PE, DVT, Pneumothorax, and Atelectasis
1/90
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
91 Terms
What is a pulmonary embolism/deep venous thrombosis?
complication of thrombus formation in the deep vein circulation
What is the 3rd leading cause of death among hospitalized patients?
pulmonary embolism
How is a thrombus formed?
- platelet and fibrin attach to plaque in the vessel which initiates clot formation
- clot can partially occludes lumen and then can fully block the vessel
What is a deep venous thrombosis?
clot formation in the deep veins in the LE and UE
What is the pathophysiology of DVT known as?
Virchow's Triad
What is Virchow's triad?
1.) Hyper-coagulable Stage
2.) Endothelial damage
3.) Venous Stasis
What are the causes of a hyper-coagulable state?
- OCP or estrogen replacements
- malignancy
- Inherited genetic defect like clotting deficiencies
What is the number one risk factor for Virchow's triad?
Venous stasis
What causes endothelial injury?
- surgery
- IV drug users
- trauma
What causes venous stasis?
- immobilization
- traveling
- hyper-viscosity
- increased central venous pressure
What is the presentation of DVT?
- u/l leg pain, redness, edema, warmth and tenderness
- palpable indurated cord-like vein
- (+) Homan's sign
What imaging is the gold standard for DVT?
venography
What is another option for imaging for DVT?
US + doppler
What labs are used for DVT?
- D dimer
- coagulation studies
- Anti-thrombin III
- CRP/ESR
Can D-dimer diagnose a DVT?
- not alone
- an elevated D-dimer: multiple clots or one MAJOR clot
- used for risk stratification
What are the risk stratification criteria called for DVT?
Well's Criteria
What is Well's Criteria?
- 1 pt for each
- Active cancer
- Bedridden > 3 days or major surgery within last 12 weeks
- Calf swelling > 3cm compared with other leg
- Superficial veins present
- Entire leg swollen
- Localized tenderness along deep venous system
- Pitting edema
- Recent paralysis, paresis or immobilization of LE
- Previous DVT hx
- 2 or more = DVT likely
What is the goal of treatment for DVT?
- prevent embolus
- prevent recurrent DVT or post-thrombotic syndrome
What is post-thrombotic syndrome?
painful extremities, edema, stasis dermatitis, and skin ulcers after a DVT from damage to vasculature
What are the categories of treatment for DVT?
1. anticoagulation
2. thrombolytic therapy
3. surgical extraction
What are 5 anticoags used for DVT?
1. Direct oral anticoagulants (dabigatran, apixaban, rivaroxaban, edoxaban)
2. Warfarin
3. unfractionated heparin
4. LMWH
5. Fondaparinux
What is the preferred treatment for DVT?
- direct oral agens (DOA)
- dabigatran, apixaban, rivaroxaban, or edoxaban
What is the MOA of direct oral anticoagulants?
inhibit thrombin (II) or cofactor X
What is the MOA Warfarin, and what do you need to monitor?
- vitamin K antagonist
- inhibit 2, 7, 9, 10
- PT/INR (2-3 sec)
How do you reverse the effects of warfarin?
vitamin K
What is the MOA of LMWH, and what are the contraindications?
- anti-coag used before PO as a bridge
- binds to and accelerates AT III
- renal insufficiency
What are the examples of LMWH?
delteparin and enoxaparin
What is the MOA of unfractionated heparin, and what needs to be monitored?
- more specifically for inactivation of thrombin
- aPTT (goal is 1.5-3x upper limit)
What is used to reverse unfractionated heparin?
protamine
What are the complications of heparin?
- hemorrhage
- HIT
What is fondaparinux?
indirectly inhibits factor Xa
What is the difference between anticoagulants and thrombolytics?
- anticoagulants: prevention of clot formation
- thrombolytics: clot busters --> given because the clot has already formed
What is recommended alone for low-risk DVT patients?
direct oral agents
What is used IM for 5-10 days to bridge to dabigatran?
LMWH
What is used IM for 5 days or until INR is within 2-3 seconds to bridge to warfarin?
LMWH
What can be used for DVT prevention in acute settings?
LMWH
What is drug of choice that is normally taken for life after d/c of anticoagulants?
Asprin (ASA)
What is the duration of anticoagulant use for a known/unknown, reversible cause?
- known cause = 3 months
- unknown cause = at least 3 months (do D dimer monitoring)
What is the duration of anticoagulant use for cancer-related causes?
3-6 months or duration of cancer
What is the duration of anticoagulant use for recurrent DVTs, or an underlying clot disorder?
indefinitely
What is the duration of anticoagulant use for pregnancy?
3 months post-delivery
What is a pulmonary embolism?
clot dislodged from peripheral venous system into pulmonary arterial system
What are 6 types of pulmonary embolism?
