AOS Unit 1Chapter 6
1/99
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
100 Terms
What is homeostasis?
Homeostasis is the maintenance of a stable internal environment despite changes in the external environment.
It ensures cells function optimally within specific limits.
Cells like specific environments or limits
Why can we stand outside in the heat for a little while before you start to feel really uncomfortable
cells don’t instantly die when the external environment of your body changes because we maintain homeostasis
stimulus-response model
a model that describes how a system responds to react to a prompt
a stimulus positive feedback system
a stimulus–response process in which the response increases the stimulus
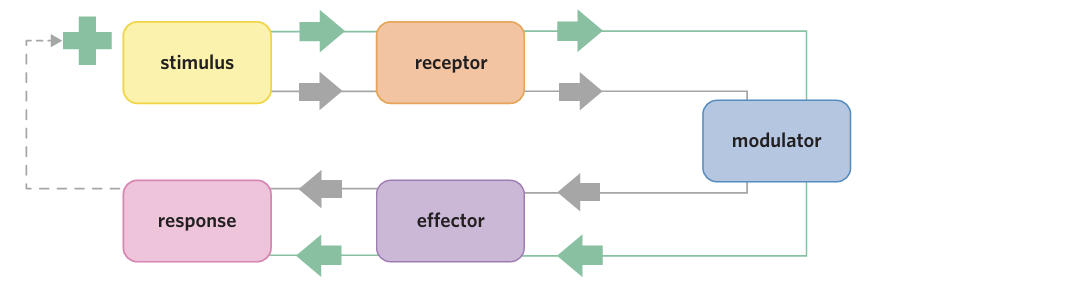
negative feedback system
a stimulus–response process in which the response counters the stimulus
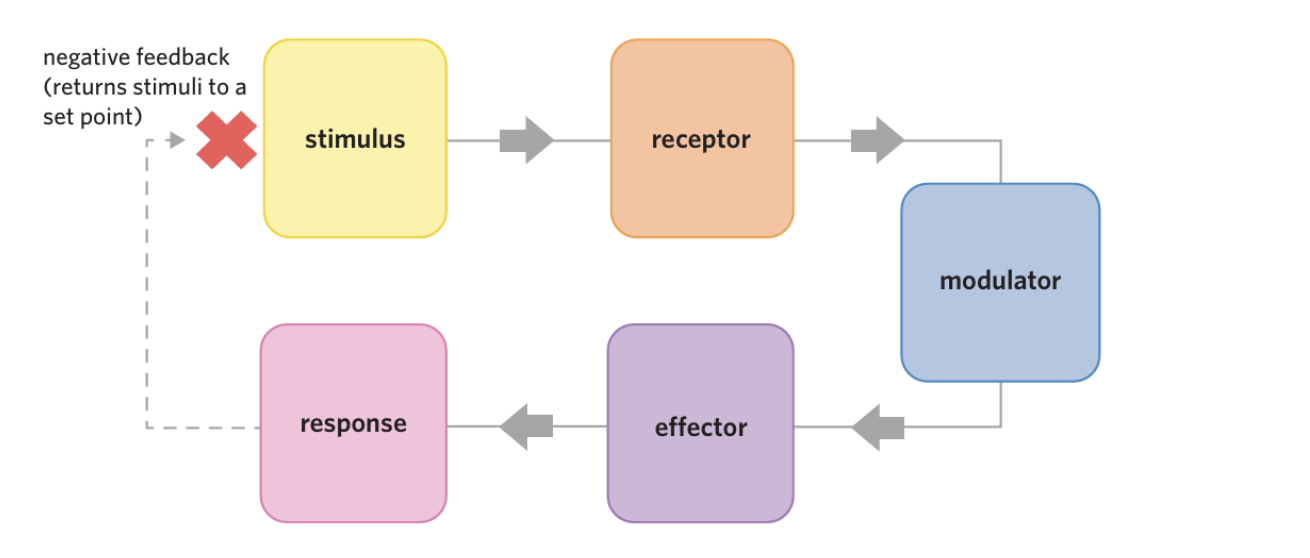
stimulus (pl. stimuli)
an event or molecule that can initiate a response
receptor
a structure that detects a signal or external change, usually a protein
modulator/processing centre
location where information from receptors is sent to and compared to a set point, and where molecules altering the functioning of an effector are released.
effector
a molecule, cell, or organ that responds to a signal and produces a response
hormone
a signalling molecule released from endocrine glands that regulates the growth or activity of target cells
response
the action of a cell, organ, or organism caused by a stimulus
What is controlled by homeostatic mechanisms
External environment changes (heat, cold, dehydration, etc.)
Internal environment must stay constant
Stimulus–Response Model
Stimulus
Change in internal/external environment
e.g. increase in temperature
Receptor
Receptor Detects the change (stimulis)
Converts it into a chemical or electrical signal for modulator
Modulator (processing centre)
Usually brain or endocrine gland
Compares to set point (ideal value)
Sends signals to effectors
Effector
hormone/Organ/cell that carries out response
e.g. sweat glands, muscles
Response
Action that occurs in response to stimulus
e.g. sweating to cool body
any change in the function of a target cell, organ, or organism

Different types of receptors
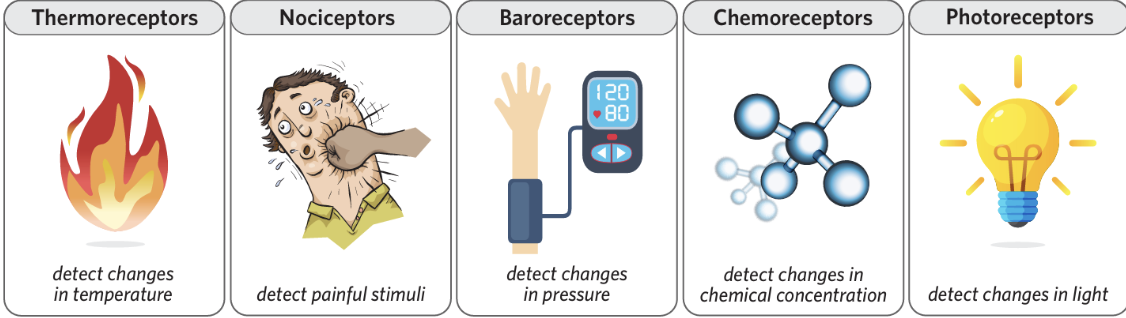
Example of stimulus response model (NOT HOMEOSTASIS)-reflex arc
Seeing a hot object and pulling your hand away
1. Stimulus
Touching a hot surface
2. Receptor
Pain/temperature receptors in the skin detect heat
3. Modulator
Spinal cord / brain processes the signal
4. Effector
Arm muscles
5. Response
Hand is pulled away quickly
Example of a Positive stimulus response model-Blood Clotting
Stimulus
A blood vessel is damaged (cut or injury)
Receptor
Platelets detect exposed damaged tissue
Modulator
Platelets release chemical signals (clotting factors)
Effector
More platelets are activated and attracted to the site
Response
Platelets stick together until sealed and form a blood clot
The response (platelet activation) amplifies itself, leading to rapid clot formation
Why is blood clotting a postive feedback response
Activated platelets release chemicals →
This attracts more platelets →
Which release even more chemicals
The response keeps increasing until the clot is fully formed
Negative feedback loop does what?
Response counteracts the stimulus
Returns system to set point
Maintains homeostasis
the response attempts to revert the system back to the state it was in before the stimulus occurred.
