as a breakdown product of bilirubin to give faeces brown colour.
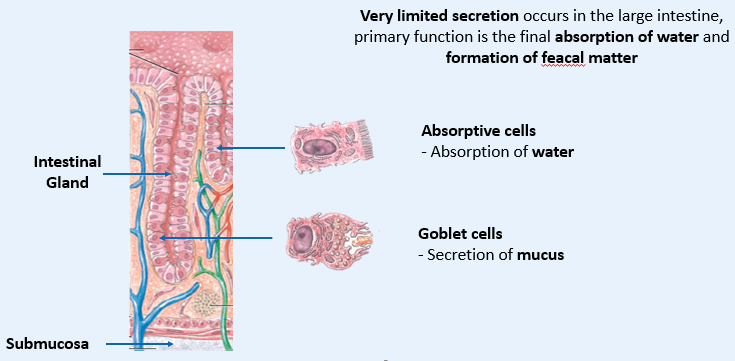
Why does the LARGE INTESTINE have LIMITED SECRETIONS?
Question 1

What are the EXOCRINE secretions of the Pancreas?
1) Exocrine acinar clusters (95%) secreting pancreatic juice
water, electrolytes, sodium bicarbonate and pro-enzymes
What are the ENDOCRINE secretions of the Pancres?
1) Endocrine pancreatic islets (5%) (Islets of Langerhans) secreting
glucagon (alpha)
insulin (beta)
somatostatin (delta)
pancreatic polypeptide (F cell)
The Exocrine Pancreas
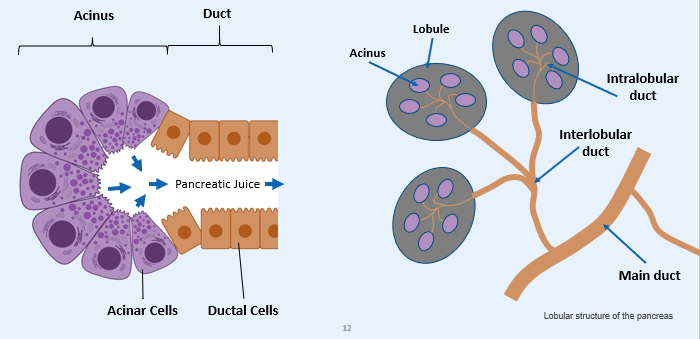
The Exocrine Pancreas - ACINAR SECRETIONS
Acinar Secretions
1) Rich in enzymes, Na+, Cl- and H2O
2) Triggered by acetylcholine from the vagus nerve
3) Triggered by CCK in response to fat/protein in chyme
The Exocrine Pancreas - DUCTAL SECRETIONS
Ductal Secretions
1) Rich in bicarbonate, Na+ and H2O
2) Triggered by secretin in response to highly acidic chyme
The Exocrine Pancreas - PANCREATIC JUICE
1) Unlike saliva, pancreatic juice remains isotonic