1. air in veins
2. amniotic fluid
3. fat (trauma related)
4. FB (IV drug users)
5. septic (endocarditis)
6. thrombus
What is the pathophysiology of pulmonary embolism, and what are the pathophysiologic consequences?
- clot travels to and lodges in part of the pulmonary arterial circulation or systemic artery
- Respiratory consequences
- Hemodynamic consequences
What are the respiratory consequence of pulmonary embolism?
- increased alveolar dead space
- hypoxemia (ventilation-perfusion mismatch)
- hyperventilation
- decreased regional surfactant
What are the hemodynamic consequences of pulmonary embolism?
- reduces cross sectional area of pulmonary vascular bed
- Increases pulmonary vascular resistance
- Increases right ventricular afterload
- may result in right-sided heart failure or ventricular failure
- pulmonary arterial vasoconstriction
What is the presentation of pulmonary embolism?
- dyspnea
- cough
- pleuritic chest pain
- tachycardia
- hypoxia
- rales
- fever
- accentuated S2
What are 7 imaging options used for pulmonary embolism?
1. Pulmonary Angiography/Venography
2. Helical CT Pulmonary Angiography
3. Ventilation-Perfusion Study
4. ECG
5. Venous U/S
6. echocardiogram
7. CXR
What is considered the gold standard for diagnosis of pulmonary embolism?
- Pulmonary Angiography
- not used super often, inject iodine contrast into pulmonary vessels
What is considered an initial test of choice for diagnosis of pulmonary embolism?
Helical CT Pulmonary Angiography
When is the VQ study used for pulmonary embolism?
used when CT not available or contraindicated
What is seen on ECG with pulmonary embolism?
- sinus tachycardia
- nonspecific ST segment and T wave changes (T wave inverted)
What 3 labs are done for pulmonary embolism?
1. D dimer
2. ABG
3. Troponin/BNP
What does an ABG show with a pulmonary embolism?
- hypoxemia
- respiratory alkalosis
What are pharm treatment options for a pulmonary embolism?
1. DOA
2. Warfarin
3. Heparin
4. LMWH
5. Fondaparinux
6. thrombolytics (alteplase)
What is a procedure treatment option for pulmonary embolism?
Inferior vena cava filter (when CI to anticoags, recurrent with therapy, or chronic PE)
What is the last resort treatment for PE?
surgical extraction (high risk of mortality)
What are the indications for thrombolytic therapy for PE treatment?
acute PE associated with hypotension where there is low risk for bleeding and anticoagulation is contraindicated
What is the prevention protocol for pulmonary embolism?
