Chem 1 midterm
1/143
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
144 Terms
what are the 4 main causes of Hypoglycemia
insulinoma, malabsorption, liver disease, Hypoactive adrenal glands
What are the symptoms of hypoglycemia? (6)
hunger, dizziness, nervousness, shaking, confusion, blurred vision
what fasting glucose level must be measured on 2 separate occasions for a diagnosis of hypoglycemia?
less than 50 mg/dL
______ is the only hormone that lowers glucose
insulin
what seven hormones raise glucose
growth hormone, ACTH, Glucocorticosteroids, Epinepherine, Glucagon, Thyoxine, somatostatin
Plasma glucose values are _____than whole blood values
higher
a normal adult fasting glucose range is _____ to _____
70-100 mg/dL in serum/ plasma 60-90 mg/dL in whole blood
critical high glucose is over ______mg/dL
700
critical low glucose is less than _____ mg/dL
40
The hexokinase glucose testing method combines what four things?
Hexokinase, Glucose 6 phosphate, NADP, G-6-PD
why must RBC’s be removed from plasma within 30 minutes?
RBC’s will continue to consume glucose in the sample
gluconeogenesis makes ____ from ____
glucose from glycerol, lactate, pyruvate, propionate, or glucogenic amino acids
The glucose-oxidase test is a ______ reaction and uses ______, _______, and ______
color change, glucose oxidase, reduced chromatin, peroxidase
NADH is used to fund ____ and produces _____ ATP
Electron transport chain, 32
Glycogenolysis turns _____ into ______ and _____
glycogen, glucose-1-phosphate and glucose
Glycolysis takes _____ ATP to run and produces ________, __________, and ________
pyruvate, 4 ATP, 4 NADH
what metabolic process breaks down glycogen into glucose?
Glycogenolysis
What 4 conditions can effect A1C interpretation
sickle cell anemia, polycythemia, hemolytic anemia, splenectomy
how do we test foe ketone bodies?
Nitroprusside test, purple dipstick
what are ketone bodies made of?
Acetoacetate, beta-hydroxybutyrate, acetone
what are ketone bodies formed from?
free fatty acids
what are common complications of diabetes/ what are diabetes associated disease states? (9)
Atherosclerosis, coronary artery disease, stroke, gangrene, high blood pressure, retinopathy, nephropathy, neuropathy, ketoacidosis
what are the criteria for diagnosis of gestational diabetes?
a 3 hour glucose tolerance test with 2 of any of the following values: 95 mg/dL fasting, 180 1 hour, 155 2 hour, 140 3 hour
what are the criteria for diagnosing pre-diabetes?
on two separate occasions either a fasting glucose tolerance test of between 100-125 or a two hour glucose tolerance test between 140-200
what is a normal fasting glucose tolerance score
70-100
what is a normal 2 hour glucose tolerance test score?
less than 140
what is a pre-diabetic fasting glucose tolerance test score?
101-125
what is a prediabetic 2 hour glucose tolerance test score?
140-199
what is a fasting diabetic glucose tolerance test score?
126+
what is a 2 hour diabetic glucose tolerance test score?
200+
what are the associated findings of prediabetes?
increased risk of atherosclerosis, electrocardiographic abnormalities, hypertension, hyperlipidemia, obesity
what are the requirements for a diagnosis of diabetes?
a 2 hour glucose tolerance test of 200+ or any of the following met on 2 separate occasions: fasting glucose 125+, random glucose 200+ with diabetes symptoms, Hgb A1C 6.5+
what are the common type 2 diabetes symptoms?
frequent infections, blurred vision, tingly/numb hands/feet, obesity
what are the lab findings of type 2 diabetes? (5)
fasting glucose 126+, abnormal glucose tolerance test, glycosuria, elevated glycated hemoglobin, decreased number of insulin receptors on tissues
What is the root cause of diabetes?
no insulin production due to autoimmune destruction of beta cells of the pancreas
what percentage of diabetes cases are type 1
5%
what percentage of diabetes cases are type 2
95%
what is the root cause of type 2 diabetes?
normal-high insulin production with insulin resistant cells
type 2 diabetes is often diagnosed in what demographic?
adults 40+
what are the common symptoms of type 1 diabetes?
polyuria, polydipsia, polyphagia, unusual weight loss, extremewh fatigue, irritability
What is A1C?
glycosylated hemoglobin
what does A1C tell us?
glucose levels over the last 6-8 weeks
what is a normal A1C range?
3.8-6.3%
what is a slightly elevated A1C range?
6.3-8.3%
what is an elevated A1C range?
8.3-12.3%
what is an extremely elevated A1C range?
12.3%+
what is proteinuria an indicator of?
kidney damage
carbohydrates are composed of what 3 elements?