2) Pancreatic juice is an enzyme rich, slightly alkaline liquid
Examples of PANCREATIC ENZYMES
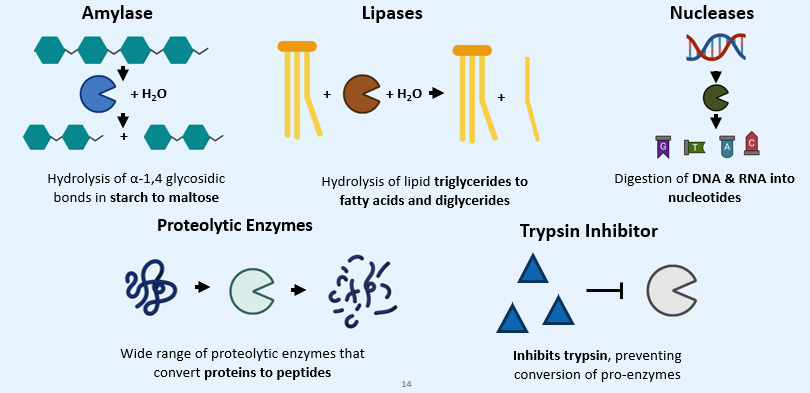
Activation of Proteolytic Enzymes
1) Proteolytic enzymes are produced as inactive precursors called zymogens
2) Small intestinal brush border enterokinase enzyme cleaves hexapeptide to form active trypsin from trypsinogen
3) Trypsin cleaves and activates other proteolytic enzymes
4) Process prevents pancreatic autodigestion (+ activity of trypsin inhibitor)
CFTR and Bicarbonate Secretions
1) Duodenal H+ causes enteroendocrine cells to produce secretin
2) Secretin binds to the secretin receptor (SCTR) at the basolateral membrane
3) Secretin binding triggers cyclic adenosine monophosphate (cAMP) second messenger pathways
4) cAMP upregulates activity of the cystic fibrosis transmembrane conductance regulator (CFTR) Cl- and HCO3− channel at the apical membrane.
5) Secretin stimulates high volume of HCO3- rich pancreatic juice to buffer acid
Phases of Pancreatic Secretions
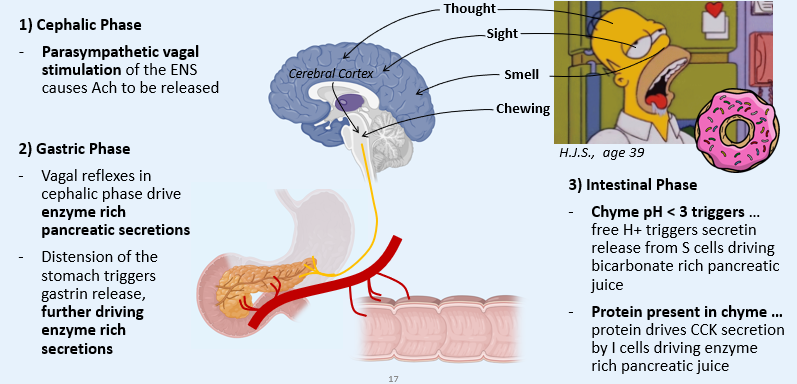
Question 2

