Gero Exam 2 Study Guide (Spring 2026)
1/55
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
56 Terms
Impaired Sensation
Condition where a person has a decreased, absent, or altered ability to receive, process
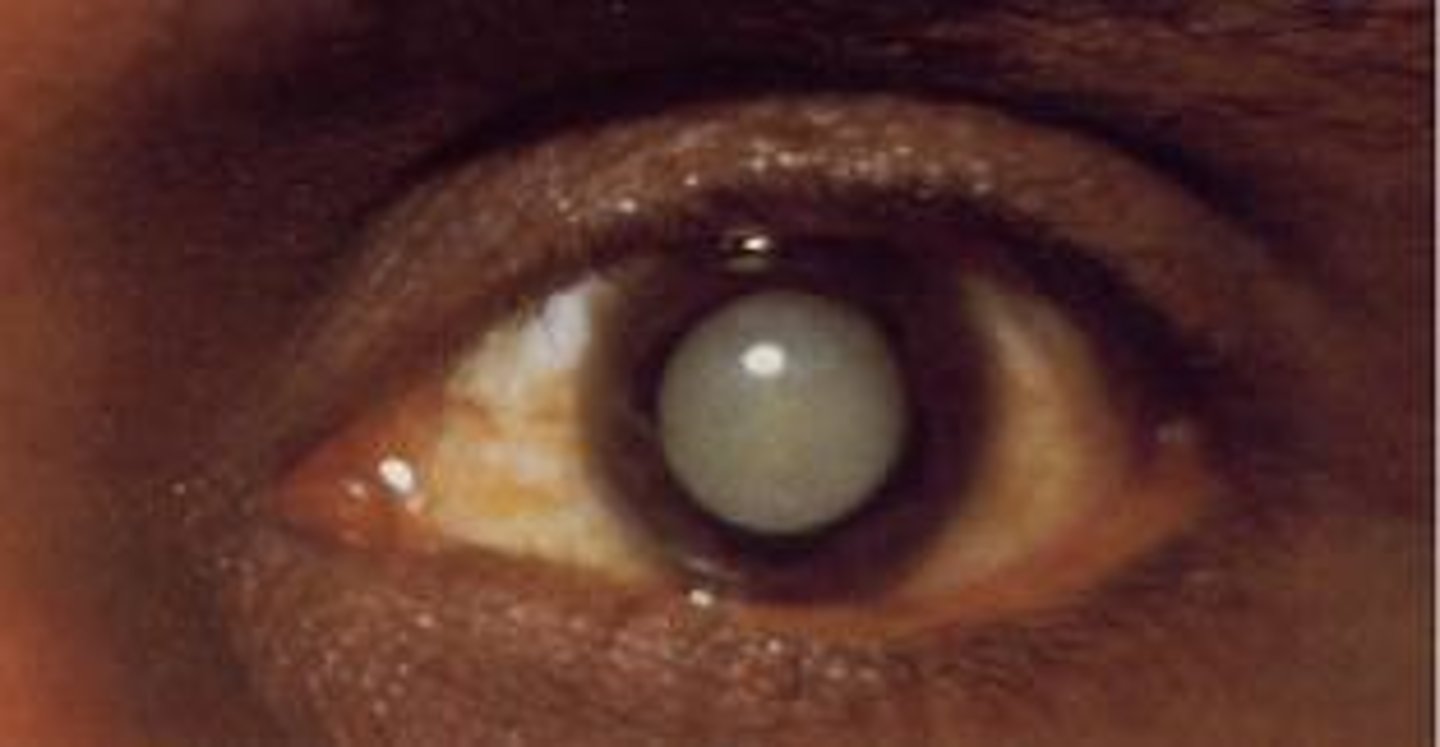
Cataracts
Common, age-related clouding of the eye's natural lens that blocks light, causing blurry vision, faded colors, and glare
Tinnitus
Perception of sound in one or both ears or in the head when no external sound is present. It's often referred to as "ringing in the ears" but can manifest as buzzing, whistling, hissing, crickets, chirping, bells, pulsating, and swishing sounds. The sounds may be constant or intermittent and are more acutely at night or in quiet surroundings.
