Lecture 25: Principles of Orthopedic Sx
1/65
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
66 Terms
What are the reasons to perform orthopedic surgery?
1. Stabilize fractured bones
2. Explore, débride, & stabilize injured joints
3. Replace damaged joints
4. Stabilize spinal column injuries
5. Decompress the spinal cord
6. Resect musculoskeletal tumors
7. Repair tendon and ligament injuries
What is bone transplanted from one animal to another of the same species?
allograft
What are apophyseal osteotomies?
procedures to enhance surgical exposure of a joint
What is bone transplanted from one site to another in same animal?
autograft
What is an avulsion fracture?
insertion point of a tendon or ligament is fractured and distracted from rest of the bone
Bridging plates span ________fracture.
comminuted
What is orthopedic wire placed around circumference of bone to compress an oblique fracture?
cerclage wire
What is a fractured bone alignment performed without surgical exposure?
closed reduction
What is a corrective osteotomy?
diaphysis or metaphysis of a bone is cut, realigned and stabilized until union occurs (elective procedures)
What is a positive cranial drawer test? What is it caused by?
abnormal movement of stifle joint elicited during physical exam → caused by tibia sliding cranially in relationship to femur (cranial cruciate ligament deficient stifle)
What is crepitation?
“grating feel” or sound w/ manipulating a fractured bone or arthritic joint
What type of bone union is formed without evidence of callus?
direct
What is endochondral bone formation?
bone formed on cartilaginous precursor
What is external coaptation?
fracture fixation w/ casts or splints
What is external fixation?
fracture fixation in which pins penetrate bone and skin and connected externally
What is a greenstick fracture?
incomplete fracture where portion of cortex is intact
What is hemicerclage wire or interfragmentary wire?
wire placed through predrilled holes in bone
What is the process of restoring fragment & limb alignment by distracting major bone segments (using animal's weight)?
indirect reduction
What is internal fixation?
fracture fixation using internal implants to secure bone
What are intramedullary pins?
implants positioned in the medullary canal of long bones
What is intramembranous bone formation?
direct differentiation of mesenchymal stem cells into osteoblasts, Bone forms without a cartilaginous precursor
What is complete dislocation of a joint?
luxation
What are healed fractures where anatomic bone alignment not achieved or maintained during healing?
malunions
_____________ plates support a reconstructed fracture.
neutralization
What type of fracture requires surgical intervention to create environment conducive to bone healing?
nonunion
What is a pin started at one end of bone, driven to fracture area, then seated at other end of bone?
normograde placement
What is a fracture repair performed after surgical approach to bone?
open (direct) reduction
What is the ortolani maneuver?
manipulation used to subluxate a dysplastic hip
What is an ostectomy?
removal of a segment of bone
What in an inflammatory condition of bone and medullary canal?
osteomyelitis
What is an osteotomy?
procedure where bone is cut into two segments
What is procruvatum?
cranial bowing of a bone
What is a valgus vs varus deformity?
• Valgus deformity - angulation of distal portion of limb laterally
• Varus deformity - angulation of distal portion of limb medially
What are the objectives in treating fractures, nonunions, or bone deformities?
bone union and return to normal function
What are the possible outcomes of improper orthopedic surgical planning?
implant failure
delayed healing
infection
nonunion
How is a fracture classified?
1. If fracture is closed or open to external environment
2. Degree of damage & displacement of fragments
3. Type of fracture
4. If fracture fragments can be reconstructed to provide load bearing (reducible or nonreducible)
5. Location of fracture
What type of incomplete fracture occurs in immature animals, leaves a portion of the cortex intact, and partially stabilizes bone?
greenstick fracture
What type of fracture occurs when insertion point of tendon or ligament is fractured & distracted from rest of bone and may be nondisplaced or displaced?
avulsion fracture
What type of fracture has a fracture line perpendicular to long axis of bone?
transverse fracture
What is an oblique fracture?
lines run at angle to line perpendicular to long axis of bone
• Short oblique: 45 degrees or less
• Long oblique: >45 degrees to perpendicular to long axis of bone
What type of fracture is similar to long oblique fractures, but wraps around long axis of bone?
