Nutri Sci Midterm 3
1/125
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
126 Terms
What happens in lipids absorption & transport? What is the emulsifier and what is formed?
Fatty acids don’t mix well with water. Bile serves as a emulsifier and micelles are formed. Micelles transport lipid digestion products into enterocytes.
What lipase action happens in the mouth, stomach, and small intestines?
Mouth - not much, some in infants. Stomach - gastric lipase but not much. Small intestine - CCK stimulates gall bladder to release bile and pancreatic lipase. Lipases break TG into monoacylgyceride and two free fatty acids.
What is triglyceride digestion?
Three fatty acids bound to glycerol backbone. Enzymes in digestive tract (lipsases) break down triglyceride and release free fatty acids.
What happens in lipid digestion and absorption?
In the small intestine, the products of fat digestion and bile acids form micelles, which move close enough to the microvilli to allow lipids to diffuse into the mucosal cells. Inside the mucosal cells, fatty acids and monoglycerides are reassembled into triglycerides and incorporated into lipid transport particples, which enter the lymph.
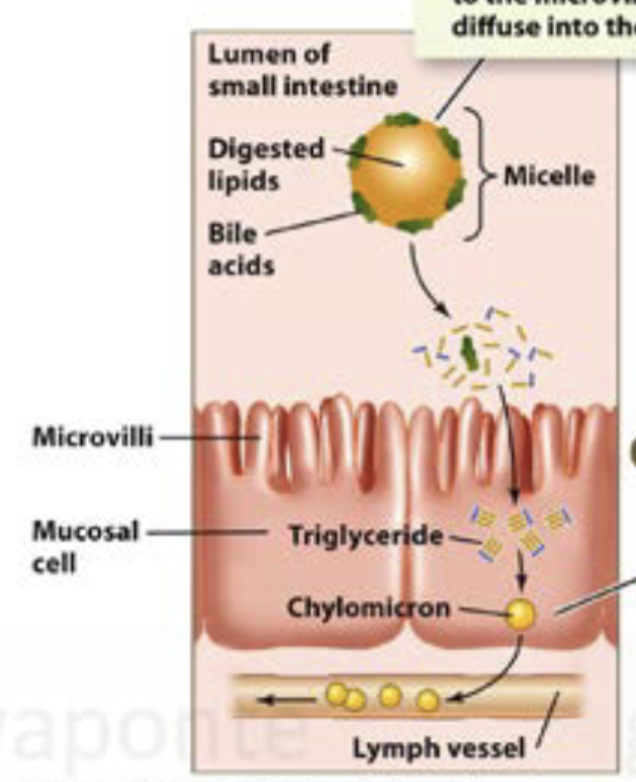
What is the enterohepatic circulation of bile?
made in the liver, stored in the gall bladder. Emulsifies fat, allowing enzymes to hydrolyze it into smaller units that cna be absorbed. Greenish fluid containing bile salts - derived from cholesterol, phospholipids (lecithin), cholesterol, bile pigments. Bile secretion stimulated by CCK.
What lipids in the body are for absorption & transport?
In the enterocyte, short & medium chain fatty acids (<14 C chain) enter portal circulation. Long chain fatty acids reassembled into TG. They combined with cholesterol, phospholipids and small proteins. These are now a lipoprotein called chylomicron. Chylomicrons enter the lymph then the bloodstream.
What are lipoprotein?
They transport lipids & cholesterol in the blood
What are lipoproteins?
Lipids in blood circulation. Chylomicrons are a type of lipoproteins. There are very low density lipoproteins (VLDL), low density lipoproteins (LDL) - CHD risk, high density lipoproteins (HDL) - protective. Protein components (apolipoproteins) involved in metabolism and final disposition of lipoprotein.
Types of lipoproteins in dietary lipids
(VLDL) very lod density lipoprotein happens in liver—> delivery of fatty acids made by liver.
Losses fatty acid to be intermediate-density lipoprotein (IDL) —> delivery of fatty acid made by liver
Loss of fatty acids to be low-density lipoprotein —> delivery of cholesterol
High-density lipoprotein (HDL) —> picking up excess cholesterol from cells for delivery back to the liver.
Chylomicron —> delivery of dietary fatty acids
How does lipid transport from the small intestine?
Chylomicrons formed in the mucosal cells pass first into the lymph, drains into the blood. They circulate in the blood, delivering triglycerides to body cells. The enzyme lipoprotein lipase, in the surface of cell lining in blood vessels, breaks down the triglycerides in chylomicrons into fatty acids and glycerol. These can then enter the surrounding cells. VLDLs are made in the liver and transport lipids away from the liver. They function similarly to chylomicrons because both particles deliver triglycerides to body cells with the help of the enzyme lipoprotein lipase. To deliver cholesterol, LDL particles bind to LDL receptors in the cell membrane. This allows the LDL particle to enter the cell, where the cholesterol and other components can be used. HDL particles pick up cholesterol from other lipoproteins and body cells and return it to the liver. Some of this cholesterol is broken down and some is transferred to organs with high requirements for cholesterol, such as those that synthesize steroid hormones.
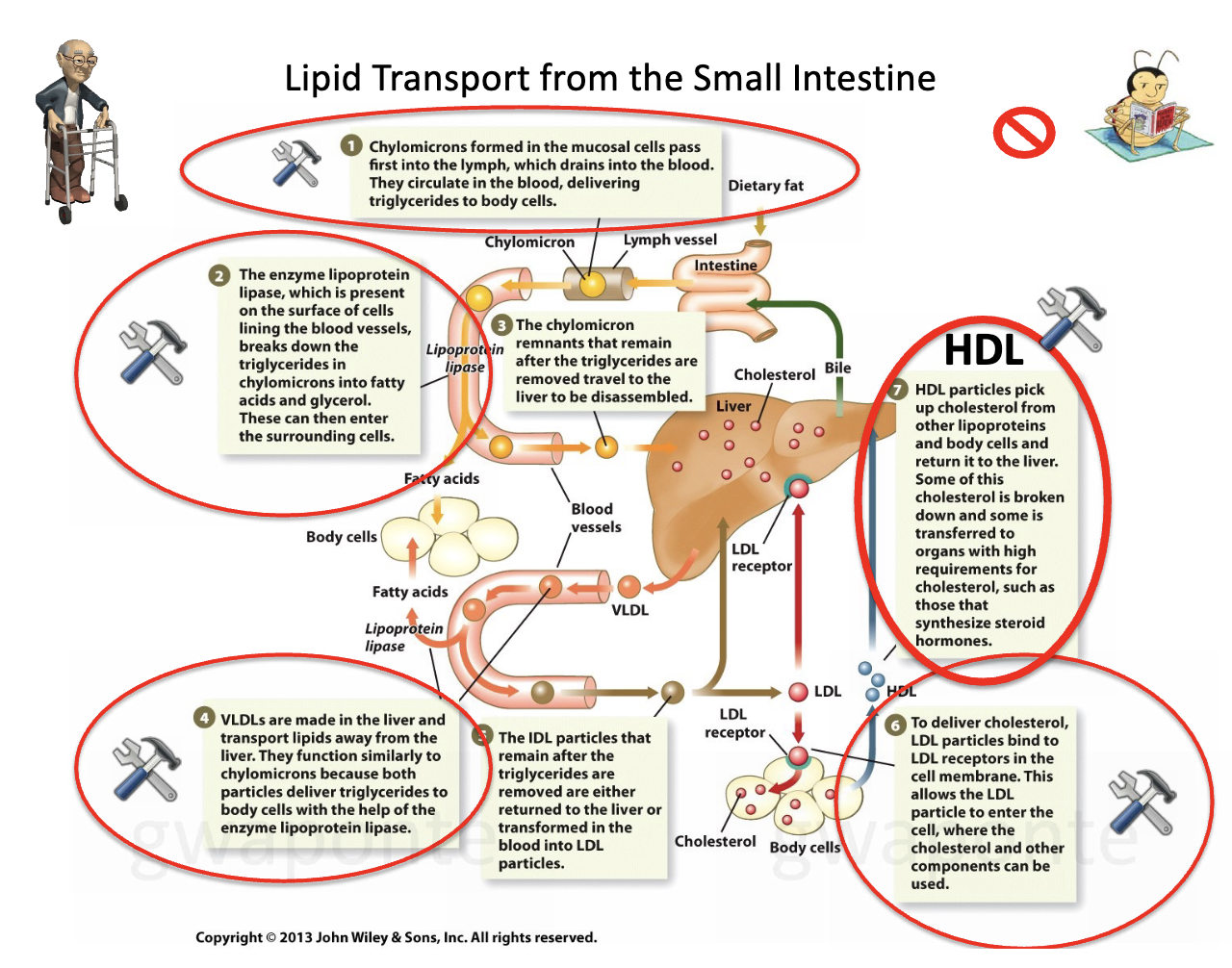
Lipid Digestion and absorption steps
A small amount of digestion occurs in the stomach due to the action of gastric lipase produced in the stomach. The liver produces bile, which is stored in the gallbladder and released into the small intestine to aid in the digestion and absorption of fat. The pancreas produces the enzyme pancreatic lipase, which is released into the small intestine to break down triglycerides into monoglycerides, fatty acids, and glycerol. Since fat absorption in the small intestine is efficient, very little fat is normally lost in the feces.
