Lewis Ch 50 Renal and Urologic Problems
1/53
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
54 Terms
A 46-year-old female patient returns to the clinic with recurrent dysuria after being treated with trimethoprim and sulfamethoxazole (Bactrim) for 3 days. Which action will the nurse plan to take?
a. Teach the patient to take the prescribed Bactrim for 3 more days.
b. Remind the patient about the need to drink 1000 mL of fluids daily.
c. Obtain a midstream urine specimen for culture and sensitivity testing.
d. Suggest that the patient use acetaminophen (Tylenol) to treat the symptoms.
c. Obtain a midstream urine specimen for culture and sensitivity testing
Diagnostic Studies- pg 1197
In a patient suspected of having a UTI, first obtain a dipstick urinalysis. This test can identify the presence of nitrites (indicating bacteriuria), white blood cells (WBCs), and leukocyte esterase (an enzyme present in WBCs, indicating pyuria). After confirmation of bacteriuria and pyuria, we may do a urine culture. A urine culture is needed in persistent bacteriuria, recurring UTIs (more than 2 or 3 per year), or complicated, CAUTI, or HAI UTIs. We may culture urine when the infection is not responsive to empiric therapy or the diagnosis is questionable.
A voided midstream technique (clean-catch urine sample) is best for obtaining a urine culture in most circumstances. A urine culture with sensitivity testing can determine the bacteria’s susceptibility to a variety of antibiotic drugs. The results allow the HCP to choose an antibiotic known to be capable of destroying the bacteria causing a UTI in a specific patient.
Some patients need imaging studies of the urinary tract. An ultrasound or CT scan may be done if we suspect an obstruction or UTIs recur.
Acetaminophen would not be as effective as other over-the-counter (OTC) medications such as phenazopyridine (Pyridium) in treating dysuria. The fluid intake should be increased to at least 1800 mL/day. Because the UTI has persisted after treatment with Bactrim, the patient is likely to need a different antibiotic. Lewis Clinical Handbook pg. 640
Which medication would the nurse associate with treatment of a patients voiding dysfunction by increasing the bladder's storage capacity?
a. Tamsulosin
b. Finasteride
c. Imipramine
d. Mirabegron
d. Mirabegron
Mirabegron is a B3-adrenergic agonist that relaxes the bladder muscle during filling, thereby improving the bladder’s storage capacity. Tamsulosin is an a-adrenergic antagonist that reduces urethral sphincter resistance. Finasteride is a 5a-reductive inhibitor that causes epithelial atrophy through androgen suppression, resulting in a decrease in total prostate size. Imipramine is a tricyclic antidepressant that reduces sensory urgency and burning of interstitial cystitis. Pg 1222
The nurse determines that instruction regarding the prevention of future urinary tract infections (UTIs) has been effective for a 22-year-old female patient with cystitis when the patient states which of the following?
a. I can use vaginal antiseptic sprays to reduce bacteria.
b. I will drink a quart of water or other fluids every day.
c. I will wash with soap and water before sexual intercourse.
d. I will empty my bladder every 3 to 4 hours during the day
d. I will empty my bladder every 3 to 4 hours during the day
Voiding every 3 to 4 hours is recommended to prevent UTIs. The use of vaginal sprays is discouraged. The bladder should be emptied before and after intercourse, but cleaning with soap and water is not necessary. A quart of fluids is insufficient to provide adequate urine output to decrease risk for UTI.
Table 50.4- pg 1198 Adequate fluid intake (8 to 9 8oz glasses/ day)
The nurse determines that further instruction is needed for a patient with interstitial cystitis when the patient says which of the following?
a. I should stop having coffee and orange juice for breakfast.
b. I will buy calcium glycerophosphate (Prelief) at the pharmacy.
c. I will start taking high potency multiple vitamins every morning.
d. I should call the doctor about increased bladder pain or odorous urine.
c. I will start taking high potency multiple vitamins every morning.
Lewis Clinical Companion pg 343- Patient Teaching
Advise the patient to take a multivitamin containing no than the recommended dietary allowance and to avoid high potency vitamins that may irritate the bladder.
Which information will the nurse include when teaching the patient with a urinary tract infection (UTI) about the use of phenazopyridine (Pyridium)?
a. Pyridium may cause photosensitivity
b. Pyridium may change the urine color.
c. Take the Pyridium for at least 7 days.
d. Take Pyridium before sexual intercourse.
b. Pyridium may change the urine color.
Patients should be taught that Pyridium will color the urine deep orange. Urinary analgesics should only be needed for a few days until the prescribed antibiotics decrease the bacterial count. Pyridium does not cause photosensitivity. Taking Pyridium before intercourse will not help reduce the risk of UTI.
Lewis Clinical Handbook- Patient and Caregiver teaching pg 640
Which finding by the nurse will be most helpful in determining whether a 67-year-old patient with benign prostatic hyperplasia has an upper urinary tract infection (UTI)?
