Wk 7 Revision Deck:
1/201
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
202 Terms
what are the functions of the digestive system?
takes in food
breaks food down into nutrient molecules
absorbs nutrient molecules into the bloodstream
rids the body of the indigestible remains
the digestive system falls into 2 main groups, what are they?
alimentary canal or gastrointestinal (GI) tract
accessory digestive organs
what is some characteristics of the alimentary canal or gastrointestinal (GI) tract? what does it do?
a continuous muscular digestive tube that winds through the body
since it is open to the external environment, it is considered to be outside of the body
it digests food and absorbs it through its lining into the blood
what are the accessory digestive organs?
organs that aid in the digestive process
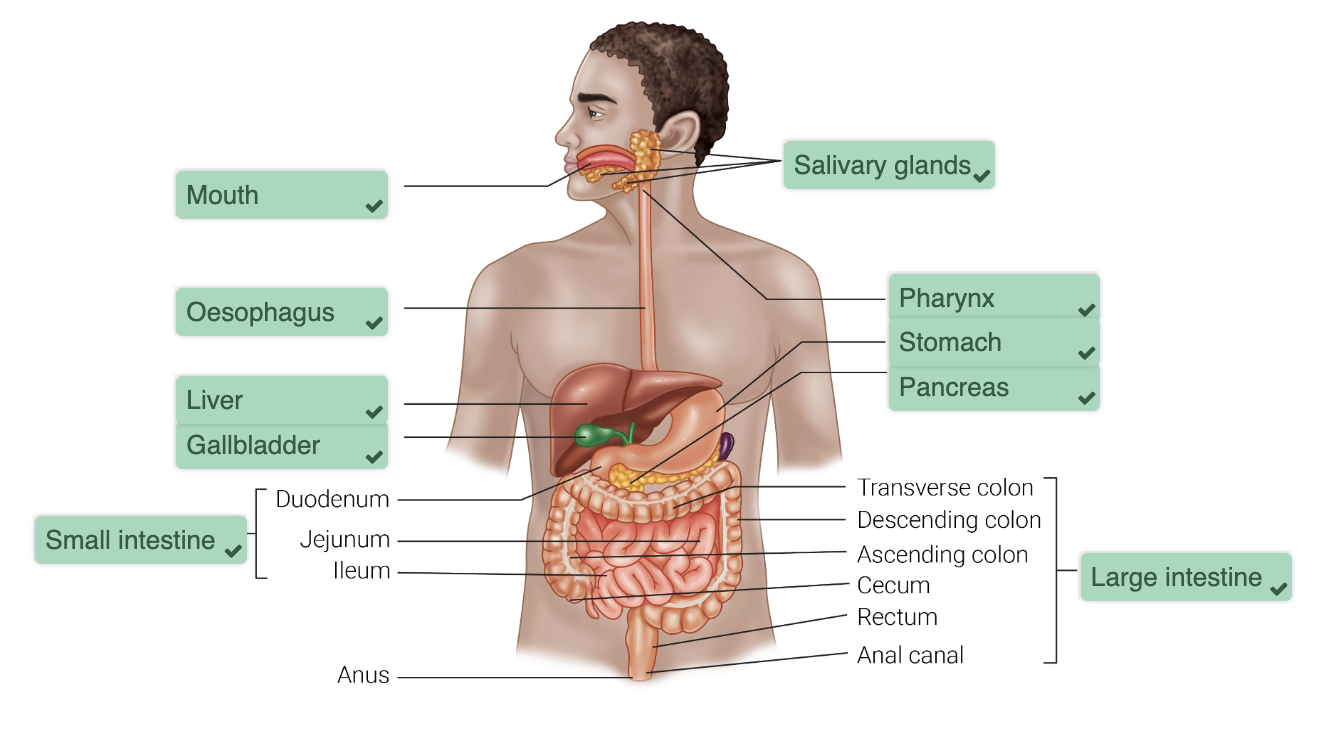
what are all the organs and structures involved in the digestive system?
mouth
salivary glands
pharynx
oesophagus
stomach
pancreas
liver
gallbladder
small intestine
duodenum
jejunum
ileum
large intestine
cecum
appendix
colon
rectum
anal canal
anus
the process of food by the digestive system involves six essential activities, what are they?