Example of negative feedback loop Body Temperature (Too Hot)
1. Stimulus
Body temperature rises above 37°C
2. Receptor
Thermoreceptors in the skin and brain detect the increase
3. Modulator
Hypothalamus compares it to the set point (37°C)
4. Effector
Sweat glands increase sweat production
Blood vessels dilate (vasodilation)
5. Response
Sweating → heat lost by evaporation
Vasodilation → more heat lost from skin
Cell Signalling
3 Steps:
Reception → detect signalmechanical, electrical, or chemical signal
Transduction → signal passed along
sending a signal between organisms, across the body, to a neighbouring cell, or back to the original receptor cell
Response → action occurs
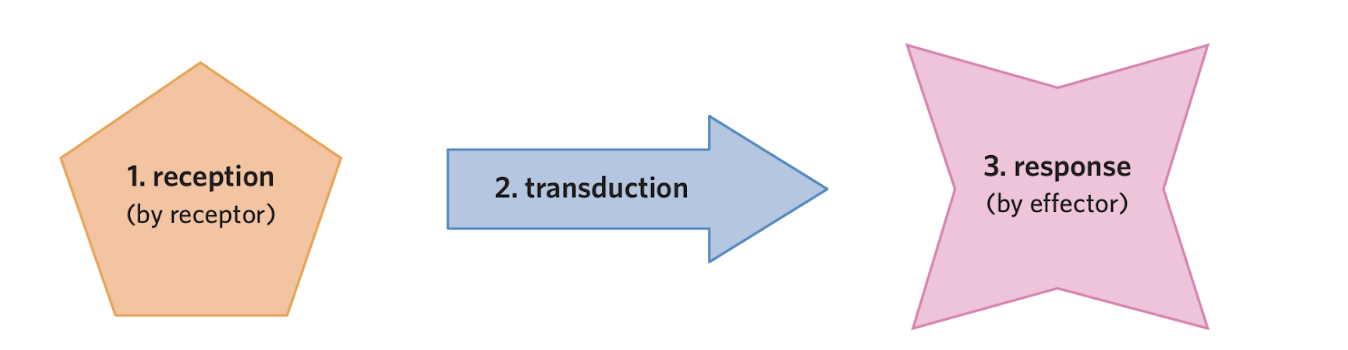
What are the four methods of heat transfer?
Conduction-
Convection -
Evaporation
Radiation -
Conduction-
The transfer of heat through physical contact with another object
When you touch something hot, heat from that object is transferred to your fingers via conduction
Convection -
The transfer of heat via the movement of a liquid or a gas between areas of a different temperature
The temperature is warmer in the second storey of your house because hot air rises, taking heat energy with it
Evaporation
-The loss of heat via the conversion of water from liquid to gas form
When you sweat, the water on your skin evaporates. Turning a liquid into a gas requires a lot of energy, and when sweat evaporates it takes away heat energy from your skin making you cool down
Radiation -
The transfer of heat via electromagnetic waves such as light (i.e. doesn’t require physical contact with another object)
The sun warms you via radiation. Conversely, when you stand in a cold room and you aren’t wearing much clothing, you lose heat to your environment via radiation
Thermoregulation occurs via
a negative feedback stimulus-response system.
Thermoregulation
the homeostatic process of maintaining a constant internal body temperature
Formula for total heat change
Total heat change= heat in + metabolic heat – heat out
metabolism
The set of chemical reactions within cells that help maintain the body’s normal functioning including converting food and drink to energy
endotherm
an animal that produces the majority of its own heat via metabolic processes
ectotherm an animal that obtains heat primarily from the environment, rather than its own metabolic heat
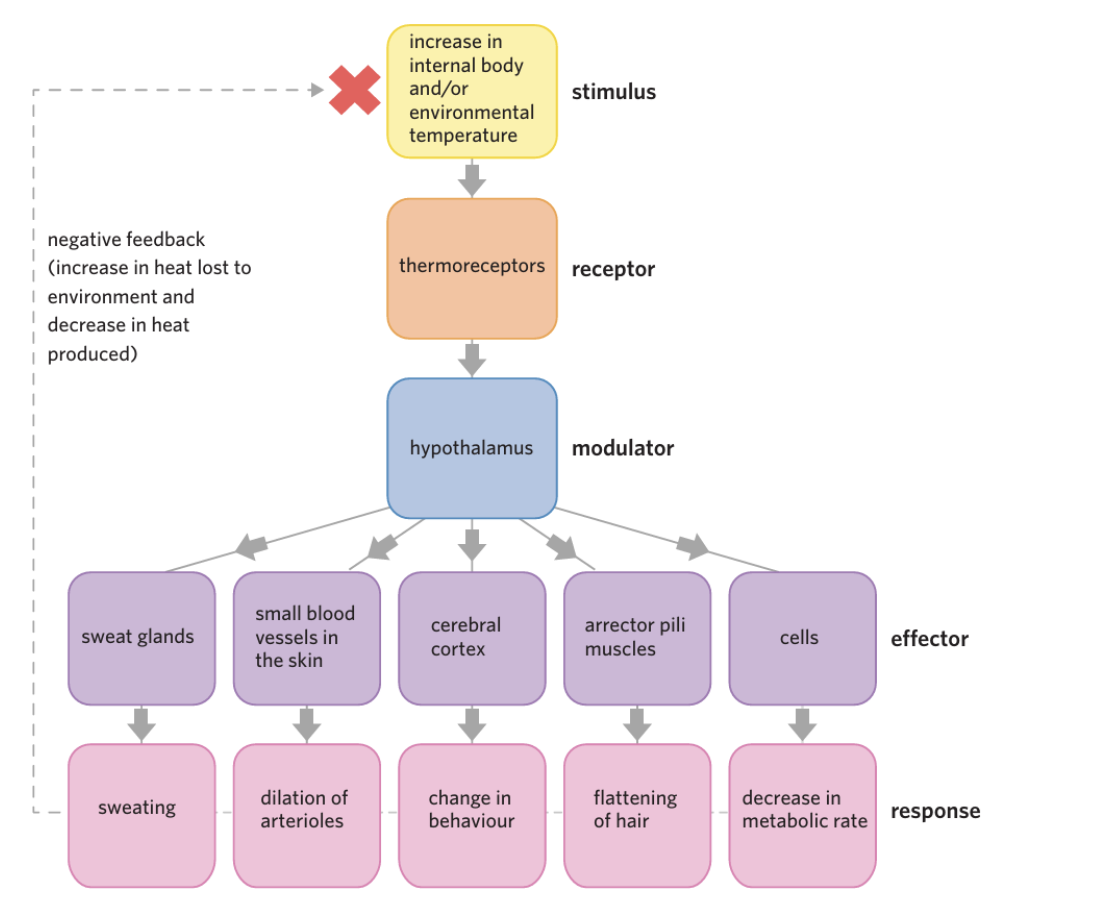
When Body is TOO HOT
Goal: lose heat + reduce heat production
increasing the amount of heat lost to the environment and decreasing the amount of heat produced by the body
• Sweat glands produce sweat which evaporates from the skin, taking heat energy with it
• Small blood vessels in the skin vasodilate, increasing surface blood flow. Blood is warm, so by increasing the amount of blood at the surface of the body the heat lost to the environment via convection and conduction is increased
• The cerebral cortex causes changes in behaviour, such as seeking shade
• Arrector pili muscles in the skin relax, which flattens body hair against the skin. Doing this increases the free flow of air against the skin, which increases the amount of heat lost due to convection
• At a cellular level, signals are sent by the hypothalamus to slow metabolic processes which reduces the amount of heat made by the body.
