AnP 2 lab 23 Urinary System
1/110
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
111 Terms
has a role in urine production
has a large blood supply
no organ receives a greater fraction of cardiac output in terms of blood flow per gram of organ weight than this organ
the kidney
explain why a large volume of blood is is necessary for the primary function of the kidney
It helps with maintaining the homeostasis of blood.
The kidney monitors and regulates blood pH and its concentration of wastes, water, and electrolytes
Blood being in the correct state of dynamic equilibrium means that interstitial fluids will be as well
if interstitial fluids are stable, then the tissues and cells
tend to stay alive and do their job
the outer most layer of the kidney is
the fibrous capsule
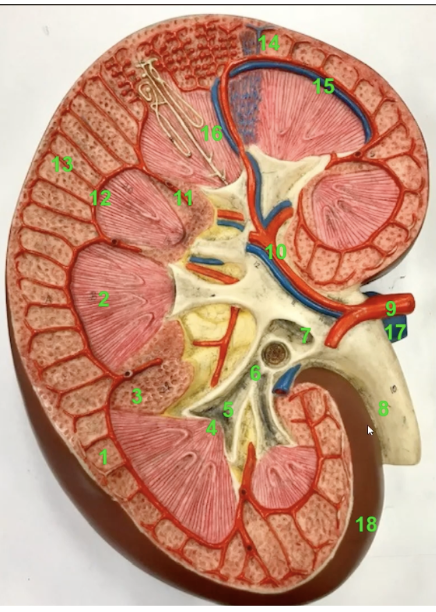
what is the function of 18? Also what is it
this is the fibrous capsule. It provides a covering of collagenous connective tissue that strengthens and protects the kidney tissue
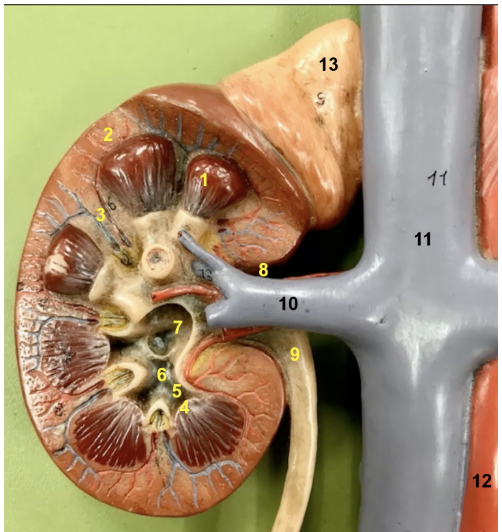
the kidney has a convex lateral surface and a concave medial surface. The medial indentation is 8 which is
the renal hilum
the hilum is the entry point for →
the hilum is the exit point for →
entry point: renal artery and renal nerves
exit: renal vein and ureter
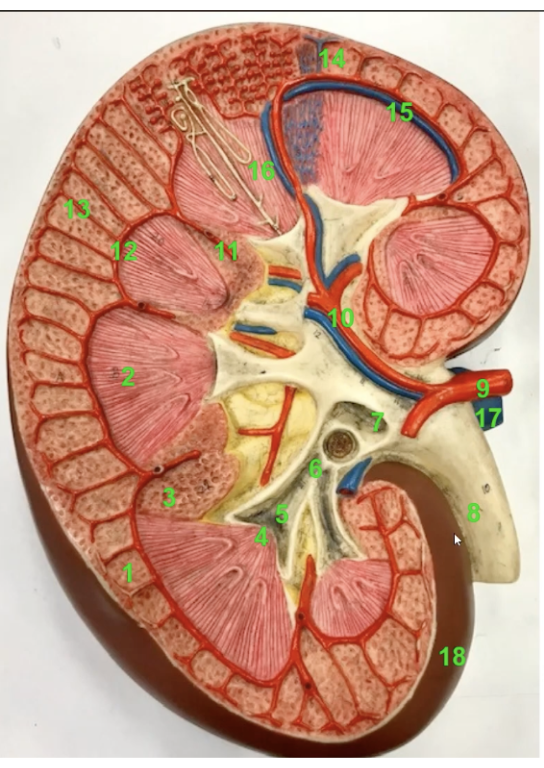
identify which number is
the renal artery
renal vein
ureter
renal artery → 9
renal vein → 17
ureter → 8
superior to the kidney is the
adrenal or supraadrenal gland
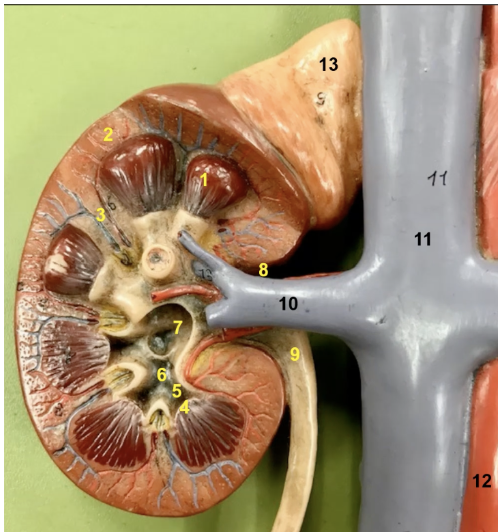