ingestion
propulsion
mechanical digestion
chemical digestion
absorption
defecation
what is ingestion?
the process of taking food or substances into the mouth to begin the digestive process
what does ingestion involve?
chewing (mastication)
swallowing (deglutition)
passage of food into the digestive tract
further breakdown and absorption
what is propulsion?
the movement of food and other substances through the digestive tract
what is peristalsis?
involuntary muscular contractions which propel the contents forwards along the length of the gastrointestinal (GI) tract with waves of contraction and relaxation, each wave starts distal to previous
what does peristalsis help with?
mixing and churning the contents of the GI tract while also aiding in the transportation of food from one digestive organ to another
what does a peristaltic contraction involve?
a single ring of contraction that travels down a segment of the GI tract, pushing its contents along
where is peristalsis most notable?
oesophagus
stomach
what is mechanical digestion?
when food is physically broken down into smaller particles, facilitating the subsequent chemical digestion and absorption of nutrients
what are 3 primary locations of mechanical digestion?
mouth
stomach
small intestine
what is the mechanical digestion happening in the mouth?
mastication (chewing and mixing with saliva)
increases the surface area for enzymatic action
what is the mechanical digestion happening in the stomach?
muscular contractions that churn and mix the food with gastric juices
breaks down food into chyme, aiding in nutrient absorption
what is the mechanical digestion happening in the small intestine?
segmentation and peristalsis that further breaks down food and mixes it with digestive enzymes, facilitating nutrient absorption
moves contents toward ileocecal valve
what is chemical digestion?
breakdown of complex food molecules into simpler molecules through the action of enzymes and other digestive substances
what is chemical digestion for?
it allows nutrients to be absorbed and utilised by the body
what are the 3 places where chemical digestion occurs?
mouth
stomach
small intestine
what chemical digestion occurs in the mouth?
the action of enzymes like amylase which breaks down carbohydrates into simpler sugars
what chemical digestion occurs in the stomach?
secretion of gastric juices containing hydrochloric acid and enzymes like pepsin work to break down proteins into amino acids
what chemical digestion occurs in the small intestine?
enzymes from the pancreas and bile from the liver further breakdown carbohydrates, proteins and fats into their component molecules:
simple sugars
amino acids
fatty acids
glycerol
what happens after the chemical digestion in the small intestine is complete?
the nutrients are then absorbed through the intestinal lining into the bloodstream and transported to cells throughout the body for energy, growth and repair
where does the majority of chemical digestion occur?
in the small intestine
what is absorption?
the process by which digested nutrients, along with water and electrolytes, are taken up from the GI tract into the bloodstream or lymphatic system for distribution throughout the body
what is a characteristic of the lining of the small intestine?
excessive folding
to increases surface area of peak absroption
has villi and microvilli
more absorption
what nutrients are absorbed at the small intestine?
the following through simple and facilitated diffusion as well as active transport:
glucose
amino acids
fatty acids
water
electrolytes
what is the absorption of water and electrolytes crucial for?
maintaining fluid balance and electrolyte levels in the body
what is defecation?
the process of expelling indigestible waste, bacteria, and other substances from the body through the anus
what is faeces?
the remaining indigestible material which consists of food particles, bacteria, cellular waster and water
what are the steps of defecation?
faeces accumulate in the rectum
nerve signals trigger the relaxation of the internal anal sphincter
faeces moves into the anal canal
the external anal sphincter, which is under voluntary control, then relaxes
expulsion of faeces from the body
there are several processes that regulate digestive activity, what are they?
neural regulation
mechanical & chemical stimuli
hormones
what is neural regulation in terms of regulating digestive activity?
the GI tract has its own enteric nervous system, sometimes called the “gut brain”
what are the 2 types of reflexes that occur in the enteric nervous system?
intrinsic
short reflexes
extrinsic
long reflexes
what do intrinsic reflexes respond to?
stimuli within the GI tract
mechanical and chemical stimuli, regulating local digestive functions.
the intrinsic nerve plexus of the digestive system is collectively called the “enteric nervous system” consists of 2 plexus. What are they and what do they control?
myenteric plexus
controls the contraction of smooth muscle in the digestive system
submucosal plexus
controls the secretions in the digestive system
what do extrinsic reflexes respond to?
respond to stimuli inside or outside the GI tract
sight, smell, taste or thought of food
what do extrinsic reflexes involve?
