Week 1: The Membrane
1/61
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
62 Terms
The cell membrane
what is it composed of
what can go through the membrane without help
What cannot go through (impermeable)
the cell membrane is composed of phospholipids
lipid-soluble molecules and gases can go through the membrane without help
Impermeable to organic anions (proteins)
Membrane permeability
What factors affect permeability: 3 factors
Definitions of permeable
What is not permeable and what 2 things can help them cross
The size, lipid solubility and charge of the molecule
Bigger size cannot get through
Charges cannot get through
More lipid-soluble molecules can get through
Permeable: something that can be able to go through the membrane by ANY MEANS (either diffusing or without help)
Gasses are diffusable
Polar molecules and ions need protein channels or carriers to cross
Types of diffusion
name them only
2 types
Simple diffusion
Facilitated Diffusion
Simple diffusion
what molecules can do this
How does simple diffusion work
What direction does it move?
What is proportional to its rate of diffusion?
What is not required for this diffusion
Is the process continuous or discontinuous?
lipid soluble and small molecules and gasses can do this
Through pores or pass directly through the lipid bilayer
Process
Goes directly through the lipid bilayer or through pores
Goes down the concentration gradient
The greater the gradient the faster the rate of diffusion (proportional)
No ATP/energy required
Facilitated Diffusion
How is it similar to the simple diffusion (2 factors)
What makes it different from simple diffusion (2 factors)
Explain the process of facilitated diffusion (3 steps)
Explain what transport system saturating is and why does it happen?
Is the process continuous or discontinuous?
Similar to the simple diffusion
No energy is required from ATP
Goes down the concentration gradient
Different from simple diffusion
Transports specific molecules
Involves an assistance of a carrier protein
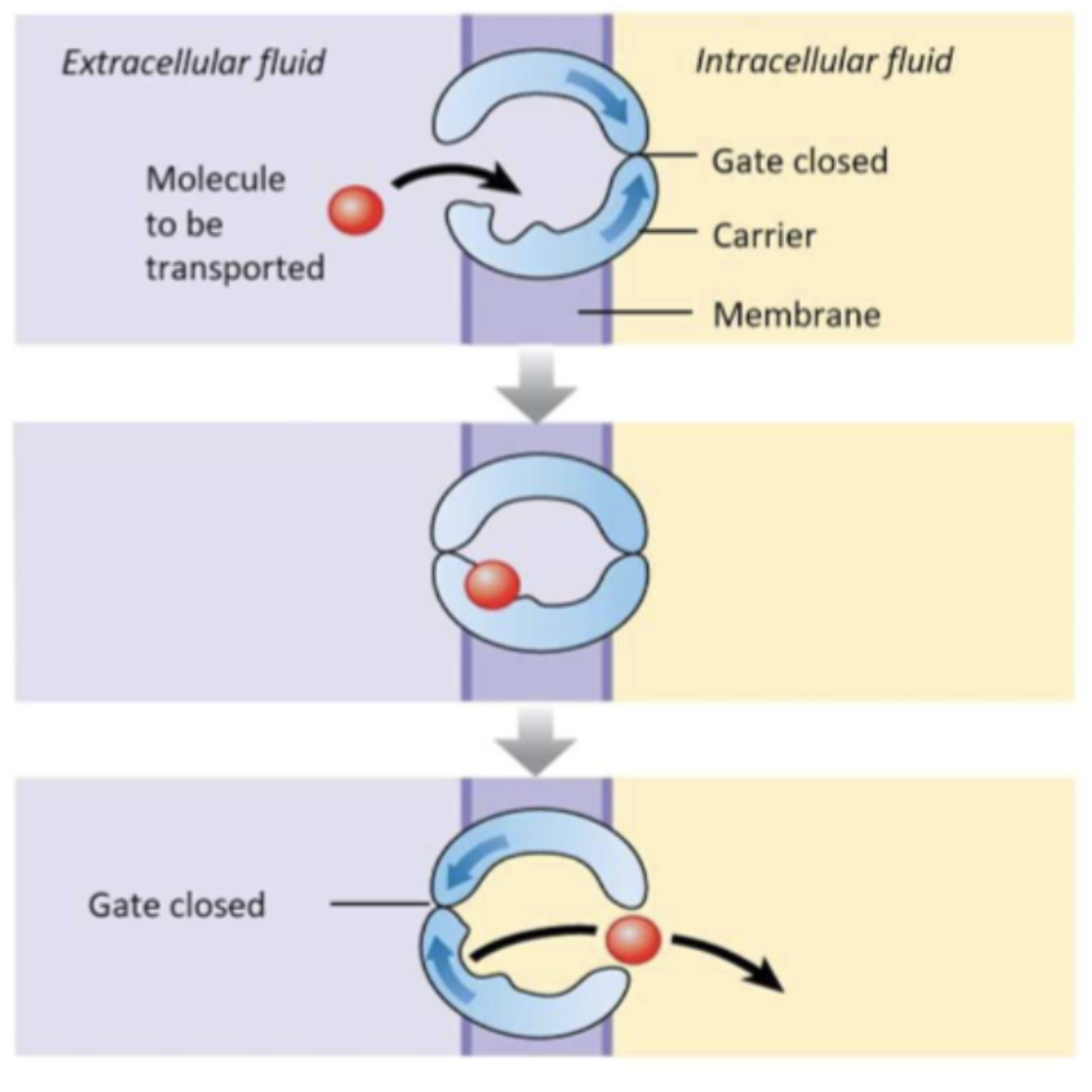
Step of facilitated diffusion
Molecule binds to the carrier protein
Carrier protein undergoes a conformational change
The change allows the translocation of the molecule to the other side
Transport system can be saturating
This when there is too must molecule that needs to be transported than there are carrier proteins
Molecules must wait until the transporters can do their job
Process is discontinuous
Primary Active transport
What does the molecules move
What does it require that makes it different from diffusion
how is it similar to facilitated diffusion (2 factors)
Give a common example of a facilitated diffusion
Molecules move against the gradient
Requires ATP hydrolysis/catabolism to produce energy
Similar to facilitated diffusion
Will move specific molecules: selective
Molecules binding to the carrier protein will result in a conformational change
ATPases (na+/K+ pump)
Secondary Active Transport
How does the molecule move through the gradient
What doesn’t need compared to primary active transport
Instead what else does it use instead to power the transportation (what does it depend on and what happens to the protein)
Against the gradient
Does not need ATP hydrolysis
Process
Secondary = 2 solutes
Dependent on the primary active transport: One down the gradient simultaneously power the movement of another solute up the gradient
Proteins undergoes conformational change during binding of substance/ions
Gated channels
What forms the channel and what is this also called
What is a pore loop what does it do
What is a gate?
