B Cell Dev
1/13
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
14 Terms
Describe B Cell Dev:
Location?
Initiation via?
Describe what happens when Pro-B → Pre-B
B Cell Dev:
Location:
mainly in bone marrow
Initiation:
via direct interaction of stromal cells
VCAM-1 (stromal) - VLA-4 (pro-B-cell)
Both are adhesion molecules
other CAMs are also invovled
Once contact has been made → C-kit (Pro-B-Cells) - SCF (stem cell factor; stromal
Pro-B → Pre-B
has IL-7 receptors
IL-7 is produced by stromal cells
req. for continued growth and maturation
Adhesion molecules on pre-B cells = down-regulated → pre-B cells detachment from stromal cells
Describe Stromal Cells
What are they?
Functions?
Describe Immunoglobulin genes
What are they?
Location?
Importance?
Stromal cells
What are they?
Nonlymphoid cells located in bone marrow
Functions:
Provide microenvironments for B cell maturation
Interact w/ pro/pre-B cells
Secretion of several cytokines, including IL-7
Immunoglobulin genes
What are they?
multiple-gene segments in the germ-line
Location:
Carried in the germ cells
Importance:
Must be rearranged into functional genes
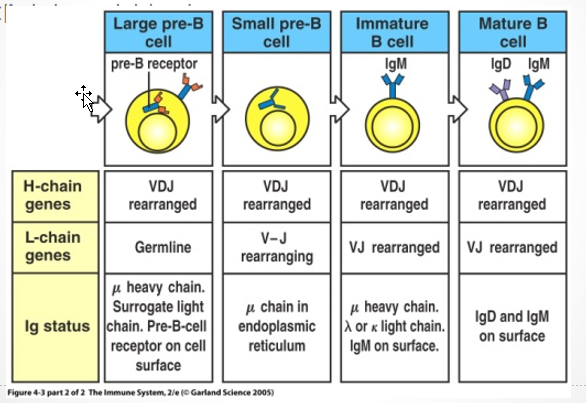
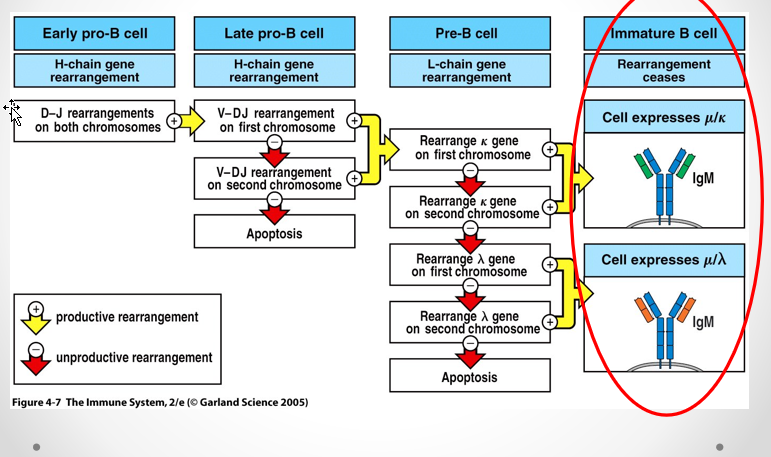
List and describe what happen in each B-cell developmental Stage
Pro-B cell
Early pro
Heavy-chain DH to JH gene rearrangement
Late Pro
VH to DH JH rearrangement
Upon completion of Heavy chain rearrangement → Pre-B Cell
NOTE:Earliest identifiable cell in the B-cell maturation process
Pre-B Cell
Expression of pre B-cell receptor
μ chain + Igα/β polypeptides (surrogate light chain molecule)
Surrogate light chains = not true immunoglobulin proteins
only found in primitive B cell precursors
μ chain + surrogate light chains reach cell surface →
signal transmission → halt heavy chain rearrangement
Begins Light-chain rearrangement
surrogate light chains ceases + pre-B cell receptor disappears from surface + μ chain trapped in ER
