Preventive Exam 3 [Periodontal Anatomy and Function: Spector]
1/32
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
33 Terms
Peri =
around
odontos =
tooth
Periodontium =
Around the tooth
Function of the periodontium according to Dr. Specter
Holds the tooth in the mouth
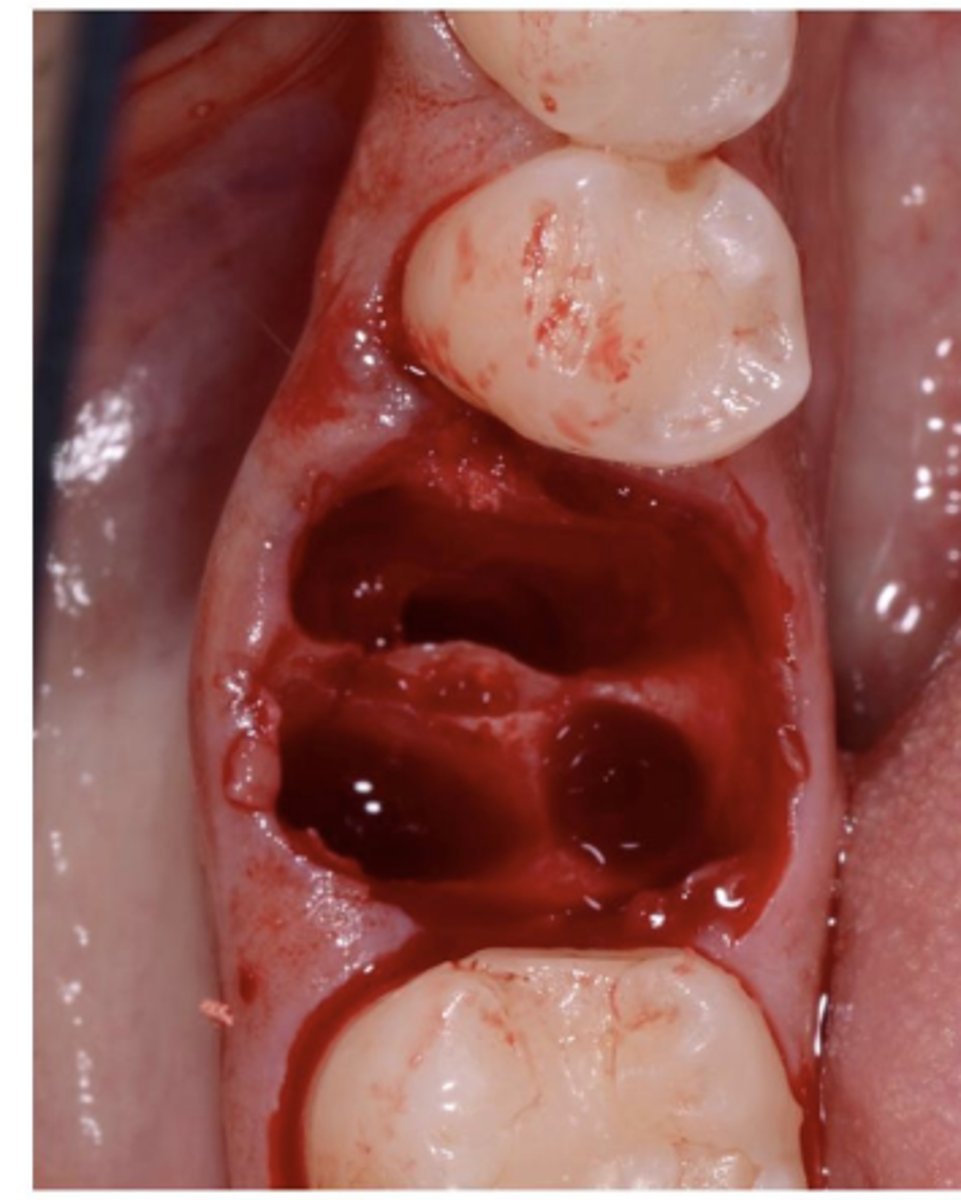
What is the periodontium and what is its main function
The periodontium is a functional unit of tissues surrounding and supporting the tooth. It is made up of the: Gingiva and the attachment apparatus
GCAP
Gingiva and the Attachment Apparatus
Attachment apparatus
cementum
Alveolar bone
Periodontal ligaments (PDL)
Gingiva
Gums- Soft tissue-
The gingiva surrounds the
roots of the teeth, alveolar bone, and underlying connective tissue
Anatomically the gingiva is made up of the
Free gingiva, interdental gingiva (interdental papilla) and attached gingiva
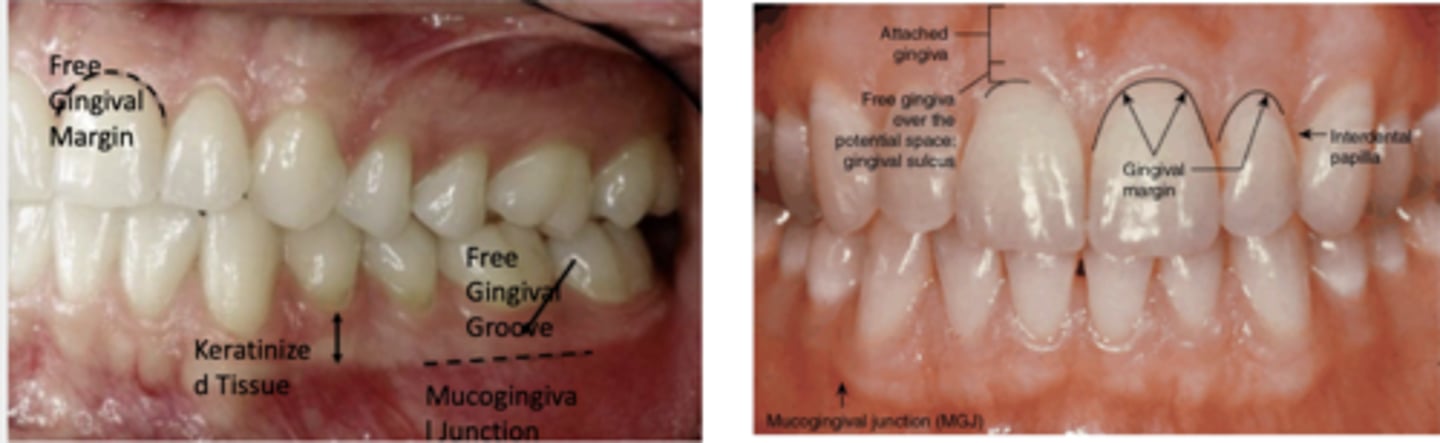
Know this image
Free gingiva: not connected to anything
Free gingival groove: separates ^⌄