vasodilation
The widening of blood vessels
cerebral cortex
The outer layer of the brain that plays a key role in a number of processes including memory, attention, and perception
arrector pili muscles
arrector pili muscles small muscles attached to hair follicles
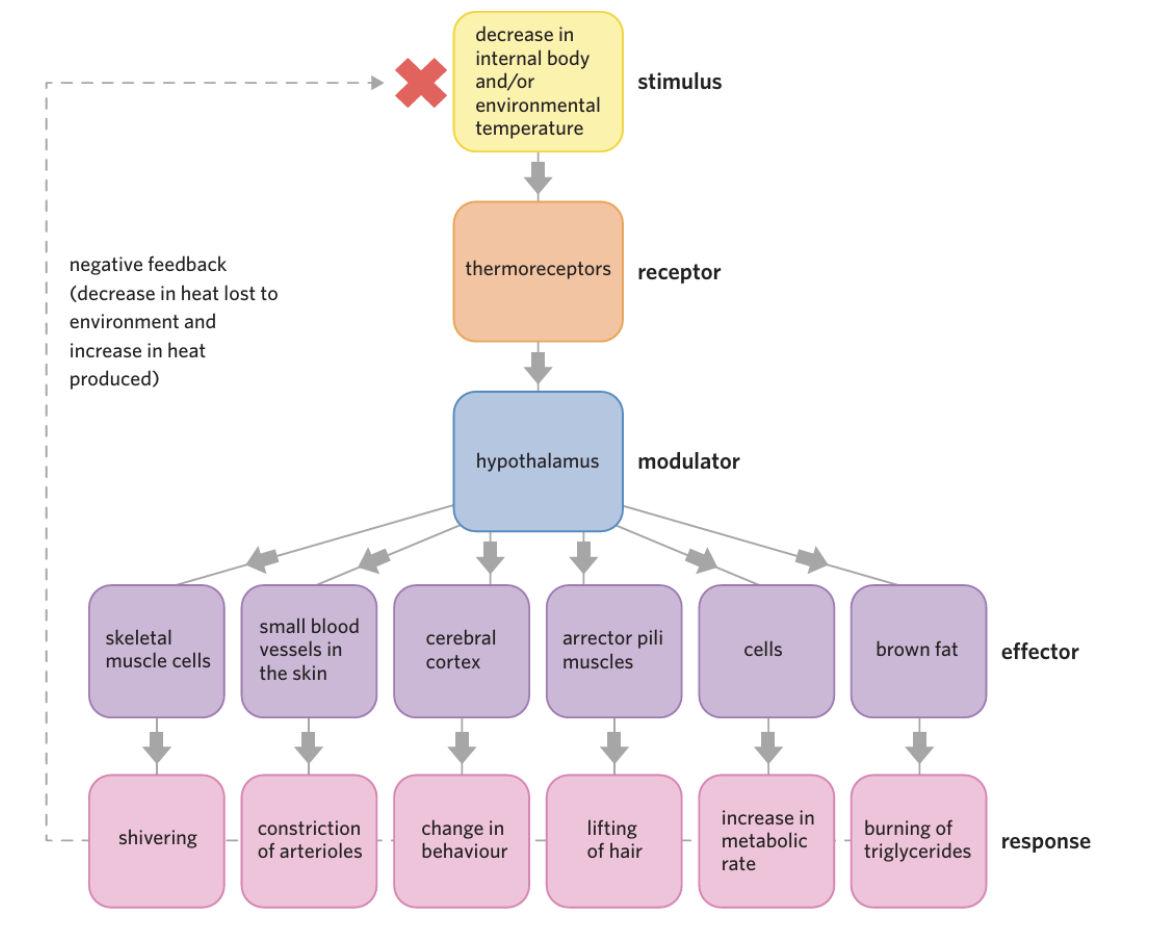
When Body is TOO COLD
Goal:decreasing the amount of heat lost to the environment, and increasing the amount of heat produced by the body
Skeletal muscles are stimulated to cause shivering, a process in which muscle cells are stimulated to move quickly which increases their metabolism and creates more heat energy
• Small blood vessels in the skin constrict through a process known as vasoconstriction, decreasing surface blood flow. This means that less body heat is lost to the environment vasodilation the widening of blood vessels s
• The cerebral cortex causes changes in behaviour, such as putting on more clothing
Arrector pili muscles in the skin contract, lifting hair follicles up, causing goosebumps, and trapping a layer of air. This layer of air serves as an insulating layer against the surrounding cold environment •
At a cellular level, signals are sent to increase metabolic processes such as cellular respiration which in turn results in more heat energy being produced • Brown fat cells are stimulated to produce heat via the burning of triglycerides.
skeletal muscle
a type of muscle that is voluntarily controlled and that is usually attached to bones vasoconstriction the narrowing of blood vessels
What is glucose?
the main source of energy for all the cells in our body.
Where do we get glucose from?
We get it from the food we eat in the form of carbohydrates
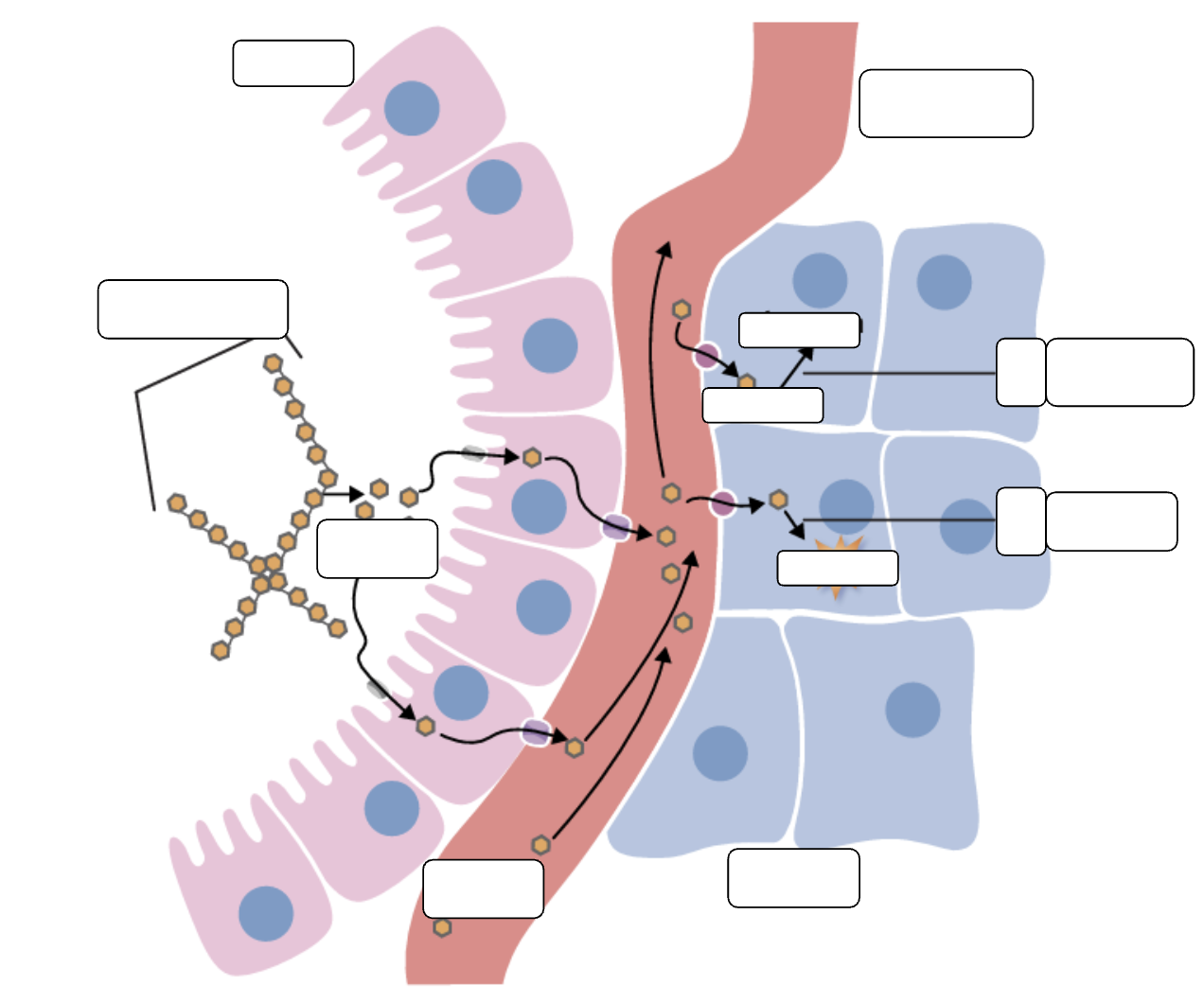
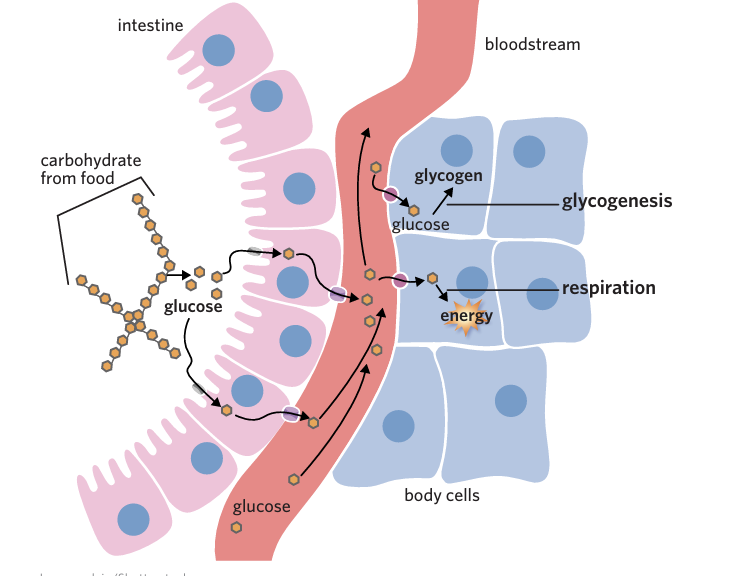
What happens when we eat carbohydrates?
