Structure and Function II Exam 3
1/117
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
118 Terms
veins 64%, capillaries 5%, arteries 15% (systemic circuit 84%), pulmonary circuit 9%, heart 7%
What is the percentage of blood in the veins, capillaries, arteries, systemic circuit, heart, pulmonary circuit
oxygenated, deoxygenated
in systemic circuit all arteries carry ______ blood and all veins carry ______ blood
deoxygenated, oxygenated
in pulmonary circuit all arteries carry _____ blood and all veins carry ______
elastic artery, muscular artery, arteriole (controls blood flow into tissues)
what are the 3 types of arteries? from closest to the heart to farthest
large vein, medium-sized vein, venule
what are the 3 types of veins? closest to the heart to farthest
tunica externa, tunica media, endothelium, tunica intima
label 1-4
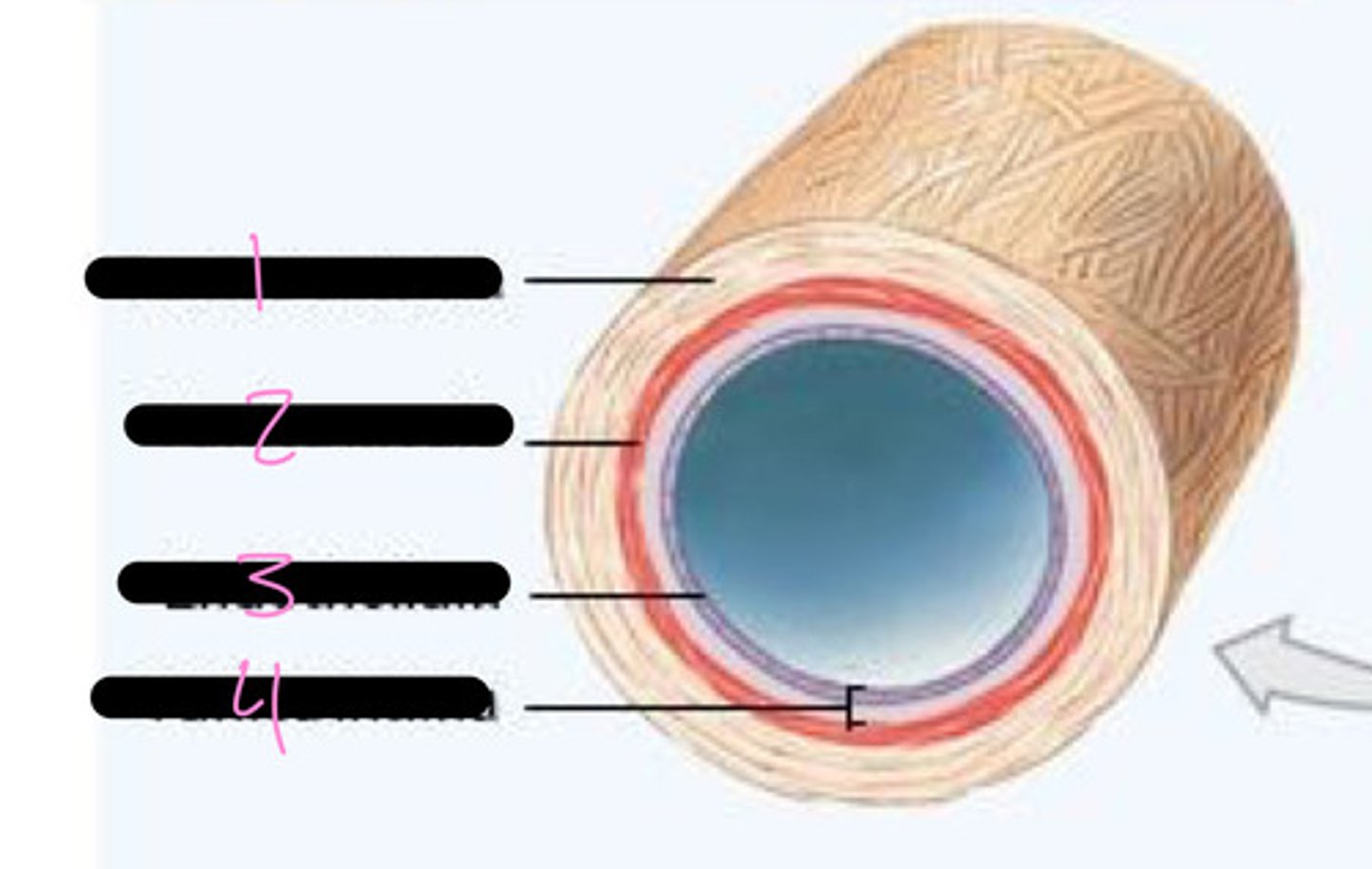
lumen
what is the "hole" in the middle of the blood vessel called
artery: thicker walls, stays open when empty, high pressure, average pressure is 90-100 mmHg (max is 120 mmHg),greater resistance, smaller lumen, pulsatile flow
veins: thinner walls, will collapse when empty, lower pressure and resistance, average pressure is 90-100 mmHg (max is 120 mmHg), veins have valves that prevent blood from flowing backwards, bigger lumen, steady flow
describe differences in an artery and vein (wall size, pressure, resistance, lumen size, valves, type of flow)
these arteries are closest to the heart, and it allows for expansion when full of blood and to absorb pressure. the walls will expand and pop back which pushes the blood forward. elasticity declines with age
distributing elastic arteries: why is elasticity important
to help raise or lower BP throughout the body, controls blood flow into an area or reroutes blood
what physiological purposes do vasoconstriction and vasodilation serve?
angiotensin II (raises BP)
what is the most powerful vasoconstrictor in the body
true
t/f in general vasoconstriction raises BP, vasodilation lowers BP