a. Bladder distention
b. Foul-smelling urine
c. Suprapubic discomfort
d. Costovertebral tenderness
d. Costovertebral tenderness
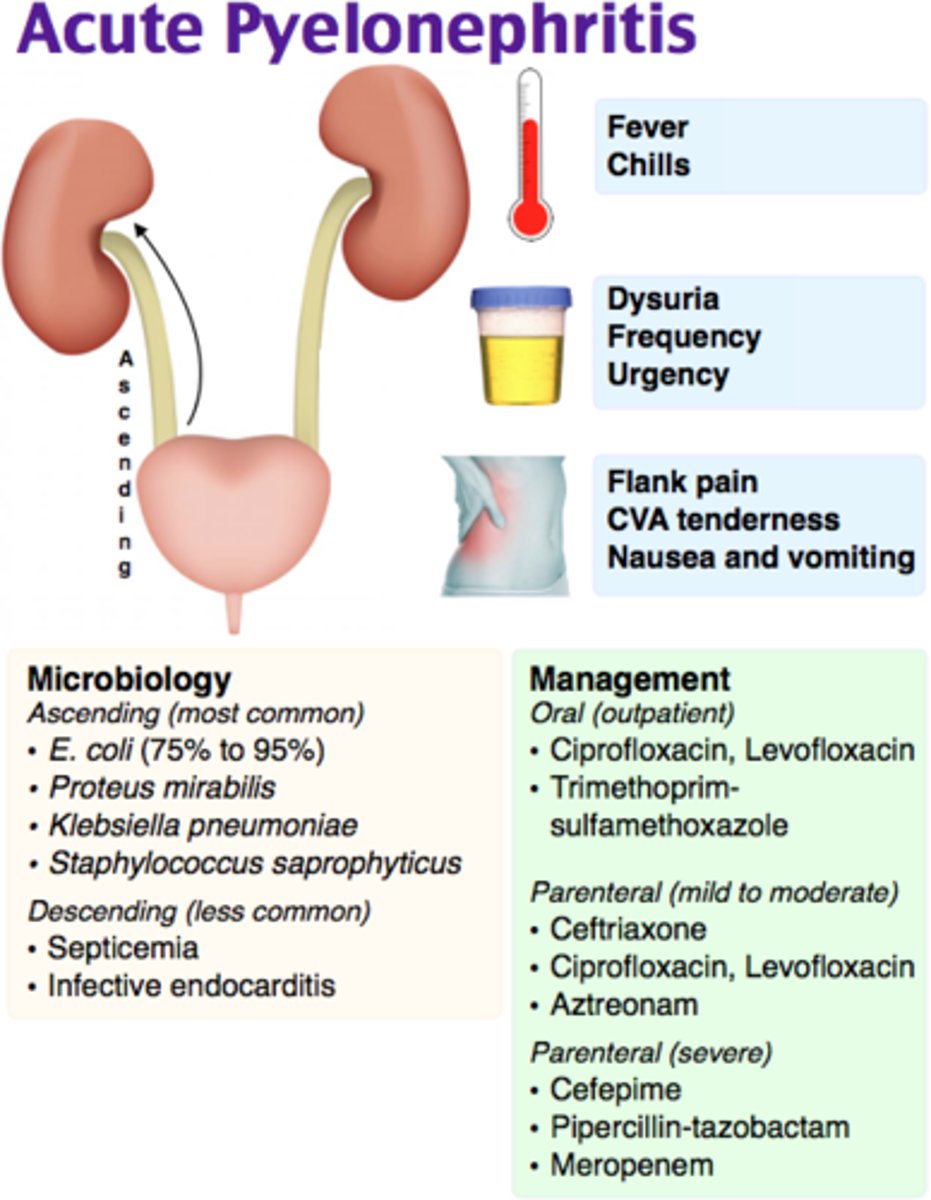
Costovertebral tenderness is characteristic of pyelonephritis. The classic manifestations include:
1. fever/chills, 2. nausea/vomiting, 3. malaise, and 4. flank pain. There may be LUTS, such as dysuria, urgency, and frequency. Costovertebral angle tenderness to percussion (costovertebral angle [CVA] pain) is typically present on the affected side. pg. 1200
BPH is a condition in which the prostate gland increases in size, disrupting the flow of urine from the bladder through the urethra. Complications of BPH: UTI and pyelonephritis can result from incomplete bladder emptying, which provides an environment for bacteria growth. Lewis Clinical Companion pg 68
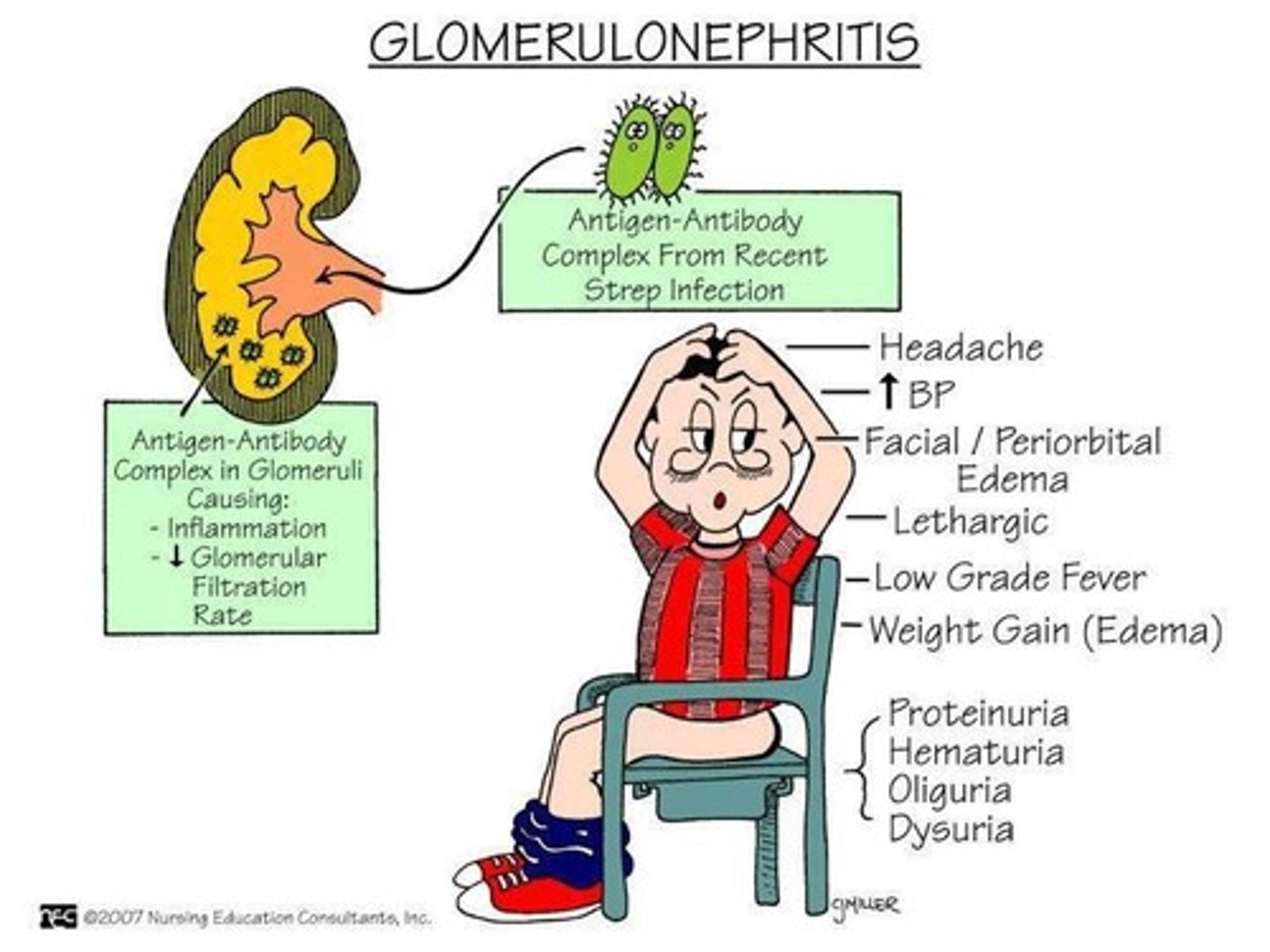
It is most important that the nurse ask a patient admitted with acute glomerulonephritis about
a. history of kidney stones.
b. recent sore throat and fever.
c. history of high blood pressure.
d. frequency of bladder infections.
b. recent sore throat and fever.
