micro chapter 17, unit 4
1/20
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
21 Terms
hypersensitivities
Immune responses that cause tissue injury
Autoimmune disease
occurs when the immune system attacks self-antigens
Type I: Immediate IgE-mediated
Type II: Cytotoxic
Type III: Immune Complex-mediated
Type IV: Delayed Cell-mediated
what are the 4 major times of hypersensitivities
Type I hypersensitivity
characterized by an allergic reaction in a sensitized individual within minutes of exposure to an antigen
ex anaphylactic shock, hay fever, hives, and asthma
Mechanism of Type I Hypersensitivity
A person becomes sensitized with first exposure to antigen (allergen).
B cells that are committed to producing IgE are activated by the antigen.
IgE activates mast cells or basophils upon second exposure to the antigen.
Mast cells and basophils release histamine and other cytokines.
Symptoms are related to the activity of histamine
Desensitization
Desensitization is a process where a patient is given gradually increasing doses of an allergen, starting at very low levels. This stimulates production of IgG antibodies, which bind the allergen before IgE, preventing mast cell activation and reducing the risk of anaphylaxis.
Type II hypersensitivity reactions
antibodies trigger the destruction of human cells
ex transfusion reactions and hemolytic disease of the newborn (erythroblastosis fetalis)
Transfusion Reactions
When an individual receives a transfusion of RBC’s that are antigenically different from his/her own (A, B, O, etc) the immune system destroys those cells
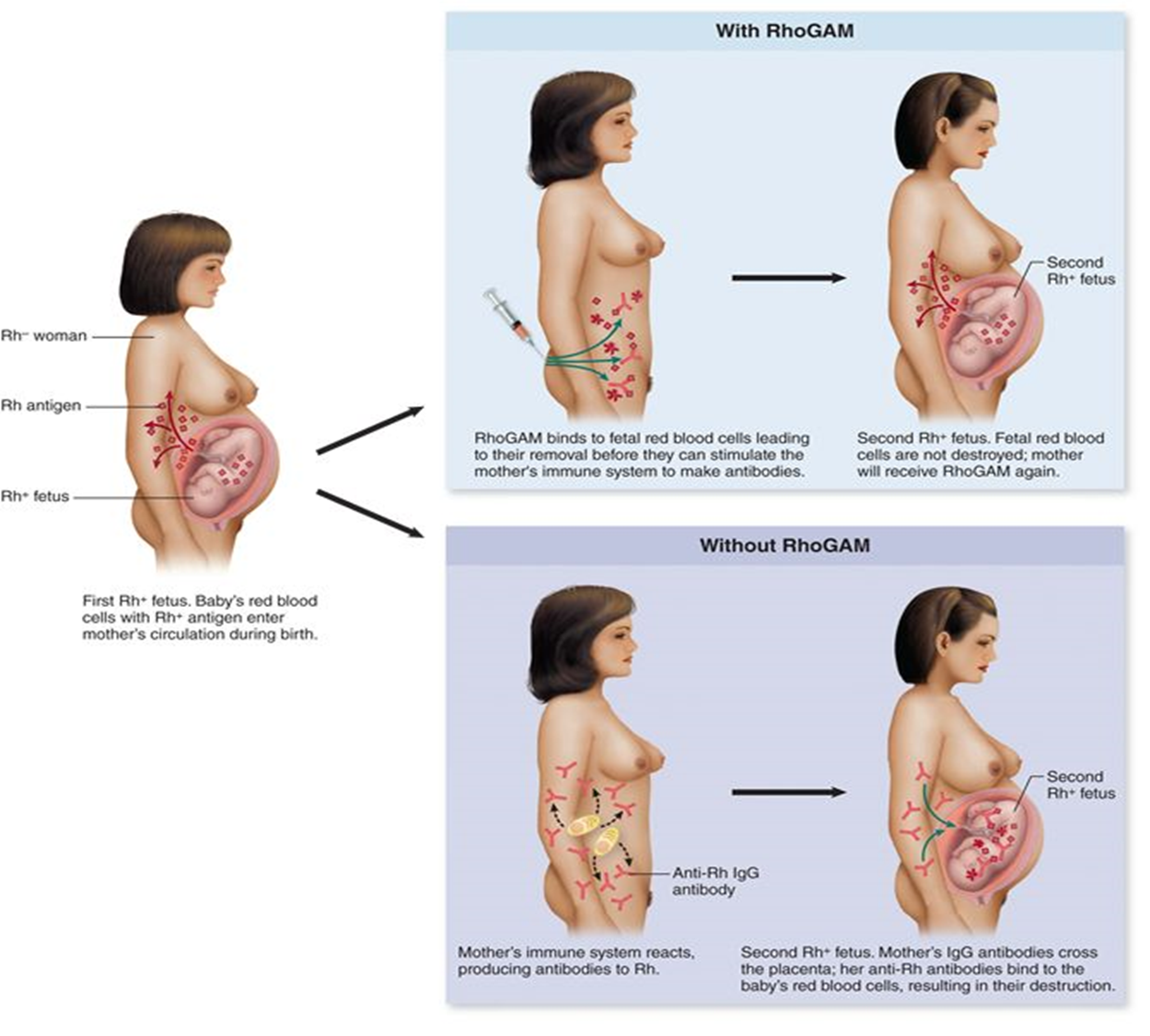
Hemolytic Disease of the Newborn
IgG antibodies against Rh antigen are produced by an Rh- mother following delivery of her first Rh+ child.