Attached gingiva: attached to the tooth and the bone
Mucogingival junction: Separates ^⌄
Alveolar mucosa
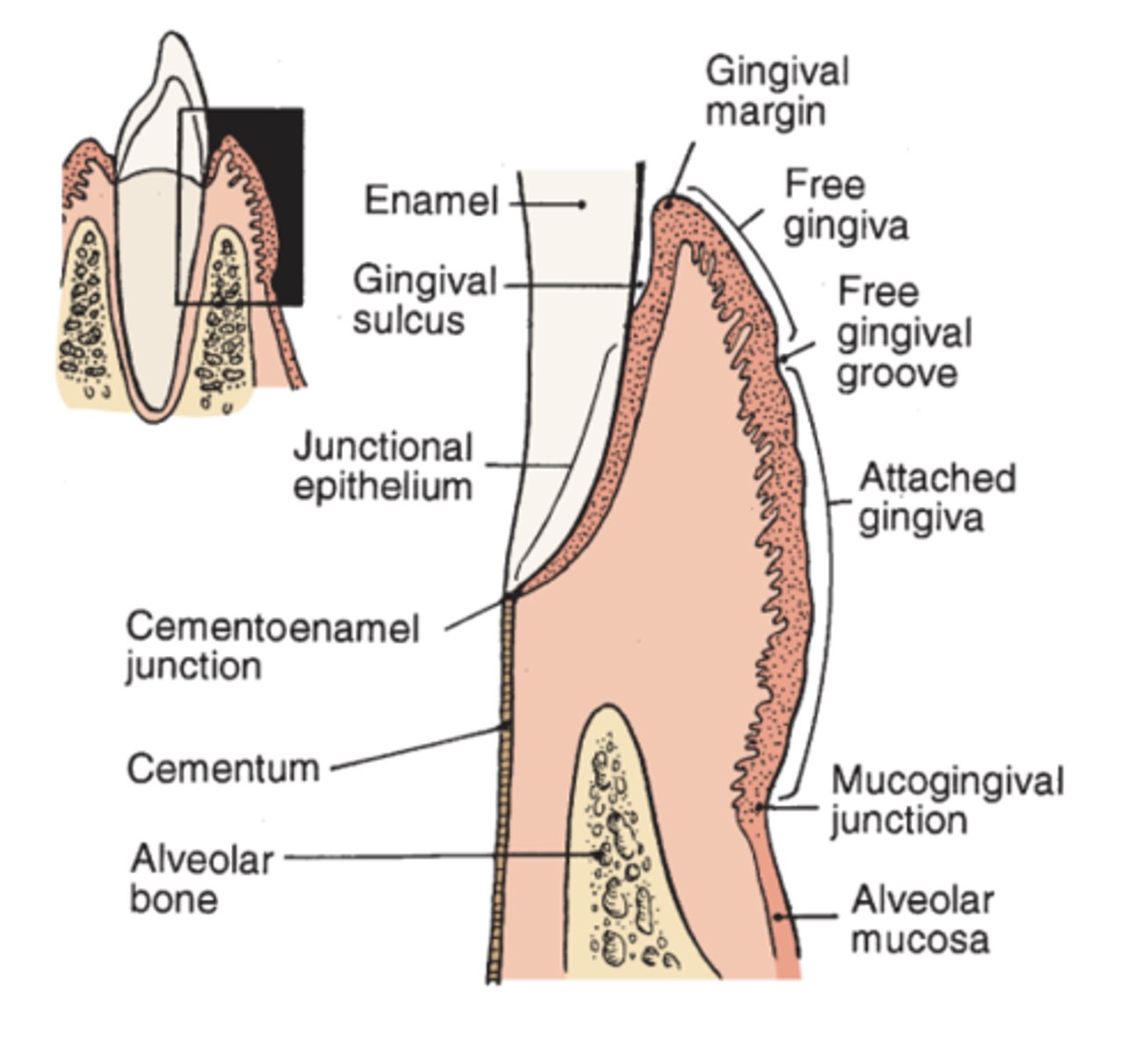
Clinical look at gingiva
Gingival margin: free gingiva and surround the tooth
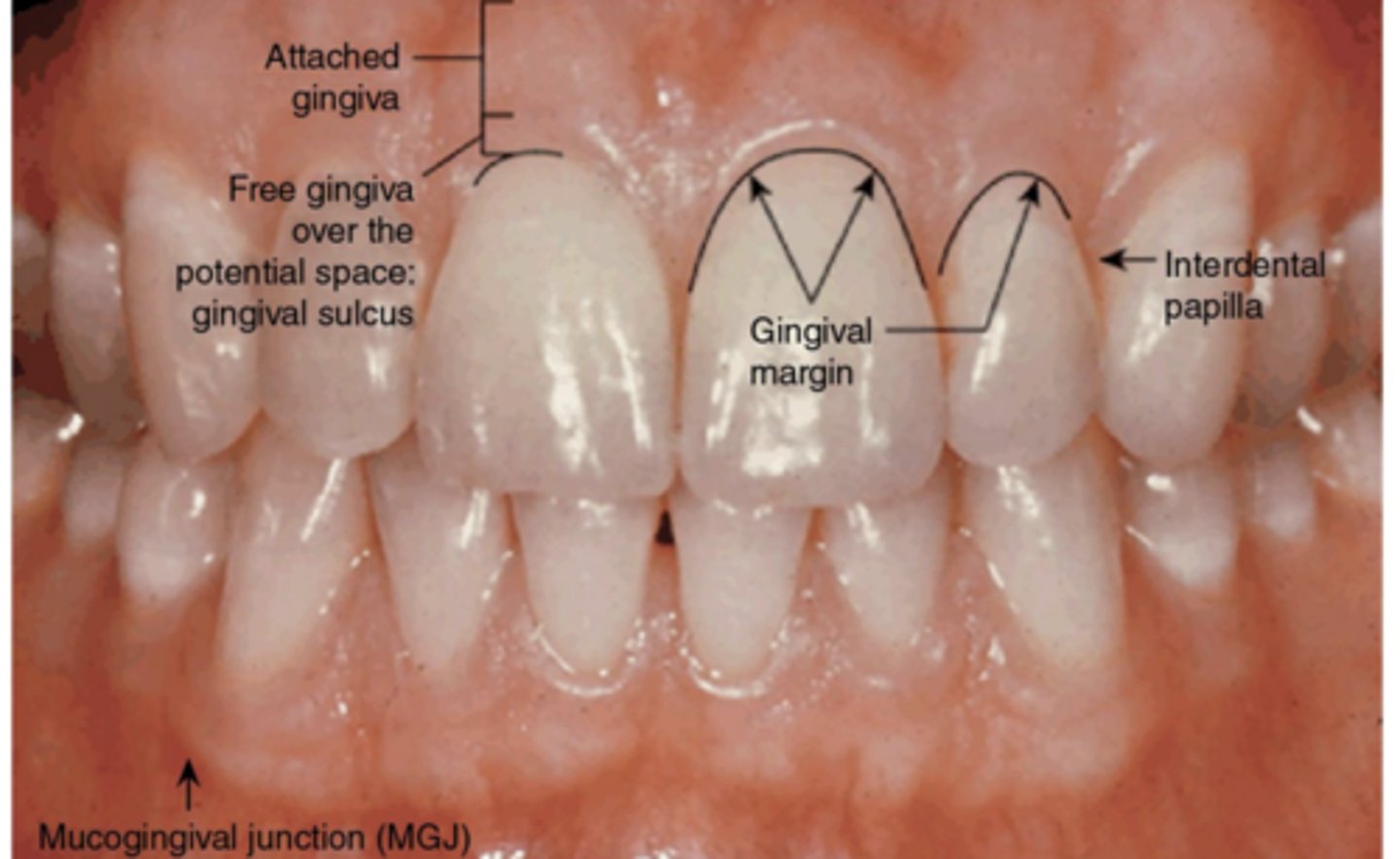
Marginal gingiva
The marginal or unattached or free gingiva is the terminal edge or border of the gingiva that surrounds the teeth in a collar-like fashion. IT can be demarcated from the adjacent attached gingiva by a shallow linear depression called the free gingival groove. The marginal gingiva is usually about 1mm wide and it forms the soft tissue wall of the gingival sulcus. It may be separated from the tooth surface with a periodontal probe
Gingival sulcus
The gingival sulcus is the shallow crevice or space around the tooth bounded by the surface of the tooth on one side and the epithelium lining the free margin of the gingiva on the other side. It is V-shaped and barely permits the entrance of a periodontal probe.