Acute poststreptococcal glomerulonephritis (APSGN) develops about 1 to 2 weeks after an infection of the tonsils, pharynx, or skin (e.g., streptococcal sore throat, impetigo) by nephrotoxic strains of group A β-hemolytic streptococci. Lewis Med Surg Clinical Companion pg 240
It is not caused by kidney stones, hypertension, or urinary tract infection (UTI).
Which finding for a patient admitted with glomerulonephritis indicates to the nurse that treatment has been effective?
a. The patient denies pain with voiding.
b. The urine dipstick is negative for nitrites.
c. The antistreptolysin-O (ASO) titer is decreased.
d. The periorbital and peripheral edema is resolved.
d. The periorbital and peripheral edema is resolved.
Because edema is a common clinical manifestation of glomerulonephritis (inflammation of the glomeruli), the resolution of the edema indicates that the prescribed therapies have been effective.
Lewis Clinical Companion pg 240
The nurse will anticipate teaching a patient with nephrotic syndrome who develops flank pain about treatment with
a. antibiotics.
b. antifungals.
c. anticoagulants.
d. antihypertensives.
c. anticoagulants.
Flank pain in a patient with nephrotic syndrome suggests a renal vein thrombosis, and anticoagulation is needed.
Hypercoagulability from the urinary loss of anticoagulant proteins increases the risk for arterial and venous thromboembolism, including pulmonary embolism and deep vein or renal thrombus.
Lewis CC, pg 413
A 56-year-old female patient is admitted to the hospital with new onset nephrotic syndrome. Which assessment data will the nurse expect?
a. Poor skin turgor
b. Recent weight gain
c. Elevated urine ketones
d. Decreased blood pressure
b. Recent weight gain
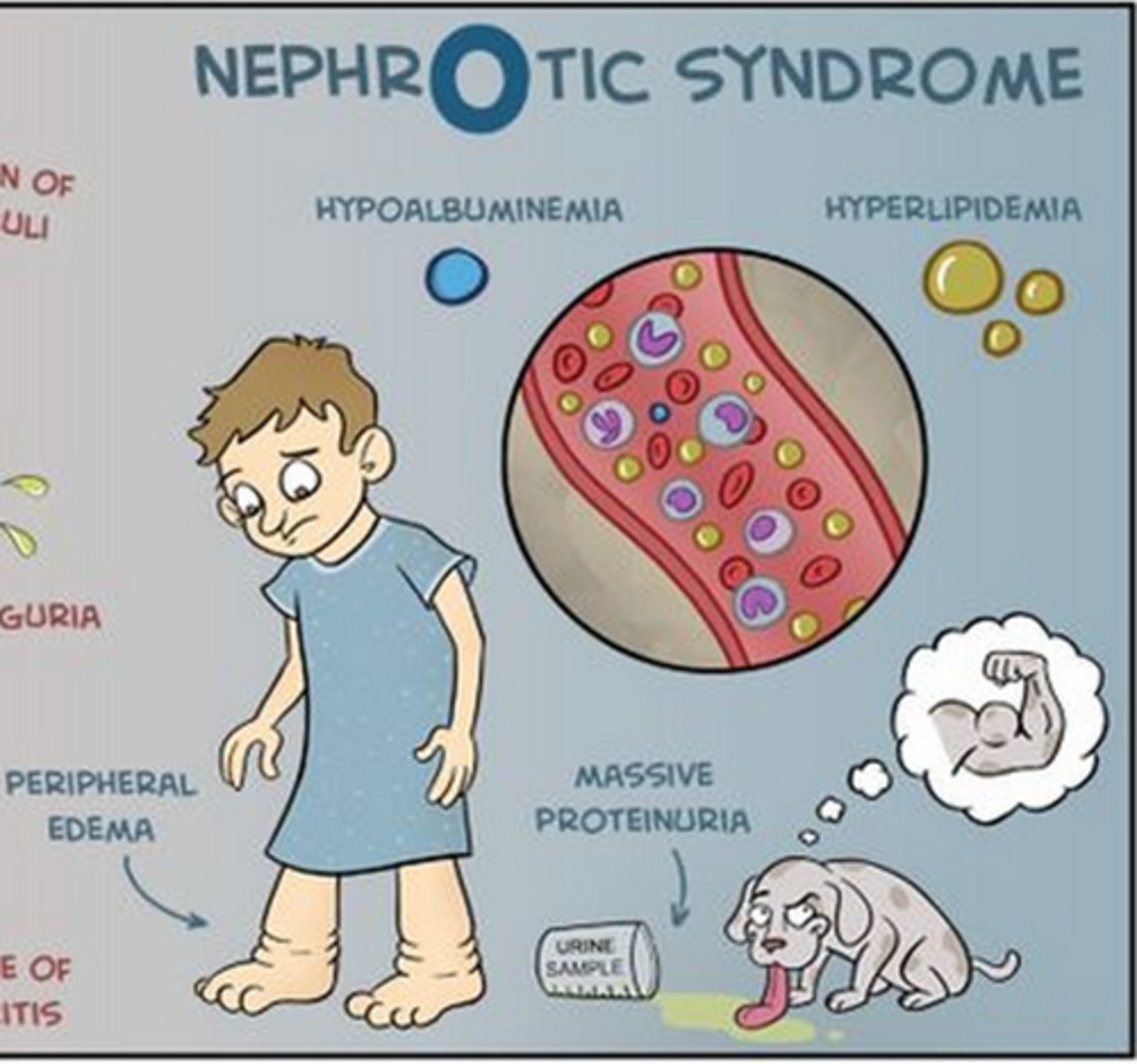
Nephrotic syndrome results when the glomerulus is excessively permeable to plasma protein, causing proteinuria that leads to low plasma albumin and edema.