During subsequent pregnancies with Rh+ children, IgG antibodies cross the placenta and destroy fetal RBC’s
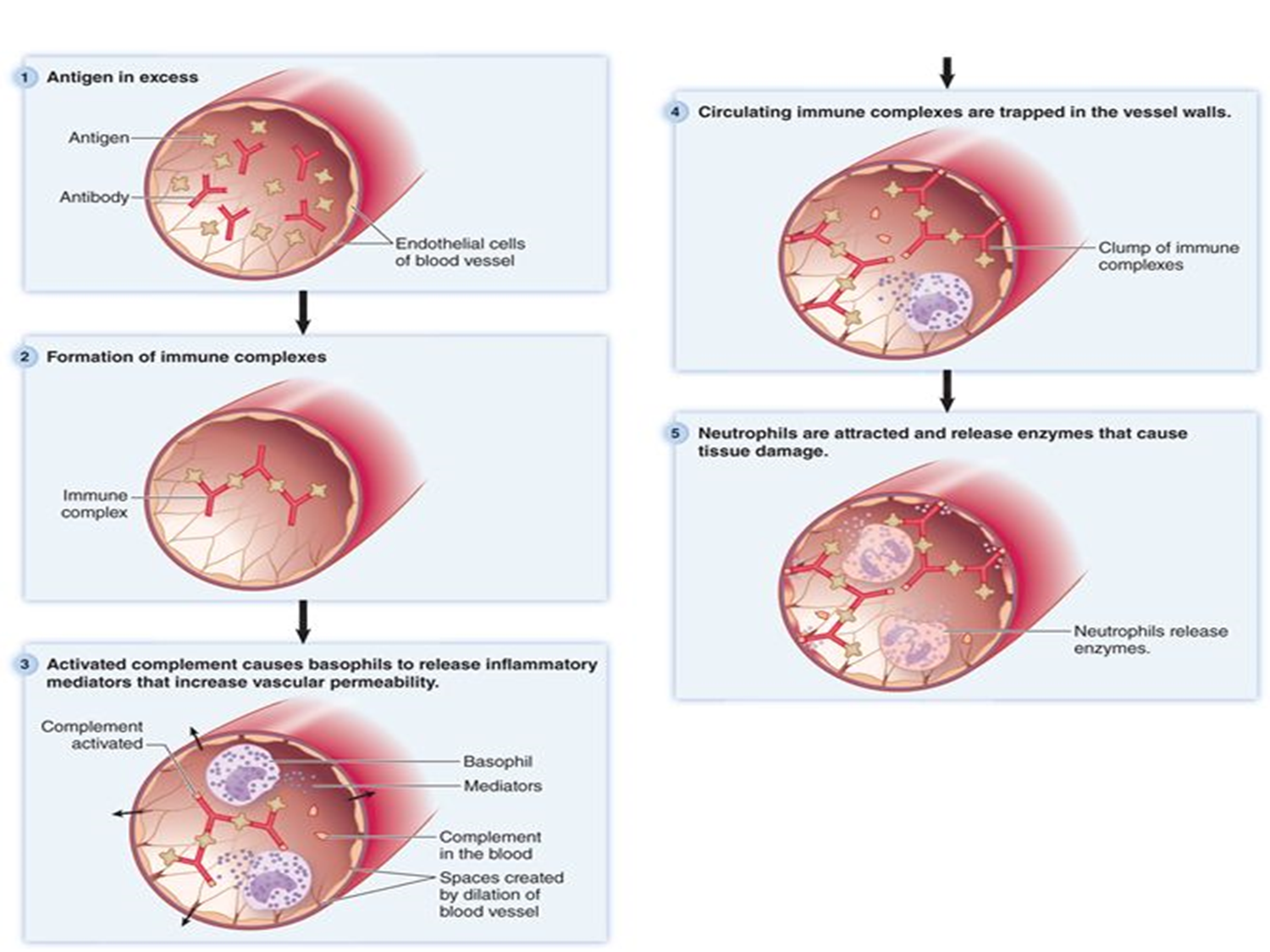
what is type III hypersensitivity and how can it cause disease
An immune complex is formed when IgG or IgM antibodies bind to antigens. Normally, they are cleared by macrophages, but when produced in excess, they deposit in small blood vessel walls (basement membranes), activate complement, and cause inflammation and tissue damage.
