COMD 4333 Exam 3
1/33
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
34 Terms
Auditory System
Explain the different forms of energy (mechanical, hydraulic, electrical, neurochemical) created in the auditory system from the external auditory meatus/tympanic membrane to the auditory nerve (cranial nerve VIII).
Sound waves → Mechanical energy (movement)
Vibration/pressure from sound waves moves tympanic membrane and ossicles
Mechanical energy → Hydraulic energy (fluid)
Movement of tympanic membrane & ossicles causes movement of fluid in cochlea
Hydraulic energy → Electrical energy (nerve impulses)
Fluid movement causes movement of hair cells in cochlea
Electrical energy → Neurochemical energy (Action potential)
Hair cells release glutamate, exciting the auditory nerve (CN VIII)
Brain Pathway
CN VIII → cochlear nucleus → superior olivary complex → lateral lemniscus → inferior colliculus → medial geniculate body → auditory cortex (Heschl’s gyrus)
Describe how the Organ of Corti functions. Be sure to mention the basilar membrane, fluid, inner and outer hair cells, and tectorial membrane.
Explain what happens when the basilar membrane moves, including what happens to the stereocilia, what tip-links are, where the potassium channels are, what causes opening of calcium channels, and what happens when calcium enters the hair cells.
Produces nerve impulses in response to sound vibrations.
Basilar Membrane: what the Organ of Corti sits on top of
Fluid: Endolymph (high in K+) causes Basilar Membrane to move up and down and thus displaces Organ of Corti
Inner Hair Cells: 1 row, sensory only, each synapse with multiple spiral ganglion neurons
Outer Hair Cells: 3 rows, sensory and motor onto each spiral ganglion neuron
Stereocilia: extend from hair cells in proximty to Tectorial Membrane (on top of Organ of Corti); arranged by length; Kinocilium being the tallest type of sterocillia
Tip Links: connect Sterocillia
When fluid moves → basilar membrane moves → organ of corti moves, stereocilia bend toward kiniocilium → tip links open → influx of K+ (potassium) ions from Endolymph enter hair cell
=> Depolarization
Depolarization opens Ca (calcium) channels, causes Ca to enter hair cells
Ca enters hair cells → triggers release of neurotransmitter Glutamate
Glutamate binds to receptors on Spiral Ganglion Neurons; their axons create auditory/cochlear portion of CN VIII
Cilia bend away from Kinocilium → tip links close → no influx/no further response from hair cell
What are outer hair cell microtubules and how do they impact hearing?
remember, outer hair cells receive efferent signals that can activate Microtubules.
Microtubules are structures that lengthen OHC cell bodies. They enhance our hearing via Electromotility.
Electromotility: conversion of Electrical energy → Mechanical forces
Increases effect of Basilar Membrane movement and thus displacement of cilia
DETECTION OF LOW INTENSITY SOUNDS
How do they impact hearing?
OHC microtubules improve detection of low intensity sounds.
100-fold increase in effect of actual basilar membrane movement
They decreases the need for a stronger signal to movie basilar membrane/triggering action potential; OHC are already lengthened enough to shear against tectorial membrane
increased effect of basilar membrane, allows us to hear sounds better
Describe the auditory pathway starting from the cochlear nerve neurons all the way to Heschl’s gyrus. Identify where there are crossovers and synapses.