CNS centers
autonomic nerves
both sympathetic and parasympathetic nerves
what can extrinsic nerves alter?
activity of intrinsic nerves
hormone secretion
can directly stimulate or inhibit smooth muscles and glands
how do mechanical and chemical stimuli regulate digestive acitivity?
mechanoreceptors and chemoreceptors respond to changes
initiates reflexes that
activate or inhibit digestive glands
stimulate smooth muscle to mix and move lumen content
how do hormones regulate digestive activity?
endocrine cells in the epithelium of the stomach and small intestine can secrete hormones for digestion
what is the role of lips and cheeks for digestion?
help keep food between the teeth when we chew
what is the palate?
the roof of the mouth
what are the 2 parts of the palate and what are their different roles/functions?
hard palate
forms the rigid surface where food is forced during chewing
slightly corrugated to help create friction against the tongue
soft palate
closes off the nasopharyngeal during swallowing
what is the role of teeth in digestion?
mastication and grinding food to break it into smaller pieces
what is the role of the tongue in digestion?
one of the accessory organs of digestion
taste buds for taste information within papillae on the tongue’s surface
gripes the food and constantly re-positions it between the teeth
mixes food with saliva to form a bolus
initiates swallowing
pushing the bolus into the pharynx
what is deglutination?
the process of digestion from intake of food to the bolus entering the stomach
how long does it take solif food to reach the stomach?
8 seconds
how long does it take liquids to reach the stomach?
1-2 seconds
what are the 4 phases of deglutination?
ingestion
buccal phase
pharyngeal phase
oesophageal phase
what happens in the ingestion phase of deglutination?
intake of food
mechanical digestion
teeth
chemical digestion
salivary amylase
lingual lipase
what happens in the buccal phase of deglutination?
propulsion of the bolus into the oropharynx and then laryngopharynx
skeletal muscle layers contract to propel the food
what happens in the pharyngeal phase of deglutination?
epiglottis closes off larynx
bolus moves from larynx to oesophagus by peristalsis