the SNS vasoontricts most blood vessels, but will dilate coronary arteries (heart), skeletal muscles arteries, and arteries of the brain
what is the SNS effect on vasoconstriction/ dilation
it is routing of blood, for example during exercise more blood will go to muscles and less blood will go to digestive organs
what is selective perfusion in an organ
5800; 17,500
average total blood flow at rest is ____ ml/min, whereas average blood flow during strenuous exercise is ______ ml/min
3/4
at any given time ____ of capillaries are shut off
continuous, fenestrated, discontinuous
what are the 3 types of capillaries
there are no gaps between endothelial cells, less permeable, these are in most tissues/ organs (ex. fat, skeletal muscles, lungs, brain)
describe a continuous capillary
have pores in endothelial cells, highly permeable, these are in kidneys, choroid plexus (in brain for csf), small intestine, endocrine organs
describe a fenestrated capillary
have big gaps in the endothelial cells, are very permeable especially to blood cells and proteins, the rarest type, are found in liver, spleen, bone marrow
describe a discontinuous capillary
filtrations is when fluid moves out of capillaries, reabsorption is when fluid moved back into capillaries
what is filtration? reabsorption?
hydrostatic pressure (HP) and colloid oncotic pressure (COP)
what are filtration and reabsorption determined by?
pressure of a fluid (blood) on a surface (capillary wall)
what is hydrostatic pressure
attractive force due to proteins (albumin)
what is colloid oncotic pressure
COP: 20 mmHg (in), HP: 33mmHg (out), net filtration (13 mmHg out)
on the arterial end of a capillary, what is the net colloid oncotic pressure (COP), net hydrostatic pressure? is it net filtration or net reabsorption
COP: 20mmHg (in), HP: 13mmHg (out), net reabsorption (7mmHg in)
on the venous end of a capillary, what is the net colloid oncotic pressure (COP), net hydrostatic pressure? is it net filtration or net reabsorption
there should be little/ no filtration to keep fluid out of the lungs
what is filtration and reabsorption like in the lungs?