How is bile STORED?
Bile is made by the hepatocytes in the liver
Storage of bile
1) Secreted via the common hepatic duct
2) Can be stored in gall bladder via cystic duct, or directly released into the intestines
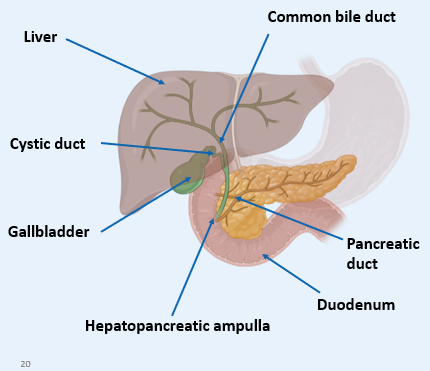
How is bile SECRETED?
Direct secretion of bile
1) Via common bile duct joining the pancreatic duct to drain into the duodenum at the hepatopancreatic ampulla
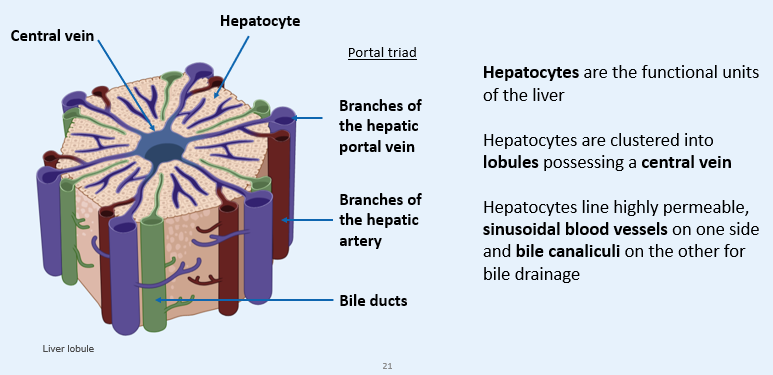
What are HEPATOCYTES?
What is BILE?
Bile is a greenish liquid containing water, salts, cholesterol, bile pigment bilirubin and electrolytes
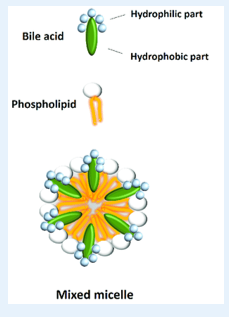
Functions of Bile - FAT DIGESTION AND ABSORPTION
Fat digestion and absorption
1) Bile salts (amphipathic) emulsify fats for digestion by pancreatic lipase and form micelles for absorption
Functions of Bile - ELIMINATION OF WASTE PRODUCTS
Elimination of waste products
1) Bilirubin (pigment) from haem in red blood cell degradation (breakdown product stercobilin gives faecal brown colour)
How is bile secretions REGULATED?
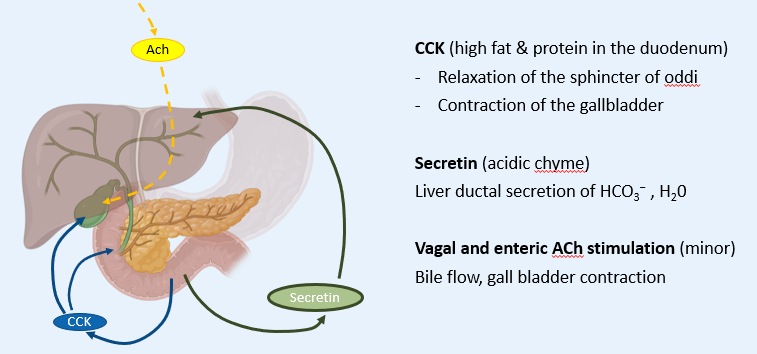
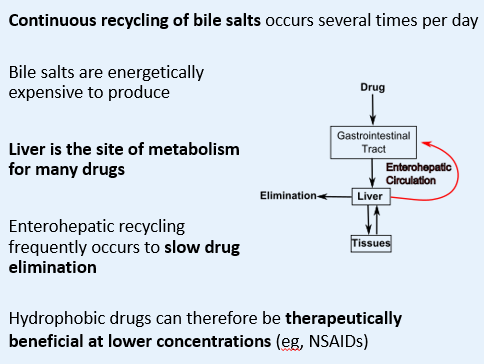
What is the ENTEROHEPATIC CIRCULATION?
Excretion of BILIRUBIN in bile
1) Haem from old/faulty RBC converted to bilirubin (orange) and transported to liver bound to albumin
2) Conjugated (made hydrophilic) with glucuronic acid and excreted in bile
3) Gut bacterial hydrolysis (b glucuronidase) deconjugates bilirubin to form urobilinogen
4) Urobilinogen reduced to stercobilin, excreted in faeces (brown colour)
Question 3

Dysfunction in Intestinal Secretions - COELIAC DISEASE

Dysfunction in Enzyme Activation Process - PANCREATITIS

Dysfunction in Ductal CFTR Cl- channel - CYSTIC FIBROSIS

Dysfunction in the Gall Bladder - GALLSTONES

What is JAUNDICE?
1) The build up of bilirubin in extracellular fluid (serum bilirubin >30-60 mmol.L-1)
2) Yellow discoloration of skin and sclera
3) May occur when underlying disease processes disrupt the production and excretion bilirubin
Causes of Jaundice - PRE-HEPATIC
Excessive RBC breakdown and build up of unconjugated bilirubin
eg haemolytic anaemia
Causes of Jaundice - HEPATOCELLULAR/CONGENITAL
Altered hepatocyte function
eg Crigler-Najjar syndrome
Causes of Jaundice - POST-HEPATIC
Obstruction to normal bile drainage, build up of conjugated bilirubin
eg gallstones
Question 4
