anesthesia maintenance and recovery
1/62
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
63 Terms
what are the 2 different ways we can maintain sedation/anesthesia?
1. IV- with continuous rate infusion/total intravenous anesthesia
2. inhalant, with volatile agents (using the anesthetic machine)
which is the better option for maintaining anesthesia- IV or inhalants?
inhalant- because it administers both O2 and gas. however, it is more expensive
what part of the anesthetic machine gives O2 to the patient?
flowmeter
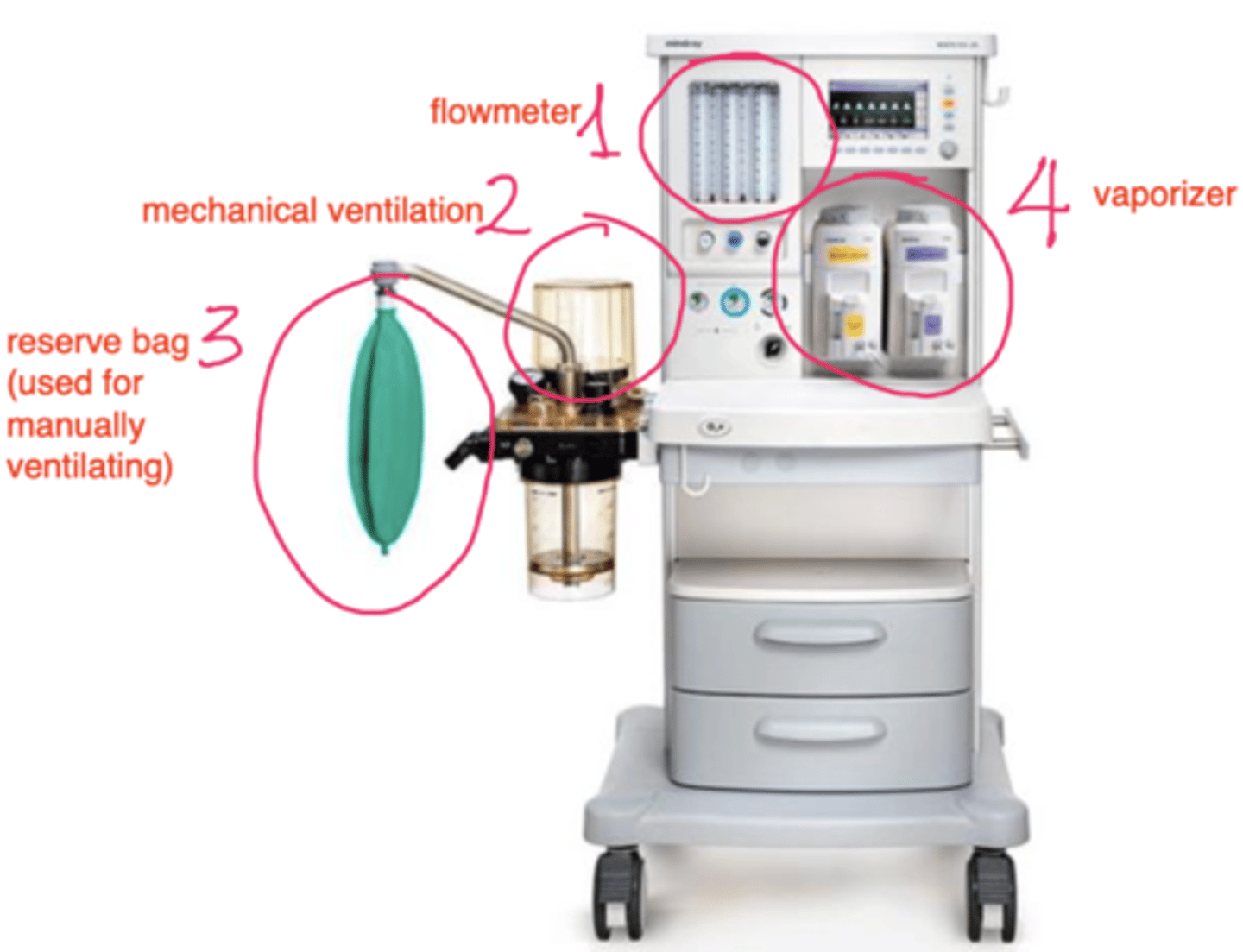