Lewis MS Clinical Companion pg 413
The common manifestations are peripheral edema, massive proteinuria, hyperlipidemia, hypoalbuminemia, and foamy urine. The increased glomerular membrane permeability is responsible for the massive excretion of protein in the urine. This results in decreased total serum protein and subsequent edema formation. Ascites and anasarca (massive, generalized edema) develop if there is severe hypoalbuminemia.
pg 1206
To prevent the recurrence of uric acid renal calculi, the nurse teaches the patient to avoid eating
a. milk and cheese.
b. sardines and liver.
c. legumes and dried fruit.
d. spinach, chocolate, and tea.
b. sardines and liver.
Organ meats and fish such as sardines increase purine levels and uric acid. Spinach, chocolate, and tomatoes should be avoided in patients who have oxalate stones. Milk, dairy products, legumes, and dried fruits may increase the incidence of calcium-containing stones.
Table 50.12 pg. 1211
The nurse teaches a 64-year-old woman to prevent the recurrence of renal calculi by
a. using a filter to strain all urine.
b. avoiding dietary sources of calcium.
c. choosing diuretic fluids such as coffee.
d. drinking 2000 to 3000 mL of fluid a day.
d. drinking 2000 to 3000 mL of fluid a day.
A fluid intake of 2000 to 3000 mL daily is recommended to help flush out minerals before stones can form.
The patient has a disorder that includes the inflammation of renal parenchyma and the collecting system. The nurse suspects?
a. Pyelonephritis
b. Interstitial cystitis
c. Urethral diverticula
d. Glomerulonephritis
a. Pyelonephritis
Pyelonephritis is an inflammation of the renal parenchyma and collecting system (including the renal pelvis). The most common cause is bacterial infection. Urosepsis is a systemic infection arising from a urologic source. If hot treated promptly, it can lead to septic shock and death.
NOTE: For residents of long term care facilities, catheter-associated urinary tract infections (CAUTIs) are common causes of pyelonephritis and urosepsis. Lewis Med Surg Clinical Companion pg 506-508
When planning teaching for a 59-year-old male patient with benign nephrosclerosis the nurse should include instructions regarding
a. preventing bleeding with anticoagulants.
b. monitoring and recording blood pressure.
c. obtaining and documenting daily weights.
d. measuring daily intake and output volumes.
b. monitoring and recording blood pressure.
Hypertension is the major symptom of nephrosclerosis. Measurements of intake and output and daily weights are not necessary unless the patient develops renal insufficiency. Anticoagulants are not used to treat nephrosclerosis.
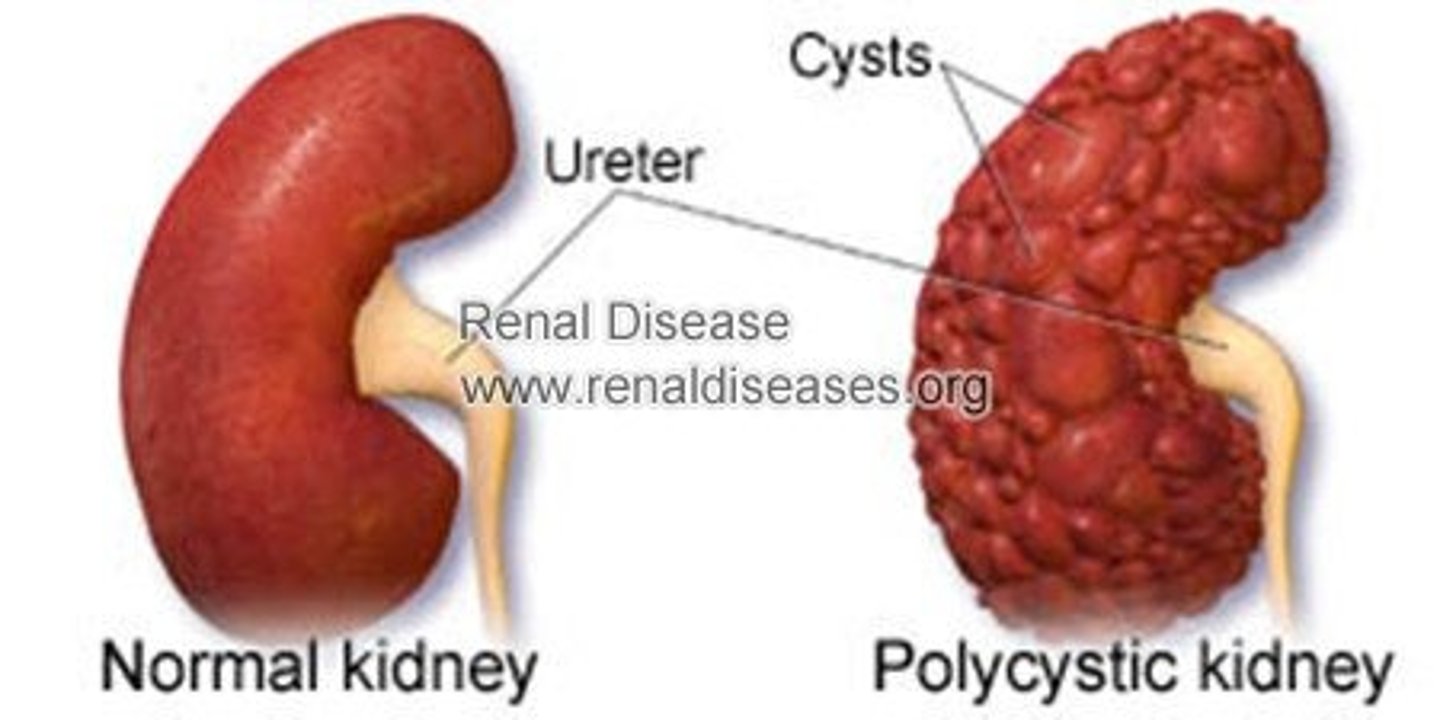
A 28-year-old male patient is diagnosed with polycystic kidney disease. Which information is most appropriate for the nurse to include in teaching at this time?
a. Complications of renal transplantation
b. Methods for treating severe chronic pain
c. Discussion of options for genetic counseling
d. Differences between hemodialysis and peritoneal dialysis
c. Discussion of options for genetic counseling
Because a 28-year-old patient may be considering having children, the nurse should include information about genetic counseling when teaching the patient. The well-managed patient will not need to choose between hemodialysis and peritoneal dialysis or know about the effects of transplantation for many years. There is no indication that the patient has chronic pain.
