Lecture 13: Bandaging & Bandaging Techniques - SA
1/52
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
53 Terms
What are the goals of a bandage?
protect wounds and speed wound healing
What are the major potential bandage complications?
result in limb amputation or can kill your patient
What are the advantages to bandages?
• Provide wound cleanliness
• Control wound environment
• Reduce edema & hemorrhage
• Eliminate dead space
• Immobilize injured tissue
• Minimize scar tissue
• Make patient more comfortable
What are the disadvantages with bandages?
• Patient discomfort
• Patient mutilation of bandage & wound
• Bacterial colonization of wound
• Ischemic injury
• Damage to healing tissues
• Become GI foreign body obstruction
What are indications for bandages?
typically used below elbow & stifle
treating injuries - reduce pain, swelling, local tissue damage
protecting wounds or devices
for transport
What bandage technique immobilizes the limb, decreases/limits soft tissue swelling, and absorbs wound exudate, but the fracture MUST be below the elbow/stifle?
modified robert jones
What are the three basic layers of a bandage?
primary (contact layer)
secondary (intermediate layer)
tertiary (outer layer)
What is the function of the primary bandage layer?
• Debrides tissue
• Delivers medication
• Transfers wound exudate
• Forms occlusive seal
• Minimizes pain
• Prevents excessive loss of body fluids
What is the function of the secondary bandage layer?
• Absorbs & stores deleterious agents
• Retards bacterial growth
• Pads wound from trauma
• Splints wound to prevent movement
• Holds primary bandage layer in place
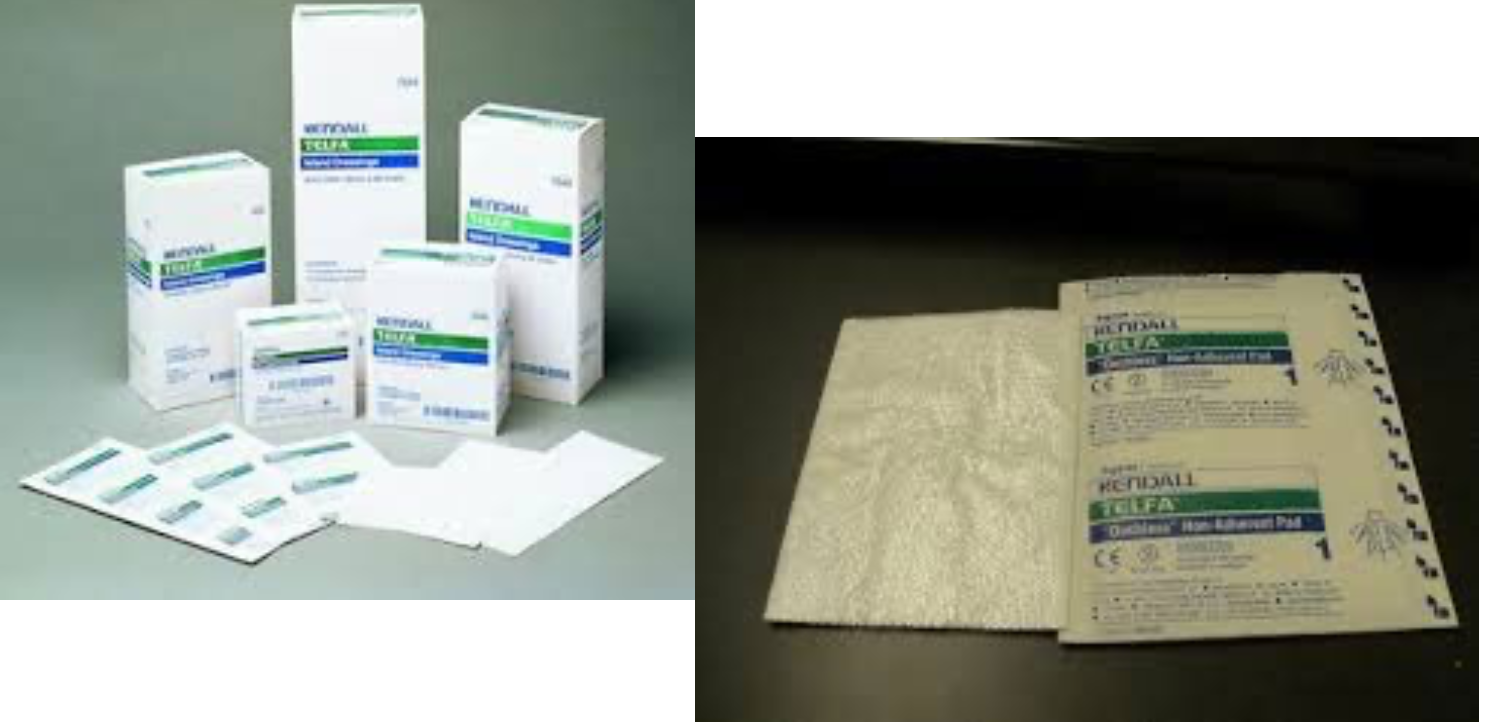
What bandage layer is this?
