Effectors
1/22
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
23 Terms
Ways to get rid of pathogens
neutralization of pathogen /toxin
the act of binding can inactivate or neutralize things
agglutination (clumping of ag)
clumps are easier for other parts of the immune system to get rid of it
opsonization
anything with ab on it will stick tight to neutrophils/macrophages when ab binds the Fc receptor makes a conformational change
complement activation
has its own collection of activities lysis, inflammation
ab dependent cell mediated cytotoxicity
Tc cells and NK cells will kill virally infected cells, coat the target cell with ab NK cell will kill it
degranulation
one specific ab good at degrading ab and MAST cells, IgE binds to trigger the degranulation of MAST cells
Plasma cell action when it encounters a MAST cell with worm
B cell will make IgA the only cell that can make ab
make ab/dimeric IgA will make a J chain which binds them together
binds Fc receptor on mucosal epithelial cells
PolyIg receptors will bind, go into a vesicle move from basal lateral to the other side and cleave the receptor wrap Fc receptor with portions of IgA and pop out a 2 headed monomer to protect it from proteases
need to protect IgA from protease bc it is in the mucus not the serum anymore
Effector function IgG
many subclasses
some human ones are good at complement activation others are not
all are good at binding the Fc receptors so it is good at acting as an opsonin
good at neutralizing IgG increase binding affinity
Effector Function IgM
good at agglutination to get swallowed and complement
first ab produced in an immune response
macrophages will be good at swallowing them
Effector function IgA
in secretions, its job is to catch pathogens while they are still in the mucosa before they contact the cell (keep them from getting too close)
anti-inflammatory doesn’t contact the mucosa or activate complement
boundaries help maintain bacteria but don’t let them sit on the cell
Effector function IgE
allergy and asthma
good at dealing with parasites (anything large)
prevalence is based on where you live in the world
good a degranulation
basophils or MAST cells
histamine holds the granules together so when broken causes inflammation
Antibiotics
we got good at making ab
can produce ab that binds a specific thing
can look at targets to make them get rid of certain health conditions
pull things out of circulation or block certain receptors
some ab can produce against bacterial toxins and keep it around as a drug
Fc Domains
Ig superfamily