function of 13
the adrenal gland will secrete a variety of hormones
cortex of the gland will secrete cortisol, aldosterone, and certain sex hormones
medulla secretes epinephrine and norepinephrine during sympathetic response
2 regions of the kidney
medulla
cortex
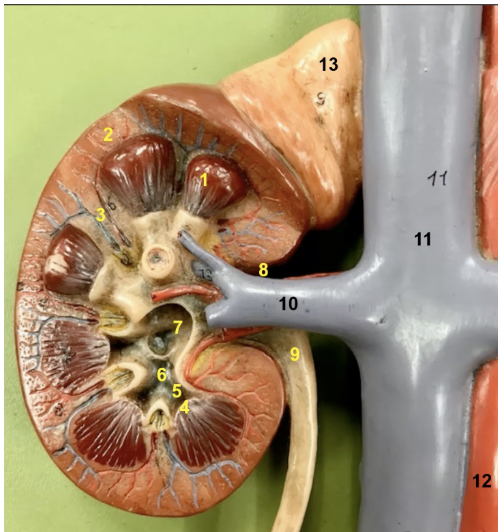
the medulla is primarily composed of triangular mass known as the ______. What number is that
renal pyramid. Number 1
The apex/tip of the renal pyramids point toward the interior of the kidney. This is referred to as the
renal papillae
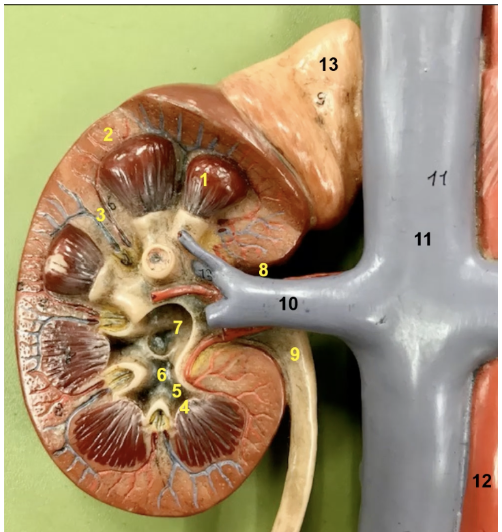
What is 2
the cortex of the kidney which is superficial to the pyramid
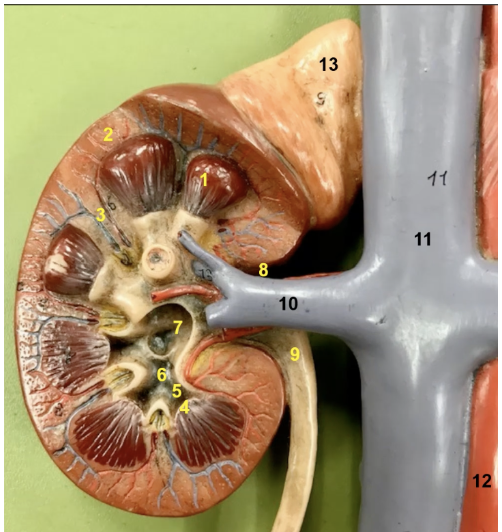
Extensions of cortical tissue in between the renal pyramids are known as ____ which is which number
renal columns. Number 3
urine is produced within the renal cortex and then travels through the renal pyramids. Why are those straitiated
due to the presence of urine carrying tubes called collecting ducts
urine constantly drips out of each renal papilla into the tube called the
minor calyx
each renal pyramid has a corresponding minor calyx. Minor calyces form to converge a
major calyx
Major calyces converge to yield a large funnel structure near the renal hilum called the
renal pelvis
the renal pelvis exits the kidney and becomes the
ureter
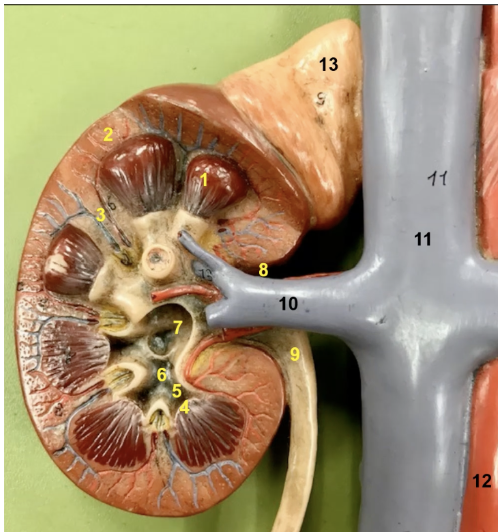
Label 5,6,7
minor calyx
major calyx
renal pelvis
pathway for urine flow in kidney
Renal cortex → renal pyramid → renal papila → minor calyx → major calyx → renal pelvis → ureter
