(Physiology) Peripheral Vascular and Lymphatic Systems: HA Ch 18
1/64
Earn XP
Description and Tags
Health Assessment Nursing Physiology
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
65 Terms
Arteries
High-pressure blood vessels that carry oxygenated, nutrient-rich blood from the heart to the capillaries are called ________.
Veins
Low-pressure vessels that carry deoxygenated, nutrient-depleted, waste-laden blood from tissues back to the heart are ________.
Capillary
The small vessel that forms the connection between arterioles and venules, allowing for fluid and gas exchange, is a ________.
Arterial pulse
A surge of blood forced through arterial vessels by each heartbeat, felt by compressing an artery against a bone, is the ________.
Brachial artery
The major artery supplying the arm is the ________.
Radial artery
The pulse palpated on the thumb side of the lateral wrist is the ________.
Ulnar artery
The deeper pulse palpated on the medial aspect of the inner wrist is the ________.
Femoral artery
The major artery supplying the leg, palpated medial to the inguinal ligament, is the ________.
Popliteal artery
The pulse found behind the knee, which may be difficult to palpate in a supine position, is the ________.
Dorsalis pedis artery
The artery located on the dorsal aspect of the foot, lateral to the big toe tendon, is the ________.
Posterior tibial artery
The artery palpated in the groove behind the medial malleolus of the ankle is the ________.
venous valves
The structure within veins that prevents backflow of blood is the ________.
Muscle pump
The mechanism of venous return where skeletal muscles contract to squeeze blood toward the heart is the ________.
Pressure gradient
Inspiration aids venous return by decreasing intrathoracic pressure and increasing abdominal pressure, creating a ________; respiratory pump
Lymphatic system
___________ collects excess interstitial fluid from tissues, transforms it into lymph, and returns it to the bloodstream via the subclavian veins near the heart to maintain fluid balance
the spleen, appendix, adenoids, tonsils, and thymus
the lymphatic system consists of the lymph nodes and lymphatic vessels as well as the organs and structures (5): ______________
Lymph nodes
Small, round filters that trap and destroy microorganisms from lymph before it enters the blood are ________.
Epitrochlear nodes
Lymph nodes located approximately 3 cm above the medial elbow that drain the lower arm and hand are ________.
inguinal nodes
In the lower extremities, the lymph drains primarily into the _________ of the upper medial thigh around the groin area
Peripheral Arterial Disease (PAD)
Intermittent claudication is the primary symptom of ________; it is characterized by muscle pain, cramping, or fatigue in the legs (usually the calf) during exercise, caused by reduced blood flow due to atherosclerosis, which is relieved by rest
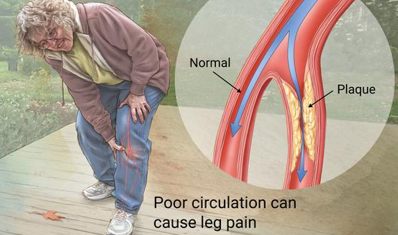
Arterial insufficiency
Skin that is thin, shiny, cool to the touch, and lacking hair distribution indicates ________.
Venous insufficiency
Rusty or brownish pigmentation around the ankles, warm skin, and edema are characteristic of ________.
Varicose veins
Raised, bulging, and tortuous veins caused by incompetent valves are ________.
Deep Vein Thrombosis (DVT)
Unilateral calf swelling, redness, and warmth are signs suggestive of ________.
Allen test
Before performing a radial artery puncture, the nurse evaluates arterial patency using the ________.
Doppler ultrasound device
Equipment used to detect unpalpable pulses or determine tissue perfusion is the ________.
Capillary refill time
The test where a nailbed is blanched to measure peripheral perfusion is ________.
2 seconds
A normal capillary refill time should be ________ or less.
2+
A normal pulse strength on the 0 to 3+ amplitude scale is documented as ________.
3+
An increased or bounding pulse strength is documented as ________.
1+
A weak, diminished pulse that is easy to obliterate is documented as ________.
0
An absent pulse is documented as ________.
Pitting edema
Fluid retention that leaves an indentation in the skin after pressure is released is called ________.
Position change test
To assess for arterial insufficiency when pulses are weak, the nurse performs the ________.
Elevation pallor
An abnormal finding during the position change test where the feet turn pale when raised is ________.
Dependent rubor
A dusky redness seen when the legs are dangling is called ________ and suggests arterial insufficiency.
Ankle-Brachial Index (ABI)
The ratio used to quantify the degree of peripheral arterial disease is the ________.
1.0 to 1.40
A normal ABI ratio, indicating no arterial insufficiency, is ________.
0.91 to 0.99
Borderline arterial insufficiency is indicated by an ABI ratio of ________.
0.3
Ischemia that is limb-threatening is indicated by an ABI ratio of less than ________.
Brachial systolic
The ABI is calculated by dividing the higher ankle systolic pressure by the higher ________ pressure.
Manual compression test
To assess for pulsations that indicate incompetent valves in varicose veins, the nurse performs the ________.
Trendelenburg test
Saphenous vein valve competence is evaluated by using a tourniquet in the ________.
Stage 0
The lymphedema stage where impaired drainage is subclinical and edema is not evident is ________.
Stage I
The lymphedema stage that is spontaneously reversible and where the affected area pits is ________.
Stage II
The lymphedema stage where skin tissue becomes fibrotic and elevation does not alleviate swelling is ________.
Stage III
The irreversible lymphedema stage known as lymphostatic elephantiasis is ________.
Pain
The "P" in the Seven Ps of PAD that refers to claudication or resting discomfort is ________.
Pallor
The "P" in the Seven Ps of PAD referring to a loss of skin color is ________.
Polar
The "P" in the Seven Ps of PAD referring to poikilothermia (coldness) is ________.
Paresthesia
The "P" in the Seven Ps of PAD referring to numbness or tingling is ________.
Pulselessness
The "P" in the Seven Ps of PAD referring to an inability to palpate a pulse is ________.
Paralysis
The "P" in the Seven Ps of PAD referring to the loss of muscle function is ________.
Perfusion
The "P" in the Seven Ps of PAD referring to blood flow through capillary beds is ________.
Lymphedema
Swelling that is typically unilateral, nonpitting, and causes induration is ________.
Bruit
A blowing, swishing sound caused by turbulent blood flow through a narrowed vessel is a ________.
Arterial ulcers
Painful sores located on pressure areas like the toes, with smooth "punched out" margins, are ________.
Venous ulcers
Superficial, painless sores located on the medial ankle with irregular borders are ________.
Profile sign
To detect nail clubbing associated with chronic hypoxia, the nurse observes the ________.
Induration
A hardening of the skin often seen in lymphedema or chronic inflammation is ________.
10 seconds
In the position change test, pinkish color should return to the toes within ________ or less.
30 minutes
To improve circulation, clients with PVD are encouraged to walk for ________ at least 3 times a week.
Smoking
A major modifiable risk factor for PAD that causes vasoconstriction is ________.
Bilateral symmetry
When inspecting extremities, the nurse compares them for ________ in size and shape.
Spleen
The lymphatic organ that produces lymphocytes and monocytes while filtering cellular debris from the blood is the ________.