What is cardiovascular disease and what are the types?
Abnormal condition of the heart and blood vessels.
Atherosclerosis is the narrowing & hardening of blood vessels that supply blood to the heart muscle, brain & other parts of the body.
Coronary Heart Disease (CHD) is the heart not receiving enough blood
Stroke is when the brain is not receiving enough blood
What happens to triglycerides when you eat and fast?
Triglycerides are continuously stored and then broken down, depending on the immediate energy needs of the body.
Feasting: when excess energy is consumed, it is stored as triglycerides in adipose tissue.
Fasting: When no food has been eaten for a while, triglycerides from adipose tissue are broken down, releasing fatty acids as an energy source.
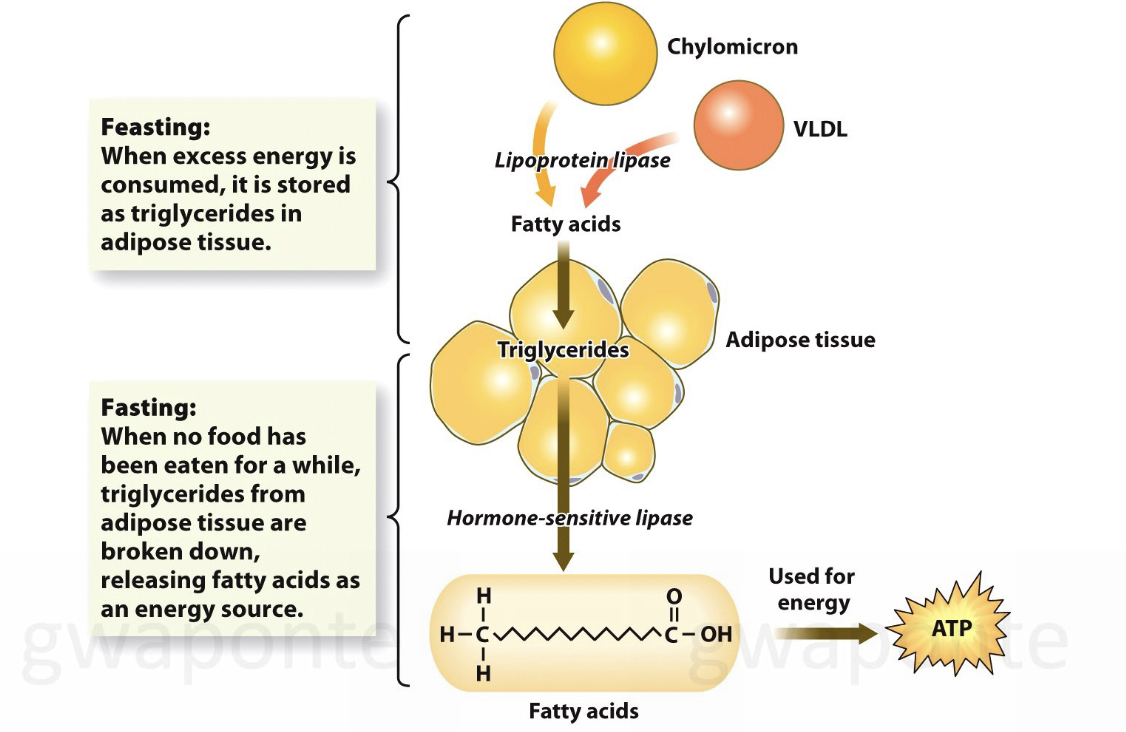
What is triglyceride energy production?
Triglycerides (from storage sites or lipoproteins in the blood)
Broken down to make glycerol and fatty acids that are released into the bloodstream)
Glycerol in the liver becomes pyruvate
Pyruvate turns into acetyl CoA and glucose
What is lipid metabolism?
Triglyceride is turned into glycerol and fatty acids
Glycerol —> pyruvate, fatty acids —> oxidation
Pyruvate and oxidation = acetyl CoA
Acetyl CoA goes through TCA cycle to release NADH + H+ and FADH2 into electron transport chain
Electron transport chain received O2 and releases H2O and CO2 to make ATP
What molecule is needed to break down fatty acids?
Carbohydrates are needed to break down fatty acids.
Carbohydrate available breaks down fatty acids chain and add CoA + Acetyl CoA to the fatty acid chain.
It goes through citric acid cycle to release CO2, making ATP and H2O in the process
What are ketones?
Ketones are used for energy. They are converted back to acetyl CoA and enter TCA cycle. This process is slow because of a lack of oxaloacetate. Protein (muslce & organs), glycerol utilized to make glucose and oxaloacetate. Brain can run on energy from ketones. Ketones “spare” protein.
How are ketones lost?
Ketones are lost in urine & breath (fruity breath), dehydration where thrist is low in pH (ketoacidosis), inefficient use of energy
what does 85% lean mean?
85% lean means 15% fat; in 100 grams, 15 grams are fat. Assuming ground beef is 55% water: 100g beef = 55 gms of water, 15 gms of fat, 30 gms prot
15gms X 9 kcals/gm = 135 kcals from fat, 30 gms X 4 kcal/gm = 120 kcals from prot
[135 kcals] / [120 kcals +135 kcals] = 53%
What are dietary factors that increase risk associated with fat intake?
Cholesterol, saturated fat, trans fat, sodium, excess sugar, excess energy
Overview of digestion and absorption of vitamins
All vitamins —> digestive processes in the stomach being the release of vitamins from food.
All vitamins —> digestive enzymes produced by the pancreas aid in the release of vitamins from food
Fat-soluble vitamins only —> bile procued in the liver (and stored in the gallbladder) acids in fat-soluble vitamin absorption.
Fat-soluble vitamins only —> fat-soluble vitamins are absorbed in the small intestine, along with dietary fat, and carried by chylomicrons into the lymphatic circulation.
Water-soluble vitamins only —> absorbed in the small intestine and released directly into the blood
Vitamin K —> made by bacteria in ileum of small intestine and in the large intestine
Fat Soluble Vitamins
Vitamins A, D, E, and K
Hydrophobic/lipophilic
Storage in cells associated with fat
Rick of toxicity is greater
Digestion, Absorption, and Circulation of FSV
FSV + Fat + Bile acids = micelles —> 2. absorbed by enterocytes in SI and packaged into chylomicrons —> 3. chylomicrons are circulated through lymph, then blood before reaching the liber —> 4. stored in fat or attached to transport protein to circulate
Roles of Vitamin A
Growth, vision, skin, trachea, epithelial differentiation, thymus lymphoid organs, immune function, reproduction
What are retinoids?
A collective term for the biologically active forms of vitamin A. Preformed Vitamin A because unlike carotenoids, they dod not need to be converted in the body to become biologically active.
What are the functions of Vitamin A
Serves as pre forms and precursors.
