KIN 240 Midterm 1
1/95
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
96 Terms
what are some stakeholders from the medical rtp?
sports physician
physical therapist
soft tissue specialist
athletic trainier
what are some stakeholders from the perfomance rtp?
s&c coach
nutrition
psychologist
sport scientist and coach
what is a certified exercise physiologist
involved in exercise testing and screening
works with gen pop, high perfomance athletes, chronic health conditions, functional limitrations or disabilities
what is a certified personal trainer
does pre-participation health screening
sub-maximal fitness assessments
works with health individuals between 15-69
what are sport medicine physicians
under the canadian academy of sport exercise medicine
not the same as a family med doc
they specialize in skills related to medical conditions
completeted further personal training in sport med fellowship or additional unit degree
what is a sport physiotherapist
A physiotherapist with additional certification focused on sport-related care
has written and practical certificates (or diploma)
similar scope of practice to athletic therapist
what is a certified athletic therapist
narrow scope
specalizes in msk injury, recognition, management, treatment and rtp
what are a sports therapist area of expertise
prevention
immediate care
clinical assessment
treatment, rehab, reconditioning
what is prevention in injury care and management?
ensuring the protective gear works
conditioning
screening and assessment to recognize and observe abnormal movement patterns
what is immediate caare in injury care and management?
acute injury recognition and management
emergency interventions and EAP
on and off field evaluation skills
what is clinical assesment in injury care and management?
understanding pathology of injuries and illnesses
coordination with other medical practitioners
what is treatment, rehab and reconditioning in injury care and management
developing theraping skills via education and workshops
exercised based treatment and rehab
knowing exercise physiology
identifying key performance indicators to guide an athletes rtp
what are the steps to build an IST from scratch?
identify needs and limitations
identify who you want to work with
build relationships with other professionals
what are the components of a sport-related concussion (SRC)?
traumatic brain injury
caused by a blow to the head, neck or body
force is transmitted to the brain and may trigger neurological and metabolic changes
symptoms either immediate or delayed
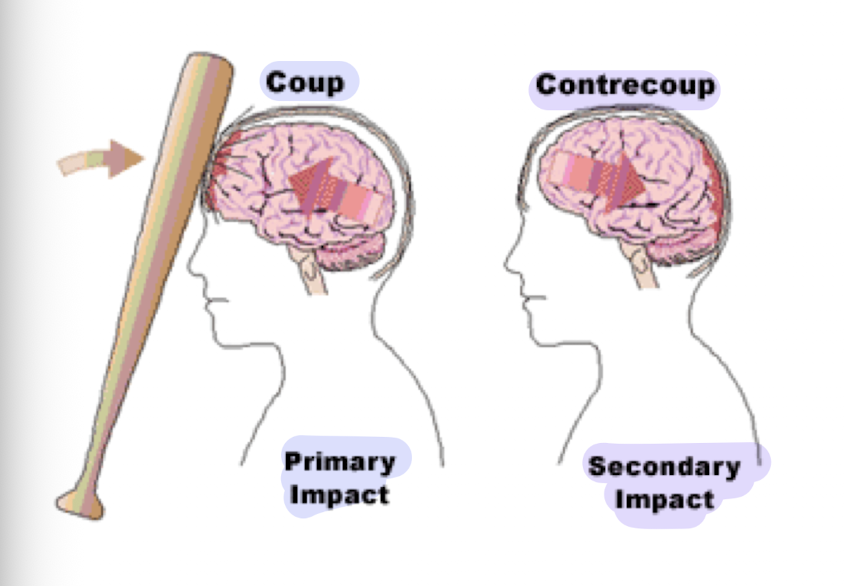
What is contrecoup?
athlete colliding with an opponent/object/surface that imparts a forc eon their body
creates an impulsive force upon the brain
forces can also lead to tension and compression tissue injury
common in sport collisions
what are the “R”’s of SRC?
recgonize
reduce
remove
refer
retern to learning/sport
what are the 4 domains of SRC symptoms?
migraine (physical)
neuropsychiatric
sleep
cognitive
how do you reduce potential of SRC in hockey?
mouthguard reduces by 28% across all ages
what are some key steps in field evaluation of a concussion?
evaluate onsite (emergency principles)
rule out cervical spine injury
stay with the athlete
monitor for deterioration
what types of sideline assessment tools exist?