how long is the oesophagus?
25 cm
what happens in the oesophageal phase of deglutination?
bolus moves from oesophagus to stomach by peristalsis
lower oesophageal sphincter opens to allow the bolus to pass into the stomach
what are the functions of the stomach?
intake of food from the oesophagus
temporary storage tank
physical digestion
desaturation of proteins
delivers chyme to the small intestines
what is the mucosal lining of the stomach composed of?
simple columnar epithelial cells that secrete mucous
what are gastric glands composed of?
mucous neck cells
parietal cells
chief cells
enteroendocrine cells
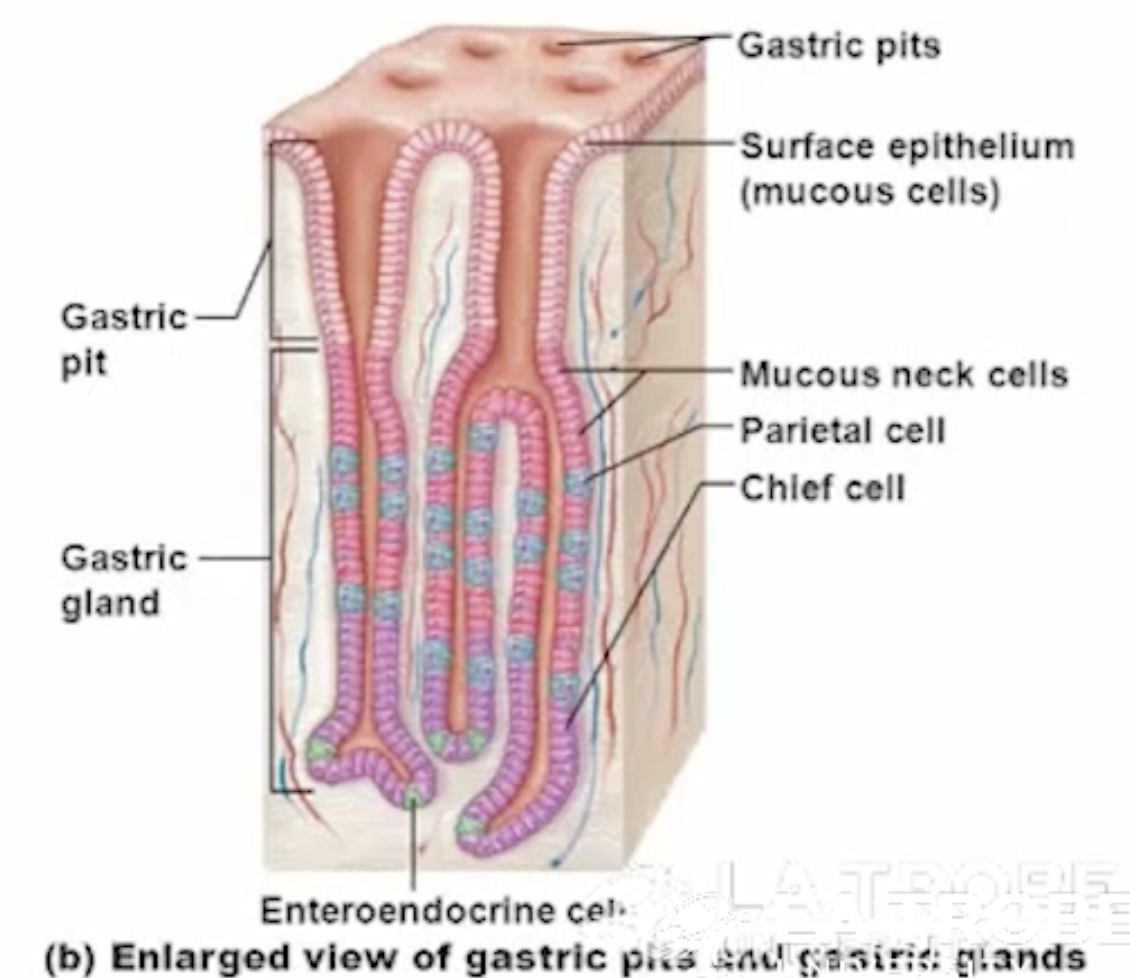
what is the role of the mucous neck cells in a gastric gland of the stomach?
its role is unknown
what is the role of the parietal cells in a gastric gland of the stomach?
secrete HCl
what is the role of the chief cells in a gastric gland of the stomach?
secrete lipase - fat digesting enzymes
what is the role of the enteroendocrine cells in a gastric gland of the stomach?
release chemical messengers that aid in digestion
there are 3 phases in the regulation of gastric secretion, what are they?
cephalic (reflex) phase
gastric phase
intestinal phase
what triggers the cephalic phase?
taste, sight, smell or thought of food
what are the steps in the cephalic phase?
hypothalamus receives info from taste buds/olfactory receptors
medulla stimulated
medulla transmits impulses via vagus nerve
impluses affect secretory and contractile activity of the stomach
what kind of stimuli does the gastric phase have?
hormonal stimuli
neural stimuli
when does gastric phase occur?
once food enters the stomach
what are the 2 parts of the intestinal phase?
stimulatory
inhibitory
when does the stimulatory intestinal phase happen?
as food fills the duodenum
what happens in the stimulatory intestinal phase?
food starts coming into the duodenum
stimulates the mucosal cells in the stomach to secrete gastrin
gastrin encourages the gastric glands to continue their secretory activity
what happens in the inhibitory intestinal phase?
enterogastric reflex
decreases gastric activity
what are the 3 types of gastric contractile activity?
