Forensic Pathology master set
1/107
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
108 Terms
What are lacerations and their key characteristics
Lacerations: wounds caused by blunt force trauma, producing tearing of tissue.
Key features:
Often associated with abrasions and bruising; crushed wound margins.
Messy compared to an incision (not clean cuts).
Types include tears, splits, grind, stretch, and flap lacerations.
Irregular, ragged edges with bridging tissue strands.
Wound openings may appear linear, Y-shaped, or star-like.
Unilateral undermining may indicate the direction of force.
Foreign material may be embedded in the wound (e.g., glass fragments from a bottle).
Usually do not give a clear impression of the exact force object.
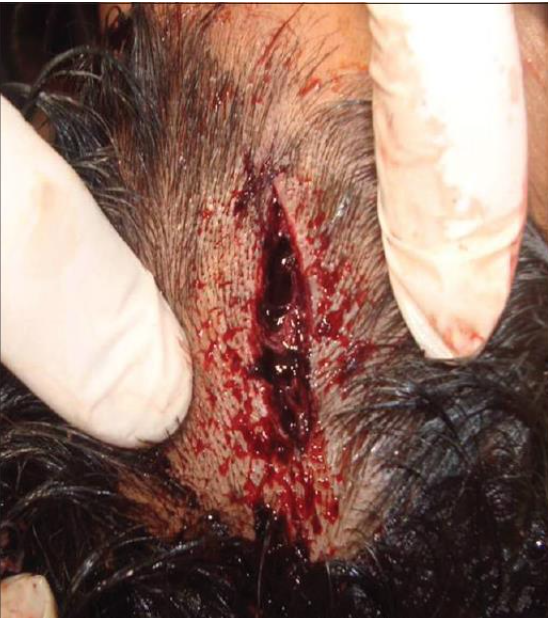
Why is it important to distinguish between lacerations and sharp force cuts in forensic pathology?
Misidentifying a wound can mislead an investigation and result in incorrect conclusions about the cause or weapon used.
Key differences to document before treatment:
Wound edges (clean vs irregular)
Residual skin bridging (present in lacerations, absent in incised wounds)
Bruising or abrasion around the wound
Surrounding hairs (often crushed in lacerations from blunt force)
Importance:
Accurate documentation helps determine how the wound was caused and whether a blunt or sharp object was involved.
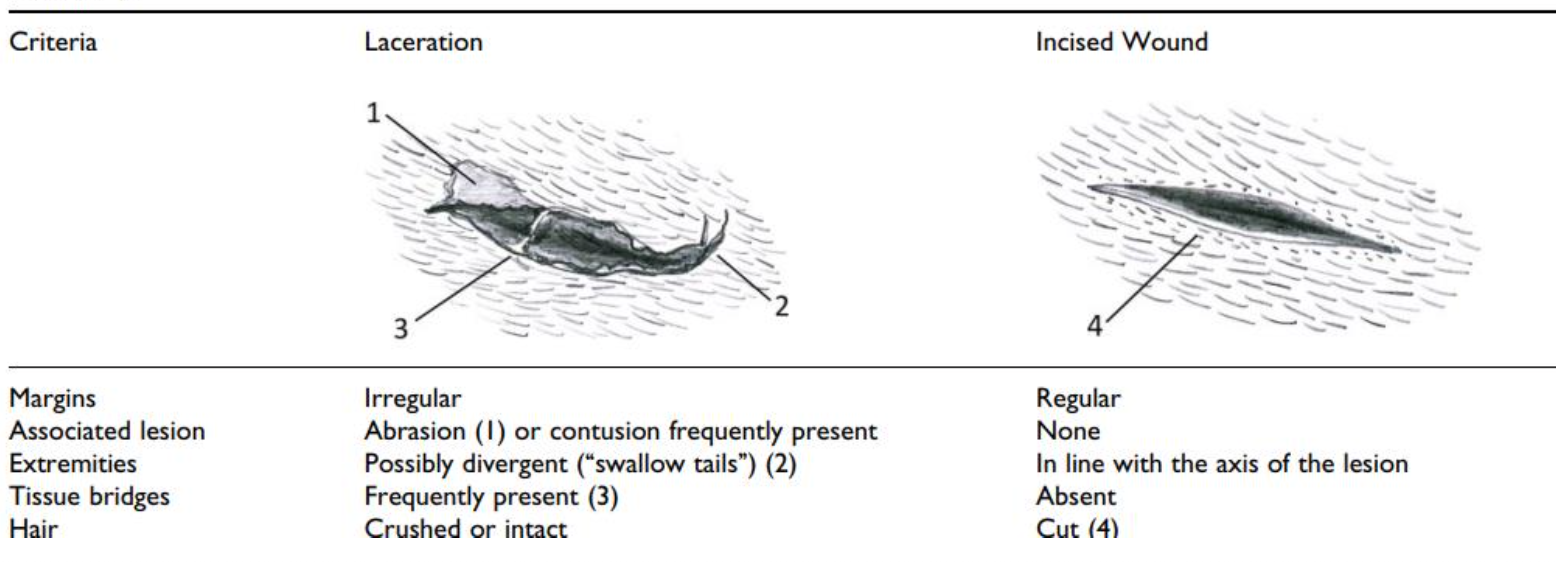
What is unilateral undermining in a wound?
Unilateral undermining is when tissue beneath the skin is separated on one side of a wound only, usually seen in lacerations caused by blunt force trauma.
Key point:
It helps indicate the direction of the force or blow.
The undermined side is typically opposite the direction of impact.
Case Study – Lacerations:
A 34-year-old was found dead with significant blood at the scene suggesting an arterial blood pattern. Autopsy revealed substantial head trauma causing arterial injury. CCTV showed he fell down the stairs, and toxicology was negative.
What was the manner of death?
Cause of death:
Head trauma causing arterial injury and severe bleeding
Manner of death:
Accidental
Key evidence:
Arterial blood pattern at the scene
Internal head trauma found during autopsy
CCTV confirming fall down stairs
Negative toxicology (not under influence)
Conclusion: Accidental death due to traumatic head injury after a fall.
What is strangulation in forensic pathology and what are its main types?
Strangulation:
Asphyxia caused by external pressure on the neck.
Main types:
Hanging – pressure from body weight via a ligature
Ligature strangulation – tightening object around neck (e.g., belt, cord, scarf)
Manual strangulation – pressure applied by hands or body parts
Key points:
Causes restricted blood flow and oxygen to the brain
Neck injury patterns help determine homicide, suicide, or accidental death
What are the key features of hanging in forensic pathology?
Hanging:
A form of strangulation where body weight applies pressure to the neck using a ligature.
Key features:
Most cases are suicidal self-suspension
Ligatures may include rope, belts, wires, scarves, or sheets
Suspension point usually on the side of the neck or above the chin
Complete or incomplete suspension of the body
Death usually occurs by asphyxia, sometimes neck fracture
Ligature furrow on the neck is the most common external sign
What is the difference between strangulation and hanging?
Strangulation
External pressure applied to the neck
Pressure from hands (manual) or tightening ligature
Usually homicide
Ligature mark typically horizontal and no suspension point
Hanging
Body weight applies pressure to the neck via a ligature
Usually self-suspension (suicide)
Ligature mark often angled upward toward suspension point
Body may be fully or partially suspended
What are incised wounds and their key characteristics?
Incised wounds:
Wounds caused when a sharp-edged instrument moved across the body surface.
Key features:
Caused by sharp objects (e.g., knife, glass)
Clean, well-defined edges
No bridging tissue present
Cut: incision through skin and underlying soft tissue
Slash: more forceful sweeping cut, often indicating intent to harm
Forensic point:
Shows sharp force injury, but usually does not identify the specific weapon used.