spiral fractures
Comminuted fractures have multiple fracture lines and range from:
• 3-piece fractures w/ butterfly fragment (fragment w/ 2 oblique fracture lines resembling butterfly's silhouette)
• To highly comminuted fractures w/ 5 or more pieces
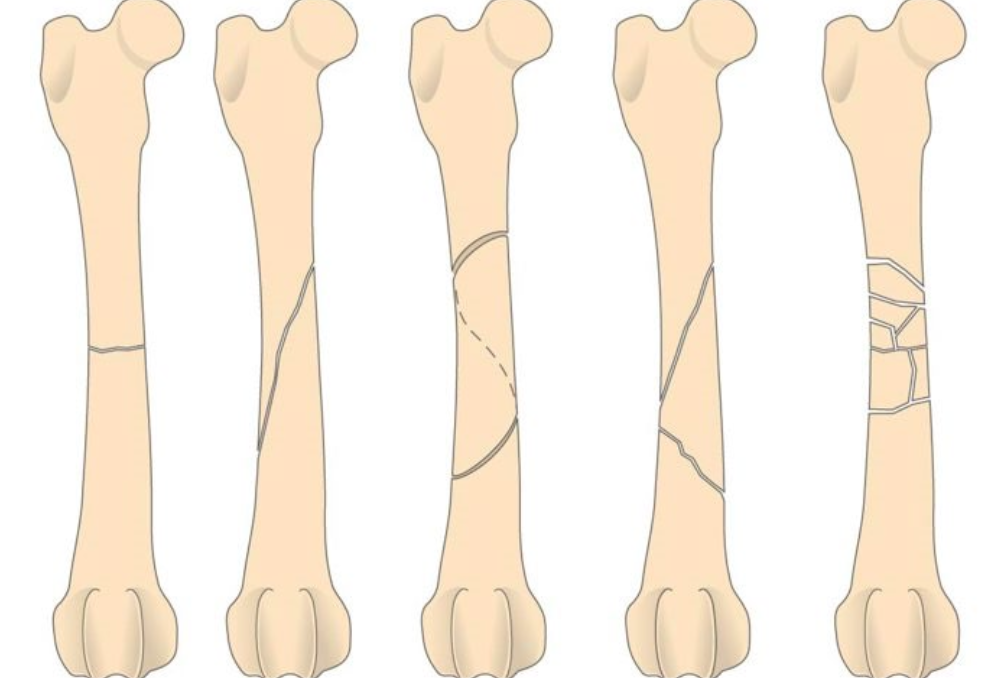
Classify these fractures from left to right.
transverse, oblique, spiral, comminuted reducible, comminuted nonreducible
What is the difference between reducible and nonreducible fractures?
reducible: single fracture line or fractures w/ no more than 2 large fragments
nonreducible: fractures w/ multiple small fragments