The clinical determination of the depth of the gingival sulcus is an important diagnostic parameter.. in clinically healthy human gingiva, a sulcus of some depth of a clinically normal gingival sulcus in humans is 1 to 3 mm without visible bleeding
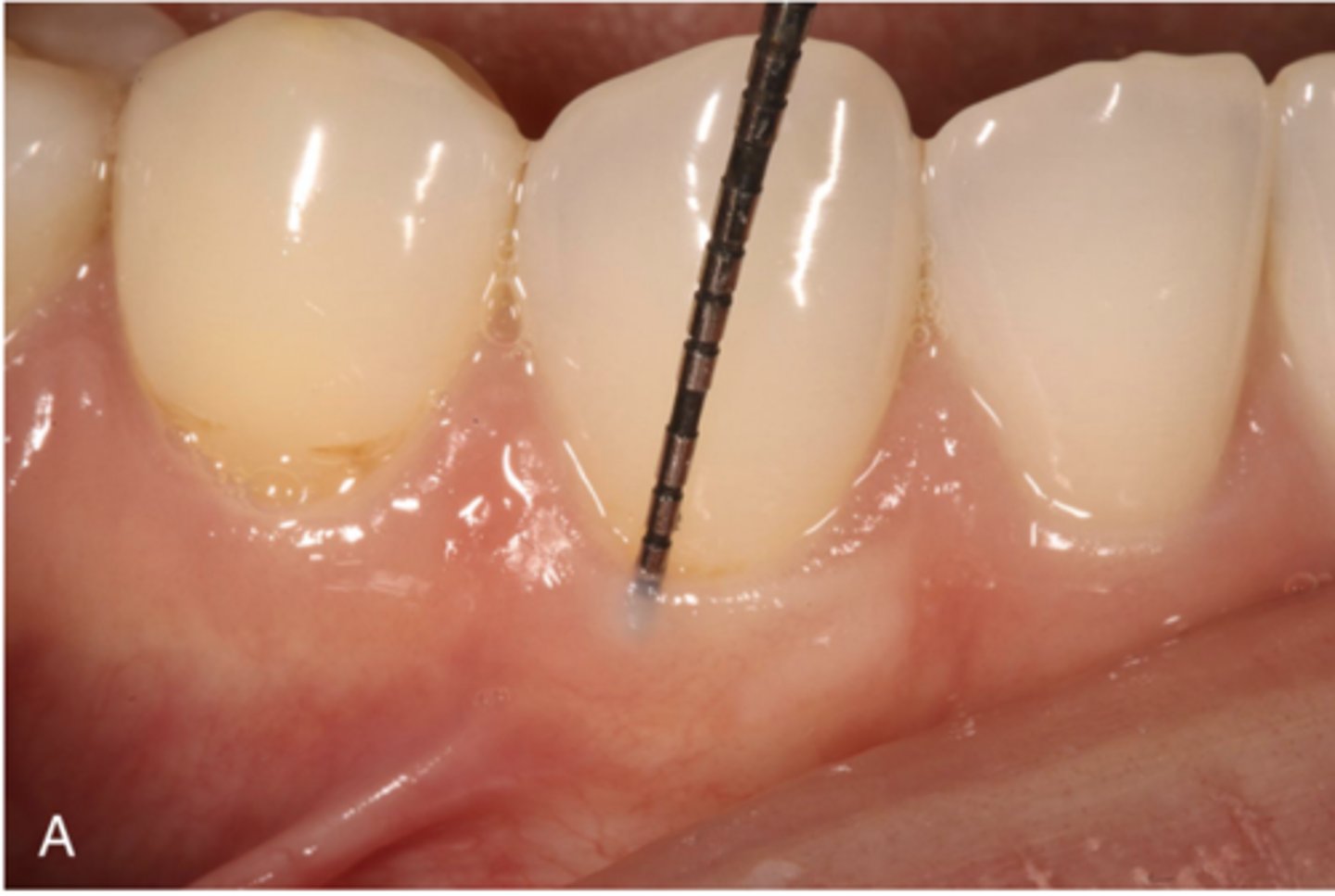
Attached Gingiva
The attached gingiva is continuous with the marginal gingiva (unattached). It is firm, resilient, and tightly bound to the underlying periosteum of the alveolar bone. It is demarcated from the relatively loose alveolar mucosa unattached gingiva by the MGJ