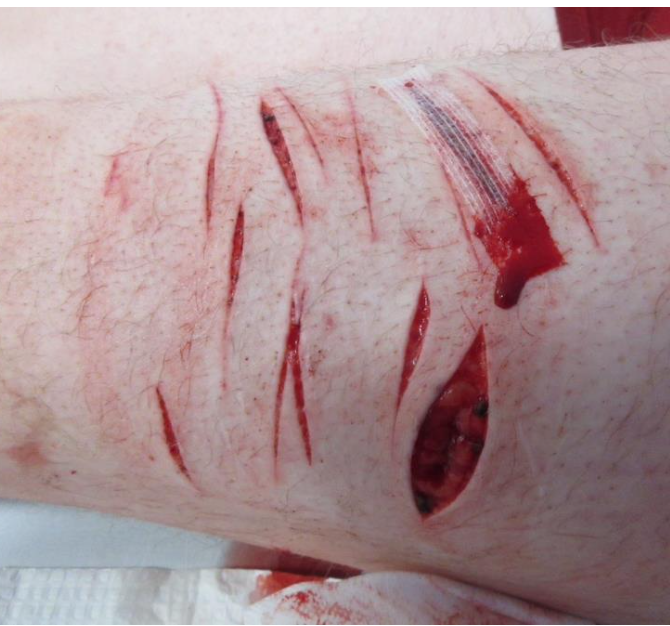
What are the key features of incised wound depth and bleeding in forensic analysis?
Depth characteristics:
Wound may be deeper at the point where the blade entered and shallower in the middle or tail.
Depth can indicate the direction of blade movement.
Skin effects:
Cleavage lines of the skin can cause the middle of the wound to gape.
Bleeding:
Incised wounds may bleed heavily, but are rarely fatal unless:
A major blood vessel is cut
The wound is very deep
There are multiple/extensive wounds
A large weapon is used
Forensic significance:
Wounds that cross irregular body surfaces can help confirm causation and intention.
What are the key features and forensic considerations of glass injuries?
Glass injuries: wounds caused by broken or intact glass, producing incised wounds or lacerations.
Common scenarios:
Burglary (broken window) → burglar often receives multiple cuts when climbing through shattered glass.
Broken glass used in assault → multiple deep incised wounds.
Intact glass breaking on impact (e.g., fall into window) → usually more superficial cuts.
Impact with intact glass object → may cause lacerations rather than clean cuts.
Forensic significance:
Important to determine when the glass broke (before, during, or after the injury).
Helps interpret intent (e.g., accident, burglary, or assault).
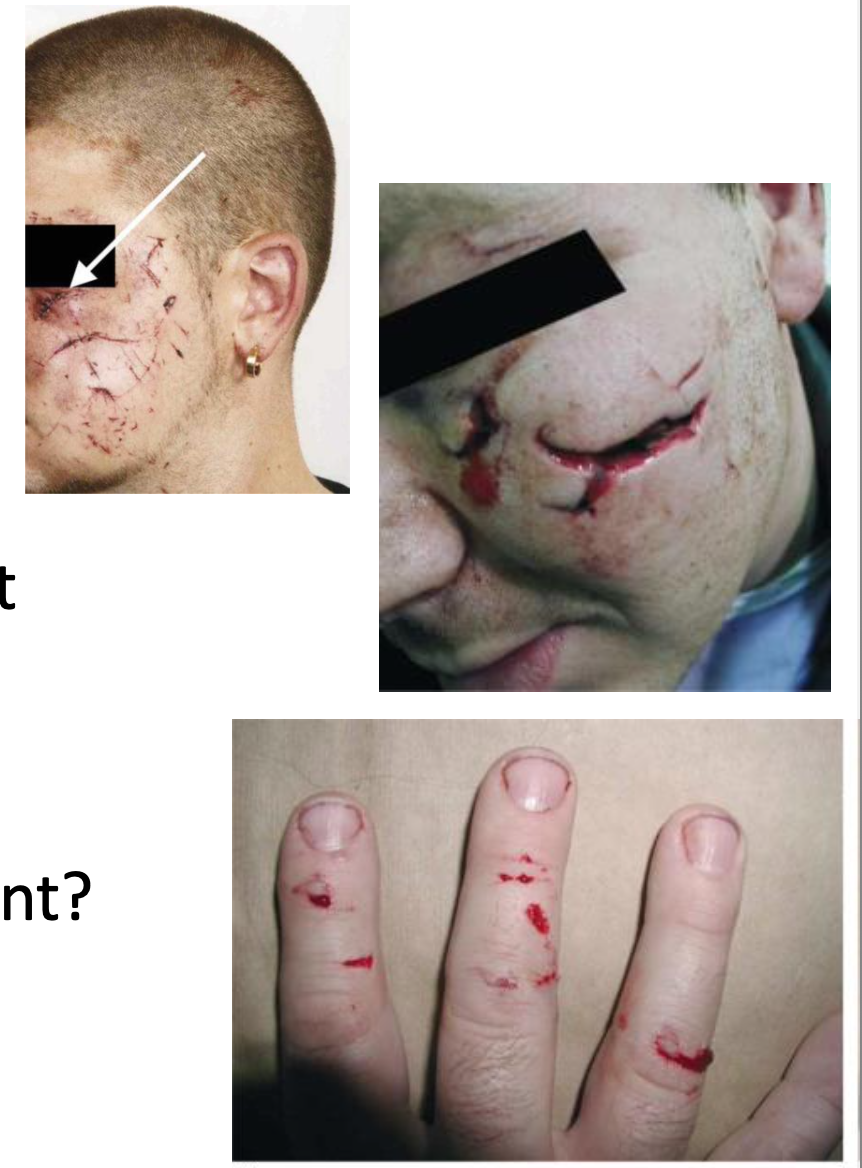
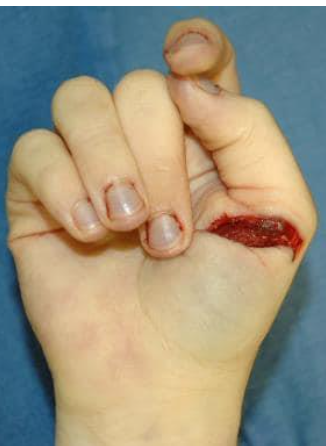
What are blade injuries and what are their key characteristics?
Blade injuries: wounds caused by sharp-edged instruments producing clean cuts.
Key features:
Penetrative force depends on blade sharpness, cutting edge, pointedness, and length.
Clean, well-defined cuts usually produced by blades.
Movement during infliction (e.g., victim defending themselves) may cause irregular wounds.
Bladed weapons are easily accessible (e.g., knives, razor blades, shivs – handmade weapons). - commonly used and seen
Weapon pattern may appear on the skin, e.g., serrated knife leaves patterned edges.
What are chop injuries and their key characteristics?
Chop injuries: wounds caused by heavy sharp-edged weapons, combining sharp force and blunt force trauma.
Common weapons:
Axes, hatchets, machetes, swords
Boat propellers or other heavy sharp objects
Key features:
Deep soft tissue transections with smooth edges
May show abrasion or bruising at wound margins due to blunt force
Often associated with underlying bone damage
Notch-like injuries in bone may be present
Forensic point:
Injury reflects both cutting action and heavy impact force.
