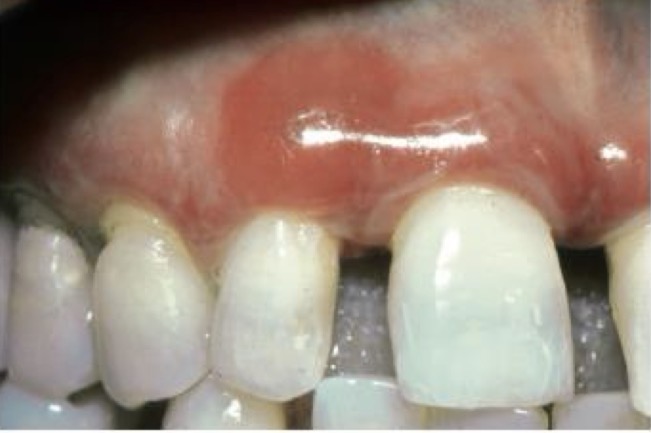
2- clinical forms of periodontal diseases
1/21
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
22 Terms
What is periodontal health?
Patient who has never had or suffered perio problems or patients who have had them but treated successfully- restored health
Clinical heath can occur in 3 distinct situations…
Intact periodontum- no loss of insertion or bone
Reduced periodontum- loss of insertion and bone
Depending on cause that caused loss- difference between…
Patient with stable periodontitis- loss due to periodontitis- successful treatment, stable
Non periodontal patient- loss due to other causes like recessions or coronary lengthening surgery
What is periodontal stability characterised by?
Treatment successful by controlling systemic and local risk factors
Less than 10% bleeding on probing and probing depth 3mm or less
What does gingival health present?
Less than 10% of locations bleed with PD of 3mm or less
Difference between localised vs generalised gingivitis?
10-30% bleeding
More than 30% BOP
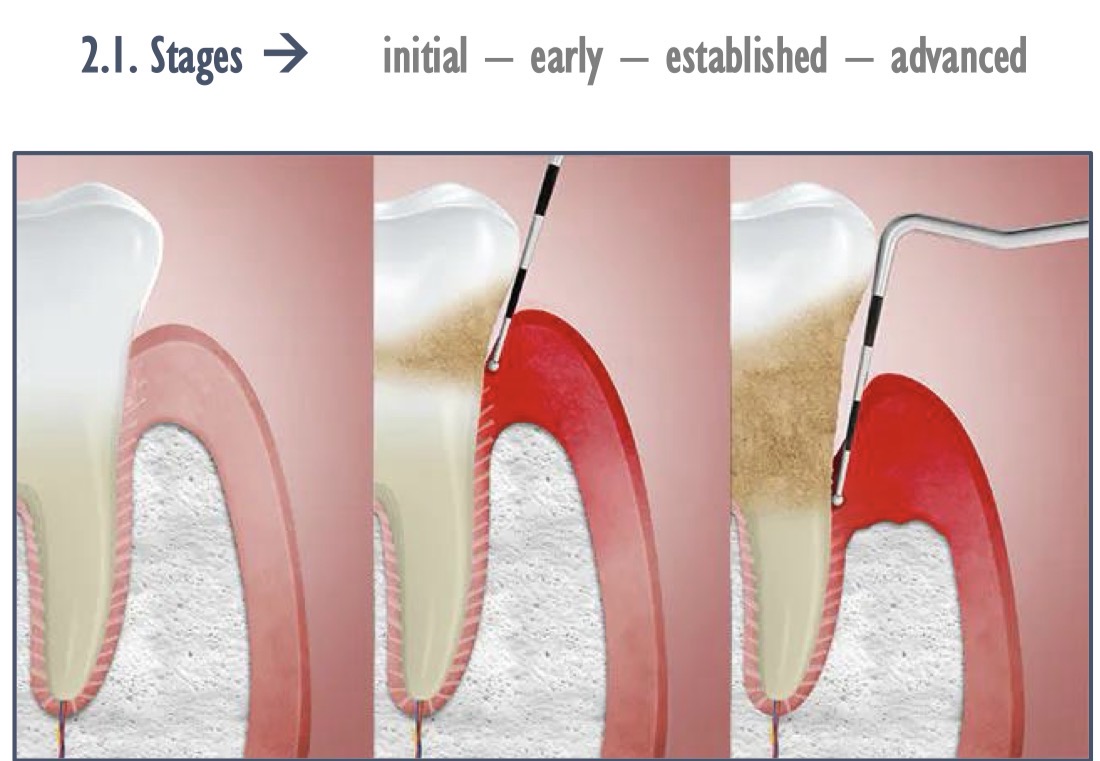
How does periodontitis start from initial- early- established to advanced stages?(4)
The first manifestations of gingival inflammation are vascular changes
Time passes, erythema signs may appear, especially capillary proliferation
Blood vessels dilate and congest, venous return is disturbed, slow blood circulation
Periodontal destruction
What changes are seen in gingiva (diseased) induced by dental biofilm?