What are the 2 types of gates
Explain what is required for each gate to open
how does it open (explain what happens to the protein)
4-5 subunits of membrane spanning proteins forms pores
A pore loop is inside the membrane
Function: creates a selectivity filter
Gate: a protein that functions to either close or open the channel under certain conditions by changing between two shapes
Types
Ligand Gated
the binding of a chemical agent to a receptor (part of the chemical signalling ) to trigger events like an activation of an enzyme or a ion channel to open
very important for synaptic transmission
Voltage gated
Voltage gradient causes channels to undergo conformational change to create an open pore
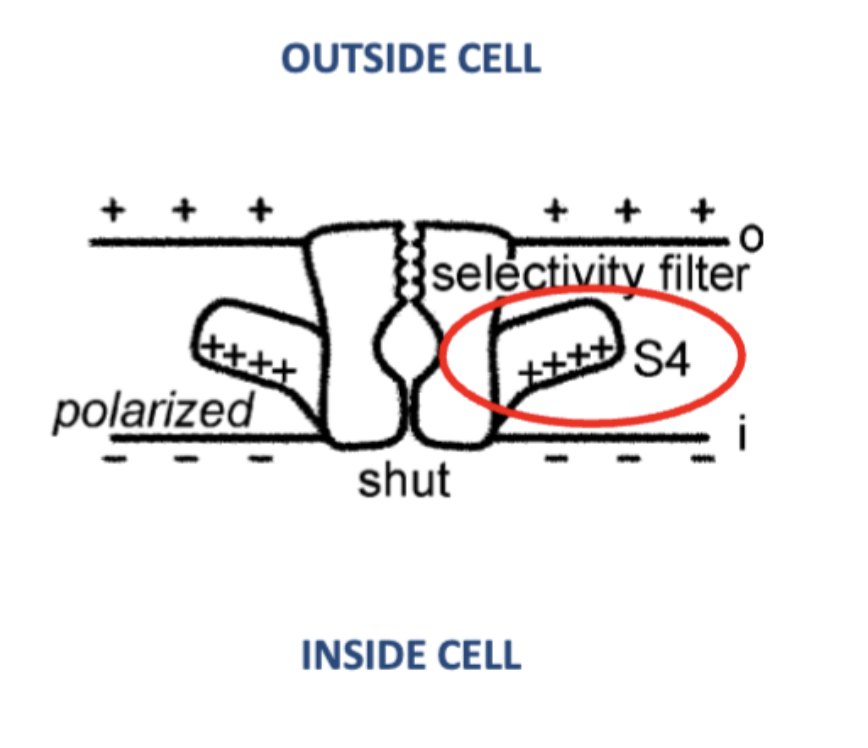
Use of the s4 segment of the protein
Positively charged attracted to the negatively charged inner membrane surface to close the pore (-70 mV)
However depolarization (-50 mV inside) is not enough attract and the wings move towards the outer membrane and allows the pore to open
Endocytosis
In one sentence describe endocytosis
What mediates this process and why?
the inwards pinching of the membrane to form a vesicle
Receptor mediated to allow the capture of specific proteins to the inside of the cell
Exocytosis
main definition
Types of exocytosis
What occurs at each type
What is the purpose of each type (when does this occur)
What is the require for the more greater exocytosis type
def: The partial/complete fusion of vesicles to the membrane for bulk trans-membrane transport of specific molecules
Inside to outside
Intracellular materials to the secreted or delivered to the membrane
Exocytosis 1: Kiss and Run - fast mechanism
Dock and fuse at specific locations called fusion pores
Connecting and disconnecting multiple times before fully emptied (each kiss only releases a bit of contents)
Low rate of signaling - slow because doing it multiple times
Exocytosis 2: Full Exocytosis
The complete fusion to the membrane
Releasing all contents at once
Purpose: for delivery of membrane proteins and higher levels of signalling
Membrane will become too big and contents inside don’t change so must be counterbalanced by endocytosis to stabilize the surface area
What do all cells generate?
What do all cells have?
membrane potential
have na+/K+ pumps
What two conditions are required for membrane potential
Create concentration gradient: enzyme ion pumps actively transports selected ions across membrane to form the gradient
Sem-permeable membrane: membrane must be able to diffuse a certain ions than others
After these 2 conditions the movement down the concentrations gradient will create an electrical gradient
Why is Na+/K+ pumps important?
What does the pumps require in order to function (recall active transport)
How much and movement of Na+ and K+ for each time
How much energy out of the entire body is needed
Overall voltage with just pumps
All cells have Na+/K+ pumps to generate MP
The Na+/K+ depends on ATPase enzyme to functions: (Na+ moves out of the cell, K+ into the cell through the breaking of ATP)
One ATP broken = 3 NA out and 2 K in
⅓ of energy of the body needs in this process
Overall -10 mV inside due to only this pump (more + ions out which makes sense)
K+ channels
purpose of K+ channels (recall the voltage of the Na+/K+ pumps vs usually voltage gradient in resting potential)
How does K+ work?
How does the diffusion work
How does the diffusion stop
Due to the increase of K+ ions inside the cell, K+ channels help in the diffusion of K+ ions out of the cell and down concentration gradient
This will stop when the diffusion of K+ is prevented by the electromagnetic force of the membrane (very high positively charged surface area of the membrane prevent K+ from entering)
With both na+/K+ pumps and K+ channels, what is the resting membrane potential of the cell
give number of the voltage
Also explain what causes this number to occur (explain the movement of ions)
-70 mV
the movement of na+ and K+ ions to move out
Equilibrium Potential
what happens when the equilibrium potential is reached
What factors determines equilibrium potential
The cation diffusion to the outside is balanced by the cation being pushed inwards due to the overall negative charge inside the cell
Mainly determined by the concentration gradient
The Nernst Equation
What does this equation describe
What doe the results indicate
One condition it must follow for the equation results to be accurate
Example of K+ equilibrium potential
What is the results number and is it accurate, if not why?
Describes the diffusion and the electrochemical repulsion force
The results describes the inside potential difference compared to the outside
Result will only make sense if there is only one ion involved
E.g. K+ Equilibrium Potential
EK+ = (RT/F) ln([K+]o /[K+]i) = -90 mV (equilibrium potential for K+)
However, usually the cell is -70 to -80 mV
From the Ernest equation previous lecture, for K+ ions the resting membrane is calculated as -90 mV (however it is not)
Reason
Rest: K+ is most permeable, Na+ and Cl- somewhat diffusing (low permeability) at the same time
Solution: expand the Ernest equation to the Goldman Equation
Goldman Equation Sample
P represents the permeability coefficient
T is temp
R is gas constant
F is the Faraway constant
[]o: concentration out
[]i: concentration in
![<ul><li><p><span style="background-color: transparent;">P represents the permeability coefficient</span></p></li><li><p><span style="background-color: transparent;">T is temp</span></p></li><li><p><span style="background-color: transparent;">R is gas constant</span></p></li><li><p><span style="background-color: transparent;">F is the Faraway constant</span></p></li><li><p><span style="background-color: transparent;">[]o: concentration out</span></p></li><li><p><span style="background-color: transparent;">[]i: concentration in</span></p></li></ul><p></p>](https://assets.knowt.com/user-attachments/ee11f93d-8f54-4d77-9637-c97df347a345.png)
Na+ Equilibrium Potential
what is the movement of Na+
When it reaches equilibrium what happens to the movement (explain why it stops)
Provide equilibrium potential for na+
If the membrane properties change to make the membrane most permeability to Na+, the Na+ will go in (influx), with an net cation accumulation inside to make the membrane potential positive
ENa+ = +60 mV
Cl- Ions
Movement of the cl- ions and why? (what is mainly inside/out of the cell that causes this movement)
Large proteins are located on the inside, the ions are only moving outside to the EC space
Overall negative concentration outside
Not due to active pump; due to anion proteins
Na+ Channels
what is the important of Na+ channels?
What type of gated channel is Na+?
