Patho Exam #3
1/30
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
31 Terms
protective structures of the pulmonary system
hairs
trap & remove foreign particles from the air
role of the mucosal lining
lines the airways & warms & humidifies the air
irritant receptors
in the nose and airway
recognize harmful agents
respond through sneeze or a cough reflex
expels foreign particles
immune protections
coating in the respiratory tract
ingest & remove bacteria through phagocytosis
inspiration
in air
expiration
out Co2
Ventilation impairments
diaphragm not working
Airway blockage/narrowing
anaphylaxis
ex. food blockage
Reduced Lung Compliance
Stiff Lungs
decreased expansion
pneumonia
rib fracture
Disrupted Nerve Signals (Brain/Nerve damage)
brain not signaling for expansion
pons, medulla = controlled breathing rate
chemoreceptors
ventilation compliance
distensibility (expandability) of the lung tissue and chest wall
ventilation resistance
the velocity & viscosity of the gas moving through the inner lumen of the airway
narrowing
mucous in the airway
adequate ventilation
appropriate lung compliance
measurement of ventilation
pulmonary function test
that measure lung volume, capacity, and air flow to diagnose conditions like asthma or COPD
tidal volume (TV)
vital capacity (VC)
forced vital capacity (FVC)
Forced expiratory volume in 1 second (FEV1)
Residual volume (RV)
Total lung capacity (TLC)
sum of VC & RV
tidal volume (TV)
an aspect of a pulmonary function test
vital capacity (VC)
diffusion
Gas exchange at alveolar capillary junctions
O2 in, CO2 out
Two major process
oxygen trying to get to all the cells
carbon dioxide is trying to escape
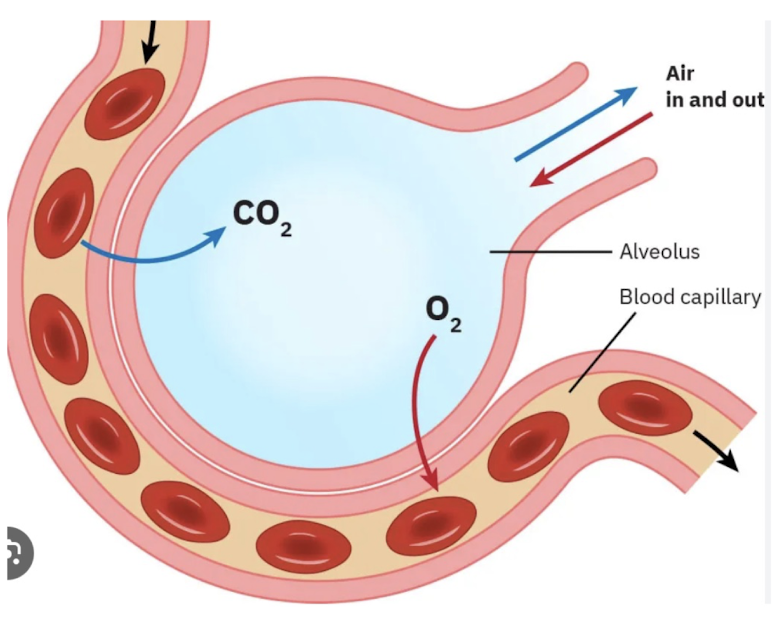
diffusion process: O2 moves in
enters lungs through inhalation
travels down to the alveoli
crosses into the blood via tiny capillaries
hemoglobin in the RBC picks up the O2 and carries it to the tissues
diffusion process": CO2 moves out
Co2 = waste product from metabolism
travels back through the blood to the lungs
Co2 cross from the blood into the alveoli & is exhaled
factors impacting diffusion
Pulmonary edema
fluid in the lungs
slows gas exchange
Emphysema
damaged alveoli
collapsed airway
collapsed alveoli
reduced surface area for diffusion
Anemia
low hemoglobin
not enough oxygen transport
Pneumonia
COPD
ARDS
Pulmonary fibrosis
Affect gas exchange
oxygen saturation (SaO2)
The percentage of hemoglobin that is carrying O2
Iron needed for O2 to bind
like a magnet
impaired diffusion
restricted transfer of O2 or CO2 across the alveolar capillary junction
Impaired ventilation (shunt)
inadequate oxygen coming into the lungs
Two major mechanisms
airway problems
neural problem
impaired perfusion (dead space)
inadequate blood flow to the lungs
PE
Low BP
Severe blood loss (hypovolemic shock)
impaired ventilation-perfusion (V/Q) mismatch
lungs are ventilated, but not perfused (dead space)
ex. PE
lungs are perfused, but not ventilated (shunt)
ex. pneumonia, atelectasis
hypoxemia
decreased oxygen in the arterial blood
hypoxia
oxygen deprivation in cells
prolonged hypoxia leads to cellular death
development of metabolic acidosis
hypercapnia
increased carbon dioxide in the blood
air trapping
retention of CO2
COPD
respiratory acidosis
crackles
fluid in the lungs
alveoli or small airways collapse during exhalation
wheezing
narrowed airways
airways are narrowed by swelling, mucus, or muscle construction
air has to squeeze through tight passages
orthopnea
SOB when lying flat, relieved when sitting up
dyspnea
difficulty breathing, sensation of not getting enough air
mechanisms of altered elimintation
Altered patency
Bowel obstruction
Altered motility
increased or decreased peristalsis
Altered neuromuscular
Spinal cord injury
Altered perfusion