85%
in reality, we only reabsorb about ___ of the water that was filtered out
high
if someone has a high blood pressure, what will hydrostatic pressure be
drop
if someone has a bad liver, albumin will decrease, what will happen to colloid oncotic pressure
the 15% of fluid that was not reabsorbed is taken by the lymphatic capillaries and that fluid is called lymph
describe lymph
they have WBC where the lymph fluid is cleaned and returned to the heart
describe lymph nodes
due to a damaged lymph system where lymphatic fluid cannot return to the heart and it accumulated and causes edema (swelling)
describe lymphedema
respiratory pump, muscular pump, valves, pressure gradient
what things drive venous return to the heart?
As muscle contracts it puts pressure on veins pushing blood to the heart
describe the skeletal muscle pump
Pressure changes occurring in the ventral body cavity during breathing create the respiratory pump that moves blood up towards heart
describe the respiratory pump
valves
why does blood only flow in the direction of the heart
faulty valves in veins cause blood to pool in the veins and they protrude out of the skin
describe varicose veins
pressure gradient (blood flows from high pressure to low pressure)
blood flows due to a ______
120; 110; 40; 30; 18; 16; 12; 7; 4.6
The flow of blood is aorta, large arteries, arterioles, arterial end of capillaries, venous end of capillaries, venules, muscular veins, central veins (IVC/SVC) and right atrium. what is the pressure in each of those blood vessels
pressure of blood against the walls of the arteries
what is the definition of blood pressure
systolic (top number) is the pressure in the arteries when the heart is in systole (contraction), diastolic (bottom number) is the pressure in the arteries when the heart is in diastole (rest/ filling)
what is systolic blood pressure? diatolic bp?
elastic
____ arteries keep systolic pressure from getting too high, and from diastolic pressure from getting to 0
mean arterial pressure, it is the estimate of the average BP in the body during 1 cardiac cycle
what is MAP and what does is stand for?
[systolic pressure + 2 diastolic pressure]/3
remember systole is 1/3 of the cardiac cycle, diastole is 2/3 of the cardiac cycle
what is the MAP equation
greater than 96mmHg; less than 65mmHg, 24 hr MAP under 90mmHg
what MAP score is a risk for adverse cardiac events and stroke? what score poses an increased risk of mortality in critically ill patients and causes hypofusion? what is the optimal range
BP= Q x SVR
Q: cardiac output (HR x SV)
HR: SNS (increases), PSNS (decreases)
SV: blood volume, venous return, EDV, preload
SVR: systemic vascular resistance
- length of blood vessels (shouldn't change in adulthood)
- viscosity of blood (if viscosity is high, SVR is high vice versa)
- diameter of blood vessels (changed throughout the day), vasoconstriction decreases diameter, so SVR increases vice versa
what is the blood pressure equation? what factors determine bp?
true
ex is a blood vessel has a radius of 1cm, another had 2cm, and another 3cm. the 1cm has a blood flow of 1 cm/sec, the 2cm 16 cm/sec, and the 2cm 81 cm/sec
t/f blood flow in our vessels increases by r^4 (radius)
normal: systolic less than 120 and diastolic less than 80
elevated: systolic 120-129 and diastolic less than 80
stage 1: systolic 130-139 or diastolic 80-80
stage 2: systolic 140 or higher or diastolic 90 or higher
crisis: systolic higher than 180 and/or diastolic higher than 120 (risk for stroke)
hypotension: systolic less than 90 or diastolic less than 60
what is normal blood pressure? elevated? hypertension stage 1? hypertension stage 2? hypertensive crisis? hypotension?
increase bp means a very high afterload, so the heart has to work extra hard to pump blood, there is a risk of stroke, and low BP means blood cannot get to all the body (hypoperfusion)
why is BP regulation necessary in the body?
