Exam 3 Pathophys - Resp, GI, Liver, Renal
1/106
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
107 Terms
Is the apex of the lungs the top or bottom?
Top (superior most)
How many lobes do the right and left lungs have?
Right - 3
Left - 2
Family of viruses that contribute to colds?
Rhinovirus, parainfluenza viruses, syncytial viruses
Signs and symptoms of colds?
- Clear, watery secretions
- Red, swollen mucous membranes, sore throat, hoarseness w pharynx/larynx involved
- Headache, malaise, fever and chills
Definition of Rhinosinitis?
- Obstruction of ostia draining sinuses
- Infections (Viral or bacterial), allergies, nasal polyps, decongestant abuse
Acute, subacute, and chronic time frame for rhinosinitis?
Acute - Viral (5-7 days), Bacterial (Up to 4 weeks)
Subacute - 4-12 weeks
Chronic - >12 weeks
Signs and symptoms of Rhinosinitis?
- Purulent discharge
- Facial pain
- Headache
- Fever
Viral influenza characteristics?
- Upper respiratory track infections, loss of mucus secreting and ciliated cells, watery discharge
- Lower tract: Shedding bronchial + alveolar cells
Signs/Symps for Viral influenza?
- Abrupt fever/chills, headache, muscle ache, profuse + watery nasal discharge, dry cough, sore throat
- Symps peak day 3-5 then gone day 7-10
Goals for influenza with rest, warmth, and fluids?
Rest - Lower resp. rate/depth for less spreading to lower resp tract
Warmth - Slows viral replication
Fluids - Hydration of epithelial cells
Hemagglutinin and Neuraminidase receptor functions?
Hemagglutinin - Entry into cell
Neuraminidase - Release out of cell
What distinguishes Influenza from Rhinosinitis?
The rapid onset of malaise = Influenza
Purulent nasal discharge = Rhinosinitis
COVID characteristics?
- Community spread droplet respirations
- Uses ACE2 for entry (also expressed in heart, intestines, kidneys, gall bladder for bp)
Signs/Symps of COVID?
- Fever, fatigue, chills, dry cough, myalgias, diarrhea
Lung dysfunction of COVID?
- Covid specifically attacks AT2 cells in lungs
- Leads to lack of secretion of surfactant, trans-epithelial water movement, and regeneration of epithelial cells
Pneumonias characteristics?
- Inflammation of parenchyma (Alveoli and bronchioles)
- Common etiology: Pseudomonas, S. aureus
Signs/Symps of Pneumonias?
- Cough (Thick and colored), fever, chills, pleuritic chest pain (pain with breathing), tiredness, weakness, muscle aches, noisy breathing, SOB
Pneumonia classification?
Type of agent
- Atypical = viral/fungal
- Typical = Bacterial
Distribution of infection
- Lobar pneumonia = A part of of or all of a single lobe
- Bronchopneumonia = More than one lobe
Setting where acquired
- Community = outside of hospital/long term care facility
- Nosocomial = In hospital/long term care facility
Consolidation term definition?
- Alveoli filled w/ bacteria, pus, and exudate
Anaplasia definition?
Loss of specialization of cell = promotes cancer cell growth
Carcinoma vs sarcoma?
Carcinoma - Started in epithelial tissue
Sarcoma - Started in Mesenchymal tissue (Anything besides epithelial)
Bronchogenic carcinomas characteristics?
- Aggressive, invasive, metastatic tumors
2 Types of bronchogenic carcinomas?
- Small Cell Lung carcinoma (SCLC)
- Non-Small cell lung carcinoma (NSCLC)
Small Cell Lung Carcinoma characteristics?
- Strongly associated w smoking
- Small, round, oval cells that grow in clusters
- Highly malignant (infectious)
Treatment = Radiation + chemo
Non-Small Cell Lung Carcinoma characteristics?
- Squamous starts in central bronchi
- Adenocarcinoma starts in alveoli
(Associated w non-smoking common type)
Treatment = Surgery, radiation, and chemo
Signs/Symps of Bronchogenic carcinomas?
- Chronic cough, SOB, wheezing, blood in sputum (Hemoptysis), Insidious onset (smoking + bronchitis), anorexia, occasional endocrine effects
Tidal volume definition?