propulsion
grinding
retropulsion
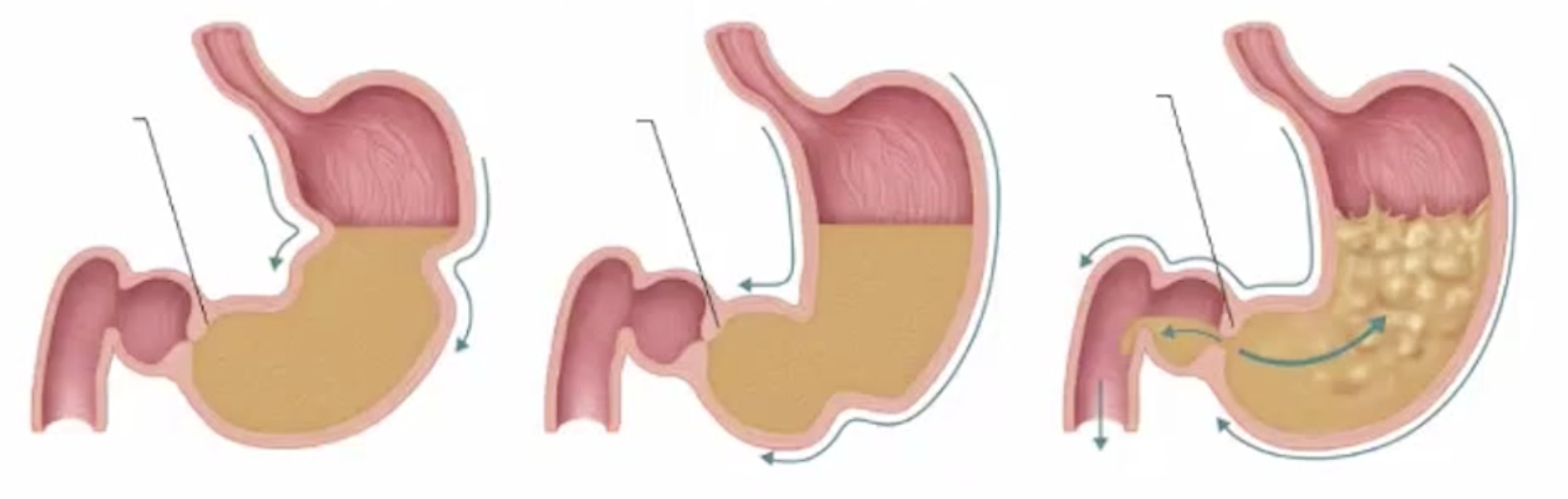
what is propulsion in terms of gastric contractile activity?
peristaltic waves move from the fungus toward the pylorus
what is grinding in terms of gastric contractile activity?
the most vigorous peristalsis and mixing action occur close to the pylorus
what is retropulsion in terms of gastric contractile activity?
the pyloric end of the stomach acts as a pump that delivers small amounts of chyme into the duodenum, simultaneously forcing most of its contained material backward into the stomach
what are 3 accessory organs associated with the small intestine?
liver
gall bladder
pancreas
what is the liver’s function?
to produce bile
what is bile?
a yellow-green solution that contains bile salts and phospholipids which aid in the digestion process
what is the role of the gallbladder?
to store bile and concentrate it by absorbing water and iron
where is bile exported?
the duodenum
what do the bile salts in bile do?
emulsify fats and facilitate fat and cholesterol absorption
what does the pancreas produce?
enzymes that break down all categories of food stuff
what is the name of the exocrine product of the pancreas?
pancreatic juice
what does pancreatic juice contain?
amylases
lipases
nucleases
proteases
what do amylases break down?
carbohydrates
what do lipases breakdown?
lipids
what do nucleases breakdown?
nucleic acids
what do proteases breakdown?
proteins
what else does the pancreas secrete apart from pancreatic juice?
alkaline bicarbonate to balance the HCl produced in the stomach
what are the 4 main layers of the small intestine?