Plaque at gingival margin where disease begins- changes gingival colour (red/blueish in interdental papillae and gingival margin)
Changes in gingival contour and groove temp- increased exudate (crevicular fluid)- bleeding from provocation (hemorrhage from smooth probing), no bone or insertion loss
Histologic modifications due to inflammation- reversible when plaque removed
How does gingivitis change gum texture?
Usually has depressions and small elevations- orange peel appearance
Dotted limited to inserted gum and mainly on subpapilalry area
Localised vs generalised marginal gingivitis affects what?
Limited to free gum of a tooth or more
Affects entire free gum of one arch or both
Localised vs generalised papillary gingivitis affects what?
Limited to one or more interproximal spaces in limited area
Affects most interproximal spaces
Localised vs generalised diffuse gingivitis affects what?
Inflammation extends from gingival margin to mucogingival line (goes apically) in 1 or more teeth
Affects entire gum, alveolar mucosa and inserted gum are inflamed, mucogingival line erased
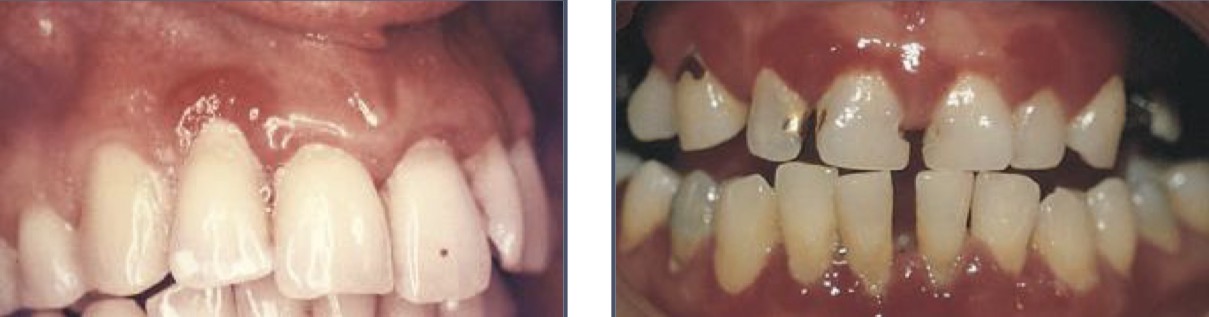
What is gum enlargement a common feature of?
Plaque induced gum disease or systemic conditions- drugs or genetics
Inflammatory enlargement
Drug-induced gingival enlargement
Idiopathic enlargement
Enlargement related to systemic diseases
Neoplasic enlargement
False enlargement- enlarged underlying tissues, bone injuries and dental tissues
Inflammatory enlargement characteristics?