-the digestive system breaks them down using enzymes into glucose.
-Glucose is then absorbed by the small intestine and released into the bloodstream via glucose transporters.
-glucose can travel around the body in the blood plasma where it gets taken up into cells.
What happens to glucose in cells
the process of respiration breaks glucose up into smaller parcels of energy called ATP that are used to power cell function
carbohydrates
a primary macronutrient and the body's main energy source, broken down into glucose to fuel cells, tissues, and the brain
glycogen
a highly branched chain of glucose molecules stored in the liver and muscles, acting as the primary, quick-access energy reserve in animals.
glucose transporter
a group of membrane proteins that transport glucose across the plasma membrane
glycogenesis
the process of creating glycogen from glucose
glycogenolysis
the process of breaking down glycogen into glucose
Glucose from body stores
Glycogenesis is the process where glucose is joined together to form glycogen in the liver and skeletal muscle cells.
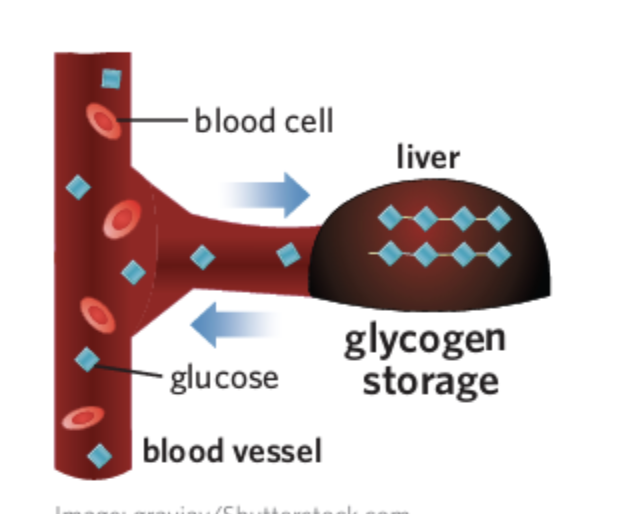
Blood glucose level
The amount of glucose in the blood at any time
Normal range: ~4.0 – 7.8 mmol/L
(≈ 1 teaspoon of glucose in the body)
hyperglycaemia
the state of having blood glucose levels above the normal range (>7.8 mmol/L)
hypoglycaemia
The state of having blood glucose levels below the normal range (<4.0 mmol/L)
How does homeostasis maintain constant blood glucose levels? negative feedback loop
by releasing insulin to lower blood glucose levels and glucagon to increase blood glucose levels.
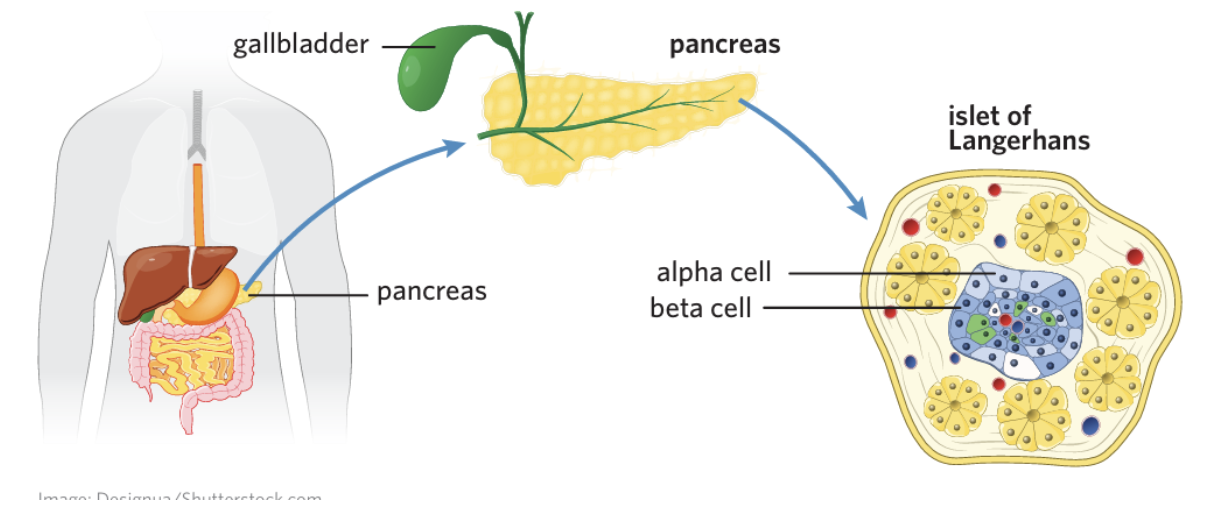
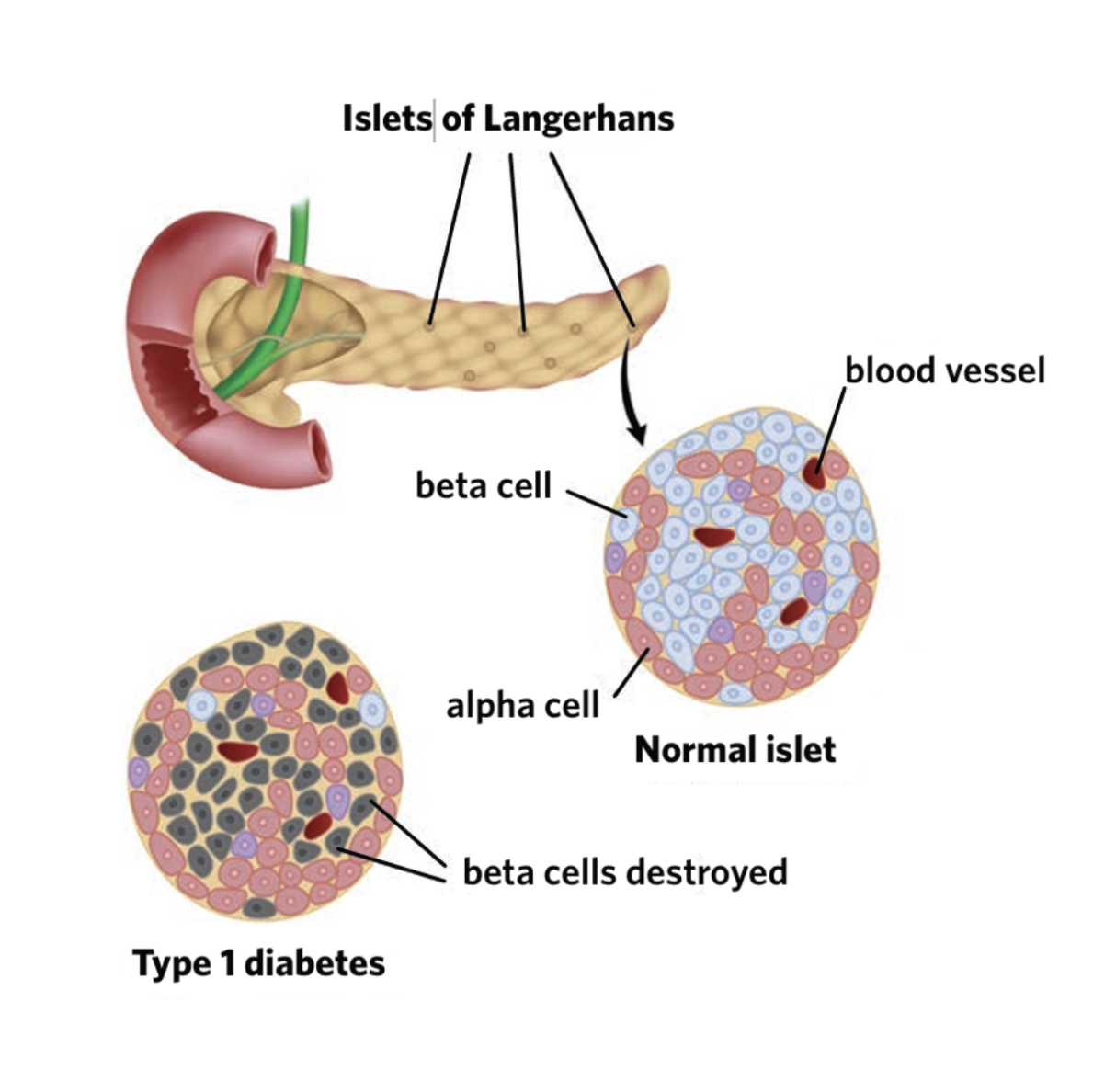
Islets of Langerhans
regions of the pancreas that contain cells that secrete hormones
alpha cells
cells that occupy the islets of Langerhans and secrete glucagon
beta cells
cells that occupy the islets of Langerhans and secrete insulin
insulin