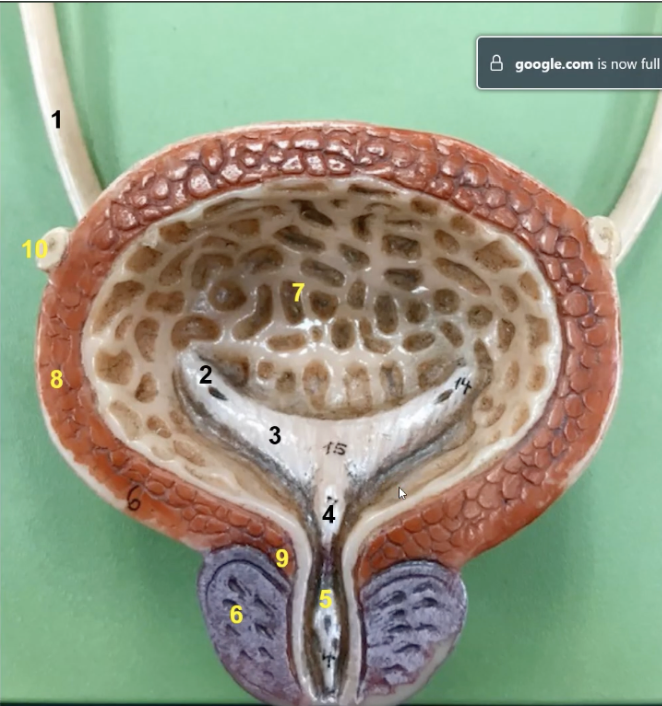
What is this and its function
this is the urinary bladder. It is a collapsible storage sac of urine that allows for urine expulsion to occur infrequently despite the that urine is always produced
the mucosa of the urinary bladder is lined by
transitional epithelium
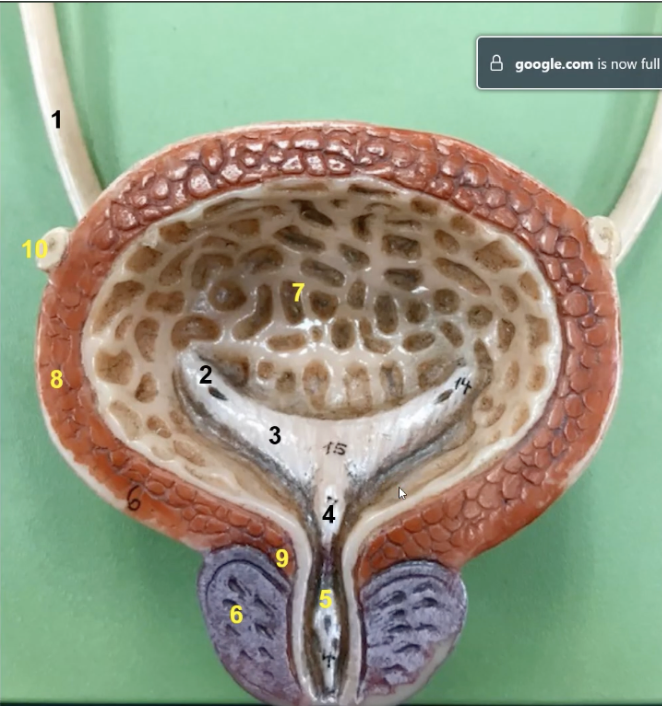
what is 7 and its function
this is the rugae. It gives the bladder expanability
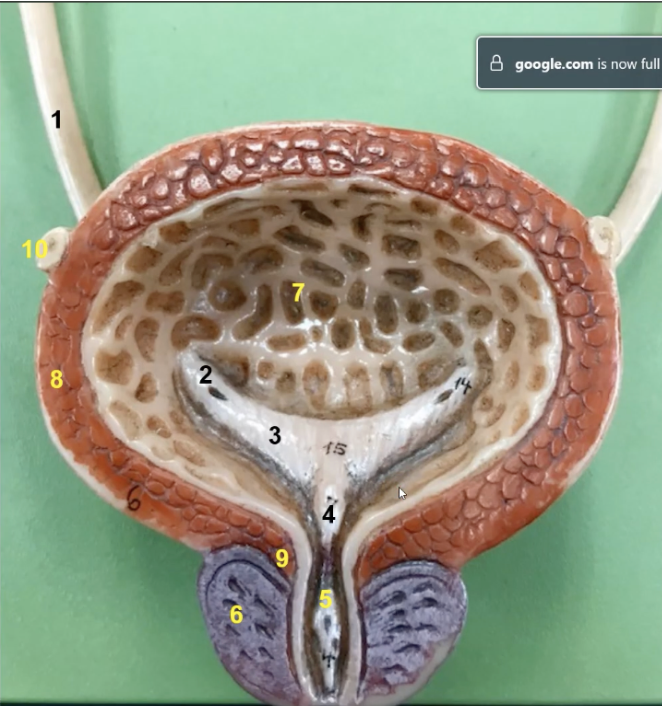
the muscularis of the urinary bladder is composed of three layers of smooth muscle called the _______ which is number 8
detrusor muscle which is 8
The urinary bladder is lined by
parietal peritoneum on its superior surface and fibrous adventitia on all other sides.
urine exits bladder via the
urethra
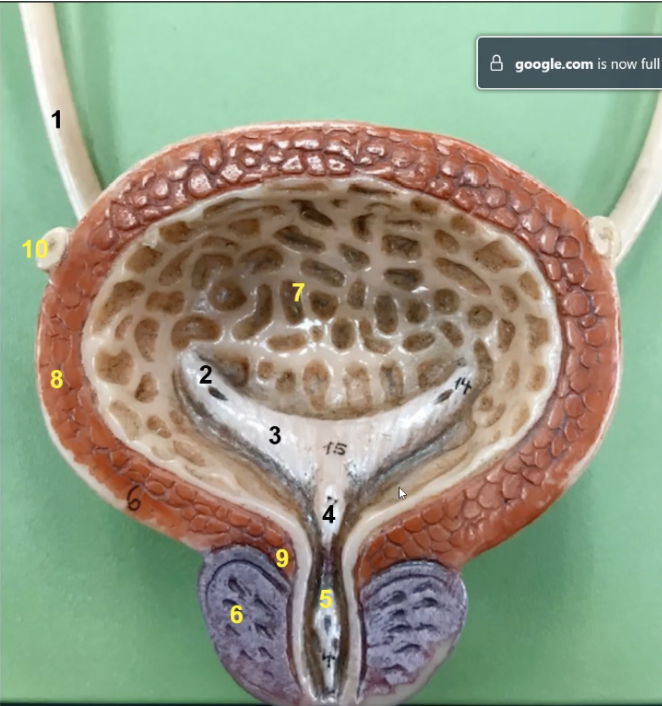
the opening to the urethra within the bladder is the _____ which is number. What is its function
internal urethral orifice which is number 5. Opens during urination
the two ureteric openings and single urethral orifice mark a smooth triangular region devoid of rugae known as the
trigone
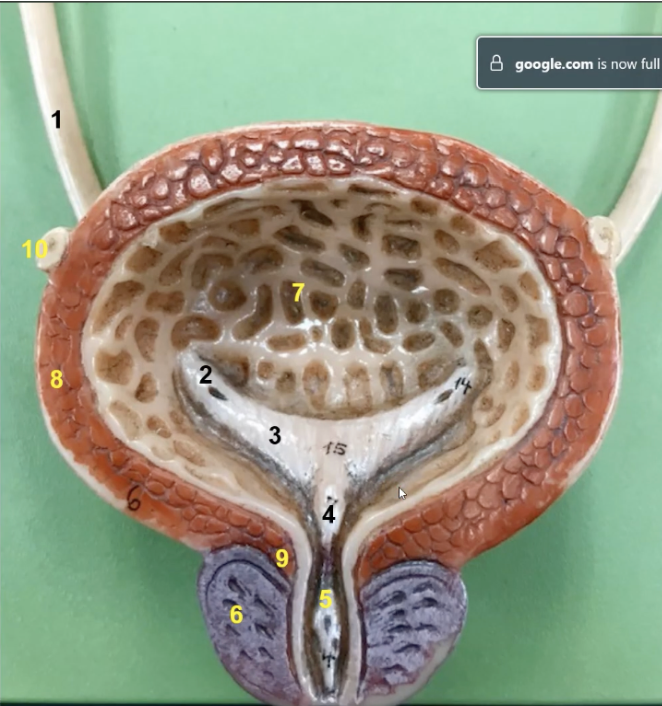
function of 3
Trigone. During urination, while the detrusor muscle contracts (expelling urine), the trigone acts to funnel urine in the urethra.
Branching off the aorta not long after its incursion into the abdominal cavity are the
paired renal arteries
within the kidney, the renal arteries begin to branch. Explain it
the first branches are the segmental arteries.