Explain the process of the gate opening and closing as well as following the voltage of the inner membrane
to generate a membrane potential
Membrane increases conductance (permeability for that ion), Na+ channels are open only for Na+
Voltage gated channel
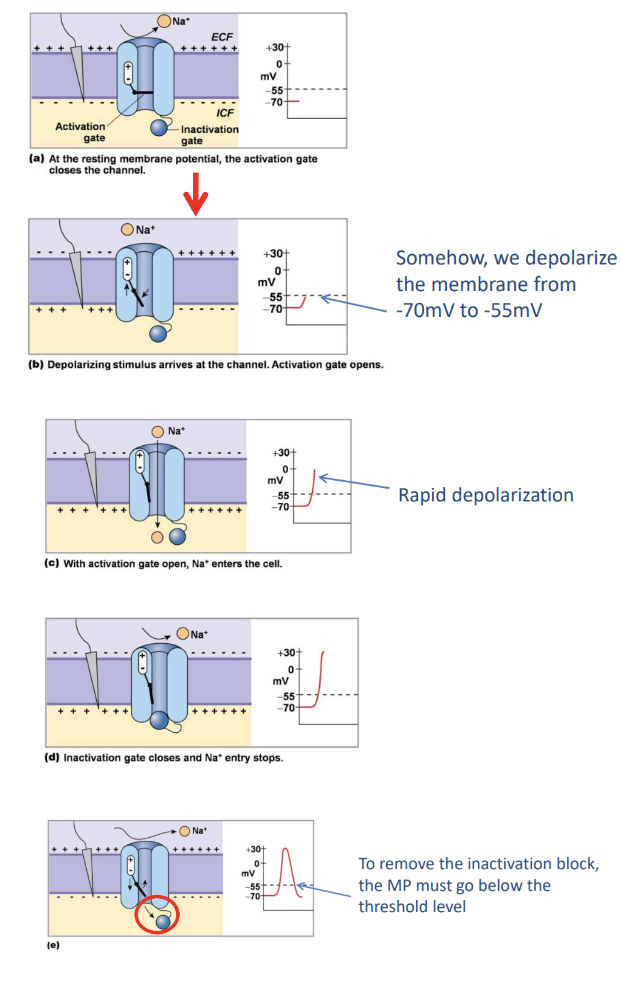
Resting MP, the channel is shut at -70 mV
Depolarize (less negative inside the cell) to open the channel! Depolarize to about -55 mV to open and close two types of gate
Activation Gate opens to allow Na+
Rapid depolarization
Inactivation Gate closes and Na+ entry as well as rapid depolarization
The gate is only removed once membrane potential goes back to threshold level (-55 mV)
Action Potential
main definition
Excitable definition for a membrane
A short lived change in MP, used as a signal
Can only be produced if there is voltage-gated Na+ channels in the membrane - therefore the membrane is ‘exitable’
Process
Na+ channels open, MP goes to ENa+ = 60 mV
Rapidly inactivates
When Na+ channels closes, the restoration of resting MP is only due to the leaking of K+ through K+ channels (K+ moves from in to outside EC fluid)
Threshold
What is the threshold for the action potential
What is regenerative mechanism? (relates to Na+ channels)
Stimulus required to have a minimum depolarization to induce regenerative mechanism for the opening of Na+ channels
Regenerative mechanism: depolarization causes Na+ channels open, Na+ to move in, depolarizes more which opens even more Na+ channels
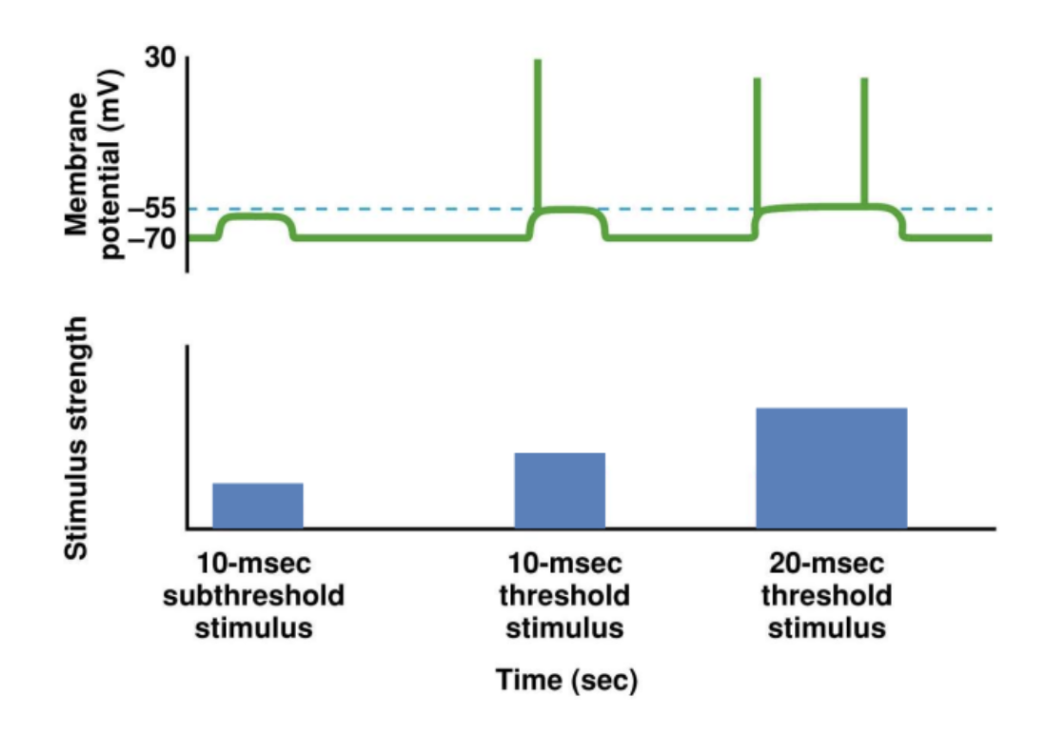
All or None Principle
quality of stimulus vs the magnitude of the potential
Name the two types of stimulus to results in a potential
What (name it) type of stimulus does not result in a potential
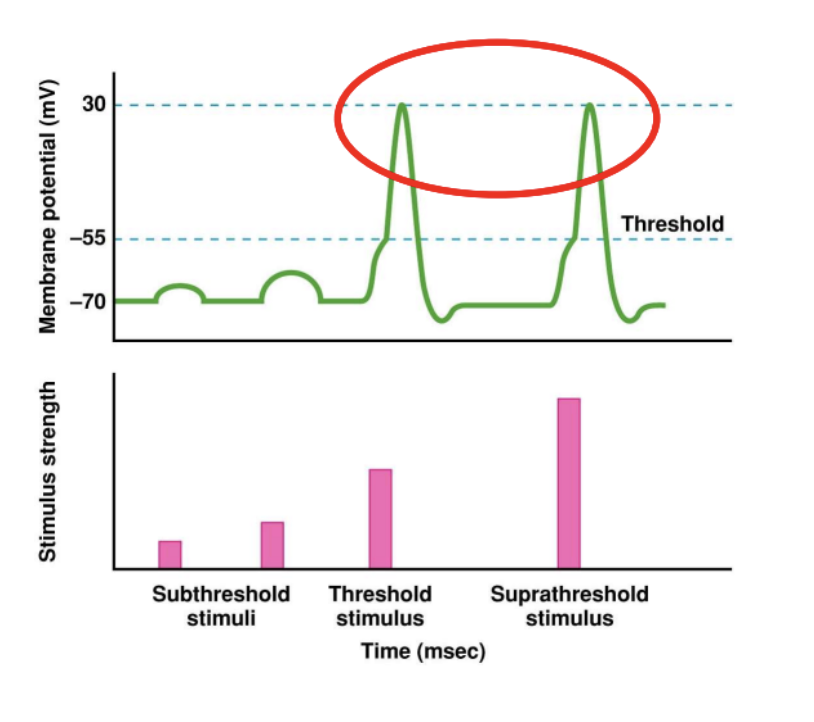
Threshold and supra threshold stimulus will result in the same action potential magnitude
Subthreshold does not result in an action potential
Frequency Coding
What is frequency coding
What does the frequency indicate about?
To code the information about the intensity of the stimulus, it is done through the changes of frequency of AP
Greater stimulus = greater frequency
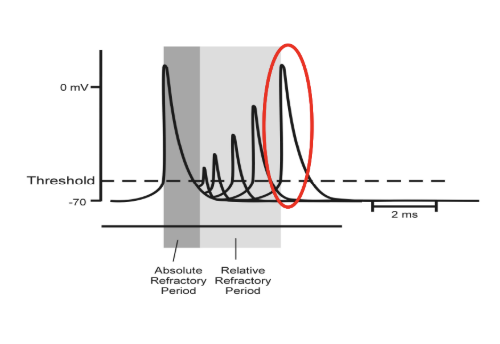
Refractory Periods
What are refractory periods
What happens during refractory periods
What are the 2 types of refractory periods
Draw a diagram of a refractory period
When action potential is generated, the Na+ channels are closed due to the inactivation gate, however the two types of gates need to reconfigure to their original form for the membrane to be ‘excited’
Types of refractory periods
Absolute RP: no channels are reconfigured and therefore no secondary actions potential
Relative RP: some but not all channels are reconfigured, the channels that are reconfigured are able to produce another AP right after
Depolarization Block
How can we create a depolarization block
What is the purpose of this?