tissues can control their own blood flow
metabolic: vasodialation can occur to wash away chemicals (CO2, H, K, LA, adenosine)
angiogenesis: technically means forming new blood vessels, but this can occur during the thickening of uterine lining (during a woman's cycle), athlete's skeletal muscles, cancer
what is auto regulation of blood supply
SNS always has the blood vessels a little vasoconstricted to maintain a blood pressure
what is sympathetic tone
corrects sudden changes in BP (only BP not HR)
what is the baroreflex
low BP is detected by baroreceptors in the walls of the elastic arteries near the heart and the glossophangeal nerve (9) sends that info the cardiac regulatory center (medulla) and the vasomotor center (medulla). the cardiac regulatory center stimulates SNS and turns of PSNS to increase HR, force, and SV, thus elevating Q. the vasomotor center stimulates SNS to vasoconstrict, thus elevating SVR. Since Q and SVR are raised, BP is also raised
describe the baroreflex for low blood pressure
high BP is detected by baroreceptors in the walls of the elastic arteries near the heart and the glossophangeal nerve (9) sends that info the cardiac regulatory center (medulla) and the vasomotor center (medulla). the cardiac regulatory center turns off SNS and turns on PSNS to decrease HR, force, and SV, thus lowering Q. the vasomotor center turns off SNS to vasodialate, thus decreasing SVR. Since Q and SVR are lowered, BP is also lowered
describe the baroreflex for high blood pressure
increase BP (most powerful vasoconstricter)
increase BP
decrease BP
increase BP
increase BP (maintains sympathetic tone)
what are these hormones effect on blood pressure? angiotensin II, aldosterone, ANP, ADH, EPI/NE
true
t/f in the brain total blood flow fluctuates less than other organs as consistency is important because even a few seconds of o2 deprivations can cause a loss of consciousness and 4-5 mins can cause permanent brain damage, however, blood can shift to different parts of the brain
yes
does the brain regulate its own blood flow in response to changes in blood pressure and blood chemistry
dilate, constrict
cerebral arteries ___ when BP is low and ____ when BP is high so that blood flow can remain stable even at high blood pressures
true
t/f high co2 lowers pH and triggers local vasodilation in the brain
brief episodes of cerebral ischemia (lack of blood flow) characterized by temporary dizziness, loss of vision, weakness, paralysis, headache, aphasia. this can be an early warning sign of a stroke and immediate treatment is needed
what is transient ischemic attacks
sudden death (infarction) of brain tissue caused by ischemia caused by atherosclerosis, thrombosis or ruptured aneurysm
what is cerebrovascular accident (CVA or stroke)
true
t/f skeletal muscles have high variable blood flow which is dependent on the state of exertion
constricted; shut down; dilated; 20x
in the skeletal muscles: at rest arterioles are ______ and most capillaries are _______, during exercise arterioles are _________ and blood flow can increase _____
true
t/f in the lungs blood flows slower through pulmonary capillaries so there is more time for gas exchange
true
t/f in the lungs oncotic pressure overrides hydrostatic pressure, so capillaries are engaged almost entirely in absorption. also, pulmonary arteries constrict in response to hypoxia and redirects blood flow to better ventilated regions
beta blockers, diuretics
ACE-inhibitors, antiogentension receptor blocker (ARBs), vasodilators
what are the 2 types of BP medications used to effect Q? the 3 used to effect SVR?
blocks the SNS effects, decreases HR, ctx force, cardiac output, blood pressure
describe beta blockers
increases urinary output, decreases blood volume, stroke volume, cardiac output, blood pressure
describe diuretics
inhibit ACE, thus there is no antiogenosein II, so no vasoconstriction and less aldosterone (thus urinary output increases). this causes vasodilation, increased UO, decreased Q, SVR and BP
describe ace inhibitors
same effects as ACE inhibitors but a different approach by inhibiting antiogentension II from binding to its receptors
describe antiogentension receptor blockers (ARBs)
will be used is BP is very very high and immediately needs to be dropped. used in ERs because it causes fainting as the blood vessels dilate quickly
describe vasodilators
-regulation of BP via BV
- regulation of osmolarity (water/salt balance)
- regulation of pH
- hormone production (EPO + renin)
- filter blood
what are the functions of the kidney's
T12-L2
what spinal cord level is the kindey at
true; behind the peritoneum (sack around the abdominal organs)
t/f the kidney is retroperitoneal. what does that mean
a by-product of blood; it varies in concentration and urine should not have blood cells or protein
what is urine? how does it differ from blood?
