Chapter 22: Microbial Diseases of the Nervous System
1/129
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
130 Terms
What is the central nervous system (CNS)?
brain and spinal cord
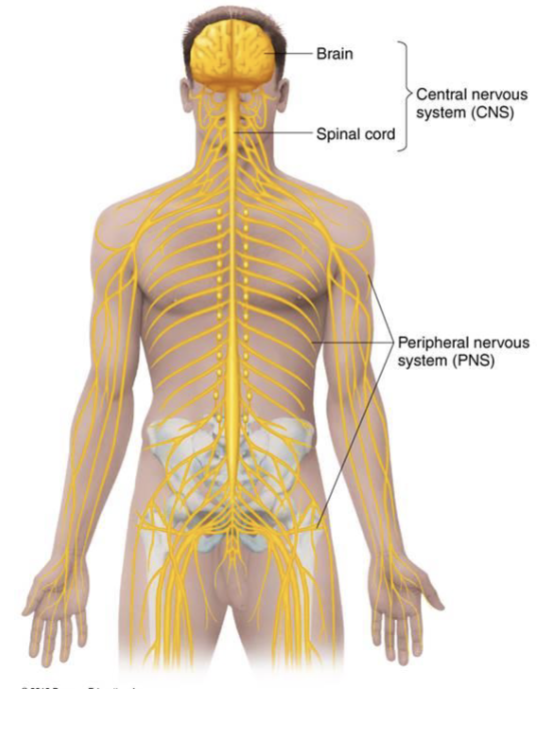
What is the Peripheral nervous system (PNS)?
nerves that branch from the CNS
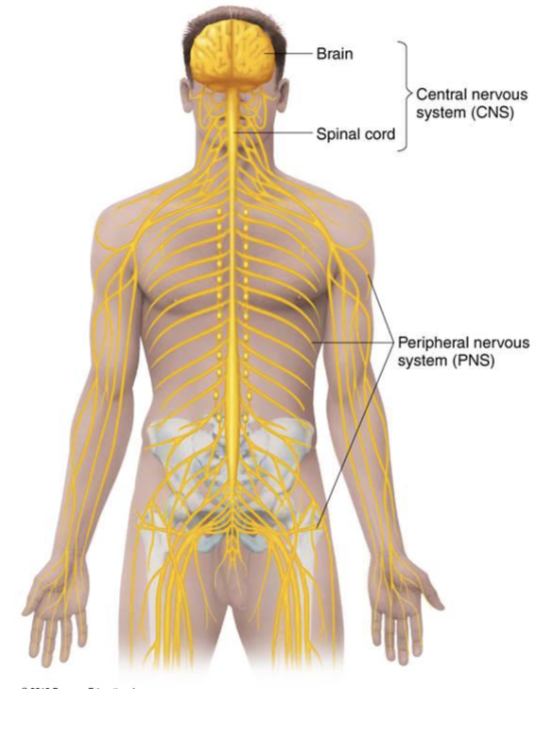
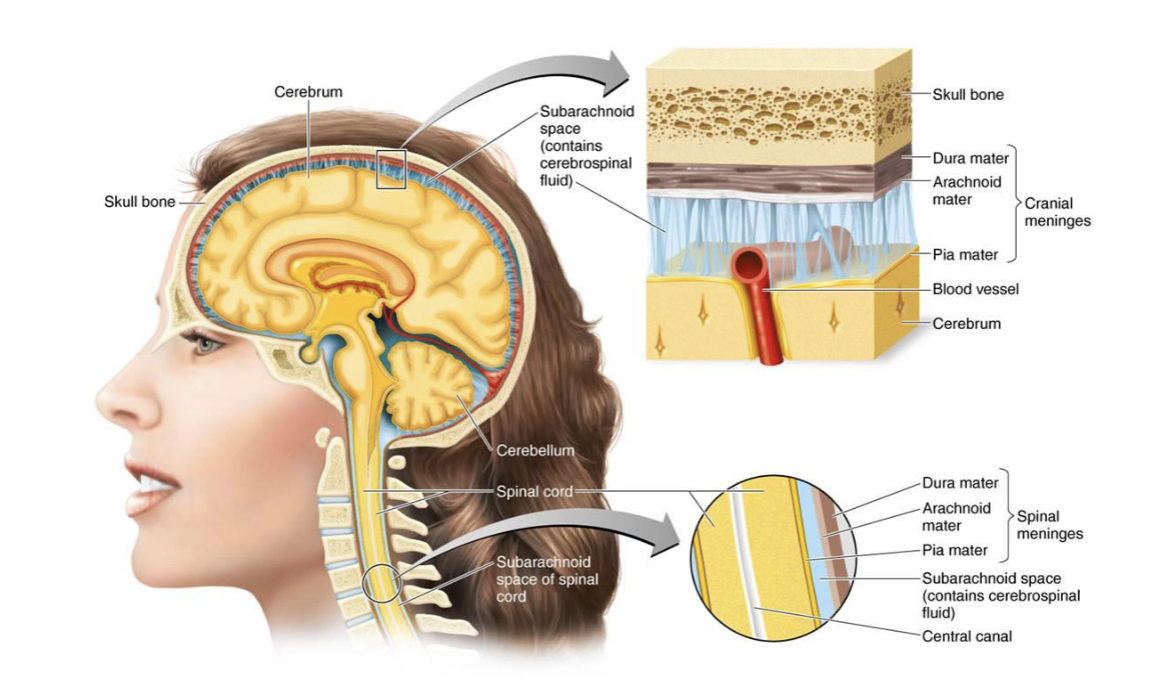
What are the Meninges?