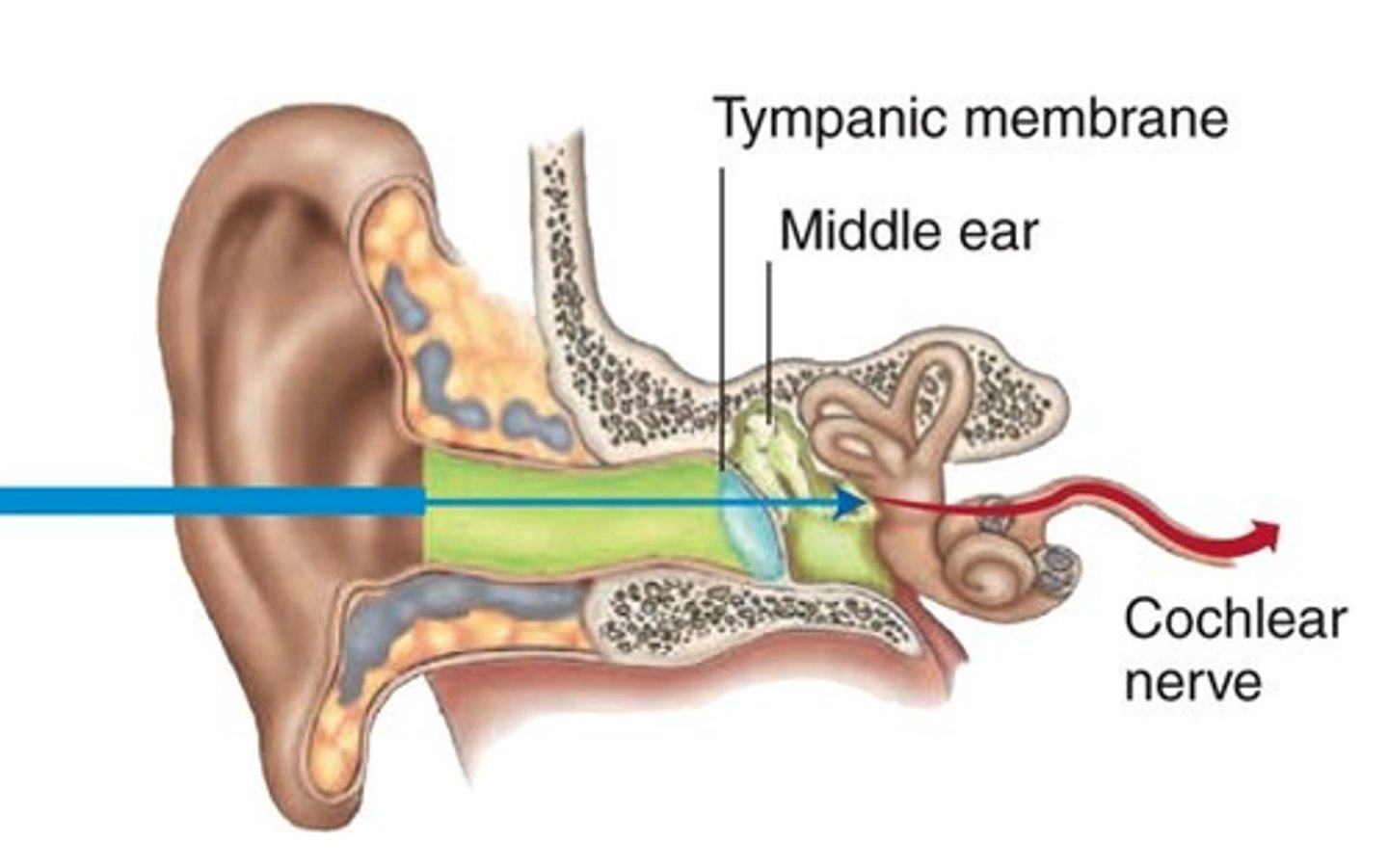
Presbycusis
Gradual, age-related, bilateral sensorineural hearing loss affecting high-pitched sounds, impacting 1 in 3 adults aged 65-74. Caused by inner ear hair cell damage, it leads to difficulty understanding speech in noisy environments.

Impacted Cerumen
Accumulation and hardening of earwax that blocks the ear canal, causing symptoms like earaches, temporary hearing loss, tinnitus, and a feeling of fullness.
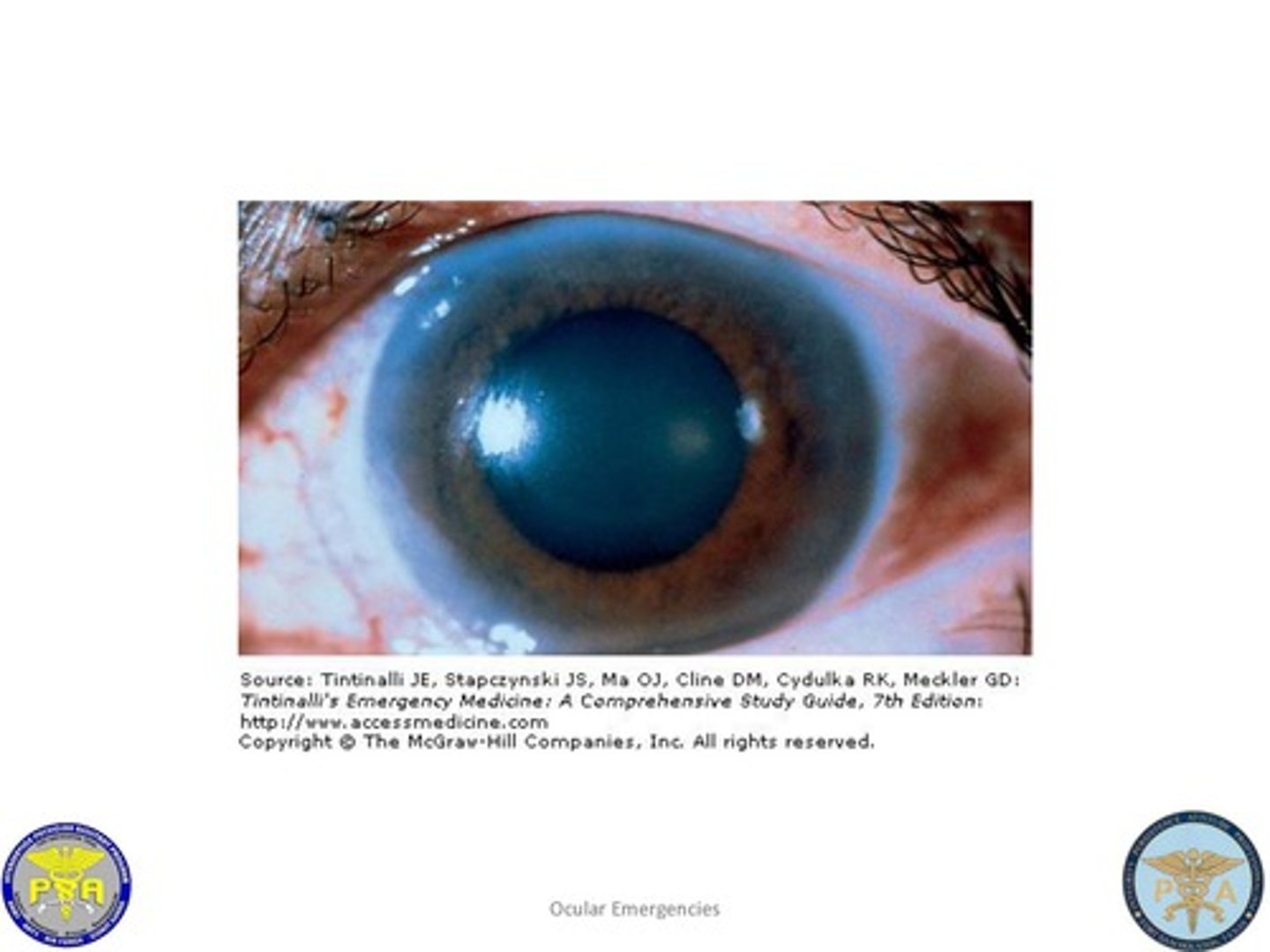
Glaucoma
increased intraocular pressure results in damage to the retina and optic nerve with loss of vision
Macular Degeneration
A progressive eye disease and leading cause of vision loss in people over 60, damaging the macula to blur central vision. It has two main forms: common "dry" (gradual breakdown) and severe "wet" (leaking blood vessels).

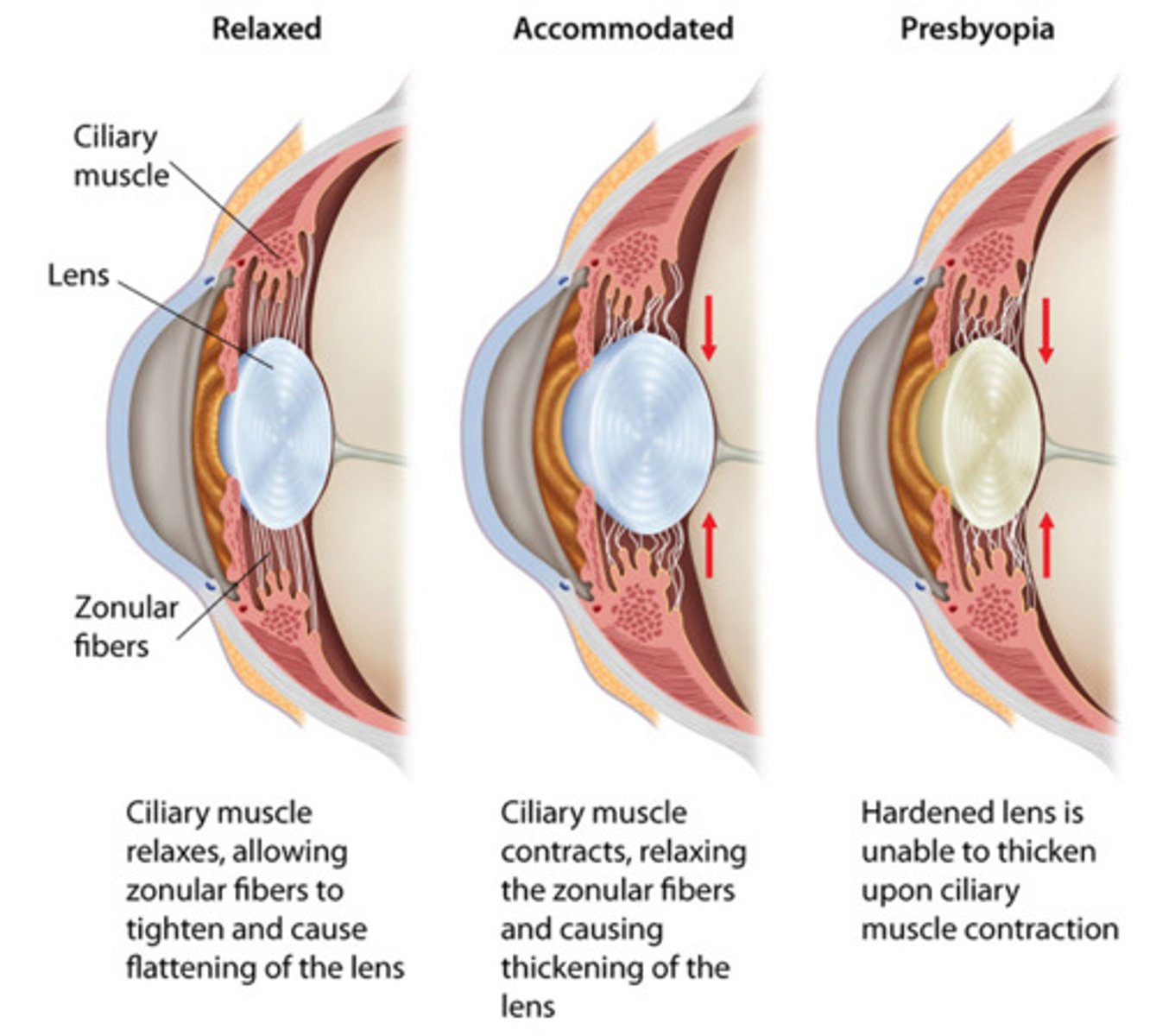
Presbyopia
Age-related loss of near vision due to a stiffening lens
Risk Factors (Impaired Sensation)
- Diabetes → neuropathy
- Stroke → sensory deficits
- Parkinson's disease
- Dementia (affects processing, not just sensing)
- Sedatives
- Antihypertensives
- Opioids
- Polypharmacy
- Poor lighting
- Clutter
- Lack of assistive devices
- Malnutrition (vitamin deficiencies)
- Social isolation
- Immobility
- History of falls
Recognizing Impaired Sensation
Vision:
- Squinting
- Trouble reading
- Bumping into objects
Hearing:
- Asking people to repeat
- Turning TV volume up
- Withdrawing from conversations
Touch / Neuropathy:
- Numbness/tingling
- Burns or injuries unnoticed
- Poor balance
- General behavioral signs
- Confusion
- Agitation
- Withdrawal
- Increased falls
Nursing Interventions (Impaired Sensation)