- Normal, passive inhale + exhale volume
Residual volume definition?
- Air left in lungs after forceful exhale
Vital capacity definition?
- Total volume inhaled and exhaled forcefully
Total inspiratory Capacity definition?
- Tidal and inspiratory capacity
Functional residual capacity volume?
- Expiratory reserve + forceful exhale volume
Pleural effusion characteristics?
- Abnormal fluid in pleural cavity
Hydrothorax - Watery serous exudates
Chylothorax - Lymph fluid
Hemothorax - Blood
Pneumothorax characteristics?
- Air trapped in pleural cavity
Spontaneous - Without cause/injury
Traumatic - Injury caused to chest walls/airways (lungs pull away)
Atelectasis definition?
- Incomplete expansion of lung due to obstruction, compression, or increased recoil
Signs/symps of Atelectasis?
- Tachypnea, Hypoxia, Shallow breath sounds
Difference between extrinsic (Atopic) and intrinsic asthma? What causes each?
Extrinsic (Atopic)
- Hypersensitivity to antigen (type 1)
Cause: Dust, Animals = any allergen
Intrinsic
- Initiated by non-immune mechanisms
Cause: Respiratory Tract Infections, Exercise
Pathway of Bronchial Asthma Pathogenesis?
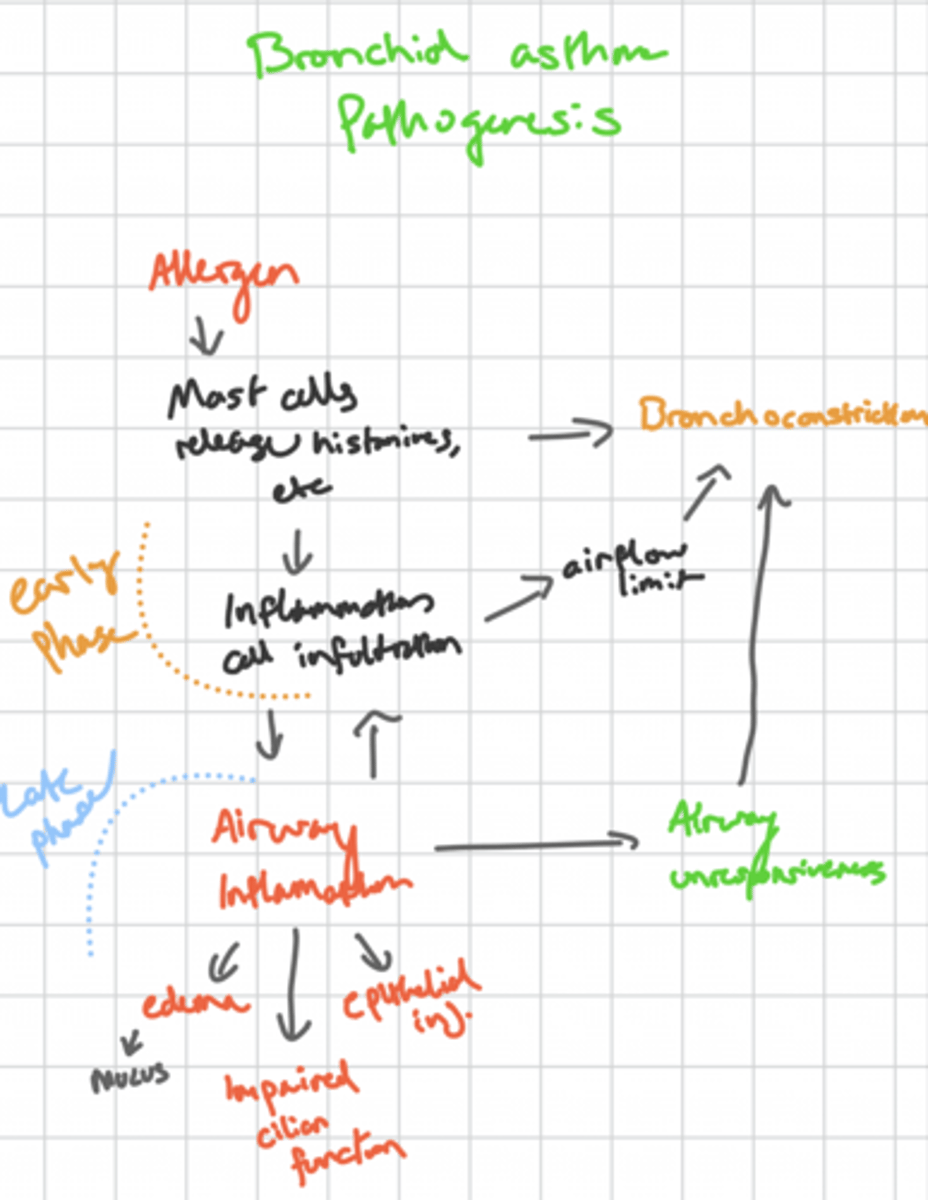
Treatment for early and late phases of asthma pathogenesis?