A 34-year-old male patient seen at the primary care clinic complains of feeling continued fullness after voiding and a split, spraying urine stream. The nurse will ask about a history of
a. recent kidney trauma.
b. gonococcal urethritis.
c. recurrent bladder infection.
d. benign prostatic hyperplasia.
b. gonococcal urethritis
The patients clinical manifestations are consistent with urethral strictures, a possible complication of gonococcal urethritis. These symptoms are not consistent with benign prostatic hyperplasia, kidney trauma, or bladder infection.
See Urethritis pg 626 Lewis MS CC book
The nurse will plan to teach a 27-year-old female who smokes 2 packs of cigarettes daily about the increased risk
a. kidney stones.
b. bladder cancer.
c. bladder infection.
d. interstitial cystitis.
b. bladder cancer
Cigarette smoking is a risk factor for bladder cancer. The patients risk for developing interstitial cystitis, urinary tract infection (UTI), or kidney stones will not be reduced by quitting smoking.
A 68-year-old female patient admitted to the hospital with dehydration is confused and incontinent of urine. Which nursing action will be best to include in the plan of care?
a. Restrict fluids between meals and after the evening meal.
b. Apply absorbent incontinent pads liberally over the bed linens.
c. Insert an indwelling catheter until the symptoms have resolved.
d. Assist the patient to the bathroom every 2 hours during the day.
d. Assist the patient to the bathroom every 2 hours during the day.
In older or confused patients, incontinence may be avoided by using scheduled toileting times. Indwelling catheters increase the risk for urinary tract infection (UTI). Incontinent pads increase the risk for skin breakdown. Restricting fluids is not appropriate in a patient with dehydration.
A 55-year-old woman admitted for shoulder surgery asks the nurse for a perineal pad, stating that laughing or coughing causes leakage of urine. Which intervention is most appropriate to include in the care plan?
a. Assist the patient to the bathroom q3hr.
b. Place a commode at the patients bedside.
c. Demonstrate how to perform the Cred maneuver.
d. Teach the patient how to perform Kegel exercises.
d. Teach the patient how to perform Kegel exercises.
Kegel exercises to strengthen the pelvic floor muscles will help reduce stress incontinence. The Cred maneuver is used to help empty the bladder for patients with overflow incontinence. Placing the commode close to the bedside and assisting the patient to the bathroom are helpful for functional incontinence.
The patient has been diagnosed with interstitial cystitis. The nurse anticipates the HCP to prescribe which oral medication?
a. Penicillin (Amoxicillin)
b. Pentosan (Elmiron)
c. Nortriptyline (Allegron)
d. Amitriptyline (Elavil)
b. Pentosan (Elmiron)
Pentosan is the only oral agent used in the treatment of interstitial cystitis.
Penicillin is used in the treatment of streptococcal infection as seen in acute poststreptococcal glomerulonephritis (APSNG). Nortriptyline and amitriptyline are tricyclic antidepressants that may be used to reduce burning pain and urinary frequency. Pg 1203
E. coli is resistant to which medication? Select all that apply.
a. Ciprofloxacin (Cipro)
b. Fosfomycin (Monurol)
c. Fluconazole (Diflucan)
d. Trimethoprim (Primsol)
e. Sulfamethoxazole (Gantanol)
a. Ciprofloxacin (Cipro)
d. Trimethoprim (Primsol)
e. Sulfamethoxazole (Gantanol)
These three drugs are used in combination to treat uncomplicated or initial UTI. Fosfomycin is a first choice drug used to treat uncomplicated or initial UTIs. Flucanozole is preferred therapy with UTI secondary to a fungal infection. Pg 1198
Following rectal surgery, a patient voids about 50 mL of urine every 30 to 60 minutes for the first 4 hours. Which nursing action is most appropriate?
a. Monitor the patients intake and output over night.
b. Have the patient drink small amounts of fluid frequently.
c. Use an ultrasound scanner to check the postvoiding residual volume.
d. Reassure the patient that this is normal after rectal surgery because of anesthesia
c. Use an ultrasound scanner to check the postvoiding residual volume.
An ultrasound scanner can be used to check for residual urine after the patient voids. Because the patients history and clinical manifestations are consistent with overflow incontinence, it is not appropriate to have the patient drink small amounts. Although overflow incontinence is not unusual after surgery, the nurse should intervene to correct the physiologic problem, not just reassure the patient. The patient may develop reflux into the renal pelvis and discomfort from a full bladder if the nurse waits to address the problem for several hours.
A patient admitted to the hospital with pneumonia has a history of functional urinary incontinence. Which nursing action will be included in the plan of care?
a. Demonstrate the use of the Cred maneuver.
b. Teach exercises to strengthen the pelvic floor.
c. Place a bedside commode close to the patients bed.
d. Use an ultrasound scanner to check postvoiding residuals.
c. Place a bedside commode close to the patients bed.
Modifications in the environment make it easier to avoid functional incontinence. Checking for residual urine and performing the Cred maneuver are interventions for overflow incontinence. Kegel exercises are useful for stress incontinence.
The home health nurse teaches a patient with a neurogenic bladder how to use intermittent catheterization for bladder emptying. Which patient statement indicates that the teaching has been effective?
a. I will buy seven new catheters weekly and use a new one every day.
b. I will use a sterile catheter and gloves for each time I self-catheterize.
c. I will clean the catheter carefully before and after each catheterization.
d. I will need to take prophylactic antibiotics to prevent any urinary tract infections
c. I will clean the catheter carefully before and after each catheterization.
Patients who are at home can use a clean technique for intermittent self-catheterization and change the catheter every 7 days. There is no need to use a new catheter every day, to use sterile catheters, or to take prophylactic antibiotics.
After a ureterolithotomy, a female patient has a left ureteral catheter and a urethral catheter in place. Which action will the nurse include in the plan of care?
a. Provide teaching about home care for both catheters.
b. Apply continuous steady tension to the ureteral catheter.
c. Call the health care provider if the ureteral catheter output drops suddenly.
d. Clamp the ureteral catheter off when output from the urethral catheter stops.
c. Call the health care provider if the ureteral catheter output drops suddenly.
The health care provider should be notified if the ureteral catheter output decreases because obstruction of this catheter may result in an increase in pressure in the renal pelvis. Tension on the ureteral catheter should be avoided in order to prevent catheter displacement. To avoid pressure in the renal pelvis, the catheter is not clamped. Because the patient is not usually discharged with a ureteral catheter in place, patient teaching about both catheters is not needed.
