Week 1 CH 1.. write questions
1/55
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
56 Terms
Immunology is the study of the ways that the body protects itself (defense mechanisms) when foreign substances, such as microorganisms, chemicals , and cells enter into the body.
Serology tests are blood tests that look for signs your immune system has responded to an infection. They mainly check for special proteins called antibodies, which your body makes to fight off germs.
If these antibodies are found, it usually means you’ve been exposed to a virus or bacteria—either recently or in the past.
Anti-bodies are good guys
Ab stands for anti-bodies
An antigen is anything foreign that gets into your body and makes your immune system react.
A good way to think of it is a kind of "bad guy" that your body needs to fight.
Immunity = In a host is the condition of being resistant to disease after infection.
Immunization is the process of becoming immune. This can happen naturally, like when you get sick, or artificially, like when you get a shot.
Serology is the study of the serum, which is the clear, cell-free part of blood that remains after clotting. It focuses on non-cellular components —especially antibodies, which are immune proteins floating in the serum.
Non-cellular means it is not composed of, or not containing, cells. These structures lack the basic cell membrane, cytoplasm, or organelles that define cellular
A vaccine is a shot or something similar that helps you become immune to a specific disease without having to actually get sick first.
Vaccines teach your immune system to see a specific agent (antigen) as an enemy. Your body then fights it off and, most importantly, remembers it.
If the real anti-gen ever shows up, your body is ready and can quickly destroy it before you get sick.
To teach your body what a germ looks like, a vaccine can use a few different methods:
Using germs that have been completely killed.
Using germs that have been made very weak.
Using just a small part of the germ, like a protein, that is enough for your body to recognize it.
Louis Pasteur, often called the "Father of Immunology," accidentally discovered the first vaccine.
He noticed that old bacteria didn't make chickens sick. Even more amazing, when he later gave those same chickens a strong, new version of the bacteria, they didn't get sick.
They had become immune. This is because the old bacteria had been weakened (attenuated), which can happen naturally over time or by using heat or chemicals.
Attenuated means weakened
Elie Metchnikoff looked at starfish under a microscope and saw that certain cells were surrounding and eating up any foreign stuff that entered the starfish's body.
He called this process Phagocytosis, and he realized it was a natural way the body fights off invaders.
This type of defense is now known as Natural, Cellular or Innate immunity because you are born with it.
Humoral or adaptive immunity is "adaptive" because
it learns to fight specific threats.
Immune system includes Innate + Adaptive immunity,
both use cell-based and fluid-based tools.
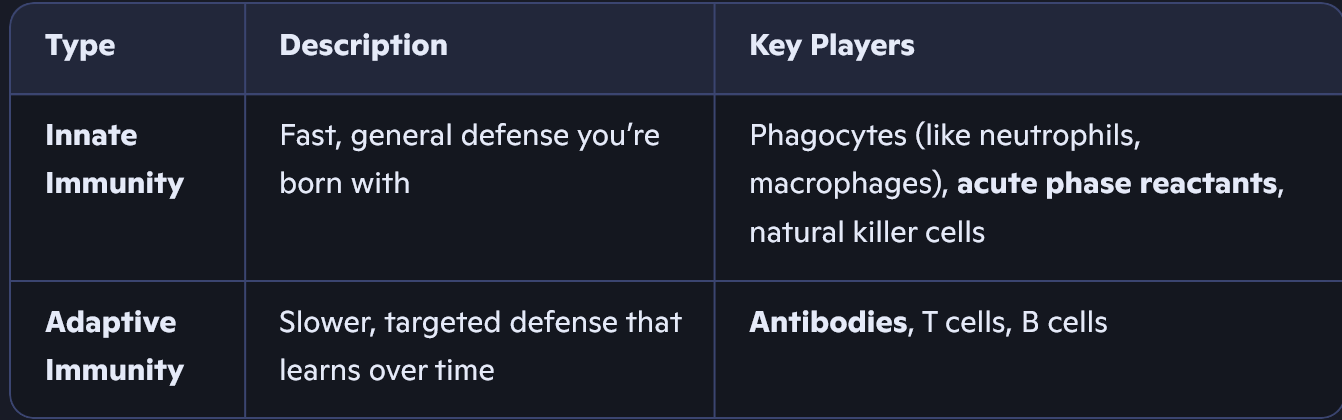
Opsonins are substances in the blood that stick to bacteria, making it easier for immune cells like anti-bodies and acute phase reactants to spot and "eat" them.
Antibodies – proteins that target specific germs
Acute Phase Reactants – proteins that rise during any infection to help the immune system respond quickly

Memorize terminology:
Phagocytosis:
Immune cells eat and break down harmful particles
Opsonization:
The process of coating an invader so immune cells can grab and eat it more easily.
Is also the process by which the charge on the microorganism surface is neutralized, making it easier for phagocytic cells to approach.
Opsonins
Proteins (or molecules) that bind to the microbe and act as the coating in order for phagocytosis to occur
Examples of opsonins are C-reactive protein, complement components, and antibodies
Chemotaxis
Migration of phagocytic cells into infected area due to the presence of acute phase reactants already present
Chemotaxis is the directed movement of immune cells toward a site of infection or injury
Chemotactic factors
chemical signals (like cytokines, chemokines, and acute phase reactants) that attract those immune cells to the area
Innate/Natural Immunity aka Non-specific Immunity
is the the protection you’re born with, working all the time as basic defense
First line of defense against infection.
It doesn’t remember past infections — it responds the same each time.
Includes physical, chemical and cellular barriers like the skin, mucus, stomach acid, and cells like neutrophils
Adaptive / Acquired Immunity (specific / humoral)
Adaptive immunity learns from an infection after exposure and often gives long-term (sometimes lifelong) protection.
It’s very specific to each germ and remembers it, so next time the response is faster and stronger
Both are needed to stay healthy.
Innate immunity
Includes barriers like skin and tears, mucus
Also includes Phagocytes (eating cells) like neutrophils and macrophages that swallow invaders.
Natural killer (NK) cells kill infected or abnormal body cells
Mast cells help start inflammation and recruit other immune cells.