Vision Support:
- Ensure good lighting
- Remove hazards (clutter, rugs)
- Provide glasses (clean + correct prescription)
- Use large print materials
Hearing Support:
- Speak slowly and clearly
- Face the patient (lip reading helps)
- Reduce background noise
- Check hearing aids (working, batteries)
Safety:
- Fall precautions
- Bed in low position
- Non-slip footwear
- Call light within reach
Sensory stimulation:
- Encourage social interaction
- Provide clocks/calendars (orientation)
- Use touch appropriately
Nutrition:
Monitor for decreased taste/smell → poor intake
Encourage balanced diet
Collaborative Interventions (Impaired Sensation)
- Audiologist → hearing aids
-Ophthalmologist/
Optometrist → vision correction, cataracts
- Physical therapy → balance training
- Occupational therapy → adaptive devices
- Dietitian → nutrition support
- Neurology (if disease-related)
Risk factors that affect hearing and vision health in an older adults
- Aging
- Family history
- Poor nutrition (vitamin deficiencies)
- Lack of routine screenings
- Long-term exposure to loud noise
- Poor lighting
- Smoking (↑ macular degeneration risk)
- Diabetes
- Hypertension
- Stroke
- Neurological disorders
- Chronic ear infections
Nursing Interventions (Promote Hearing and Vision Wellness for Older Adults)
Communication:
- Speak slowly, clearly, and in a low tone
- Face the patient (lip reading)
- Use short, simple sentences
- Do NOT shout
Environment:
- Reduce background noise (TV, hallway noise)
- Ensure quiet setting for communication
Assistive Devices:
- Check hearing aids
Environment:
- Increase lighting (especially at night)
- Use nightlights
- Reduce glare
Safety:
- Remove clutter, loose rugs