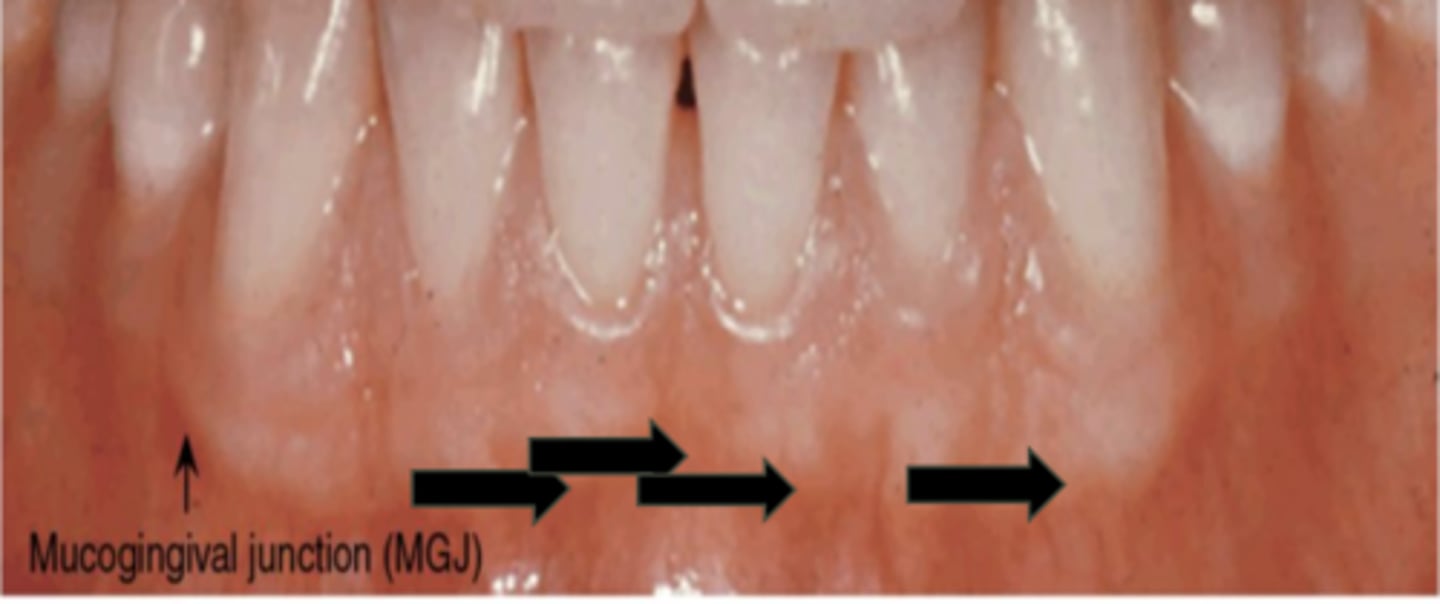
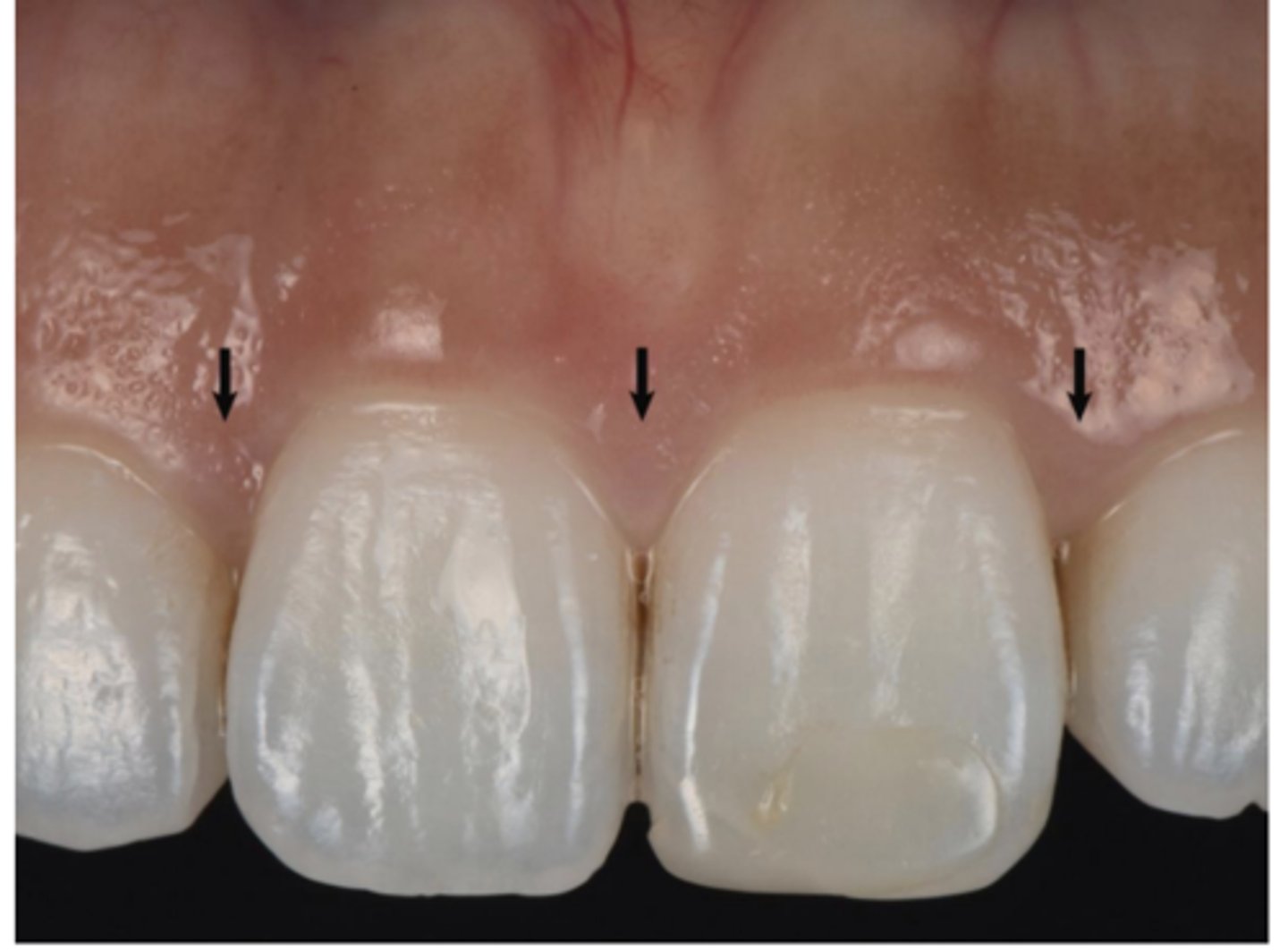
Interdental Gingiva
The interdental gingiva (between teeth) occupies the gingival embrasure, which is the interproximal space beneath the area of tooth contact. The interdental gingiva can be pyramidal, or it can have a "col" shape. The shape of the gingiva in a given interdental space depends on the presence or absence of a contact point between the adjacent teeth, the distance between the contact point and the osseous crest Serves to protect underlying osseous structure
Cementum