Complement proteins can either tags the invaders, kill them by punching holes in them, or can call for backup
Adaptive Immunity
custom-made response to a specific germ, takes longer to start, and creates memory for next time
APCs (antigen-presenting cells) pick up bits of germ and show them to T cells to begin the adaptive response
The activated T cells can either help B cells make antibodies or directly kill infected/abnormal cells
B cells make antibodies that fit the antigen like a key fits a lock, neutralizing or marking the germ for removal
Anti-bodies
Anti-bodies are the good guys
Antibodies don’t kill invaders directly. Instead, they:
neutralize
tag
or activate complement proteins (these can punch holes into the invaders or trigger inflammation aka call for back up
Anti-gen
foreign substance that invades your body
Babies anti-bodies are from their mother
During Pregnancy IgG antibodies (the most common type) cross the placenta from mother to baby.
White Blood Cells (WBC) aka Leukocytes
• WBC aka leukocytes are found in blood and lymphoid organs (like lymph nodes)
• WBC aka leukocytes help defend the body through two types of immunity:
Innate (fast, general defense)
Adaptive (slow, targeted defense)
Innate immunity includes:
Neutrophils
Eosinophils
Basophils
Monocytes/Macrophages
Mast Cells
Dendritic Cells
NK cells (Natural killer)
What do dendritic cells do?
Dendritic Cells:
Innate Role: They patrol tissues and detect foreign invaders (like bacteria or viruses).
Action: Once they find something suspicious, they engulf it, break it down, and carry pieces (called antigens) to nearby lymph nodes.
Adaptive Role: In the lymph nodes, dendritic cells present these antigens to T cells using special molecules called MHC (Major Histocompatibility Complex).
This activates T cells, which then launch a targeted immune response.
Adaptive Immunity Cells includes
T lymphocytes aka T cells
B lymphocytes aka B cells
Plasma cells
B cells that produce lot of anti-bodies
Different type of B cells but if a B cell makes anti-bodies then they are called plasma cell
🔹 only plasma cells make antibodies
All blood cells (including WBCs) start as Hematopoietic Stem Cells (HSCs) in the bone marrow.
These Hematopoietic stem cells (HSC) split into two main branches:
CMP = Common Myeloid Precursor aka the myeloid line
CLP= Common lymphoid precursors aka the lymphoid line
After CMP, the cells can mature more and become
Monocytes
become macrophages (big eaters)
granulocytes
includes neutrophils, eosinophils, basophils
platelets
helps with blood clotting
erythrocytes (red blood cells)
carries oxygen
After CLP, the cells can mature more and become different types of lymphocytes (depending on where they mature):
T cells: if matures in bone marrow
B cells: if matures in the thymus
How do Hematologist group Cells base on Appearance (Under Microscope)