Mild swelling of the papilla and marginal gum
Bulge covering part of the crown
Slow and painless
Localized/ generalized/ papillary/marginal/diffuse
Acute or Chronic
Drug induced enlargement characteristics
Small lobe in papilla and MGV vb + lingual
Pale pink color and resistance to touch
Inflammation secondary to drugs without or little plaque
Painless
Papillary
Drugs: Anticonvulsants/Immunosuppressants/Calcium channel blockers/hypertension
What drugs can cause gingival enlargement?
Phenytoin
Ethotoin
Mephenytoin
Valproic acid
Nifedipine
Diltiacem
Cyclosporine
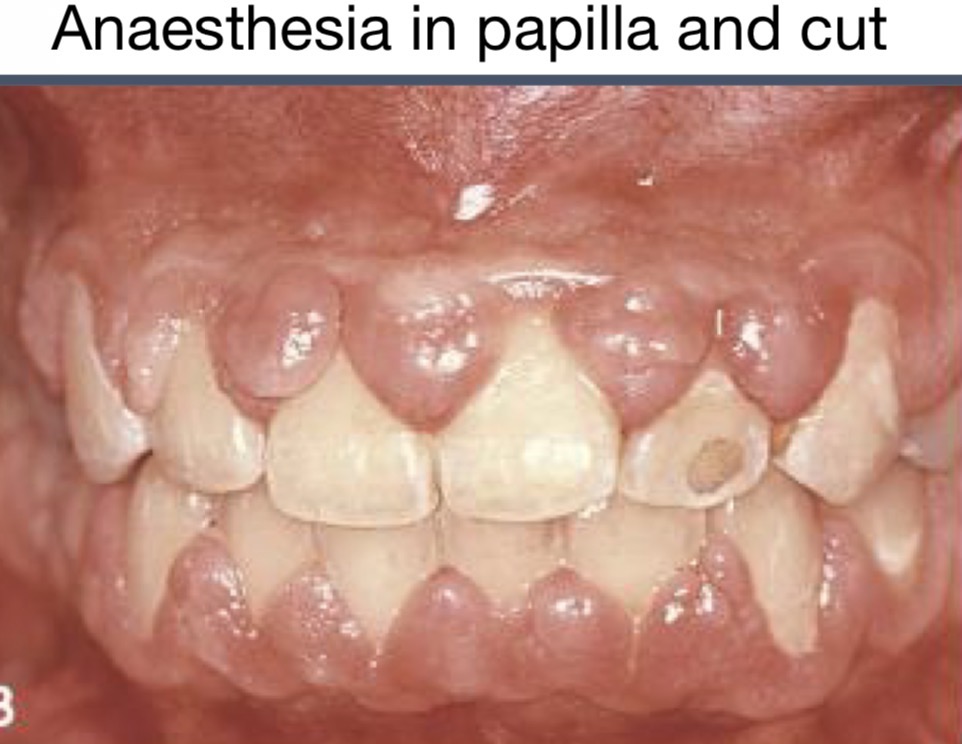
Idiopathic enlargement characteristics
Rare lobed alteration in inserted gum---in papilla and MGV
Pale pink color, firm and completely covers the crown
Unknown cause
Painless
In primary or secondary dentition
Surgical treatment
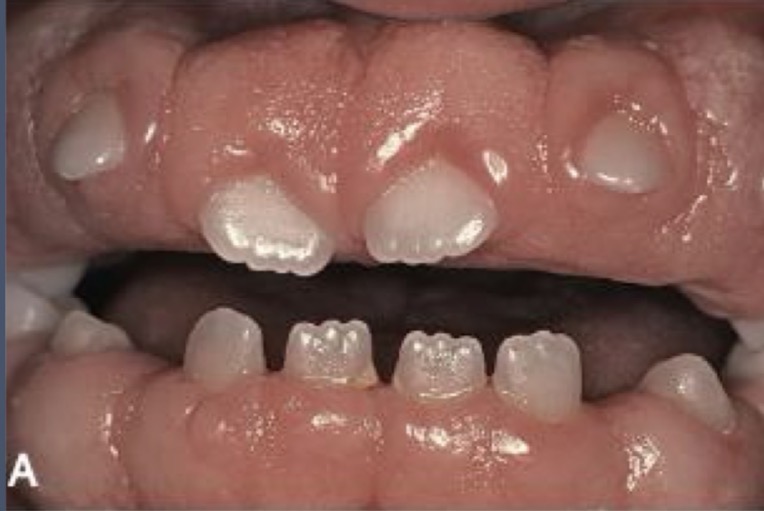
What systemic diseases can cause enlargement?
