BIO202 Unit 6/Lab 9 Urinary System
1/60
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
61 Terms
Kidney - renal cortex
outer region of the kidney
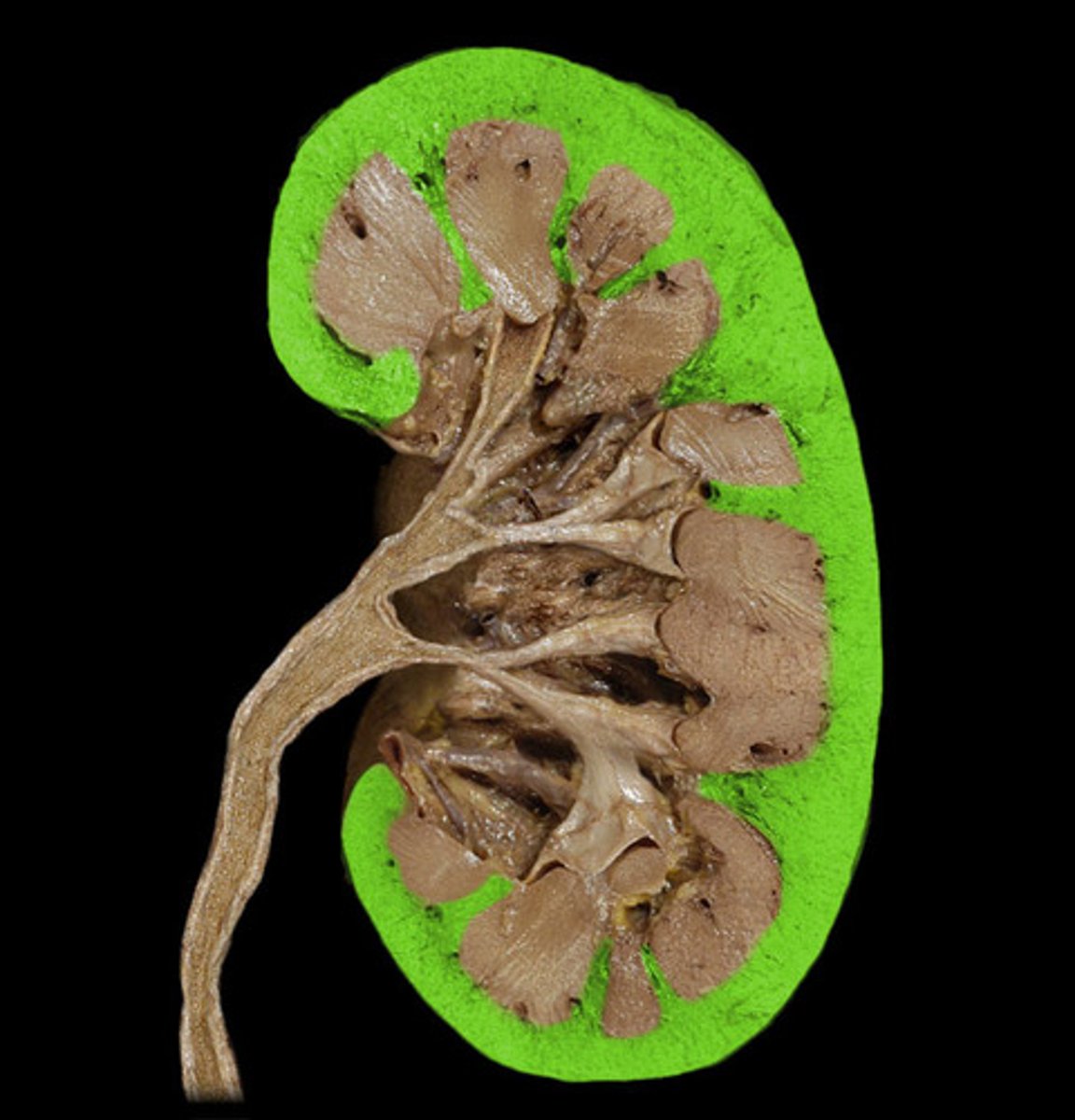
Kidney - renal medulla
middle area of the kidney
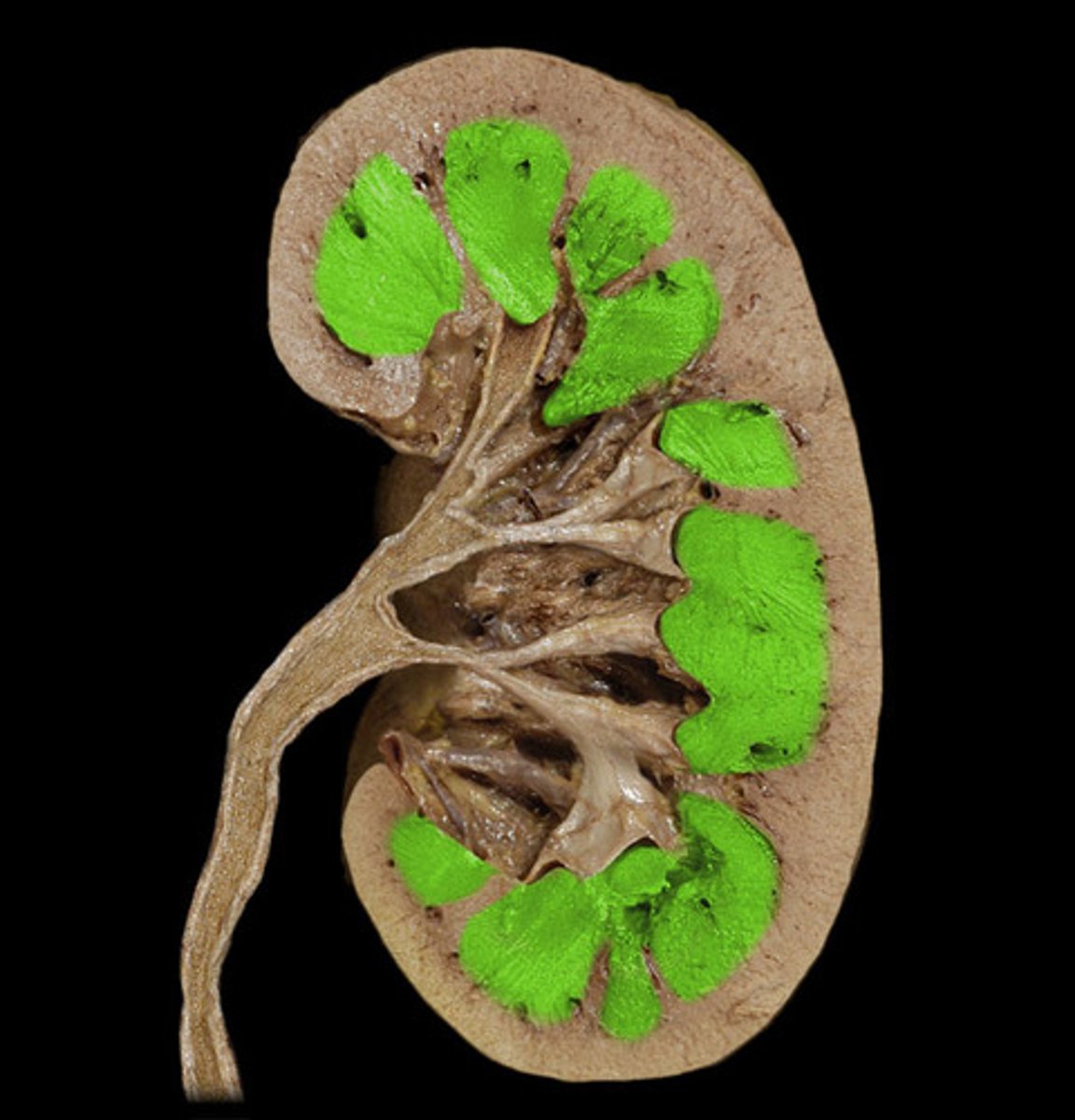
Kidney - renal pelvis
the funnel-like dilated part of the ureter in the kidney
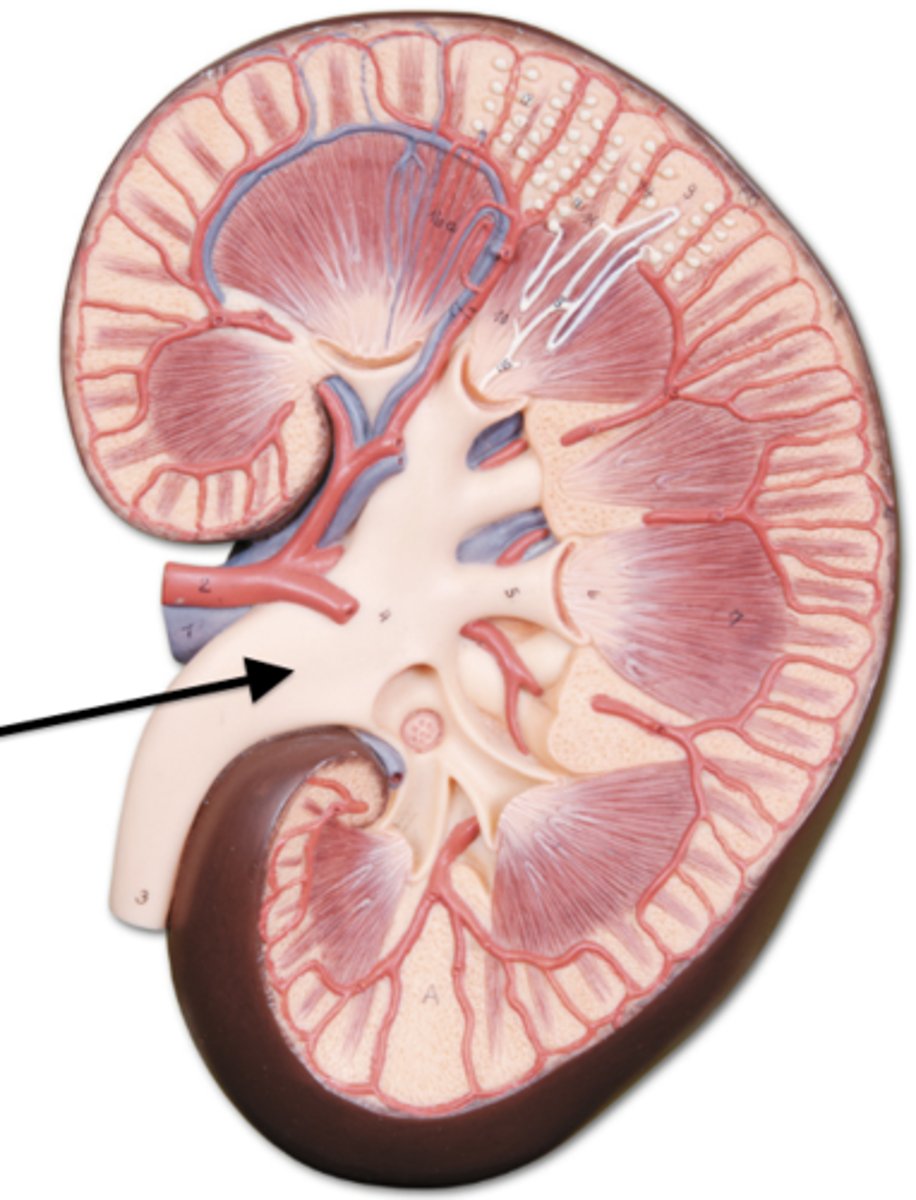
Renal
pertaining to the kidney
Renal artery
carries blood from the aorta into the kidney
Nephron
functional unit of the kidney that filters the blood & forms urine
Functions of the Kidneys
Main = filter wastes from blood. Also:
make urine,
convert vitamin D to active form,
metabolic waste disposal,
blood volume regulation.
Urinary Bladder - daily urine volume production