Early phase
- Beta-2 Agonists, anticholinergics
Late phase
- Anti-inflammatories
Changes in bronchial walls of chronic asthmatics?
- Increased goblet cells = More mucus makers
- More mucus overall
- Thickened basement membrane and thickened smooth muscle
- Thickened lamina propria
- Increased cellular infiltrates
- Increased glands and secretions from the glands
Change in %FEV due to changes in bronchial walls of chronic asthmatics?
Lowered %FEV due to many obstructions
Emphysema characteristics?
- Obstructive lung disease
- Caused from chronic exposure to harmful substances or genetic alpha-anti-trypsin deficiency
- Causes tissue damage leading to inflammation and neutrophil recruitment
Protease and Anti-protease balance about emphysema walkthrough?
- Neutrophils release elastase to break down elastin in alveoli
- Normally, alpha-anti-trypsin inhibits elastase, but free radicals like tobacco smoke inactivate alpha-anti-trypsin
- This leads to the continued destruction of alveolar walls = loss of elastic recoil and more lung compliance
Signs/Symps of Emphysema?
- Loss of elastic recoil, increased lung compliance = Lungs not returning to og state and being very moveable for air trapping = barrel chest
- Reduced gas exchange from less alveolar SA from elastin
- Dyspnea from reduced lung function
- More RTIs = impaired clearance of mucus and debris
Affect of emphysema on tidal volume and residual volumes?
- Decreased tidal volume, increased residual volume
Chronic Bronchitis characteristics?
- Obstructive lung disease
- Comes from chronic irritation from smoking or pollutants and excess mucus plugging of airway lumens
- Less %FEV from less space due to inflammation and mucus
Signs/Symps of Chronic Bronchitis?
- Productive cough for 3 consecutive months in at least 2 consecutive years
- Progressive SOB
- Lower respiratory rate and greater tidal volume = Easier for more air in than out
Characteristics of Cystic fibrosis?
- Obstructive lung diease
- Recessive gene mutation for chloride channels in epithelial cells = abnormal Na+ and water absorption for thick and viscous mucus
- Less %FEV from obstructive mucus plugging alveoli
Signs/Symps for Cystic Fibrosis?
- Viscous mucus in bronchi
- Impaired lung clearance
- Chronic infections like bronchitis
- Atelectasis present from collapse of alveoli due to fluid, compression, and a mucus plug
Characteristics of Chronic Interstitial Diseases (AKA Restrictive lung diseases)
- Often end in osis = ex: asbestosis
- Idiopathic progressive fibrosis of lung
- Injury to alveolar epithelium, chronic inflammation and fibrosis of inter-alveolar spaces
- Stiff, noncompliant lungs with high elastic recoil but normal airway function
- Less Tidal volumes and more Respirations per min = More resps to make up for inability to fill lungs fully
- Greater %FEV
Pneumoconiosis = Diseases caused by inhalation of inorganic dusts
Examples of Pulmonary Vascular Disorders with definitions?
Pulmonary Embolism
- Thrombus, air, fat, or amniotic fluid in lungs resulting in dyspnea w/ pleuritic pain, rapid and shallow breathing, cough w blood
- Large emboli can result in obstructive shock
Pulmonary Hypertension
- Primary pulmonary HTN due to thickened blood vessel walls = fibrosis potential
- Cor pulmonale = abnormal enlargement of right ventricle due to pulmonary HTN
Acute Respiratory Distress Syndromes (ARDS) characteristics?