Increased pre existing plaque inflammation + conditioned enlargement:
Pregnancy / Puberty / Vitamin C deficiency / Plasma cells / Pyogenic granuloma
Systemic diseases that cause gingival enlargement:
Leukemias, Granulomatous diseases, Wegener's granulomatosis/Sarcoidosis
What benign vs malignant tumours can cause neoplastic enlargement?
Benign tumors
- Fibromas
- Papilomas
- Peripheral or central giant cell granuloma
- Leukoplasia
- Gingival cysts
Malignant tumors
- Squamous cell carcinoma
- Malignant melanoma
- Sarcoma
- Metastasis
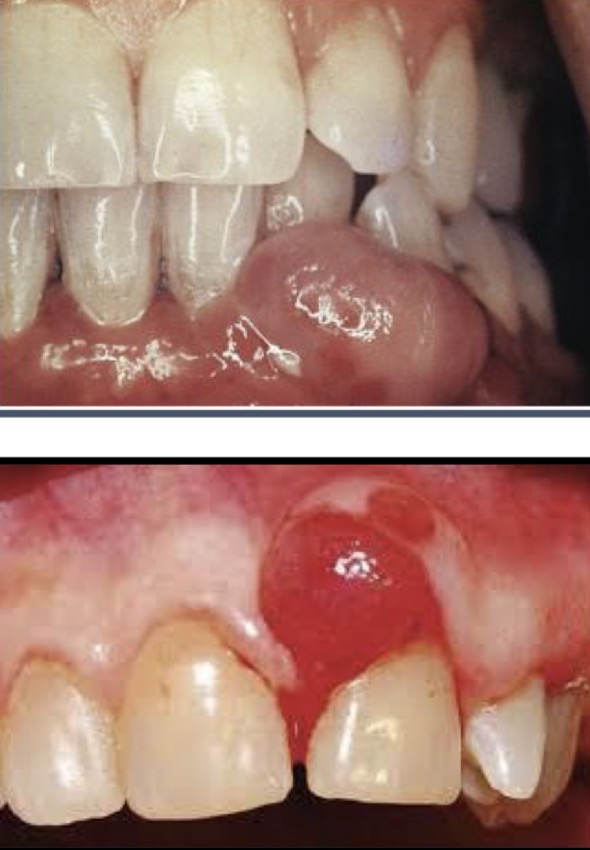
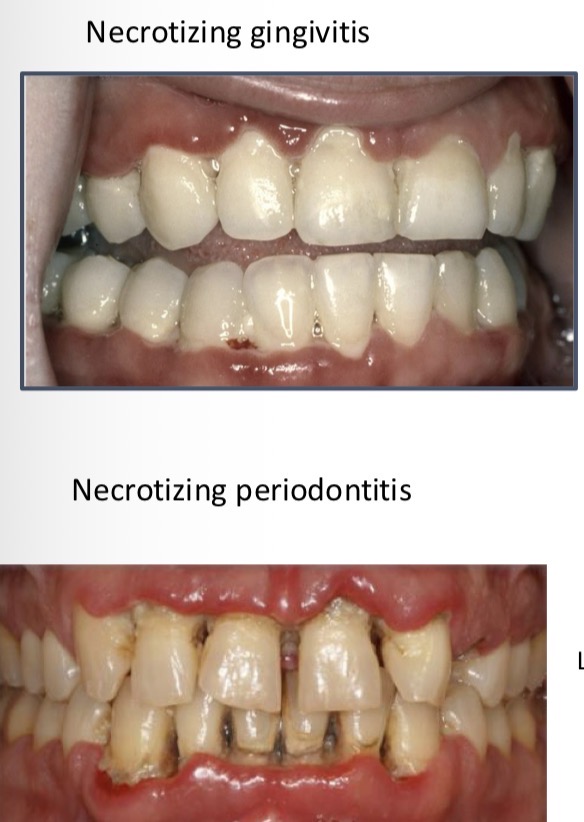
What is necrotising ulcerative gingivitis- etiology, location, signs, symptoms, treatment?