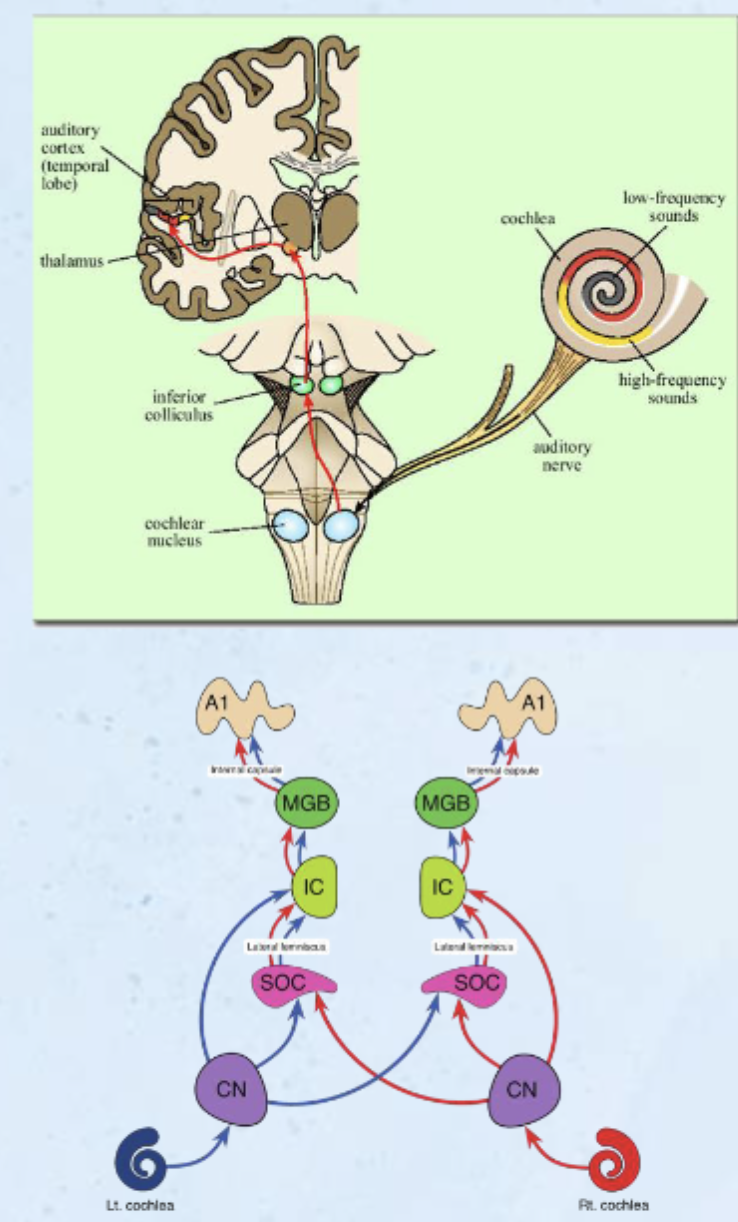
C-SLIMA
spiral ganglion axons —> brainstem, synapse in cochlea nuclei
Cochlear Nuclei synapse
ipsilateral, monaural processing
80% cross over to contralateral SOC
ALL processing is Binaural beyond cochlear nuclei
CROSS OVER Superior Olivary Complex WHERE SOUND LOCALIZATION OCCURS synapse
receives information from both ears
localizes based on time delay and intensity difference
Lateral Leminiscus no synapse
Tract between SOC and Inferior Colliculus/SOC extend through Lateral Leminiscus
Inferior Colliculus synapse
Some signals sent from Inferior Colliculus to superior colliculus for auditory-visual integration
synapse in Inferior Colliculus
Medial Geniculate Body (in thalamus) synapse
from ipsilateral Inferior Colliculus
A1/Heschl’s Gyrus synapse
from Ipsilateral MGN
What thalamic nuclei does the information from the auditory system synapse in?
How are frequency, intensity, and localization coded?
What neuroanatomical structures are involved in how these attributes of sound are coded?
Frequency
Place Coding: hair cell location on basilar membrane (base = high; apex = low)
Characteristic Frequencies: hair cells respond best (fire more action potentials) to specific sound frequencies
Tonotopic Organization: specific frequencies map to specific places
Intensity
number of Action Potentials
number of Neurons sending action potentials
Localization
Interaural Time and Intensity Differences
The difference in arrival time of a sound between two ears.
The difference in intensity between the two ears.
sound wave travels around the head; reaches second ear later and a bit softer
neuroanatomical structures: cochlea, C-SLIMA
What benefit comes from having binaural stimuli in the superior olivary complex? Hint: interaural time delay
The benefit of having binaural input in the superior olivary complex is that it allows the brain to detect interaural time differences, or the timing differences in when a sound reaches each ear.