- Mark edges of stairs
- Keep frequently used items within reach
Assistive Support:
- Encourage use of glasses
- Clean lenses regularly
- Provide large-print materials
Coping
How a person manages stress, challenges, or difficult situations
Concept of Coping
- Adaptive (effective):
problem-solving, seeking support, acceptance
- Maladaptive (ineffective): denial, withdrawal, substance use, aggression
Loss
Absence of something valued (person, function, role, independence)
- Actual (death, amputation)
- Perceived (loss of independence)
- Anticipatory (expected death)
- Situational (retirement, illness)
Grief
Emotional response to loss
Risk Factors for Altered Coping
- Multiple losses (spouse, friends, independence)
- Chronic illness
- Cognitive decline (dementia)
- Social isolation
- Fixed income/financial stress
Psychological:
- History of depression/anxiety
- Poor coping skills
- Low self-esteem
Environmental:
- Lack of support system
- Institutionalization (nursing home)
- Major life transitions
SELYE'S Stress Response Theory
Alarm, Resistance, Exhaustion
Anticipatory grief
A period of mourning when the dying person or his family is expecting the death
Acute grief
The intense physical and emotional expression of grief occurring as the awareness increases of a loss of someone or something significant
Shadow grief
Moments of intermittent sadness and may be accompanied with temporary disruption of day-to-day function (healthy, restorative)
Complicated grief
Prolonged or significantly difficult time moving forward after a loss
Disenfranchised grief
Grief following the loss that is not openly acknowledged, socially, accepted, or poor understanding of the meaning of loss.