a hormone secreted by beta cells of the pancreas when blood glucose levels are elevated
glucagon
a hormone secreted by alpha cells of the pancreas when blood glucose levels are low
when blookd glucose levels are high
Stimulus:
Blood glucose rises above ~5 mmol/L (e.g. after eating)Receptor:
Beta (β) cells in the islets of Langerhans (pancreas) detect the increaseModulator:
Pancreas (islets of Langerhans)
→ decides to release insulinEffector(s):
Skeletal muscle & fat cells
Liver cells
Response:
Blood glucose levels decrease back to normal (~5 mmol/L)
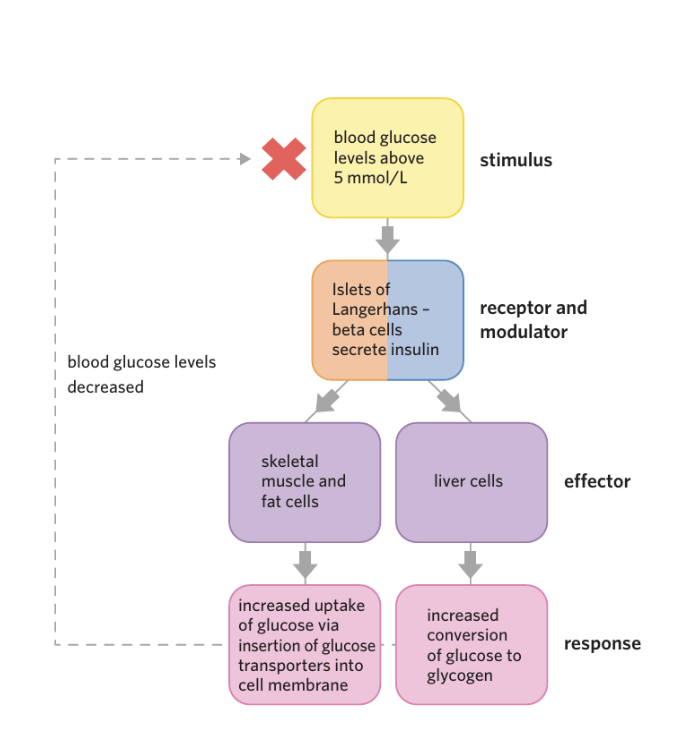
Effect number 1 of Insulin (When Blood Glucose is High)
Effector 1: Skeletal Muscle & Fat Cells
Insulin binds to receptors on these cells
Causes insertion of glucose transporters into the cell membrane
→ increases glucose uptake via facilitated diffusion
Why needed:
Glucose is hydrophilic → cannot pass through lipid membrane easily
Once inside the cell:
Used in cellular respiration → ATP (energy)
Stored as:
Glycogen in skeletal muscle
Fatty acids in fat cells (long-term storage)
Insulin activates enzymes for glycogenesis
→ converts glucose into glycogen for storage
Note:
Liver already absorbs glucose
Insulin mainly increases conversion to glycogen, not uptake
Effect number 2 of Glucagon (When Blood Glucose is low)
Liver Cells
Glucagon Stimulates liver cells to to break down glycogen into glucose and release it into the bloodstream via glycogenolysis.
Glycogen → glucose
Glucose is then released into the bloodstream
🔁 Negative Feedback Link
When blood glucose returns to ~5 mmol/L:
Alpha cells stop releasing glucagon
Liver stops breaking down glycogen
→ System switches off
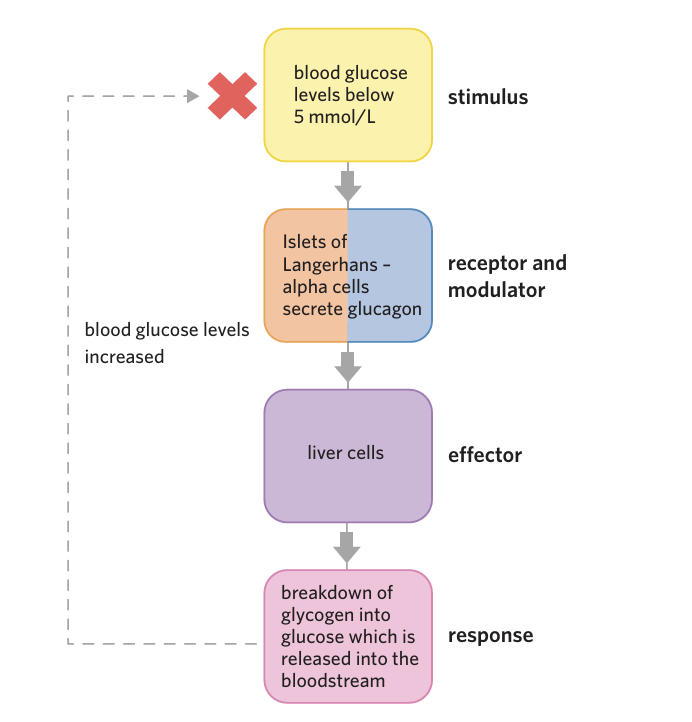
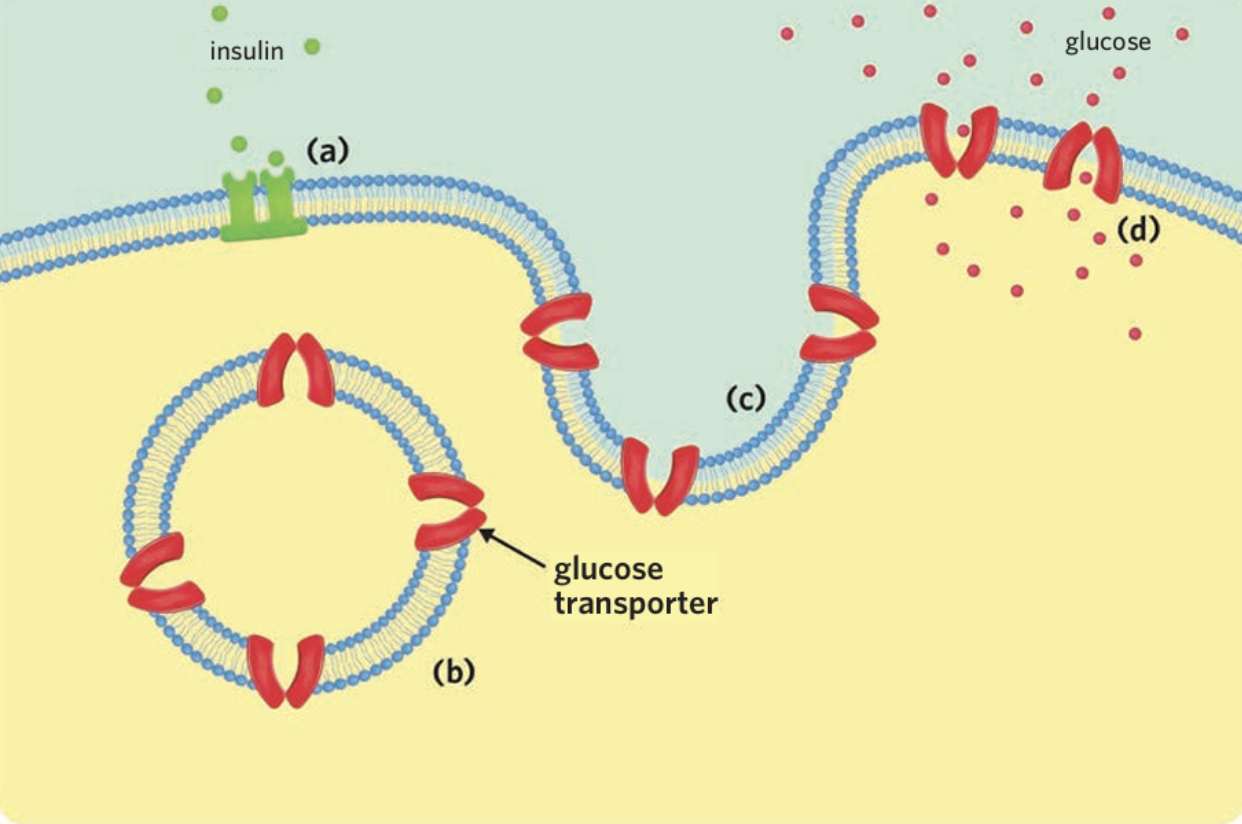
a) Insulin binds with receptors on skeletal muscle cells, causing (b) vesicles embedded with glucose transporters to (c) fuse with the cell membrane, (d) allowing more glucose into the cell.
