9 - Common co-occurring experiences
1/26
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
27 Terms
what is the difference between autistic individuals and the rest of the populations’ mortality?
Autistic people live ~6 years less than avg. ~7 with intellectual disability. -> coproduced with 4 autistic people and a representative from the NAS.
Anonymised data from GP practises, medical records of diagnosed autistic people
171,300 non-autistic, 17,130 autistic, with learning disability, 64,500 non-a, 6,450 a
There is a gender difference too, a lot of variation -> those who
People with an autism diagnosis have a shorter life expectancy than those without
what are the limitations on the study of life expectancy
absence of information on cause of death
no information on gender diversity
underdiagnosis - not possible to generalise findings
how may GP’s confidence in caring for autistic people act as a barrier to healthcare?
~40% of GPs had no formal autism training, limited knowledge of how to provide better healthcare to autistic people, if GPs had a higher score on this scale the provision was better
many did not have the confidence to support autistic people
what are some adverse outcomes in delayed and additional healthcare treatment
untreated mental health and physical health
missed specialist referral
should have attended sooner
additional treatmenr
untreated life threat
didnt attend screening
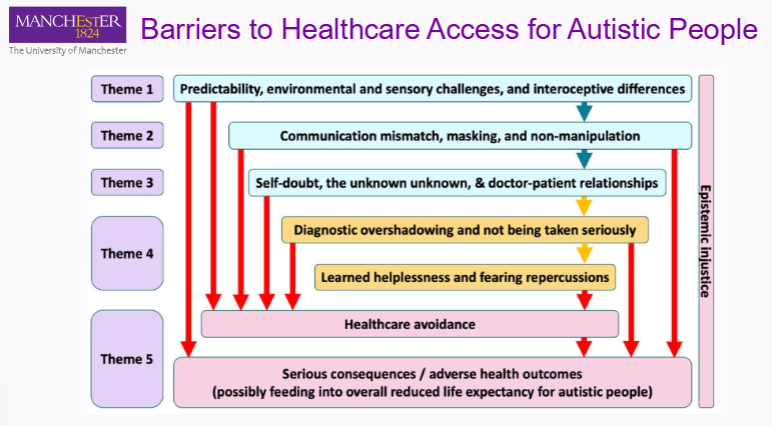
what are some barriers to healthcare access
early barriers; including predictability, environmental challenges and sensory/interoceptive differences.
communication mismatch ; e.g. masking
doubt in self and doctors; self-doubt, doctor-patient relationships
helplessness and fear
healthcare avoidance and adverse health outcomes
What does the SPACE framework propose would help?
sensory, predictability, acceptance, communication, empathy
how may you support sensory needs?
turn off/down artificial lights
consider environmental sound/provide noise cancelling headphones
avoid wearing strong perfume, consider ventilation
respect sensory preferences when considering nutrition
promote sensory-friendly clothing choices
understand the need for proprioceptive input
be aware that non-verbal reports of pain where possible
how may you make acceptance and empathy more suitable
neuro-affirming approach, understand distress behaviour
empathy may look different in autistic people, understand that it may be hard for healthcare providers to empathise
how can healthcare be made better for autistic individuals
training, knowledge and awareness
avoid fear and embarrassment and have transparent communication
involve them in healthcare decision making
what are the % of autistic people that also experience ADHD, Anxiety and depression
ADHD 28%
Anxiety 20%
Depression 11%
are autistic people more likely to be given diagoses of co-occuring mental health issues
yes, but many of these are perhaps misdiagnoses as autistic characteristics become confused with symptoms of a mental health condition and so are not treated properly
define camouflaging
pressure to ‘fit in’ with neurotypical social communication, individuals with autism may develop coping strategies
what are the three subscales measured by the CAT-Q
masking: strategies used to hide autistic characteristics or portray a non-autistic persona
compensation: strategies used to actively compensate for difficulties in social situations
assimilation: strategies that reflect trying to fit in with others in social situations
what group of people are most likely to score highly on the CAT-Q
female, gender diverse and late-diagnosed individuals
why does camouflaging happen
lack of autism awareness and acceptance in society
what is the impact of camouflaging on autistic individuals
spending lots of time camouflaging is the most damaging for autistic adults mental health, however some believed it helped them too
what is the influence of environmental factors on camouflaging
participants camouflaged less when there were autism-affirming cues, however, high inter-partcipant variability
pps who more strongly identified with the autistic community responded with more intensity to autism-affirming (vs stigmatising) cues
what were the findings of camouflaging in the 2 year longitudinal study
baseline camouflaging associated with baseline MH difficulties, camouflaging was stable over time
people with higher initial camo. there was a decrease in MH difficulties
what is autistic burnout
a syndrome conceptualised as resulting from chronic stress and a mismatch of expectations and abilities without adequate supports. characterised by a pervasive long-term (3 months+) exhaustion, loss of function and reduced tolerance to stimulus
what are potential solutions to burnout
individual/community/peer support
attending to autistic needs/unmasking
reduced activity, setting boundaries asking for help
understanding patterns and making strategic decisions
what is the estimated prevalence of AuDHD
28%
what does camouflaging look like in AuDHD
camo. more than adults who just have ADHD
what is the co-occurance rate of learning disabilities and autism
1/3
more significantly unmet medical and MH care and poorer care-giver reported health quality
why are those with learning disabilities often excluded from research
difficulties with consenting
less than ½ of studies use adaptations or accomodations, few co-produced studies, only 2/24 self-report measures validated for autistic people
what does research show that AFAB autistic people struggle with more
higher BMI
reproductive health diagnoses
pre-diabetes symptoms
irregular puberty onset
menstrual irregularities
outline issues surrounding birthing based on the SPACE model
Sensory: feeling overstimulated
Predictable: the need to build rapport with healthcare professionals, the need for factual information
Acceptance: feeling judged, poor understanding of autism
Communication: not asking for help doesnt mean not needing help, need for autism tailored communication
Empathy: feeling uncared for
how do autistic people experience menopause
2 studies found autistic people worse menopause symptoms than non-autistic people
said menopause symptoms impacted work and relationships
changed how autistic people felt about themselves