primary

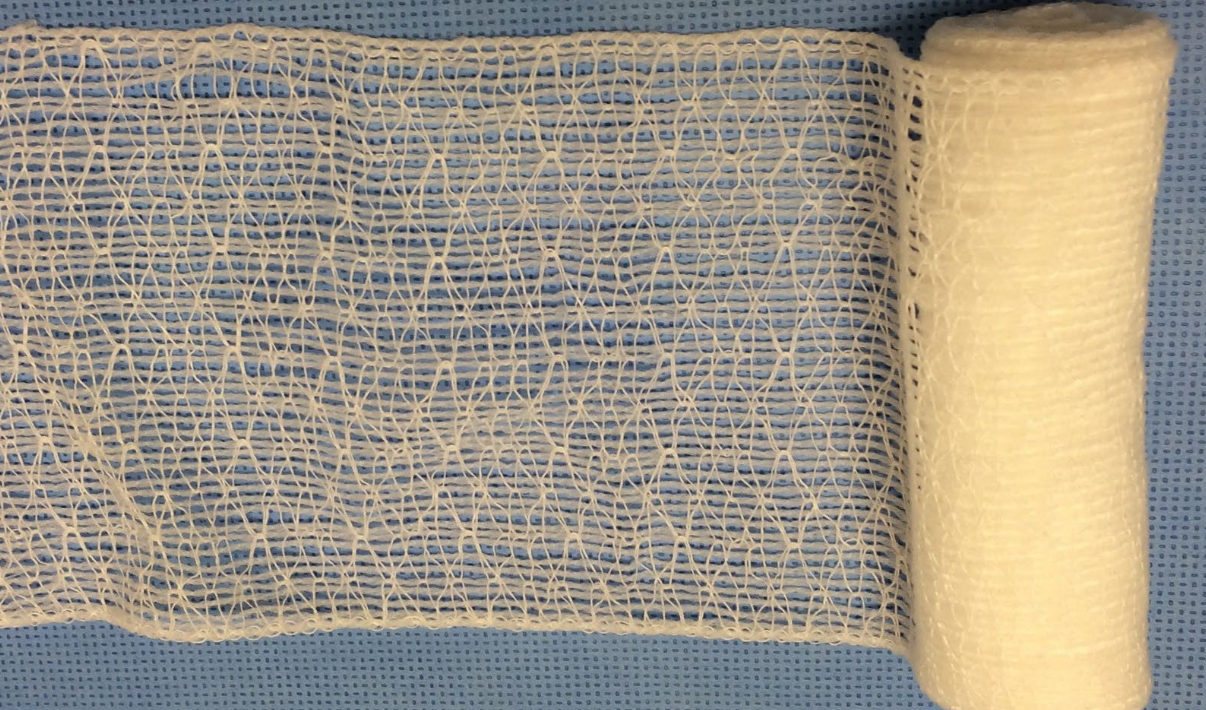
What bandage layer are these?
secondary
What is the function of the tertiary bandage layer?