signal transduction
ITAMS = stimulatory
ITIMS = inhibitory bind unbound ab and tell the B cell that they are overshooting
gamma
Signal transduction pathway
all use the same pathway to get information through the cell
but you can switch what triggers the pathway.
we see this structure over and over
certain drugs can cause bad affects because the pathway has meany different triggers which can cause weird side effects
Timing of ab
ab is not good at dealing with things already in the cell
odd timing
see the target stick to it
cytoskeleton rearranges shifts to the problem site
two cells stay together then separate
not an instant death not punching holes in the membrane it will die internally
How CTL kills cells
perforin polymerize into a barrel we can see holes it punches in the membrane
cell does not explode like they normally would when they activate complement
instead goes through apoptosis swallowed no inflammation
These holes allow granzyme (protease) into the target cell
CTLs recognize and kill infected or tumor cells via TCR
Perforin/granzyme pathway
we have a target cell and Tc
granules in Tc have both perforin and granzyme in them
perforin forms a pore the purpose is to allow granzyme access to the target cell
granzyme will activate caspase (the normal apoptosis pathway that all cells carry)
trigger the activation of a normal pathway (all cells want to go through apoptosis at some point)
when granzyme is release things to chop DNA into fragments, cytoskeleton pulls the membrane into vesicles makes it easier for macrophages to phagocytize and recycle
cytoplasms doesn’t spill into circulatory (explode)
if it does the trigger damaged associated molecular molecules = inflammation
Fas pathway joins the same pathway to trigger apoptosis
granzyme is triggering here
FADD fast associated death domain molecules on the surface of cells ask if they need to undergo apoptosis
Evolution and viruses
turn down MHC I so they cant be detected
Tc wont see them to kill them
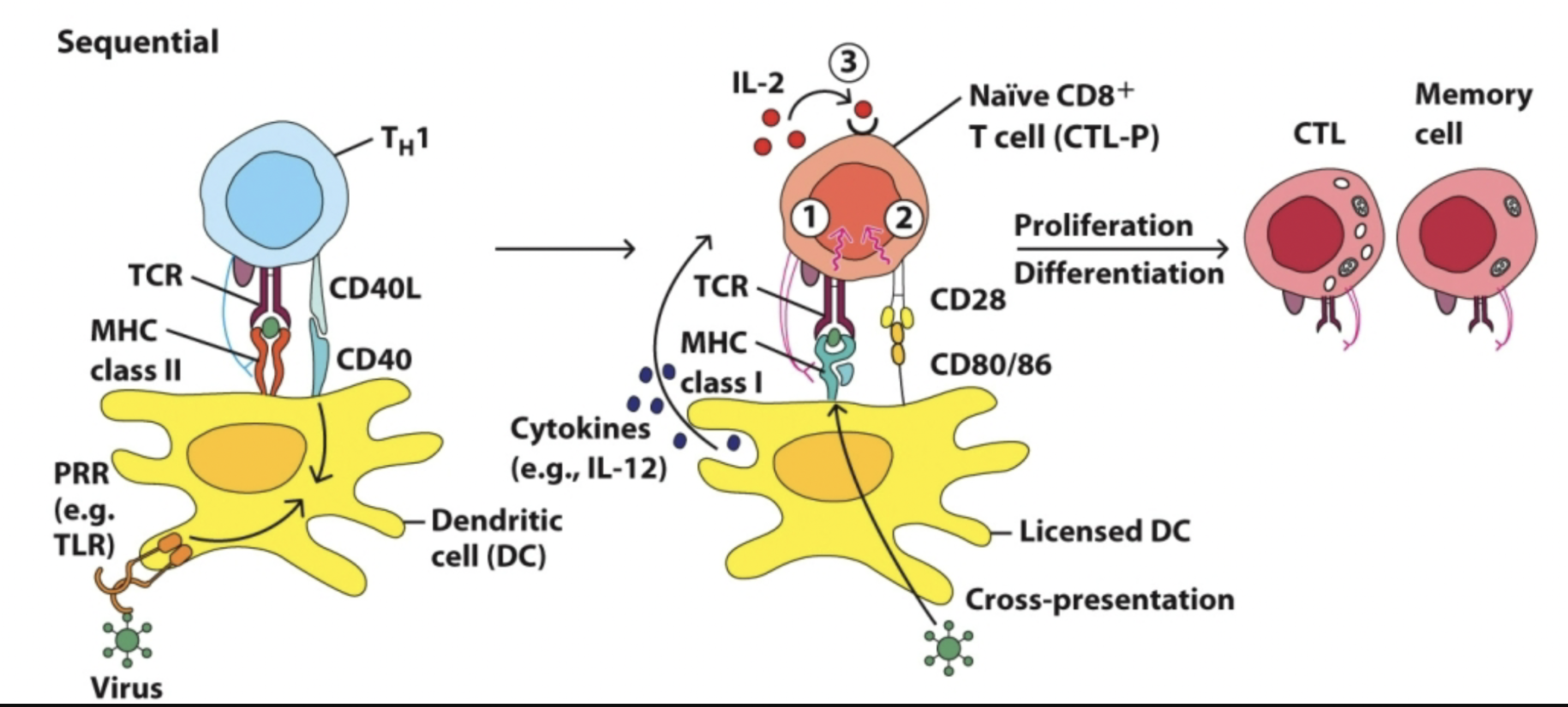
Sequential
Th
virus has a protein encoded extracellular form
phagocytic cells recognizes the verions in circulation and bind to them using trigger pattern recognition molecules
which are turned up in the phagolysosome present in MHC II to Th cells and get Th cells specific for viral peptides to start produce IFN-gamma
Tc
see ag in MHC I and response to that is to kill the cell that presented it unless it is a licensed dendritic cell
Dendritic cells will swallow virus and produce some of the peptides in MHC I and present co stimulatory molecules to convince Tc to not kill it but to continue to replicate it