- ambulation
- hydration
- anticoagulation
- compression stockings
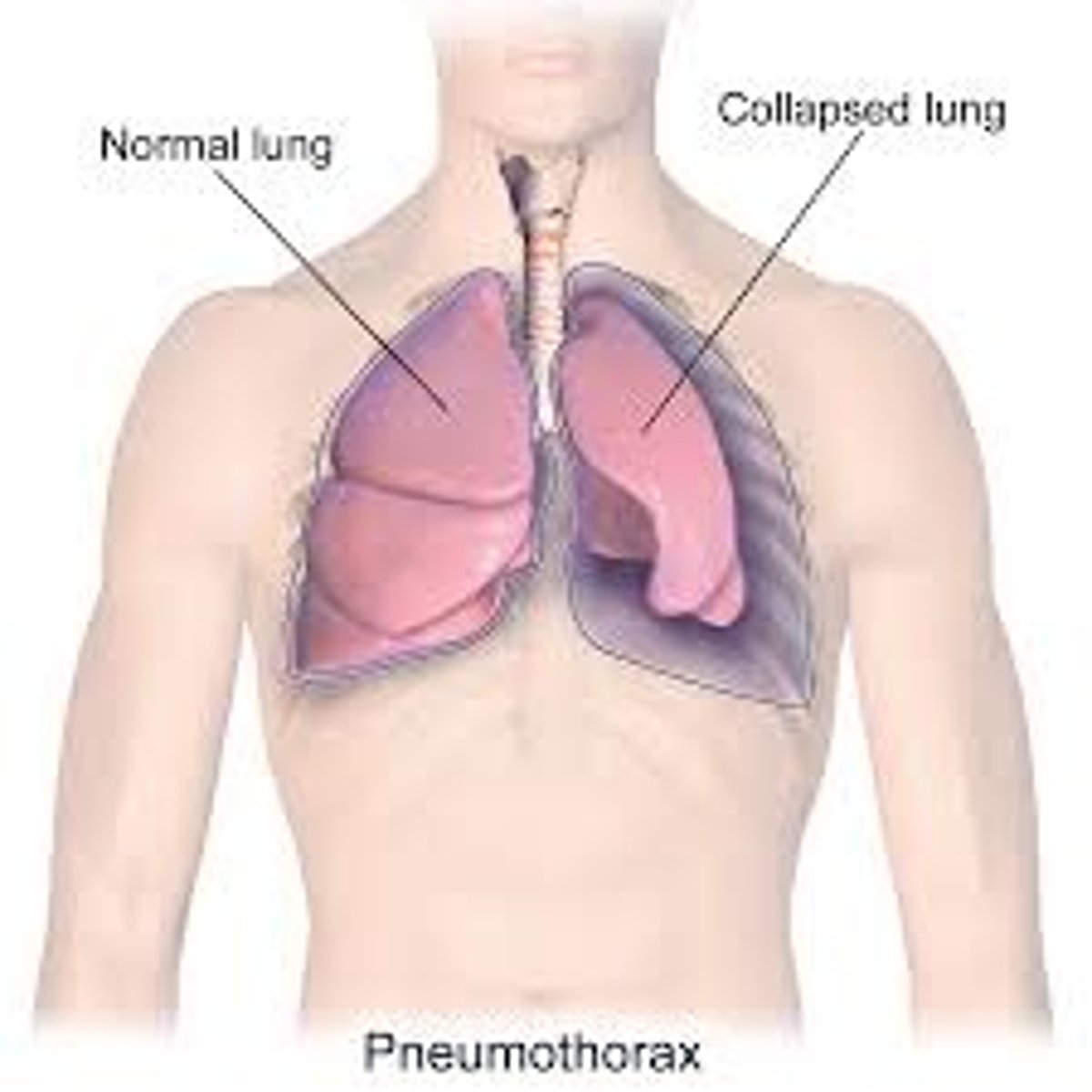
What is a pneumothorax, and what is it caused by?
- accumulation of air in the pleural space known as a collapsed lung
- caused by trauma or is spontaneous
What are 5 types of pneumothorax?
1. primary spontaneous
2. secondary spontaneous
3. traumatic
4. iatrogenic
5. tension
What kind of pneumothorax is associated with no underlying disease or trauma?
Primary Spontaneous
What is the typical presentation of a primary spontaneous pneumothorax?
- tall, thin male
- age 10-30 years
- +/- hx of smoking
- Fx of pneumothroax
- Subpleural apical blebs/bullae rupture
What kind of pneumothorax is associated with complication from a pre-existing lung disease like COPD, asthma, CF, TB or interstitial lung disease?
Secondary Spontaneous
What kind of pneumothorax is associated with a blunt force trauma?
traumatic
What kind of pneumothorax is associated with post-medical procedure?
iatrogenic
What kind of pneumothorax is associated with penetrating trauma, infection, CPR, or mechanical ventilation?
tension
Which type of pneumothorax is most dangerous?
tension
What is the pathophysiology of pneumothorax?
- pleural space fills with gas due to a rupture of lung blebs
- Gas pressure outside lung overcomes gas pressure inside lung = lung collapse
What is the presentation of pneumothorax?
- sudden chest pain on the affected side
- sudden dyspnea
- tachycardia
- respiratory faliure
- decrease breath sounds on affected side
- hyperresonance percussion sounds on affected side
- decreased tactile fremitus sounds on the affected side
- low chest movement sounds on affected side
What is the presentation of tension pneumothorax?
- hypotension
- mediastinal/tracheal shift
- Hyperresonance of affected side
- hypoxia
What is seen on CXR with pneumothorax?
-visceral pleural line with no lung markings beyond the affected lung portion ("companion line")
- pleural effusion
- deep sulcus sign (deep and dark costophrenic angle)
What is seen on CXR with tension pneumothorax?
- large amount of air in the affected side
- shift of mediastinum toward the unaffected side
What is a skin complication of pneumothorax?
subcutaneous emphysema → below the skin bubbles (gross video, affected side cracking)
What is the treatment for asymptomatic pneumothorax?
supportive care and treat depending on risk of recurrence
What is the treatment of small pneumothorax?