Polymorphonuclear cells (PMNs) aka granulocytes both include these 3
Neutrophils, Eosinophils, Basophils
Mononuclear cells
Monocytes, Macrophages
Other key cells
Mast cells, Dendritic cells, NK lymphocytes
How do Hematologist group Cells base on location
Cells that circulate in the blood aka peripheral blood
Neutrophils, Eosinophils, Basophils, Monocytes
Tissues
Macrophages, Mast Cells, Dendritic Cells, NK Cells
How do Hematologist group Cells base on function (how they attack the pathogen)
Phagocytic Cells (They eat invaders)
Mononuclear which includes
Monocytes, Macrophages, Dendritic Cells
Polymorphonuclear which includes
Neutrophils, Eosinophils
Mediator cells (release chemicals to help your immune system out) includes:
Basophils, Mast Cells, Platelets, NK Cells
These mediator cells:
Increase vascular permeability aka allow stuff into the blood vessels (to let immune cells in)
Squeeze smooth muscles (like in allergic reactions)
Increase the inflammation response
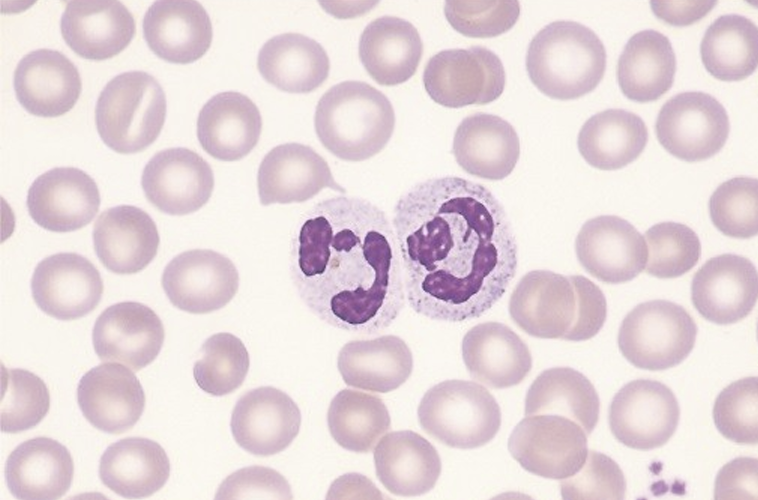
Neutrophils
Nuetrophil is part of the innate immunity:
Make up 50–70% of white blood cells in blood
Main job:
phagocytosis (they eat and destroy invaders)
Have a multi-lobed nucleus (3–6 lobes)
Granules in their cytoplasm don’t stain strongly—they look neutral
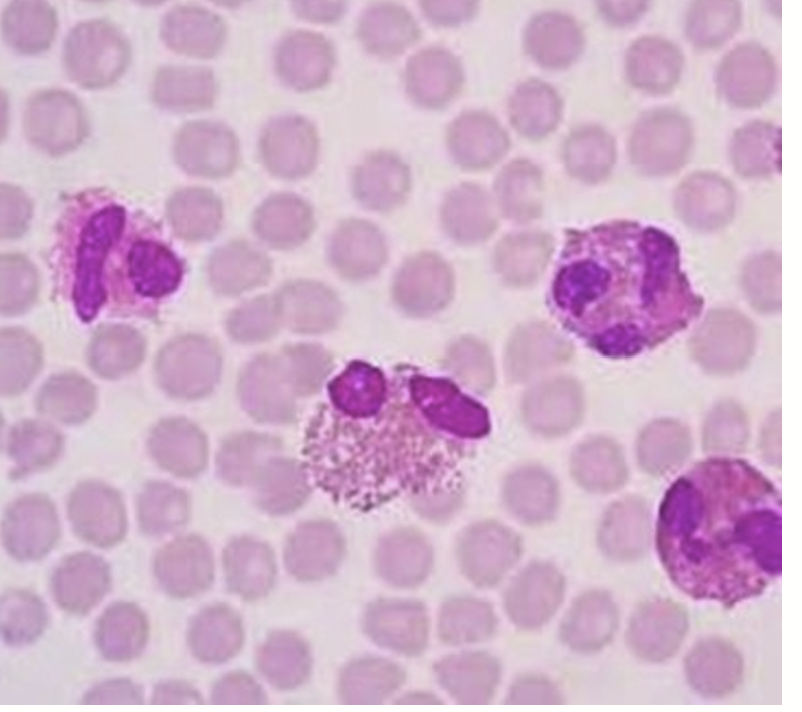
Eosinophil
Eosinophil is part of the innate immunity
Nuclweus is bilobed (2 lobes) or oval-shaped
Granules are red-orange in color
Functions include:
Phagocytosis
Neutralizing allergy-related chemicals
releases chemical to help with allergy
Killing parasites
Releasing cytokines (chemical messengers to guide immune response)
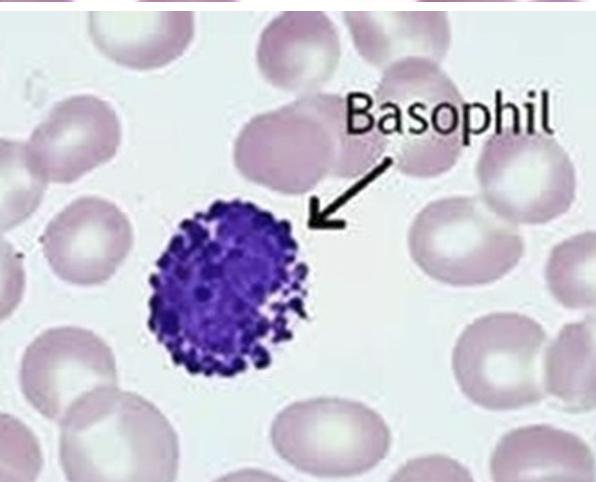
Basophil
Innate Immunity Cells - Basophils
Have a 2-lobed nucleus and deep blue-purple granules
Granules release histamine and heparin → these chemicals trigger and maintain allergic reactions
They bind IgE antibodies, which are made during allergies
Monocytes
Innate Immunity Cells - Monocytes
Largest WBCs with a horseshoe-shaped nucleus and gray-blue cytoplasm
Contain digestive vacuoles and fine granules
Main jobs:
Phagocytosis (they eat invaders)
Release digestive enzymes to break down what they consume
They’re precursors to macrophages
once monocytes enter tissues, they mature into macrophages (the cleanup crew)
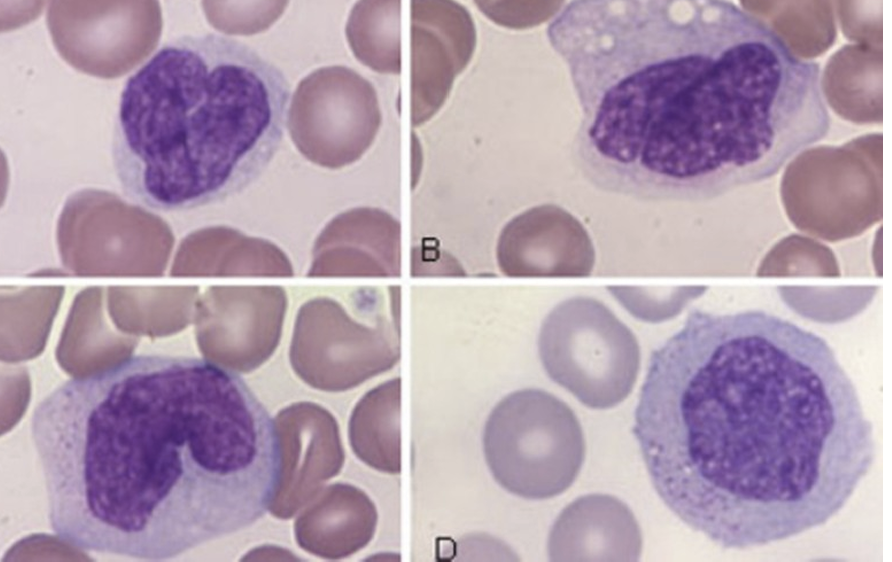
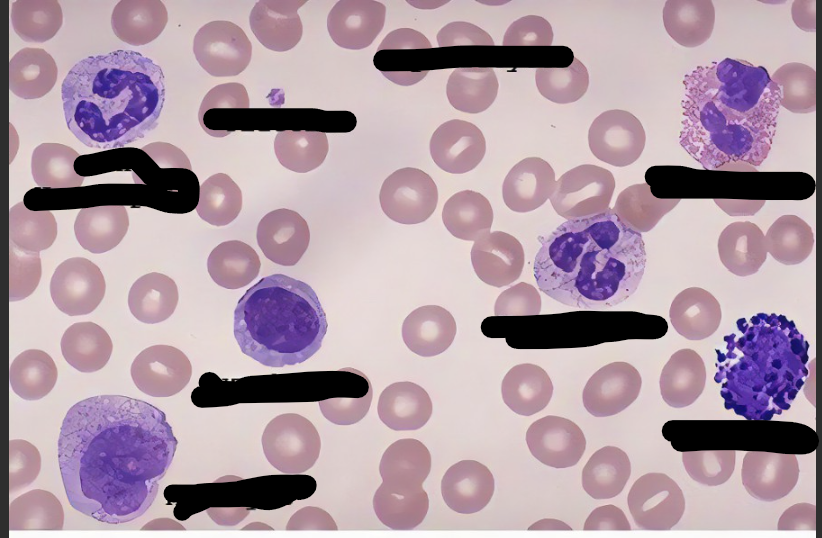
Label
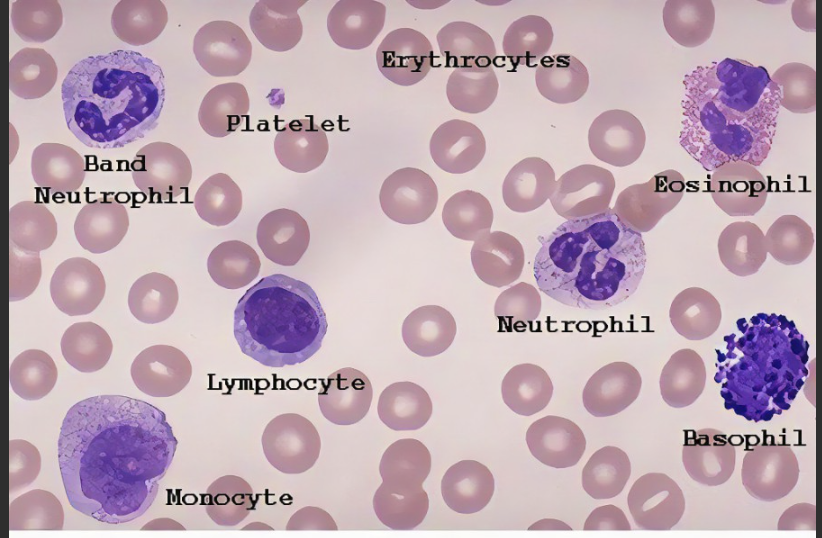
Macrophages
Innate Immunity Cells: Macrophages
Macrophages start as monocytes (a type of white blood cell) but once they move into the body tissues, they transform into macrophages
Macrophages are
bigger then monocytes
Macrophages have more vacuoles inside them
Innate immune functions for macrophages
Phagocytosis (eat and digest) and microbial killing
They can attack and kill cancer cells.