nephron; Arthur Grollman 1957
"plasma undergoes modification to urine in the _____" (who said this)
no (it's a kidney tubule)
is a nephron a blood vessel
1) filtration
2) reabsorption
3) secretion
what are the 3 processes to form urine in the nephron
hyperglycemia means there in an increase in filtered glucose, which exceeds the ability of transporters to reabsorb it, so it stays in the urine
why can glucose show up in the urine of someone with diabetes mellitus
1) bowman's capsule
2) proximal convoluted tubule (PCT)
3) loop of henle (descending limb & ascending limb)
4) distal convoluted tubule (DCT)
5) collecting duct (CD)
what are the 5 parts of a nephron
true
t/f several nephrons can share a collecting duct
afferent; efferent; pertitubular capillary
blood goes into the glomerulus (the fenestrated capillary of the urinary system) in the _____ arteriole and exits in the ______ arteriole and that branches into what vessel
glomerulus in the bowman's capsule
where is blood filtered in the urinary system
everything in blood gets filtered out if it can fit through the holes of the capillaries and is not highly charged (ex. proteins); filtrate
what gets filtered in the glomerulus? what is that filtered stuff called
blood hydrostatic pressure: 60 mmHg (out)
colloid oncotic pressure: 32 mmHg (in)
bowman's capsule hydrostatic pressure: 18 mmHg (in)
net pressure: 10mmHg out (filtration)
what are the pressures of the glomerulus that causes the net filtration
glomerular filtration rate, the volume of filtrate formed by both kidneys per minute; 125 mL/min
what is GFR, what is the set point
high, thus urinary output would be high and that can lead to dehydration
low, thus uo would be low as there is too much reasborption, that can lead to toxicity
if there was no regulation: if MAP was high, what would GFR be and what would be the opposite
PCT (proximal convoluted tubule) 65-75%; due to the Na gradient and low hydrostatic pressure and high oncotic pressure
where does most reabsorption occur in the nephron and why
6%
___% of the bodies ATP is used in the PCT to drive the Na/K pump
water; high (1200); salts; low (100)
on the descending limb of the loop of henle, ______ is reabsorbed making the osmolarity _______, on the ascendingn limb _____ is reabsorbed making the osmolarity______
hypertonic (that draws water out of the collecting duct via aquaproins to produce concentrated urine and conserve water)
the loop of henle creates and maintains a _____ ISF via the countercurrent multiplier which allows the collecting duct to concentrate the urine if necessary
the top part of the ascending limb, the distal convoluted tubule (DCT) and collecting duct (CD)
where in the nephron do hormones go to work
papilla, minor then major calyx, renal pelvis, ureter, bladder
out of the collecting duct, what is the path of urine
high; ADH; aquaporins; water; lowers; increases (plasma osmolarity can get as high as 1200)
If someone is dehydrated, their plasma osmolarity will be (HIGH OR LOW) and ___ will be released which causes the _____ in the wall of the collecting duct to open and reabsorb _____, this (RAISES OR LOWERS) urinary output and (INCREASES OR DECREASES) urine concentration.
low; will not; raises; decreases (plasma osmolarity can get as low as 50)
If someone very hydrated, their plasma osmolarity will be (HIGH OR LOW) and ADH (WILL OR WILL NOT) be released, this (RAISES OR LOWERS) urinary output and (INCREASES OR DECREASES) urine concentration.
renal blood flow and blood pressure
what drives the process of filtration?
1) vasoconstriction of afferent arteriole (when BP is high, this decreases blood flow into the glomerulus, and decreases GFR)
2) vasodilation of afferent arteriole (when BP is low, this increases BF and GFR)
3) vasoconstriction of efferent arteriole (when BP is low to build pressure)
How do the kidney's maintain a relatively constant GFR
the kidney's ability to regulate its own blood flow and GFR
what is renal autoregulation
smooth muscles response to stretch
- If BP is high, there will be an increased stretch on the wall of the afferent arteriole and it responds by contracting, and lowering blood flow into glomerulus
- If BP is low, wall of afferent arteriole relaxes, which increases blood flow into glomerulus
what is the myogenic mechanism of renal autoregulation