The segmental arteries give off branches to the interlobar arteries
at the base of the renal pyramids are the arcuate arteries
extending radially from the arcuate arteries into the renal cortex are the interlobular arteries (13)
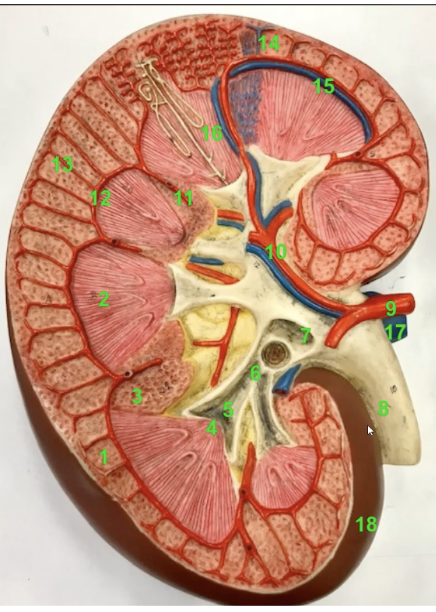
label 9, 10, 11, 12, 13
9 → renal arteries
10 → segmental arteries
11 → interlobar arteries (also around 16)
12 → arcuate arteries (also around 14)
13 → interlobular arteries
Branching off of each interlobular artery are
afferent arterioles
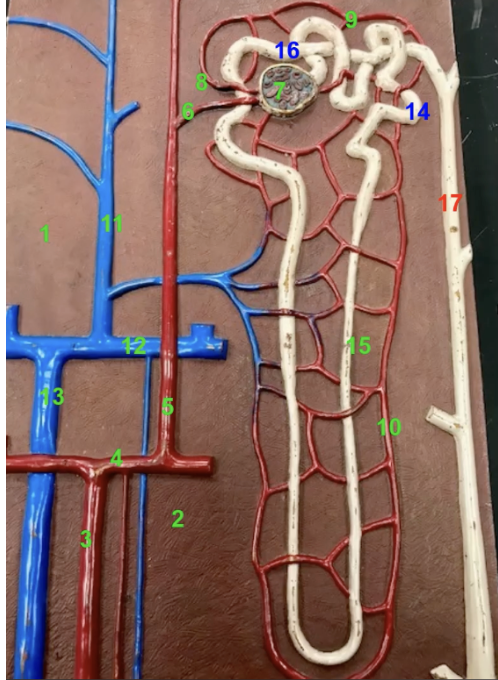
where are the afferent artioles
6
Each afferent arteriole delivers blood to a spherical capillary cluster known as the
glomerulus
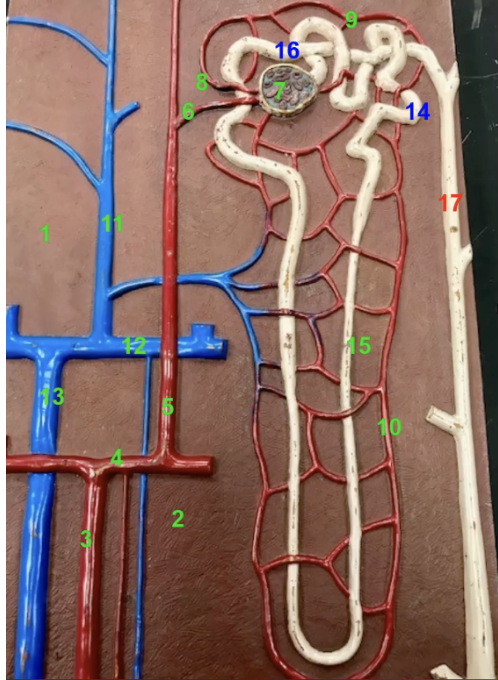
function of 7
the glomerulus. Place where the filtration of blood (first step of urine formation) take place before it goes to renal tubules
exiting rach glomerulus is an _____ arteriole.
efferent arteriole
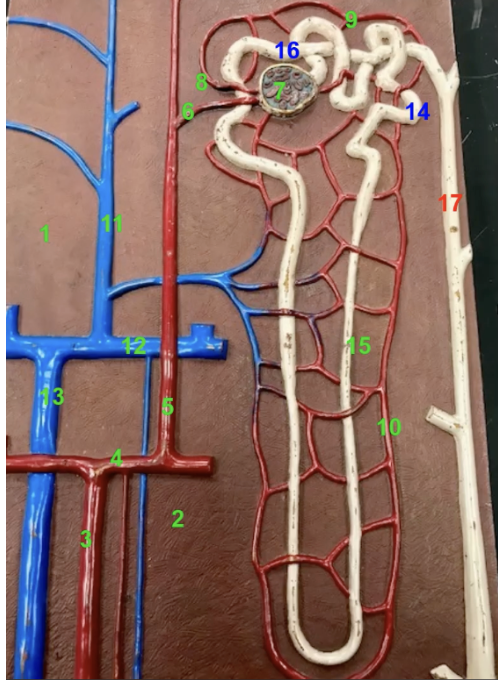
what is 8? describe its volume of blood
efferent arteriole. The volume of blood in the efferent arteriole is usually only about 80% of the afferent arteriole since a fraction of blood plasma is filtered in the glomerulus
Each efferent arteriole will typically empty into a second set of capillaries referred to as the
peritubular capillaries

why is 9 named what it is
peritubular capillaries. Named so because of their close proximity to a set of structures called renal tubules
At the peritubular capillaries, the vast majority of fluid filtered at the glomerulus is
reclaimed
Some efferent arterioles empty into a set of straight vessels known as the
vasa recta while others give rise to the peritubular capillaries
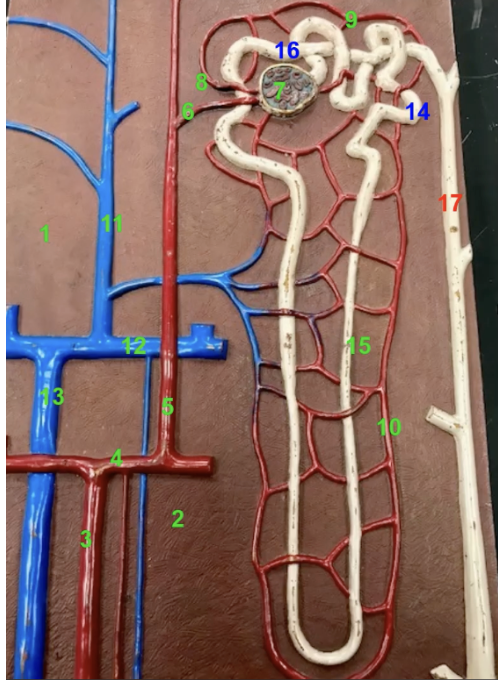
what is 10
vasa recta
Blood from the peritubular capillaries and vasa recta travels to the
interlobular veins which are are adjacent to the interlobular arteries.