Because sound reaches one ear slightly before the other, neurons in the superior olivary complex compare the timing of input from both ears. This enables the system to precisely localize sound from the left or right side.
How is the primary auditory cortex organized and where is it?
organization: Tonotopic Organization
location: dorsal surface of Superior Temporal Gyrus

What is cortical deafness? How is it caused? How does it compare to pure word deafness?
Cortical Deafness
what is it? rare form of hearing loss
cause: Bilateral damage to Heschl’s Gyrus, intact peripheral auditory system & pathways to cortex
Impaired speech comprehension, repetition, recognition of noise/music, impaired hearing insensitivity
Pure Word Deafness
what is it? rare form of hearing loss
cause: damage to White Matter between primary and association areas
Impaired Comprehension of speech sounds (they sound like noise; uninterpretable)
Preserved reading, writing, speaking, GOOD auditory perception of NOISES
Vestibular System
What is the difference between semicircular canals and otolith organs?
3 Semicircular Canals
Anterior semicircular canal
Posterior semicircular canal
Lateral semicircular canal
At right angles
Function: rotation and angular acceleration
SEMICIRCULAR = ROTATION, ANGULAR
2 Otolith Organs
Utricle (horizontal)
Saccule (vertical)
Function: linear acceleration
UTRICLE, SACCULE, LINEAR
-le = linear
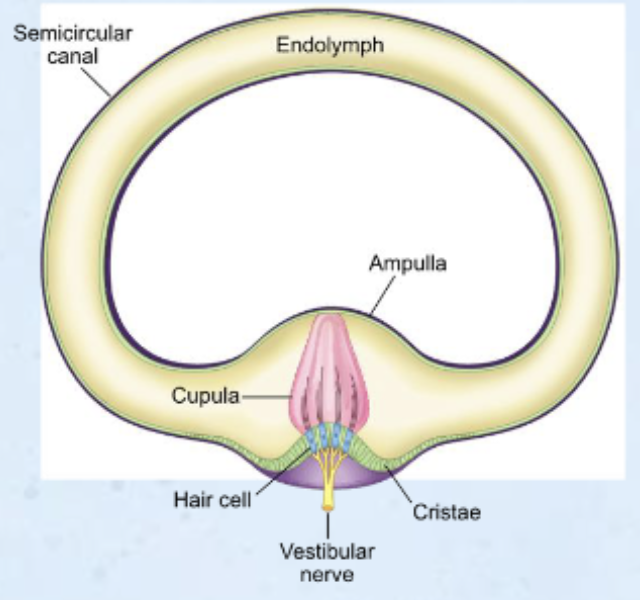
Explain how the semicircular canals are related to maintaining balance (e.g., with head movement) and what causes action potentials in vestibular nerve axons (include the ampulla, cupula, cristae, and hair cells)
help maintain balance by detecting rotational head movements
base of each canal is an enlarged region called the ampulla, which contains the crista ampullaris (cristae), a ridge of sensory hair cells. The stereocilia of these hair cells project into a gelatinous structure called the cupula.
ampulla: at base of each canal, contains crista (sensory organ, contains hair cells); these hair cells, which have sterocilia on top of them, encased in cupula (gelatinous structure)
movement of head causes → movement of endolymph in semicircular canals causes → movement of cilia toward kinocilium opens → K+ channels causes depolarization opens → calcium channels triggers → glutamate release
GLUTAMATE BINDS TO RECEPTORS ON SCARPA GANGLION NEURONS (vestibular portion of CN VIII) → creates EPSPs
these EPSPs send information about head movement to the brain, helping maintain balance and spatial orientation
WHAT CAUSES ACTION POTENTIALS IN VESTIBULAR NERVE AXONS? Glutamate released from depolarized hair cells binds to receptors on Scarpa’s ganglion neurons, generating EPSPs that summate to trigger action potentials in vestibular nerve axons.
movement of cilia away from kinocilium → closing of K+ channels → hyperpolarization & no signal
example: As your head rotates, the fluid in the semicircular canals lags behind due to inertia. This pushes the cupula in the ampulla, bending the hair cells in the cristae. In the left ear, the stereocilia bend toward the kinocilium, increasing firing in the vestibular branch of the Vestibulocochlear nerve, while in the right ear they bend away, decreasing firing.