Hospice
Treats the person holistically, not the disease/ quality of life, interdisciplinary teamwork, cost-effective treatment
- Doctors referral
- 6 months or less
Palliative Care
Similar to Hospice care; taking care of the whole person holistically with the goal of giving patients with life-threatening illnesses the best quality of life they can have through the aggressive management of symptoms
- No strict criteria like Hospice
Maladapting Coping
- Withdrawal or isolation
- Denial of reality
- Anger or irritability
- Substance use
- Noncompliance with care
- Excessive dependence
- Depression
- Anxiety
- Hopelessness
- Sleep disturbances
Nursing Interventions (Coping)
Emotional Support:
- Encourage expression of feelings
- Use therapeutic communication
- Validate emotions ("That sounds really difficult")
Promote Adaptive Coping:
- Identify past successful coping strategies
- Encourage problem-solving
- Promote independence when possible
Cognitive Support:
- Reframe negative thoughts
- Provide clear, simple information
Stress Reduction:
- Relaxation techniques
- Routine and structure
Social Support:
- Encourage family involvement
- Promote group activities
Nursing Collaboration (Coping)
- Social worker → resources/support
- Psychologist/psychiatrist → therapy/meds
- Support groups (grief counseling)
- Spiritual care (chaplain)
Stages of Grief
- Denial
- Anger
- Bargaining
- Depression
- Acceptance
Nursing Interventions (Loss and Grief)
Emotional Support:
- Encourage storytelling/memories
- Active listening (don't interrupt or rush)
Allow Time:
- Do NOT rush grieving process
- Respect cultural practices
Support Systems:
- Facilitate family presence
- Recommend support groups
Monitor Mental Health:
- Depression/suicidal thoughts
- Refer as needed
Spiritual Care:
- Offer chaplain or religious support if desired
Nursing Collaboration (Grief and Loss)
- Social worker → resources
- Therapist → grief counseling
- Physician → medications if severe depression
Grief and Loss Care Plan
- Grieving
- Complicated grieving
- Ineffective coping
- Social isolation
Goals/Outcomes:
- Patient expresses feelings openly
- Demonstrates healthy coping strategies
- Engages with support system
Shows gradual acceptance of loss
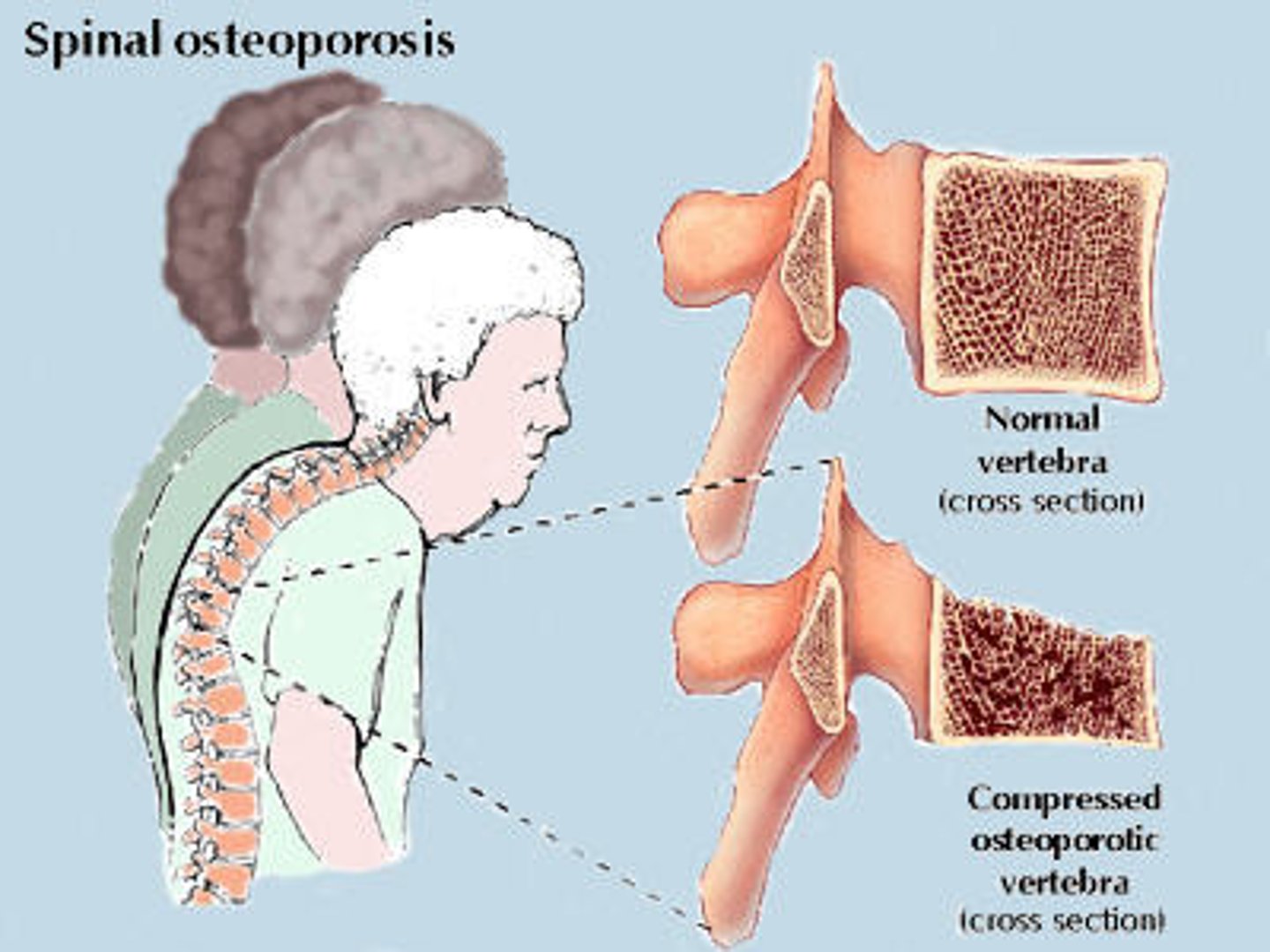
Osteoporosis
A condition in which the body's bones become weak and break easily.
- Silent disease
- Mainly in white, older, and thin females
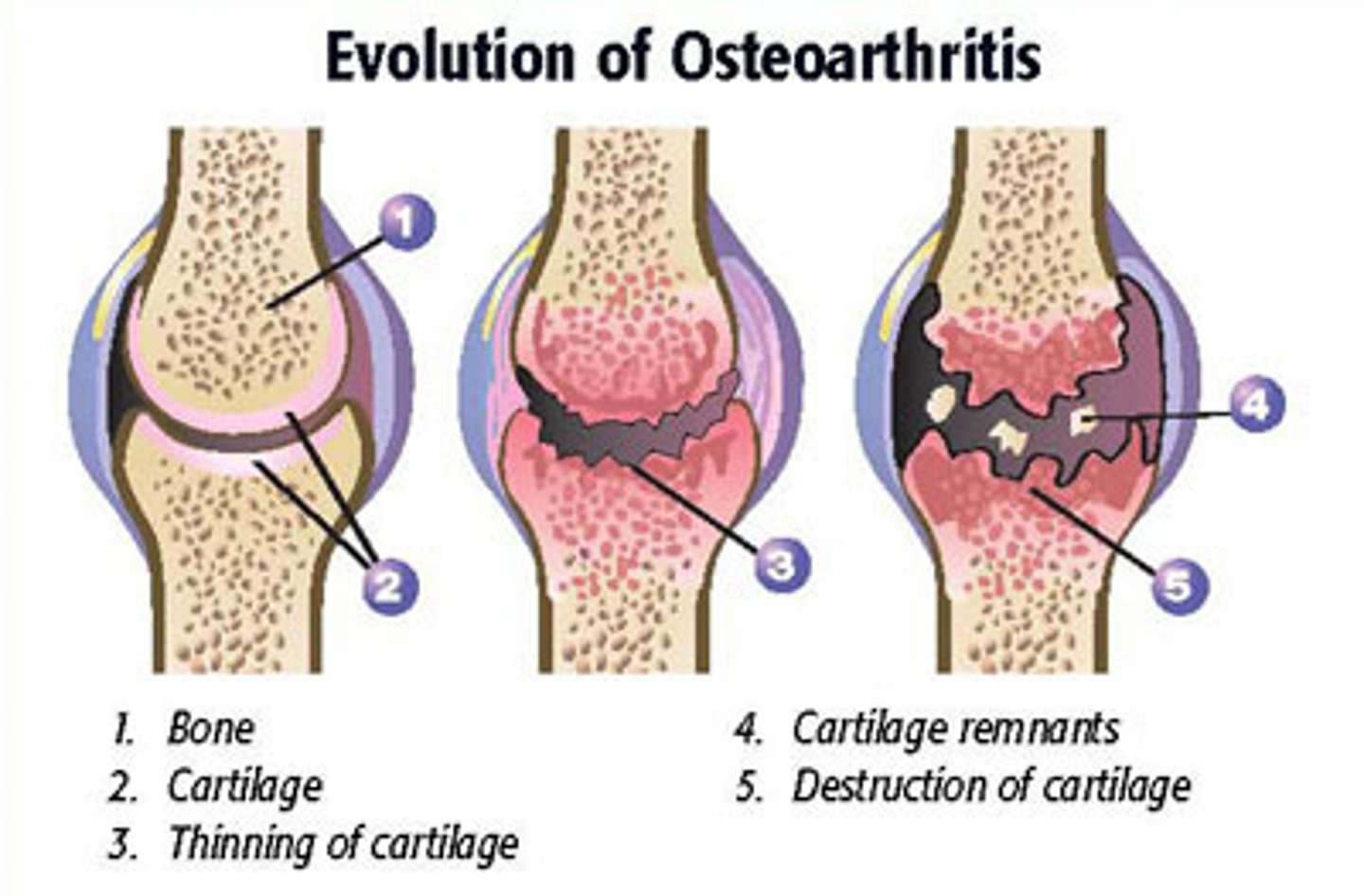
Osteoarthritis
inflammation of the bones and joints