A 68-year-old male patient who has bladder cancer had a cystectomy with creation of an Indiana pouch. Which topic will be included in patient teaching?
a. Application of ostomy appliances
b. Barrier products for skin protection
c. Catheterization technique and schedule
d. Analgesic use before emptying the pouch
c. Catheterization technique and schedule
The Indiana pouch enables the patient to self-catheterize every 4 to 6 hours. There is no need for an ostomy device or barrier products. Catheterization of the pouch is not painful.
A patient who had surgery for creation of an ileal conduit 3 days ago will not look at the stoma and requests that only the ostomy nurse specialist does the stoma care. The nurse identifies a nursing diagnosis of
a. anxiety related to effects of procedure on lifestyle.
b. disturbed body image related to change in function.
c. readiness for enhanced coping related to need for information.
d. self-care deficit, toileting, related to denial of altered body function.
b. disturbed body image related to change in function.
The patients unwillingness to look at the stoma or participate in care indicates that disturbed body image is the best diagnosis. No data suggest that the impact on lifestyle is a concern for the patient. The patient does not appear to be ready for enhanced coping. The patients insistence that only the ostomy nurse care for the stoma indicates that denial is not present.
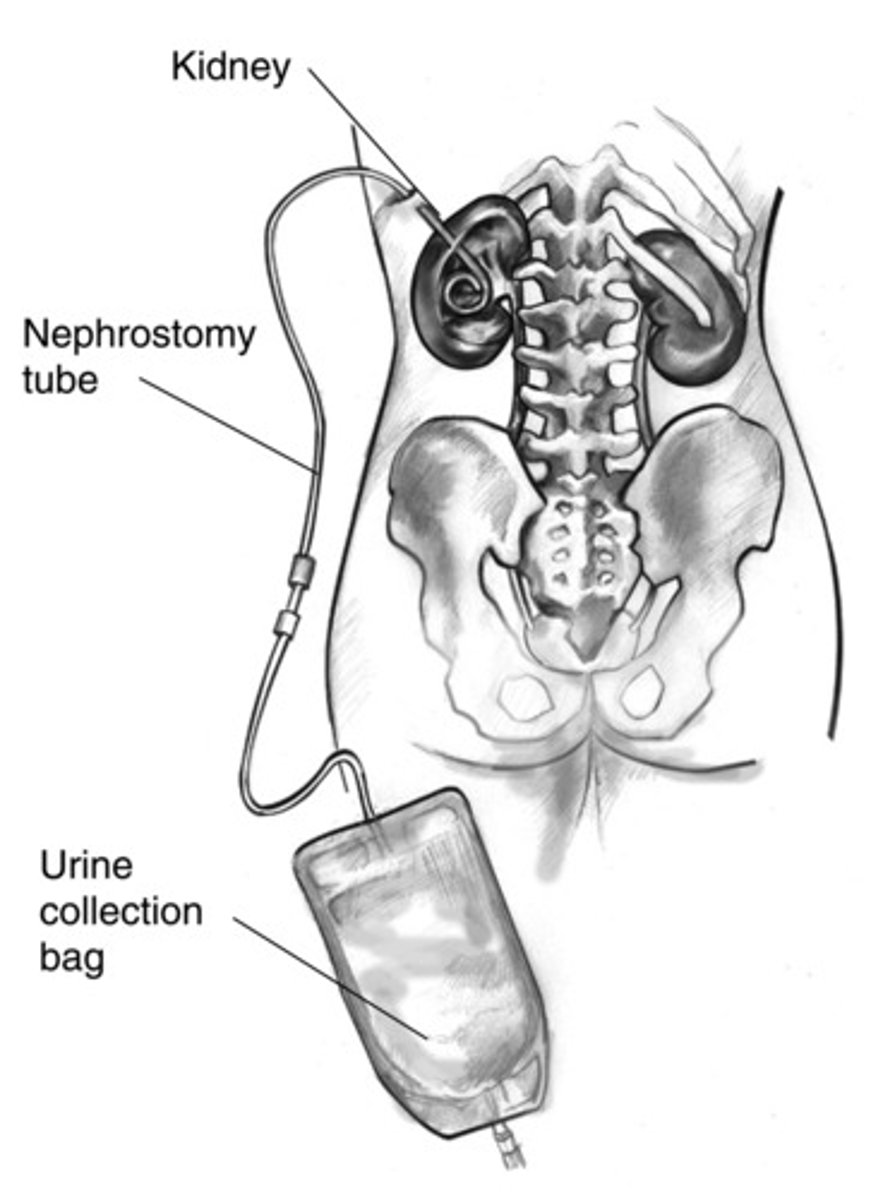
For a patient with a newly inserted nephrons to my tube, which intervention would the nurse perform during the postoperative period? Select all that apply
a. Clamp the nephrostomy catheter during ambulation
b. Observe the amount, color, and consistency of urine
c. Attend to caring for the stoma and collection device
d. Measure urinary output every 1 or 2 hours at least
e. Measure drainage from the catheters and surgical dressing
b. Observe the amount, color, and consistency of urine
d. Measure urinary output every 1 or 2 hours at least
e. Measure drainage from the catheters and surgical dressing
Observing the amount, color, and consistency or urine is important because urine with increased amounts of mucus, blood, or sediment may occlude the drainage tubing or catheter. Measuring and recording urine output is important because the total urine output should be at least 0.5 mL/kg/hr. It is important to assess urine drainage from the catheters and on the dressings to estimate the minimum amount of urine output. Never clamp the catheter unless ordered to do so by a health care provider. There is no stoma after a nephrectomy; the stoma and its care are an integral part of procedures such as ileal conduit. Pg 1226
Which information from a patient who had a transurethral resection with fulguration for bladder cancer 3 days ago is most important to report to the health care provider?
a. The patient is voiding every 4 hours.
b. The patient is using opioids for pain.
c. The patient has seen clots in the urine.
d. The patient is anxious about the cancer.
c. The patient has seen clots in the urine.
Clots in the urine are not expected and require further follow-up. Voiding every 4 hours, use of opioids for pain, and anxiety are typical after this procedure.
When preparing a female patient with bladder cancer for intravesical chemotherapy, the nurse will teach about
a. premedicating to prevent nausea.
b. obtaining wigs and scarves to wear.
c. emptying the bladder before the medication.
d. maintaining oral care during the treatments.
c. emptying the bladder before the medication.
The patient will be asked to empty the bladder before instillation of the chemotherapy. Systemic side effects are not usually experienced with intravesical chemotherapy.