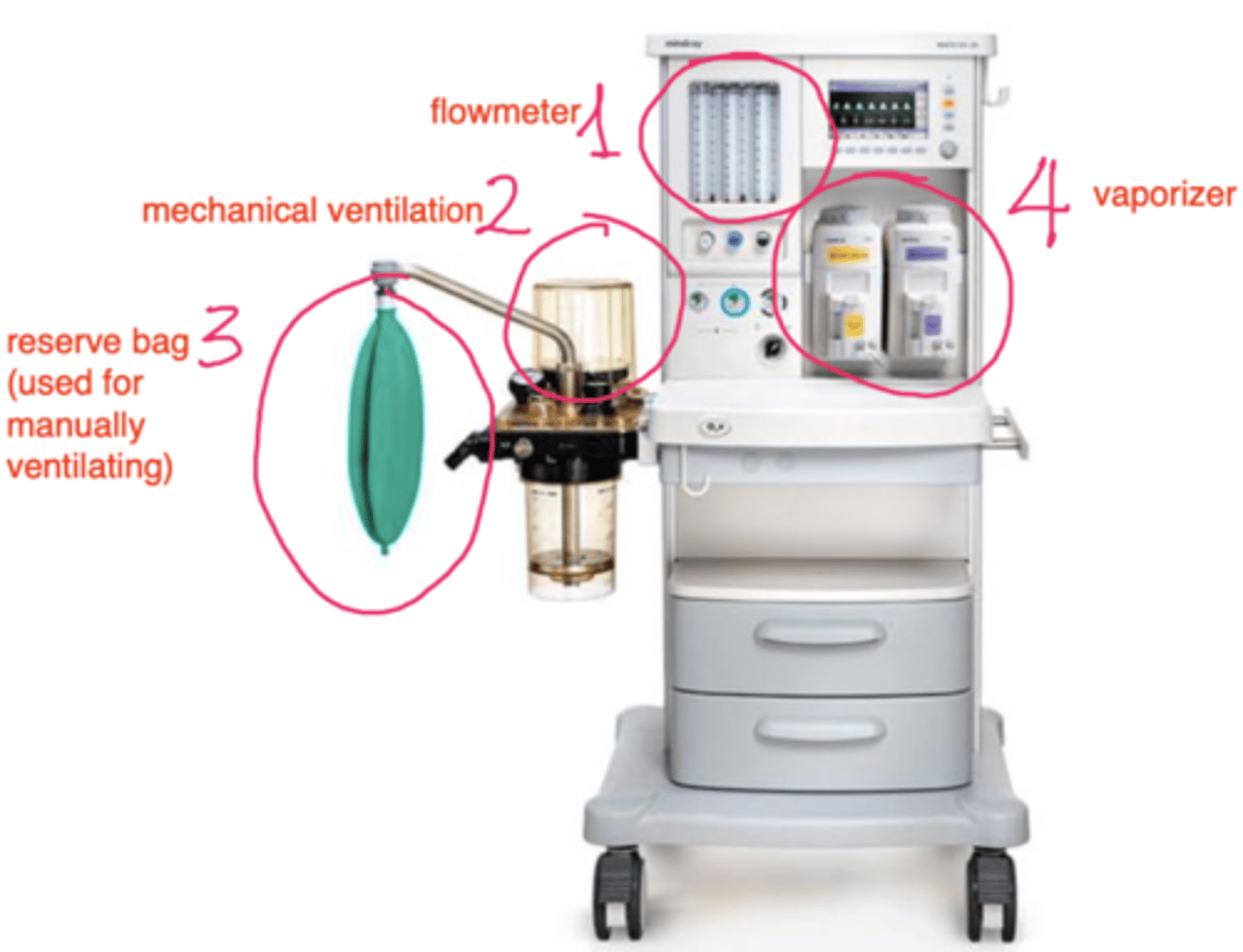
which part of the anesthetic machine gives anesthetic gas to the patient?
vaporizer
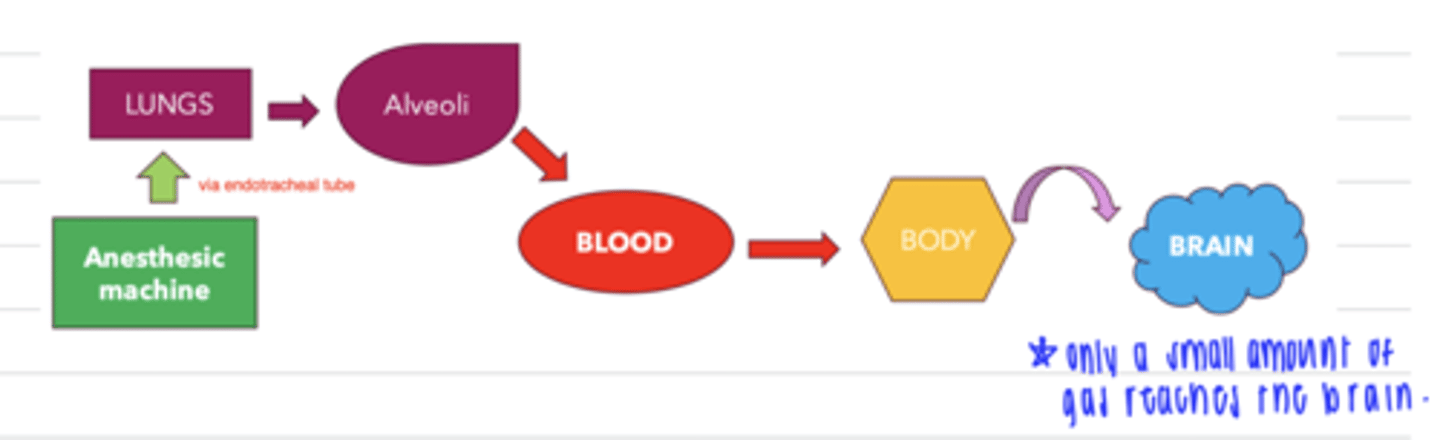
what is the pathway of volatile agents to the patient (starting from the anesthetic machine)?
anesthetic machine → lungs → alveoli→ blood → body → brain
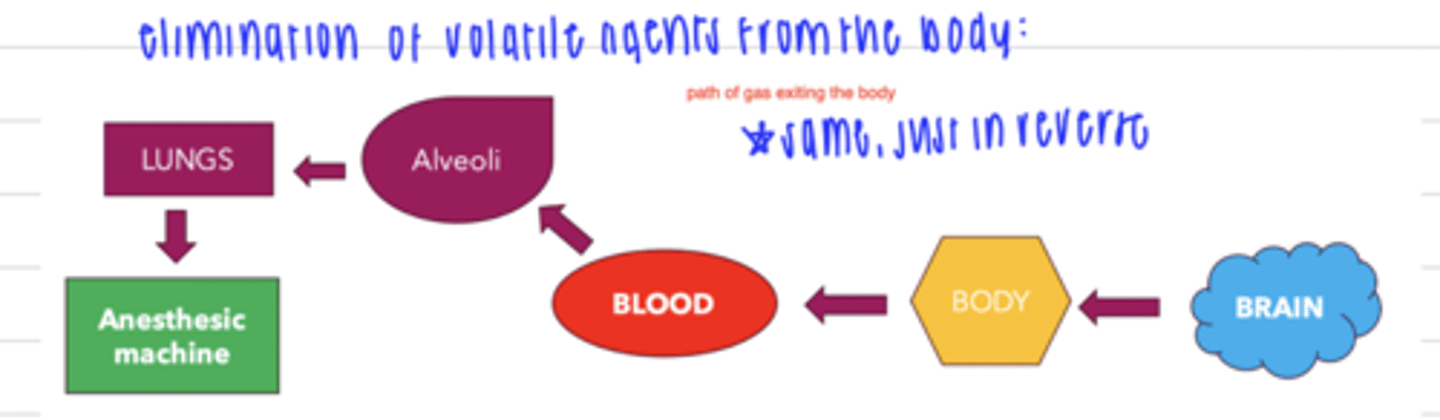
what is the pathway of volatile agents being eliminated from the body?
brain → body → blood → alveoli → lungs → anesthetic machine
the administration and elimination of volatile agents depends on _____
ventilation
what physiological component is necessary for the absorption and elimination of gas?
good alveolar perfusion
the pharmacokinetics of the volatile agents may be altered when _____ is impaired
ventilation or perfusion
if we have a good control of _______, we will have a good control of anesthesia
ventilation and BP
what are the 3 anesthetic gases we use in vet med?
isofluorane
sevoflourane
desfluorane
are the vaporizers good for use with any volatile agent, or are they specific to a certain type?
they are each specific for a certain type of gas.
we cannot use a vaporizer with a gas that it is not meant for.