Morse Fall Scale
Tool used to identify risk factors for falls in hospitalized patients
- Fall history
- Gait
- Mental status
- IV therapy
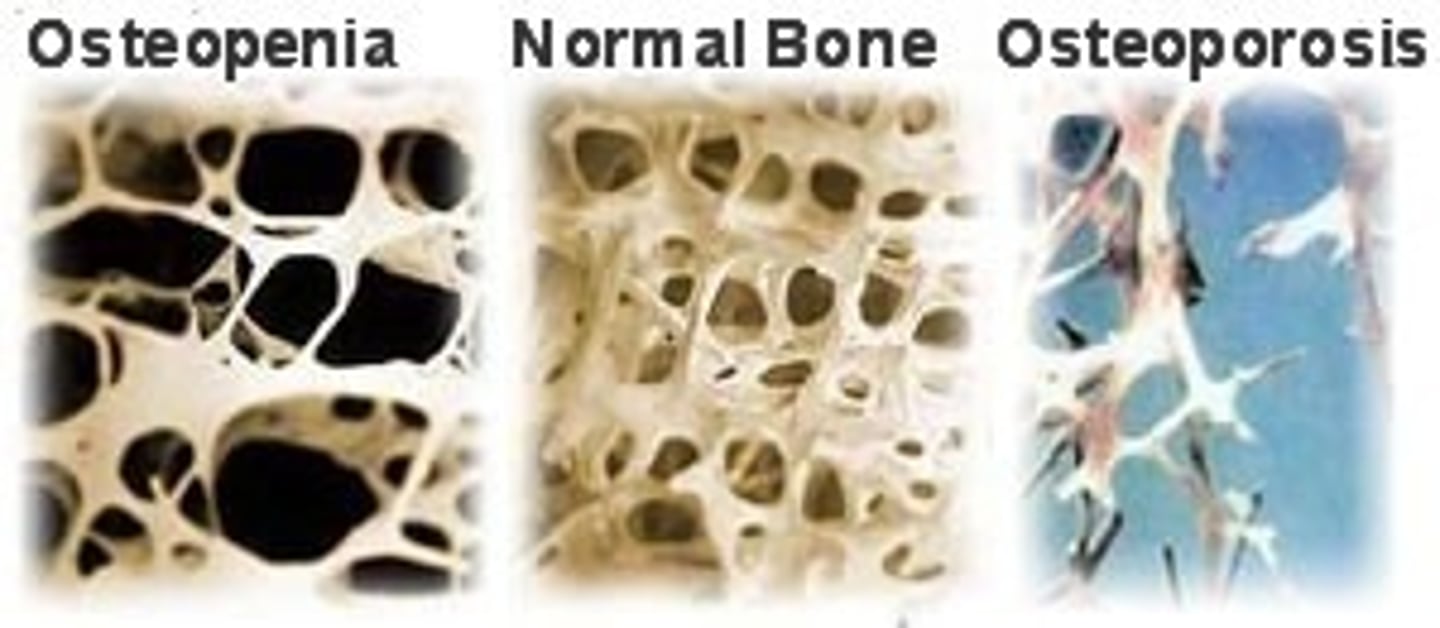
Osteopenia
Abnormal reduction of bone mass
Teaching Strategies (Mobility)
Home Safety:
- Loose rugs
- Clutter
- Poor lighting
Add safety:
- Grab bars (bathroom)
- Handrails on stairs
- Non-slip mats
- Nightlights
Mobility & Footwear:
- Wear non-slip, supportive shoes
- Avoid walking in socks
- Proper use of cane/walker
Medication Teaching:
- Identify fall-risk meds:
- Sedatives
- Opioids
- Antihypertensives
Teach:
- Change positions slowly (orthostatic hypotension)
- Speak clearly and slowly
- Repeat instructions
- Use demonstration + return demo
- Include caregivers/family
Lifestyle & Prevention:
- Exercise (strength + balance)
- Hydration
- Vision/hearing exams
Factors Contributing to Falls
- Muscle weakness
- Poor balance/gait
- Vision impairment
- Cognitive impairment (confusion, dementia)
- Chronic illness (stroke, Parkinson's)
- Orthostatic hypotension
- Polypharmacy
- Sedatives
- Antidepressants
- BP medications
- Poor lighting
- Slippery floors
- Clutter
- No assistive devices
National Needs Associated with the Aging Metabolism.