What dictates the number of fragments in a fracture and damage to surround soft tissues?
velocity of forces
Open fractures are classified according to:
1. Mechanism of puncture
2. Severity of soft tissue injury
What is a grade I open fracture?
• Small puncture hole located in skin in proximity of fracture caused by bone penetrating to outside
• Typically ~1cm
• Bone may or may not be visible in wound
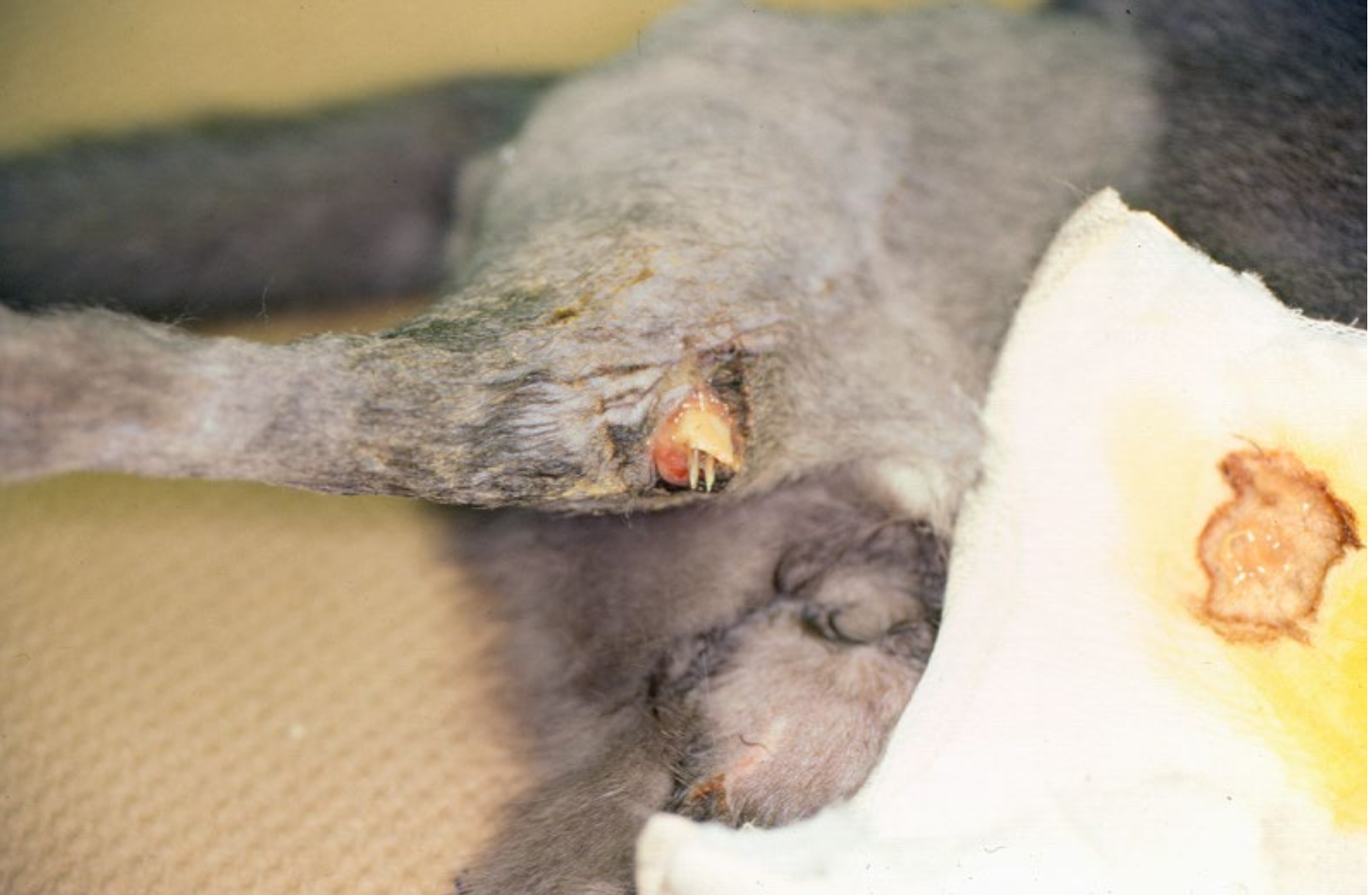
What grade of open fracture is this?
I
What is a grade II open fracture?
• Variably sized skin wound associated w/ fracture that resulted from external trauma