Interlobular veins empty into
arcuate veins
arcuate veins empty into the
interlobar veins
The interlobar veins converge to yield the renal vein, which exits the renal hilum and
delivers blood to the inferior vena cava
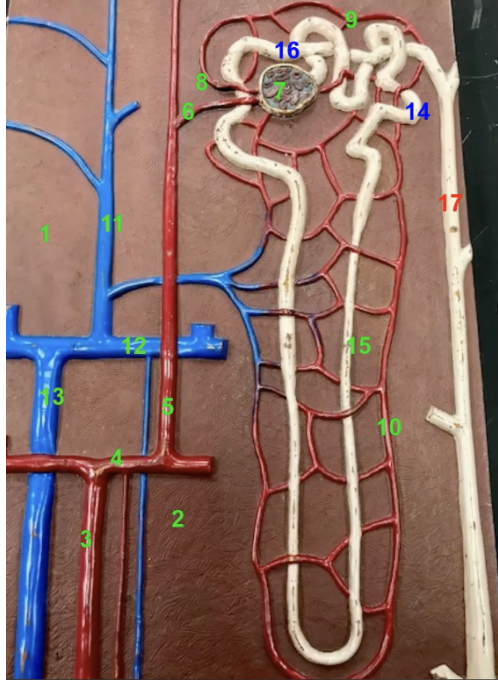
what is 9-13
peritubular capillaries
vasa recta
interlobular veins
arcuate veins
interlobar veins
pathway for renal blood flow
Abdominal aorta → renal artery → segmental artery → interlobar artery → arcuate artery → interlobular artery → afferent arteriole → glomerulus → efferent arteriole → peritubular capillaries/vasa recta → interlobular vein → arcate vein → interloar vein → renal vein → inferior vena cava
Renal structures that work with the glomerular and peritubular capillaries to produce
urine
Surrounding each spherical glomerulus is a structure known as the
glomerular capsule
The relationship between the glomerulus and the glomerular capsule is like that of a fist punching a balloon
first → glomerulus
balloon → capsule
Portion of the capsule lying directly on the glomerulus is its _____layer which is composed of cells called
visceral layer; podocytes
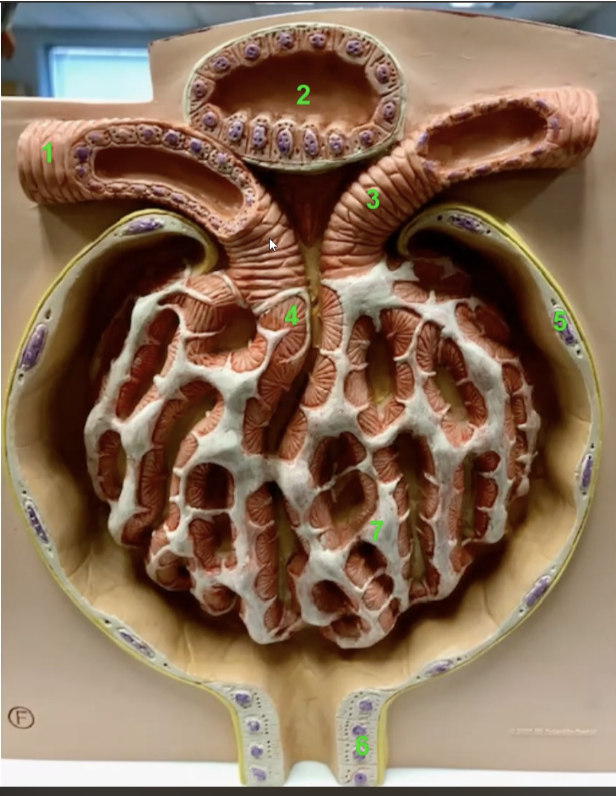
what is 5 and what is it made of
parietal layer of the glomerular capsule. It is its outer layer and composed of simple squamous epithelium
Collectively, the glomerulus and the glomerular capsule are known as the
renal corpuscle
High pressure in the glomerular capillaries forces fluid from their lumen to the
lumen of the capsule (space between its parietal and visceral layers)
Podocytes help ensure that
no formed elements or plasma proteins leave the glomerulus
The fluid that enters the lumen of the capsule is referred to as
filtrate
filtrate contains solutes of two varieties which are
Things we’d like to keep → nutrients
Excretions (wastes)
Flitrate exits the glomerular capsule and enters a tortuous tube known as the
proximal convoluted tubule
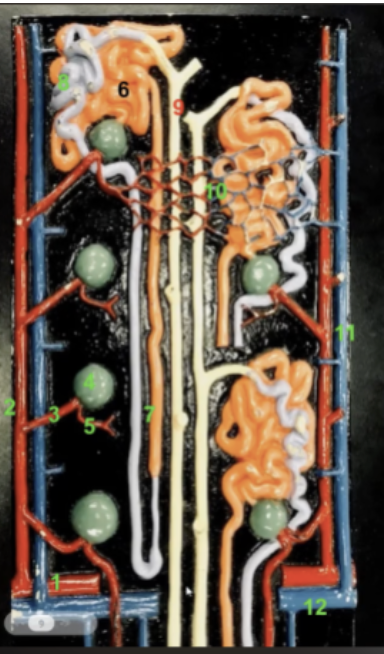
characteristics of 6
proximal convulated tubule
lined by simpled cubodial epithelium laden with microvilli