nerves that protect the brain and spinal cord
What consists of the Meninges?
Dura, arachnoid and pia mater; outer, middle, and innermost layers, respectively
Subarachnoid space contains cerebrospinal fluid (CSF)
What is the blood-brain barrier?
Drugs can cross if small and lipid-soluble
immune cells
What is Meningitis?
Inflammation of the meninges
What is Encephalitis?
Inflammation of the brain
What is Meningoencephalitis?
Inflammation of both the meninges and the brain
What are the initial symptoms of Bacterial Meningitis?
fever, headache, and stiff neck
followed by nausea and vomiting
can progress to convulsions and coma
How can someone die from Bacterial Meningitis?
from shock and inflammation
due to endotoxin and cell wall release
How does bacterial Meningitis compare to viral meningitis?
it is more common and mild
What is Haemophilus influenzae Meningitis?
Gram-negative aerobic bacteria; normal throat microbiota
Can enter the bloodstream
Pathogenicity due to capsule antigen type b
Who is affected by Haemophilus influenzae Meningitis?
children (6 months to 4 years old)
How is Haemophilus influenzae Meningitis prevented?
Hib vaccine
How many bacterial meningitis cases does Haemophilus influenzae Meningitis account for & what morality rate?
45%; 6% mortality
What is Neisseria meningitidis Meningitis (Meningococcal Meningitis)?
Aerobic, gram-negative diplococcus with a capsule
six serotype associated with the disease
What is the percentage of healthy people that are nasopharyngeal carriers?
40%
How does Neisseria meningitisdis Meningitis begin?
a throat infection, rash (does not fade when pressed), and bacteremia
What is the morality rate of Neisseria meningitidis Meningitis?
9-12% with antibiotic therapy; 80% without
Where do outbreaks of Neisseria meningitidis Meningitis start?
dorms and military barracks
Which serogroups does the vaccination of Neisseria meningitidis Meningitis protext against and not protect against?
protects against serogroups A, C, Y, A and B but not X
What is Streptococcus pneumoniae Meningitis (Pneumococcal Meningitis)?
Gram-positive, encapsulated diplococcus
What is the percentage of nasopharyngeal carriers on Streptococcus pneumonia Meningitis?
70% of people are healthy nasopharyngeal carriers
What does Streptococcus pneumonia Meningitis cause?
pneumonia and otitis media
In what age is Streptococcus pneumonia Meningitis most common?
children (1 month to 4 years)
What is the morality rate of Streptococcus pneumonia Meningitis?
8% in children, 22% in the elderly
How is Streptococcus pneumonia Meningitis prevented?
conjugated vaccine
How is Bacterial Meningitis most commonly diagnosed?
Sample cerebrospinal fluid CSF via a spinal tap or lumbar puncture
pathogens in CSF do not survive storage or changes in temp
Latex agglutination tests
Chemotherapy initiated before diagnosis
Broad-spectrum third-generation cephalosporins
What is Listeriosis caused by?
Listeria monocytogenes
gram-positive rod
How is Listeriosis spread?
foodborne or symptomatic
meningitis more common in the immunocompromised
What can Listeriosis invade?
bloodstream, which causes sepsis
How does Listeriosis reproduce?
in phagocytes
spread phagocyte-to-phagocyte
How does Listeriosis affect pregnant women?
crosses the placenta which leads to still birth
What is tetanus caused by?
Clostridium tetani
gram-positive, endospore-forming, obligate anaerobe
Where does tetanus grow?
in deep wounds with anaerobic conditions
What toxin is released in tetanus?
Tetanospasmin neurotoxin is released from dead bacterial cells
What is the process of the Tetanus toxin being released from bacterial cells?