3 active retinoids: retinol, retinal, and retinoic acid
Food sources: liver, eggs, fortified milk or cereals
Storage form in liver: Retinyl ester
VA precursor: carotene
Food soruces: orange, red, yellow, and dark green fruits and vegetables
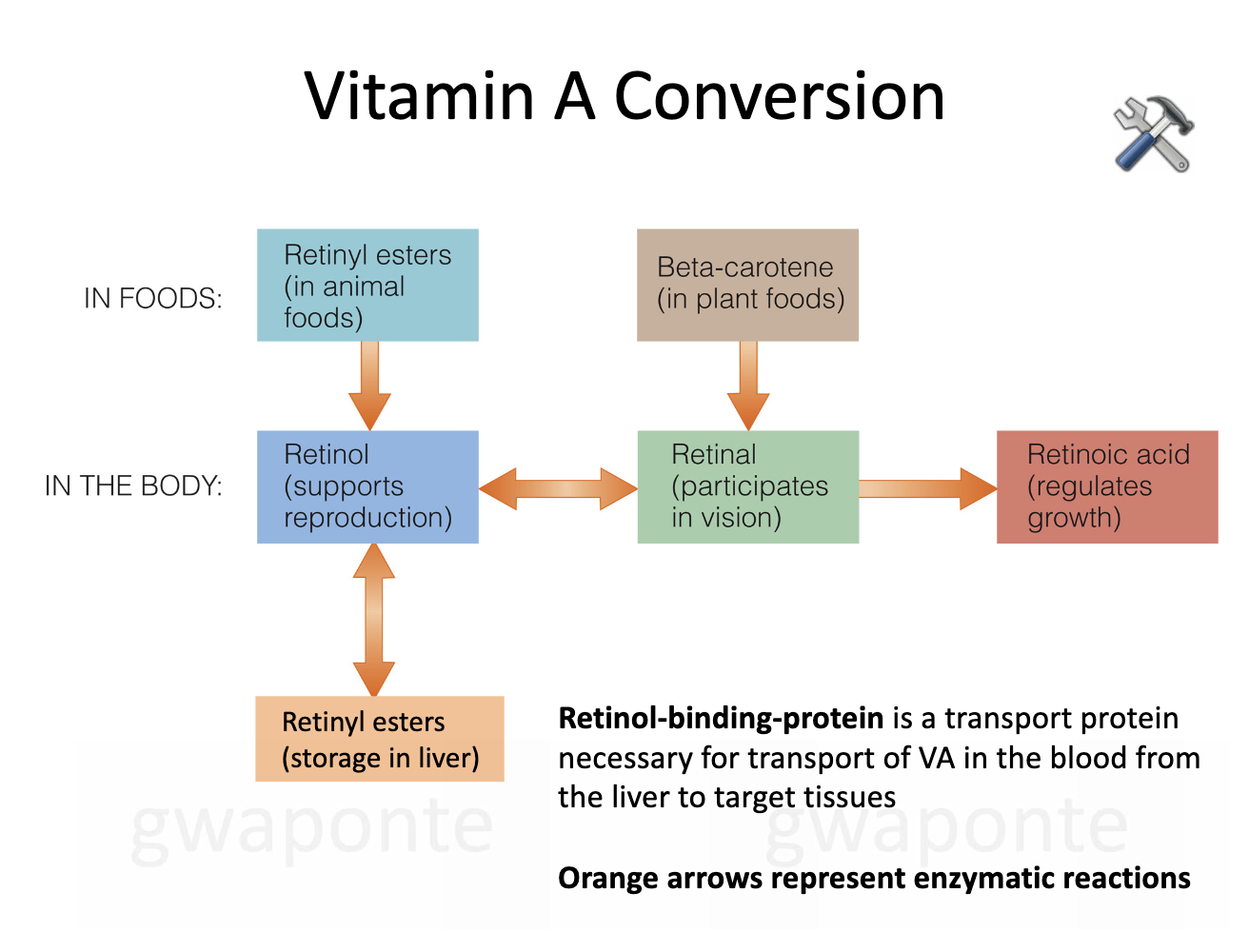
Vitamin A Conversion
In foods: retinly esters (in animal foods) and beta-carotene (in plant foods)
Moves to the body: retinol from retinyl to support reproduction and reinal from beta, and retinoic acids
Retinol makes retinyl esters to store in the liver. All from enzymatic reactions
Retinol-binding protein is a transport protein necessary for transport of VA in the blood from the liver to target tissues.
Role of vitamin A in protein synthesis and cell differentiation
Epithelial cells of skin and mucus membranes are 1st line of defense against infection. Supports differentiation and antibody prodctuion in T and B cells for specific immune responses
Role of VA in vision
Helps maintains cornea (retinoic acid)
Involved in conversation to light energy into nerve impulses in the rod cells of the retina (retinal)
Why is VA consumption important?
Consuming the right amount of VA is critical to overall health. A very low (deficient) or very high (toxic) VA intake can produce harmful symptoms and even lead to death.
VA deficiency
Occurs when insufficient VA intake or protein deficiency
Night blindness
Increased mortality from infectious disease
Zerophthalmia
keritinization
VA toxicity
Occurs when VA is in excess of binding proteins and damagers cells
Retinoid supplements are typically 750-1500 ug and many foods are fortified
increased bone fractures and osteoporosis
Birth defect
Excess b-carotene can lead to skin discoloration but is not toxic
How does Vitamin E form?
Antioxidant that protects cell membranes from free radical oxidation, 8 compounds, dietary sources: plant oils and nuts
What is free radical damage?
Damage in a molecule because it has an odd number — an “unpaired” electron. A normal molecule has an even number of paired electrons. This can occur during oxidation in the human body because it damages cell membranes and other structures including cellular proteins, lipids and DNA. When oxygen is metabolized, it creates “free radicals” which steal electrons from other molecules, causing damage.
Vitamin E deficiency
VE deficiency is rare, can occur in diseases of fat malabsorption and premature infants. Hemolytic anemia: too few red blood cells because membranes rupture. Neuromuscular dysfunction.
How does Vitamin K form?
Necessary for blood clotting and bone formation. Synthesized by gut bacteria. Dietary sources: green vegatables and plant oils.
Vitamin K Deficiency
Deficiency is rare, can occur with fat malabsorption, antibiotics, and anticoagulant drugs. Hemorrhaging, low bone density. Newborn infants have sterile GI tract at birth and are given a VK supplement.
Vitamin D roles
The active form of VD is a hormone, which regulates gene transcription. Maintains blood concentrations of calcium and phosphorous. Regulates cell proliferation and differentiation. Immune function.
Factors affecting VD synthesis in the body
Latitude, season, time of day, skin pigmentation, sun exposure, sunscreen use
How does vitamin D form?
Body can synthesize from cholesterol and UV light. VD2 in plant sources and supplements. VD3 in animal source foods and human body. VD2 is less biologically active tahn VD3. VD-binding protein required for transport in blood.
Rickets and Osteomalacia
Deficiencies from vitamin D which cause bowed legs and ribs.
VD synthesis and activation
Synthesis is in the skin:
7-dehydrocholesterol (a precursor made in the liver from cholesterol —> ultraviolet light from the sun makes previtamin D3 —> heat from the body to make vitamin D3
From the diet: Vitamin D2 (plants) and vitamin d3 (animals)
Activation:
In the liver — hydroxylation turns into calcidiol
In the kidney — hydroxylation turns into calcitriol
Role of Vitamin D
Synthesized in the skin or obtained form dietary sources, vitamind D ultimately functions as a hormone.