SCAT6
app-based tools
subjective assessment (like where the athlete reports symptoms)
when you do a neurophysical assesment?
done after the symptoms resolve
most sensitive when compared to baseline
aids in RTP decisions
whats the best first step in concussion management?
recognize symptoms and remove activity
refer to a healthcare practitioner
what are the 3 steps to return to learning
do daily activities that do not result in more than mild exacerbation of symptoms
do school activities; homework, reading
return to school part time - half day at school, breaks during school
return to school full time
athlete shouldnt go back to sports until they are back to school w/o symptoms getting worse
what is step 1 in returning to sport?
symptom limited activity
daily activities that don’t provoke symptoms and not specific
want to have a gradual integration of cognitively stimulating activity
what is step 2 in returning to sport?
aerobic activity
controlled activities that don’t put the athlete at risk and they are not sport specific
2A: light, lower than 55% maxHR
2B: mod, 70% maxHR
activities such as stationary cycling (preferred), treadmill walking
what is step 3 in returning to sport?
sport specific exercise
no activity where risk of head impact or contact exists and removed from team enviornment
do sport specific skills that are isolated and cognitively challenging
ex: juggling, passing, throwing, catching
what needs to be done before transitioning into stage 4-6 when managing return to sport
symptom free with no aggravation of symptoms
presence of symptoms with 4-6 tasks means athlete should return to stage 3 until symptoms resolve
what is stage 4 in returning to sport?
non-contact training drills
high intensity drills and activities and return to usual resistance training
technical and tactical drills that involve interacting with teammates and requires rt/decision making
what is stage 5 of returning to sport?
full contact practice in controlled situations (should be cleared by a HCP)
introduce sport specific contact and restore confidence through exposure
what is stage 6 of returning to sport?
return to sport
completed stage 5 with no hesitancy and has full confident in abilities and health
can return due to enough conditioning
the first game may bring on symptoms again but to pass this stage, no symptoms should arise post game
why is baseline testing for SRC not as affective in children compared to adults
they are constantly growing their neurocognitive abilities
what are some symptoms athletes may experience when theres an injury to the skull or brain?
loss of consciousness
disorientation or amnesia
motor deficits