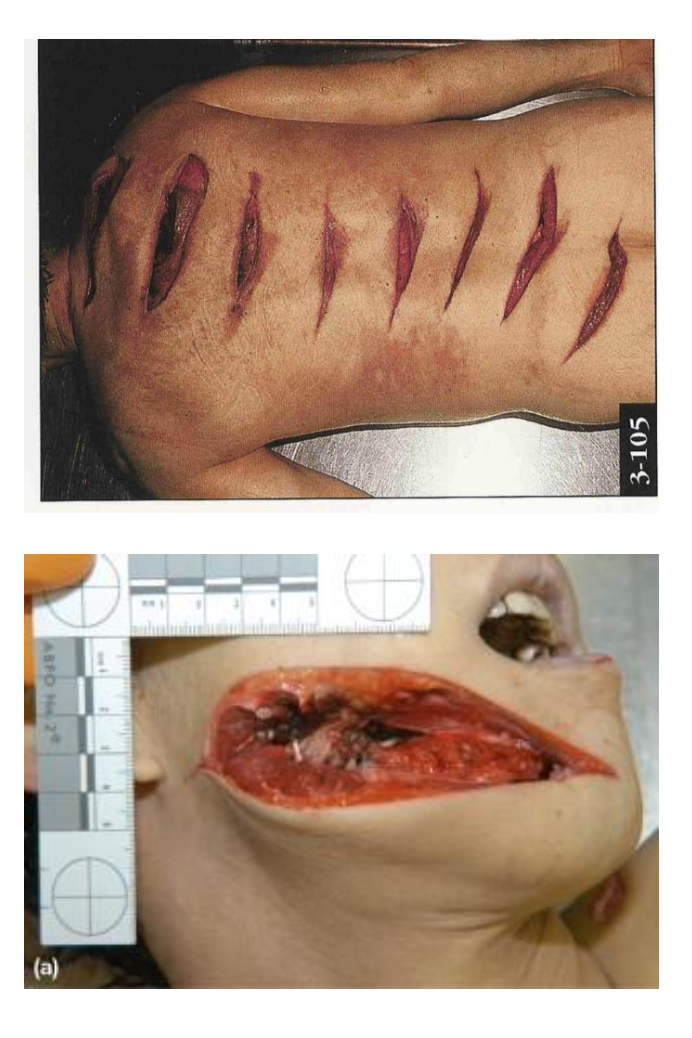
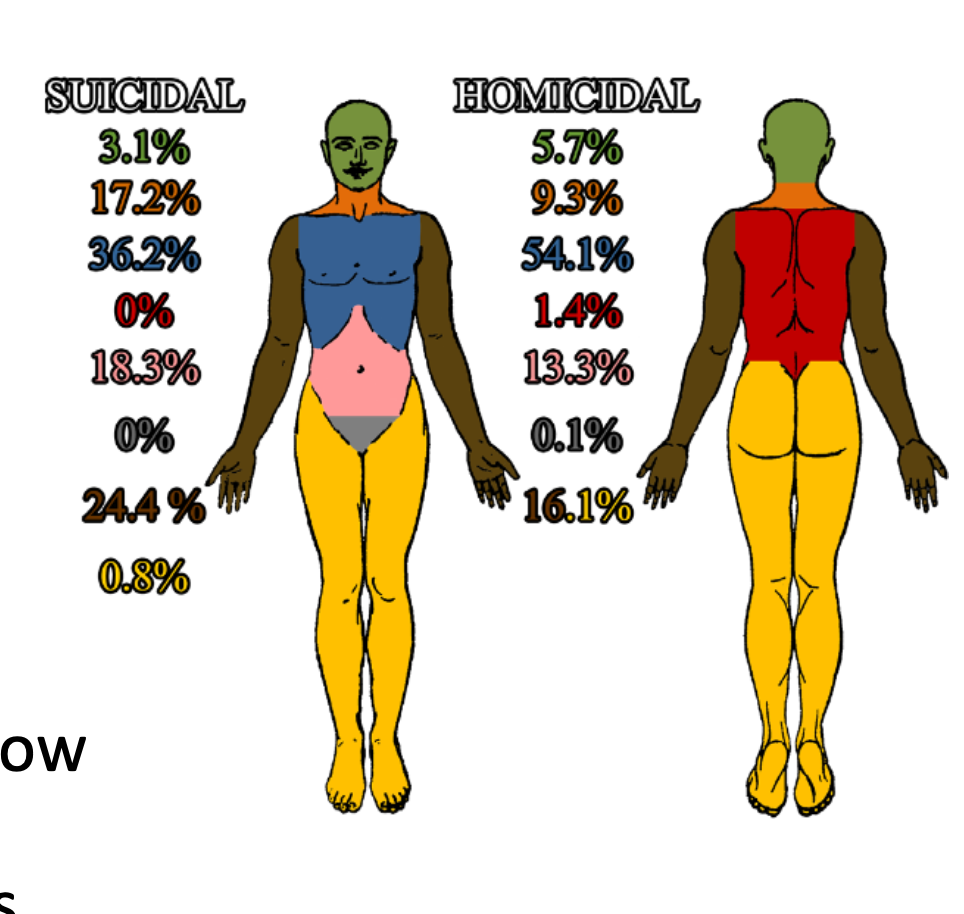
Why is the placement of incised wounds forensically significant?
The pattern and location of incised wounds can provide clues about the manner of death.
Suicide:
Wounds often located in areas suggesting a fatal outcome
Common sites: wrists, neck, knee, ankle joint, chest, arm
Homicide:
Wounds typically found in areas accessible to the offender
Common sites: face, neck, trunk, back
Forensic significance:
Injury placement helps guide lines of enquiry in investigations and support interpretation of suicide vs homicide.
Evidence supported by a review of 3000+ cases (De-Giorgio et al., 2015).
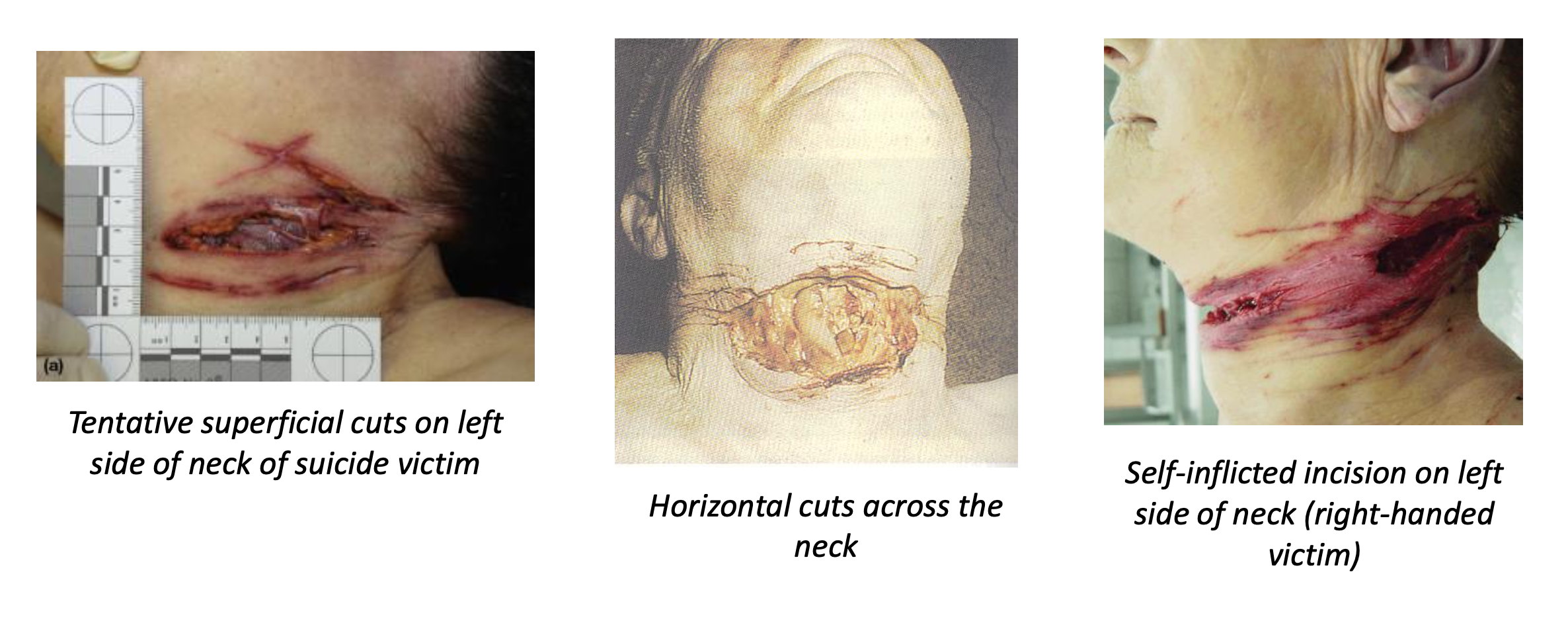
What are the key characteristics of suicidal neck incisions?