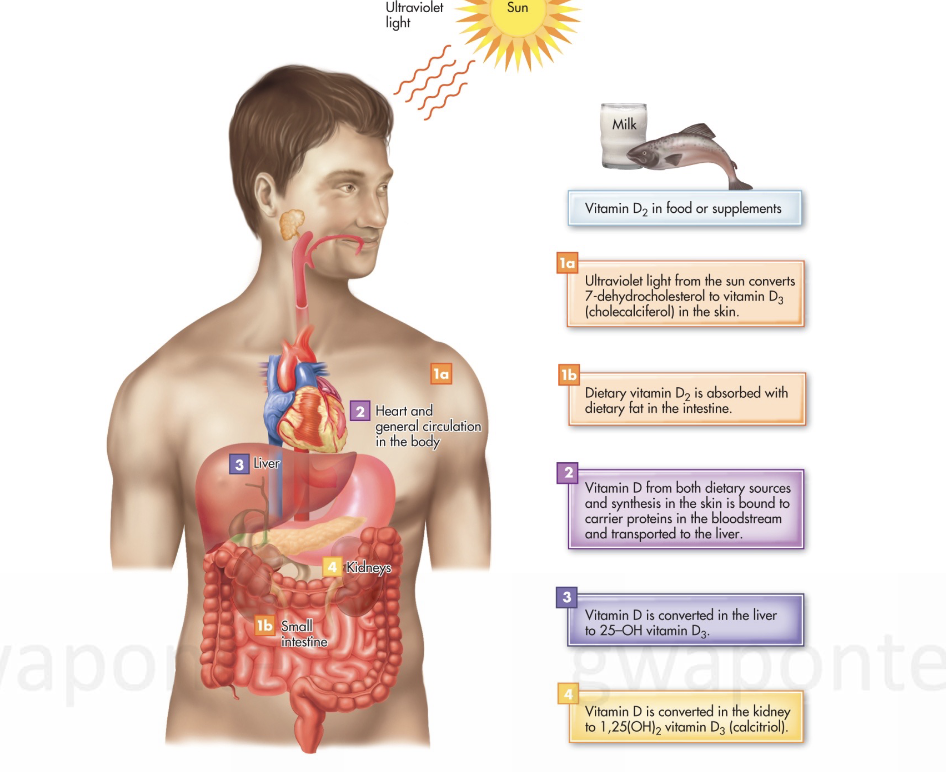
Functions of Calcium
Bone structure, release of neurotransmitters, blood pressure, muscle contraction, cell metabolism, regulate enzyme activity, blood clotting
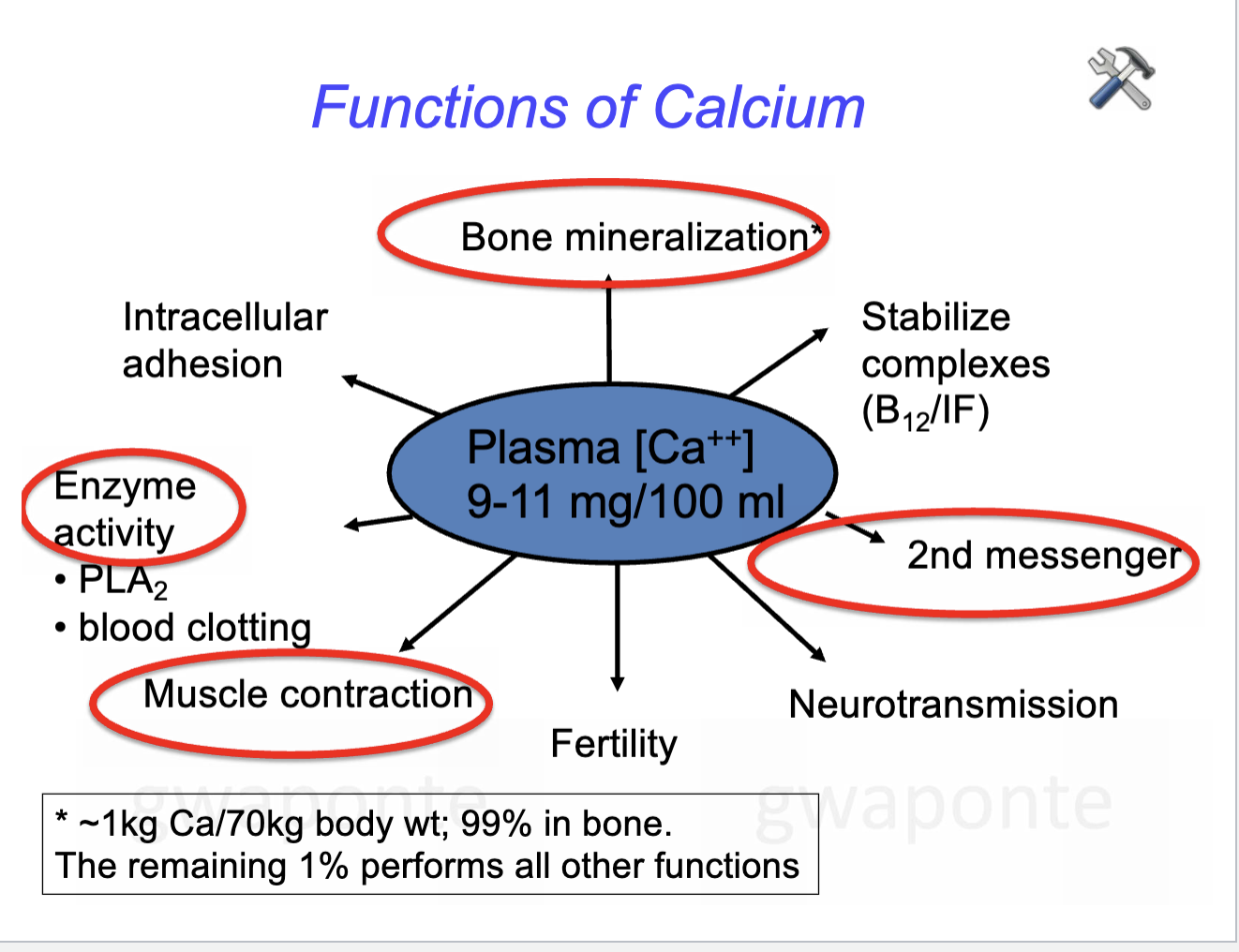
Trabecular bone (spongy)
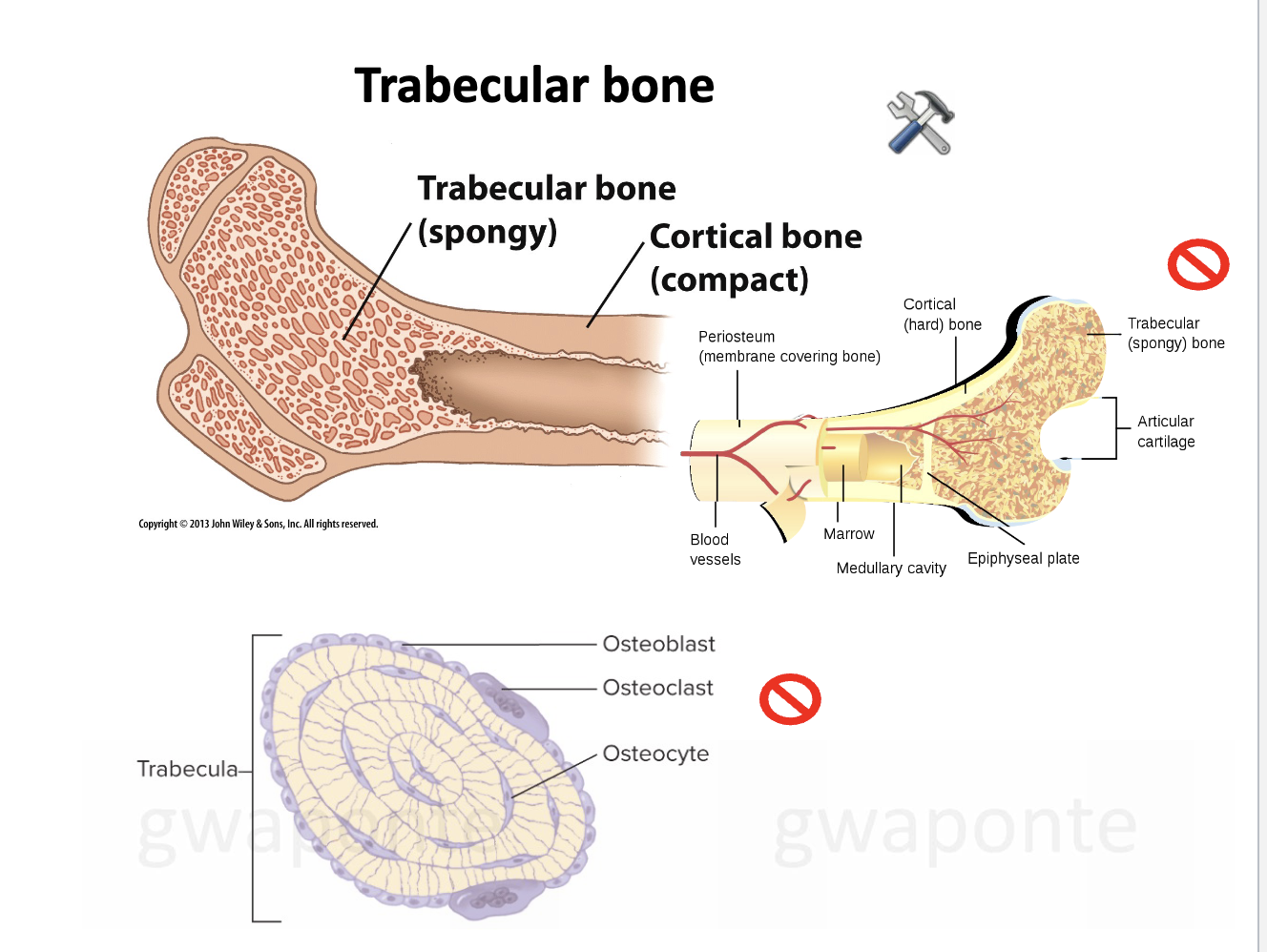
What is bone remodeling?
Bone mass is maintained by continual degradation of existing bone and synthesis of new bone. The continual remodeling facilities: adjustment to new stregnth level, adjustment ot new shape, replacement of degrading matrix (collagen and proteoglycan) during normal turnover
key players in bone remodeling
Osteoblasts are cells that produce that protocollagen and proteoglycans that ultimately constitute the “matrix of bone. Vitamin C is inovled in protocollagen syntehsis. They respond to changes in OH2D via VD receptors.
Osteocytes are osteoblasts that become entrapped in the polymerizing collagen fibers.
Osteoclasts act to degrade bone.
