MOD 1.2 Midterm
1/40
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
41 Terms
deficient enzyme in cystinuria? presentation? lab result?
cystine transporter (SLC3A1 + 7A9)
cystine stones
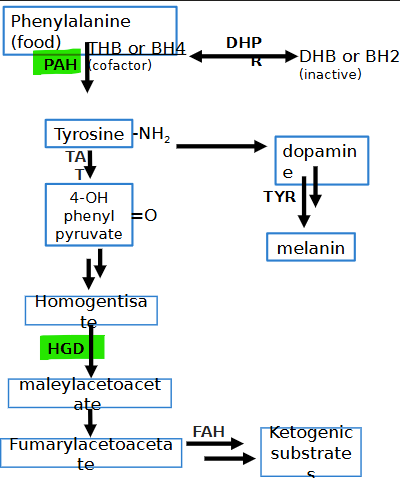
deficient enzyme in phenylketonuria (PKU)? presentation? lab result?
phenylalanine hydroxylase (PAH) *BH4
musty odor, eczema, neuro disabilities, tremors
low tyrosine/melanin, high phenylalanine/phenyl ketones
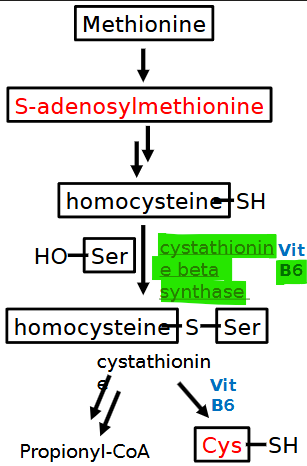
deficient enzyme in homocystinuria? presentation? lab result?
cystathionine beta synthase (CBS) B6 OR met. synthase *B12
ectopia lentis, skeletal w/ marfanoid features
high homocysteine/methionine + low cysteine
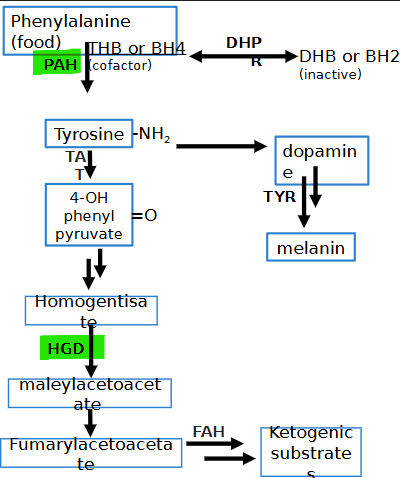
deficient enzyme in alkaptonuria? presentation? lab result?
homogentisate 1,2-dioxygenase (HGD)
dark urine/skin/eyes, cartilage damage = stiff joints
high homogentistic acid + low ketogenic substrate
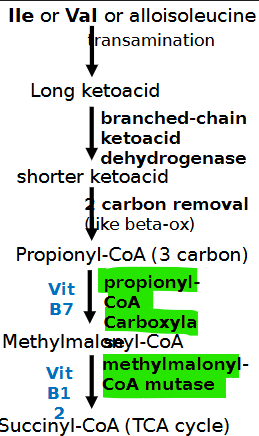
deficient enzyme in maple syrup urine disease (MSUD)? presentation? lab result?
branched-chain alpha-keto acid dehydrogenase (BCKDH)
sweet smelling urine, muscular rigidity, seizures, opisthotonos, vomiting, lethargy
ketosis + inc. BCAA (leucine, isoleucine, valine)
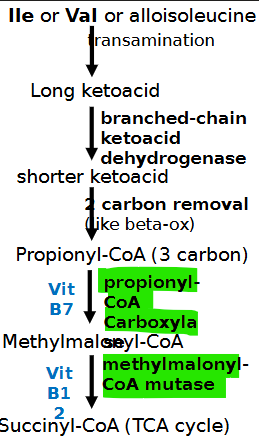
deficient enzyme in propionic acidemia? presentation? lab result?
propionyl-coa carboxylase PCAA or PCCB gene
vomit after feeding, seizures, coma, death, cardiomyopathy, hypotonia, encephalopathy
VOMIT (dec. Val, OCFA, Met, Ile, Thr), AGMA, inc. propionic acid + ketones in urine
deficient enzyme in isovaleric acidemia? presentation? lab result?
isovaleryl-coa dehydrogenase
sweaty feet odor, vomit, encephalopathy, tachypnea
ketoacidosis, hypoCa, hypoglycemia, hyperammonia
deficient enzyme in methylmalonic acidemia? presentation? lab result?