General:
Neck incisions are usually suicidal or homicidal, rarely accidental.
Typical features of suicidal cuts:
Often begin on the opposite side of the dominant hand
e.g., right-handed person → cut starts on left side of neck
Deeper at the origin and tails off as the cut progresses
May appear horizontal, linear, and clean
Other indicators:
Tentative/hesitation wounds (multiple shallow cuts nearby)
Deep incisions may sever hyoid bone and thyroid cartilage and leave marks on vertebrae
Possible causes of death:
Asphyxiation
Exsanguination (severe blood loss)
Air embolism
What are the typical characteristics of homicidal neck incisions?
General features:
Usually less organised or less planned in appearance
Wound characteristics:
Often deep with irregular edges
May sever the larynx and major blood vessels
Forensic indicators:
Depth and direction of the wound can indicate where the offender stood
Additional injuries on the body (e.g., defence wounds on hands or arms)
Bloodstain patterns help determine the victim’s position during the attack
Significance:
These features help differentiate homicidal injuries from suicidal cuts.
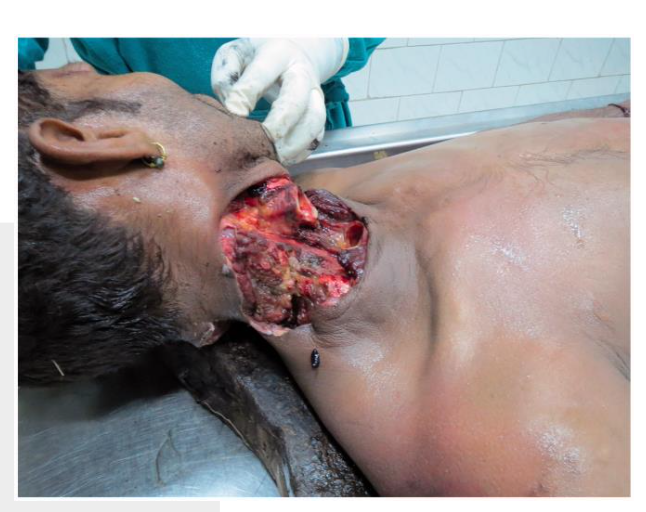
How do incised wounds differ from stab wounds?
Incised wounds (cuts):
Caused by a sharp blade moving across the skin
Longer on the surface than they are deep
Clean, well-defined edges
Stab wounds:
Caused by a pointed object thrust into the body
Deeper than they are wide on the skin surface
Penetrate deeper tissues and internal organs
Key difference:
Incised = longer than deep
Stab = deeper than wide
What are the typical forensic features of wrist incisions?
Self-inflicted wrist incisions:
Multiple, parallel cuts on the wrist or lower forearm
Usually on the opposite side of the dominant hand
Often occur with other self-inflicted cuts on the body
Typically superficial wounds
Homicide consideration:
Cuts on wrists or hands may also be defensive injuries if the victim tried to protect themselves.
Why are unusual incision sites forensically significant?
The location of incised wounds can suggest possible motives, behaviours, or circumstances.
Examples:
Mouth, nipples, eyes, genitals → may indicate sexual crime or self-inflicted injury linked to mental distress
Back or difficult-to-reach areas → suspicious, may suggest assault
Face → possible intent to disfigure
Face or trunk → may indicate torture, cultural rituals, or self-punishment
Forensic significance:
Unusual wound placement helps guide investigative lines of enquiry and interpretation of events.
What is the forensic significance of healed incisions?
Healed incisions (scars) may provide information about a person's past history or circumstances.
Possible interpretations:
Evidence of previous self-harm
Signs of past abuse or torture
Surgical scars that may help with identification
May suggest repeat victimisation
Forensic significance:
Healed wounds can provide context about the victim’s history, lifestyle, and possible prior violence which may support investigative enquiries.
Case Example – Incised Wounds:
A 32-year-old woman was pushed from a balcony and died from her injuries. She had multiple incised wounds to the face and neck, caused by a glass shard, which severed the internal jugular vein. Incisions were also found on the suspect’s hand.
What was the forensic interpretation?
Cause of death:
Exsanguination from severed internal jugular vein due to incised wounds
Weapon:
Glass shard
Key forensic evidence:
Multiple incisions on victim’s face and neck
Glass fragment identified as weapon
Incised wound on suspect’s hand linking them to the assault
Manner of death: Homicide.
Case Example – Incised Wounds:
A 51-year-old man was found dead in his car with a deep slanted incised neck injury. There was no weapon at the scene and no hesitation or defence wounds. What was the forensic interpretation?
Key findings:
Deep incised neck wound
Severed carotid artery
No hesitation wounds (unlikely suicide)
No defence injuries (victim unaware of the attack (came from behind?))
No weapon found at the scene
Forensic interpretation:
Wound delivered from behind, suggesting the offender was seated behind the victim in the car.
Manner of death: Homicide.
What are stab wounds and their key forensic characteristics?
Stab wounds: injuries caused when a pointed object is thrust into the body.
Key features:
Deeper than they are wide on the skin surface
Occur when the object overcomes the elasticity of the skin and penetrates internal tissues
Greater force usually produces more severe internal injury
Wound shape (morphology) may reflect features of the weapon (e.g., blade shape or tip)
Clothing damage and bloodstain patterns are also important in forensic evaluation.
Why is identifying stab wounds so important in the UK
Stab wounds are important to identify because sharp instruments account for a large proportion of homicides in the UK.
Key point:
Around 36–41% of homicides (2011–2021) were committed using sharp instruments such as knives.
Forensic significance:
Helps determine cause and manner of death
Assists in weapon identification and reconstruction of the attack
Important evidence in criminal investigations involving knife crime.
What factors influence the severity of stab wound injuries?
Stab wound severity depends on several factors affecting how the wound is created.
Key factors:
Properties of the weapon (e.g., knife type, sharpness)
Speed, direction, and force of the blow
Movement or reaction of the victim
Additional influences:
Weapon movement, impact, and removal can change wound appearance
Removing the weapon may increase bleeding as it no longer plugs the wound
Resistance of internal organs may require greater force to penetrate
Forensic significance:
Depth and severity may indicate intent to cause harm
Important for legal interpretation (e.g., accidental vs intentional injury)
Force required scale: weak → moderate → severe (intent)
What surface wound characteristics are examined in stab wounds?
Key aspects examined:
Number, location, relationship, and characteristics of the stab wounds
Important features:
Limited external bleeding may occur if the weapon remains in the wound (acts as a plug)
Wound shape and size may help indicate the type of implement (blade size, shape, tip)
Bruising or lacerations around the wound may suggest a blunt weapon or serrated knife
Forensic investigation:
Investigators conduct a direct search for the weapon at the scene or from the suspect.
Why can stab wound surface patterns be irregular and difficult to interpret?
Stab wounds can appear irregular due to movement between the assailant and victim during the attack.
Common features:
L-, Y-, or V-shaped wounds or central notches from movement
Blade rocking may increase penetration depth (may suggest intent)
Stabs through skin folds or creases can create incised stab wounds
Single thrust may produce multiple wounds
Other factors:
Elastic fibre contraction can change wound shape, making the same weapon appear different
Depth of injury may exceed blade length, sometimes shown by hilt marks or blood staining.
What is the forensic importance of wound tracks in stab wound analysis?
Wound tracks describe the internal path of a penetrating injury through the body.
Key information obtained:
Direction, depth, and force of the wound
Internal injuries to organs and tissues
Mapping surface wounds to internal damage
Additional indicators:
Score marks on bone if the weapon impacts bone (useful even with skeletal remains)
Possible remnants or fragments of the weapon
Techniques used:
Invasive methods (autopsy dissection)
Non-invasive methods (e.g., imaging techniques).
What are the typical characteristics of homicidal stab wounds?