Osteomalacia vs. Osteoporosis
Osteomalacia — organic bone matrix normal, but not calcified matrix > calcium
Osteoporosis — matrix/calcium ratio normal, both reduced. Thin and brittle bones.
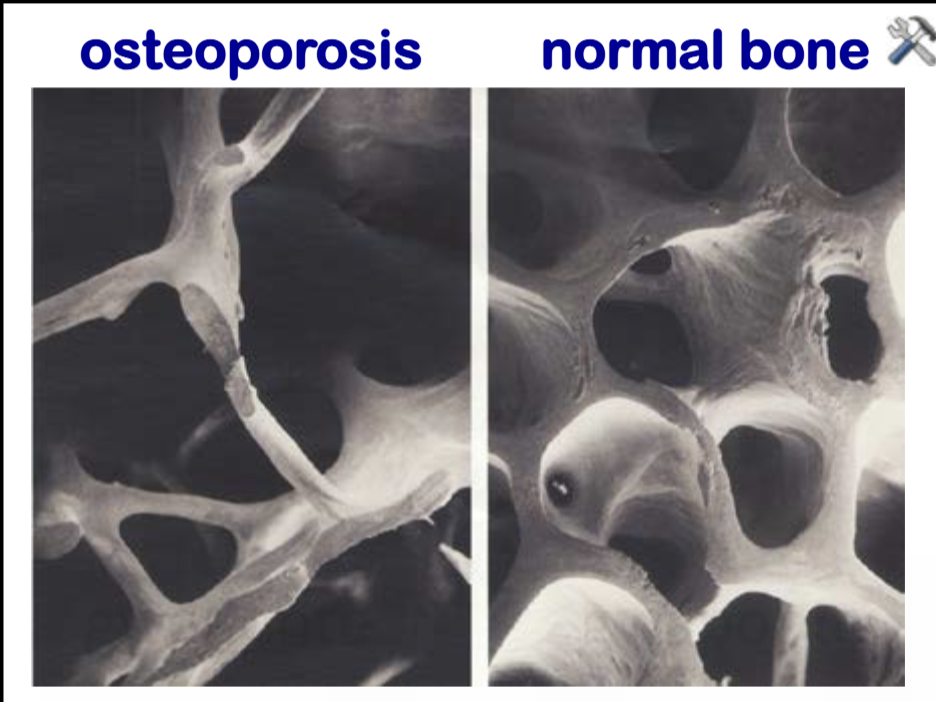
Osteoporosis
ratio of mineral:matrix is normal. Amounts of both are reduced bones are thin and brittle.
Risk factors: Being female, race, small stature, sedentary
Menopause- bone mass drops due to decrease in estrogen levels
What is the relationship between peak bone mass and osteoporosis
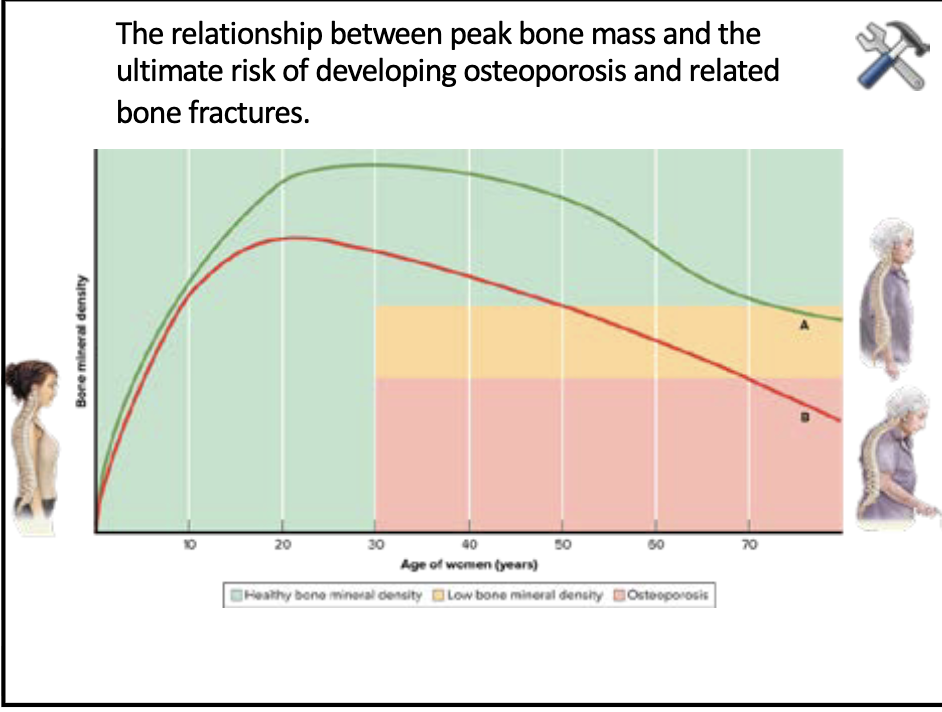
Intestinal function of calcitriol
Calcitriol — the hormone produced from Vitamin D3, is the only hormone that can induce the intestine to absorb dietary Ca++
Without VD and its conversion into calcitriol, dietary Ca++ absorption by the intestine is severely impaired.
Calcium absorption
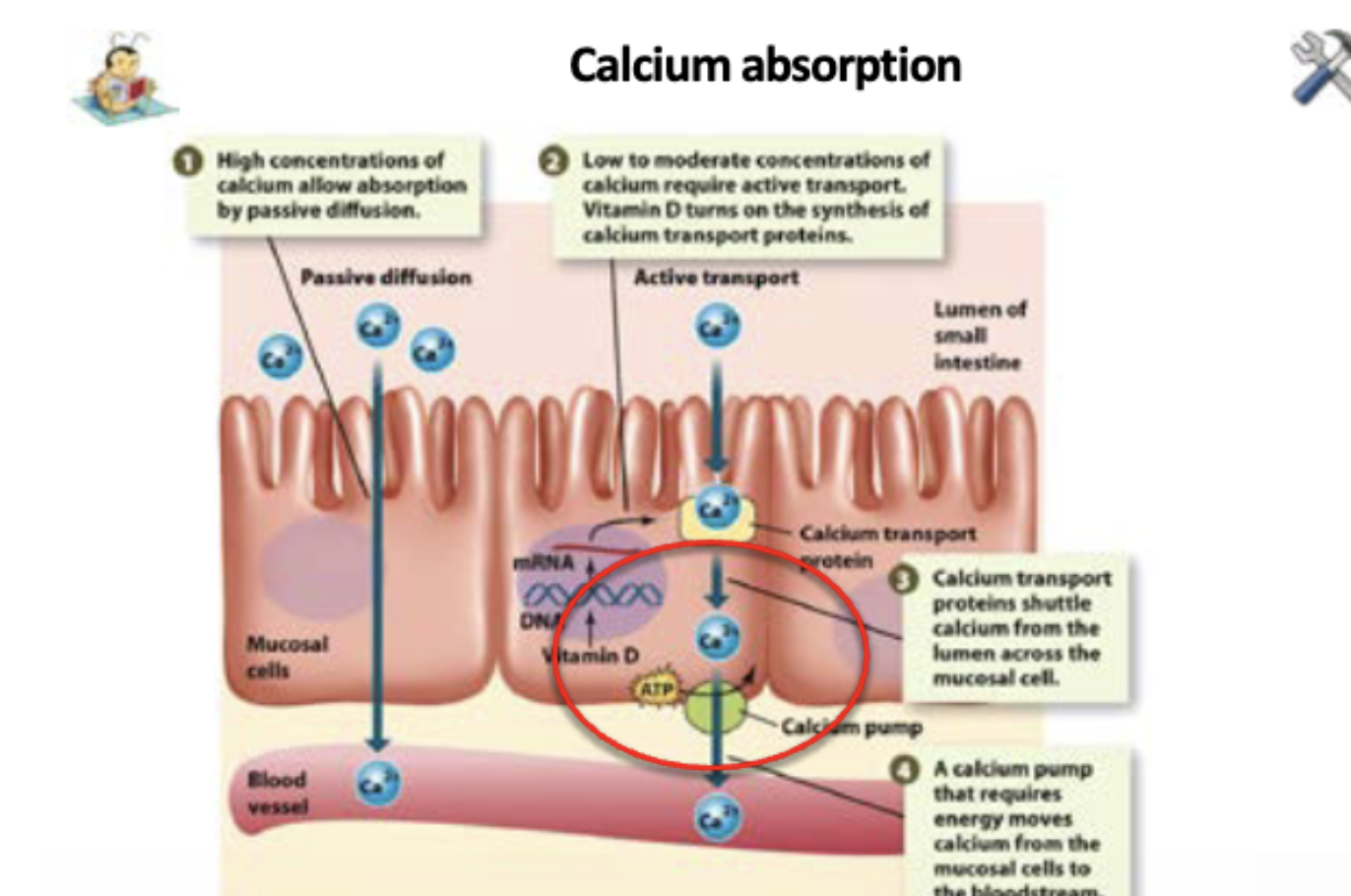
What role do hormones play in serum calcium?