Immature B-cell
light-chain gene rearrangement
Kappa (κ), or Lambda (λ)
Ig gene rearrangements completed
Def: Light chain + heavy chains rearrangements completed → creates specificity
express IgM on the cell surface
Mature B-Cells
Coexpression of IgD and IgM
via production of 2 mRNAs ( one for μ + δ )
Low expression of IgD
levels increases when cells goes towards lymphoid organs
Negative Selection:
If fail → Dev. arrest + additional rearrangement → tests again (final test)
Describe these diseases associated w/ B cell dev
Describe X-linked agammaglobulinemia
Pathophysiology
Consequences
Treatments
Describe Burkitt’s lymphoma (FAB L3)
pathophysiolgoy
Consequences
X-linked agammaglobulinemia
Pathophysiology:
B-cell development arrested @ pre B-cell stage → No circulating antibodies
b/c lack of essential signal transduction molecules
X-linked
Consequences:
recurrent infections from extracellular bacteria
Haemophilus influenzae
Streptococcus pneumoniae
Streptococcus pyogenes
Staphylococcus aureus
Treatment:
antibiotics and immunoglobulin from pooled blood
Burkitt’s lymphoma (FAB L3)
Pathophysiology:
MYC proto-oncogene (Chr8) + (translocation) immunogloblin heavy-chain gene (Chr14)
or to kappa light chain gene (Chr2)
or to lambda light chain gene (Chr22)
Consequences:
many B cells tumors
Describe B1 cells
Developmental Orgins:
Compared to B2:
Receptors:
Antibodies:
Lifespan:
Chronic lymphocytic leukemia (CLL)
Source:
Initiating event
Risk Factors:
Testing
B1 cells:
Developmental Orgins:
from stem cells during prenatal development
precedes dev. of B2 cells (normal B cells)
Compared to B2:
Cell Surface: CD5, CD86, IgM, and IgD (variable existance)
Not part of adaptive immune system
No memory cells
Rearranged heavy chain genes = less diverse
thus → low affinity antibodies
polyspecificity
Antibodies:
against common bacterial polysaccharides
not against protein antigens
no evidence of somatic hypermutation