Thin layer of calcified connective tissue that covers the tooth from the CEJ to and around the apical foramen
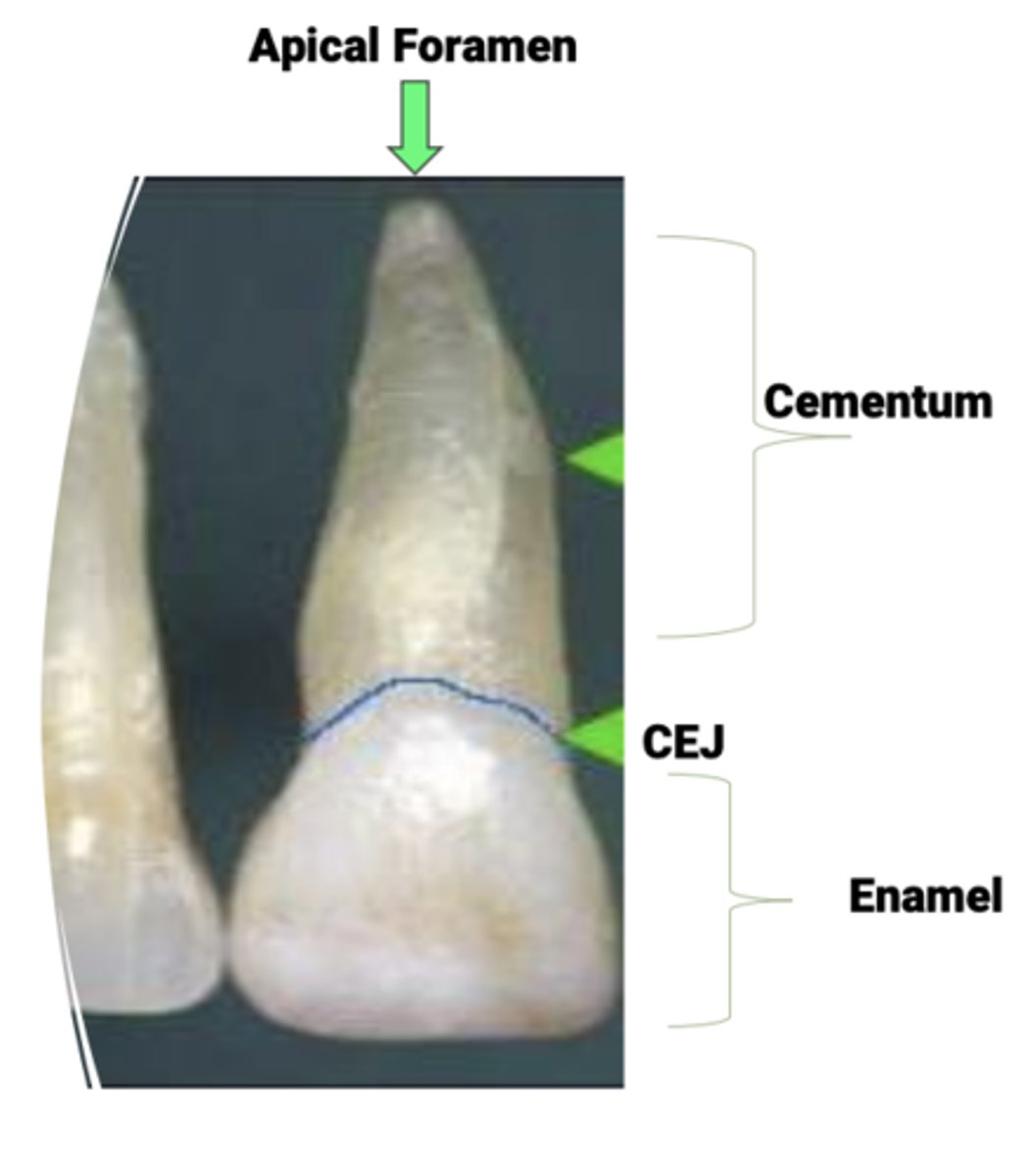
Cementum function
Supports the tooth along with the alveolar bone by serving as the attachment for periodontal fiber groups of the PDL
Seals the tubules of the root dentin
Cementum: Characteristics
50-200 microns thick (very thin)
Thickness increases with age
Two types
- Acellular cervical half to two thirds of the root and is where the PDL attaches
- Cellular apical third or half and serves to repair tissue to fill defects