what is the MOA of the volatile agents?
they affect the GABA receptors
if a gas is more soluble, will there be a slower or faster induction/recovery?
SLOWER

a less soluble gas will have a _____ (longer/shorter) induction and recovery time?
shorter

which- isofluorane, sevofluorane, or desfluorane, is the most soluble?
isofluorane

which- isofluorane, sevofluorane, or desfluorane, is the least soluble?
defluorane

anesthetic gases are eliminated via :
exhalation
are most volatile agents metabolized?
no, most are eliminated unchanged
why must be be careful not to remove the endotracheal tube too early?
because the patient will then exhale gas, and it can intoxicate the staff
what is MAC?
minimal alveolar concentration- it is the minimum amount of gas that reaches the alveoli at which 50% of animals do not move in response to a painful stimulus
how can we tell if a sedated animal is feeling pain?
the heart rate increases
which animals- small or large- need a higher concentration of anesthetic gas?
small- because they have a faster metabolism
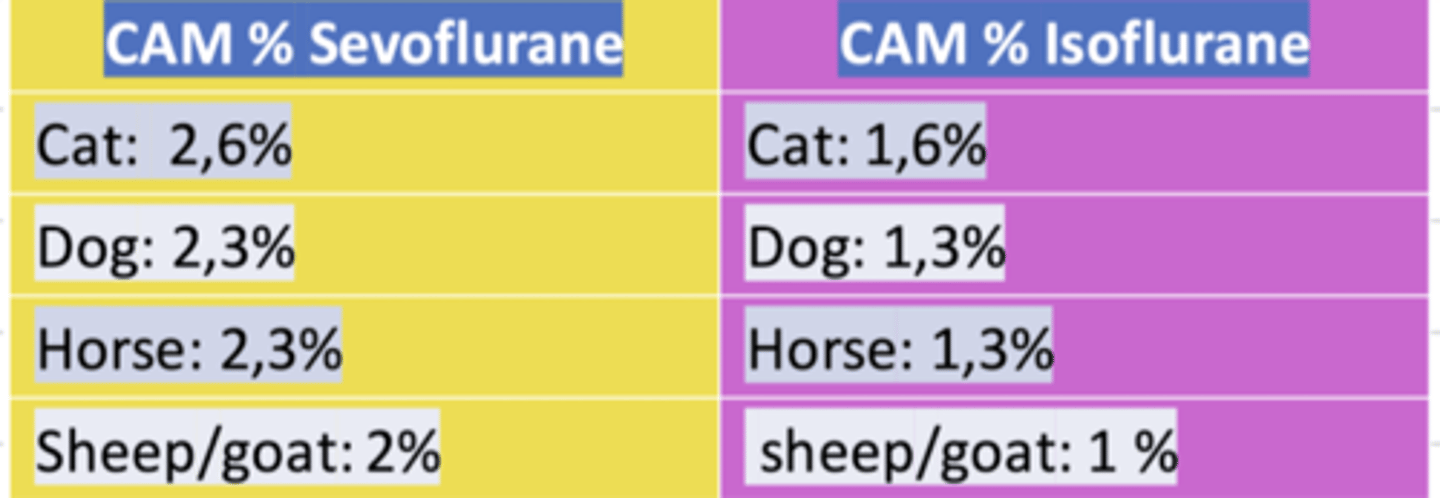
is it a good idea to put a higher MAC into the anesthetic machine just in case the animal needs a heavier sedation?
no- we NEVER put more than necessary. begin at the advised MAC and then can increase/decrease little by little if needed.
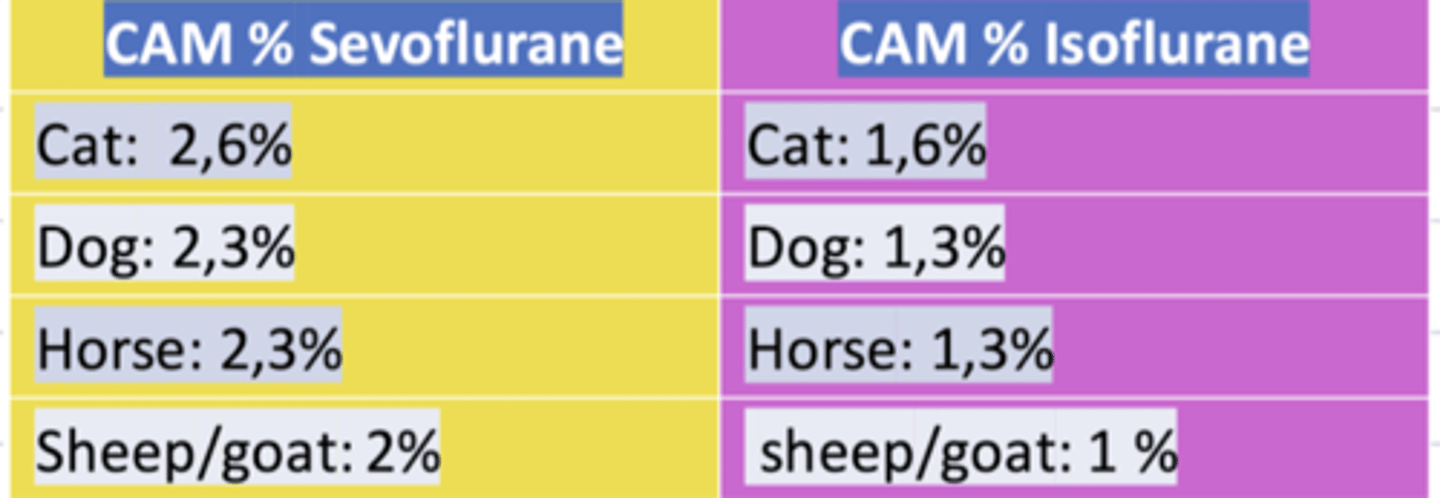
does a patient with tachycardia need a higher or lower MAC?
higher
a patient with hyperthermia requires a __________ (higher/lower) MAC
higher
we should _______ (increase/decrease) the MAC for a patient with hyperthyroidism
increase
an animal with hypertension requires a ________ (higher/lower) MAC
higher
what patient factors might lead us to need to increase the amount of anesthetic gas?
increased cardiac output (tachycardia)
hyperthermia
hyperthyroidism
hypertension
what patient factors might lead us to need to decrease the amount of anesthetic gas?
hypothermia
drugs
pregnancy
hypothyroidism
should we increase or decrease the amount of anesthetic gas given to the patient if they are pregnant?
decrease
if a patient is hypothermic, how do we adjust the level of anesthetic gas given (increase or decrease)?
decrease
a patient with hypothyroidism should be given ______ (more/less) anesthetic gas
less
what are the 3 main physiological effects of volatile agents?
CNS depression
CV depression
respiratory depression
how do volatile agents impact the cardiovascular system?
depression:
vasodilation
hypotension
decreased cardiac output
bradycardia
which volatile gas is the most potent?
isofluorane