Bladder Cancer, pg 75 MS CC book
Nursing staff on a hospital unit are reviewing rates of hospital-acquired infections (HAI) of the urinary tract. Which nursing action will be most helpful in decreasing the risk for HAI in patients admitted to the hospital?
a. Encouraging adequate oral fluid intake
b. Testing urine with a dipstick daily for nitrites
c. Avoiding unnecessary urinary catheterizations
d. Providing frequent perineal hygiene to patients
c. Avoiding unnecessary urinary catheterizations
Because catheterization bypasses many of the protective mechanisms that prevent urinary tract infection (UTI), avoidance of catheterization is the most effective means of reducing HAI. The other actions will also be helpful, but are not as useful as decreasing urinary catheter use.
Which assessment data reported by a 28-year-old male patient is consistent with a lower urinary tract infection (UTI)?
a. Poor urine output
b. Bilateral flank pain
c. Nausea and vomiting
d. Burning on urination
d. Burning on urination
Pain with urination is a common symptom of a lower UTI. Urine output does not decrease, but frequency may be experienced. Flank pain and nausea are associated with an upper UTI.
A 58-year-old male patient who is diagnosed with nephrotic syndrome has ascites and 4+ leg edema. Which nursing diagnosis is a priority for the patient?
a. Activity intolerance related to rapidly increased weight
b. Excess fluid volume related to low serum protein levels
c. Disturbed body image related to peripheral edema and ascites
d. Altered nutrition: less than required related to protein restriction
b. Excess fluid volume related to low serum protein levels
The patient has massive edema, so the priority problem at this time is the excess fluid volume. The other nursing diagnoses are also appropriate, but the focus of nursing care should be resolution of the edema and ascites
A 76-year-old with benign prostatic hyperplasia (BPH) is agitated and confused, with a markedly distended bladder. Which intervention prescribed by the health care provider should the nurse implement first?
a. Insert a urinary retention catheter.
b. Schedule an intravenous pyelogram (IVP).
c. Draw blood for a serum creatinine level.
d. Administer lorazepam (Ativan) 0.5 mg PO.
a. Insert a urinary retention catheter.
The patients history and clinical manifestations are consistent with acute urinary retention, and the priority action is to relieve the retention by catheterization. The BUN and creatinine measurements can be obtained after the catheter is inserted. The patients agitation may resolve once the bladder distention is corrected, and sedative drugs should be used cautiously in older patients. The IVP is an appropriate test but does not need to be done urgently.
Lewis’s MS CC book pg 67-75
Which nursing action is of highest priority for a 68-year-old patient with renal calculi who is being admitted to the hospital with gross hematuria and severe colicky left flank pain?
a. Administer prescribed analgesics.
b. Monitor temperature every 4 hours.
c. Encourage increased oral fluid intake.
d. Give antiemetics as needed for nausea.
a. Administer prescribed analgesics.
Although all of the nursing actions may be used for patients with renal lithiasis, the patients presentation indicates that management of pain is the highest priority action. If the patient has urinary obstruction, increasing oral fluids may increase the symptoms. There is no evidence of infection or nausea.
The nurse is caring for a patient who has had an ileal conduit for several years. Which nursing action could be delegated to unlicensed assistive personnel (UAP)?
a. Change the ostomy appliance.
b. Choose the appropriate ostomy bag.
c. Monitor the appearance of the stoma.
d. Assess for possible urinary tract infection (UTI).
a. Change the ostomy appliance.
Changing the ostomy appliance for a stable patient could be done by UAP. Assessments of the site, choosing the appropriate ostomy bag, and assessing for (UTI) symptoms require more education and scope of practice and should be done by the registered nurse (RN).
Which assessment finding is most important to report to the health care provider regarding a patient who has had left-sided extracorporeal shock wave lithotripsy?
a. Blood in urine
b. Left flank bruising
c. Left flank discomfort
d. Decreased urine output
d. Decreased urine output
Because lithotripsy breaks the stone into small sand, which could cause obstruction, it is important to report a drop in urine output. Left flank pain, bruising, and hematuria are common after lithotripsy.
A 44-year-old patient is unable to void after having an open loop resection and fulguration of the bladder. Which nursing action should be implemented first?
a. Assist the patient to soak in a 15-minute sitz bath.
b. Insert a straight urethral catheter and drain the bladder.
c. Encourage the patient to drink several glasses of water.
d. Teach the patient how to do isometric perineal exercises.
a. Assist the patient to soak in a 15-minute sitz bath.
A Sitz baths will relax the perineal muscles and promote voiding. Although the patient should be encouraged to drink fluids and Kegel exercises are helpful in the prevention of incontinence, these activities would not be helpful for a patient experiencing retention. Catheter insertion increases the risk for urinary tract infection (UTI) and should be avoided when possible
The nurse observes unlicensed assistive personnel (UAP) taking the following actions when caring for a female patient with a urethral catheter. Which action requires that the nurse intervene?
a. Taping the catheter to the skin on the patients upper inner thigh
b. Cleaning around the patients urinary meatus with soap and water
c. Disconnecting the catheter from the drainage tube to obtain a specimen
d. Using an alcohol-based gel hand cleaner before performing catheter care
c. Disconnecting the catheter from the drainage tube to obtain a specimen
The catheter should not be disconnected from the drainage tube because this increases the risk for urinary tract infection (UTI). The other actions are appropriate and do not require any intervention.
A 58-year-old male patient who weighs 242 lb (110 kg) undergoes a nephrectomy for massive kidney trauma due to a motor vehicle crash. Which postoperative assessment finding is most important to communicate to the surgeon?
a. Blood pressure is 102/58.
b. Urine output is 20 mL/hr for 2 hours.
c. Incisional pain level is reported as 9/10.
d. Crackles are heard at bilateral lung bases.
b. Urine output is 20 mL/hr for 2 hours.
Because the urine output should be at least 0.5 mL/kg/hr, a 40 mL output for 2 hours indicates that the patient may have decreased renal perfusion because of bleeding, inadequate fluid intake, or obstruction at the suture site. The blood pressure requires ongoing monitoring but does not indicate inadequate perfusion at this time. The patient should cough and deep breathe, but the crackles do not indicate a need for an immediate change in therapy. The incisional pain should be addressed, but this is not as potentially life threatening as decreased renal perfusion. In addition, the nurse can medicate the patient for pain.