Microbial disease causing death and destruction of gingival tissue
Previous acute respiratory disease, lifestyle- stress, tobacco, nutrition, altered immune system
Marginal gum
Crater-like depressions on crest of interdental papilla
Halitosis, hyper salivation, pain, metallic taste, spontaneous bleeding
Scaling and root planing - Reversible- no loss of bone- papilla height given by bone so papilla can grow back
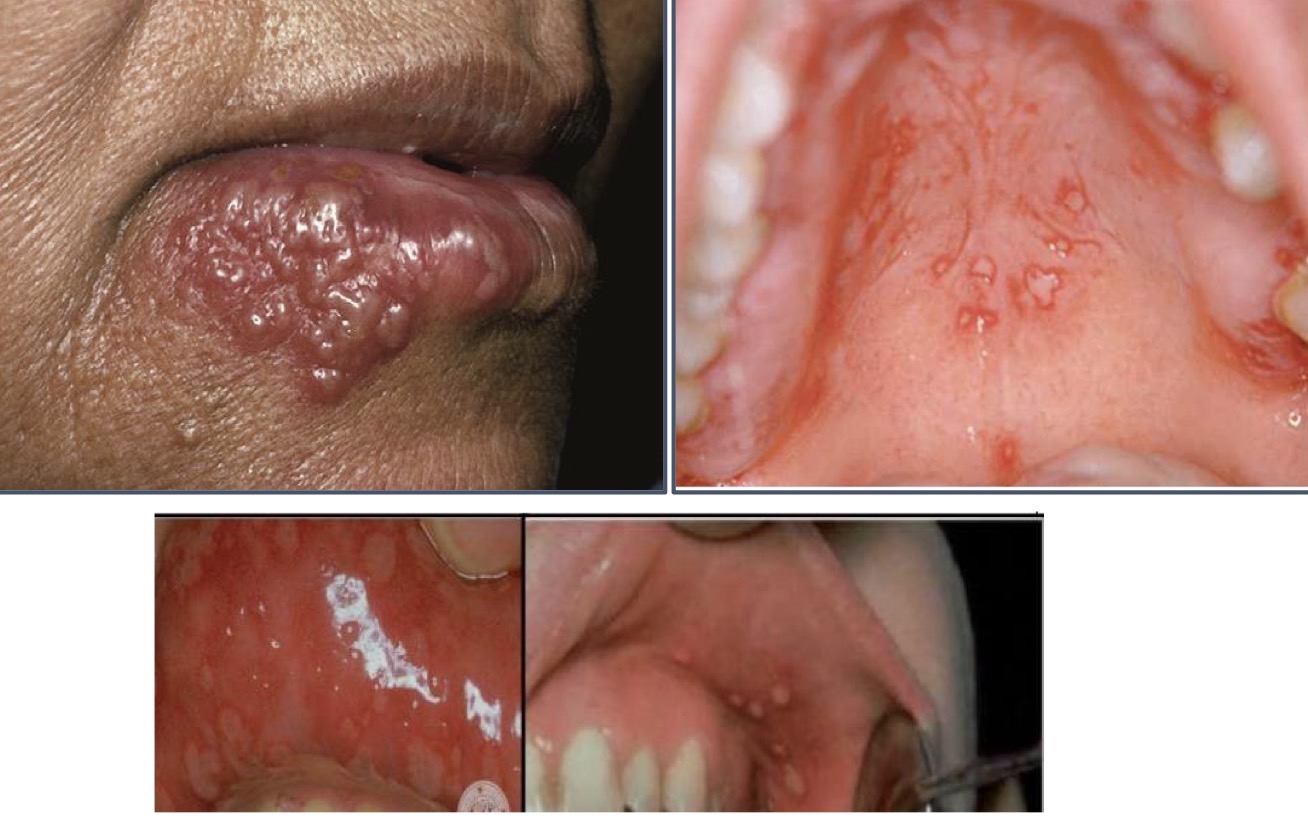
What is primary herpetic gingivostomatitis- who, signs, symptoms, presentations, place, treatment?