make memory and effector cells
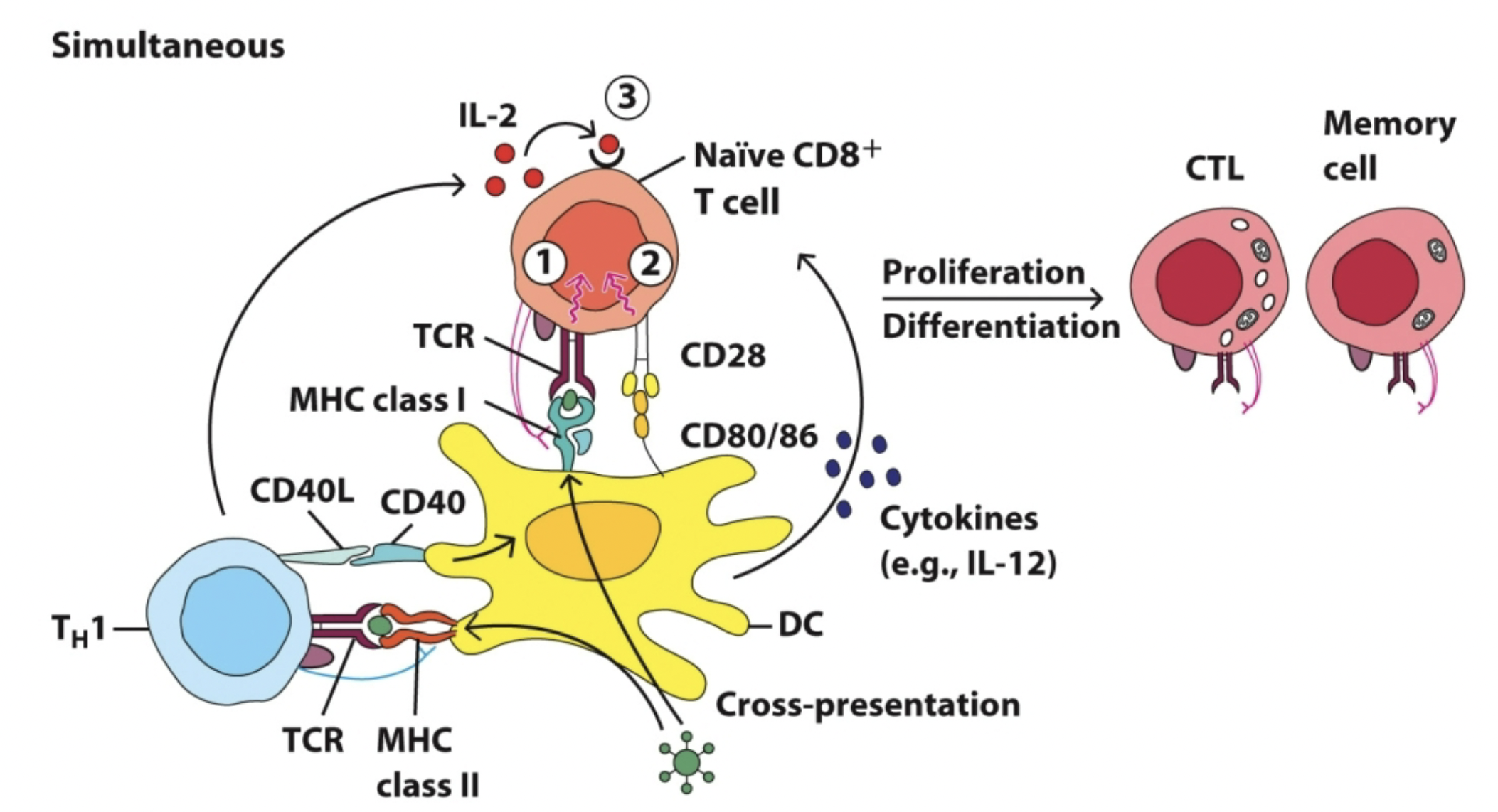
Simultaneous
in nodes clusters of cells
dendritic cells pull ag and drop it into the node
Tc and Th cells then decide what to do next
Graph
titer is a biological concentration (activity per volume)
virus titer is how many viral plagues are we going to have
virally specific Tc we don’t see till later
surge of NK cells
early IFN - alpha and beta which is good for antiviral activity they turn down protein transduction and cause the sick feeling
NK vs Tc cells
Tc looks for ag and NK cells always looks for activated ligands but they are inhibited by inhibitory receptors that bind MHC I
look for absence of something
tension between killing or not
reason bc MHC I is the way that Tc sees viral ag and if the virus turns off MHC I it would be invisible (fail safe)
Tolerance
Has MHC I inhibitory signal to turn off NK cells and prevent it from killing the cell
Missing self
No MHC I no inhibitory signal so MK cells activation is on and will kill the cell
Balanced signals
up regulation of stimulatory cells due to DNA damage
stress molecules increase to get NK cells to delete them
KIR killer inhibitory receptors get damaged cells to delete
NK cells and MHC I
Nk cells ask for MHC I and if it has it then there is a inhibitory signal and lets the cell through
No MHC I will stimulate NK cells and kill it
virally infected cells produce more stimulatory molecules to NK cells even if no MHC I if there are enough signals it will delete the cell
NKT cells
Tc cells kill by apoptosis and triggered by fas or perforin/granzyme
Th looks for ag on MHCII, Tc look for ag on MHC I
NK cells no MHC I will kill the cell
Immune system needs something the middle so NKT cell sees MHC but not I or II looks for ag on CD1
nonstandard MHC present ag in glyccolipid no VDJ recombination
main idea is that yes there is killing or not but there is also a mechanism in the seems
Innate lymphoid cells
myeloid cells run this and lymphoid cells run specific immune system
NK cells are not ag specific but they are lymphoid specific
ILC 1 response (Th1)
IFN-gamma
viral
ILC 2 response (Th2)
IL4,5,13
fungal
ILC 3 don’t rearrange their ag receptor but they produce cytokines
IL17A,22
cells in the mucosa
Th1 cells are long and difficult to make slow
ILC can make many for less time and energy produce similar cytokines to support action of Th cells they create less issues with autoimmunity because they are under the control of a t cell