Which clinical manifestation would the nurse associate with a patient's diagnosis of an upper UTI?
a. Fever
b. Chills
c. Afebrile
d. Flank pain
e. Clear, yellow urine
a. Fever
b. Chills
d. Flank pain
Upper UTI symptoms include fever, chills, and flank pain. The patient will not be a febrile, and urine will likely be cloudy, not clear and yellow. Pg. 1197
A 63-year-old male patient had a cystectomy with an ileal conduit yesterday. Which new assessment data is most important for the nurse to communicate to the physician?
a. Cloudy appearing urine
b. Hypotonic bowel sounds
c. Heart rate 102 beats/minute
d. Continuous stoma drainage
c. Heart rate 102 beats/minute
Tachycardia may indicate infection, hemorrhage, or hypovolemia, which are all serious complications of this surgery. The urine from an ileal conduit normally contains mucus and is cloudy. Hypotonic bowel sounds are expected after bowel surgery. Continuous drainage of urine from the stoma is normal.
A 32-year-old patient with a history of polycystic kidney disease is admitted to the surgical unit after having shoulder surgery. Which of the routine postoperative orders is most important for the nurse to discuss with the health care provider?
a. Infuse 5% dextrose in normal saline at 75 mL/hr.
b. Order regular diet after patient is awake and alert.
c. Give ketorolac (Toradol) 10 mg PO PRN for pain.
d. Draw blood urea nitrogen (BUN) and creatinine in 2 hours.
c. Give ketorolac (Toradol) 10 mg PO PRN for pain.
The nonsteroidal antiinflammatory drugs (NSAIDs) should be avoided in patients with decreased renal function because nephrotoxicity is a potential adverse effect. The other orders do not need any clarification or change.
Which instruction to prevent recurrent UTI would the nurse provide female patients?
a. Restrict purines in your diet
b. Schedule a follow up urine culture
c. Wipe back to front after urinating
d. Empty your bladder before and after sexual intercourse
d. Empty your bladder before and after sexual intercourse
Pg 1200

A 22-year-old female patient seen in the clinic for a bladder infection describes the following symptoms. Which information is most important for the nurse to report to the health care provider?
a. Urinary urgency
b. Left-sided flank pain
c. Intermittent hematuria
d. Burning with urination
b. Left-sided flank pain
Flank pain indicates that the patient may have developed pyelonephritis as a complication of the bladder infection. The other clinical manifestations are consistent with a lower urinary tract infection (UTI).
A patient in the urology clinic is diagnosed with monilial urethritis. Which action will the nurse include in the plan of care?
a. Teach the patient about the use of antifungal medications.
b. Tell the patient to avoid tub baths until the symptoms resolve.
c. Instruct the patient to refer recent sexual partners for treatment.
d. Teach the patient to avoid nonsteroidal antiinflammatory drugs (NSAIDs).
a. Teach the patient about the use of antifungal medications.
Monilial urethritis is caused by a fungus and antifungal medications such as nystatin (Mycostatin) or fluconazole (Diflucan) are usually used as treatment. Because monilial urethritis is not sexually transmitted, there is no need to refer sexual partners. Warm baths and NSAIDS may be used to treat symptoms.
Which action will the nurse anticipate taking for an otherwise healthy 50-year-old who has just been diagnosed with Stage 1 renal cell carcinoma?
a. Prepare patient for a renal biopsy.
b. Provide preoperative teaching about nephrectomy.
c. Teach the patient about chemotherapy medications.
d. Schedule for a follow-up appointment in 3 months.
b. Provide preoperative teaching about nephrectomy.
The treatment of choice in patients with localized renal tumors who have no co-morbid conditions is partial or total nephrectomy. A renal biopsy will not be needed in a patient who has already been diagnosed with renal cancer. Chemotherapy is used for metastatic renal cancer. Because renal cell cancer frequently metastasizes, treatment will be started as soon as possible after the diagnosis.
Which information about a patient with Goodpasture syndrome requires the most rapid action by the nurse?
a. Blood urea nitrogen level is 70 mg/dL.
b. Urine output over the last 2 hours is 30 mL.
c. Audible crackles bilaterally over the posterior chest to the midscapular level.
d. Elevated level of antiglomerular basement membrane (anti-GBM) antibodies.
c. Audible crackles bilaterally over the posterior chest to the midscapular level.
Crackles heard to a high level indicate a need for rapid actions such as assessment of oxygen saturation, reporting the findings to the health care provider, initiating oxygen therapy, and dialysis. The other findings will also be reported, but are typical of Goodpasture syndrome and do not require immediate nursing action.
A patient is admitted to the emergency department with possible renal trauma after an automobile accident. Which prescribed intervention will the nurse implement first?
a. Check blood pressure and heart rate.
b. Administer morphine sulfate 4 mg IV.
c. Transport to radiology for an intravenous pyelogram.
d. Insert a urethral catheter and obtain a urine specimen.
a. Check blood pressure and heart rate.
Because the kidney is very vascular, the initial action with renal trauma will be assessment for bleeding and shock. The other actions are also important once the patients cardiovascular status has been determined and stabilized.
After change-of-shift report, which patient should the nurse assess first?
a. Patient with a urethral stricture who has not voided for 12 hours
b. Patient who has cloudy urine after orthotopic bladder reconstruction
c. Patient with polycystic kidney disease whose blood pressure is 186/98 mm Hg
d. Patient who voided bright red urine immediately after returning from lithotripsy
a. Patient with a urethral stricture who has not voided for 12 hours
The patient information suggests acute urinary retention, a medical emergency. The nurse will need to assess the patient and consider whether to insert a retention catheter. The other patients will also be assessed, but their findings are consistent with their diagnoses and do not require immediate assessment or possible intervention.
A patient has been diagnosed with urinary tract calculi that are high in uric acid. Which foods will the nurse teach the patient to avoid
(select all that apply)?
a. Milk
b. Liver
c. Spinach
d. Chicken
e. Cabbage
f. Chocolate
b. Liver
d. Chicken
Meats contain purines, which are metabolized to uric acid. The other foods might be restricted in patients who have calcium or oxalate stones.
Which predisposing factor would the nurse associate with the development of calcium oxalate calculi?
a. Acidic urine
b. Hyperoxaluria
c. Urinary tract infection
d. Primary hyperthyroidism
b. Hyperoxaluria
Pg 1209
For the patient scheduled for insertion of a suprapubic catheter, which disorder would the nurse associate with this intervention?
a. Bladder cancer
b. Spinal cord injury
c. Neurological disease
d. Bladder outlet obstruction
a. Bladder cancer
Urethral, prostate, and bladder surgeries use insertion of a suprapubic catheter because the catheter provides an alternate route for elimination and promotes healing. Pg 1225