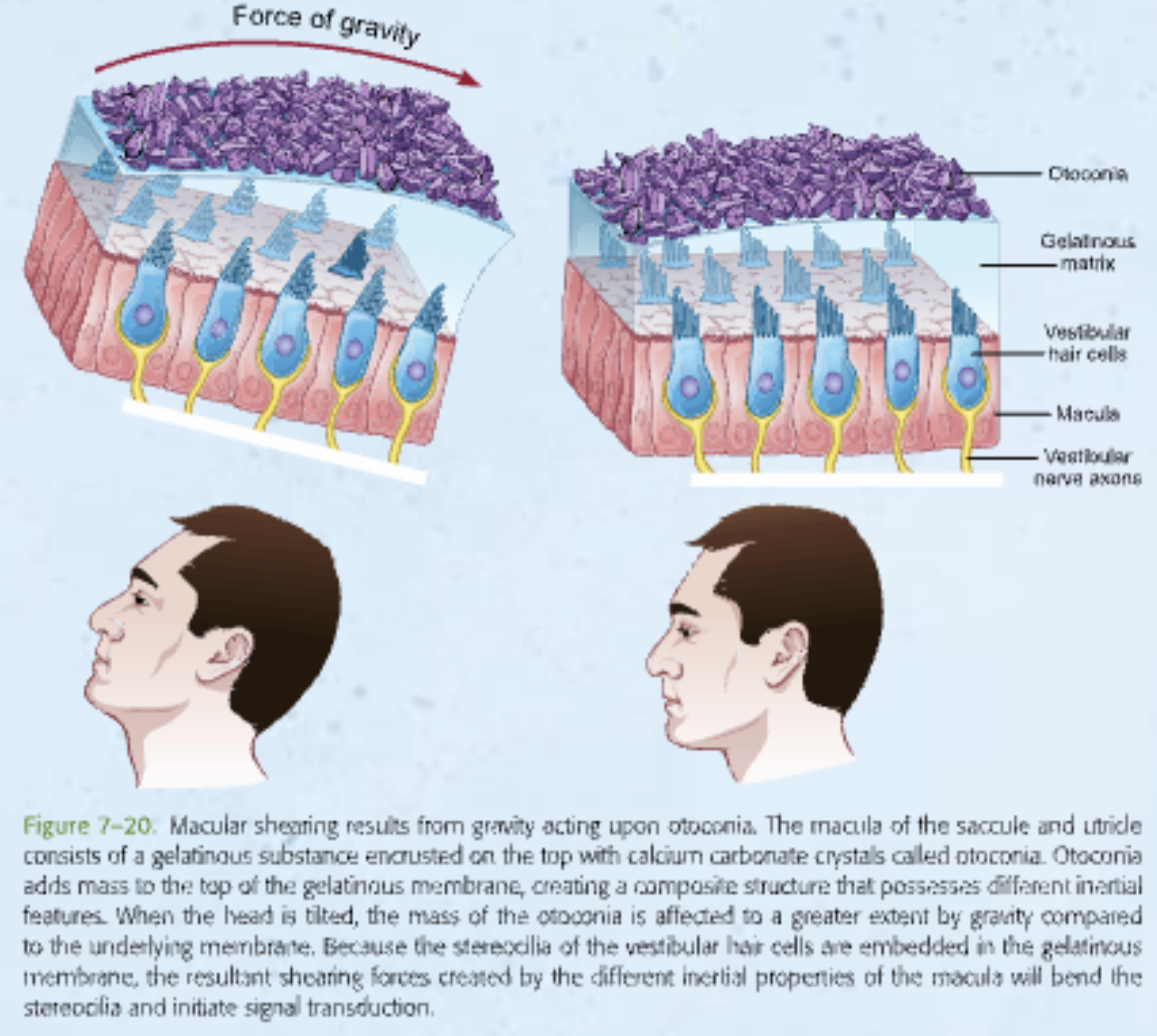
Describe the otolithic organs including their names, where they are located, the maculae, otolithic membrane, and otoconia. How are action potentials generated in the vestibular nerve axons?