General features:
May involve single or multiple stab wounds
Bone injuries may occur with greater penetration force
Defence wounds or assailant injuries may be present
Blood patterns and transfer evidence may help reconstruct the attack
Single stab wound:
Often precise
May be “stab and run”
Victim may be immediately incapacitated
Multiple stab wounds:
First blow rarely incapacitates the victim
May indicate a frenzied or prolonged attack
Sometimes associated with mutilation.
What are the typical characteristics of suicidal stab wounds?
Common features:
Often a single deep stab wound (but not always)
Victim may remove clothing or bare the skin before stabbing
Frequently located in the precordium (chest over the heart) or abdomen
Other indicators:
Stab wounds to the neck are more difficult to interpret
Weapon may be partially withdrawn and reinserted
Hesitation marks (small superficial incisions) may be present
Forensic significance:
These features help distinguish suicide from homicide, but interpretation must consider all evidence from the scene and autopsy.
What are the typical characteristics of accidental stab wounds?
Common features:
Often a single stab wound with less penetration
Weapon usually found nearby at the scene
Can be difficult to distinguish from assault without witnesses
Common environments:
Kitchens
Building sites
Abattoirs
Forensic consideration:
Accidental injury is sometimes claimed as a defence in homicide cases, so evidence must be carefully evaluated.
Example:
Damilola Taylor case (2000) – initially argued the victim fell onto a broken bottle accidentally, but later new forensic evidence led to convictions years later.
Case Example – Stab Wounds:
A 40-year-old man was found dead at his front door with a screwdriver under his body and 39 groups of injuries (54 blows). Although the weapon was present, what was the forensic conclusion?
Key findings:
Phillips-head screwdriver found under the body
39 injury groups (54 separate blows)
Injuries to back, head, wrist, skull, and chest
Cruciate (cross-shaped) wounds consistent with a screwdriver tip
Forensic interpretation:
The large number of injuries and distribution across the body are inconsistent with self-infliction
Manner of death: Homicide.
Case Example – Stab Wound (Ice Pick):
A 16-year-old was attacked by a classmate with an ice pick, creating small circular stab wounds that penetrated the lung and left ventricle. What was the cause of death and forensic significance?
Key findings:
Small circular stab wounds (~0.4 cm) from an ice pick
Wound track penetrated the lung and left ventricle
Large amount of blood in the chest cavity
Cause of death:
Cardiogenic shock due to severe heart injury
Forensic significance:
Very small external wounds can cause severe internal damage
Demonstrates how stab wound tracks are critical for understanding injury severity.
What are the key forensic characteristics and indicators of gunshot wounds (GSWs)?
General features:
Complex, violent, traumatic injuries
Usually associated with suicide or homicide
In the UK, firearms account for ~4–8% of homicides
Mechanism:
Injury occurs when projectiles are fired from a firearm by gunpowder and penetrate the body.
Entry vs exit wounds:
Exit wounds usually larger and everted
Entry wounds often smaller
Range indicators:
Contact wounds → seared or blackened edges
Soot in wound track and powder tattooing indicate close-range shooting
Wound diameter increases with distance
Shotgun wounds and shooting distance:
< 20 cm (very close range):
Pellets remain tightly grouped, producing one large entry wound.> 20 cm (greater distance):
Pellets spread apart, producing multiple separate pellet wounds.
Other forensic indicators:
Bullet trajectory through body tissues
High-velocity bullets may pass completely through the body
Bullet angle may produce D- or P-shaped wounds
Expanding bullets cause severe internal damage
How do investigators distinguish between suicide and homicide in gunshot cases?
Determination relies on scene evidence and autopsy findings.
Suicide indicators:
Usually a single gunshot wound
Close-contact shot
Located at accessible areas (e.g., head, chest)
Weapon typically found near the body
Homicide indicators:
Often multiple gunshot wounds
May be shot from a distance
Wounds can occur anywhere on the body
Additional forensic evidence:
Blood spatter on the firearm (close-range shooting)
Gunshot residue (GSR) on hands or clothing of the shooter
Case Example – Gunshot Wound:
A 40-year-old woman was found dead in bed with a 9mm semi-automatic handgun in her right hand. Autopsy revealed two entry wounds on the right scalp and two exit wounds on the left forehead affecting deep central brain structures. What was the forensic interpretation?
Key findings:
Two entry wounds on the right side of the scalp
Two exit wounds on the left forehead
Bullet paths through deep central brain structures
Blood spatter evidence placed the husband near the shooting
Forensic interpretation:
Multiple gunshot wounds inconsistent with self-inflicted suicide
Evidence suggested the scene had been staged
Manner of death: Homicide – husband later convicted of murder.
What factors are considered in forensic interpretation when determining manner of death?
Wounds alone are not enough to determine the manner of death. Investigators must consider additional evidence.
Key considerations:
Presence of a suicide note
Medical or psychiatric history and medications
Whether a weapon is present nearby
Signs of a struggle
Injury location and accessibility (could the victim reach the area?)
Clothing and scene context
Internet search history indicating intent
Witness accounts
Criminal history of victim or suspect
Conclusion:
Determining manner of death requires combining:
Autopsy findings + Scene investigation + Witness information + Victim history + Forensic evidence.
What is the forensic significance of suicide notes?
Key points:
Most suicide cases do NOT leave a note, so the absence of one is not suspicious.
If a note is found, it must be carefully evaluated.
Considerations:
Could it have been written under pressure or coercion?
Is the handwriting authentic?
Does other evidence (scene, history, digital activity) support the note’s claims?
Forensic principle:
A suicide note cannot be taken at face value and must be assessed alongside all other forensic and investigative evidence.
What is forensic pathology?
Forensic pathology is the investigation of sudden, unexpected, or violent deaths.
Key aspects:
Applies forensic science and medical pathology techniques
Forensic pathologists are medically trained doctors
They must understand multiple scientific fields, including forensic science
Work with medicolegal authorities (e.g., coroner)
Main role:
Conduct autopsies and post-mortem examinations
Determine cause, manner, and time of death
What are the cause, manner, and time of death in forensic investigation?
Cause of death:
The process, injury, or disease that directly leads to death.
Examples: head injury, drowning.
Often related to trauma, injury, disease contribution, or violence.
Manner of death:
The circumstances surrounding the cause of death.
Categories include:
Accident (e.g., fall, car crash)
Homicide (murder by another person/object)
Suicide
Natural causes
Undetermined / unexplained
Time of death:
An estimate of when death or injury occurred.
Methods include:
Body temperature (algor mortis)
Stomach contents
Corneal cloudiness
Vitreous humour analysis
Example: TSD (time since death) = 12–18 hours.
What are the three main stages of a forensic death investigation?
1. Initial investigation (scene):
Examination of the death scene
May not always occur (e.g., if the person dies in hospital)
2. Body examination (mortuary):
External autopsy – examination of the outside of the body
Internal autopsy – examination of internal organs and structures
Ancillary tests – specialised tests after autopsy (e.g., toxicology)
3. Follow-up investigations:
Interpretation of findings
Reporting results and presenting evidence in court
What is the role of a forensic pathologist during scene examination?
At the scene:
Pathologists may be on call 24/7 and attend the scene if required
Perform in-situ examination of the body
Key observations:
Post-mortem changes
Body position and possible manipulation
Ambient and deep body temperature recordings
Evidence preservation:
Ensure forensic evidence is preserved before the body is moved
Important areas (e.g., hands for defensive evidence) may be protected for later analysis
Body handling:
Supervise packaging and removal of the body for transport to the mortuary
What is examined during the external examination in an autopsy?
Purpose:
To establish identity and document physical features of the deceased.
Key aspects recorded:
Individual traits: height, weight, sex/gender, ethnicity, hair and eye colour, scars, tattoos
Forensic evidence: injuries, trace evidence, post-mortem changes
Additional features: clothing, medical treatments or devices, identifying marks
Injury documentation:
Injuries are described by shape, size, direction, placement, edges, angles, and estimated age.
What occurs during the internal examination of an autopsy?