They can destroy parasites that live inside cells.
They release chemical signals to alert and guide other immune cells.
Adaptive immune functions for macrophages
They break down germs and show the pieces (antigens) to T cells so the body learns to fight them better.
They release cytokines (messenger proteins) that control how strong or weak the immune reaction is.
Mast Cells
Innate immunity for Mast Cells
Resembles basophils but comes from a different lineage
Mast cells are bigger and filled with more granules (tiny packets of chemicals) than basophils
Mast cells live in many tissues in the body like skin, lungs, gut, and bladder, making them common all over.
They cause and keep allergic reactions going.
They cause allergy symptoms (hypersensitivity reactions) because IgE antibodies stick to them, making them release histamine and other chemicals.
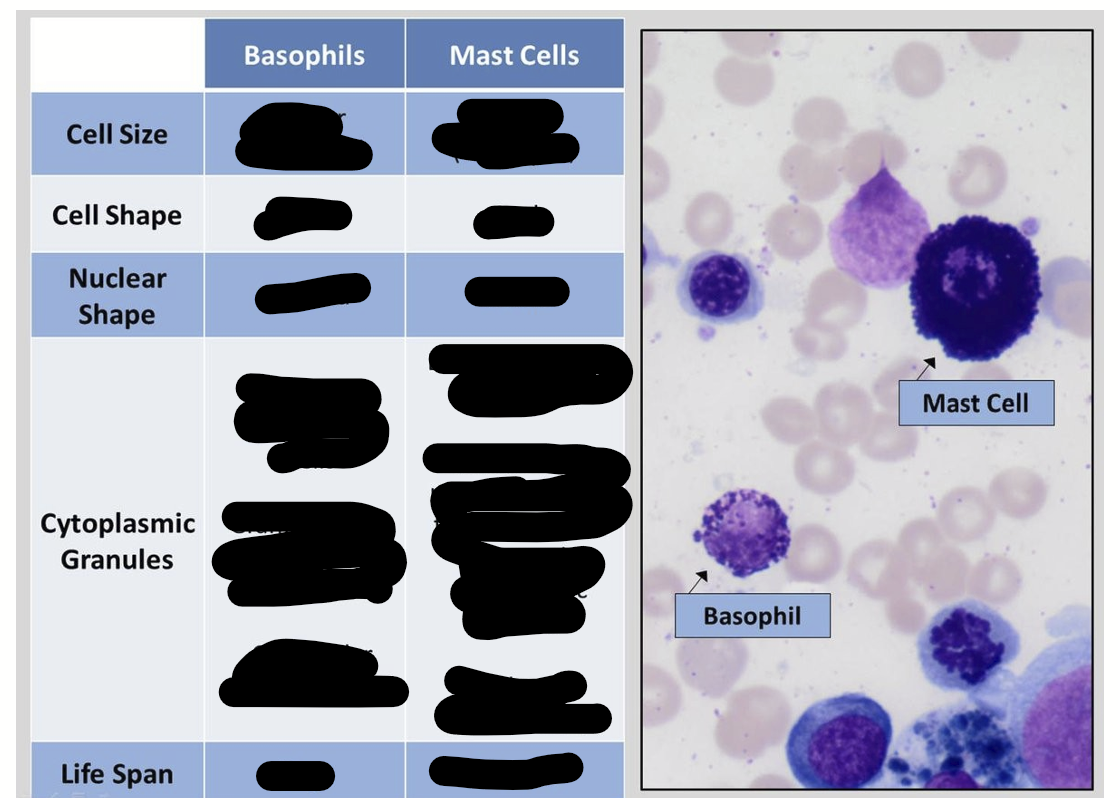
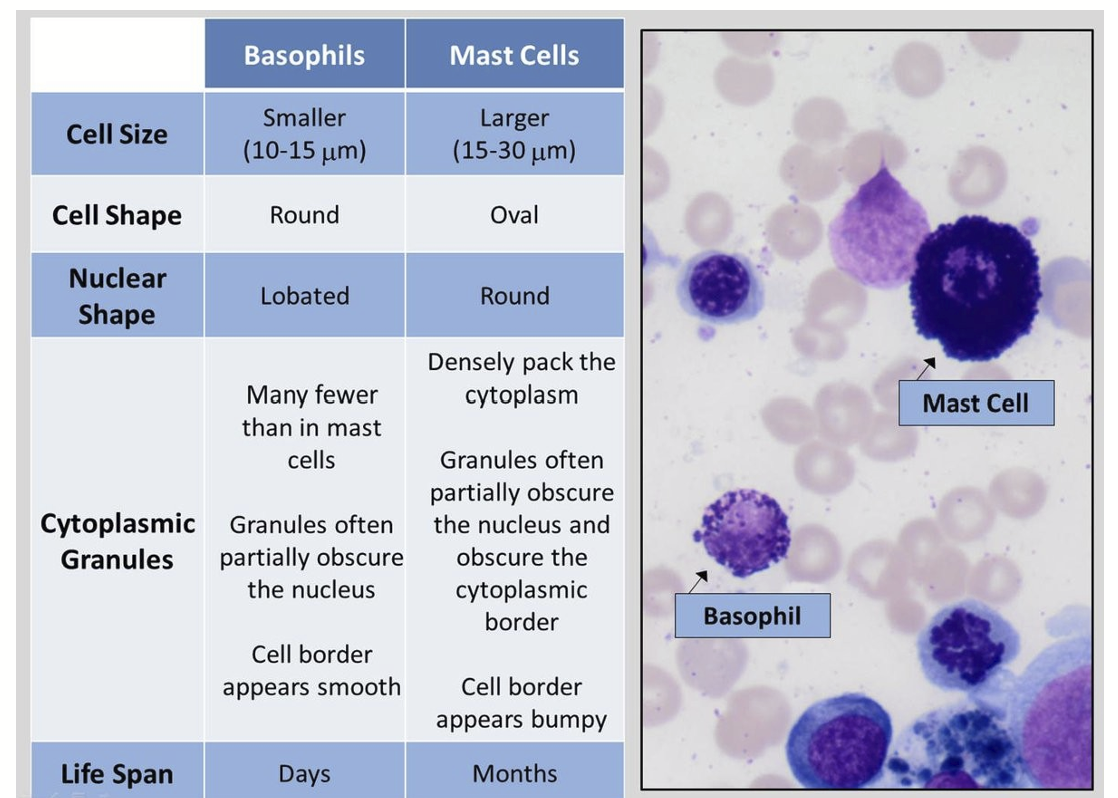
vacuoles vs granules
Dendritic cell
Dendritic cells for innate immunity
Made in the bone marrow
Travel to tissues to look for invaders
Use long arms to grab antigens
Then move to lymph nodes to activate T cells
Dendritic cells are grouped by where they're found in the body and by certain markers on their surface.
Dendritic cells also act as messengers between Innate & Adaptive Immunity.
Dendritic cells are the best at eating germs (phagocyte cell) and the most powerful antigen-presenting cell (APC) aka showing antigens to T cells.
Natural Killer (NK) lymphocytes
Natural Killer (NK) lymphocytes for innate immunity
Natural killer (NK) cells are a group of innate lymphocyte cells with kidney shaped nucleus and granular cytoplasm
NK make up about 10-15% of lymphocytes in the blood.
NK are made in bone marrow and move to immune organs like tonsils, lymph nodes, and spleen.
NK lymphocytes have no unique marker, but they usually express CD16 and CD56
CD16 and CD56 are surface antigens—proteins on the cell’s surface
Scientists use antibodies that bind to CD16/CD56 to detect NK cells
Continue on with NK cells lymphocytes
NK cells are the first line of dense against virus infected cells
Are called NK cells because NK cells can kill cancer or virus-infected cells without needing to "learn" about them first.
NK cells don't phagocytes (eat) cells; instead, they kill them directly through a process called cytotoxicity.
NK cells kill by making cell to cell contact with the target cell.
NK cells punch holes (create pores) in the target cell and send in toxic granules, making the cell burst and die.
NK cells also release cytokines that enhances both fast (innate) and specific (adaptive) immune defenses.
Platelets
Platelets for innate immunity cells
Platelets are tiny cells without a nucleus, and are derived (made) from megakoryocytes in the bone marrow.