Capable of self-renewing
dependent on IL-10
Receptors:
IgM + IgD receptors
more IgD then IgM
Antibodies:
Secrete IgM and IgG3 antibodies
IgG3
small percentage of IgG antibodies
potent mediators of effector functions compared to other IgG subclasses:
ADCC
opsonization
complement activation
neutralization
Lifespan:
eventually stop dev. in bone marrow
In adults: cell replications in peripheral circulation
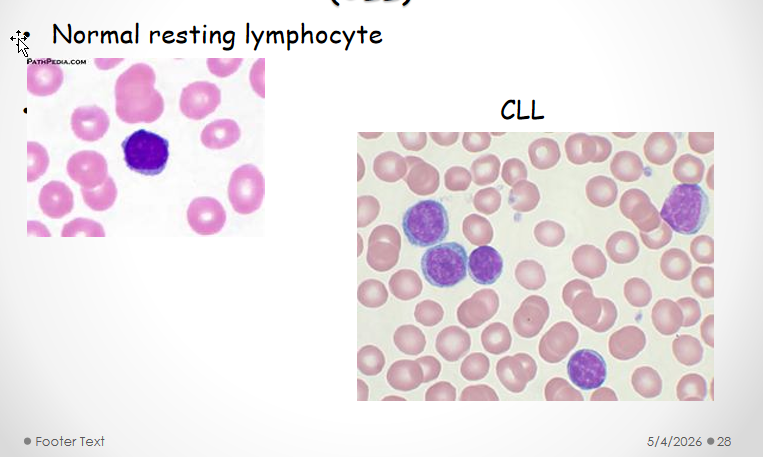
Chronic lymphocytic leukemia (CLL)
Source: B1 cells
Initiating event = unknown
Risk Factors:
Pesticides,
chemical fertilizers
Smoking
Heavy metals
Medical radiation
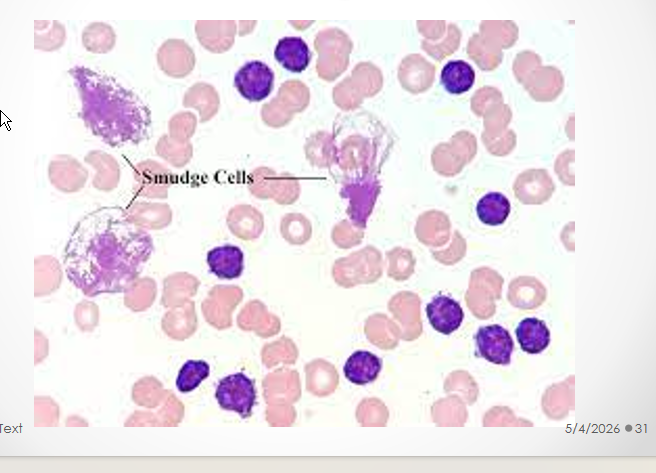
Testing: cannot withstand smear pressure → smudge cells
What happens when B cell Dev is complete
After B cell development is complete
mature, naïve B cell leaves bone marrow → Recirculates between btw blood/secondary lymphoid tissues
secondary lymphoid tissues is where B cells encounter antigen
B Cell Activation
Activation Steps
Effects
Describe ofmration of primary follicle
B Cell Activation:
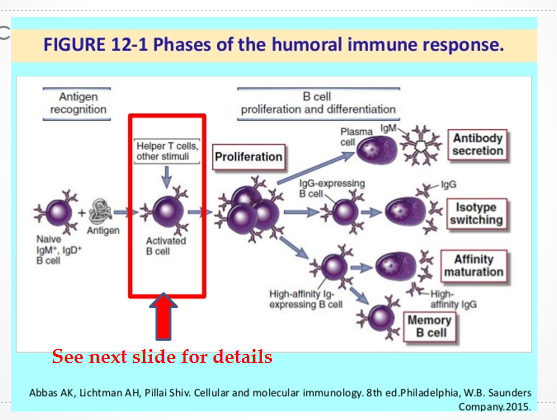
B cell encounters antigen → held in T cell areas → activated by CD4 T-Helper Cells → proliferate + dif. into plasma cells (in lymph nodes and spleen) → change in heavy-chain mRNA processing → synthesis of secreted form of Immunoglobulin
Effects:
Antibody Secretion
Isotype Switching
Affinity Maturation
Memory B Cell formation
Describe Primary Follicle Formation:
DC w/ antigen → migrate from Subcapsule to paracortical area (of LN) → interact w/ T cells (migrating through HEV) → B cells travels through HEV → pass through paracortex/primary follicle → interacts w/ T cells → both T/B proliferate to form primary focus
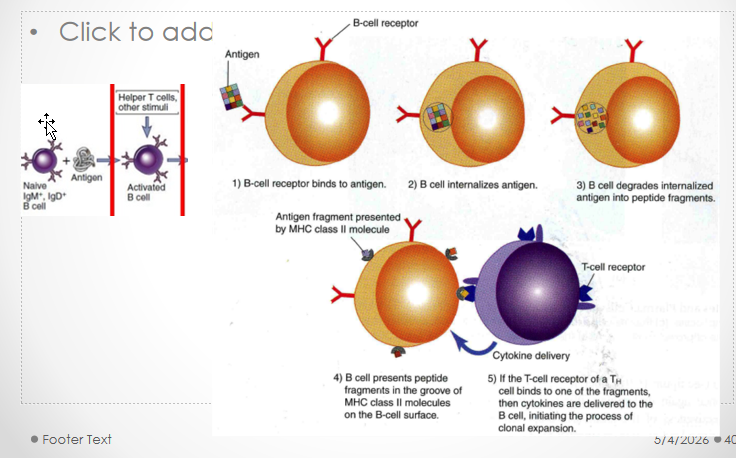
Describe Plasma Cells
Function
Properteis
Plasma Cells:
function:
constitutive synthesis and secretion of antibody
protein synthesis cellular organelles = highly dev.