that with its long length give it a larger surface area
caries and modifies the flitrate at the glomerulus
Wrapped around the exterior of the PCT are the peritubular capillaries. What do these two do together
These work in tandem to perform the processes of reabsorption and secretion
explain reabsorption in the context of the PCT and peritubular capillaries
Any solute that was filtered at the glomerulus but should not be excreted in urine (i.e glucose) will be transported from the lumen of the PCT to the lumen of the neighboring peritubular capillary
explain secretion in the context of the PCT and peritubular capillaries
Any solute that was not filtered at the glomerulus but should be excreted in urine is transported from the lumen of the peritubular capillary to the lumen of the PCT
The filtrate that has been modified by reabsorption and secretion will exit the PCT and enter the
loop of henle
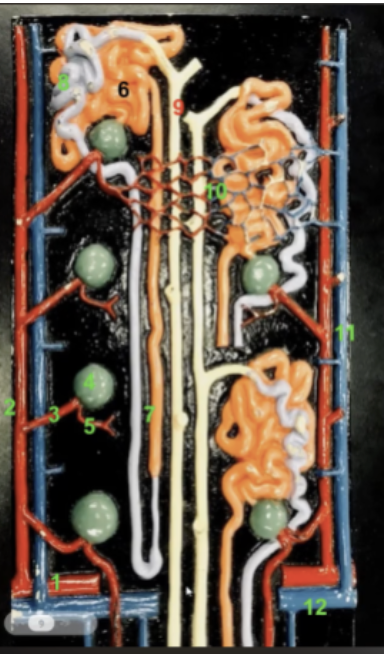
what is 7 and its function
loop of henle. hair pin turn. primarily Augments the kidney ability to concentrate urine. Helps us reabsorb water from urine to concentrate it
adjacent to the loop of henle are the
long straight capillaries of the vasa recta. They will work together to help concentrate urine
from the loop of henle, the filtrate will enter another tube to which the loop of henle connects to
distal convoluted tubules
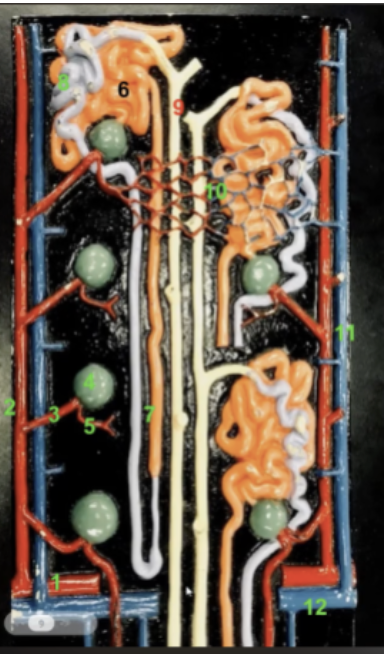
8 function
DCT. As flitrate flows through the DCT, its ionic content is modified as necessary
Multiple distant convoluted tubules will drain into a single
collecting duct
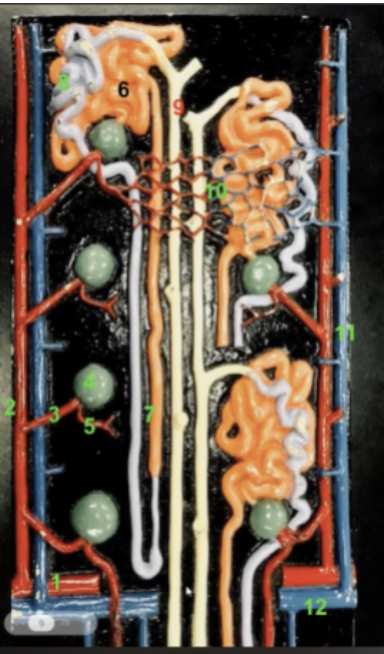
function of 9
the collecting ducts carry urine down through the medullary pyramoid and terminate at a renal papilla. The cells of collecting ducts will reabsorb water from urine as is necessary
The entire set of tubes carrying filtrate to the collecting duct is referred to as a
nephron
Each kidney has about 1 million nephrons and it is due to
their collective effort that blood is filtered and urine is produced