Platelets main job is to stop bleeding by forming clots.
In allergic reactions, platelets can release histamine and other chemicals from their granules, which can cause tissue damage.
Time for adaptive immunity
Lymphocytes
Lymphocytes are part of the adaptive immunity cells
Lymphocytes make up 20-40% of white blood cells.
Lymphocytes are small WBC's with a large, round nucleus, and little, light blue cytoplasm.
Under a microscope, all lymphocytes look the same, so we tell them apart using flow cytometry (a test that looks at surface proteins called CD markers).
B cells -
Make antibodies.
T cells -
Help control immune responses and kill infected cells.
Natural killer (NK) cells -
Kill virus-infected and cancer cells without prior exposure.
lymph is short for
What are CD markers?
Lymphs is short for lymphocyte
CD markers (special proteins on cell surfaces), which helps scientists tell different immune cells apart.
Memorize these CD markers
T cells:
CD3 - Found on all T cells (basic T cell ID tag).
CD4 - helps to identify Helper T cells
CD8 - helps to identify Cytotoxic (killer) T cells
Memory trick:
3 for all T Cells, 4 helps, 8 kills.
B Cells:
CD19 - Main B cell marker.
CD21 - Works with CD19 as a co-receptor.
NK Cells
CD16 - Helps NK cells grab antibody-coated targets.
CD56 - Main NK cell marker to identify NK cells
B lymphocytes
B lymphocytes are part of the adaptive immunity
B lymphocytes aka B cells
B cells mainly make antibodies that help fight infections.
B-Cells have surface protein markers called: (CD19, CD20, CD21,
and MHC II).
B cells fully develop (mature) in the bone marrow.
When a B cell meets a germ (antigen), it changes into a plasma cell, which makes antibodies.
Plasma Cells
Plasma Cells are part of the adaptive immunity
Plasma cells have off-center oval nuclei and their job is to release antibodies.
Plasma cells represent the end stage of B lymphocyte lineage.
Plasma cells make and release antibodies (also called immunoglobulins).
B cell finds an antigen and grabs it.
Helper T cell gives a signal to confirm it’s a real threat.
B cell activates and multiplies into many copies.
Some copies become plasma cells that release antibodies to fight that specific antigen.
❓Why does the B cell need the T cell’s signal?
Think of it like two-factor authentication for your immune system:
The B cell says: “I found something suspicious!”
The T cell checks and says: “Yep, that’s dangerous — go ahead!”
This extra checkpoint helps prevent false alarms and autoimmune mistakes, like attacking your own body by accident.
Ag stands for antigen
antigen is any foreign molecule that enters your body
T lymphocytes
T Lymphocytes aka T cells are part of the adaptive immunity
T cells finish developing in the thymus gland, and all of them carry a marker called CD3+.
There are different types of T cells, each with its own job.