osmolality
the total concentration of solute in a given weight of water
keeps stable water balance in the body Keeps osmolality
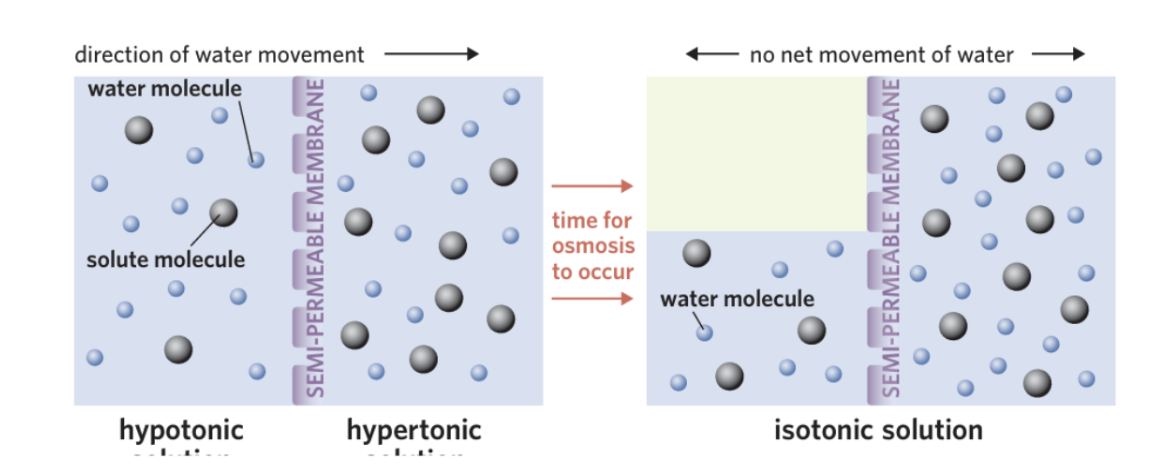
Water moves by osmosis:
From low solute → high solute
What Happens if Balance is Wrong?
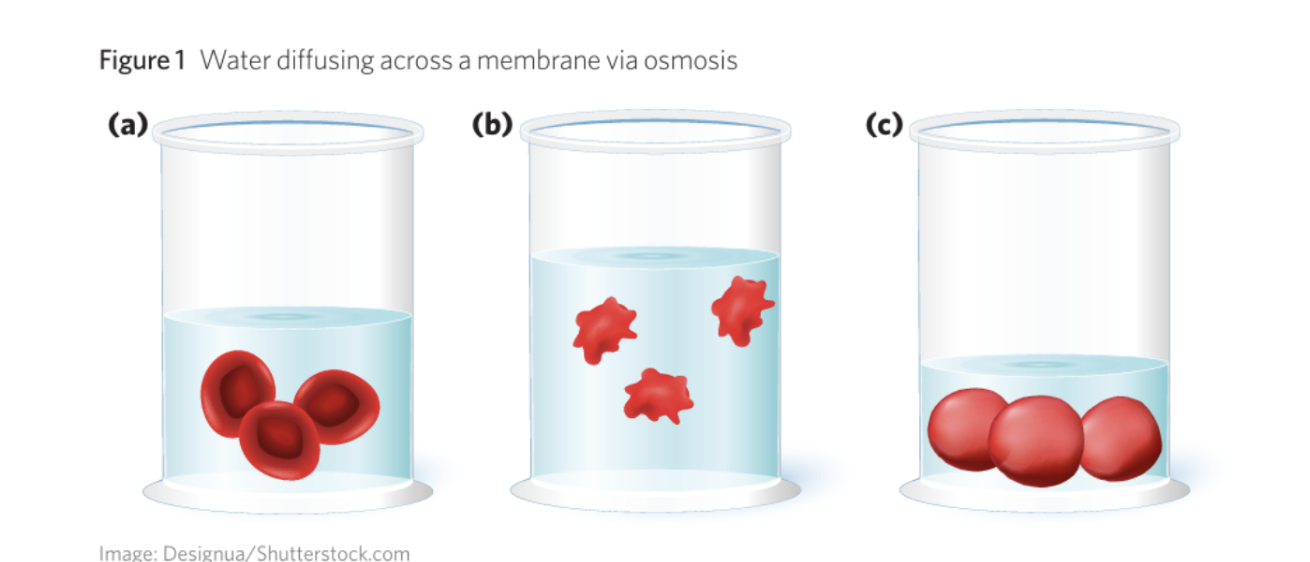
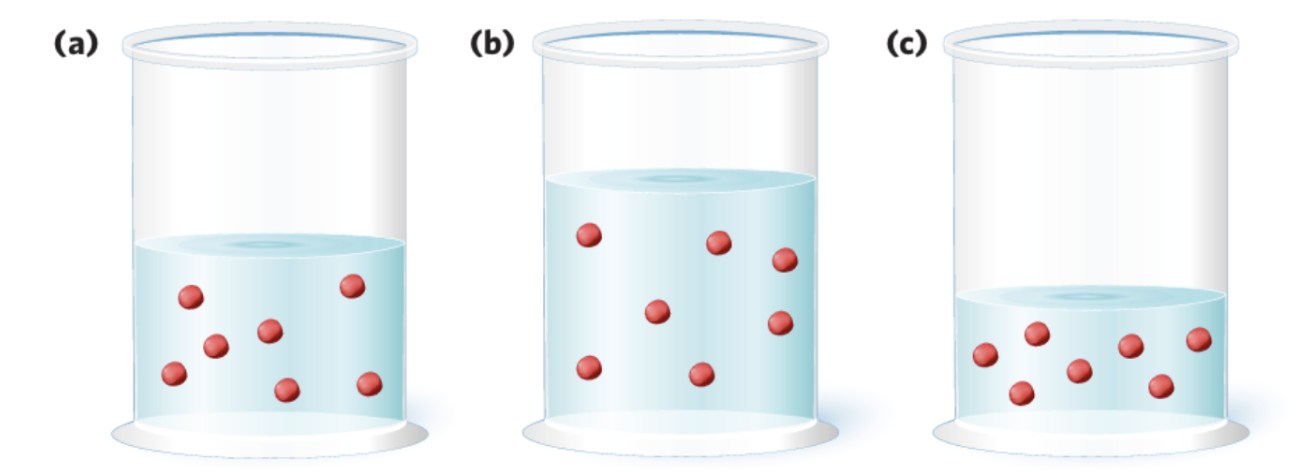
Hypertonic environment (extracellular fluid -high solute concentration)
Water moves out of cells via osmosis
Cells shrink (crenate)
→ cannot function properly
Hypotonic environment (the extracellular fluid-low solute concentration,)
Water moves into cells
Cells swell / may burst
Isotonic (ideal)
Equal solute concentration
→ no net water movement
How the Body the imbalance of water
Easier to change water amount than solutes
So body:
Adds water → lowers concentration
Removes water → increases concentration
Goal:
Keep extracellular fluid isotonic to cells
Water balance controls cell size + function
Controlled by adjusting water in body fluids
Prevents:
Cell shrinking
Cell bursting
Water balance = keep cells stable (not too swollen, not too shrunk)”
Other functions of water
1. Production of Urine
helps:
-Dissolve urea and other wastes
-Remove waste via the excretory system
2. Removal of Heat (Thermoregulation)
Loss of sweat, heat energy lost
3. Maintaining Blood Volume
Blood plasma is about 92% water
Maintains:
Blood pressure
Efficient transport of substances (e.g. glucose, hormones)
4. Protection of the Brain & CNS
Water forms cerebrospinal fluid (CSF)
CSF:
Surrounds brain and spinal cord
Acts as a shock absorber
Formula for total water change
Total water change = water in + metabolic water – water out
What is the stimulus response model when water levels decrease?