methylmalonyl-coa mutase *B12
renal failure, hypotonia, hepatomegaly, thrombopenia
high MMCA, homocysteine, ammonia, ketoacidosis
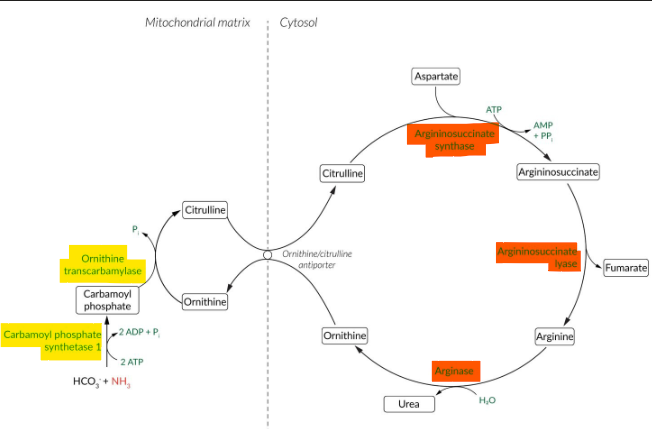
what enzymes are deficient in proximal urea cycle disorders? labs? presentation?
carbamoyl phosphate synthetase (CPS1) or N-acetyl glutamate synthase (NAGS) def.
low citrulline + Arg, hyperNH3, resp. alk., normal orotic acid
ornithine transcarbamylase (OTC) def.
““, high orotic acid + X-linked
presentation → lethargy, vomit, seizure, cerebral edema
treat w/ protein restriction
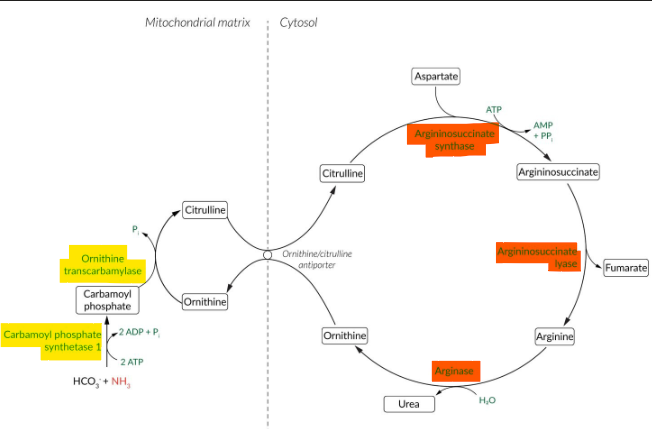
what enzymes are deficient in distal urea cycle disorders? labs? presentation?
argininosuccinate synthetase (ASS) (= same as prox.) OR argininosuccinate lyase (ASL) def.
high citrulline + glutamine, low arginine, hyperNH3, resp. alk
ASL → trichorrhexis nodosa (brittle, beaded hair)
arginase-I def.
““ + high arginine
spasticity, dev. delay, regression
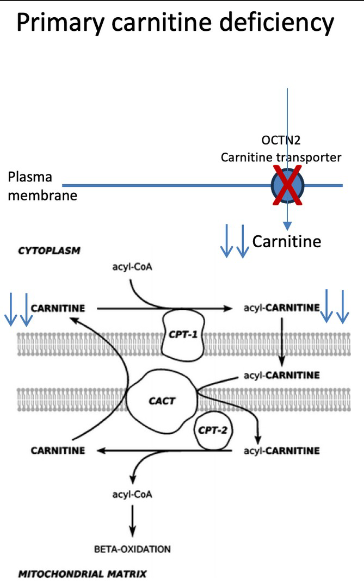
primary carnitine deficiency lab results? presentation?
OCTN2 or SLC22A5
low plasma carnitine
cardiomyopathy, muscle weakness, fasting intolerance
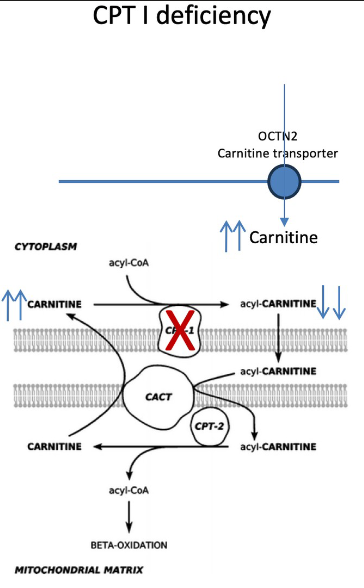
carnitine palmitoyl transferase I (CPT1) deficiency lab results? presentation?