Helper T lymphs/Cell (Th; CD4+) send out signals (cytokines) that help B cells make antibodies and also help other T cells fight infections.
Regulatory T lymphs/Cell (Treg; CD4+) tells the immune system to calm down once the infection is under control.
Cytotoxic T lymphs/Cells (Tc; CD8+) directly attacks and kill cancer/tumor cells or cells infected with viruses.
All of these T Lymphs/Cells can attack transplanted organs over time, causing chronic rejection.
Mature T lymph/Cells can survive for several months or years, whereas the average life span of the B lymphs/Cells is only a few days.
The immune system needs many different types of lymphocytes to fight many threats.
T Lymph/Cell Response:
When your body detects a new threat (antigen), specific T cells multiply rapidly — up to 1000 times!
This multiplication is called clonal expansion — like building an army.
After the threat is gone, most of those T cells die off — that’s the contraction phase.
Only a small group (less than 10%) stick around as memory T cells, ready to respond faster next time.
After the immune response is over and the infection is gone, most antigen-presenting cells (APCs) and activated T cells die off
As we get older, the body makes fewer new lymphocytes, but overall the total number of B and T lymphs/cells stays about the same
Low T cells is called lymphopenia
Naive lymphocytes (those not yet exposed to an antigen) move freely between the blood and secondary lymphoid organs through lymphatic ducts.
This movement allows the lymphocytes to come in contact with antigens(Ag) and to spread memory cells all over the lymphatic system
Lymph fluid, lymphocytes, and antigens enter a lymph node through the afferent duct (entry point).
After being filtered and checked, they exit through the efferent duct (exit point).
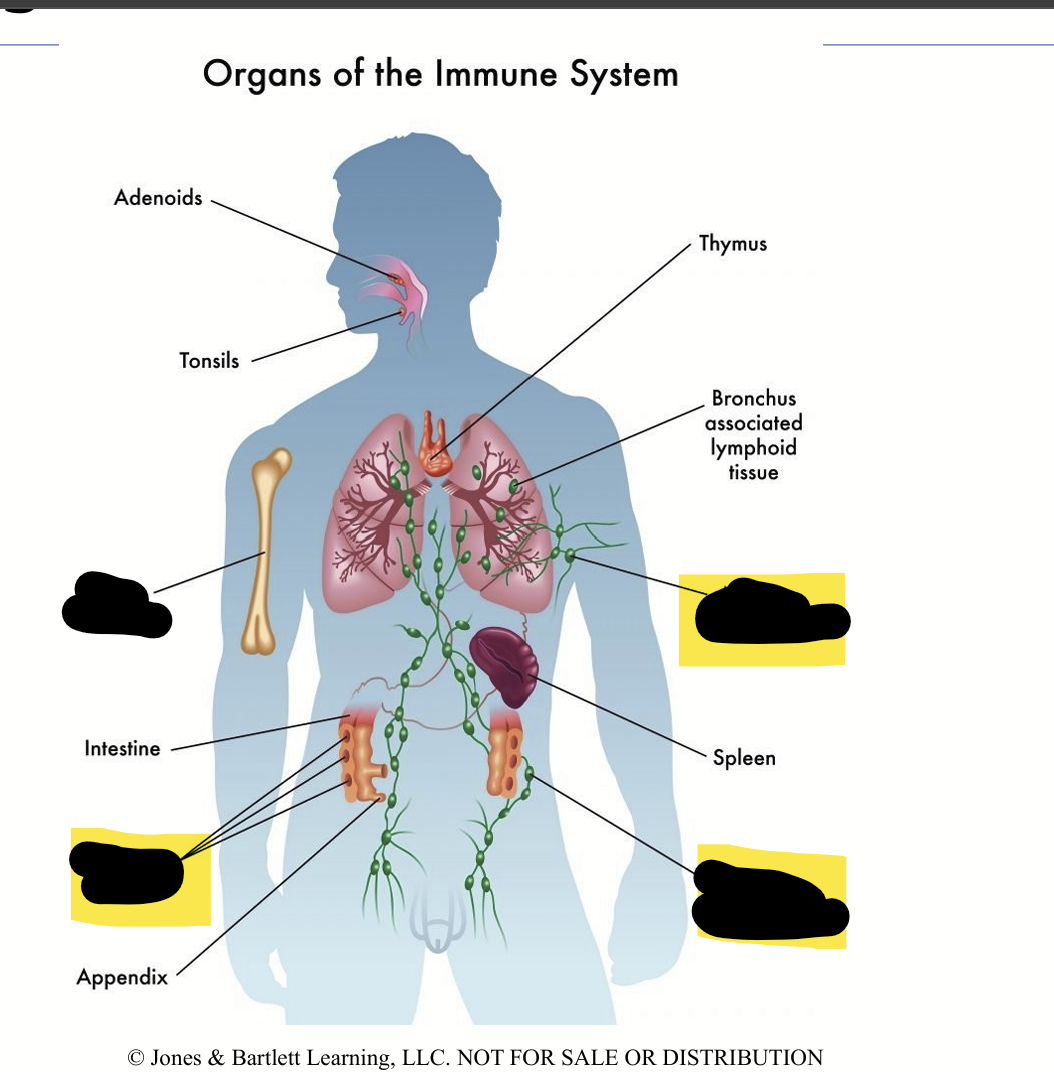
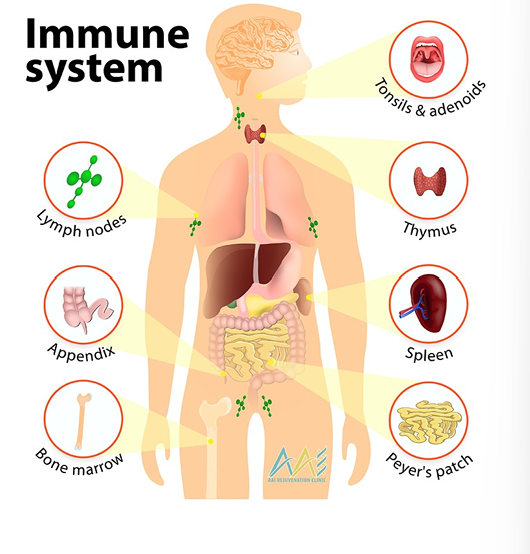
Main secondary lymphoid organs:
Lymph nodes — tiny checkpoints scattered throughout the body
Axillary lymph nodes are a specific group of lymph nodes located in your armpits (axilla)
Spleen — filters blood and catches blood-borne antigens
MALT (Mucosa-Associated Lymphoid Tissue) — includes tonsils, Peyer’s patches in the gut, etc.