Alveolar bone
The alveolar bone is a specialized part of the mandibular (lower jaw) and maxillary (upper jaw) bones with primary function to support the teeth
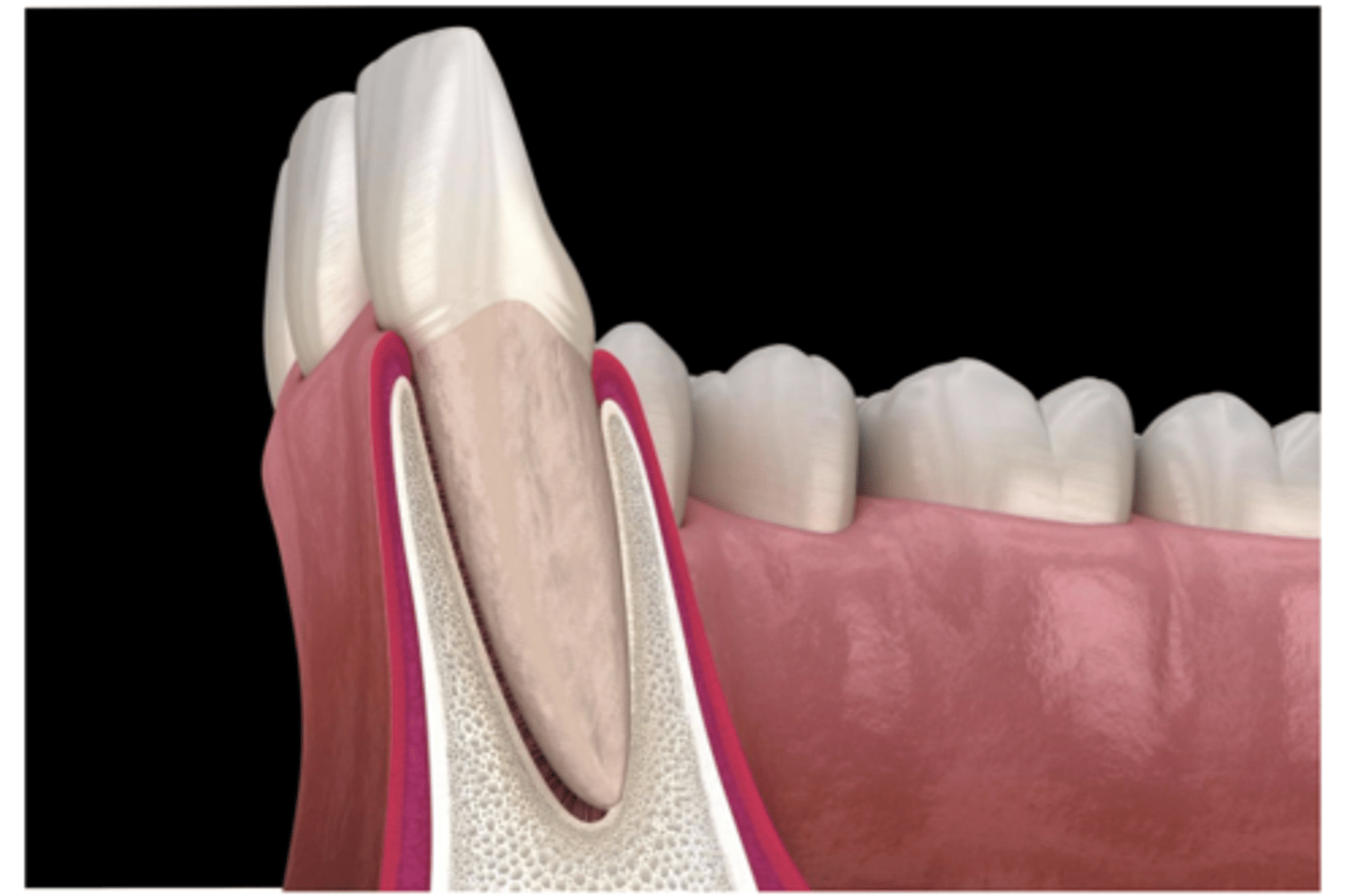
Alveolar bone function
Undergoes rapid and continual remodeling due to demands of tooth eruption orthodontic tooth movement and occlusal forces
The architecture is similar to other bone tissues, but the rate of remodeling is unquie to alveolar bone. When teeth are lost the alveolar bone is progressively resorbed
Periodontal ligament