- Acute lung injury resulting in more permeability of alveolar capillary membranes
- Permeability = fluid entering alveoli causing no gas exchange, difficulty breathing
- Neutrophils enter lungs resulting in inflammation, proteolytic enzyme distribution for less surfactant, fibrosis, hypoxia, and potentially multiple organ failure
- Decreased Tidal volume and residual volume
Causes of ARDS?
Aspiration
- Near drowning = aspiration of gastric contents
Drugs, Toxins, Therapeutic agents
- Heroin, gases, radiation
Infections
- Bacteria or viral
Trauma
- Burns, lung bruising
Gastro-esophageal Reflux Disease (GERD) characteristics?
- Comes from reflux of gastric contents from an incompetent lower esophageal sphincter that causes metaplasia of the lower esophagus
- Barett Esophagus = Persistent reflux leading to mucosal damage, erosion, scarring that leads to strictures, dysphagia, and metaplasia that causes risk of esophageal cancer
Signs/Symps of GERD?
- Local irritation, inflammation, heartburn, epigastric pain, belching 30-60 mins after meal, worse when laying
Acute gastritis characteristics?
- Self limiting inflammation
- Associated w/ irritants
- Mild heartburn, gastric distress, vomiting, bleeding
Chronic gastritis characteristics?
H. Pylori gastritis
- Enzymatic toxins from bacterial infection
Autoimmune gastritis
- Antibodies against parietal cells (risk of gastric carcinoma)
Chemical gastritis
- Chronic alkaline reflux from duodenum via an incompetent pyloric sphincter following GI surgery
Peptic Ulcer characteristics?
- In duodenum or gastric areas
- Cyclical exacerbations and remissions
- Caused by H. Pylori infections or NSAID overuse
- Can cause burning, recurring midline pain between meals
- Complications include perforations (peritonitis), bleeding
Stress Ulcer characteristics?
- Ulcerations following severe psychological stress
- Come from stomach ischemia, tissue breakdown resulting in acidosis, and increased intracranial pressure
- Cushing Ulcer = Hypersecretion of HCl due to increased intracranial pressure
Irritable bowel syndrome characteristics?
- Intestinal disorder
- RELIEVED BY DEFECATION
- Comes from dysregulation of intestinal motility by CNS, exacerbated by stress or menstruation
- Results in bloating, flatulence, nausea, anorexia, alternating diarrhea and constipation for at least 12 consecutive weeks (3 months) in a year
Inflammatory Bowel Disease characteristics?
- Symps include marked diarrhea, lower abdomen pain w/ exacerbations and remissions, weight loss
Crohn's disease and Ulcerative colitis similarities?
- General inflammation
- Overactive immune system cause
- Genetic component
- Marked diarrhea
- Abdomen pain
- Malabsorption and nutrition deficiencies
Crohn's disease inflammation, tissue level, rectal bleeding, and areas affected?
- Cobblestone
- Submucosal
- Rare
- Ileum and colon
Ulcerative colitis inflammation, tissue level, rectal bleeding, and areas affected?
- Continuous
- Mucosal
- Common
- Rectum and colon
Viral enterocolitis characteristics?
- Caused from rotavirus and adenovirus
- Infection causes death of epithelia mucosal cells
- Less water secretion and absorption = diarrhea with a concern of dehydration
- Spread fecal-oral
- Immune contamenent = repopulation of cells produces relief
Bacterial enterocolitis characterics?
- More severe from endo/exotoxins from the bacteria that cause inflammation, peristalsis, hemorrhage, and cell necrosis
- Causes cramping, watery bloody diarrhea, toxemia, renal failure, anemia, and potentially neurological problems
C. Diff - Antibiotic associated colitis, hospital setting (fecal oral)
E. coli - Food borne by unpasteurized milk, fecal contaminated, undercooked food
Celiac disease characteristics?
- Immune-mediated disorder to gluten-containing complexes
- IgA antibodies against variety of antigens (transglutiminase, endomysium, gliadin)
- Genetic component
- Causes malabsorption of nutrients if severe due to loss of absorptive villi in small intestine
- Symps: diarrhea and abdominal comfort, failure to thrive in infants, iron deficiency
- Must remove gluten from diet
Diverticulosis characteristics?