Non-invasive examination:
Virtual autopsy techniques such as post-mortem CT, MRI, 3D scanning, or LiDAR
If further investigation is needed:
Invasive autopsy involving surgical removal and dissection of organs
Can be complete (full body) or limited (specific areas)
Other key aspects:
Samples or materials related to cause of death may be retained
Procedures must follow legal regulations, including the Human Tissue Act (HTA)
What are ancillary tests in an autopsy and why are they used?
Ancillary tests are additional laboratory or specialist tests used to help determine the cause of death when the autopsy alone is not sufficient.
Common tests include:
Toxicology (drugs, alcohol, poisons)
Histology (microscopic tissue examination)
X-rays or specialised dissections
Chemical or microbiological testing (e.g., bacterial or fungal infections)
Forensic evidence analysis:
Recovery of bullets from gunshot wounds for ballistic analysis
Finger mark bruising around the neck may allow fingerprint collection
Bodily fluids collected in suspected sexual assault cases
Purpose:
Provide additional scientific evidence to support conclusions about the cause and circumstances of death.
What occurs during follow-up investigations in forensic death cases?
Follow-up investigations occur after the autopsy to gather additional information and finalise conclusions.
Key activities:
Additional evidence review, which may take days or weeks
Collaboration with police and forensic investigators
Review of medical records and history
Await results from ancillary tests (e.g., toxicology, histology)
Attendance at secondary post-mortems (often requested by the defence)
Final steps:
Preparation of formal reports
Providing witness statements
Giving testimony in court
What principles are important in forensic interpretation of injuries and evidence?
Key principles:
Interpretation varies in precision and complexity depending on the evidence.
Specificity of injuries: some injuries give clear clues (e.g., footwear marks from stamping), while others are non-specific (e.g., a black eye).
Injuries must be interpreted collectively, not individually (e.g., patterns of defence injuries).
Appropriate language is used, such as “consistent with” or “indicative of”, because conclusions cannot be 100% certain.
All relevant information must be considered, and none should be excluded.
Additional expertise:
Specialists may assist with ancillary test interpretation (e.g., toxicologists, microbiologists for blood alcohol levels or infections).
What is the process for forensic death investigation in the UK?
Investigations are conducted by registered Home Office forensic pathologists (≈ 39 in the UK).
All procedures must comply with the Human Tissue Act (2004).
The Senior Investigating Officer (SIO) reports the case to the coroner’s office.
The coroner appoints a forensic pathologist to conduct the autopsy.
The SIO or Crime Scene Manager (CSM) may attend the autopsy.
The pathologist prepares a written report and submits it to the coroner.
In the UK forensic investigation process, who decides to consult a forensic pathologist and why can this be problematic?
Decision-maker:
The Senior Investigating Officer (SIO) usually decides whether to involve a forensic pathologist.
Issue identified:
A Home Office review found cases where SIOs failed to request a forensic pathologist.
Example problem:
In 10 murder cases, pathologists were not called because the victims were elderly, and deaths were assumed to be natural.
Forensic concern:
These assumptions and bias led to missed investigations and inaccurate conclusions.
Key point:
Deaths may appear natural but still require forensic assessment if circumstances are suspicious.
How can bias affect decision making in forensic pathology and death investigations?
Bias in investigations:
Bias is widely reported in policing, law enforcement, and forensic analyses.
Examples include racial bias: disproportionate stop-and-search, and unequal sentencing outcomes.
Potential bias in forensic pathology:
Forensic pathologists must remain objective, but bias can still affect interpretation of evidence.
Example case:
A premature baby died two days after leaving hospital.
The pathologist failed to properly review medical records.
The mother was wrongly charged with murder (blunt force trauma and strangulation).
Key principle:
Thorough investigation and review of all evidence is essential to avoid bias and wrongful conclusions.
What is an example of racial contextual bias in forensic pathology?
Study example – Nevada, USA (child deaths):
Research found that contextual information influenced forensic pathologists’ conclusions.
Key findings:
Higher rates of homicide rulings were recorded for Black children compared to White children.
Bias appeared linked to who was caring for the child:
Black child with mother’s boyfriend as caretaker → more likely ruled homicide
White child with grandparent as caretaker → less likely ruled homicide
Forensic significance:
Demonstrates how contextual and racial bias can influence death classification.
Highlights the need for objective interpretation based on evidence rather than assumptions.
What are the possible outcomes of a forensic death investigation?
Key outcomes:
Death registration and funeral arrangements
Identification of cases requiring criminal investigation (e.g., homicide)
Recommendations to prevent future deaths (public safety measures)
Civil actions, such as wrongful death claims
Case Example – Forensic Interpretation:
A 75-year-old woman was robbed and assaulted, suffering craniofacial and electrocution injuries. She later developed chest pain in hospital and died from cardiac arrest. The autopsy identified cardiomyopathy (weakened heart). Why was the death ruled homicide?
Key findings:
Victim had underlying cardiomyopathy
Stress and trauma from the assault triggered cardiac arrest
Death occurred after the attack, while in hospital
Forensic interpretation:
Although the underlying heart disease contributed to death, the assault initiated the fatal event.
Manner of death: Homicide
Legal significance:
Offenders who intended robbery only were still convicted of murder, because their actions caused the chain of events leading to death.
Case Example – Awaab Ishak:
What was the cause of death and forensic outcome in the Awaab Ishak case?
Case details:
Awaab Ishak lived in rented housing with severe black mould.
Complaints about the mould were repeatedly reported but not addressed.
He presented to hospital with flu-like symptoms and breathing difficulties.
Cause of death:
Acute airway oedema with severe granulomatous tracheobronchitis
Caused by environmental mould exposure
Outcome and significance:
The case highlighted failures in housing safety.
Led to legal changes requiring landlords to address mould hazards promptly (“Awaab’s Law”).
What were the main causes of death in England & Wales (2022) by sex?
Male deaths:
Accidental: 3.5%
Suicide: 1.4%
Homicide / probable homicide: 0.2%
Natural causes: 281,052 deaths
Female deaths:
Accidental: 2.6%
Suicide: 0.5%
Homicide / probable homicide: 0.1%
Natural causes: 277,188 deaths
Key point:
The vast majority of deaths in England & Wales are due to natural causes, with accidents, suicide, and homicide representing a small proportion.
What are the key statistics and patterns of homicide in England & Wales?
General statistics:
696 homicide victims → 11.7 per million population
Mass events can affect yearly trends
Demographics:
72% of victims and 93% of suspects are male
Highest victim group: ages 16–24
71% of victims are White, but higher homicide incidence among Black ethnic groups (≈ 39.7 vs 8.9 per million)
Domestic homicide:
134 domestic homicides
Victims typically female
>50% involve a current or former partner
Offender relationships:
Strangers more often suspects in male homicides (15% vs 3% for female victims)
54 child victims, with parent/step-parent suspected in 26%
Circumstances:
53% involve arguments, loss of temper, or revenge
Sharp force trauma in 41% of homicides
Strangulation: 18% female victims vs 5% male
Location & substances:
Most homicides occur in or around the home
Male homicides more often occur away from home
33% of victims and 29% of suspects were under the influence of drugs or alcohol
What are the key suicide statistics and patterns in England & Wales?
General statistics:
5,642 suicides → 10.7 per 100,000 population
74% of victims are male
Age patterns:
Highest rates: ages 50–54
Lowest rates: ages 10–24
Trends change as prevention efforts target different groups
Other patterns:
Geographical variation (e.g., differences between North East and London)
Registration delays can occur (≈ 195 days after death)
Methods of suicide:
Hanging / strangulation / suffocation: 59.7% (most common)
Poisoning: more common in women
Other methods (drowning, falls, jumps, sharp objects): <4%
Forensic note:
Distinguishing suicidal hanging from homicidal strangulation can sometimes be difficult.
What is a wound in forensic pathology and what are the main types?
Definition:
A wound is damage to any part of the body caused by mechanical force.