The PDL is the fibrous connective tissue that surrounds and attaches the alveolar bone to the cementum
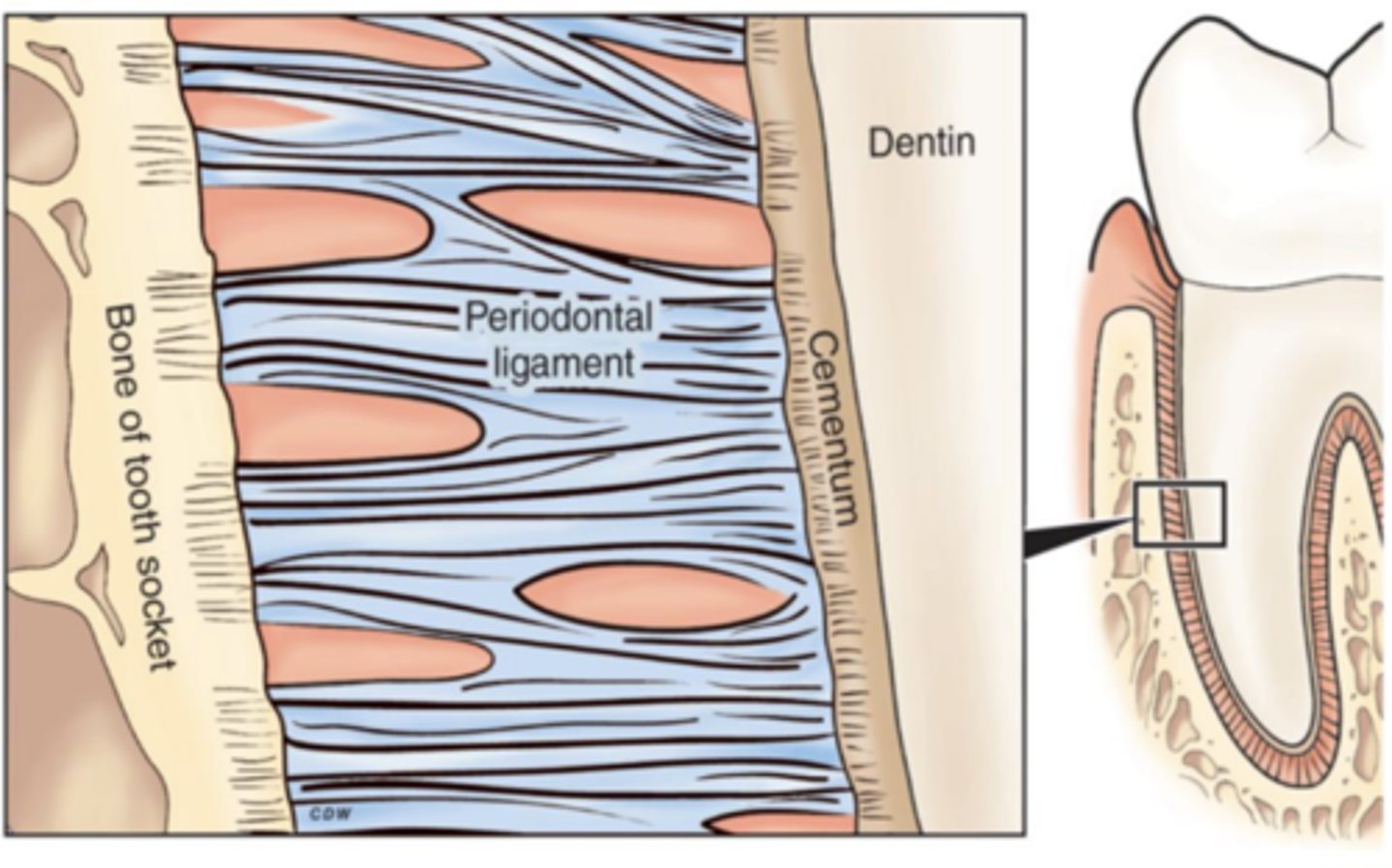
Functions of the PDL
acts as interface between bone and tooth and allows for movement to distribute the chewing forces (ligament in medicine is bone to bone)
Composition of PDL
It is composed of cells and an extracellular compartment. Cells include osteoblasts, osteoclasts, fibroblasts, epithelial cells, and cementoblasts (HAS CELLS)
The extracellular compartment contains collagen fiber bundles in a ground substance
Inflammation cardinal signs