• Holds other bandage layers in place
• Protects against external bacterial colonization
• Cosmesis

What bandage layer is this?
tertiary
What are the four types of primary bandage layers?
• Adherent
• Nonadherent
• Occlusive
• Semi-occlusive
What is the primary/contact bandage layer selection based on?
• Phase of wound healing
• Amount of exudate
• Wound location & depth
• Presence of absence of eschar
• Amount of necrosis or infection
What type of primary bandage layer is used when wound debridement is require and may be wet or dry?
adherent
What type of primary bandage layer is used during repair phase or if no necrotic debris, retains moisture to promote epithelialization & prevent dehydration, and drains excess fluid and prevents maceration?
nonadherent
What type of primary bandage layer is impermeable to air and is used on nonexudative wounds to keep moist and in partial thickness wounds w/o necrosis or infection?
occlusive
What is the advantage to occlusive primary bandage layers?
speeds rate & quality of healing compared to dressings allowing desiccation
What is the most commonly used primary bandage layer that allows air to penetrate and allows exudate to escape?
semi-occlusive
What are the 5 steps to applying a soft padded bandage?
1. Tape Stirrups
2. Primary Layer
3. Secondary Layer
4. Tertiary Layer
5. Labeling
How are tape stirrups applied?
• Distal 1/3 of limb
• Medial & Lateral or Dorsal & Palmar/Plantar?
• Tabbed ends or tongue depressor to help separation
Why is cotton placed between toes in a modified robert jones/soft padded bandage technique?
decreases moisture build-up
increases patient comfort
(don’t forget dewclaw)
What bandage layer is nonadherent, can have medication, is usually sterile, and is wicking?
primary layer
What bandage layer is absorbent, supportive, and applied distal to proximal, overlapping, and with firm, even pressure?
secondary
How are the tape stirrups used when applying the secondary bandage layer?
separate tape stirrups
rotate stirrups proximally while twisting 180°
secure stirrups to underlying wrap
prevents distal slipping
How is the tertiary layer applied?
distal to proximal
overlapping
firm, even pressure
neatly - this is what client sees !!
What should be written on a bandage label?
date
initials
reminders
warnings
When is a tie-over bandage used?
when the wound is in an area inaccessible to standard bandaging techniques (ex. hip, shoulder, axilla, or perineum
How is a tie-over bandage placed?
Apply sutures or skin staples w/ loose loops around edges of wound
Apply primary & secondary bandage layers
Hold tertiary layer in place → Lacing umbilical tape or heavy suture through loose skin sutures or staples
When is a pressure relief bandage used?
usually over bony prominence
to treat/prevent pressure sores
When is a pressure bandage used?
control minor hemorrhage, edema, & excess granulation tissue (direct application of corticosteroid ointment to wound helps control excess granulation tissue)
the more convex the surface, the greater pressure exerted by dressing on tissue
When should wet adherent bandages be used and how are they used?
wound surface has necrotic tissue , foreign matter, or viscous exudate
sterile wide mesh gauze soaked in: sterile saline solution, 0.05% chlorohexadine solution
necrotic tissue & foreign material adhere to gauze & removed w/ bandage
When should dry adherent bandages be used?
when wound surface has loose necrotic tissue & foreign material
when wound has large quantity of low-viscosity exudate that does not aggregate
What is the purpose of robert jones bandages?
temporary immobilization of fractures (must be below elbow/stifle)
decreases/limits soft tissue swelling
absorbs wound exudate
What is the difference between the modified robert jones and robert jones bandage technique?
modified adds splint material
robert jones uses very large/thick bandage and rolled/sheet cotton and is wrapped w/ more compression
How should proximal extremity lesions be bandaged?
continue bandage up leg, around chest or abdomen & between legs to create spica type bandage
How is a paw bandage placed?
like leg bandage except digits are covered
after placing stirrups & contact layer, reflect cast padding over digits from dorsal to ventral - then ventral to dorsal
wrap padding around distal limb
conform bandage to limb w/ elastic gauze
secure bandage w/ elastic tape in similar fashion
What are the disadvantages of a traction splint (shroeder-thomas splint)?
labor intensive
soft tissue complications
lacks predictability
What is a spica splint used for?
immobilization of shoulder
What is a ehmer sling used for?