cognitive deficits
what is a cerebral contusion/hematoma?
small hemorrhages or intracerebral bleeding within the cortex, brain stem or cerebellum
may occur when the head strikes a stationary object at high velocity or force
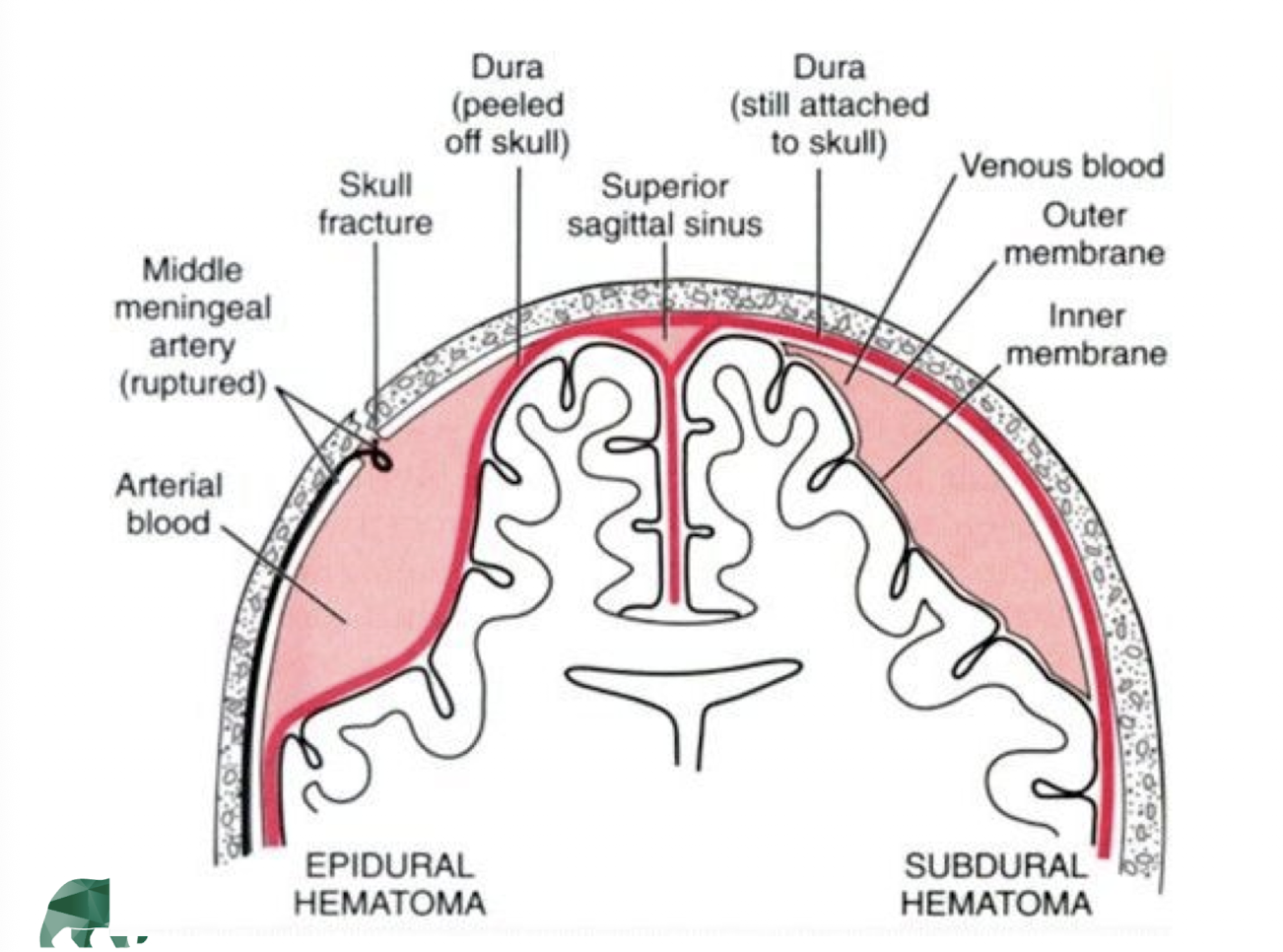
what are some signs and symptoms of a cerebral contusion/hematoma?
may experience immediate loss of consciousness or severely altered consciousness
dilation of one pupil, depression of pulse and respiration
how do you manage a cerebral contusion/hematoma?
recognize severity of symptoms
activate EAP
requires ongoing medical management, extended rehab and RTP process
what is a scalp/upper face laceration? whats a key symptom?
blunt trauma or penetrating trauma tends to be the cause
may occur with a serious head trauma
bleeding is often extensive
how do you manage a scalp/upper face laceration?
first aid
wound bigger than 1/8 in depth - referral to a physican
smaller wounds, covered with a protective covering and gauze
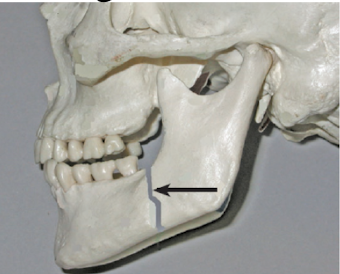
whats a mandible fracture and some of its signs and symptoms?
direct blow to the jaw (fractures near the front angle)
s&s nclude deformity, loss of occlusion of teeth, bleeding around the teeth and lower lip anesthesia
how do u manage a mandible fracture?
immobilize and refer to urgent care
what is a mandibular subluxation or dislocation?
involves injury to the temporomandibular joint (TMJ)
MOI is a blow to the open mouth from the side
what are the signs and symptoms of a mandibular subluxation/dislocation?
subluxed: a decrease in ROM, pain at end ranges, isolated pain to TMJ and surrounding musculature
dislocated: locked-open position, easily noted by misaligned teeth
how do u manage a mandibular subluxation/dislocation
manage acute symptoms and stabilize if needed
Refer for medical management
May be physician, could also be trained MSK therapist
what is a nasl fracture? and is its signs and symptoms?
a direct blow to the nose
there is hemmorrhaging and possible deformity
also check for a src
how do u manage a nasal fractute?
check for src
control bleeding and if needed refer for an x-ray
heel smash method
what is a tooth fracture and its s&s?
impact to the jaw or direct truama
s&s include fractures with framents, bleeding if complicated, possible x-ay needed
how do u manage a tooth fracture?
uncomplicated crown fractures do not require immediate attention
root fractures: refer to a dentist asap
what are some things to consider when assesing the eye?
use extreme caution
eyes should be covered together
movement of unaffected eye will cause movement in affected eye
what are signs and symptoms of foregin bodies in the eye?