2 Otolithic Organs
Utricle (horizontal)
Saccule (vertical)
IN VESTIBULE OF INNER EAR!
macula: sensory patches inside utricle/saccule, embedded with hair cells
otolithic membrane: gelatinous structure; where cilia is embedded
otoconia: calcium carbonate crystals, on top of otolithic membrane
head movement shifts → otolithic membrane (shifting enhanced by weight of otoconia)
cilia bend toward kinocilium → open K+ channels → depolarization → open Ca2+ channels → release of neurotransmitter
Glutamate then binds to receptors on neurons in Scarpa's ganglion, which are part of the vestibular portion of the Vestibulocochlear nerve. This binding produces excitatory postsynaptic potentials (EPSPs); if these EPSPs reach threshold, they generate action potentials in vestibular nerve axons that transmit information about head position and linear movement to the brain. If the stereocilia bend away from the kinocilium, the opposite occurs (hyperpolarization and reduced firing rate).
sensory patches within the inner ear's utricle and saccule, vital for balance by detecting linear acceleration and head tilt. They consist of hair cells embedded in a gelatinous membrane weighted with calcium carbonate crystals (otoconia) that shift with gravity.
What is the function of the vestibular system? Where do different projections from the vestibular nuclei go to carry out these functions?
maintain balance, spatial orientation, and stable vision during movement
eye movement; head/eye position; visual fixation with head movement
movement and reflex coordination
maintain balance/equilibrium; proprioception
visercal-autonomic activities; cause of sea-sickness/motion sickness
vestibular nuclei projections
superior colliculus (midbrain)
cerebellum (vestibulocerebellum)
spinal cord
reticular formation
Olfaction and Gustation
What kind of receptors do olfaction and gustation rely on?
Smell (olfaction) and taste (gustation) are Chemical Senses sensed by
Chemoreceptors.
Where are the olfactory receptors? Where are the gustatory receptors?
Olfactory Receptors
olfactory epithelium
Gustatory Receptors
tongue, (pharynx, palate, epiglottis)
Know that the thalamus plays a role in sensory processing for every sense except olfaction.
What is anosmia? What is ageusia?
What are the similarities and differences between conductive anosmia and sensorineural anosmia?
Anosmia
loss of sense of smell
2 types of Anosmia
Conductive anosmia: blockage of transmission
Cold
Allergies
Tumors
Sensorineural anosmia: caused by damage to neurons/pathways involved in cell
TBI
Alzheimer’s Disease
Parkinson’s Disease
Healthy Aging
both are associated with a loss of sense of smell, but differ in causes.