Hormones play important roles in regulating serum calcium.
PTH leads to an increase in reabsorption of Ca by the kidney to the plasma
PTH increase release of Ca and P from the bone to the plasma
PTH plus VD leads to absorption of dietary Ca from intestine which is given to the plasma
*PTH
What does Calcitonin do?
Moderates effects of PTH (parathyroid hormone)/1,25 (OH)2D
Calcitonin is secreted by the thyroid gland when plasma [1,25(OH)2D] and [Ca] are high.
Calcitonin reduces plasma [Ca] by reducing osteolytic activity, reducing formation of new osteoclasts, increasing osteoblast activity
What does the regulation of blood calcium levels and PTH do?
Increases blood calcium.
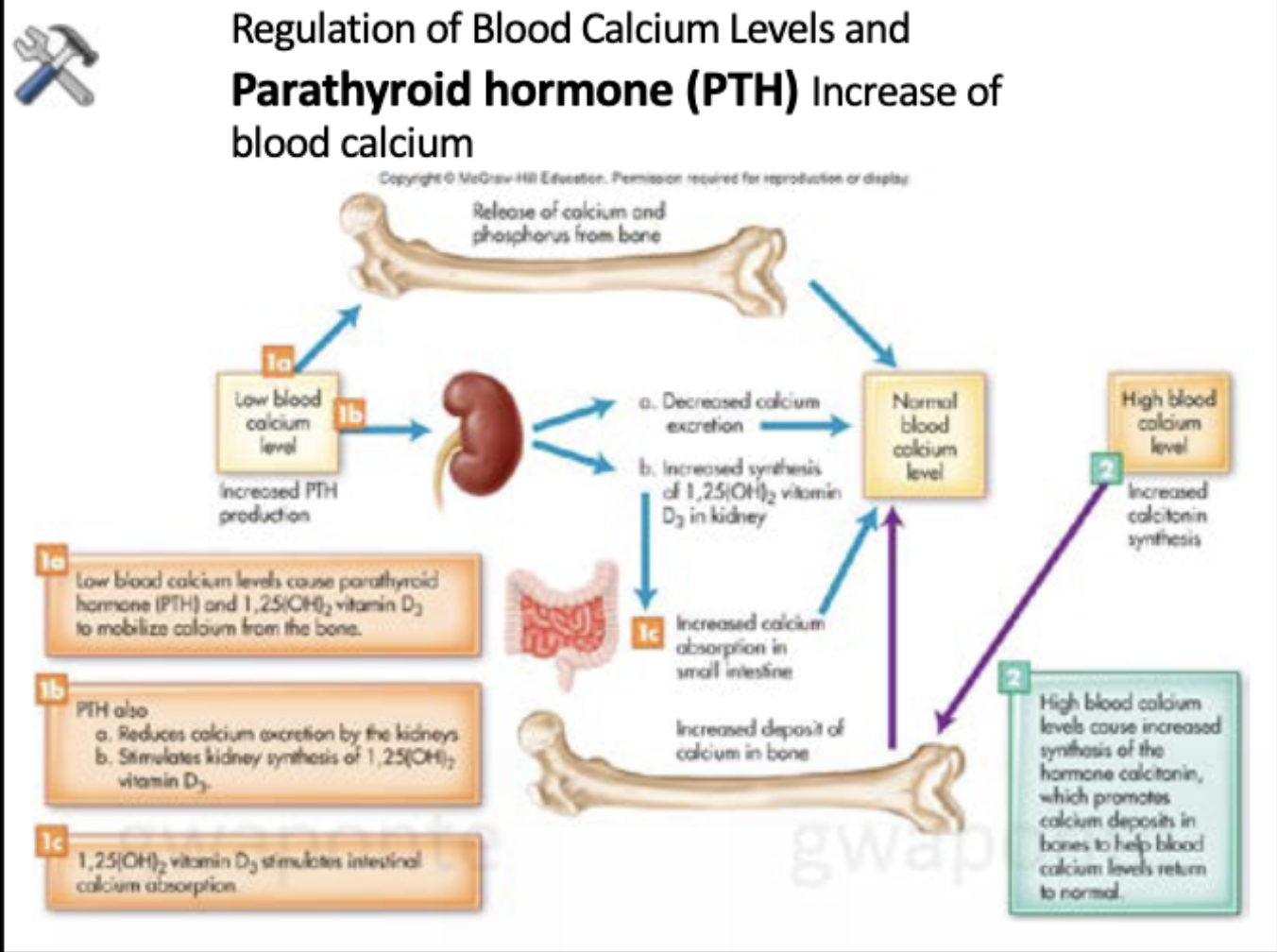
Regulation of blood calcium levels with calcitonin
High blood calcium:
In the thyroid gland, high blood calcium causes the release of calcitonin from the thyroid gland. Calcitonin inhibits calcium release from the bone. PTH stimulates calcium release from bone.
Low blood calcium:
Low blood calcium causes the release of PTH from the parathyroid gland. PTH promotes calcium reabsorption by the kidney. PTH stimulates the activation of VD by the kidney. Active VD increase intestinal calcium absorption.
What does VD toxicity do?
Megadoses through supplementation. Hypercalcemia: elevated blood calcium concentrations that can lead to calcification of tissues (kidney stones)
VD toxicity modeled
Plasma Ca++ is a mediator for muscle contraction, neurotransmission blood clotting in the bone structure.
Hypocalcemia —> tetany —> death ← soft tissue Ca++ ← hypercalcemia
Functions of phosphorous
Bone mineralization, energy transfer (ATP, ADP, GTP, creatine phosphate, etc.), acid-base buffer, components of RNA & DNA, protein modification (phosphorylation of enzymes), signaling molecules, phospholipids, structural components of teeth.
Sources of plasma calcium and phosphorus
Calcium:
from food — dairy products, tofu, green leafy vegatables
Adults need ~ 1g/day
Important for bone remodeling
Phosphorous:
From food — Ubiquitious deficient only if low energy and protein intakes
~1g/day
Important source for bone remodeling
Types of trace minerals
Co
General principles of bioavailability, competition, chemical form
Bioavailability: % of a nutrient can be absorbed
Competition: Too much of one nutrient cause deficiency of another
Chemical form: solubility, organic ligands
What is important about trace minerals? What are their functions? What happens when there are deficiencies?
Essential, daily need less than 100 mg
Biological functions: components of enzymes, DNA synthesis
Not a source of energy
Deficiency produces abnormalities. Ancient civilizations knew about iron and anemia, dwarfism in Middle East due to Zinc deficiency
Trace minerals missing in total parenteral nutrition formulas
Why is it difficult to study trace minerals?
Trace metal contamination is everywhere. Acid-washed, ultra clean glassware. Double-distilled, deionized water, filtered air, ultra purified diet components, stainless steel or plastic cages.
Tests us blood samples, but blood may not be sensitive measure exa. calcium
Marginal deficiencies may not be detected.
What is the toxicity of supplements?