fxn: acyl-coa → acylcarnitine
hypoketoic hypoglycemia, high free carnitine, low acyl carnitine
hepatomegaly, poor feeding, lethargic, hypotonic
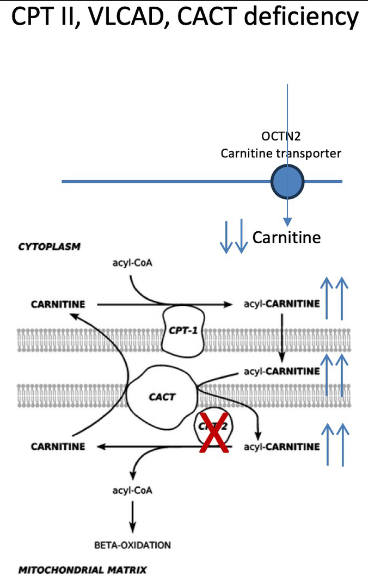
carnitine palmitoyl transferase II (CPT2) deficiency lab results? presentation? what other deficiencies cause this?
fxn: acylcarnitine → acyl coa (B-ox)
hyoketotic hypoglycemia, inc. C14-C18 acyl carnitines
myopathy rhabdomyolysis, urine discoloration after exercise (myoglobin)
also via: carnitine-acylcarnitine translocase (SLC25A20) (CACT)+ very long chain acyl coa dehydrogenase (VCLAD)
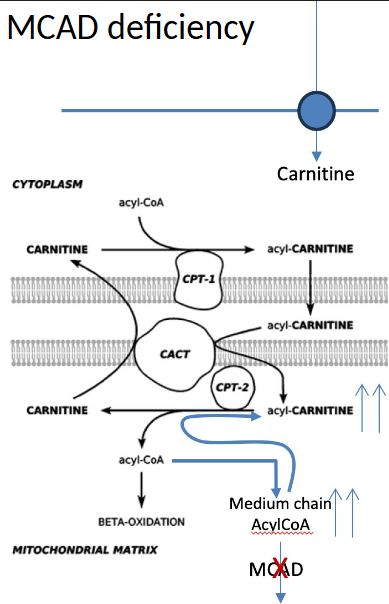
medium chain acyl coa dehydrogenase deficiency lab results? presentation?
MCAD + ACADM/S/L
hypoketotic hypoglycemia, inc. C6-C10 acyl-carnitines
seizures, hepatomegaly, sudden death
full agonist? partial agonist? inverse agonist?
full → produce same max response as endogenous ligand when binds receptor (=full efficacy)
partial → produce partial response when binds receptor (regardless of conc.)
inverse → produces opposite response to full or partial agonist when binds receptor
antagonist function? competitive vs non competitive?
prevent agonist from binding receptor (but has no response when binds = affinity NOT efficacy)
competitive (w/ agonist/reversible) → parallel + shifted up curve
noncompetitive (diff. receptor/irreversible)
types of antagonism?
pharmacological → same receptor
physiological → agonist response mediated thru receptor is antagonized by agonist on different receptor
chemical → forms complex w/ agonist to reverse its actions
therapeutic index? LD50? ED50? EC50?
relates dose of a drug required to produce desired effect to that which produces undesired effect
TI: LD50/ED50 → lethal dose for 50%/effective dose for 50%
ED50 → which dose produces 50% max. response
EC50 → effective conc. for 50% effect
down regulation? up regulation?
down: phosphorylation → internalize membrane receptor + regulate receptor gene → # of receptors on membrane dec. (tolerance)
up: chronic exposure to antagonist initially inc. response of receptor (super sensitivity), then inc. # of receptors on membrane surface
gradual (cont.) dose response curves? quantal (all or none) dose response curve?
graded → btwn dose + magnitude of drug effect in particular tissue type
determine max. efficacy of drug in single subject
quantal → btwn dose + cumulative percentage of subjects exhibiting an all or none effect
shows sensitivity of a pop. to a drug
additive effect? synergism? potentiation?
additive → equal to sum of individual drug effect (e.g 2+2=4)
synergism → effect is greater than sum of individual drug effects A & B (e.g 2+2>4)
potentiation (similar to synergism) → drug B has no therapeutic effect alone, enhance therapeutic action of drug A (e.g 2+0>2) = parallel + left shifted curve
signal transduction pathway? permissive effect? tachyphylaxis?
path → ligand bind = conformation change in receptor, receptor interaction w/ effector molecule/2nd messenger (cAMP, IP3, DAG, Ca) = response
permissive → presence of substance A required for full effect of substance B
tachyphylaxis → acute dec. response to drug after initial/repeated administration
affinity (KD)? efficacy or intrinsic activity? potency?