• More damage to soft tissue w/ grade II than w/ grade I open fractures
• While extent of soft tissue damage varies- fracture is minimally (or not) comminuted
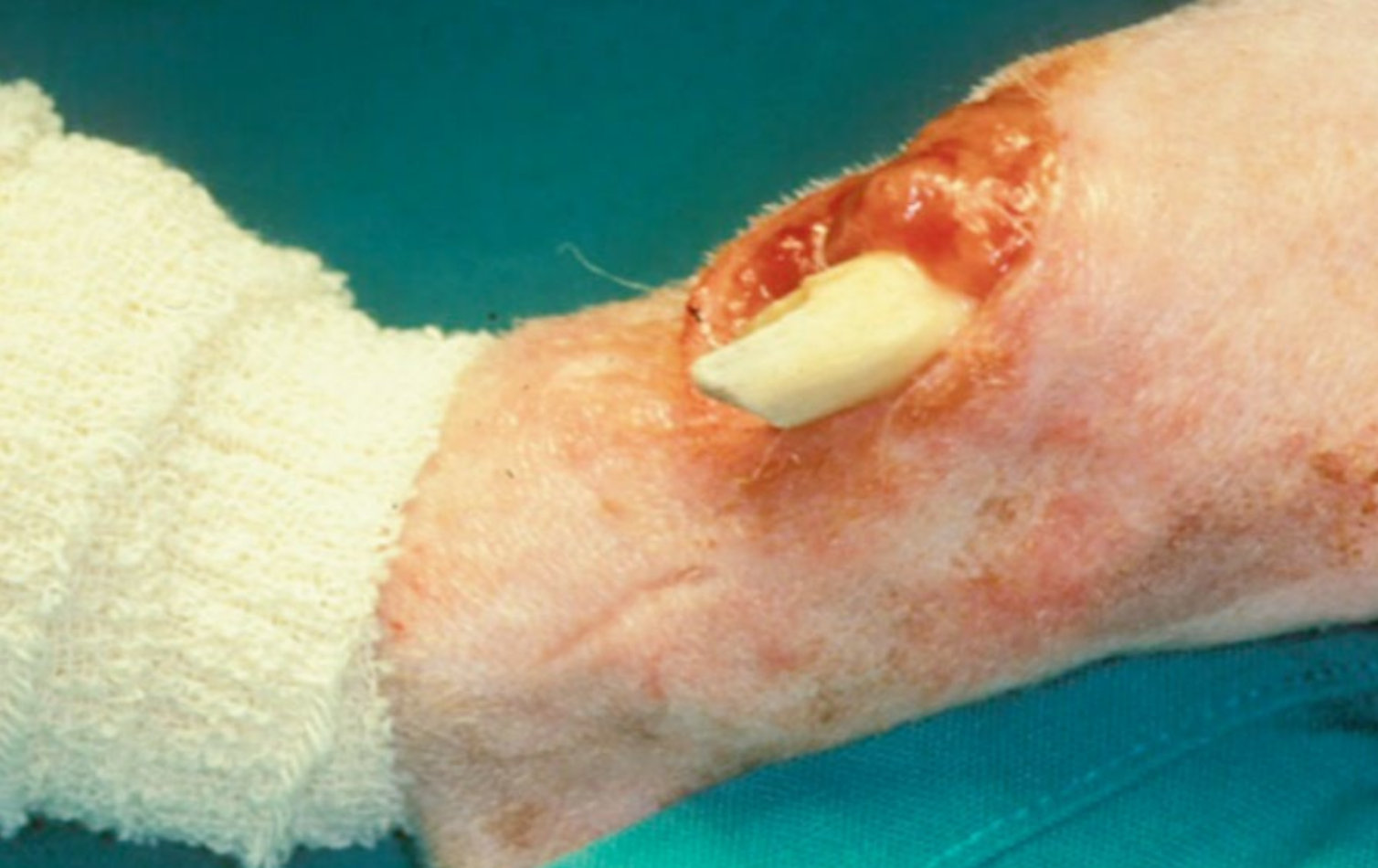
What grade of open fracture is this?
II
What is a grade III open fracture?
• Severe bone fragmentation w/ extensive soft tissue injury (With or w/o skin loss)
• Usually high-velocity comminuted fractures: Gunshot injuries, Shearing type of injuries of distal extremities
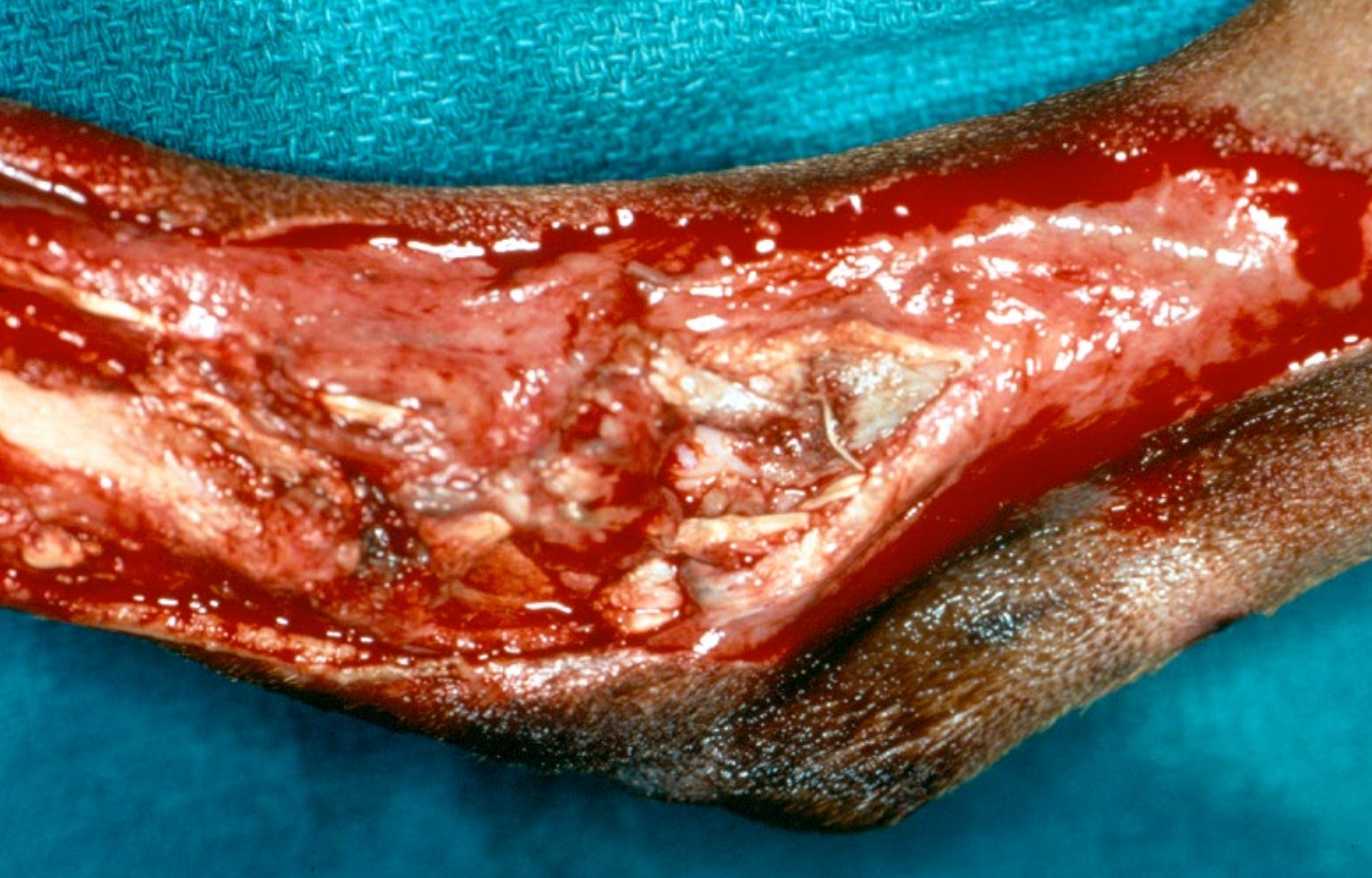
What grade of open fracture is this?