Lymphatic Node:
A small, bean-shaped checkpoint
Role includes: Filtering lymph fluid and checks for invaders
Lymphatic Duct
A tube or vessel, is like a highway for lymph fluid
Role includes: Carrying lymph fluid between nodes and tissues
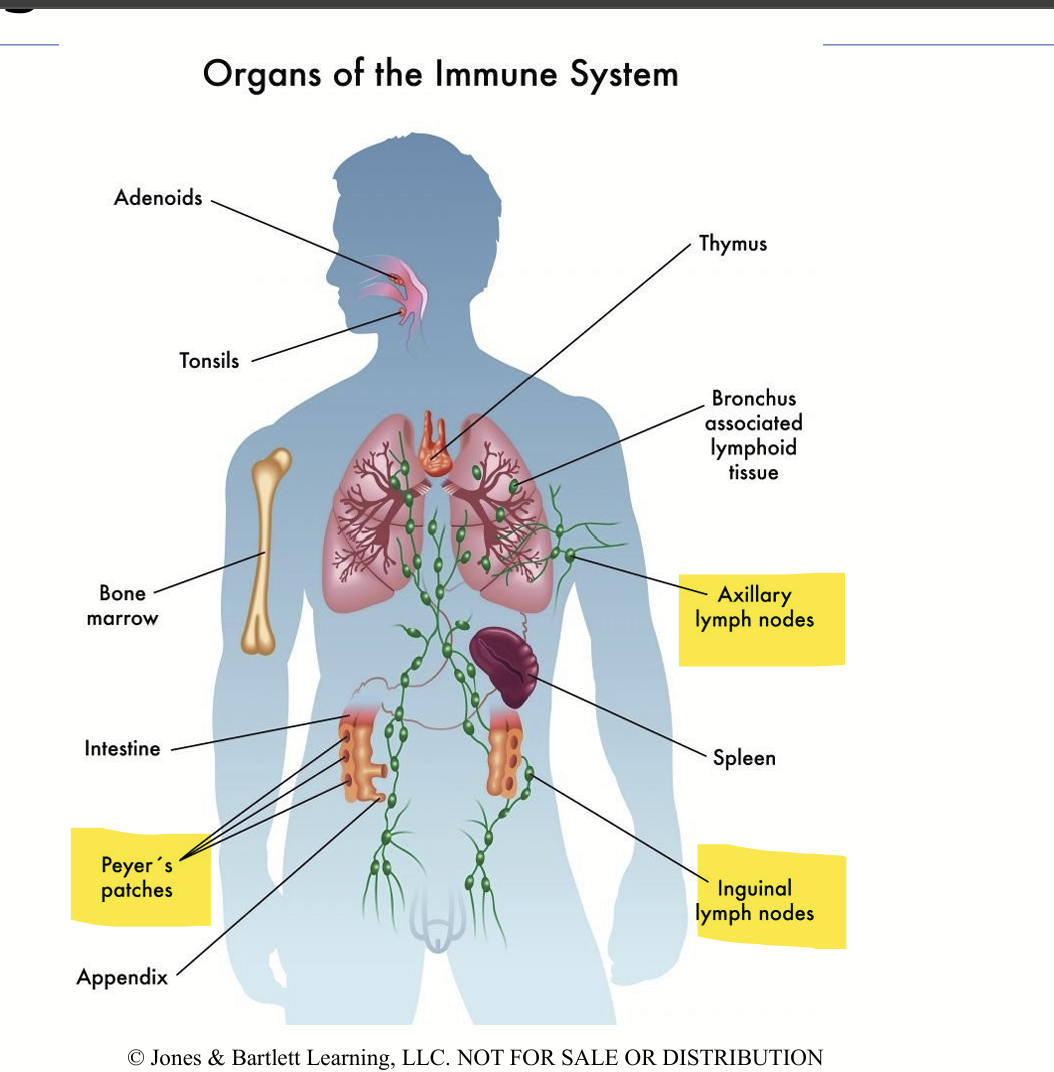
Organ of the Immune system: Primary lymphoid organs
Primary lymphoid organs where B and T lymph/Cells mature:
Bone marrow
Thymus
Bone marrow produces hematopoietic stem cells which are the master cells that can turn into many types of blood cells.
These hematopoietic stem cells can develop into:
Red blood cells (carry oxygen)
White blood cells (fight infection — includes lymphocytes, monocytes, granulocytes)
Platelets (help with clotting)
Lymphocytes (B cells; T cell)
B cells/Lymph fully mature in the bone marrow.
T Cells/Lymph mature in the thymus.
Organ of the Immune system: Secondary lymphoid organs
Secondary lymphoid organs
These secondary lymphoid organs receive mature lymphocytes (B and T lymph/Cells) from primary lymphoid organs.
These matured B and T lymph/Cells are placed where they can meet anti-gens
Some placement sites include:
Spleen
Lymph nodes
Mucosal-associated lymphoid tissue (MALT)
Cutaneous-associated lymphoid tissue (CALT)
Biggest secondary lymphoid organ:
The spleen is the biggest secondary lymphoid organ.
The "red pulp" part of the spleen has many macrophages that clean out and recycle old red blood cells.