foreign objects causing lots of pain and disability
do not rub eye to try and remove or recover with fingers
how do u manage foreign bodies in the eye?
close eye and determine location; either upper or lower lid
wash eye with saline and rinse with affected eye at bottom
if object is embedded, close and patch both eyes and refer to a physician
whats a corneal abrasion or laceration and its s&s?
direct contact to eye with a sharp object (ex; fingernail)
there may be severe pain and watering of the eye
how do u manage a corenal abrasion or laceration?
patch both eyes and refer to a physician
what is a hyphema and its s&s?
blunt blow to the eye
causes collection of blood in anterior chamber of eye
vision is partially or completely blocked
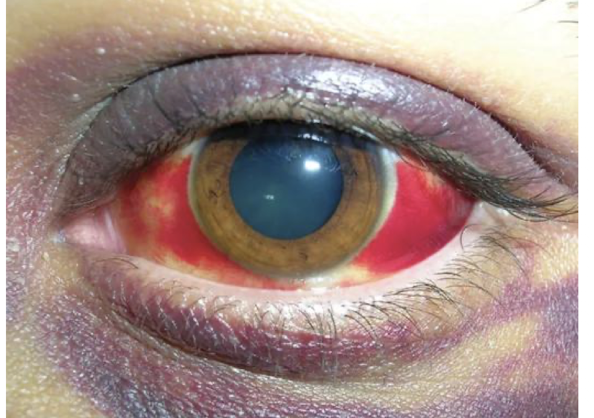
how do u manage hyphema?
patch both eyes and refer to a physician
what is acute conjunctivits?
pink eye
cause by bacteria or allergens
conjuctival irritation causd by wind, dust, smoke, air pollution
aso caused by a cold or upper resp conds
what ate s&s of acute conjunctivitis and how do u manage it?
eyelid is swelling with discharge and itching
highly infectious; stay home and contain
how do u strengthen the cervical spine?
muscle strengthening to resit hyperflexion, extension and rotational forces
athlete should brace neck (double chin) prior to impact
isometric exercise to strengthen or sport specific exercise
how do prevent injury at the thoracic spine?
correct posture and avail rom (flexion and extension)
functional strength and biomechanics
how do u prevent injury at the lumbar spine?
avoid unnecessary stresses and strains of daily living and positions/posturs that causes injury
correct asymmetries or deficiences
conditioning to emphasize trunk flexibility
strengthen spinal extensor and abdnominal musculature
what is the mcgill big three
core exercise that strengthen and support the lumbar spine
creating an unstable base to build strength around the lumbar spine
what is lordosis?
anterior tilt of the pelvis
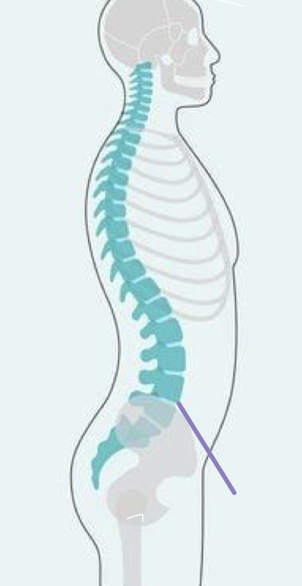
what is kyphosis
rounded thoracic
head tilt forward significantly and can cause pain
how should u asses the cervical spine?
assess position of the head and neck
symmetry of shoulders
assess rom
What symptoms indicate facet joint involvement in the thoracic spine?
Unwilling to rotate or side flex
Pinpoint pain with movement
What symptom suggests costal-vertebral involvement in the thoracic spine?
Pinpoint pain with deep inhalation
what are some things to remember when observing the lumbar spine and sacroiliac joint?
coordinated movement of the lower back involves the pelvis, lumbar spine and sacrum
equal levels in the shoulders and hips (illiums)
what are some things to remember when palpating the lumbar spine and sacroiliac joint?
palpate over spinous processes; any sharp pain is a red flag
palpate over transverse process; rib articulations
what is a cervical fracture?
axial load through top of the head with a flexed spine
other neck positions can result in varying forms of structural damage
how do you manage a cervical fracture?
stablize the patients neck/spine regardless of level of consciousness
use extreme care and caution
know scope
what are acute strains of the neck/upper back? what are the signs and symptoms?