What is the voltage of a depolarization block
Explain the process to create a depolarization block
Keep the membrane depolarized, keep at 20 mV
This prevents the Na+ channels from undergoing reconfiguration back to its original state
Process
Prevent the K+ channel from leaking K+ ions out of the cell
Destroy the gradient by introducing more K+ into the extracellular space (KCl injection)
Remains in absolute refractory state and membrane is in-excitable
After-Hyperpolarization
What helps with hyper polarization
What is the max voltage it can reach?
More polarized due to the extra K+ voltage-gated channels which flow K+ ions outwards
Even more polarized then resting potential
Possibly repolarized to -80 mV
Impulse Conditions
hint: What is impulsing
What occurs during the impulse
Due to action potential, does the reverse of of the potential difference across the membrane (- inside to + inside)
Source of the depolarizing current to the adjacent membrane and Na+ channels opened in the adjacent
Therefore, AP propagates across the entire membrane/cell
Excitable Cells
is there many or very few cells that are exitable?
Explain why
If not, explain what else they do? (recall all cells have membrane potential)
Which type of cell is usually excitable and explain why
What is the issue of action potential travelling long distances? (propagating)
Explain the solution (what is it called: hint: think of something that looks like an axon in real life)
What affects the speed of action potential
What two properties are useful to adjust to solve the issue
Most cells are not ‘excited’ due to the lack of Na+ voltage-gated channels
Don’t produce APs, instead conduct passive currents because their main goal is to not carrying a signal across a distance
Only neurons with long axons will generate propagating action potentials
Issue with propagating action potentials
Signals start to get weaker the longer the AP travels across the membrane
Solution:
Cable Properties
Length constant 𝜆 and will measure how quickly the potential difference disappear as a function of distance
Conduction velocity of an AP depends on the 𝜆
Main useful properties to increase 𝜆 (current or voltage)
Increase diameter to decrease internal resistance and the lost of voltage
Increase the membrane resistance to get less current leaking out
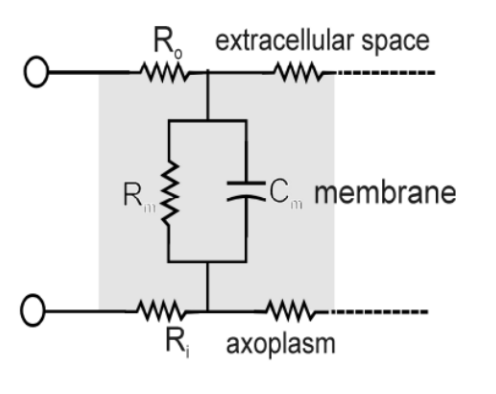
Length Constant
what three factors define length constant
Which one is removed?
What does the calculation results tell you? (1 correlation)
If you were to change the value of the length constant, how would you, and why would you?
What is the equation (hint: use the picture provided)
Defined by the internal resistance, EC fluid resistance and membrane resistance
However EC fluid resistance removed from calculates as its not easily adjustable
Defined to calculate the the distance you can travel until the voltage drops 37% of its original value
Ideally, increasing 𝜆 is good so the depolarizing current travels a long distance
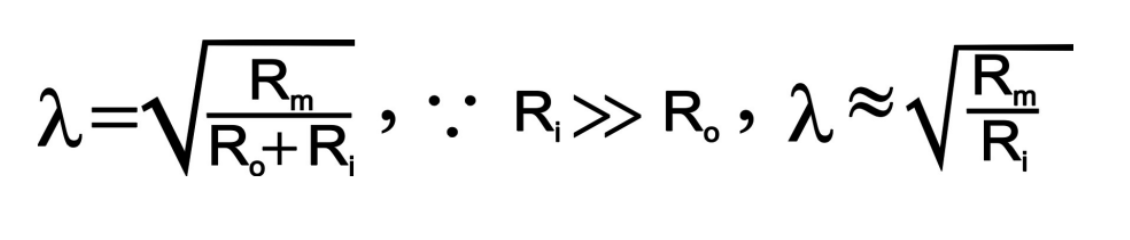
Myelination
how do you increase conduction velocity (one thing)
Give an example in the nervous system
What is the places called when they are not mylinated in the nervous system
what is the disease called that affects myelination? What happens in this disease
Increasing membrane resistance the easiest way to increase conduction velocity
E.g. specialized ‘glial’ cells or Schwann cells assists the peripheral nervous system (for the central nervous system it is the oligodendrocyte) through this way by wrapping themselves 50-100 layers around the axon to form a myelin sheath to increase membrane resistance and prevent leakage of current between nodes
Nodes of Ranvier: places where the axon is not myelinated (myelinated in sections)
Issue: multiple sclerosis
The nervous system will attack the myelin and gets damaged
Saltatory Conduction
What areas in the axon can produce action potential and why
What is this conduction movement called
For this movement, how far can it travel (in terms of the next APs)
What is the advantage of having this movement
What type of membrane potential is happening in the areas that cannot produce action potential?
Only axons that are exposed are excitable and can generate AP because only those areas are where the exposed Na+ channels are, in between are not generating AP
Known as the jumping mode of conduction
One AP can generate APs for the next 5-10 nodes to -55 mV
10th node of each section will serve as the depolarizing force for the next 10
**note that even if the first 2 nodes are damaged, AP can still travel to the next healthy node or unmyelinated axon (doesn’t stop the track)
Between nodes is passive currents
Unmylienated Axons
What is the disadvantage of this
What is the advantage of this
Which wins for most axons?
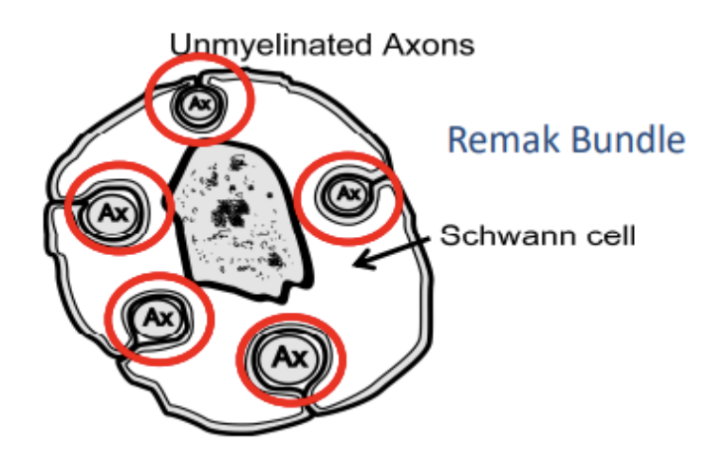
What is a remak bundle?
What type of glial cell can do this
Bad because
Lots of current leakage and slows down conductance velocity (speed of conductance) due to small axon diameter and low membrane resistance
Good because
Lots of Na+ and K+ are found in these area
Overall: many axons are unmyelinated
***Remak Bundle AXON IS STILL surrounded by schwann cell and oligodendrocyte but on only for insulation and no winding
Axon Terminal
what happens to the membrane potential conduction at the exon terminal
Why doesn’t it go backwards (recall what is required for the next AP)
Conduction ends at the axon terminal
Reason it cannot go backwards: the Na+ channels are still inactivated during the refractory period so the current just dies out
Synapses
Give the main definition
Only list the two types of synapses
Functional association of a neuron with another neuron or effector organs (muscle/gland)
Types of synapses
Electrical
Chemical
Electrical synapse
What are they known as
How far apart are neighbouring membranes
What are they bridged by and what is their function (what is transferring in between the membranes (2 types))
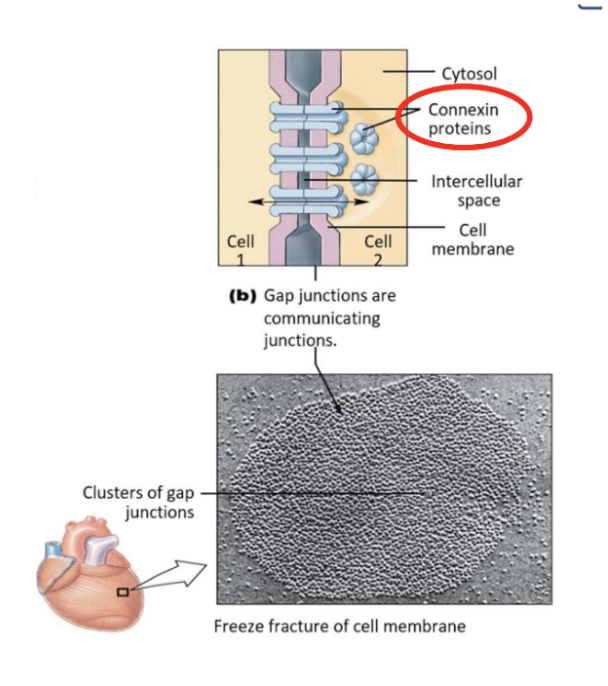
Known as gap junctions
Adjacent membranes 35Å apart and bridged by Connexins transmembrane proteins allowing small ions and depolarization to cross
Chemical Synapse
What is transferring in between the membranes
What is the membrane called that releases it
What is the membrane called when it receives it?