Enters CNS
Blocks the relaxation pathway in muscles, causing muscle spasms
death occurs from spasms of respiratory muscles
How is Tetanus prevented?
vaccination with a Tetanus toxoid (DTaP)
Stimulates antibodies that neutralize the toxin
Booster required every 10 years
How many cases of Tetanus are there and what is the morality rate?
Fewer than 10 cases per year
25-50%
What is the treatment for Tetanus?
immune globuilin (TIG)
What has to be removed with Tetanus?
infected tissue removed via debridement
What is Botulism caused by?
Clostridium botulinum
gram-positive, endospore-forming, obligate anaerobe
What does the intoxication of Botulism come from?
ingesting the botulinal endotoxin
specific for the synaptic end of the nerve
blocks release of the neurotransmitter acetylcholine causing flaccid paralysis
How do people die from Botulism?
respiratory or cardiac failure
What are the different types of Botulinal?
Type A toxin
fatality: 60-70%
Heat-resistent and proteolytic
Type B toxin
Fatality: 25%
Type E toxin
produced by organisms in marine and lake sediments
less heat resistant than other strains
How are the different types of Botulinal types diagnosed?
inoculating immunized mice with patient samples
What is Infant botulism?
C. botulinum growing in the intestines of infants due to a lack of intestinal microbiota
associated with honey
What is Wound botulism?
growth of C. botulinum in wounds
How do you treat infant and wound botulism?
respiratory assistance and antitoxins
How do you prevent infant and wound botulism?
proper canning and the use of nitrites in foods
What is Leprosy caused by?
aka Hansen’s disease
Caused by Microbacterium leprae
Acid-fast rod that grows best as 30 degrees C
Generation time of 12 days
Where does Leprosy grow?
peripheral nerves and skin cells
survives macrophages and invades the myelin sheath
How is Leprosy transmitted?
requires prolonged contract with an infected person or the inhalation of secretions
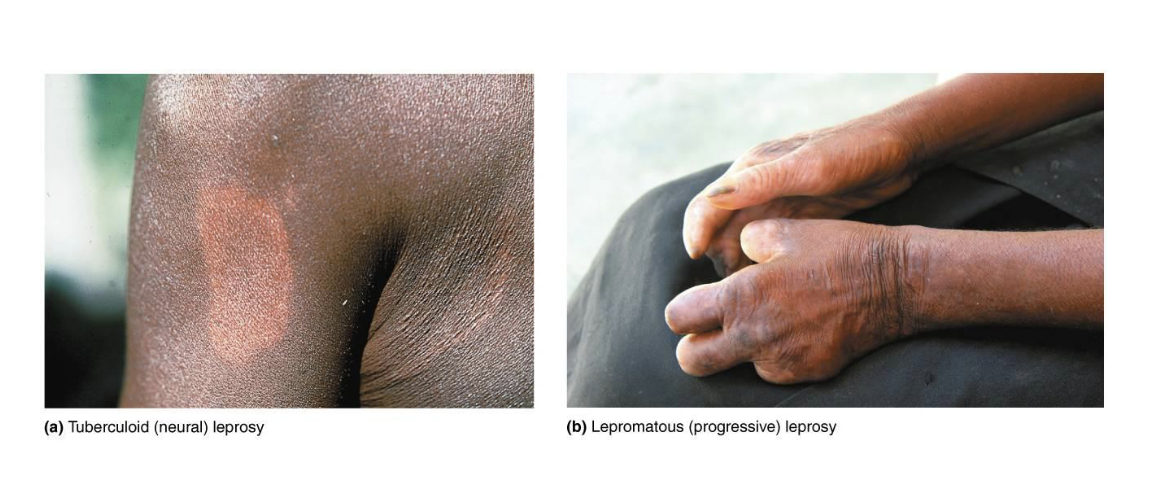
What is Tuberculoid (neutral) form?
A form of leprosy where there is a loss of sensation in skin areas
What is Lepromatous (progressive) form?
A form of Leprosy in which disfiguring nodules over the body; mucous membranes are affected
How many cases of Tuberculoid and Lepromatous are there?
100 per year, most immigrants from endemic countries
How do you diagnose Tuberculoid and Lepromatous?
skin biopsy or skin smear, blood test
How do you treat Tuberculoid and Lepromatous?
antibiotics (Capsone, Rifampin, and Clofazimine) for 6 to 24 months
What is Poliomyelitis caused by?
Poliovirus
How is Poliomyelitis transmitted?
ingestion of water containing feces containing the virus
What are the initial symptoms of Poliomyelitis?
sore throat and nausea
What can occur in Poliomyelitis?