affinity → ability to bind receptor
efficacy → ability of drug to produce response
potency → comparative measure of 2 drugs that produce same effect
what are GPCR? Ga subunit function? types?
adrenoreceptors → act. via epinephrine
Ga subunit = site of GTP hydrolysis
Ga (stim.) → B-adrenoreceptor + D1 dopaminergic
Ga (inhibit) → M2, a-adrenergic 2, D2 (MAD 2s)
Ga (stim.) → histamine 1, a-adrenergic 1, vasopressin, M1, M3 (HAVe 1 M&M)
Ga subunit mechanism?
Gas (stim.) → inc. AC → inc. cAMP → act. PKA → phos. enzyme protein
Gai (inhibit) → dec. AC → dec. cAMP → deact. PLA → dephos. enzyme protein
Gaq (stim.) → act. phospholipase C → inc. IP3 + DAG → inc. Ca → combine w/ DAG → act. PKC → phos. enzyme proteins
ligand gated ion channel function? activation? receptors?
open when they bind → ion channels open
act. via furosemide
receptors:
GABAa: Cl ion flux → hyperpolarization
nicotinic receptor: Na ion influx → contraction
what are membrane bound enzymes? activation? receptors?
cyclooxygenase, phospholipase A2
act. via aspirin + glucocorticoid
receptors:
guanylate cyclase → atrial natriuretic factor (ANF)
tyrosine kinase → insulin, epidermal growth factor (EGF), nerve growth
nucleic acid role in protein receptors?
act. by cyclophosphamide
type 1 nuclear receptor: target for sex hormones
type 2 nuclear receptor: for nonsteroid ligands like thyroid hormone, vit. A, vit. D, retinoid
what are the sphingolipidoses disorders?
gaucher
niemann pick A/B + C
tay sachs
krabbe
fabry
metachromatic leukodystrophy
deficient enzyme/gene in gaucher disease? characteristics?
B-glucocerebrosidase (GBA)
crumpled paper MO, hepatosplenomegaly, bone abnormality (aseptic necrosis, osteoporosis, pancytopenia)
deficient enzyme/gene in niemann pick A/B? characteristics?
sphingomyelinase (SMPD1)
foamy/lipid laden MO, cherry red spots, bone issues, hepatosplenomegaly
deficient enzyme/gene in niemann pick C? characteristics?
NPC gene mut.
above + speech problems, seizures, ataxia, down gaze palsy
deficient enzyme/gene in tay-sachs? characteristics?
hexosaminidase A (HEXA)
GM2 gangliosides accumulate, cherry red spots (retinal pallor) + neurodegeneration (seizures, weakness, blind → startle response)
deficient enzyme/gene in krabbde disease? characteristics?
galactocerebrosidase
globoid cells, demyelination (peripheral neuropathy + optic atrophy), fever, muscle weakness, stiff, posture, deafness seizures
deficient enzyme/gene in fabry disease? characteristics?
a-galactosidase A (x-linked)
skin issues, hypohidrosis, peripheral neuropathy, angiokeratomas
adult; cardio issues, stroke, renal failure
deficient enzyme/gene in metachromatic leukodystrophy? characteristics?
arylsulfatase A (ARSA)
central + peripheral demyelination → ataxia + dementia
neuro, hearing, vision + muscle/gait issues
what are the mucopolysaccharidoses disorders? what accumulates?
hurler (MPS I) + hunter (MPS II)
heparan + dermatan sulfate accumulate
deficient enzyme/gene in hurler (MPS I)? characteristics?
a-L-iduronidase
corneal clouding, glaucoma, coarse facial features, macrocephaly, bone/joint disease (dysostosis), hepatosplenomegaly, umbilical hernias, cardiac issues
deficient enzyme/gene in hunter (MPS II)? characteristics?
iduronate 2 sulfatase (x-linked)
aggression, bone disease, coarse features, cardiomegaly, death
deficient enzyme/gene in I cell disease? characteristics?
mycolipidosis disorder
N-acetylglucosamine (NAG) phosphotransferase GNPTA
coarse features, umbilical hernias, MSK issues, cloudy corneas, gingival hyperplasia, macroglossia, inclusion cells accumulate
deficient enzyme/gene in pompe disease? characteristics?
glycogen storage disorder
lysosomal a-glucosidase (maltase)
floppy baby, cardiomegaly, macroglossia, MSK weakness, dev. delays, pulm. issues