Ageusia
loss of sense of taste
Impairments often lead to loss of appetite and weight loss
Visual System
Describe the function of the different types of cells found in the retina (rods, cones, bipolar cells, ganglion cells)
Compare and contrast the functions and distribution of rods and cones
Rods
type of photoreceptor, responds to light
function: detect shape, size, brightness
light doesn’t matter; fine in strong or low
location: distributed throughout retina, not Fovea
Cones
type of photoreceptor, responds to light
function: detect color (r, b, g), fine detail
best in strong light
location: primarily in Fovea
RODS: SHAPE; SIZE; BRIGHTNESS; LIGHT DONT MATTER; DISTRIBUTED THROUGHOUT RETINA
CONES COLOR (r, b, g) AND FINE DETAL; BEST IN STRONG LIGHT; FOVEA
Bipolar Cells
connects Photoreceptors to Ganglion Cells
Ganglion Cells
their axons extend out of eye to form Optic Nerve
AXONS OF GANGLION CELLS FORM OPTIC NERVE (CN II)
rods, cones, bipolar cells, ganglion cells
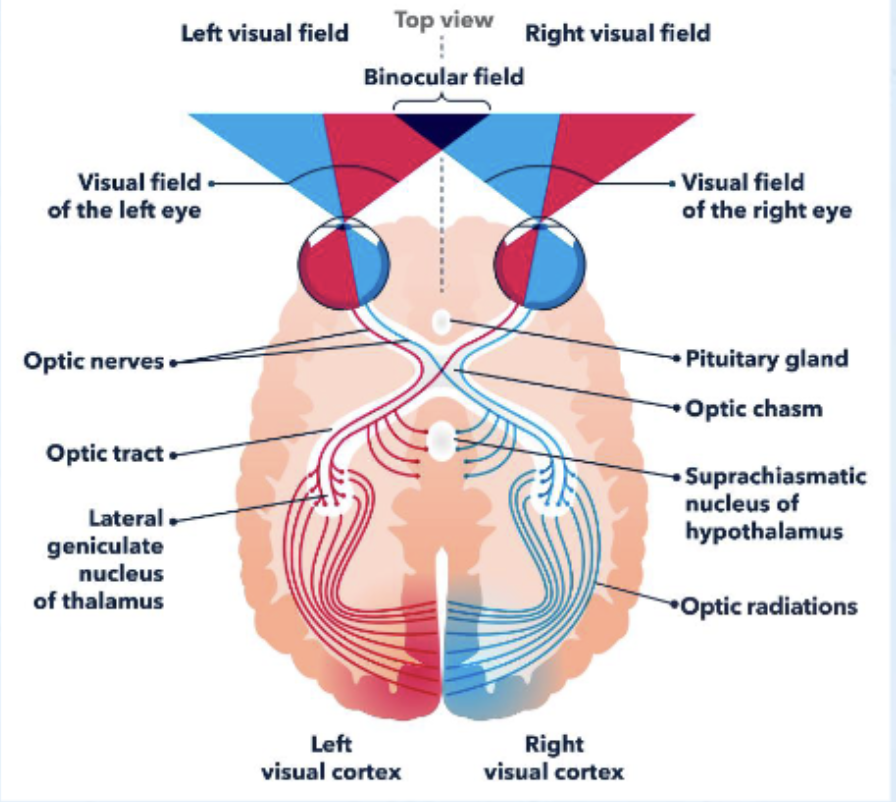
Be able to label all regions of the visual pathway from the retina to the occipital lobe including where the synapses are.
What regions do fibers in the optic tract branch of to? For what functions?
What information crosses over at the optic chiasm?
What thalamic nuclei does the information from the visual system synapse in?
Retina
Optic Nerve (CN II)
Optic Chiasm
Where fibers decussate
Information that crosses over: Nasal retinal field axons (temporal retinal field axons stay ipsilateral)
Optic Tract
Some fibers branch off from optic tract to synapse on:
Suprachiasmatic nucleus of hypothalamus: function=circadian rhythm
Superior colliculus: function-orientation of head to visual stimuli, allows for blindsight
what thalamic nuclei does the info from the visual system synapse in? Lateral Geniculate Nucleus (thalamus)
Synapse of contralateral visual field axons; NEW NEURON STARTS
Optic Radiation
Occipital Lobe/V1
retina, optic nerve, optic chiasm, optic tract, lateral geniculate nucleus, optic radiation, V1
Know the difference between visual and retinal fields.
Visual Fields
What you see; External area visible to eyes without movement
Refers to the actual environment you see (external space)
Divided into left and right visual fields
👉 Example:
Everything to your left of fixation = left visual field
Everything to your right = right visual field
Retinal Fields
image refracted onto retina; focused representation of visual fields
Refers to where light hits on the retina inside the eye
Image is inverted and reversed
👉 Key rule:
Left visual field → right side of each retina
Right visual field → left side of each retina
Left visual field hits:
Nasal retina of left eye
Temporal retina of right eye
Right visual field hits:
Nasal retina of right eye
Temporal retina of left eye
For each eye, the visual field on the same side projects to the nasal retina, while the opposite visual field projects to the temporal retina due to image reversal by the lens.