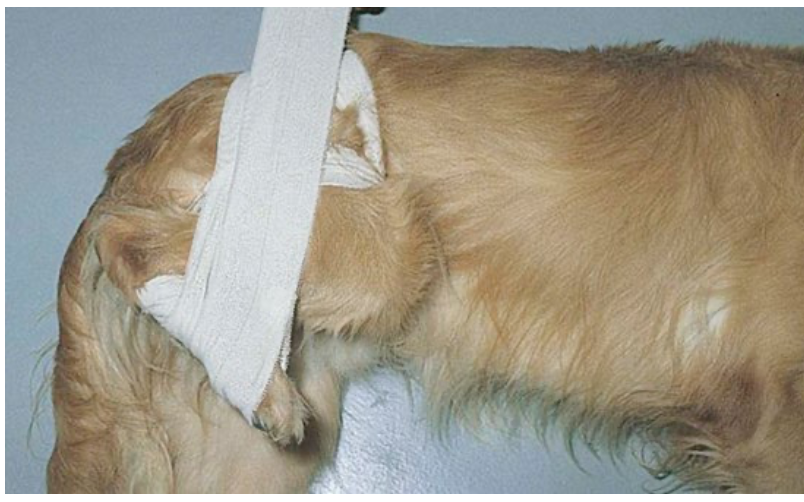
prevents pelvic limb weight bearing post hip reduction or acetabular fractures
What is a velpeau sling used for?
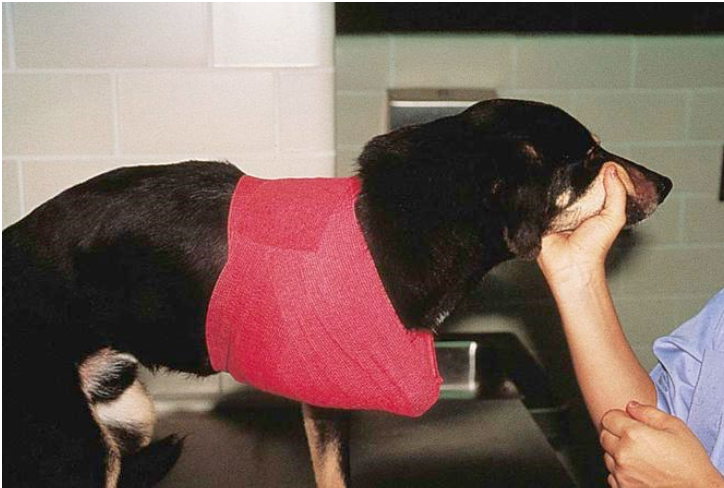
prevents forelimb weight bearing after shoulder/forelimb procedures
When are casts used for fractures?
stable minimally displaced fractures
young rapidly healing animals
only injuries distal to elbow/stifle
unable to repair w/ surgical techniques
What type fracture should NOT be casted?
open fractures
What should always be done after casting?
radiographs: must have >50% overlap of fracture ends in each of 2 radiographic views
Why should a cast be placed with the limb in a standing position?
encourages use when walking
limits muscle atrophy & joint stiffness
shortens recovery period after removal
What are some common complications of casts?
• Slipping / loosening
• Water or urine-soaked
• Joint stiffness & muscle atrophy
• Pressure sores: Hard materials or constricting bands, Prominences
Bandage change frequency depends on:
age
activity
cleanliness
associated wounds
swelling
What are signs to remove a bandage?
odor
swelling
changes in toe temperature compared to other foot
nail bed cyanosis
What should be left exposed when bandaging?
middle 2 toes (claws) when possible
Bandages start at toes & go up limb to avoid _______.
swelling
What is the tension applied during bandage application proportional to?
the amount of padding and size of patient
How much of your bandaging should overlap?
1/3-1/2 the width of your wrap