______% of isofluorane is metabolised by the patient
0.2

which volatile agent has a very strong smell? is this an advantage or disadvantage?
isofluorane
this is advantageous because it can tell us when there is a leak or a bad intubation

which anesthetic gas is marked in purple?
isofluorane

______% of sevofluorane is metabolised by the patient
2
does sevofluorane have a stong odor?
no
what volatile gas is labeled in yellow?
sevofluorane
what color label does sevofluorane have?
yellow
what is the problem with mixing sevofluorane with the old absobants?
it produces component A, which is nephrotoxic
this is not a problem anymore because the new absorbants do not do this
which anesthetic gas is blue?
desfluorane

which volatile agent is gas at room temperature, so cannot be simply opened and has to be placed directly onto the vaporizer?
desfluorane

what color is desfluorane labeled with?
blue

which volatile agent requires an electric vaporizer?
desfluorane

which volatile agent has a very high MAC?
desfluorane (7-9%)

which volatile agent is a pollutant, and can intoxicate the air in the room if there is a leakage?
desfluorane

which volatile gas has the fastest speed of action?
desfluorane
(because it is the least soluble)

which is the cheapest volatile agent?
isofluorane
which volatile agent is the least potent?
desfluorane
which volatile agent is most metabolized?
sevofluorane
do patients have a fast or slow recovery from anesthetic gas?
fast, because it is quickly eliminated through exhalation (it only takes around 5 minutes)
how long does it take for a patient to recover from anesthetic gas?
around 5 minutes
can volatile agents accumulate in the body?
yes, in adipose tissue
so, overweight animals have a slower recovery
what are the advantages and disadvantages of using volatile gases (inhalants) for anesthetic maintenance?
advantages: easy to control the depth of anesthesia, fast recovery, airway control
disadvantages: CV and respiratory depression, expensive, pollution, anesthetists may breathe the gas
with inhalants, is it easy to control the depth of anesthesia?
yes
what is "recovery" from anesthesia?
the process of going from unconscious to conscious
why are complications common during the recovery stage of anesthesia?
because there are less monitors and we need to physically monitor the patient. there is also less staff caring for the patient.
what are the potential complications we might experience during the recovery phase of anesthesia?
dysphoria
vocalizations
pain
if the recovery is longer than normal, what problems can this cause in the patient?
hypoglycemia
hypothermia
hypotension
impairment of the metabolism of other drugs
electrolyte disturbances