- Mucosal layer of intestinal walls herniates through muscularis layer due to functional (chronic) constipation or anatomical abnormalities
- Causes a change in bowel habits, bloating or flatulence, bleeding in small amount, relatively asymptomatic
Diverticulitis characteristics?
- Inflammation of the pockets made from diverticulosis
- Intense lower left abdominal pain, tenderness, fever
- Perforation of diverticula can cause peritonitis, bleeding, or bowel obstruction
Appendicitis characteristics?
- Obstruction or twisting of appendix
- Causes abrupt epigastric/periumbilical pain and nausea, pain localizes to lower right quadrant, tenderness, fever, raised WBCs
- Potential complications include rupture, peritonitis, abscess, or septicemia
Small volume diarrhea characteristics?
- More motility of intestines due to inflammation or disease
- Colicky pain or cramping associated
Large volume diarrhea characteristics?
- Lactose intolerance = Osmotic LV diarrhea
- Painless, watery stool w/out blood = Secretory LV diarrhea
Intestinal obstructions characteristics?
- Impairment of movement of contents that causes abdomen distension, pain, absolute constipation, and vomiting
Mechanical
- External hernia, tumors, strictures, Intestinal folding or twisting
- Complication = Tissue strangulation, necrosis
Paralytic
- Neurogenic or muscular impairment of peristalsis from surgery, inflammation, or toxins
Neoplasms characteristics?
- Most common is adenomatous polyps
- Proliferation of epithelium
- Increased risk of colorectal cancer
- Asymp. or slight bleeding
Colorectal cancer = Adenocarcinoma characteristics?
- Increased risk due to family history, ulcerative colitis, adenomatous polyps, a diet high in fat and sugar, low in fiber
- Rectal bleeding, change in bowel habits, increased urgency, feeling of incomlete bowel emptying
Jaundice (Icterus) characteristics?
- Yellowish skin = high bilirubin in blood
- Dark urine, light colored stool
- High ALT , AST, GGT = Damage in liver results in release of enzymes
- Lower plasma albumin
- High prothrombin time
- High alkaline phosphatase
3 Jaundice (Icterus) types and definitions?
Extrahepatic
- High breakdown of RBCs
Hepatocellular
- Dysfunction of hepatocytes resulting in decreased liver uptake or conjugation of bilirubin
Cholestatic
- Increased bile duct obstruction
Acute Hepatitis characteristics?
- Autoimmune disease related
- Viral infection related
- Reactions to drugs, toxins, or chemicals
Chronic Hepatitis characterisics?
- Chronic alcoholism
- Autoimmune disease related
- Viral infection related
- Reactions to drugs, toxins, or chemicals
- Associated w type B and C
- Symps include malaise, anorexia, bouts of jaundice for years
Fulminant hepatitis characteristics?
- Rapid onset of encephalopathy in 2-3 weeks
- Causes include HAV and HBV related, drug toxins, or chemical
- Can lead to liver failure
Hepatitis A characteristics?
- ssRNA virus
- 15-35 day incubation
- Usually benign and self-limiting
- Abrupt onset with mild symps of fever, malaise, nausea, anorexia, and jaundice
- Fecal oral transmission
- Vaccine available
- Common in areas w/ poor sanitation and contaminated food/water
Hepatitis B characteristics?
- dsDNA virus
- Can cause chronic hepatitis, cirrhosis, or tissue necrosis
- Insidious onset with fever, chills, weakness, and hepatocellular jaundice
- Infected blood, saliva, STD transmission
- Vaccine available
Hepatitis C characteristics?
- ssRNA virus
- Can cause chronic hepatitis, cirrhosis, carcinoma
- Insidious onset with asymptomatic or mild symptoms
- Persistent and chronic
- 6-26 week incubation
- Blood borne (needle sticks) transmission
- No vaccine
Clinical course of hepatitis?
Acute asymptomatic
- Incidentally detected by elevated LFTs, common with HCV
Acute symptomatic (Pre-Icteric phase)
- Progressive symptoms of malaise, fatigue, anorexia, nausea, vomiting, diarrhea, mild right abdomen pain
Icterus phase
- Chills, fever, high AST and ALTs, jaundice, tenderness, pruritus = itchy skin
Alcoholic liver disease stages?