How far apart is the neighbouring membranes
Explain how the transferring in the chemical synapse works
3 steps
Explain why this doesn’t always work? Give statistics
What is being prepared before chemical synapse transfer occurs
Transmitter released between the EC space between membranes
Presynaptic membrane: Where the membrane released the transmitter and the surface is known as the bouton containing the vesicles
Post Synaptic Membrane: receives the neurotransmitters through binding with the specific protein receptors located on this membrane
About 200 Å apart
Processing station
Boutons filled with vesicles of neurotransmitters
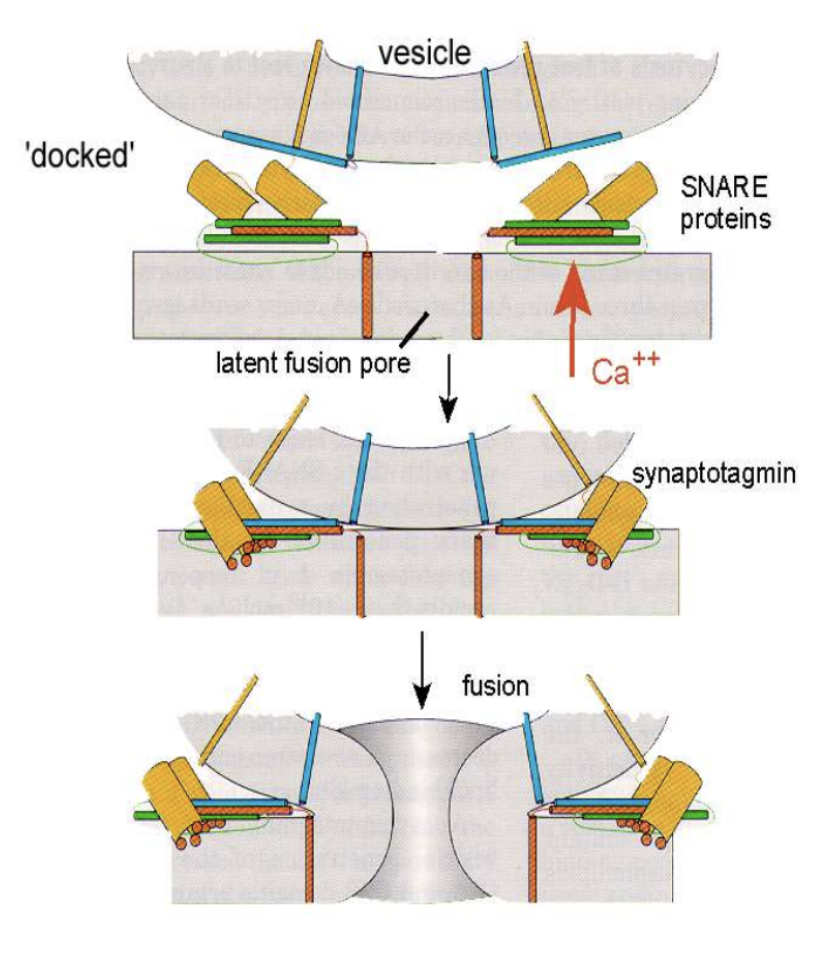
Once the terminal gets depolarises the voltage gated Ca+ channels open and allow Ca in the terminal and the depolarizes the cell to -50 mV; this trigger the exocytosis (can be either kiss or run or full exocytosis) of the vesicles synaptic contents and these will bind to the postsynaptic cell
Binding of the neurotransmitters will trigger a response in the cell
**releasing vesicles are only probabilistic: 1 AP will have a 10-90% chance to releasing neurotransmitters
Vesicles are already lined up with the presynaptic surface with the help of SNARE proteins located on the cell’s membrane
Post-Synaptic Receptor
What is this receptor? Where is it located
What happens when the neurotransmitter binds to it?
Why is the receptor more important than the neurotransmitter?
List two types of receptor effects
Neurotransmitters diffuse and bind to the receptor protein in the postsynaptic membrane which then changes the shape of the protein
** the receptor are responsible for what happens or the effects, not the neurotransmitter (that why we can have different neurotransmitter e.g. man made to do something)
Types of receptor effects
Ionotropic effect
Metabotropic effects
Ionotropic
*____ binds to ____
Types of *___
four types
Are they only limited to ionotropic things?
What is post-synaptic potential
How long is this potential about?
Two types of PSP (two types of ions for each)
Give an example (hint: nicotine)
Ligand binds results in opening of an ion channel
Types of ligzands **all these ligands can also bind to the metabotropic receptor (this is why it’s very important to know that the receptor is what effects everything)
Ach: Acetylcoline
Glutamate
GABA
Glycine
Post-Synaptic Potential: Because of the opening of ion channels results in the change of the post-synaptic membrane potential
Time: 20-40 ms (as long of the neurotransmitters are still there)
Specificity
EPSP (excitatory): for depolarizing (Na+, K+)
IPSP (inhibitory): for hyperpolarizing (K+ or Cl-)
E.g. nicotinic receptor for Acetylcholine (neurotransmitter)
Metabotropic
Main definition
__ binds to ___
Explain what happens after the binding (2 possible things that could happen)
Give the types of things released for the 2nd type
Types of ___ (6 kinds)
Explain one specific neurotransmitter and effects (B-Adrenoreceptor)
What is it commonly used for
(initiates a metabolic cascade to activate an enzyme)
The ligand binds to the receptor, then activates the enzymes that is G-protein coupled
Types of ligands
ACh: Muscarinic receptor
Peptides: B-endorphin, ADH, substance P
Catecholamines: noradrenaline, dopamine
Serotonin
Purines: adenosine, ATP
Gases: NO, CO
Enzyme either increases production or destroys 2nd messengers (to the next enzyme)
2nd messengers then activate other enzymes
**********cAMP, cGMP, InP3
Example: phosphokinases will phosphorylates membrane protein and other proteins which will modify their ion currents
Example of metabolic receptor and their effect: B-Adrenoreceptor
Neurotransmitter: Noradrenalin (NA)
Activates adenylyl cyclase through the G-protein alteration
Increase production of cAMP
cAMP activates kinases that phosphorylates Ca++ chanell
Increase Ca++ influx
Commonly for beta-blockers (help heart muscles and increase contractility)
Main difference between two effects (ionotropic vs metabotropic)
Speed of effect
Membrane potential
Change of membrane potential
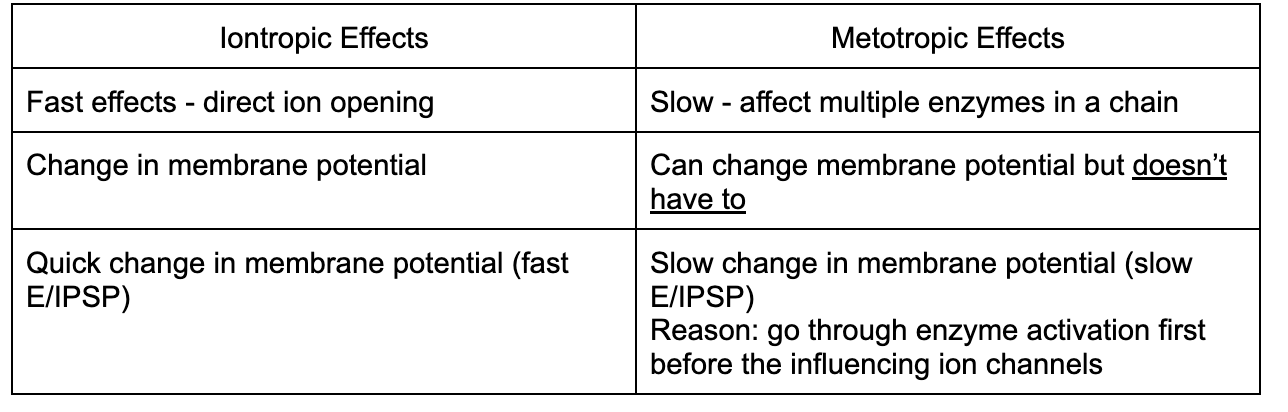

Spread of PSP
when does spread of PSP occurs
In what are of the neuron does it occur in?