mucosa
submucosa
muscularis external
serosa
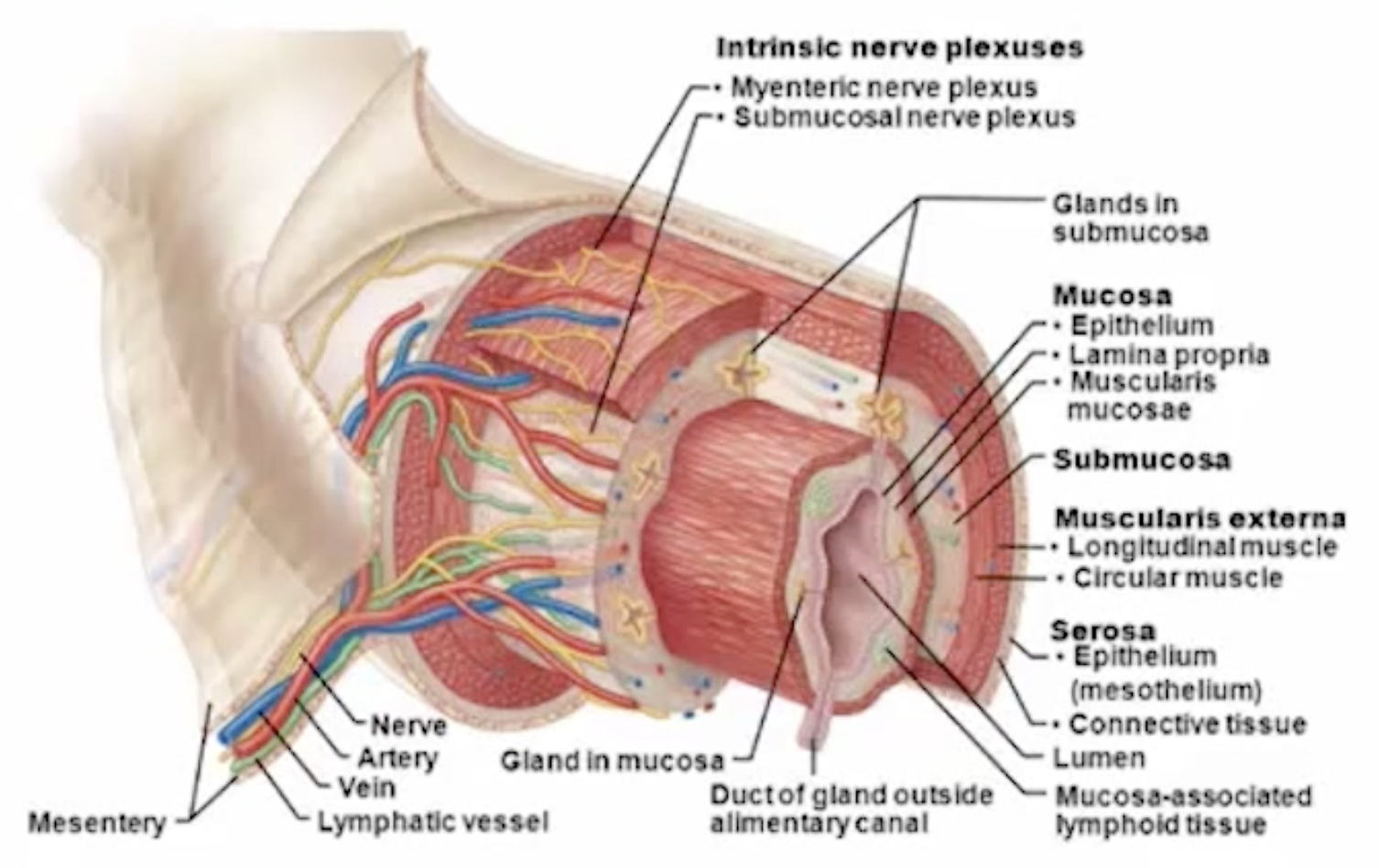
what is the mucosa of the small intestine?
the innermost layer
the mucosa of the small intestine consists of 3 parts what are they?
epithelium
lamina propria
muscularis mucosae
what does the epithelium of the mucosa of the small intestine do?
secretes mucous and digestive enzymes and hormones
what does the lamina propria of the mucosa of the small intestine do?
contains capillaries for nourishment and absorption
what does the muscularis mucosae of the mucosa of the small intestine do?
smooth muscle that produces local movements of the mucosa
what are some characteristics of the submucosa of the small intestine?
external to the mucosa
has a rich supply of blood
location of lymphatic vessels & follicles & nerve fibres
what is the muscularis external of the small intestine responsible for?
segmentation and peristalsis
what is the serosa of the small intestine?
the protective outermost layer