1.5 liters
Urinary bladder capacity
-a moderately full bladder is about 5 inches long and holds about 500 ml of urine
-Capable of holding twice that amount of urine
Urinary bladder - tissue type found in the walls
Transitional Epithelium
Ureters
The tubes that carry urine from the kidneys to the bladder.
Urethra
tube leading from the urinary bladder to the outside of the body
Urethra - length
Females: 3-4 cm
Males: 20 cm
Urethra - female
Carries urine out of the body
Urethra - male
Serves as the passage way for sperm and fluids from the reproductive system and urine from the urinary system. While the reproductive fluids are passing through the urethra, sphincter contract tightly to keep urine from entering the urethra.
renal ptosis
condition in which one or both kidneys drop to a lower position
-Can be caused by loss of surrounding fatty tissue capsule that holds kidneys in normal position
pyelonephritis
•Infection or inflammation of entire kidney
anuria
abnormally low urinary output (less than 50 ml/day)
nocturia
frequent urination at night
antidiuretic hormone (ADH)
•Causes principal cells of collecting ducts to insert aquaporins in apical membranes increasing water reabsorption
•As ADH levels increase -> increased water reabsorption
aquaporins
channel proteins that facilitate the passage of water
myogenic mechanism
general tendency of vascular muscle tissue to contract when stretched
pyuria
presence of white cells (pus) in the urine, usually indicating infection
Glomerulus filtration - how does it work?