What does it not generate
Where does PSP go to?
What is this area called?
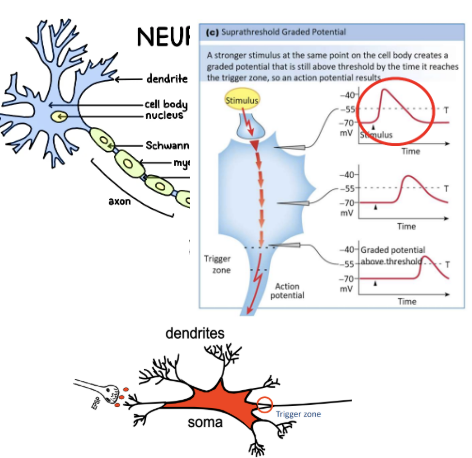
Generated in area with a lack of voltage-gated Na+ channels (inexcitable membranes)
Neuronal dendrites and cell bodies
**do not initiate an AP, only generates passive conduction
Will travel to the nearest excitable membrane Trigger Zone (at the beginning of the axon)
PSP Summations
Why do we have PSP summations (what is the issue if we did not have this?)
What are the two types of summations?
Explain each type and how they can create AP
The loss of current/potential before reaching the trigger zone
Types of summation
Spatial Summation
Multiple synchronous EPSPs all reach the trigger zone at the same time to create a suprathreshold
Temporal Summation
Strong EPSPs and last about 30-40 ms before dying out
Successive input (not all at once) on any synapse generates subsequent APSES that add on to pre-existing EPSP that, within a short period of time (e.g. 10 ms apart), can sum up to create a AP
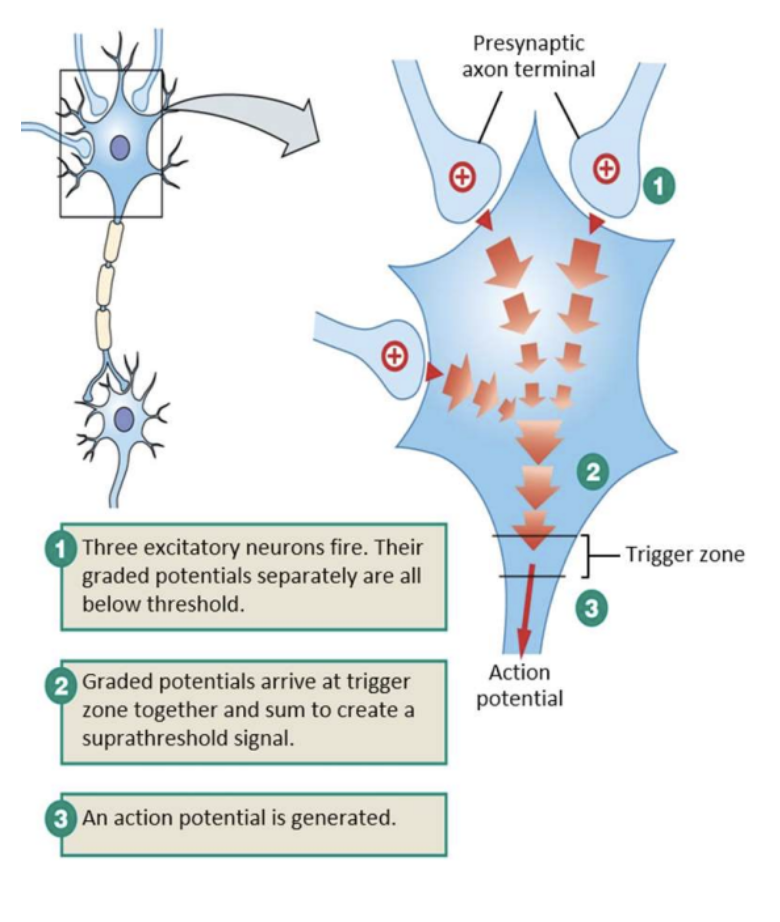
Inhibitory Post-Synaptic Potential
where is it located?
What is the advantage of the location
In which cells is it more commonly found in and why would it be important there?
Explain the process of inhibiting the PSP/AP
3 steps
Located at cell soma (cell body) found halfway between the site where EPSP in generated and the trigger zone
Advantage of location on the soma: the shunt (divert) the EPSP current away from trigger zone and out of cell
Found commonly in the nervous system and more important than EPSPs
Process
All IPSP have a Cl- channel
Equilibrium potential of Cl- is the similar to resting potential
Depolarization of the membrane results in the repolarization by Cl- channels back to -70 mV (inhibitory effect by preventing depolarization and excitation)
AP Spike Train
How long does it last
When does an AP spike train occur (what type of stimulus)
Steps to generate the AP spike train
What are the requirements for a spike train (1 things and where it must be located)
Powerful synaptic input that can last up to 500 ms
Very powerful inputs requires a continuous stream of APs (Spike train) to code for it
Process to generate a AP spike train
After depolarization, the voltage-gated Na+ channels remain inactive (refractory period)
Right after each spike must immediate hyperpolarize the restore the channels back to its original state and overcome depolarization block
Requirements for spike train
K+ channel must be located at the trigger zone to cause hyperpolarization and reconfigure the Na+ channels back to original state
This way the MP will shoot back immediately
Receptor Potential
Main definition
Explain the process
What two things happen after a receptor potential
First type
For the second type pls explain what happens for the amplification (2) and the process (6 steps)
Definition: a change in the membrane potential due to an external sensory cue signal
Process
Generally causes depolarization as it reacts with membrane proteins
Then depolarizes the sensory receptor upon the receipt of a specific energy (signal)
Exception: a receptor that hyperpolarizes (e.g. photoreceptors)
Receptor protein located in sensory cell membrane
Will change shape when a specific energy is received
What happens after change of protein shape
Directly open ion channels
Depolarizes the membrane by opening cation channels
Enzyme is activated via G-protein coupling
Increase the produce of 2nd messenger which amplifies the signal
Stages of amplification of just one stimulus
G-protein activates number of diff enzyme molecules
Each enzyme molecule produces lots of 2nd messengers (cAMP)
Summary: just one stimulus creates many messengers
Process
Binding of chemical stimulus to a metabotropic receptor
Activation of G-protein
Activate enzyme adenyl cyclase
Production of cAMP - 2nd messengers
cAMP activate kinases
Kinases interacted with ion channels or phosphorylates other proteins
Olfactory Receptor
what binds to an olfactory receptor
Explain the process that causes depolarization
Explain what must also happen for an AP to work
Receptor proteins binds to a specific odorant
Process
Odorant binds to the specific receptor to activate the G-protein, G-protein activates the adynyl cyclase, production of cAMP, cAMP binds to ion channels to allow Na+ and Ca++ inside, depolarization of the membrane
The passive current must reach towards the trigger zone
Sensory Cell Transmission
Only state the types of transmissions that can occur in a sensory cell
generates AP
releases vesicles when depolarizes
Sensory cells generate AP
where is the start of the occurance
Where does the AP go?