Cause:
Can result from kinetic or non-kinetic energy
Main types of wounds:
Blunt force injuries
Abrasions
Lacerations
Bruises
Caused by impact with a hard surface or object
Sharp force injuries
Incised wounds (cuts)
Stab wounds
Gunshot wounds
Caused by projectiles fired from a firearm
Why is wound examination an important aspect of forensic pathology
Wound examination helps investigators reconstruct events surrounding injury and death.
Key questions addressed:
How was the wound caused?
When was it inflicted?
Before death (possible repeated violence)
At the time of death
After death
What weapon or object caused the injury?
e.g., knife, screwdriver, pencil
Did the wound contribute to or cause death?
Was the wound self-inflicted or caused by another person?
Could the wound have been altered by decomposition, body handling, or mortuary storage?
What methods are used to examine wounds in forensic pathology?
Basic examination:
All wounds are carefully examined and documented
Documentation techniques:
Digital photographs
Body mapping to record the location of wounds
Laboratory and imaging methods:
Microscopy – assess features such as healing stage
Histology – identify cellular changes (e.g., white blood cells indicating healing)
Radiology (CT, MRI) – examine internal injury and damage
Specialised methods:
Endoscopic examination – internal visualisation (e.g., throat or genital areas in assault investigations)
3D reconstruction technologies to help analyse and present wound patterns
How is the age of a wound estimated in forensic pathology?
Purpose:
To determine whether the injury occurred before death, at the time of death, or after death, and how long the victim survived after the injury.
Key indicator – Vital reactions:
Body responses that occur only if the person was alive when the injury happened, such as:
Haemorrhage (bleeding)
Inflammatory cell infiltration
Granulation tissue formation
Blood clotting visible under microscopy
Methods used:
Morphological analysis
Cytological examination
Molecular techniques
Common tissues examined:
Skin
Skeletal muscle
Brain tissue
How are vital reactions used to identify wounds inflicted before death (antemortem)?
Vital reactions are biological responses that occur only if the person was alive when the injury happened.
Examples and how they are detected:
Haemorrhage (bleeding): seen during autopsy or microscopy as blood leaking into surrounding tissues
Inflammatory cell infiltration: detected with histology, showing white blood cells in injured tissue
Granulation tissue formation: visible under microscopy, showing new connective tissue and blood vessels (healing)
Blood clotting: seen under microscopy as fibrin and platelet clots
Key principle:
Presence of vital reactions indicates the injury occurred before death.
What features are examined during the macroscopic examination of wounds?
Macroscopic examination involves visual inspection of wounds during autopsy.
Key features observed:
Haemorrhage and blood clotting
Signs of active bleeding and clot formation
Tissue reaction
Inflammation, swelling, redness
Wound edges
May appear everted, irregular, or swollen
Forensic significance:
These features can help determine whether the injury occurred while the person was alive and provide clues about how the wound was caused.
What features are examined during the microscopic (histological) examination of wounds?
Histological examination involves studying tissue samples under a microscope to identify signs of injury and healing.
Key findings:
Leukocyte infiltration
White blood cells (WBCs) present at the wound margins
Fibrin deposits and tissue repair
Fibrin deposition (blood clot formation)
Fibroblast activity
Granulation tissue formation
Forensic significance:
These findings indicate the wound occurred while the person was alive and healing had begun.
What biochemical markers are used in forensic wound analysis?
Biochemical markers help identify biological responses to injury and indicate if a wound occurred before death.
Key markers:
Enzymatic activity
Enzymes linked to inflammatory cells (e.g., cathepsins)
Cytokines
Their presence indicates an immune or inflammatory response
D-dimer testing
Elevated D-dimer levels indicate fibrinolysis (breakdown of blood clots)
Forensic significance:
These markers help confirm vital reactions and wound healing processes.
How are spectroscopy and molecular analysis used in forensic wound examination?
These methods analyse molecular changes in tissues to help determine wound vitality and healing processes.
Key indicators:
RNA degradation
Presence of specific RNA molecules can indicate vitality (injury occurred before death)
Molecular markers of inflammation and coagulation
Detection of proteins and cytokines involved in immune response and clotting
Common laboratory techniques:
ELISA – measures proteins such as cytokines
Western blot – detects specific proteins
RT-PCR – identifies and measures RNA molecules
What are bruises and how do they form?
Bruises (contusions):
Injuries caused by blunt, compressive, or squeezing force, leading to discolouration of the skin.
How they form:
Blood vessels are damaged
Blood leaks into surrounding tissues
Where they occur:
Beneath the skin
Within muscles
Inside internal organs
Key points:
Discolouration may vary and may or may not be visible
Bruises are commonly seen in victims of violence
What are petechial haemorrhages and why are they important in forensic pathology?
Petechial haemorrhages:
Small pinpoint spots of bleeding caused by blood leaking from tiny capillaries.
Cause:
Increased intracapillary pressure
Key characteristics:
Appear as tiny red or purple dots
Can occur during straining or resuscitation
Forensic significance:
Often associated with manual strangulation or asphyxia
Their presence prompts examination of neck structures for signs of strangulation
What is the difference between intradermal and subcutaneous bruises?
Intradermal bruises:
Superficial bleeding within the dermis (upper skin layer)
May produce patterned injuries
e.g., tyre marks, shoe marks, whip marks
Subcutaneous bruises:
Occur deeper beneath the skin
Often appear darker as blood spreads toward the surface
Typically have a blurred or indistinct outline on the skin surface
Forensic significance:
The depth and pattern of bruising can help identify the type of force or object involved.
What are tramline bruises and what causes them?
Tramline bruises:
A pair of parallel bruises with pale skin in between, caused by impact with a cylindrical object.
How they form:
The object compresses the skin in the centre, squeezing blood away (central pallor)
Blood vessels rupture at the edges, creating two parallel bruises
Often leaves a distinctive patterned injury
Common causes:
Strikes from cylindrical objects (e.g., rods, sticks, batons)
Forensic significance:
Pattern may help compare the bruise with the suspected weapon
Seen in cases of assault or child abuse
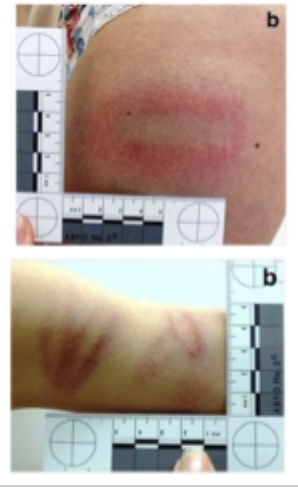
What are finger pad bruises and what do they indicate in forensic investigations?
Finger pad bruises:
Small round or oval (discoid) bruises, often found in clusters.
Key features:
Usually caused by pressure from fingertips
May be accompanied by fingernail scratches
DNA may sometimes be recovered from the area
Forensic significance (location clues):
Neck → manual strangulation
Shoulders/arms → forceful restraint
Wrists/ankles → dragging
Chest → resuscitation attempts
Inner thighs → possible sexual assault
Important note:
Clustered finger pad bruising is often associated with physical abuse or forceful contact.
What are defensive bruises and where are they commonly found?
Defensive bruises:
Bruising that occurs when a victim attempts to protect themselves during an attack.
Common locations:
Ulnar surface of the forearms (outer forearm) from blocking blows
Extremities (arms and hands)
Mouth or lips – when a hand is forcibly placed over the mouth
Shoulders – when the victim is pushed or forced against a wall
Forensic significance:
Indicates the victim attempted to ward off the attack and protect vital organs.
What are deep bruises and why are they important in forensic pathology?
Deep bruises:
Bruising that occurs within internal tissues or organs, often due to blunt force trauma.
Key points:
Surface bruises usually indicate circumstances of assault or injury but are rarely fatal
Deep internal bruising can be life-threatening or fatal
May not be visible on the skin, so they are often identified during autopsy
Associated causes:
Blunt force trauma
Falls
Assaults
Accidents
Possible consequences:
Splenic rupture
Cardiac arrest
Respiratory failure
Brain swelling
Forensic significance:
Internal bruising helps identify hidden trauma and potential cause of death.