Phosphorus: diarrhea, nausea, vomiting
Iron: constipation, nausea, vomiting, reduced zinc uptake, iron overload
Zinc: nausea, vomiting, immune suppression, impaired Cu uptake
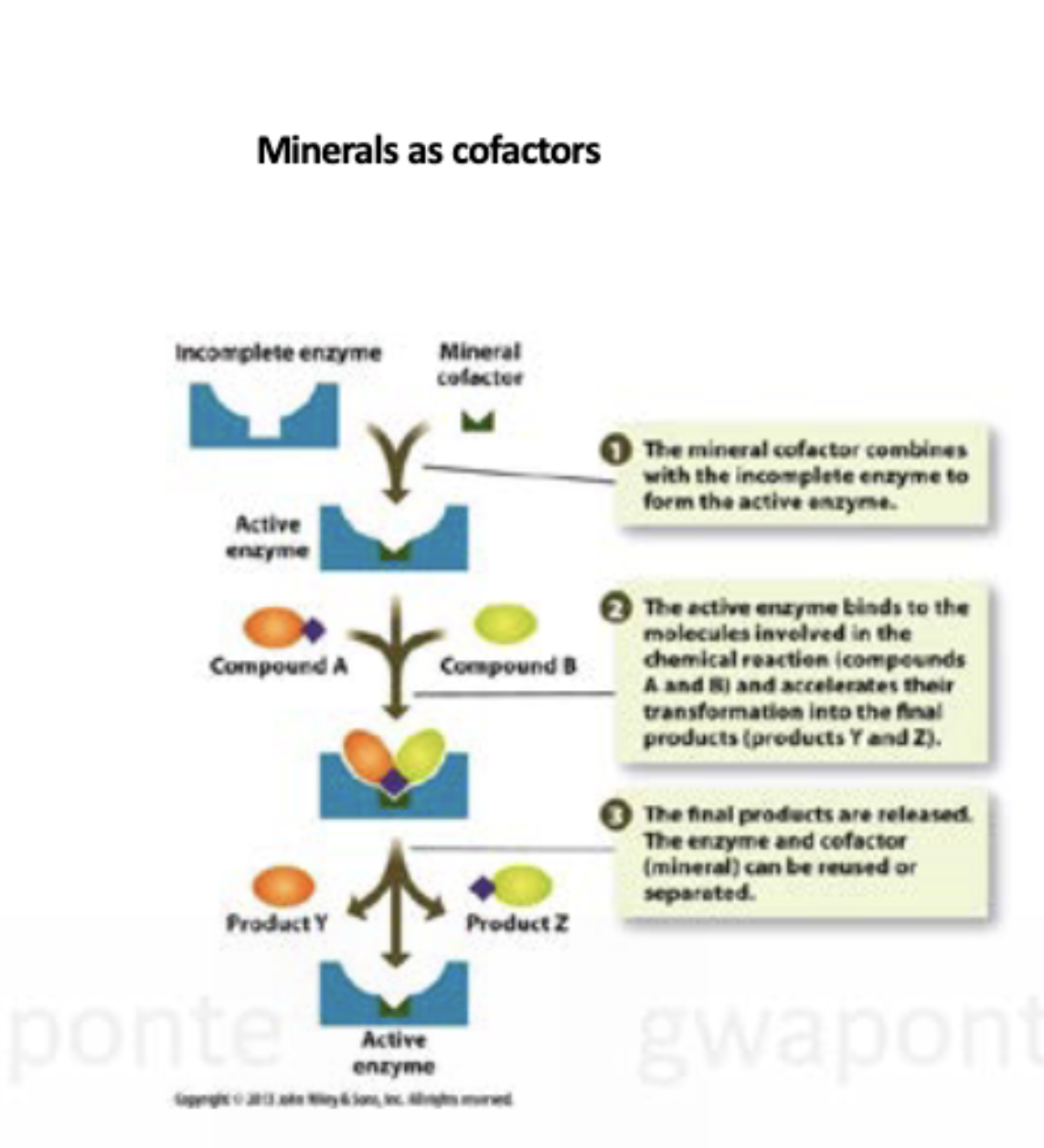
How do minerals act as cofactors?
The mineral cofactor combines with the incomplete enzyme to form the active enzyme. The active enzyme binds to the molecules involved in the chemical reaction and accelerates their transformation into the final products. The final products are released. The enzyme and cofactor can be reused or separated.
What happens when there is too little iron in the body? What about too much?
Too little iron is a reduced oxygen-carrying capacity and energy generation (women and children)
Too much iron creates free radical mediated damage, susceptibility to infection, risk of heart disease, especially in men
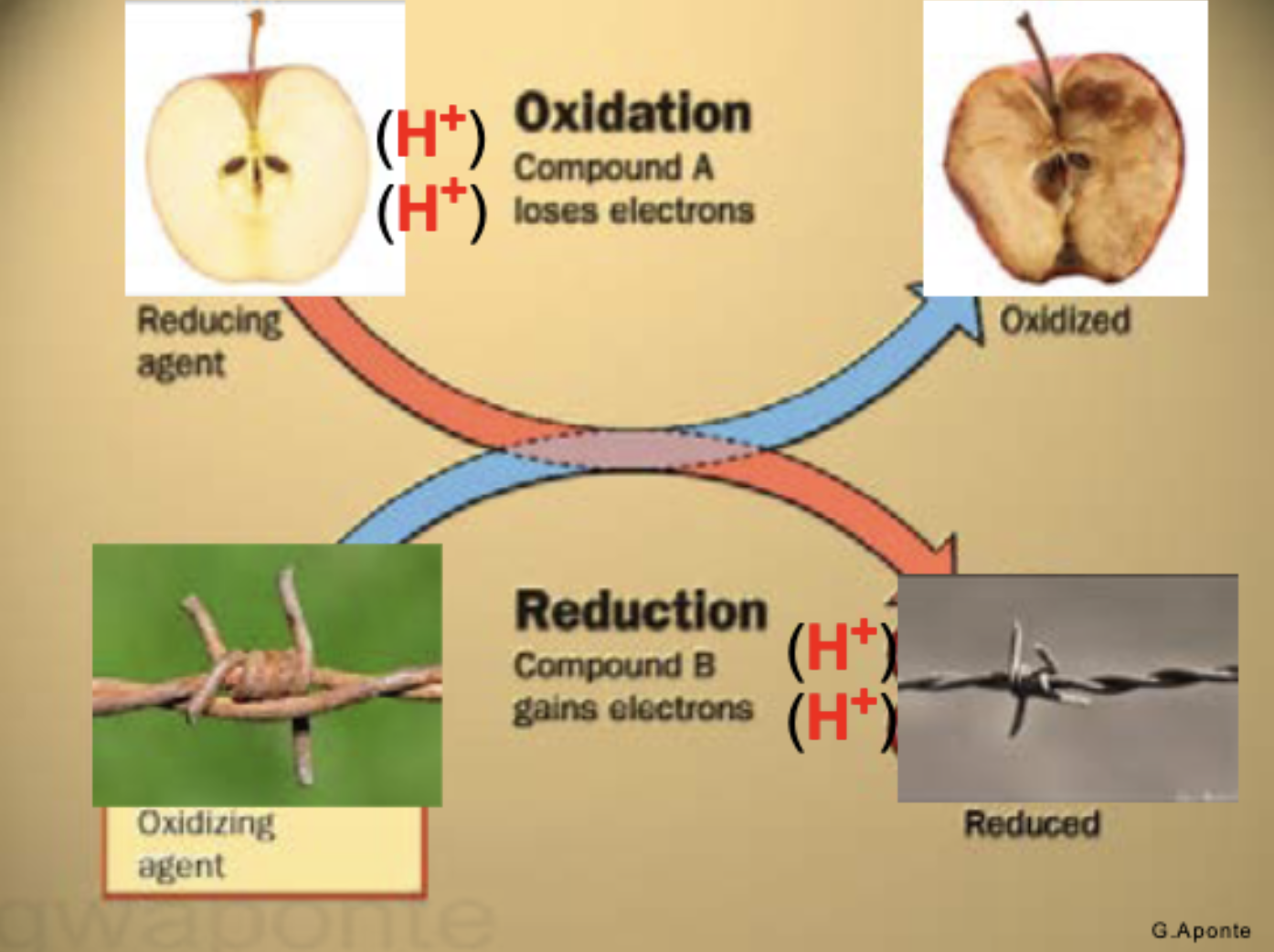
VItamin C and Iron
Oxidation - compound loses electrons
Reduction - compound B gains electrons
Functions of iron
Oxygen transport from hemoglobin and myoglobin
Enzyme cofactor (more than 200 enzyme reactions)
Immune function generates free radicals
What are the major iron-containing proteins?
Hemoglobin - carries oxygen and carbon dioxide in blood
Myoglobin - carries oxygen to muscles
Cytochromes - energy generation
Ferritin - storage for iron, excess becomes hemosiderin
Transferrin - transports iron in blood
What are the dietary iron sources?

What about non heme iron absorption? What does it do, and what food sources?
Food sources: meat, kidney beans, peas, sauerkraut, iron cooking skillets
Enhancers: need low body stores vitamin C gastric acid, meat protein factor
Mechanisms: reduces, solubilizes iron
Inhibitors: phytates, calcium, oxylates, polyphenols, antacids
Mechanism: Binds iron, forms insoluble compounds
What is iron absorption influenced by?
Body iron stores, red blood cell synthesis in bone marrow, blood hemoglobin concentration, blood oxygen content, presence of inflammatory cytokines
What happens in the pools of iron?
Storage: Ferretin found in liver, many iron atoms, measured by serum ferretin
Transports: Transferrin can bind and transport 2 iron atoms, measured by % saturation in blood,
Cellular: enzymes, transport proteins, measured by hemoglobin, hematocrit
Iron deficiency
Mild: fatigue, impaired physical work performance, congnitive & behavior abnormalities in children, body temperature regulation, decreased immune function
Severe: Anemia
Anemia
Iron deficiency results in small red blood cells that do not contain enough hemoglobin
Symptoms: fatigue, pale skin, impaired work performance, depressed immune function, impaired memory
What is Iron overload: Hemochromatosis?