Excitement occurs at the point of branch, Receptor potential must travel and generate summation to the trigger zone to get action potential
Sensory cell releases vesicles when depolarizes
What does it not produce, instead what does it do?
How does this process work (explain the involvement of a cation channel)
what is an example receptor that does this
The depolarizing current won’t produce action potential
Instead the current will depolarize the membrane enough to cause the influx of Ca+ ion through the Ca+ channels and trigger the exocytosis vesicles to release contents in the sensory cell
E.g. Taste Receptors
Adaptation
main definition
State and explain the two main types
What occurs in both
What the main purpose of each type of adaptation (what kinds of changes in stimuli are the body interested in?)
Adaptation: the membrane potential the decaying over time even though the stimulus intensity is the same
Types
Slowly adapting
The receptor potential is sustained during stimulus but is only interested in any overall changes in magnitude of stimulus
Rapid adapting
Receptor potential elicited by the change in stimulus energy and decays to zero when constant
Very interested in the velocity of the stimulus being delivered
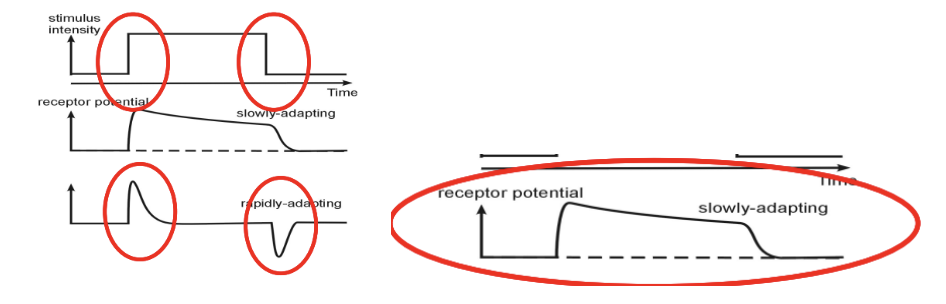
Habituation
main definition
Do all cells have this?
the response to successive stimuli in time
Def: when repeated identical stimuli occurs, will elicit weaker responses each time
Depends on the cell if they do this or not (degree of habituation)
Coding of Stimulus Intensity
How is the intensity of the stimulus coded: recall prev lecture slides
What is the limitation of this
How is the limitation overcomed
Receptor potential (initial) will vary depending on the intensity of the stimulus
greater stimulus = greater receptor depolarization = more transmitters released or higher AP frequency and faster the membrane is brought back up from hyperpolarization
The frequency of AP (Impulse frequency) limited to the refractory period
Solution to being limited by the refractory period
Include more higher threshold sensory neurons (require higher thresholds) for greater stimulus
Post Synaptic Receptors
What are the two methods to determine the intensity of the simulus, based on the previous flashcard
Methods to determine the intensity of the stimulus
Increasing frequency of AP from receptor A at the excitable membrane indicates stronger stimulus
When the stimulus strength continues to increase, add another receptor B with a higher threshold
Different receptors indicate the intensity of the stimulus (e.g. receptor A is lower intensity and receptor B is higher intensity)
Very useful if limited by the refractory period
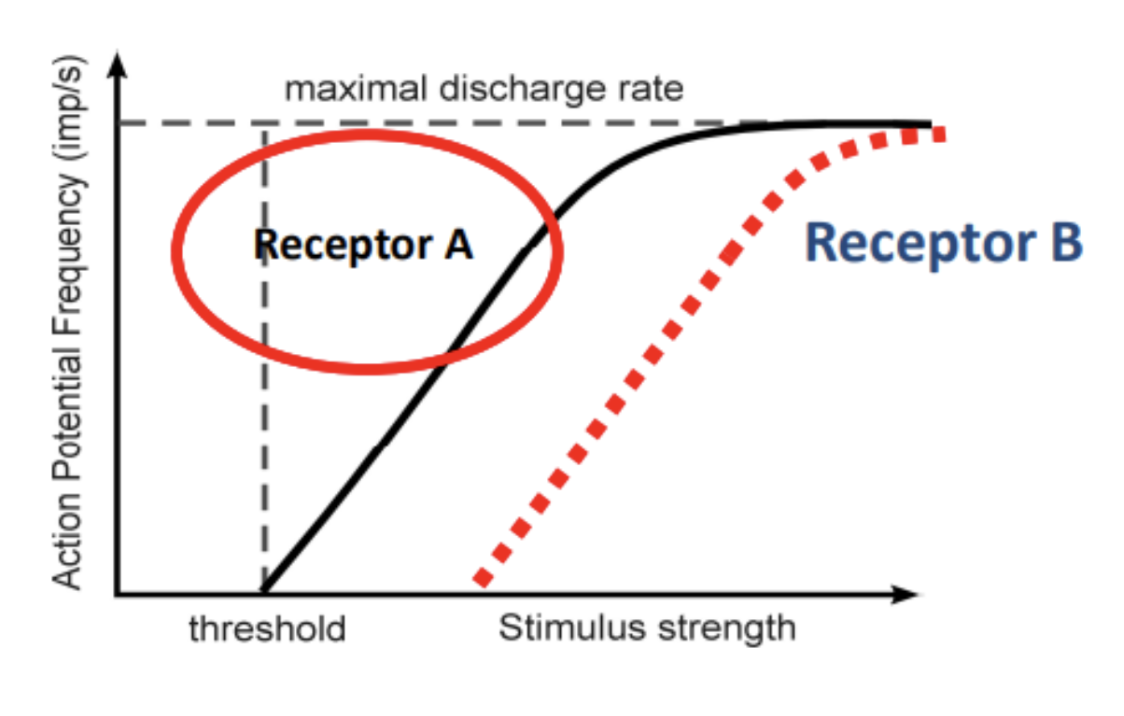
Coding for Modality
What is modality of a stimulus?
One modality = mutliple ___
What is the main issue for coding for modality?
What is the solution (what is this solution called?)
What is another kind of solution (how are the two solutions different from each other?)
Coding for modality = the quality of the stimulus
One modality = multiple stimulus qualities
Issue: many diif receptor to indicate quality is difficult
Solution: Population Code
The ratio of activity from a limited number of receptor types (receptor types = population of receptors)
Labelled line strat
The specific activity in one pathway indicates the quality ONLY = level of response
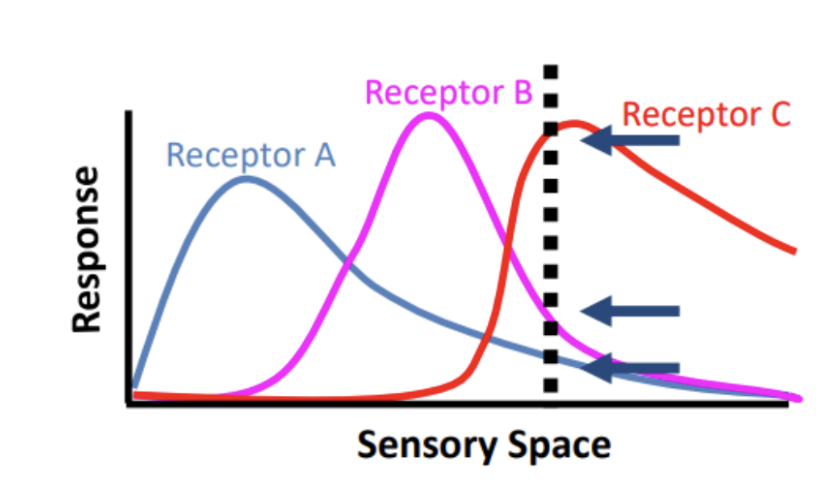
Receptive Field
main definition of a receptive field
give an example with the cutaneous sensory neuron
Types of receptor fields you can find in this type of sensory neuron
Receptive field: Each sensory neurons responses to a particular area (e.g. a patch of skin)
That field is where you can activate that specific neuron
Every sensory neuron have their own receptive field
E.g. cutaneous sensory neuron has receptive field of the skin territory
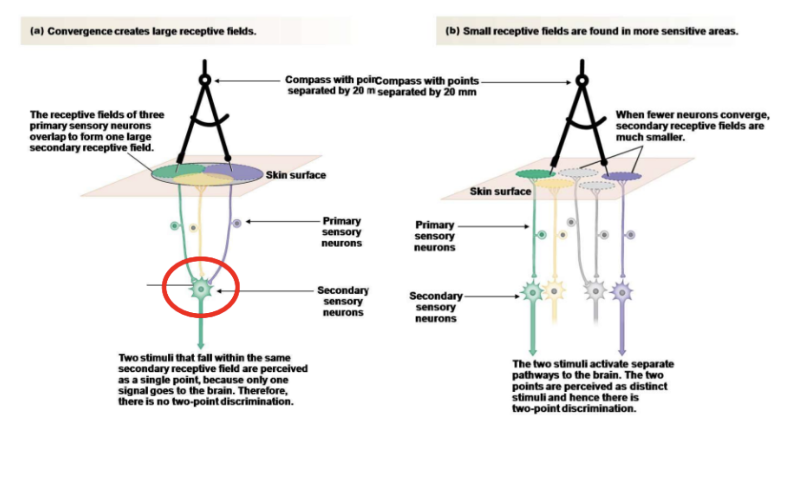
10-20 mm across for each neuron
Smaller secondary receptive fields found in more sensitive areas in order to have more specific location determination based on stimuli - two point discrimination
Larger secondary receptive field results in stimuli perceived in one point - no two-point discrimination
Blood Brain Barrier
What is the purpose of a blood brain barrier
How is this done?