1. observe
2. supplemental oxygen
3. serial CXR
4. consider small-bore catheter for air aspiration
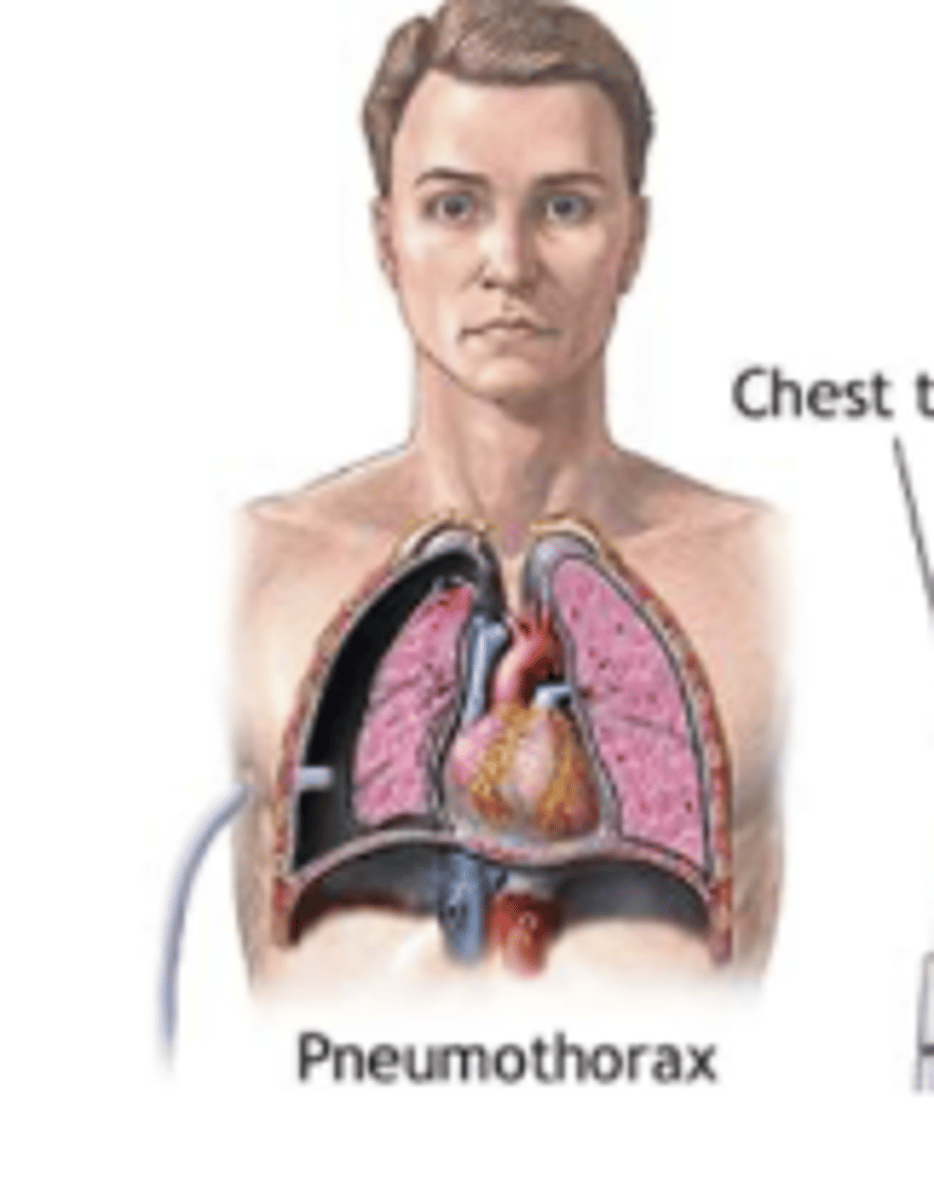
What is the treatment for large pneumothorax?
chest tube with oneway valve for air aspiration
What is the treatment for tension pneumothorax?
1. needle aspiration in 2nd ICS @ MCL
2. chest tube placement
What is the prognosis of pneumothorax?
- 30% of patients with spontaneous pneumothorax will have a recurrence
- prevent with d/c of smoking
What is atelectasis?
- collapse of the alveoli in the lung
- prevents normal exchange of O2 and CO2
- hypoventilation occurs
What are 2 types of atelectasis?
obstructive and non-obstructive
What is post-surgical atelectasis?
anaesthesia & surgical manipulation cause loss of surfactant
What is obstructive atelectasis?
- most common type
- caused by obstruction somewhere between alveoli and trachea
- FB, mucus plugging, or tumor
What is non-obstructive atelectasis?
- loss of contact between parietal and visceral pleura
- due to pleural effusion or pneumothorax
- compression of the lung forces air out of alveoli
- loss of surfactant (adhesive atelectasis)
What are RF for atelectasis?
- elderly
- obese
- smokers
- post-op
What is the presentation of atelectasis?
- fever
- tachypnea
- tachycardia
- elevated diaphragm
- rales, decreased breath sounds, and dullness to percussion
- hypoxemia in severe cases
What is seen on CXR for atelectasis?
- lobar collapse
- mediastinum
shifts toward the side of the collapse
What is the prevention protocol of atelectasis?
- coughing
- incentive spirometer
- early mobilization
- position change
What is the treatment of atelectasis?
- chest percussion
- coughing
- Nasotracheal suction
- Bronchoscopy
- CPAP or O2 supplement
What drug should be avoided with atelectasis and why?
- narcotics
- suppress the cough instinct which is bad for these pts
What should patients with COPD + atelectasis be treated with?
- SABA/ICS
- mucolytics