What factors influence the appearance and distribution of bruises?
Factors affecting bruise appearance:
Force and depth of injury – stronger force often produces larger bruises
Highly vascular areas bruise more easily
Subcutaneous fat or loose skin increases bruising
Infants and elderly often develop larger bruises
Co-morbidities, medications, or alcohol can make bruising more likely
Bruise movement:
Bruising may appear away from the original injury site as blood moves through tissues and collects in areas of least resistance or gravity
Examples:
Broken jaw
Forehead or scalp injury
Skull fracture
Tooth removal
Humerus fracture
What are the key considerations in bruise aging in forensic pathology?
Vitality:
Bruises usually indicate injury occurred during life
Post-mortem bruising can occur from passive blood ooze, but typically lacks inflammation
Interpretation of multiple bruises:
Bruises at different healing stages may indicate:
Repeated assault or abuse
Disease (e.g., leukaemia)
Lifestyle factors (e.g., contact sports)
Recent bruises:
Provide the most useful information about cause of injury
Limitations:
Bruise appearance varies due to size, depth, body location, health, age, and sex
Visual aging is subjective and not standardised
Evidence example:
Maguire et al. (2005): fewer than 40% of bruises in children were correctly dated within 24 hours
Why do bruise colours change over time?
Bruise colour changes occur due to the chemical breakdown (degradation) of haemoglobin from leaked blood in tissues.
Stages of colour change:
Initial injury – fresh blood in tissue
Haemoglobin – red/blue-purple colour
Biliverdin – green colour
Bilirubin – yellow colour
Hemosiderin – brown colour
Resolution – bruise gradually fades
Key idea:
The colour changes reflect the body breaking down blood pigments as the bruise heals.
How are bruises detected and what factors affect their visibility?
Detection:
Bruises are usually identified by visible skin discolouration.
Importance:
Accurate detection is crucial for clinical assessment and legal investigations.
Factors affecting visibility:
Lighting and observation conditions
Skin colour
Depth of the bruise
Key point:
Higher melanin levels in darker skin can reduce the visibility of subcutaneous bruising, making injuries harder to detect.
How can alternative light sources (ALS) improve bruise detection?
Alternative light sources (ALS) help reveal bruises that may not be visible under normal white light.
How it works:
Uses specific wavelengths of light (≈350–535 nm).
Haemoglobin and its breakdown products absorb light, making bruising more visible.
Key findings from studies:
415 nm and 450 nm wavelengths with a yellow filter are most effective.
ALS detected bruising in ~98% of strangulation cases.
Detection decreases as bruises age (≈12% reduction every 24 hours).
Bruises were more detectable in females and fatty tissues.
Important result:
ALS is ~5× more effective than white light for detecting bruises on darker skin types.
Case Example – Bruising and Elder Abuse:
A 78-year-old woman was found dead at home with multiple bruises on her face at different stages of healing. What was the forensic interpretation?
Key findings:
Multiple facial bruises
Bruises at different stages of healing
Evidence of neglect and repeated injury
Cause of death:
Heart disease
Forensic interpretation:
Pattern of bruising indicated ongoing abuse and neglect
Conclusion: The woman had been abused by her son, and the injuries helped identify elder abuse contributing to the circumstances of death.
Case Example – Tramline Bruising in a Child:
A 5-year-old boy was found dead in bed with tramline bruises on his leg at different stages of healing and additional skin markings from traditional therapy. What was the forensic interpretation?
Key findings:
Tramline bruises on the leg
Bruises at different healing stages
Marks consistent with traditional therapeutic practices (e.g., cultural massage/therapy techniques)
Forensic significance:
Patterned injuries initially raised concern for child abuse
Investigation showed some marks were associated with traditional therapy
Key lesson:
Forensic pathologists must consider cultural practices and full contextual evidence before concluding abuse or assault.
What are abrasions and what do they indicate in forensic pathology?
Abrasions:
Superficial injuries caused by tangential dragging or friction, resulting in removal or damage of the epidermis (outer skin layer).
How they occur:
Pressure combined with movement across the skin surface
Causes scraping and surface damage
Forensic significance:
May help indicate the direction of force due to the pattern of skin damage
Often associated with blunt force trauma, friction, or dragging
What are scratch abrasions and what is their forensic significance?
Scratch abrasions:
Superficial injuries caused by fingernails scraping or dragging across the skin.
How they occur:
Static pressure or skidding of nails on the skin surface
Forensic significance:
Often seen as defence or resistance injuries during an attack
Can occur on both the victim and the suspect
Common locations:
Inner thighs or genital area → possible sexual assault
Face or neck → possible strangulation
Evidence potential:
May contain trace DNA from the attacker under the victim’s nails
What are grazed abrasions and what is their forensic significance?
Grazed abrasions:
Injuries caused by friction against a broad, rough surface, removing the outer skin layer.
Common causes:
Road traffic accidents
Falls
Body dragging before or after death
Key features:
Often cover a large area of the body
Depth varies depending on surface roughness and speed of movement
Common when a person is thrown from a vehicle
Forensic significance:
Vital reactions can help determine if the abrasion occurred before or after death
May contain embedded trace evidence (e.g., soil, dirt, carpet fibres) from the surface involved
What are patterned abrasions and what types exist?
Patterned abrasions:
Abrasions caused by perpendicular force on the skin, leaving an imprint of the object or surface involved.
Types:
Pressure abrasions
Caused by prolonged compression with minimal force
Impact abrasions
Caused by a swift blow with greater force
Often occurs when someone is thrown against a surface
Examples:
Ligature marks
Auto vs pedestrian accidents
Forensic significance:
The pattern of the abrasion may help identify the object or surface responsible.
Case Example – Patterned Abrasion in Infant Death:
A 4-month-old baby was found deceased with a patterned abrasion matching clothing marks. The infant had become lodged between the mattress and wall. What was the forensic interpretation?
Key findings:
Patterned abrasion consistent with clothing imprint
Infant found trapped between mattress and wall
No prior medical conditions
Resuscitation attempts unsuccessful
Cause of death:
Asphyxiation due to positional entrapment
Forensic significance:
The patterned abrasion helped reconstruct the position of the body and supported an accidental cause of death.
Case Example – Scratch Abrasions:
A 42-year-old man was found dead in his garden with multiple injuries and scratch abrasions on the eyelid, forehead, and neck. What was the forensic interpretation?
Key findings:
Multiple scratch abrasions on the eyelid, forehead, and neck
Injury mapping used to analyse the pattern and direction of contact
Injuries consistent with contact between two individuals
Forensic interpretation:
Evidence suggested a physical struggle or fight
Injuries were limited to one attacker
Outcome:
A suspect with matching scratches was identified and arrested.
What is blunt force trauma?
Injury caused by impact with a blunt object such as a bat, rock or fist.
What injuries are associated with blunt force trauma?
Contusions (bruises), abrasions (scrape) and lacerations (deep irregular cut).
How can abrasions indicate the direction in which force was applied?
Torn fragments of skin are dragged towards the furthest edge of the wound
What is a contusion?
A bruise caused by ruptured blood vessels beneath the skin.
What is an abrasion?
A superficial scrape of the skin caused by friction.
What is a laceration?
A tear in the skin caused by blunt force trauma.
What is tissue bridging?
Nerves and blood vessels stretching across a wound indicating blunt force trauma.
What is sharp force trauma?
Injury caused by sharp objects such as knives, glass or razors.
What is an incision?
A clean cut wound caused by a sharp object.
What are characteristics of incisions?
Smooth edges, no tissue bridging and longer than deep.
What is a stab wound?
A deep penetrating wound caused by a sharp object.
What are defensive wounds?
Injuries sustained when a victim attempts to protect themselves during an attack.
Where are defensive wounds usually found?
Palms, forearms and fingers.
A lack of ‘vital reaction’ occurs when death by hanging is a result of
A homicide disguised as a suicide
Damage to the hyoid bone is a characteristic sign of:
Manual strangulation