Where is the primary visual cortex located? How is it organized?
location: occipital lobe
retinotopic organization: ordered mapping of the visual field from the retina onto target areas of the brain
Be able to label and explain the visual field defects caused by damage to the optic nerve, optic chiasm, optic tract, geniculocalcarine fibers, and primary visual cortex.
Optic Nerve lesion
Monocular Blindness: loss of vision in ipsilateral eye
Damage to the optic nerve causes monocular blindness because it interrupts all visual information from one eye before any fibers cross to the opposite side.
Optic Chiasm lesion
Bitemporal Heteronymous Hemianopia (“tunnel vision”): Loss of temporal (peripheral) visual fields in both eyes
Caused by damage to crossing nasal fibers
Damage to the optic chiasm causes bitemporal hemianopia because it disrupts the crossing nasal retinal fibers, which carry information from the temporal (peripheral) visual fields of both eyes.
Optic Tract lesion
Homonymous Hemianopia: Loss of vision in same visual half of each eye
Damage to the optic tract causes homonymous hemianopia because each optic tract carries information from the opposite visual field of both eyes.
Geniculocalcarine Fibers lesion
Homonymous quadrantanopsia: Loss of vision in same visual quadrant of each eye (L/R)
Damage to the geniculocalcarine fibers causes homonymous quadrantanopsia, which is the loss of vision in the same quadrant of both eyes, because these fibers carry information from specific portions (quadrants) of the contralateral visual field from the lateral geniculate nucleus.
Primary Visual Cortex lesion
Homonymous Hemianopsia with central sparing
Blindness in opposite field of vision in each eye
Central vision can be spared
Damage to the primary visual cortex causes homonymous hemianopia with macular sparing because each hemisphere processes the opposite visual field, and central vision is often preserved due to dual blood supply.
What kind of information is processed in V3, V4, and V5?
V3 – form
V4 – color & form
V3a & V5 – motion
form / color and form / motion
Describe the dorsal and ventral visual pathways and what kinds of deficits can occur with damage to each.
Dorsal Visual Pathways
“Where” pathway
Goes to parietal lobe
Function: To determine locations of objects in space
Damage:
Difficulty localizing objects in space
Can name & describe object, would have difficulty picking it up
Visual disorientation, difficulty using a map
Ventral Visual Pathways
“What” pathway
Goes to inferior temporal lobe
Function: To identify objects/images
Damage:
Agnosia- inability to recognize objects, words, faces, etc.
Define/describe apperceptive agnosia, associative agnosia, achromatopsia, akinetopsia, cortical blindness, and blindsight.
Apperceptive agnosia
Difficulty recognizing an object due to a perceptual deficit
WAY TO TEST: ability to draw or copy something; bad drawinf
Difficulty recognizing something because they have a hard time perceiving it
Associative agnosia
Difficulty recognizing or attaching meaning to an item with preserved perception
WAY TO TEST: can copy pictures perfectly but could not name the object RECOGNIZING WHAT SOMETHING LOOKS LIKE, WITH WHAT IT IS; perfect drawing, cant name it
Ex: show a key, cant visually identify it, but if given to hold it, they can use other senses to identify
Achromatopsia CHROM-TOPSIA
difficulty recognizing colors (severe = no color vision)
Akinetopsia KINE-TOPSIA
difficulty recognizing movement, loss of perception of movement
V3a, V5
Cortical Blindness
profound vision loss caused by damage to the brain's occipital cortex (VI) rather than the eyes
Blindsight
neurological phenomenon where patients with damaged primary visual cortex (V1) report being blind but can unconsciously detect, localize, and react to visual stimuli aka without conscious visual awareness
patients with damaged primary visual cortex (VI) can respond to visual stimuli in their blind fields without conscious perception.
Patients might accurately guess the orientation of a line, point to a light, or navigate around obstacles despite reporting that they see nothing.
What are the names, numbers, and functions of the cranial nerves involved in the senses above (auditory, vestibular, vision, olfaction, gustation)?