Stimulus:
Decrease in body water
→ causes:Increased blood osmolality
decreased blood volume & pressure
Receptors:
Osmoreceptors (hypothalamus) detects the increased osmolality
Baroreceptors (heart, arteries, kidneys) detects the decreased pressure/volume
Modulators:
Hypothalamus + posterior pituitary gland → ADH pathway
Kidneys → renin pathway
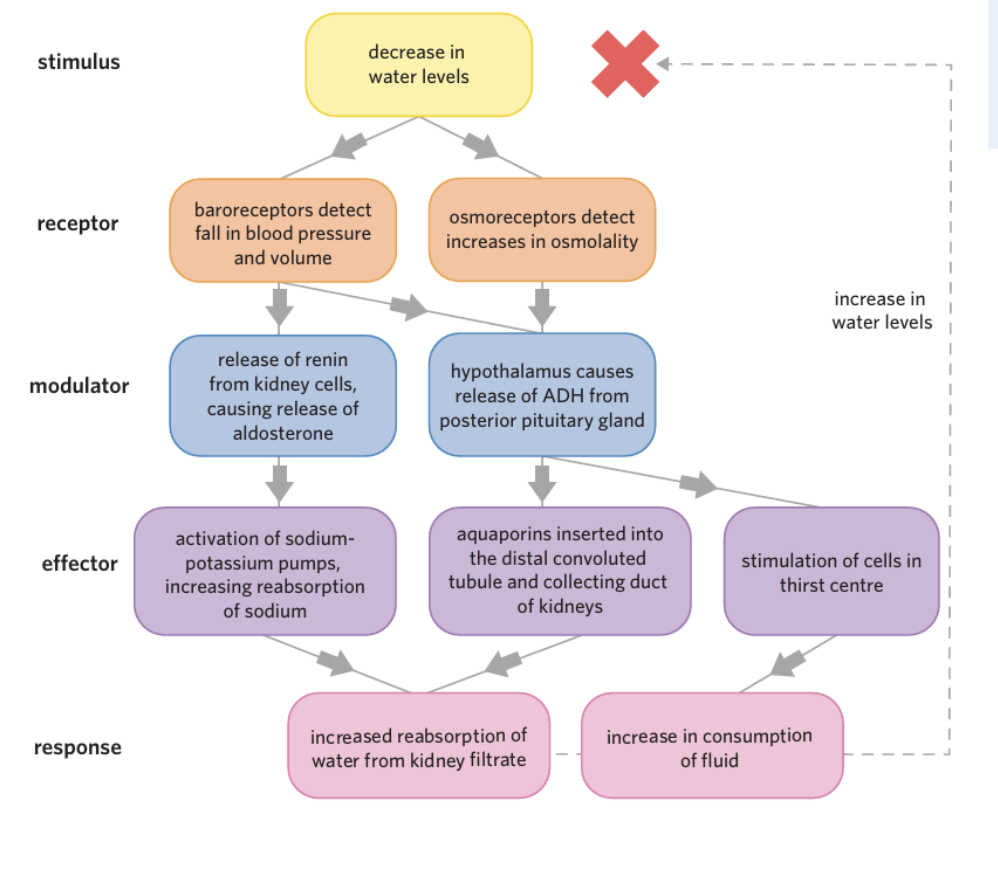
What is the ADH hormone?
Antidiuretic Hormone
ADH pathway
ADH Pathway (Osmoreceptors)
Posterior pituitary releases ADH
ADH acts on:
Distal convoluted tubule
Collecting duct
👉 Causes:
Insertion of aquaporins
increased water reabsorption into blood
👉 Also:
Stimulates thirst centre → drink more water
The body retains more water, the osmolality of blood decreases.
Renin–Aldosterone Pathway (Baroreceptors)
Kidneys release renin
→ leads to aldosterone release
👉 Causes:
↑ sodium reabsorption in kidney
Water follows via osmosis
Aldosterone activates sodium potassium pumps in the cells lining the distal convoluted tubule and collecting duct,
increased reabsorption of water from kidney filtrate
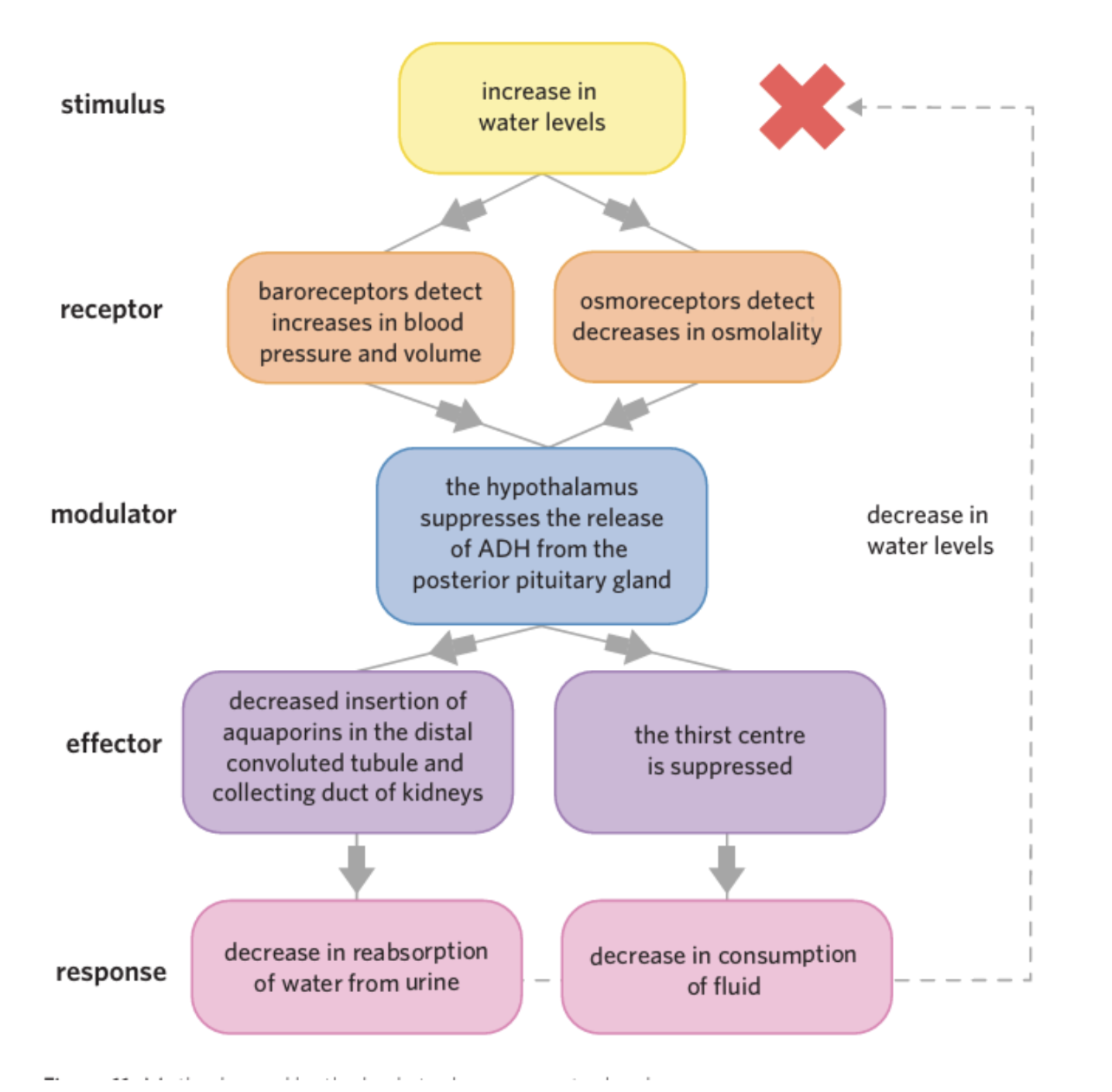
When water levels increase (Negative feedback loop)
🔹 Full stimulus–response modelstimulus
Increase in body water
decreased blood osmolality (more diluted)
Increased blood volume & pressure
Receptors:
Osmoreceptors (hypothalamus) → detects decreased osmolality
Baroreceptors (blood vessels & heart) detects increased pressure/volume
Modulator:
Hypothalamus + posterior pituitary gland
↓ ADH (antidiuretic hormone) release
Effectors:
Kidneys (distal convoluted tubule + collecting duct)
Thirst centre (hypothalamus)
Response:
Less ADH → fewer aquaporins inserted
decreased water reabsorption from kidney filtrate
more water stays in urine
Urine becomes dilute (light colour, high volume)
Thirst centre suppressed
↓ fluid intake
🔁 Final outcome (negative feedback)
Water levels ↓ back to normal
Blood osmolality ↑ back to normal
Blood volume & pressure ↓ to set point
Crenate
when a cell shrinks due to water leaving the cell by osmosis in a hypertonic environment.
osmoreceptor
a type of receptor found primarily in the hypothalamus that detects changes in osmolality
baroreceptor
a type of receptor found throughout the body that detects changes in blood pressure
Antidiuretic hormone (ADH)
Is a hormone released from the posterior pituitary gland that increases water reabsorption in the kidneys, helping the body conserve water and maintain blood osmolality.
aquaporin
a family of transmembrane proteins facilitating the transport of water into and out of a cell
Renin
is an enzyme released by the kidneys when blood pressure or blood volume is low. It starts a process that helps the body reabsorb more water and increase blood pressure.