The glomerular capillaries are fenestrated, allowing fairly large molecules to pass through
fenestrated
having openings
Glomerulus
A ball of capillaries surrounded by Bowman's capsule in the nephron and serving as the site of filtration in the vertebrate kidney.
urethritis
inflammation of the urethra
Internal Urethral Sphincter
smooth muscle, involuntary
External Urethral Sphincter
skeletal muscle, voluntary
micturition
another term for urination
Percentage of filtrate eventually reabsorbed back into the blood from the kidneys?
99%
Filtrate
fluid that passes from the blood through the capillary walls of the glomeruli of the kidney
Filtrate composition
-blood plasma (including water, glucose, electrolytes, ions & urea)
-minus blood proteins
In children, how does the nervous system relate to control of the urinary system?
•Incontinence normal in infants: control of voluntary urethral sphincter develops with nervous system
diuretic
agent that increases urine output
diuretics - examples
•ADH inhibitors, e.g., alcohol
•Na+ reabsorption inhibitors (and resultant H2O reabsorption), e.g., caffeine, drugs for hypertension or edema
•Loop diuretics inhibit medullary gradient formation
•Osmotic diuretics - substance not reabsorbed so water remains in urine, e.g., high glucose of diabetic patient
Urine - odor
•Slightly aromatic when fresh
•Develops ammonia odor upon standing as bacteria metabolize solutes
•May be altered by some drugs and vegetables
abnormal urine constituents
glucose (glycosuria),
proteins,
ketone bodies,
hemoglobin,
bile pigments,
erythrocytes (hematuria),
leukocytes (pyuria)
normal urine constituents
Water, urea, creatinine, electrolytes.
Glycosuria
glucose in urine
hematuria
RBCs (erythrocytes) in urine
renal calculi
-Kidney stones in the renal pelvis;
-crystallized calcium, magnesium, or uric acid salts
renal calculi - treatment
-First, pain management with NSAIDs and Narcotics, IV fluids for hydration
-Lithotripsy - non-invasive use of shockwaves to break stones so they can be passed
urinary tract infection (UTI)
invasion of pathogenic organisms (commonly E. coli bacteria) in the urinary tract, especially the urethra and bladder; symptoms include dysuria, urinary frequency, fever, chills and malaise, possible back pain
UTI - common causes in females
•Improper toilet habits, such as wiping back to front after defecation
•Most UTIs occur in sexually active women - Intercourse drives bacteria from vagina and external genital region toward bladder
dysuria
painful urination
incontinence
inability to control urination
stress incontinence
-the inability to control the voiding of urine under physical stress such as running, sneezing, laughing, or coughing
-common after childbirth (vaginal delivery) which can weaken the pelvic floor muscles & urinary sphincter
Acidosis & Alkalosis similarities
-both involve disruption of normal body pH balance
-if left untreated, both result in death
cystitis
inflammation of the urinary bladder
often caused by a urinary tract infection (UTI) and can be treated with antibiotics. Other causes include chemicals, radiation, and interstitial cystitis, and treatment options vary depending on the underlying cause.
respiratory alkalosis
A rise in blood pH due to hyperventilation (excessive breathing) and a resulting decrease in CO2.
-corrected by the kidneys
respiratory acidosis
A drop in blood pH due to hypoventilation (too little breathing) and a resulting accumulation of Co2.
-corrected by the kidneys
metabolic acidosis
decreased pH in blood and body tissues as a result of an upset in metabolism
-compensated by an increase in ventilation to decrease blood CO2 & kidneys
metabolic alkalosis
elevation of HCO3- usually caused by an excessive loss of metabolic acids
-compensated by decrease in ventilation to increase blood CO2 & kidneys
acidosis pH
below 7.35
alkalosis pH
greater than 7.45
Alcoholism and metabolic acidosis
Alcoholism can lead to metabolic acidosis, specifically alcoholic ketoacidosis (AKA), a condition characterized by high ketone levels and an elevated anion gap, often occurring after binge drinking and poor nutrition
Hypertonic blood & relation to ADH
In response to hypertonic blood, the body releases antidiuretic hormone (ADH) to increase water reabsorption in the kidneys, thus diluting the blood and restoring osmolarity.
hypoventilate
shallow, inadequate breathing
hyperventilate
excessively rapid and deep breathing
dialysis
Process for removing waste from the blood for people with renal failure