Examples of Type III hypersensitivity
post-streptococcal glomerulonephritis, Arthus reaction, and serum sickness
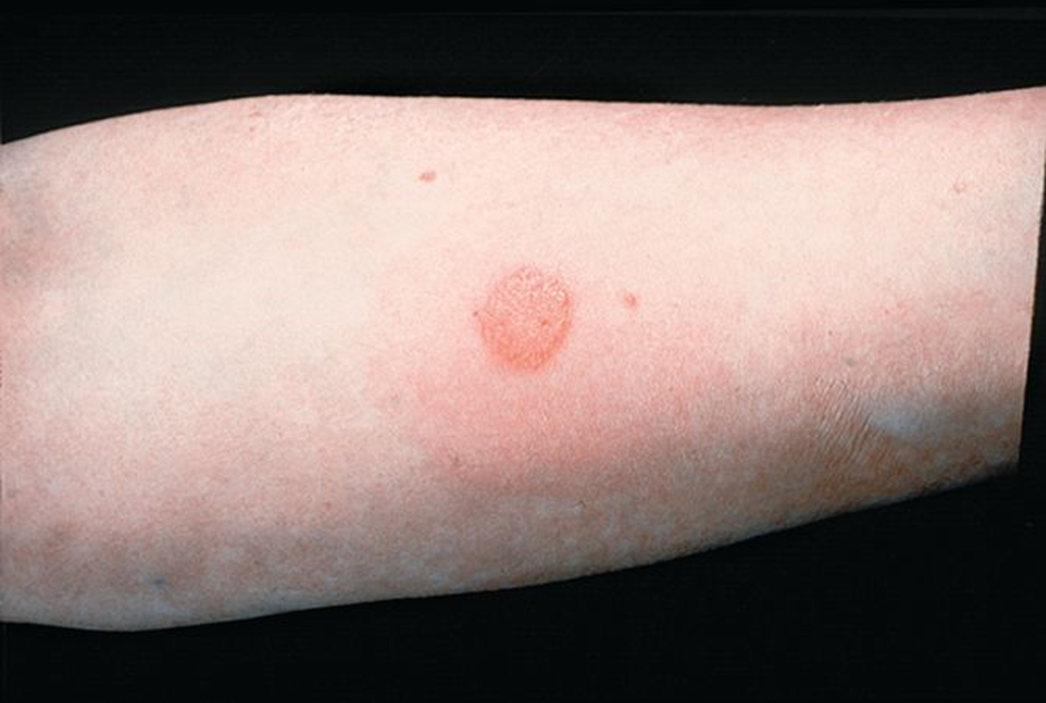
Type IV hypersensitivity is a T cell–mediated (delayed) immune response where sensitized T cells release cytokines, recruiting macrophages and causing inflammation. This leads to rash, blistering, and scaling in contact dermatitis. Common allergens include poison ivy/oak, metals, cosmetics, and latex.
What is Type IV hypersensitivity and how does it cause contact dermatitis?
Type IV Hypersensitivity
Delayed hypersensitivity results from the harmful effects produced by cell-mediated immunity.
The reaction peaks at 2-3 days rather than in minutes (as with Type I).
ex contact dermatitis, granuloma formation, and graft rejection
tuberculosis, leprosy, and histoplasmosis
what are the 3 infections that are responsible for granulomas?
granuloma
walls off intracellular infectious organisms, preventing the infectious microbe from escaping to infect other cells
Autoimmune disease
when the immune system responds to tissues of the body as if they were foreign
Immunodeficiency
when the body is incapable of making or sustaining an adequate immune response
2 categories
Primary Immunodeficiency
Secondary Immunodeficiency
Primary Immunodeficiency
genetic or developmental abnormalities result in dysfunctional B or T lymphocytes.
Secondary Immunodeficiency
result from environmental, rather than genetic, factors.
Caused by malignancies, advanced age, viral infections, immunosuppressive drugs, or malnutrition
DiGeorge syndrome (Primary Immunodeficiency)
the thymus fails to develop.
Therefore, T cells do not mature. Individuals suffer from repeated infections with eukaryotic pathogens, viruses, and obligate intracellular bacteria
Severe combined immunodeficiency(SCID) (Primary Immunodeficiency)
neither T nor B lymphocytes are produced in the bone marrow.
Children with SCID die of infectious disease at an early age without bone marrow transplant.