What is the three key components of the BBB
What disease and a type of drug causes the BB to break down
When is there a purpose of not having a BBB
Purpose + Two example
Brain and spinal cord must be protected from the outside circulation and body
How?
By controlling the ionic composition outside the neuron’s extracellular fluid space through Blood-Brain Barrier
No random neurotransmitters around
Avoid stopping AP (e.g. injection of K+ ions to prevent K+ ions leakage from the membrane)
Two key parts and with blood capillaries
Fluid Bathing Neurons
Fluid in Ventricles/Cerebrospinal Fluid
E.g. of unhealthy BBBs
Parkinson’s disease
MSGs
Lack of blood brain barrier
Purposes: for the interactions with the endocrine system or require sensitivity to metabolites (chemicals and other things) in plasma (liquid part of the brain)
E.g. the hypothalamus require different kinds of hormones to function = no BBB
E.g. circumventricular organs around 3rd ventricle have neurons needing to sense different chemicals = no BBB
Brain Encasing
Three main parts
Two parts only list
last part has many different membranes, please state all
4 main membrane parts
1 main area name as well (what is in it and why it is important)
Talk a little about the blood vessels and how molecules can pass through
Skull
Meninges (parts)
Dura Mater (tough membrane, sac like containing brain and spinal cord)
Arachnoid membrane (delicate membrane)
Pia mater (membrane directly on top of brain) that is tethered to arachnoid by arachnoid (memorization tip: spiders - pic looks like it) ‘Trabeculae’
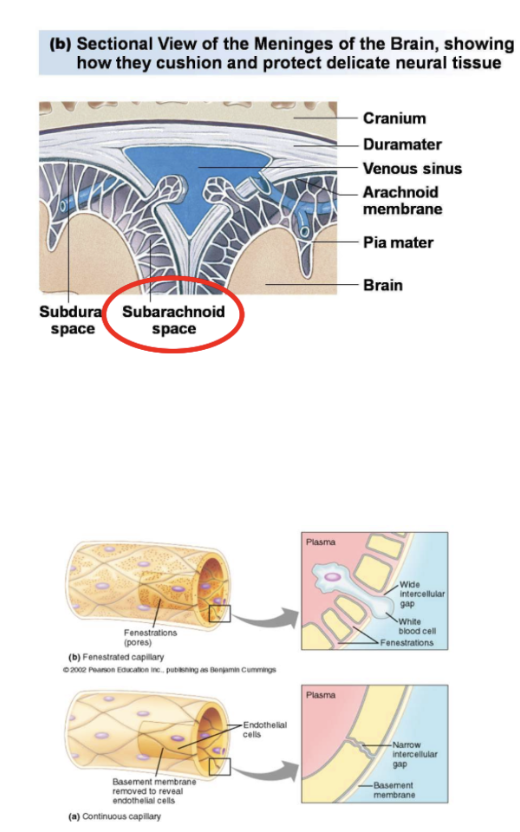
Between pia mater and arachnoid known as the subarachnoid space have fluid CSF to float brain and prevent mechanical stress
Subarachnoid space has
Blood vessels > capillaries to the brain tissue > BBB (between capillaries and brain tissue)
Endothelial lining of the blood vessels has fenestrations (large gaps/pores) so that molecules can pass except for the brain (molecules SHOULD NOT PASS unless through the BBB)
Reticular Formation
Ventricles
What are ventriles and what are the filled with
State all ventricles found in the brain and the order in which contents are moved
Four parts
Addition 2 area names it goes through
How is draining CSF done?
Where does it go?
What is arachnoid villi?
ventriles: cavities deep inside the brain
All filled with cerebrospinal fluid
The parts (in each hemisphere) and process of contents moving
Lateral Ventricle (LV) paired across the midline
Release contents into 3rd ventricle (located in the middle of the brain under hemisphere)
Communicate via “Aqueduct of Sylvius” to move content to the 4th ventricle
4th ventricle contents moves in the “Central Canal” (found in the center of the spinal cord)
Draining CSF
CSF goes to the ventricle in the central canal
Moves to the outer parts of the brain and exists at venous sinuses located at the midline to be drained
Arachnoid Villi: where the CSF drains into the venous sinuses/system
Pouching out of the arachnoid tissue, through the dura mater, into the venous sinuses so the CSF is drained there
CSF
What is it
What is it produced by
Main thing produces it
Secondary smaller part that produces it
Where is CSF in?
Where does it all go afterwards and to where??
Compare CSF contents with blood contents
Two things that are similar
Two things that are different
Total volume of CSF and how it is distributed among 2 parts
1 part has two subparts
How is CSF diagnosed
From plasma that is produced by the ‘choroid plexus’ which lines all ventricles
However some is produced in the capillaries in the brain
Choroid plexus is made up of epithelial cells connected by tight junction
Has a network of capillaries ballooning out into the ventricular wall
All ventricles filled with CSF
All CSF eventually drained by the venous sinuses
CSF continuously produced a day for cleansing (550 ml/day)
Comparing with bloods
Same Na+ concentration and osmolarity
Reduced Ca2+ Mg2+ and K+ concentrations compared to blood
Volume: total avg is 215 mL
Cranial CSF: 140 ml (115 ml subarachnoid space > 25 ml ventricles)
More in subarachnoid space to serve as cushion = most important function
Spinal cSF: 75 ml
Diagnostic/therapeutic: lumbar puncture (spinal tap) to collect sample of CSF
Astrocytes
What is it a type of
Where is it typically located and function for neurons (location indicates purpose)
How does signalling of neurons involve astrocytes (explain the process)
Has four main steps (one of them is a specific function the astrocytes does)
three main functions
One function is very specific; explain why it does this well and the process
What is latching?
Astrocyte is a type of glial cell
Capillaries are plastered at astrocytes feet that allow as a bridge between the capillaries and neurons
Process of communication for signalling of neurons
Blood vessels have glucose
Goes through the blood-brain barrier to the astrocyte
Astrocyte does efficient glycolysis to produce lactate
Lactate is a starting material (substrate) for ATP production
Functions of astrocytes
Removing neurotransmitters
Produce energy substrates (lactate) for neurons
Regulating Blood flow
Due to already being a bridge between the neurons and blood vessels can indicate when to constrict or dilate blood vessels
detect neural signalling increasing at the synapse and send their own metabolic signal outward to the blood vessels to tell about the increased activity level
Process
Glutamate in synapses trigger the Ca2+ release in glial cell, the wave of increased Ca2+ travels to the end-foot and triggers prostaglandin (PGE2) release (prostaglandin causes vasodilation = more blood flow)
Latching
Following to latch on to blood vessels
Feet either latches on the blood vessels or the neurons to create the bridge