- Metabolism slows down
- Muscle mass decreases
- Body needs fewer calories
- Risk of fat gain increases
(Older adults need fewer calories but MORE nutrients)
National Needs (Malnutrition)
- Malnutrition in older adults (often missed)
- Obesity + malnutrition at the same time
- Dehydration in elderly
- Vitamin deficiencies (Vitamin D, B12, iron)
- Food insecurity in older adults
Malnutrition
Lack of proper nutrition
Strategies to Meet Nutritional Needs
- Small, frequent meals
- High-protein foods (eggs, fish, chicken, beans)
- Nutrient-dense foods (more nutrition, less volume)
- Soft foods if chewing is difficult
Hydration:
- Offer fluids often
- Don't wait for thirst (older adults don't feel thirst well)
Nursing Intervention (Age Related Changes Malnutrition)
- Monitor weight regularly
- Track food intake
- Assist with meals if needed
- Check for swallowing problems
Nursing Collaboration (Age Related Changes Malnutrition)
- Dietitian → meal planning
- Speech therapy → swallowing issues
- Social worker → food access programs
Clear Liquid Diet
Transparent liquids (water, broth, pulp-free juice, plain gelatin) that are easily digested, leaving minimal residue in the digestive tract
Full Liquid Diet
Liquids and foods that turn into liquid at room temperature, including milk, strained cream soups, and smoothies
Pureed Diet
Foods have been blenderized to liquid form; consistency based on client's needs, nectar or honey thick, can be long term
Mechanical Soft Diet
Foods that are soft, moist, and easy to chew, often chopped, ground, or blended to a texture requiring minimal chewing
Diabetic Diet
Balanced intake of protein, fats, and carbohydrates of about 1,800 calories
Perfusion
The supply of oxygen to and removal of wastes from the cells and tissues of the body as a result of the flow of blood through the capillaries.
Normal Age-Related Perfusion Changes
- Reduced overall cardiac output (about 1% per year)
- Lowered blood volume due to decreased body water
- Arteries become stiffer (arteriosclerosis), causing higher systolic blood pressure, while cerebral blood flow reduces, particularly reducing regional oxygen supply to the brain
Nursing Interventions (Impaired Perfusion)
Improve Circulation:
- Encourage frequent ambulation (as tolerated)
- Change position every 2 hours if immobile
- Avoid crossing legs (reduces blood flow)
Prevent orthostatic hypotension:
- Teach patient to rise slowly
Lying → sitting → standing
- Monitor BP sitting and standing
Promote oxygen delivery:
- Position in semi-Fowler's
- Monitor SpO₂ levels
- Give oxygen if ordered
Support heart function:
- Monitor HR, BP, edema, lung sounds
- Administer cardiac meds (antihypertensives, diuretics)
- Watch for heart failure signs
Protect tissues:
Check skin often (especially feet, heels, sacrum)
Keep extremities warm
Encourage hydration (if not restricted)
Patient education:
- Stop smoking (major perfusion risk)
- Heart-healthy diet (low sodium, low fat)
Report:
- Chest pain
- SOB
- Leg pain when walking
Normal Age-Related Changes (Oxygenation)
Lung changes:
- Lungs lose elasticity → harder to expand
- Alveoli decrease in number and function → less gas exchange
- Residual volume increases (air gets trapped)
- Vital capacity decreases
Chest wall changes:
- Chest becomes stiffer
- Weaker respiratory muscle
- Less chest expansion
Airway changes:
- Increased mucus production
- Cilia function decreases → harder to clear secretions
Gas exchange changes:
- Decreased oxygen exchange → lower O₂ levels
- Increased risk of hypoxia
Control of breathing:
- Reduced sensitivity to CO₂ and O₂ levels
- Slower response to low oxygen
Nursing Interventions (Oxygenation)
Positioning:
- High-Fowler's or semi-Fowler's
- Promotes lung expansion
Promote lung expansion:
- Encourage deep breathing exercises
- Incentive spirometer
- Encourage coughing to clear secretions
Increase Mobility:
- Early ambulation
- Turn/reposition every 2 hours if immobile
Maintain airway:
- Provide suctioning if needed
- Encourage fluid intake (if not restricted) to thin mucus
Oxygen therapy:
- Monitor SpO₂
- Administer oxygen as prescribed
- Watch for signs of hypoxia:
- Confusion (early sign in elderly!)
- Restlessness
- Cyanosis (late sign)
Prevent complications:
-Oral care (reduces pneumonia risk)
Vaccinations:
- Flu
- Pneumonia
Patient education:
- Stop smoking
- Avoid respiratory irritants
Report:
- SOB
- Cough
- Fever