👃 Olfaction (Smell)
Olfactory nerve (CN I)
→ Function: Carries sensory information for smell from the olfactory epithelium to the brain
👁 Vision
Optic nerve (CN II)
→ Function: Carries visual information from the retina to the brain
👅 Gustation (Taste)
Facial nerve (CN VII)
→ Function: Taste from anterior 2/3 of the tongue
Glossopharyngeal nerve (CN IX)
→ Function: Taste from posterior 1/3 of the tongue
Vagus nerve (CN X)
→ Function: Taste from epiglottis and lower pharynx
👂 Auditory (Hearing)
Vestibulocochlear nerve (CN VIII)
→ Function: Hearing (cochlear branch)
⚖ Vestibular (Balance)
Vestibulocochlear nerve (CN VIII)
→ Function: Balance, head movement, spatial orientation (vestibular branch)
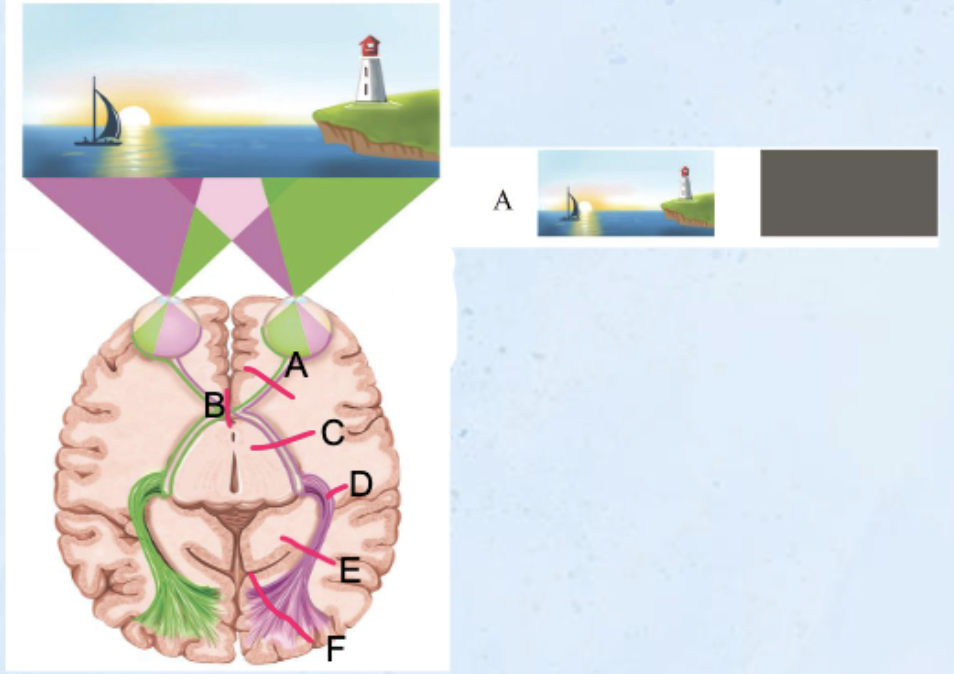
CN II Optic Nerve
UNILATERAL LOSS OF ALL VISION
monocular blindness
Optic Chiasm

Loss of vision in temporal visual
fields = tunnel vision
Bitemporal heteronymous hemianopsia
Optic Tract

Loss of vision in same visual half of each eye
Homonymous hemianopsia
Example: Right optic tract lesion
You lose:
Left visual field from left eye
Left visual field from right eye
Each optic tract carries one entire visual field from both eyes, not one eye.
Axons from contralateral visual field

Interruption of portion of geniculocalcarine fibers
Loss of vision in same visual quadrant of each eye (L/R)
Homonymous quadrantanopsia
these fibers carry quadrant-specific information from the contralateral visual field of both eyes, so a lesion removes the same visual quadrant bilaterally.
V1 one side damage

Blindness in opposite field of vision in each eye
○ Central vision can be spared
Homonymous hemianopsia with central sparing