results in an unexpected movement of the head
may involve traps, scm, scalenes, levator scapulae
s&s involves localized pain, point tenderness and restricted ROM
must rule our csp invovement when on field
how do u manage an acute strains of the neck/upper back?
immobilization
refer to sports med phys with x-rays, pain management, nerve involvement
what is a brachial plexus neurapraxia? (burner)
stretching/compression of brachial plexus
disrupts peripheral nerve function
common in contact sports
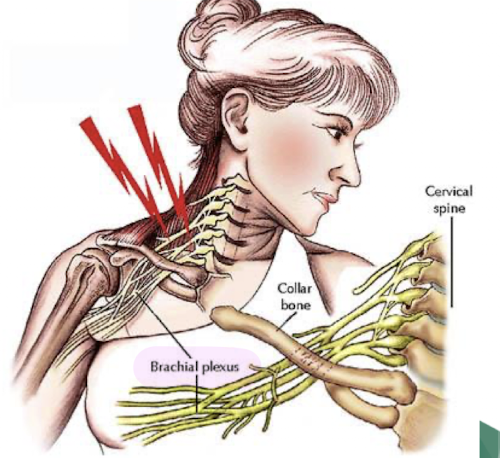
what are the signs and symptoms of a burner?
burning sensation, numbness and tingling
may include pain extending from shoulder into hand
severity injury will influence duration of return
how do u manage a burner?
return to activity once s&s resolve
also once able to achieve pre-injury strength and sensation
what is acute torticollis? (wryneck)? what is its signs and symptoms
pain on one side of the neck upon wakening
result of a synovial capsule impingement within a facet
s&s include palpable point tenderness and muscle spasm, restricted rom and muscle guarding
how do you manage wryneck
traction (pulling, seperation b/w vertabrae)
superficial heat
soft tissue treatments
what is low back pain?
poor mechanics during loaded/unloaded tasks
back trauma
muscle imbalances
repetitive patterns
what are the signs and symptoms of low back pain?
pain
general weakness, antalgic gait
what is spondylosis
generation of the vertebrae due to congenital weakness
aka stress fraacture
happens on on side of vertebrae
what is spondylolistheis?
development of sppondylosis to both sides of the verebrae
slipping of one verebrae above or below anohe
what are the signs and symptoms of spondylolysis and listhesis
spondylolysis begins unilaterally
pain and persistent aching
low back stiffness with increased pain after activity
frequent need to change position
segmental hypermobility
how do u manage spondylolysis and listhesis?
acute symptom management
exerises directed at controlling/stabalizing hypermobile segements
trunk strengthening
dynamic core strengthening
abdominal work
what is SI joint dysfunction
truamatic causing an upshift of one illium
irrirtation and stretching of sacrotuberous or sacrospinous ligaments
what are some of the signs and symptoms with SI joint dysfunction?
palpable pain and tenderness over the joint medial to PSIS (w/ muscle guarding)
pelivc asymmetries
pain may radiate posteriorly, laterally or anterioly down the thigh
sitting is comfy but you experience pain when first getting up/extending through SI joint
what ate the 3 forces causing injury to tissue?
compression
tension
shearing
what are the forces causing injury to long bones?
bending
torsion
what is a compression force?
a force with enough energy to crush tissues
can be from 1 blow or repeated submaximal blows = damage in tissue (or even a fracture in bone)
what is a tension force?
pulling force which stresses tissue beyond yield point
results in sprain, strain or avulsion type injury
what is a shearing force?
a force moving paralell across the tissue
what is a bending force?
bone bending occurring under axial load (2 point contact)
external force going opposite of other 2 points of load
what is a torsion force?
loads caused by twisting of the bone in oppsite directions from opposite ends
rotation force
could cause spiral fracture
what is a life-threatneing injury?
places athlete at immediate risk of their health, wellbeing, life
what is a serious injury?
a debilitating injury that has significant implications on the ability of an athlete to continue participating in sport
may impact adl
may require surgery or rehab
whats a non-life threatning or non-seriosu injury
majoirty of sports injuries fall in this category
wide variety of debilittation, time loss and rehab needed
what is an acute injury?
immediate onset, injury occuring after MOI
athlete may not report pain right away
accompanied with signs of SHARP (swelling, heat, altered function, redness, pain)
requires immediate intervention
what is a chronic injury?
a number of small acute events or micro-traumas
may not be able to identify source and could be caused by a numerous factors
what are the 3 key roles in an EAP?
charge person
call person
control person