Aldosterone
hormone from the adrenal glands that helps the kidneys reabsorb sodium and water, and excrete potassium, raising blood volume and pressure.
type 1 diabetes
an autoimmune disease in which beta cells of the pancreas are destroyed, resulting in an inability to regulate blood glucose levels
What causes type 1 diabetes?
-body’s immune system recognises beta cells in the pancreas as non-self and attacks them using autoantibodies
leads to
- no insulin
-blood glucose are left un regulated
-alpha cells are also impaired and can no longer function properly.
autoantibodies
proteins created by the immune system that destroy an organism’s own tissues
type 2 diabetes
a disease in which the body becomes resistant to the effects of insulin and/or doesn’t produce enough insulin to maintain normal blood glucose levels
What can lead to hypoglycaemia and hyperglycaemia
As a result of beta cell attack, people with type 1 diabetes are insulin deficient
hyperglycaemia
the state of having blood glucose levels above the normal range (>7.8 mmol/L)
Why is insulin important for the regulation of blood glucose levels?
it facilitates the entrance of glucose into cells as well as the production of glycogen. Because glucose can’t be absorbed by people with type 1 diabetes, they are at risk of hyperglycaemia.
Short term effects of type 1 diabetes
increased urination and excessive thirst
– if levels of glucose in the blood are high, glucose can push through the walls of the glomerulus and end up in the kidney filtrate.
-The presence of glucose in the filtrate increases its osmolality, meaning that the normal osmotic processes that reabsorb water in the nephron don’t function properly.
-As a result, water remains in the filtrate and a larger amount of dilute urine is produced .
-This can cause a person with type 1 diabetes to lose large amounts of water, become dehydrated, and feel thirsty
• excessive hunger and lethargy
- because their cells aren’t receiving the glucose they need to function properly, people with type 1 diabetes often feel tired and lethargic.
-In an attempt to correct the lack of glucose entering the system, the body stimulates the sensation of hunger •
weight loss – the loss of large amounts of water and the inability of cells to grow and function normally due to a lack of glucose can lead to weight loss in people with type 1 diabetes.
Long term effects of type 1 diabetes
vision loss – the tiny vessels carrying blood to the eye become damaged and leaky, leading to swelling and reduced blood flow
) • heart disease and stroke – the blood vessels supplying the heart and brain can become damaged and blocked, causing cells to be deprived of oxygen and die
• tingling or numbness in the feet and/or hands – nerves are sensitive to elevated blood glucose levels and can become damaged
• prolonged wound healing – the damaged blood vessels in people with long term wounds take longer to heal or won’t at all
• kidney damage – the blood vessels that carry blood to the kidney are very small and sensitive, and can easily be damaged by increased blood glucose levels.
hypoglycaemia
the state of having blood glucose levels below the normal range (<4.0 mmol/L)
How can someone become hypoglycaemic
Too much insulin injected
Not enough food
Too much exercise
↓ glucagon (alpha cells also impaired)
Effects of hypoglycaemia
Weakness, dizziness
Can lead to loss of consciousness or death
Management of Type 1 Diabetes
Insulin injections (short + long acting)
Insulin pump (automatic control)
Regular blood glucose monitoring
Hyperthyroidism
condition where the thyroid gland produces too much T3 and T4, increasing metabolic rate.
triodothyronine
a hormone produced and secreted by the thyroid gland. Also known as T3
-regulating metabolism, growth, body temperature, and heart rate
thyroxine
-a hormone produced and secreted by the thyroid gland. Also known as T4
-essential for regulating metabolism, heart function, muscle control, and brain development.
Graves diseaae (autoimmune)
-The immune system produces an autoantibody called thyroid-stimulating immunoglobulin (TSI)
-antibody recognises and binds to the TSH receptors on the thyroid, stimulating the thyroid to release T3 and T4
Leads to
-elevated levels of thyroid hormones
-constant stimulation to release hormones
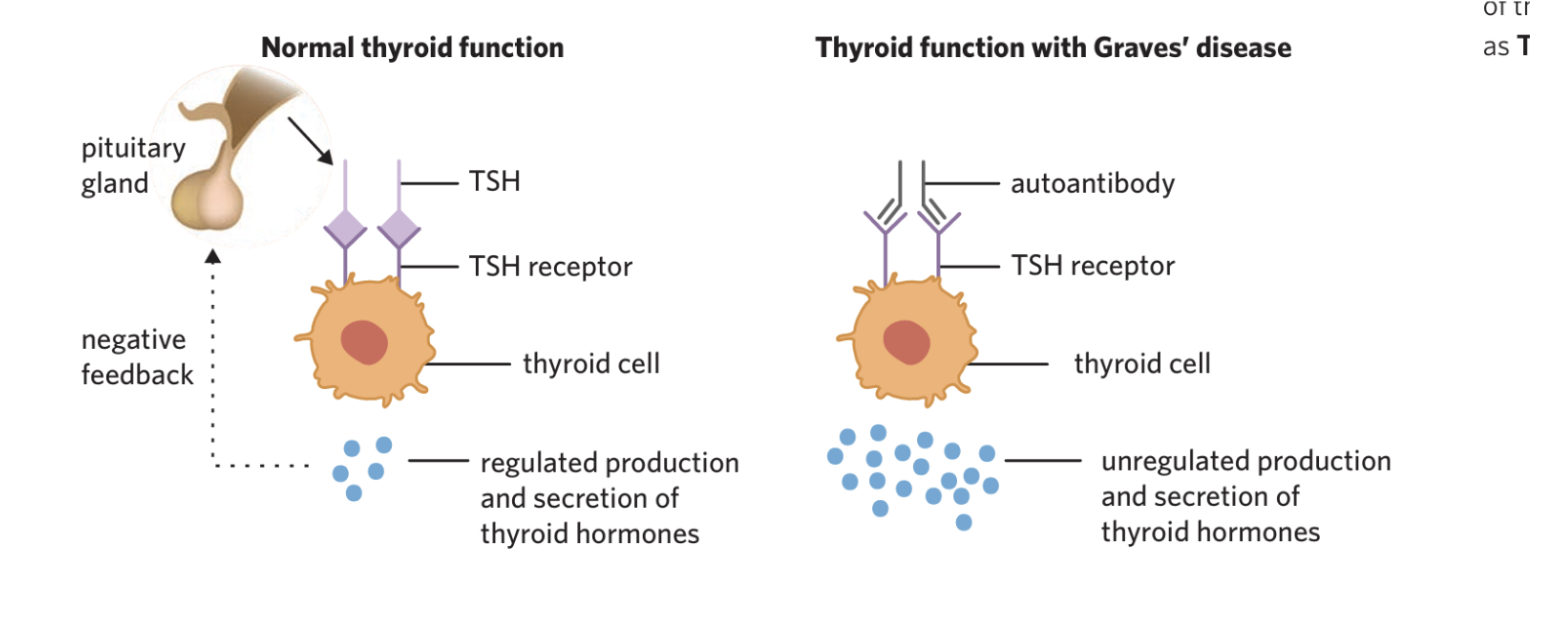
The components of the body when thyroid levels are elevated

Treatment
Medication (reduce hormones)
Radioactive iodine
Surgery (remove thyroid)