10-20% of total protein is antibody
Properties:
Terminally differentiated and cease to divide
Does not express cell-surface immunoglobulin or MHCII molecules
can’t respond to antigen/interact w/ T cells
Life span = 4 weeks
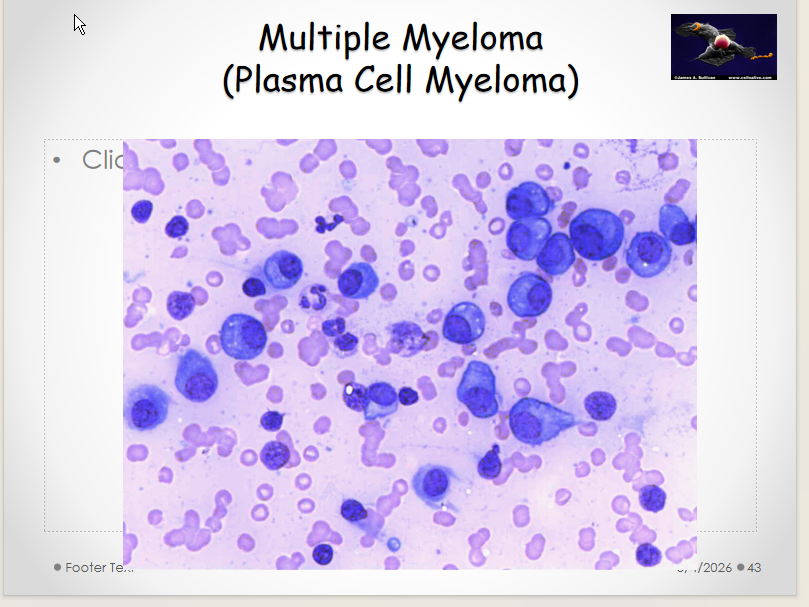
Describe Multiple Myeloma
Pathophysiology
clinical manifestations
Multiple Myeloma and Calcium
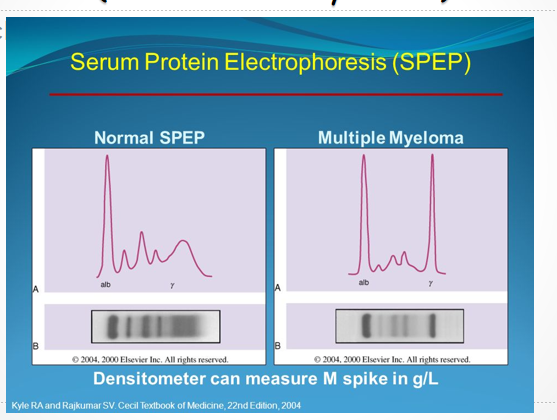
Multiple Myeloma
Pathophysiology:
Loss of control over B cell proliferation/antibody production
chromosomal translocation: heavy chain genes + oncogene → genomic instability → additional mutations and translocations
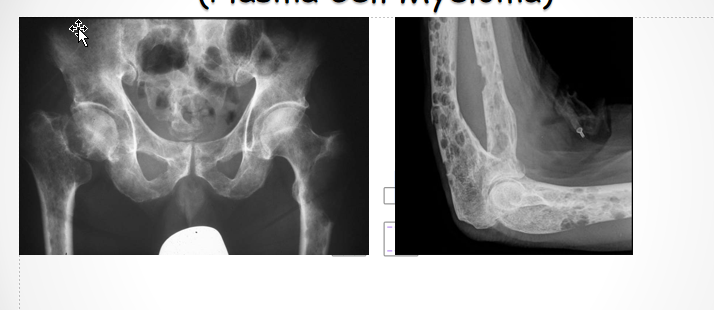
Clinical Manifestations
Pain in the lower back, long bones or ribs
Generalized malaise
Infections
fever
Bleeding
Symptoms of hypercalcemia
Nausea
Fatigue
Thirst
Symptoms of hyperviscosity
Headaches
Bruising
Ischemic neurologic symptoms
Other neurologic symptoms
Peripheral neuropathy
Meningitis
Multiple Myeloma and Calcium
RANKL
membrane protein belonging to TNF family
High Expression: lungs, thymus, lymph nodes
Low Expression: bone marrow, stomach, peripheral blood, spleen
Function: bone regeneration and remodeling control
Multiple Myeloma → overexpression of RANKL → act. osteoclasts → hypercalcemia