Genetic disease where accumulated iron damages cells: progressive hepatic, pancreatic, cardiac, and other organ damage
Made worse with alcohol, prevalence: 1 in 13
What is copper?
Binds to ceruloplasmin in the liber for iron delivery to the tissues by oxidizing Fe2+ iron to Fe3+ iron which can then be bound to transferrin.
Copper-containing proteins are involved in iron and lipid metabolism, connective tissue synthesis, maintenance of heart muscle, immune and central nerve systems, electron transport chain
Copper
30-40% of Cu in diet is absorbed. High Zinc intake strongly inhibits Cu absorption. Cu absorption is reduced by high intake of iron, other metals, large doses of VC and antacids. Absorbed copper is bound to albumin and transported to liver.
What are the functions of zinc?
Cofactor (RNA synthesis), stabilizes proteins that regulate gene expression, functions in 300 enzymes for growth, protein synthesis, sexual maturation, stabilizes cell membranes
What happens to zinc in the digestive tract?
Absorption regulated by zinc transport proteins. Amount of zinc that enter the blood is regulated by metallothionein
What happens when zinc is incorporated into intestinal metallothionein?
If the body does not need zinc, zinc sloughed off with intestinal cells
When body needs zinc, zinc is transported into bloodstream
What is iodide?
Iodine is present in food as iodide. Thyroid gland requires iodide for thyroxin synthesis. Thyroid metabolism requires: iron, selenium, zinc
What is thyroxin
T4: inactive, T3: active. T3 increases BMR
Affects mood, metabolic rate through thermogenesis, lipid homeostasis, cardic acceleration & output, growth development bone growth & turnover
What are the disorders of thyroid glands?
Hyperthyroid — irritability, nervousness, muscle weakness, tremors, sleep disturbances, impaired fertility, rapid heartbeat, heat sensitivity
Hypothyroid — Fatigue, tire easily, forgetfulness, weight gain, depression, mood swings, dry coarse skin & hair, hoarse voice, intolerance to cold
Food sources of iodide
iodized salt, seafood, plant sources are dependent on soil content. Goitrogens inhibit iodide metabolism: present in cassava, millet, raw turnips, cabbage, brussels sprouts
Summary of trace elements Iron
Sources: red meats, leafy greens, dried fruits, whole and enriched grains
Intake 8-18 mg/d
Major functions: part of hemoglobin, delivers oxygen to cells, myoglobin, holds oxygen in muscle, and electron carriers in the electron transport chain; needed for immune function
Deficiency: iron deficiency anemia: fatigue, weakness, small pale red blood cells, low hemoglobin
Groups at risk: infants and preschool children, adolescents, women of childbearing age, pregnant women, athletes
Toxicity: gastrointestinal upset, liver damage
UL: 45 mg/d
Summary of trace elements Zinc
Sources: meat seafood, whole grains, eggs
Intake 8-11 mg/d
Major functions: regulates protein synthesis, functions in growth, development, wound healing, immunity, and antioxidant protection
Deficiency: poor growth and development, skin rashes, decreased immune function
Groups at risk: vegetarian, low-income children, elderly
Toxicity: decreased copper absorption, depressed immune function
UL: 40 mg/d
Summary of trace elements Copper
Sources: Organ meats, nuts, seeds, whole grains, seafood, cocoa
Intake 900 ug/d
Major functions: a part of proteins needed for iron absorption, lipid metabolism, collagen synthesis, nerve and immune function, and antioxidant protection
Deficiency: anemia, poor growth, bone abnormalities
Groups at risk: those who oversupplement zinc
Toxicity: vomiting
UL: 10 mg/d
Summary of trace elements Iodine
Sources: iodized salt, salt water fish, seafood, dairy products
Intake 150 ug/d
Major functions: needed for synthesis of thyroid hormones
Deficiency: golter, cretinism, mental retardation, growth and developmental abnormalities
Groups at risk: populations in areas with low-iodine soil and iodized salt is not used
Toxicity: enlarged thyroid
UL: 1110 ug/d
What is a healthful body weight?
A weight that is appropriate for your age and physical development.
A weight that you can achieve and sustain without severely curtailing your food intake or constantly dieting.
A weight that is based on your genetic background and family history of body shape and weight
A weight that is compatible with normal blood pressure, lipid levels, and glucose tolerance.
A weight that promotes good eating habits and allows you to participate in regular physical activity
A weight that achieves good fitness
Dieting college and high school students with semi-starvation
Normal dieting may be more closely related to psychological and health risks associated with chronic semi-starvation than has commonly believed.
High-fat, low-carbohydrate, high-protein diets
Types of diets contain about 55% to 65% of total energy intake as fat, less than 100g of carbohydrate per day, with the balance of dialy energy intake as protein.
Low-fat and very low-fat diets
Diets contain 11% to 19% of total energy as fat, whereas very low-fat contain less than 10% of total energy as fat.
Moderate-fat, high-carbohydrate, moderate-protein diets
Moderate- fat, high-carbohydrate, moderate-protein diets that are balanced in nutrients typically contain 20% to 30% of total energy intake as fat, 55% to 60% of total energy intake as carbohydrate, and 15% to 20% of energy intake as protein
Genetic factors that affect body weight: thrifty gene theory
Thrifty gene theory suggests that come people posses a gene that causes them to be energetically thrifty. This means that a rest and even during active times, these individuals expend less energy than people who do not posses this gene.
Set-Point theory
Suggests that the body is designed to maintain weight within a narrow range, or “set point”. In many cases, the body appears to respond in such a way as to maintain a person’s current weight
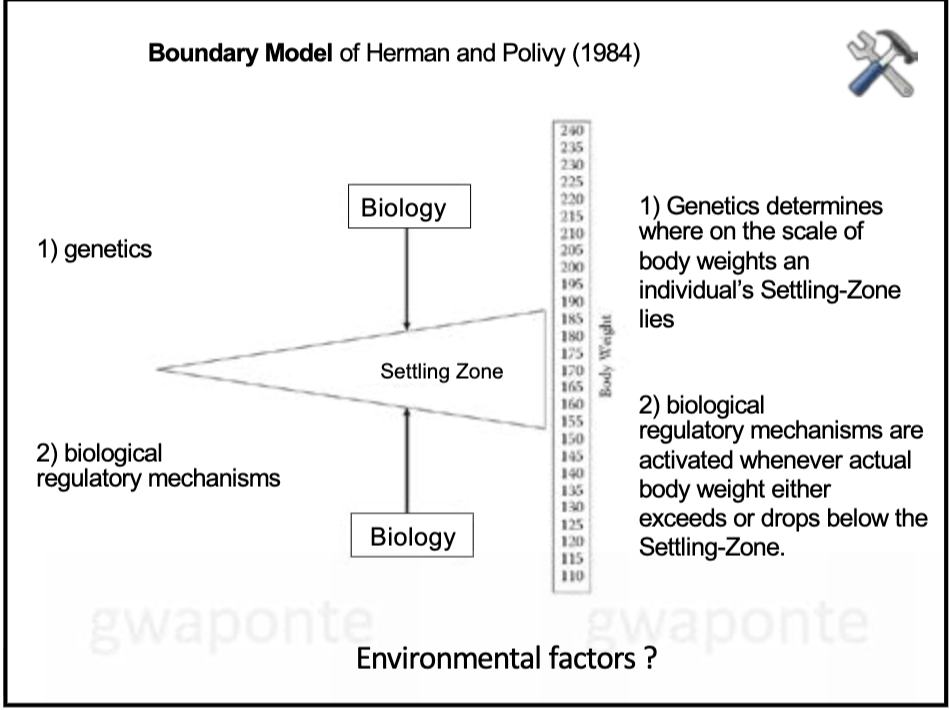
Boundary Model
Genetics determines where on scale of body weights an individual’s setting zone lies
Biological regulatory mechanisms are activated whenever actual body weight either exceeds or drops below the settline-zone
What accounts for the rise in obesity?
Overeating eating more meals outside with increase in serving, fat, calories, salt less fruits and vegetables
Increase in sugary drinks
Physical activity
Processed foods
Behavior
How do you examine body weight? What is a healthy body weight
Body weight: bone, muscle, fat, tissue, fluid, blood
A healthy body weight is adequate lean and fat tissues, promotes good eating habits and allows for regular physical activity, a weight associated with reduced disease risk, obesity is associated with diabetes, high blood pressure, heart diease