Fatty liver
- Steatosis = accumulation of fat in hepatocytes
- Asymptomatic or slightly enlarged liver
Alcoholic hepatitis
- Inflammation and death of hepatocytes
- Binge drinking association
Alcoholic cirrhosis (Irreversible step)
- Fibrosis from repeated alcohol related hepatotoxicity
- Bad tissue remodeling from compression, cholestasis, and portal HTN
- Progresses to liver failure and death
Cirrhosis characteristics?
- Represents end stage chronic liver disease
- Damaged hepatocytes replaced with fibrosis
- Common in chronic viral hepatitis, chronic drug toxicity, biliary obstruction, or heart failure
- Jaundice, weakness, ascites (fluid in peritoneal cavity), bleeding, hepatomegaly, abdomen pain, portal HTN
- Results in lack of urea/uric acid from ammonia
Liver cancers characteristics?
Hepatocellular carcinoma
- Most common
- Hepatocyte involved
- Risk factors: HBV, HCV, Cirrhosis
Cholanglocarcinoma
- Involves bile duct cells
- Risk factors: Chronic inflammation of bile duct cells
Cholelithiasis characteristics?
- Gall stones
- No obstruction is asymptomatic
- Present obstruction: abrupt pain, upper right epigastric pain, cholestatic jaundice
- Potential causes:
Abnormal compilation of bile (Drug induced, obesity)
Stasis of bile (ductal stenosis/scarring)
Inflammation of gall bladder (Excessive absorption of water and bile salts)
Cholecystitis characteristcs?
- Gall bladder attacks
Acute
- Complete/partial block of bile duct that leads to local irritation, bacterial infections, ischemia, mucosal necrosis, and perforation with unrelenting pain, fever, elevated WBCs and LFTs
Chronic
- Related episodes of acute and chronic irritation with vague intolerance to fatty meals, belching, indigestion, and colicky pain
Nephritic syndromes? (2)
- Acute post infectious glomerulonephritis
- Rapid progressive glomerulonephritis
Acute Post Infectious Glomerulonephritis characteristics?
- Post step infection, Hep B, or malaria infection
- Immune complexes stuck in glomerulus
- Abrupt onset of hematuria, proteinuria, water retention, and oliguria (low urine output) with reduced GFR and renal salts
Rapid Progressive Glomerulonephritis characteristics?
- Autoantibodies against glomerulus
- Continued poor function leads to irreverisble damage
- Inflammation in capillary walls
- Decreased GFR
- RBCs in urine = Hematuria
Nephrotic syndromes characteristics?
- Non-inflammatory damage to glomerular filtration barrier that increases glomerular permeability
- Heavy proteinuria, albuminuria
- Edema from reduced GFR = Potential for pulmonary edema --> dyspnea, pleural effusions
Heavy proteinuria causes?
- Immunoglobulins and complement -->immunodepression
- Clotting and anti-clotting proteins --> thrombosis or bleeding
- Albumin --> altered drug distribution and kinetics with edema
Secondary glomerular disorders characteristics?
Diabetic Glomerulosclerosis (Neuropathy)
- Sclerosis, glomerular basement membrane thickening
Hypertensive Glomerular Disease
- Sclerosis, decreased perfusion from untreated/poorly controlled HTN
Systemic Lupus Erythematosus Nephritis
- Autoimmune disease where immune cells deposit into glomerulus
What needs to happen to the detrusor muscle and sphincter for urine to flow?
- Detrusor contracts and sphincter releases
Obstructive Uropathy?
- Acute or chronic, bilateral or unilateral obstruction to urine flow
Ex: Calculi, pregnancy, benign prostatic hyperplasia, tumors, scarring, chronic inflammation
Renal Calculi (Nephrolithiasis) characteristics?
- Kidney stones
- Renal pain, stretching of ureter, excruciation pain on affected sides, hematuria, nausea, vomiting
Prerenal acute kidney injury description and causes?
- Reduced blood flow to kidneys
- Embolisms, hemorrhage, dehydration, heart failure, any reduced cardiac output
Intrinsic acute kidney injury description and causes?
- Damage to tubules, glomerulus, or blood vessels of kidneys
- Acute tubular necrosis, glomerulonephritis, SLE = Lupus, Vasculitis
Postrenal acute kidney injury description and causes?
- Obstruction of urine outflow
- Calculi, BPH = pelvic tumor