C,H,O
what term refers specifically to blood glucose concentration
glycemia
Glucose of best classified as what type of carbohydrate?
monosaccharide
a fasting plasma glucose value of 110 mg/dL is most consistent with what condition?
impaired fasting glucose
which specimen tube is preferred to prevent glycolysis during glucose testing?
gray top
a small wavelength corresponds with _____ energy light where as a large wavelength corresponds with a ______ energy light
high, low
what is Beer’s law in words
when a monochromatic beam of light is shone through a solution the amount of light absorbed is directly proportional to the number of particles in solution
what is lambert’s law in words?
when a monochromatic beam of light is shone through a solution the amount of light absorbed is proportional to the distance the light traveled
what is Beer’s law equation?
A= l e c
what is the equation relating absorbance and percent transmittance
Absorbance = 2- log(percent transmittance)
how is beer’s law rearranged to relate concentrations and absorbance for knowns and unknowns?
unknown concentration= (absorbance unknown/absorbance standard) * standard concentration
in spectrophotometry what does absorbance represent?
amount of light absorbed by sample
according to Beer’s law, absorbance is directly proportional to ______
analyte concentration
which factor is controlled by using standard cuvettes in spectrophotometric assays
path length
as the concentration of an analyte in solution increases the amount of transmitted light _____
decreases
percent transmittance is calculated by comparing ______ to _______
transmitted light to incident light
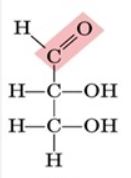
what kind of sugar is this?
aldose
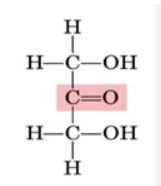
what kind of sugar is this?
ketose
glucose is only able to be metabolized in the ______ conformation
open
starch and glycogen form highly ______ chains
branched
cellulose is also known as _____
fiber
pyruvate made via glycolysis is turned into ______ before entering the Krebs cycle
acetyl-CoA
the Krebs cycle produces 4 products ________, ________, __________, and _______
1 ATP, 3 NADH, 1 FADH, 2 CO2
in a test tube glucose decreases at a rate of ______% per hour
7%
why are oxalate and sodium fluoride added to chemistry blood samples?
prevents clotting and stops glycolysis
why is a glucose test carried out on CSF?
to diagnose bacterial meningitis
POC glucometers consistently measure _________ than serum glucose tests
lower
what is the most common cause of hyperglycemia?
diabetes
in the US _____% of the population has diabetes, _____ out of _____ people have prediabetes, and ______ out of _____ people have gestational diabetes
8%, 1/3, 6-8%
what is the second largest organ in the body?
liver
what do bile ducts do?
remove waste from liver, pancreas, and gull bladder into the duodenum
what are the two physiologic functions of the liver?
circulation and hematopoietic (formation of blood cells in developing embryo)
all venous blood from the stomach, pancreas, and intestines first stops at ______
the liver
arteries carry blood _______ the heart
away from
what vein sends blood through the liver?
hepatic portal vein
what does the liver being part of the first pass metabolism mean?
the liver gets first dibs on nutrients and intercepts any bacteria
what are liver lobules
hexagonal liver tissues
what are bile cannaliculi?
the space between two rows of hepatocytes where hepatocytes dump toxins, ends at a bile duct
what are hepatic stellate cells?
liver cells that store fat soluble vitamins
what are Kupffer cells?
liver cells that remove foreign debris and particles that came from the hepatic portal system
what are liver sinusoidal endothelial cells?
cells that maintain immune function in the liver
what are the six roles of hepatocytes?
protein synthesis, protein storage, metabolism and storage of carbohydrates, synthesis of cholesterol bile salts and phospholipids, detox modification and excretion of substances, initiation of formation and secretion of bile
what cells convers ammonia to urea?
hepatocytes
hemoglobin is made out of 2 _____ chains, two ______ chains, and 4 heme molecules. each heme molecule contains ______ iron molecule(s)
alpha, beta, 1
what cells destroy old erythrocytes to recycle the iron inside?
macrophages
the first step of recycling iron is to breakdown heme into ______ using _______ and ______
biliverdin, oxygenase, molecular oxygen
the second step in recycling heme is to turn _______ into _________ using the enzyme _______ and _______
biliverdin, bilirubin, bilirubin reductase, NADPH
the final step in recycling heme is to convert ________ into _______ using the enzyme _______ to add 2 molecules of _________ creating ________
unconjugated bilirubin, conjugated bilirubin, uridine glucouranyl transferase, glucuronic acid, soluble bilirubin
how can bacteria unconjugate bilirubin?
via fermentation
what is bilirubin turned into for excretion via pee?
urobilin
what is bilirubin turned into for excretion via poop?
stercobolin
what three non-hemoglobin proteins use heme?
myoglobin, catalases, cytochrome P450 enzymes
what eight items are on a standard hepatic pannel?
AST, ALP, ALT, GGT, albumin, total protein, bilirubin total, bilirubin direct