III
What are the salter harris classifications of physeal fractures?
• Salter-Harris type I: run through physis
• Salter-Harris type II: run through physis & portion of metaphysis
• Salter-Harris type III: run through physis & epiphysis & generally articular
• Salter-Harris type IV: also articular - running through epiphysis, across physis, & through metaphysis
• Salter-Harris type V: are crushing injuries of physis
• Salter-Harris type VI : describes partial physeal closures from damage to portion of physis - Causing asymmetric physeal closure
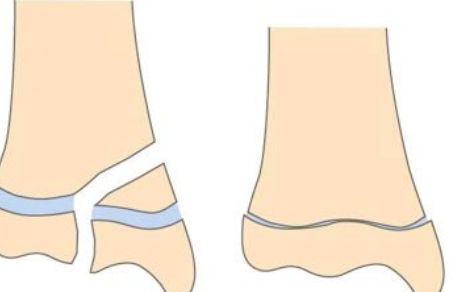
What are these two types of salter harris fractures?
IV and V
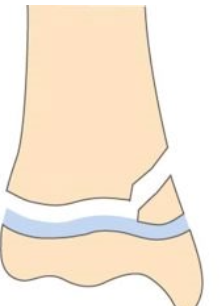
What is this type of salter harris fracture?
II
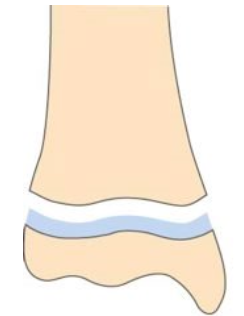
What is this type of salter harris fracture?
I
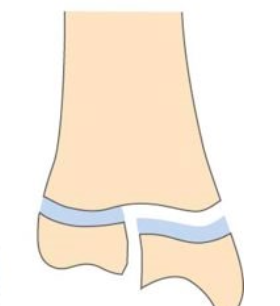
What is this type of salter harris fracture?
III
What type of fracture patterns is the result of bending forces?
transverse
What type of fracture patterns is the result of torsional forces?
spiral
What type of fracture patterns is the result of axial loading forces?
oblique or comminuted, nonreducible if high energy
What type of fracture patterns is the result of bending and axial compresion forces?
comminuted, reducible
What assessment guides the types of implants chosen?
fracture-assessment score that reflects: mechanical factors, biologic factors, and clinical factors
What are the mechanical factors for patient fracture assessment?
Conditions on left (1): nonreducible & multiple limb injury
Maximum stress on implant system
Requires careful implant choice & application
Conditions on right (10):
Less stress to implant system
Reduced risk of complications
What are the biologic factors for patient fracture assessment?
Patient factors on left do not favor rapid healing:
Implant system must function for prolonged periods
old patient, poor health, cortical bone, poor soft tissue envelope, extensive approach, high-velocity injury
Patient factors on right favor rapid healing:
Implant only needs to function for a short time
juvenile, excellent health, good soft tissue envelope, cancellous bone, low-velocity injury, closed
What are the clinical factors for patient fracture assessment?
Clinical factors on left require comfortable implant system:
Requires little postoperative maintenance
poor client and patient compliance, wimp, high comfort level required
Clinical factors on right use any implant system:
Regardless of postoperative maintenance
good client and patient compliance, stoic, comfort level not a consideration
How are FASs scores generally interpreted?
high = 8-10, moderate = 4-7, low = 1-3
fractures with high scores heal successfully with few complications
fractures with lower scores potentially less successful with more complications