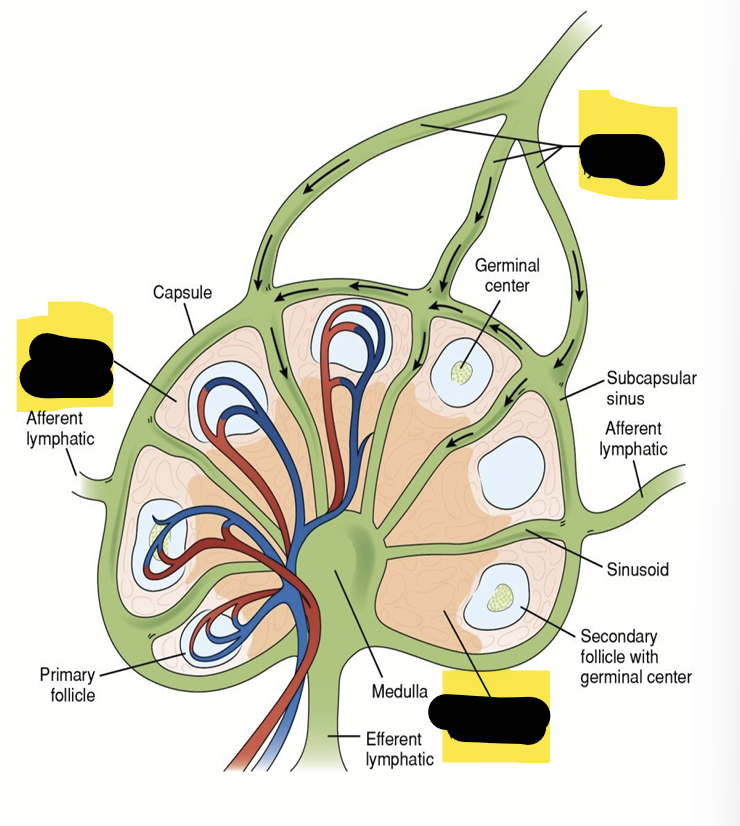
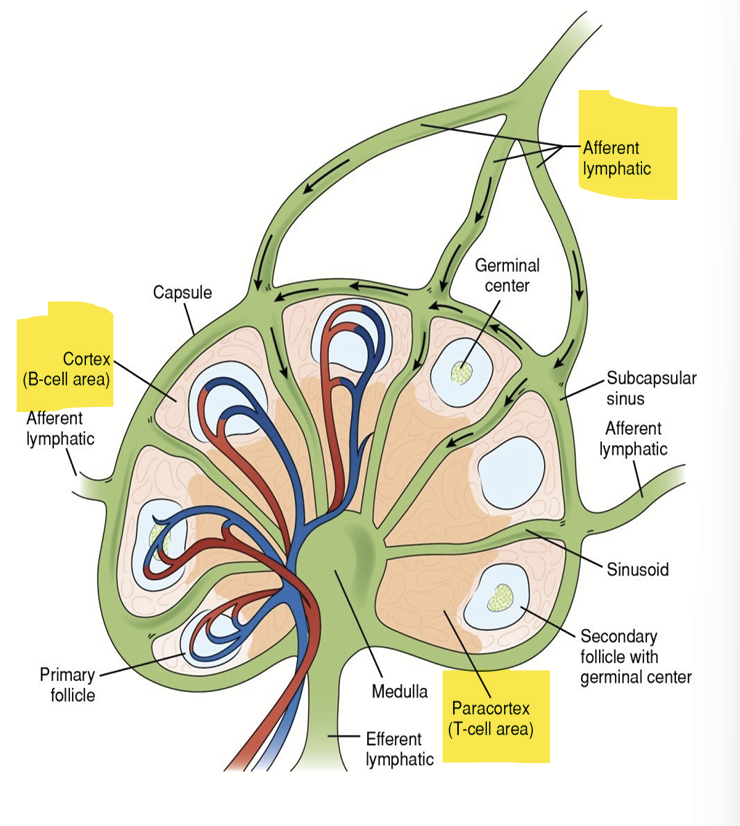
Lymph Nodes
Lymph Nodes are located along lymphatic ducts, especially near joints and where arms and legs join the body
Lymph fluid, with white blood cells and germs, flows into the lymph node through the afferent vessel.
B lymph/cells cluster in round "follicles" in the outer part of the node (the cortex).
T cells are found mostly in the middle zone of the node (paracortex).
Mucosal-associated lymphoid tissue (MALT)
Mucosal-associated lymphoid tissue (MALT) is an immune tissue found in the gastrointestinal (gut), respiratory (airway), and urogenital tracts (urinary tract)
Since germs often enter through these areas, MALT is a first defense and has numerous macrophages and lymphocytes present.
Examples of MALT are tonsils, appendix, and patches of tissue in the small intestine.
Cutaneous-associated lymphoid tissue (CALT)
CALT is the immune defense in the skin, containing T cells, monocytes, macrophages, and dendritic cells
Innate immunity are the natural defenses you're born with. They act fast but are not specific to one germ.
Adaptive immunity are learned defense. It targets specific germs, remembers them, and uses B & T lymphocytes.
All blood cells arise from hematopoietic stem cells in the bone marrow.
The 5 main white blood cells (WBC) are neutrophils, eosinophils, basophils, monocytes, and lymphocytes.
all can enter tissue if need to
Immune cells in tissues are mast cells, dendritic cells, and macrophages.
These are like permanent guards
The "eating" cells of innate immunity are neutrophils, monocytes, macrophages, and dendritic cells.
Lymphocytes (B & T cells) are the main players in adaptive immunity.
B lymph/cells grow and mature in the bone marrow.
When B cells meet a germ, they turn into plasma cells that release antibodies against that germ.
T lymph/Cell consist of three major subtypes:
helper T cells (Th),
cytotoxic T cells (Tc),
regulatory T cells (Treg).
Natural Killer (NK) cells destroy virus-infected or cancer cells without previous exposure
Bone marrow (B cells) and thymus (T cells) are where lymphocytes finish maturing.
Lymphocytes meet anti-gen in secondary organs like spleen, lymph nodes, MALT, and CALT.
Student Learning Outcomes
• Match the common terminology of Immunology with the appropriate definition.
• Describe the 3 different ways in which vaccines can be made from pathogens.
• Describe the relationship between the use of vaccines and the growth of Immunology.
• Distinguish between innate/natural and adaptive/acquired immunity.
• Differentiate the appearance and function of the cells involved in innate and adaptive immunity.
• Describe the types of WBC’s capable of phagocytosis.
• Identify the body sites populated by T & B lymphocytes and compare the life span of the T & B lymphocytes.
• Differentiate the functions of the 3 major categories of lymphocytes.
• Describe the antigen activation of B lymphs and the maturation path for plasma cells.
• Recognize the characteristics of plasma cells and describe their function.
• Match common CD markers with the appropriate lymphocyte category.
• Describe the primary & secondary lymphoid tissues and their roles in T & B lymphocyte & plasma cell development