Red
Heat
Swelling
Pain
Loss of function
Gingival health
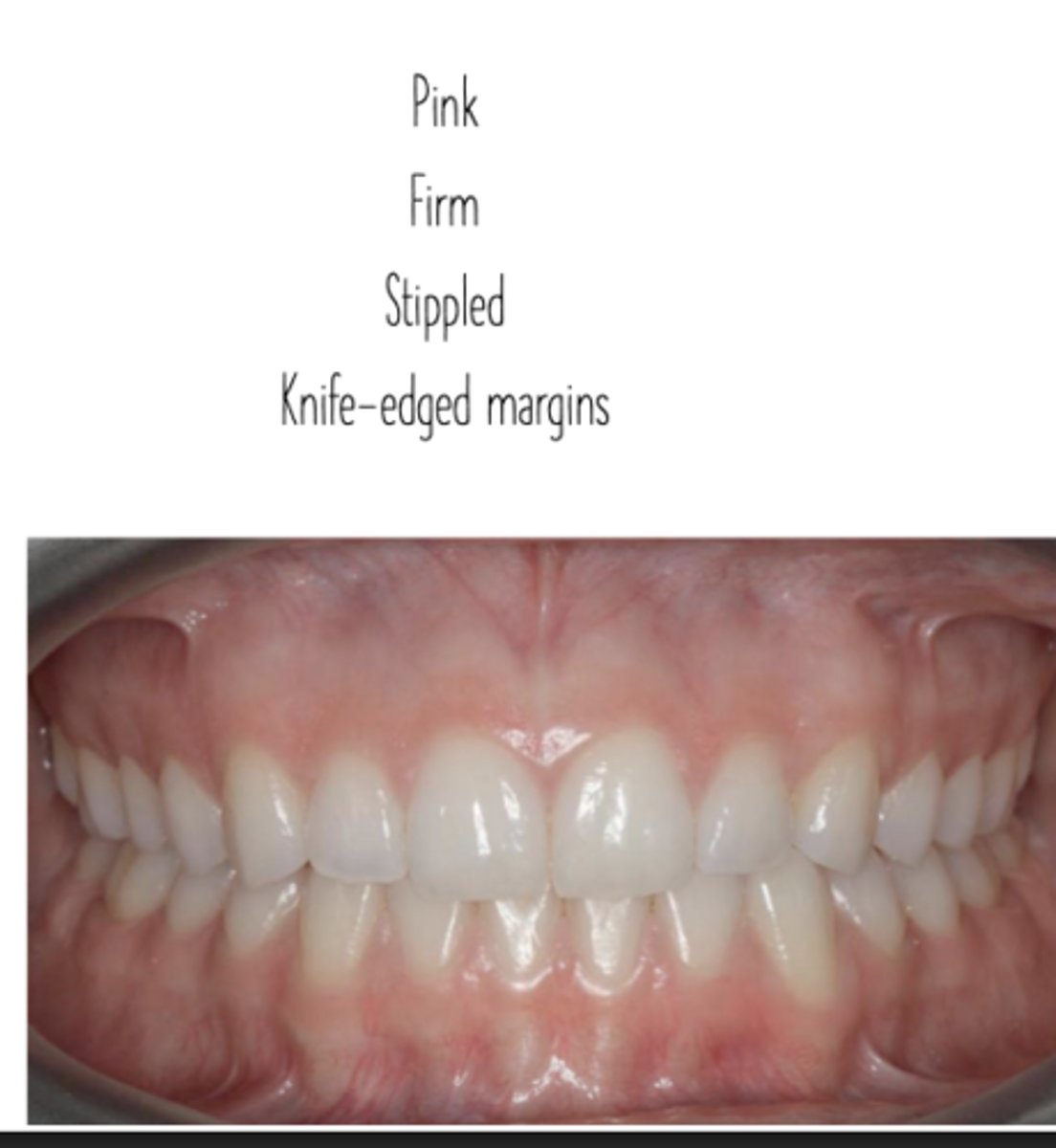
Gingival Inflammation
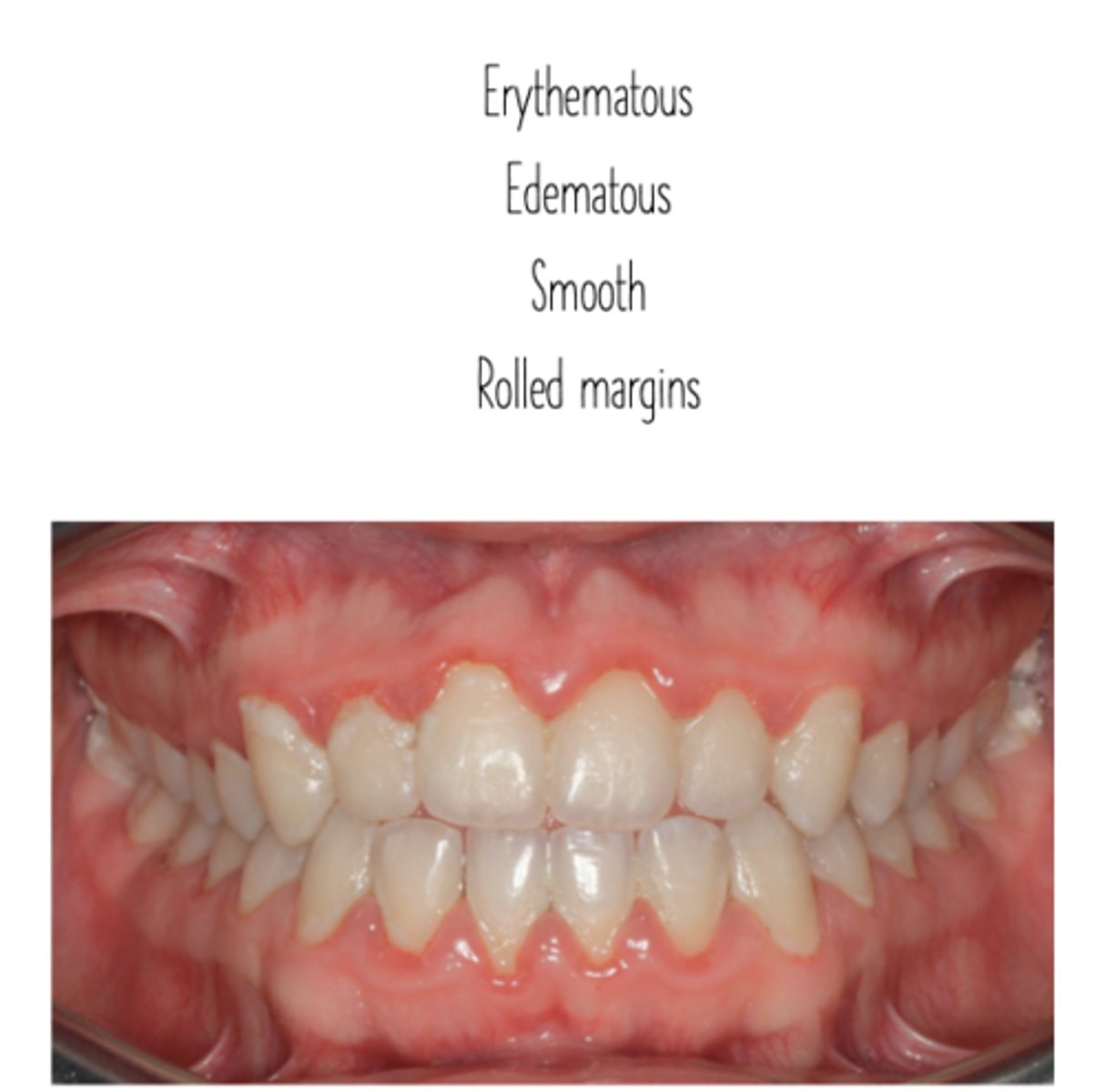
Gingivitis Affects
just the gingiva
Gingivitis is inflammation that is
reversible
- no bone loss
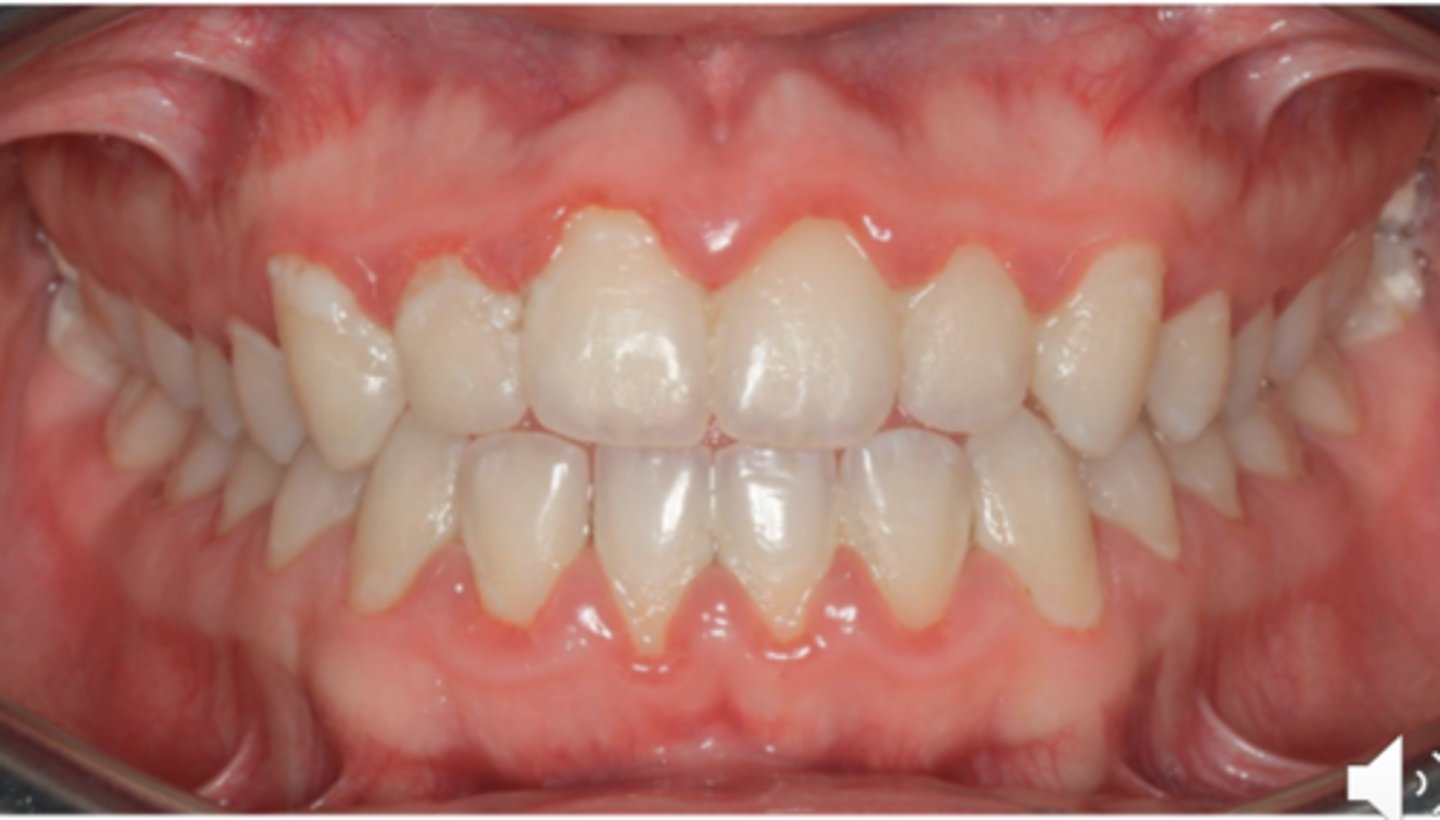
Periodontitis
Presence of inflammation at the sites where there is loss of alveolar bone and connective tissue
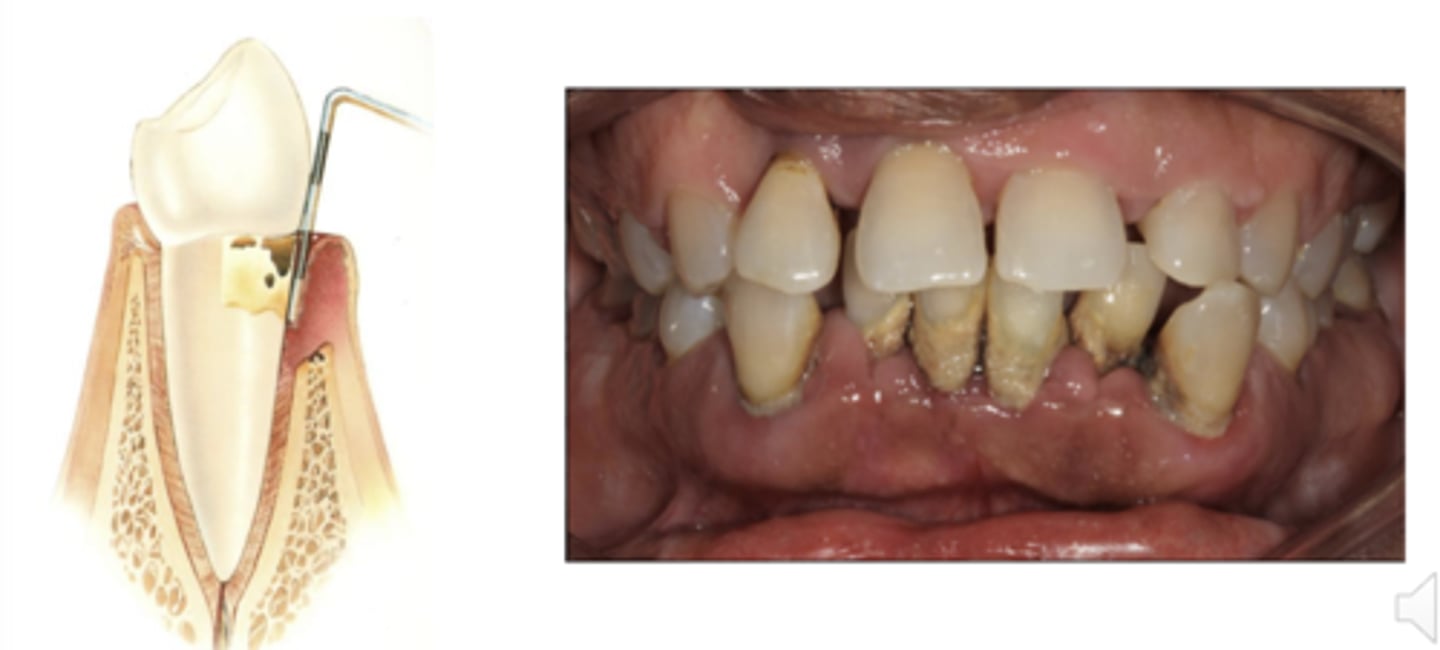
Periodontitis is not
reversible
Progression of periodontal disease
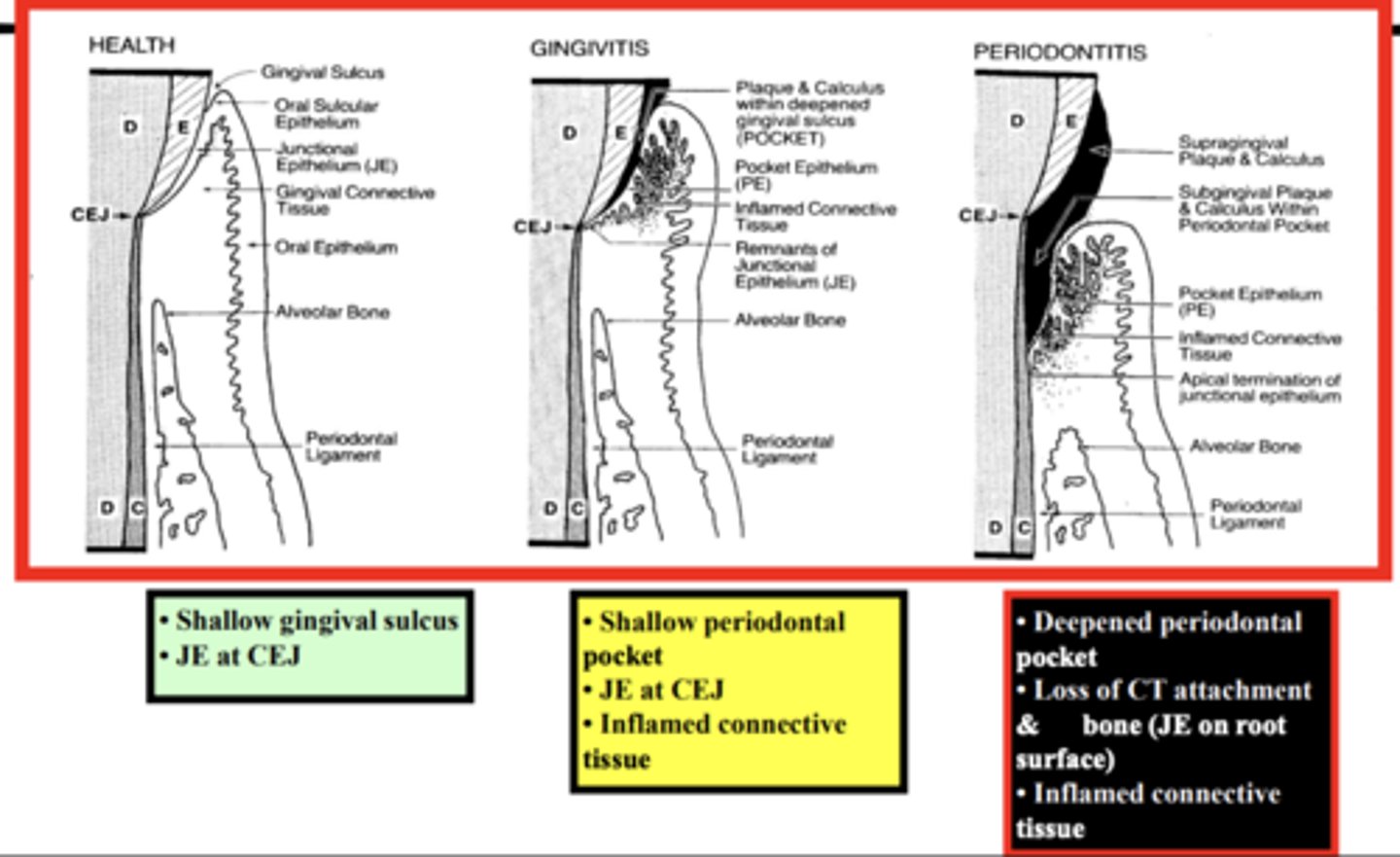
END
FIN