UI: Human Phys Chap 20
1/51
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
52 Terms
Somatic Chromosome Counr
46 (Diploid), 23 Homologous Pairs
Gamete Chromosome Count
23 (Haploid), 1 member/pair
Autosome
22 pairs for general characteristics
Sex Chromosomes
Two types: X and Y
Sex Determination Role
Anatomical and Functional Distinctions
Palindromes
Regions of DNA bases that read the same from either direction.
X Chromosome Inactivation
One active only (either parent)
Barr Body
Inactive X chromosome; stored as dense heterochromatin, compensates for extra X
Primary vs Secondary Reproductive Organs
1°: Testes & Ovaries
2°: Ex-Genitalia, Accessory Glands, Reproductive Tract
Reproductive Tract
Transports gametes after produced
Accessory Sex Glands
Wolffian and Mullerian Ducts
Accessory Sex Glands Purpose
Develops reproductive organs based on whether MIF or Testosterone is present.
SRY Gene
Sex determining gene for excreting testosterone (Testis Determining Factor)
Yes MIF
Mullerian ducts degenerate
No MIF
Uterus & uterine tubes
Yes Testosterone (Accessory)
1) Epididymides, ductus deferentia, ejaculatory ducts
2) Prostate
3) Penis, scrotum
No Testosterone (Accessory)
1) Wolffian ducts degenerate
2) Vagina, Labia, Clitoris
Male Reproduction Difference
1) Mature sperm produced continuously (~30-100 million/day)
2) Testosterone release continuously
3) Reproductive potential continues throughout life
4) Begins at Puberty
Female Reproduction Difference
1) Ova released intermittently in small numbers
2) Cyclical hormone release
3) Reproduction potential ends during menopause
4) Begins at Puberty
(M) Primary Reproductive Organ
Testes: Produce sperm (in seminiferous tubules) and secrete testosterone
(M) Testes Compartments
1) Seminiferous Tubules: Spermatogenesis
2) Interstitial Tissue: Leydig cells (Produce Testosterone)
(M) Secondary Structures
Epididymis: Sperm Storage
Vas Deferens: Transport from scrotum to pelvic cavity
Ejaculator Duct: Joint of vas deferens and seminal vesicles
Seminal Vesicles: Forms semen volume / neutralizer (Prostate)
Urethra: Semen to exterior
(M) Spermatogenesis
Sperm from spermatogonia, continuous, 1 germ cell = 4 sperm
(M) Spermatogenesis Mechanism
Meiosis → (1 primary) → First meiotic division (2 secondary) → Second MD (4 spermatids) → spermiogenesis (4 sperm)
(M) Spermatogenesis Fun Fact
Body is allergic to sperm.
(M) Blood-Testis Barrier / Sertoli Cells
Protects WBC from killing sperm
Testosterone can freely move to mature sperm
Provides nourishment
Secrete androgen-binding protein (Testosterone no leave)
Release inhibin (FSH) to regulate
(M) Sperm parts
Head: DNA
Acrosome: Enzyme vesicle for penetration
Midpiece: Mitochondria (lots of energy)
Tail: Motility (moving against fluid)
(M) GnRH
Formed in hypothalamus to anterior pituitary gland:
LH → Leydig cells → Testosterone → Spermatogenesis
FHS → Sertoli cells → Inhibin or Spermatogenesis
(M) Endocrine Regulation
Testosterone inhibits LH
Inhibin inhibits FSH
(M) Erection/Ejaculation
Dilation of arterioles (PNS; NO), like a sponge