as filtrate flows from the glomerular capsule to the distal convoluted tubule:
a. its glucose content would _____
b. its water content would ____
c. its creatinine (a waste product would) ____
a. decrease
b. decrease
c. increase
why is the PCT epithelium so heavily endowed with microvilli
they provide the necessary surface area for the enamours amount of reabsorption that occurs
as blood flowed from an efferent arteriole to an interlobular vein
a. its glucose content would ____
b. its water content would ____
c. its creatinine (waste product) content would ___
a. increase
b. increase.
c. decrease
arrange the following in the correct order of the filtrate/urine flow
a. major calyx
b. pct
c. renal papilla
d. DCT
e. urethra
f. ureter
g. collecting duct
h. loop of henle
b → h → d → g → c → a → f → e
in each of the following situations, select the location with the greater hydrostatic pressure
A. glomerular capillary—glomerular capsule
b. distal convoluted tubule—loop of henle
c. minor calyx—major calyx
D. arcuate vein—interlobular vein
a. glomerular capillary
b. loop of henle
c. minor calyx
d. interlobular vein
many desert dwelling animals exhibit extremely long loops of henle. Why?
it allows them to super concentrate their urine which helps retain water. THis is necessary in an arid environment
what structures allow urination to be discontinuous even though urine production is continuous
urinary bladder and urethral sphincters
how could damage to podocytes affect the protein content of urine
it would decrease their filtering ability and larger molecules such as proteins could start appearing in urine
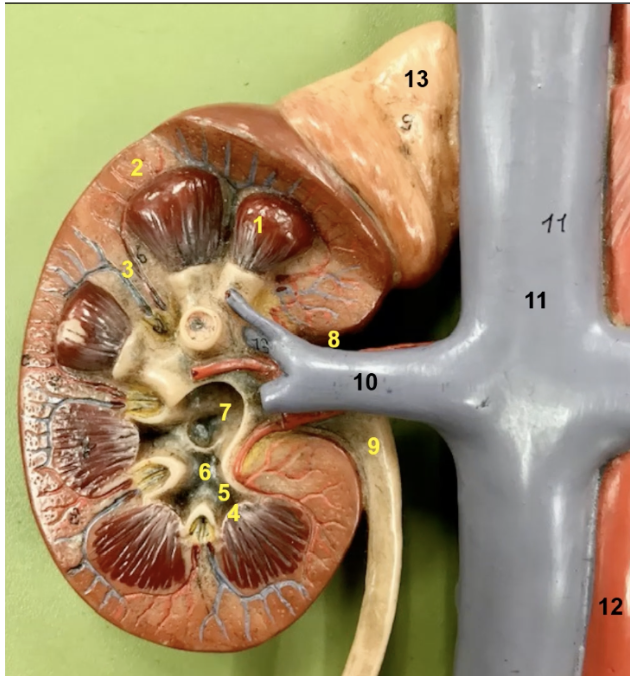
label
renal pyramids
renal cortex
renal columns
renal papilla
minor calyx
major calyx
renal pelvis
renal hilum
ureter
renal vein
inferior vena cava
abdominal aorta
site of urine formation
renal cortex. From there, urine flows through the renal pyramids and exits at each renal papilla. Then it goes to a minor calyx
ureter carries urine to the
urinary bladder