Infection of oral cavity by HSV 1
Under 6 yrs- sometimes adolescents and adults
Small spherical grey vesicles, after 24hrs painful ulcers with raised red margin, yellow central portion
Painful, avoid hot foods, lasts 7-10days
Oral mucosal soft palate, pharynx, floor of mouth, tongue, sublingual area
Antivirals- shorten duration and severity, antipyretics, systemic analgesics and analgesic mouthwashes
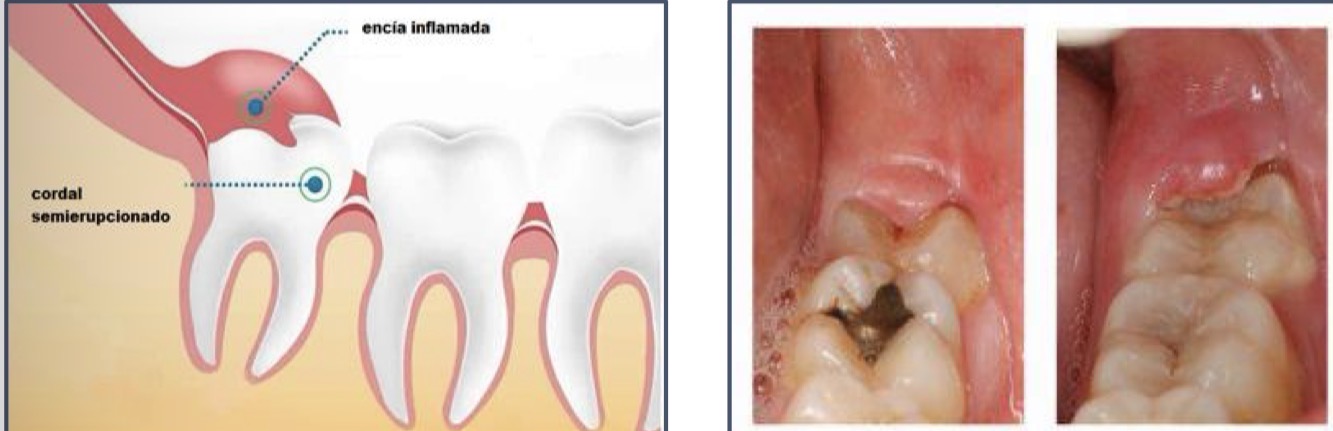
What is pericoronitis- presentations and treatments?
Inflammation of gum and/or alveolar mucosa of partially erupted tooth- mainly in L3M- operculum
Swollen, suppurating, painful red lesion- halitosis, sensitive to touch, may interfere with mouth closure, extraoral swelling in corner, lymohoadenopathy, fever sometimes
ATB therapy, systemic anyipyretics, antiseptic mouthwash- no antibiotics unless fever
What is desquamative gingivitis- injury, place, symptoms, cause?
Gingival erythema, desquamation, severe ulceration of free + inserted gum
Diffuse inflammation reaching mucogingival line
Range from burning sensation to severe pain
Usually dermatological origin