Release (SNS)
(F) Reproduction
Oogenesis (Ova)
Reception and transport of gametes for union (fertilization)
Fetus maintenance / Form placenta (temp. organ lifeline)
Birth (parturition) / milk (lactation)
(F) Primary Organs
Ovaries: Storage and endocrine function
(F) Secondary Organs
Oviducts (FT): close to ovaries, pick-up, fertilization site
Uterus: maintenance / expelling of fetus
Vagina: Uterus to external
Cervix: Lower vagina, passageway
(F) Hormone, Constant cycle
Estrogen: Ova maturation/release, sexual characteristics, breast development
Progesterone: Prep environment (endometrium)
(F) Oogenesis
~2 million primary oocytes at birth:
Oogonia stem cells
~400k at puberty
Primary matures, released from follicle each month
~400 total in lifetime; degenerate
(F) Oogenesis mechanism
Primary (46) → 2nd/Polar (23) → 1 mature, 3 polar (triggered by sperm entry)
(F) Ovarian Follicle
Start of Menstrual: 10-25 follicles mature
After ~1 week, one survives (Dom follicle = Graafian)
Releases estrogen, continues to grow, fluid pressure increases
(F) Corpus Luteum
Begins forming after follicle matures and releases egg:
Ovulation → Corpus Luteum → Corpus Albicans
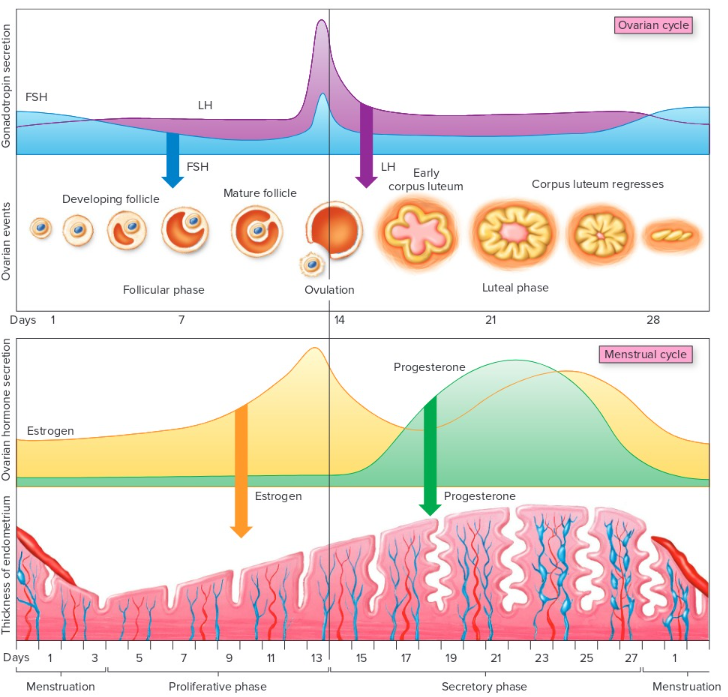
(F) Ovarian Cycle
Lasts 28 days, begins at puberty, normally interrupted only by pregnancy, terminated by menopause
(F) Follicular Phase
Days 1-13, First Half:
FSH stimulates - follicle growth, granulosa to secrete estrogen
LH stims theca to produce androgens for granulosa for estrogen (estradiol)
Low progesterone, gradual increase of estrogen
(F) Ovulation
Day 14:
Spike in estrogen, LH, & FSH (LH > FSH), ova released
(F) Luteal Phase
Day 15-28, Last Half:
Old follicular cells → Corpus luteum (functional within 4 days after ovulation)
Continues size increase for 4-5 days
Ovum not fertilized = CL degenerates, starting menstrual cycle
Gradual increase of progesterone (“glue”) and estrogen
(F) Uterine / Menstrual Cycle
Lasts ~28 days, same time as Ovarian Cycle
Hormonal changes during OC
Menstrual Bleeding
(F) Menstrual Cycle
Days 1-4, start of new cycle:
Discharge of blood
Release Uterine prostaglandin
Vasoconstriction of endometrial vessels (endometrium death)
Stims rhythmic uterus contractions
Blood Clot: Golf (Good), Baseball (Bad)
(F) Proliferative Phase
Days 4-14, same time as last part of Follicular:
Endometrium proliferates, makes new follicles
Lasts from end of menstruation to ovulation
(F) Secretory Phase
Days 14-28, same time as Corpus Luteum:
CL secretes many progesterone and estrogen
PRG stims endometrial glands → glycogen
No fertilization/implantation → CL degens → new FP and MP
(F) Fertilization
Fallopian tubes site
Must occur within 24 hours of ovulation
Reproductive tract aids in migration:
Myometrium contractions
Mature eggs release Allurin
(F) Fertilization Race
First sperm to reach ovum:
Fuse with plasma membrane of ovum
Chemically penetrates, and blocks other sperm
Head separates → fuse with egg → zygote
(F) Contraception
Oral, Rhythm (time the days), IUD, Barriers