Viremia may occur; enters the CNS
One percent of cases become paralytic
Destruction of motor nerve cells
death from respiratory failure
What are the vaccines of Poliomyelitis?
Salk vaccine: inactivates vaccine; injected
Sabin vaccine: attenuated vaccine; oral; lifelong immunity
What is the cure for Polio?
no cure, but fell 99% from 1988 to 2000
Where is Polio still present?
Nigeria, Pakistan, and Afghanistan
What is Rabies caused by?
rabies virus
Genus Lyssavirus; bullet-shaped
Single-stranded RNA; easily developed mutants
How is rabies transmitted?
saliva of an animal bite
can also cross mucous membranes
What is the most common cause of Rabies?
Silver-haired bats
What are the initial symptoms of Rabies?
muscle spasms of the mouth and pharynx; hydrophobia
Where does the Rabies virus multiply?
skeletal muscles and travels through the PNS to the brain cells, causing encephalitis
average incubation of 30-50 days
forms Negri bodies in the brain stem
What is furious (classical) rabies?
animals are restless, then highly excitable
What is paralytic (dumb or numb) rabies?
animals seems unaware of their surroundings; minimally excitable
What is the pathology of Rabies infection?
Rabies virus enters the host via a bite from a rabid animal
Virus proliferates in the PNS
Virus travels up the PNS to the CNS
Virus reaches the brain (CNS) and causes fatal encephalitis
How do you diagnose Rabies?
bodily fluids with the direct fluorescent-antibody (DFA) test
What is postexposure prophylacis (PEP)?
vaccine plus immune globulin
human diploid cell vaccine (HDCV)
human rabies immune globulin (RIG)
Describe the treatment for Rabies?
very little effective treatment
What kinds of animals does Rabies occur in?
bats. skunks, foxes, raccoons, and domestic animals
rarely in squirrels, rabbits, rats, and mice
How many humans get rabies annually?
6
What are related Lyssavirus Encephalitis with Rabies?
Clinically indistinguishable from classic rabies
Found in countries free of rabies
Australian bat lyssavirus (ABLV)
European bat lyssavirus (EBLV)
What is Congenital infections?
cross the placenta and cause serious damage to a fetus
What are some viral diseases with the vertical transfer that are harmful to developing babies?
Zika virus disease
Neonatal herpes
Cytomegalovirus (CMV) infections
What are some bacteria and protozoan that can cross the placenta and cause disease
Treponema pallidum
Listeria monosytogenes
Group B Streptococcus
Elizabethkingia
Toxoplasma gondii
What is the test that screens pregnant women for diseases that transmit vertically?
TORCH
What is the TORCH test?
Panel of tests that screen for antibodies to infections in pregnant women
Toxoplasmosis
Other (Such as syphalis, chickenpox, HIV, measles, mumps, and hep B)
Rubella
Cytomegalovirus
Herpes simplex virus
What is Arbovirus Encephalitis?
anthropod-borne virus
belong to several families
What is Arboviral Encephalitis caused by?
mosquito-borne viruses
What are the two different types of Erboviral Encephalitis?
Eastern equine encephalitis (EEE) and western equine encephalitis (WEE)
What is the morality of Eastern equine encephalitis (EEE) and western equine encephalitis (WEE)?
30% in humans
What does Eastern equine encephalitis (EEE) and western equine encephalitis (WEE) cause?
brain damage, deafness, and neurological
What is St. Louis encephalitis (SLE)?
Distributed mostly in the central and eastern US
Fewer than 1% of the infected show symptoms
What is California encephalitis (CE)?
Mild and rarely fatal
What is West Nile virus (WNV)?
Maintained in the bird-mosquito-bird cycle
Carried by Culex mosquitos
Can cause polio-like paralysis and fatal encephalitis
What is Heartland virus disease?
Neurological problems, thrombocytopenia, leukopenia
What is Powassan virus (POW)
Distributed mostly in northeastern US and Great Lake region
Long-term neurological problems may occur
Morality of 10-15%
What is Japanese encephalitis?
found in the Far East and South Asia
One percent show symptoms, but there is a 20-30% morality in those with symptoms
How is Abroviral Encephalitis diagnosed?
ELISA tests (to identify IgM antibodies)
How can you prevent Arboviral Encephalitis?
controlling mosquitos
How is Zika Virus transmitted?
the bite of infected Aedes spp. moquitos
other include sexual intercourse, mother to child, and blood transfusions
What perfect of people infected with the Zika virus show symptoms?
20%, symptoms are usually mild
What happens if a pregnant women gets the Zika Virus?
increases the risk of microcephaly in infants