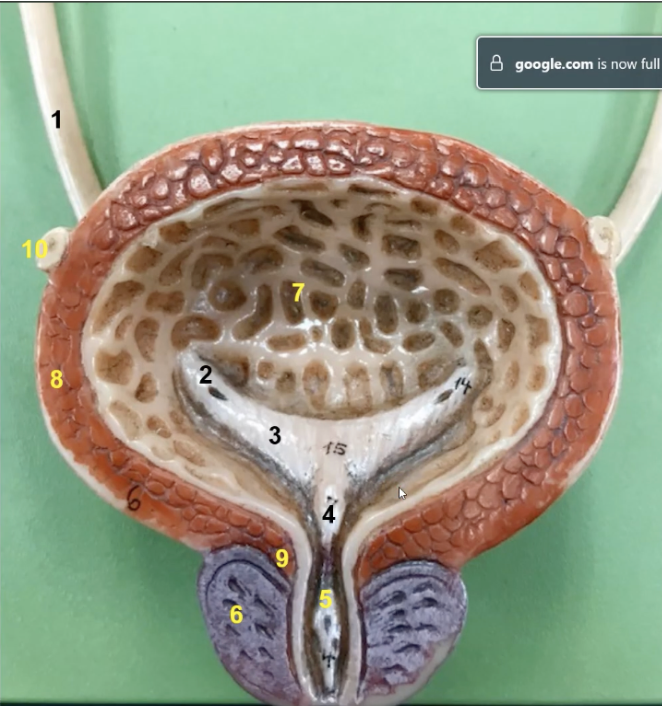
label
2 ureter
opening for ureters
trigone
internal urethral oriface
prostatic urethra
prostate gland
rugae
detrusor muscle
inter urethral sphincter
vas deferenes
prostatic urethra runs through the
prostate gland

label
adrenal gland
renal cortex
renal pyramid
renal papila
minor calyx
major calyx
renal pelvis
ureter
renal vein
renal artery
inferior vena cava
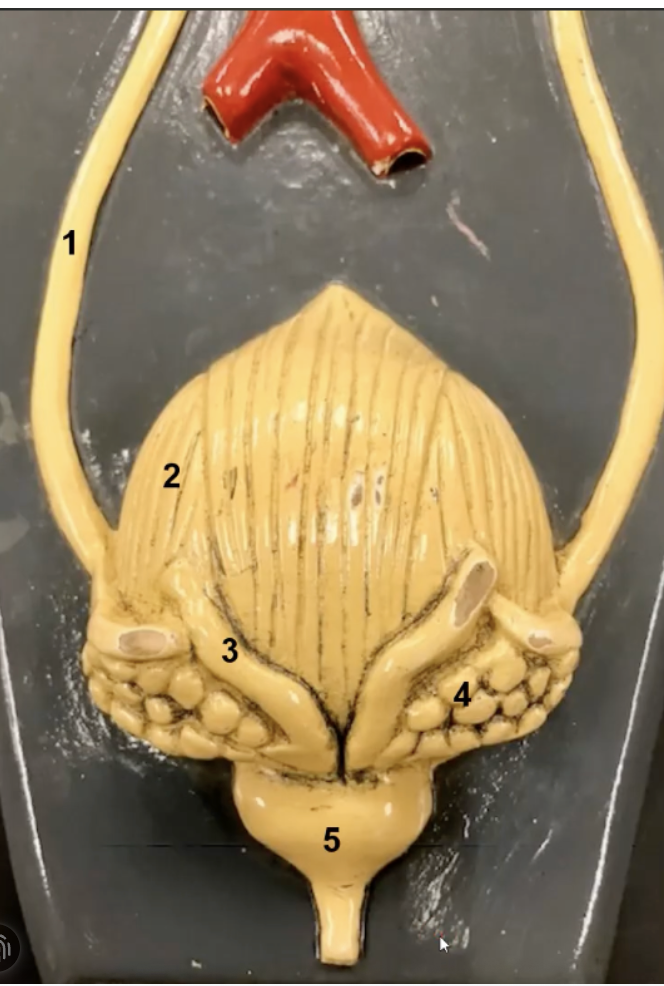
label
ureter
urinary bladder
vas deferens
seminal vessel
prostate gland
function of vas deferens, seminal vesicle, prostate gland
vas deferens → carries testicular fluid and sperm from testis
seminal vesicle → add seminal fluid
prostate gland → prostatic fluid
these three things make majority of fluid
seminal vesicle
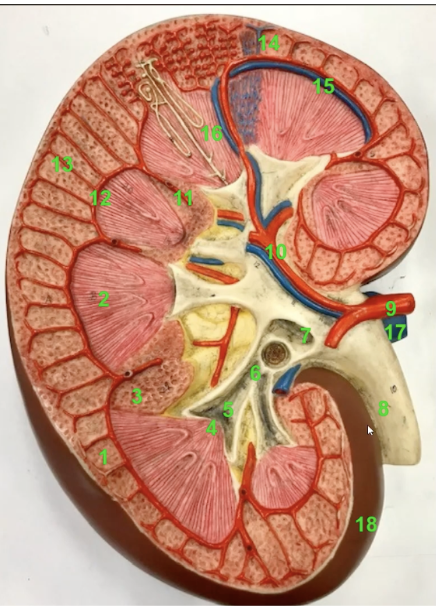
label
Renal cortex
Renal pyramid
Renal column
Renal papilla
Minor calyx
Major calynx
Renal pelvis
Ureter
We can trace blood flow through the major renal blood vessels
Renal artery
Segmental artery
Interlobar artery (runs between the pyramids)
Arcuate artery
Interlobular artery
Interlobular vein
Arcuate vein (+plus artery)
Interlobar vein
Renal vein
fibrous capsule
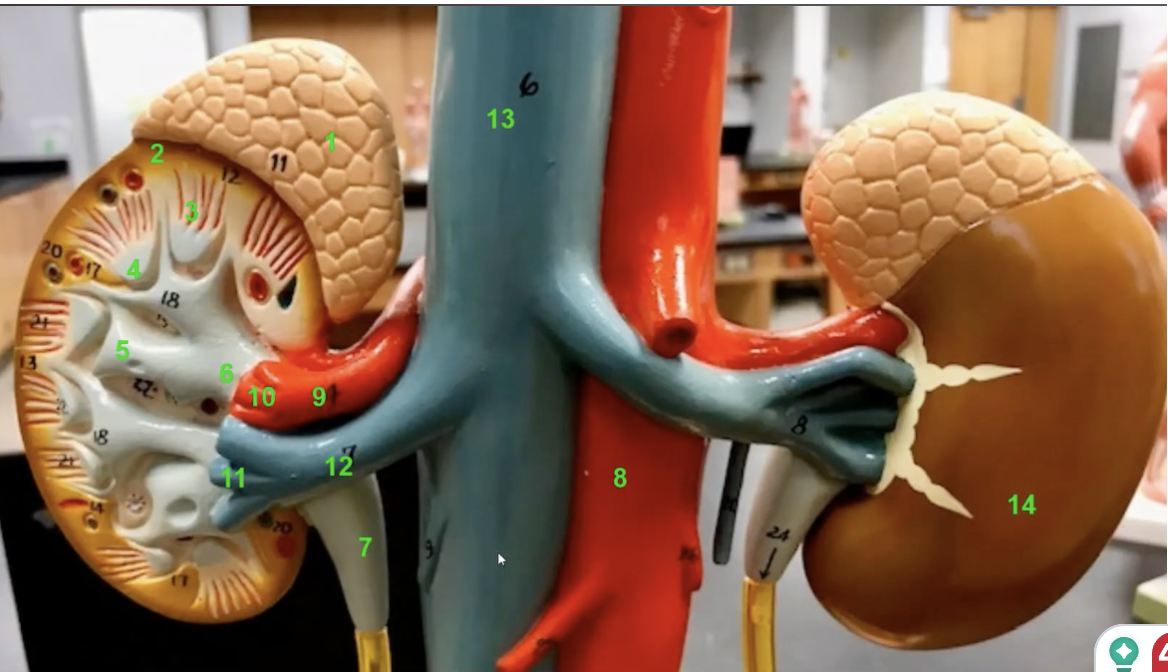
label
Adrenal gland
Renal cortex
Renal pyramid
Renal papila
Minor calyx
Renal pelvis
Ureter
Abdominal aorta
Renal artery
Segmental artery
Interlobar vein
Renal vein
Inferior vena cava
Fibrous capsule
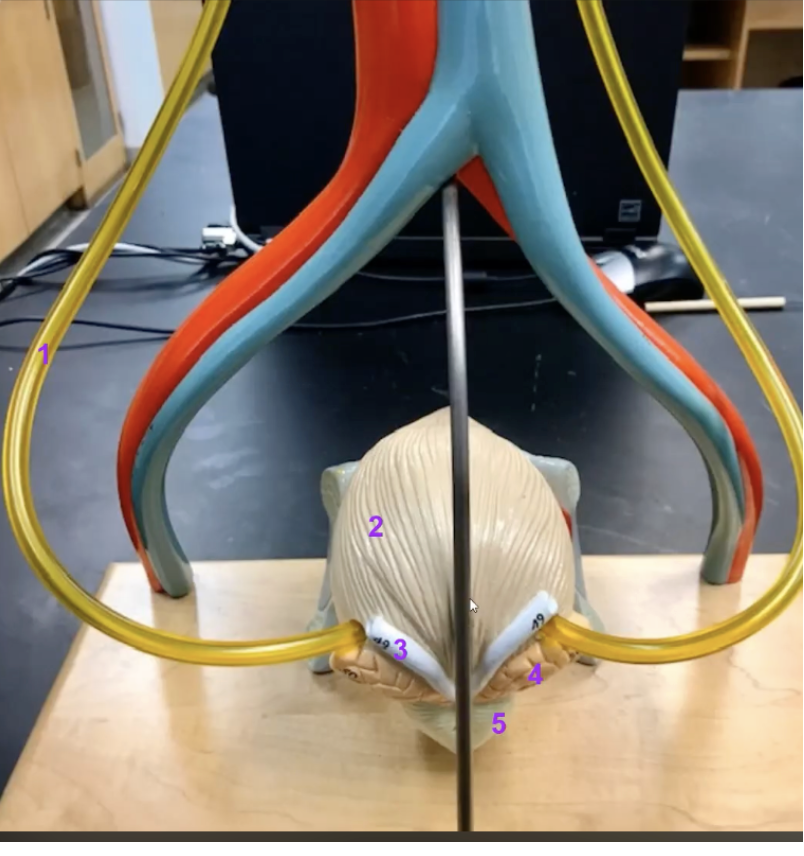
label
Ureter
Urinary bladder (posterior view)
Vas deferens
Seminal vesicle
Prostate gland

label
renal cortex
renal medulla
interlobar artery
arcuate artery
interlobular artery
afferent artiole
glomerulus
efferent arteriole
peritubular capillaries
vasa recta
interlobular vein
arcuate vein
interlobar vein
proximal convoluted tubule
loop of henle
distal convoluted tubule
collecting duct
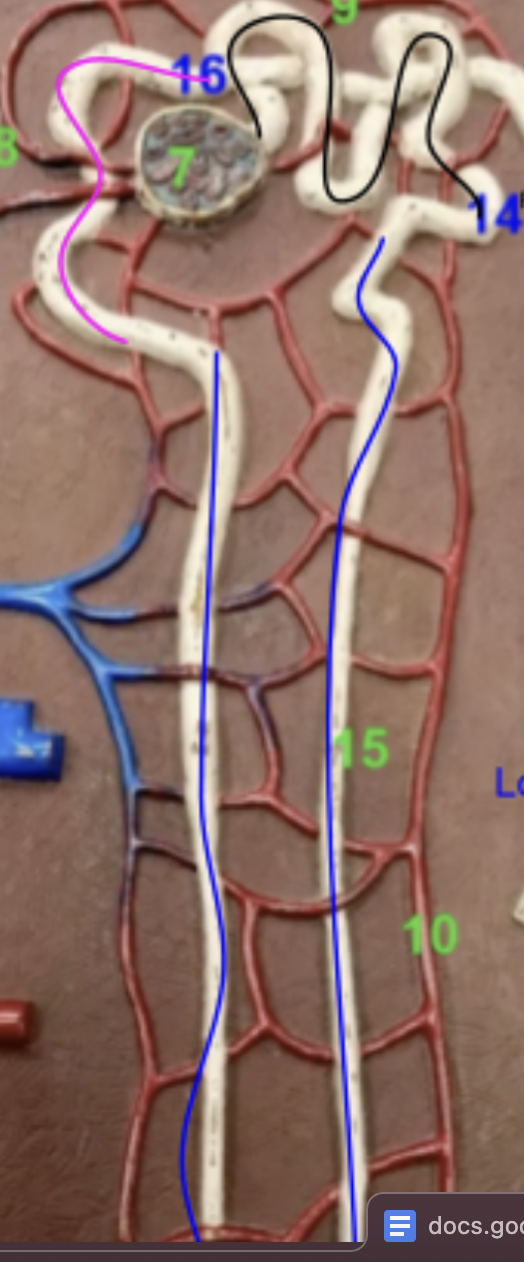
what is the color of each
black —> proximal contoluted tubule (connects to loop of henle)
blue → loop of henle
pink → distal convoluted tubule → connects to collecting duct