Patho Week 11 (Hematology)
1/319
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
320 Terms
What are hematopoietic stem cells?
Multipotential stem cells that give rise to all the blood cells we know
What are some properties of hematopoietic stem cells?
- Capable of self renewal
- Differentiate into progenitor cell that gives rise to colonies of cells
What do hematopoietic stem cells respond to?
Respond to the need for blood cells with growth factors (based on oxygen concentration, bleedability, clotting ability)
What is the path of creating mature blood cells starting with hematopoietic stem cells?
Hematopoietic stem cell --> progenitor cells --> precursor cells (blasts) --> mature cells
Should we see premature cells in the peripheral blood (what we draw from the vein)?
NO!! If we do see them, we can suspect something is wrong
What are the 2 major subcategories of hematopoietic stem cells?
- Lymphopoietic line (makes our B and T lymphocytes, natural killer cells)
- Multipotential cell line (create granulocytes, monocytes, erythrocytes and thrombocytes)
What are blood cells?
Any of the kinds of cells normally found circulating in the blood, including WBCs, RBCs, and platelets
Maintained within our plasma
What is hematopoiesis?
The production of all types of blood cells including formation, development, and differentiation of blood cells
What is erythropoiesis?
Specifically referring to the production of RBCs
What are the different components of blood?
- RBCs
- WBCs
- Platelets
- Plasma
What are RBCs? What is their role?
Erythrocytes
primary role is oxygen transport throughout the body
Erythrocytes are released from the bone marrow as:
How long do they circulate
Reticulocytes
Circulate for about 1-2 days
What differentiates Mature RBC from Reticulocytes
reticulocytes maintain a nucleus (have larger volume than classic RBC)
What is the average lifespan of an RBC?
120 days
What are white blood cells? What is their function?
Leukocytes, main role is to fight infection and mount the immune response
What are the 5 main types of white blood cells?
- Neutrophils
- Basophils
- Eosinophils
- Lymphocytes
- Monocytes
What are platelets?
- structure
- role
Megakaryocytes, small colorless disk-shaped cell fragment without a nucleus
Have the biggest role in stopping our bleeding, key step in primary hemostasis
Platelet function is .....
Highly dependent on what is happening in the body
How are platelets involved in hemostasis?
Platelets are a key step --> they rush to the sites of vascular injury and adhere to the injured vessel wall with the help of fibrin
What is thrombopoietin (TPO)? What does it do?
Produced by the liver, it is the main signal from our body to tell us to make platelets
Stimulates production and differentiation of platelets
What is hemoglobin?
A red protein transporter of oxygen in the blood
What does hemoglobin need for synthesis
Needs iron for synthesis --> any deficiency in iron will decrease our ability to transport oxygen throughout the body
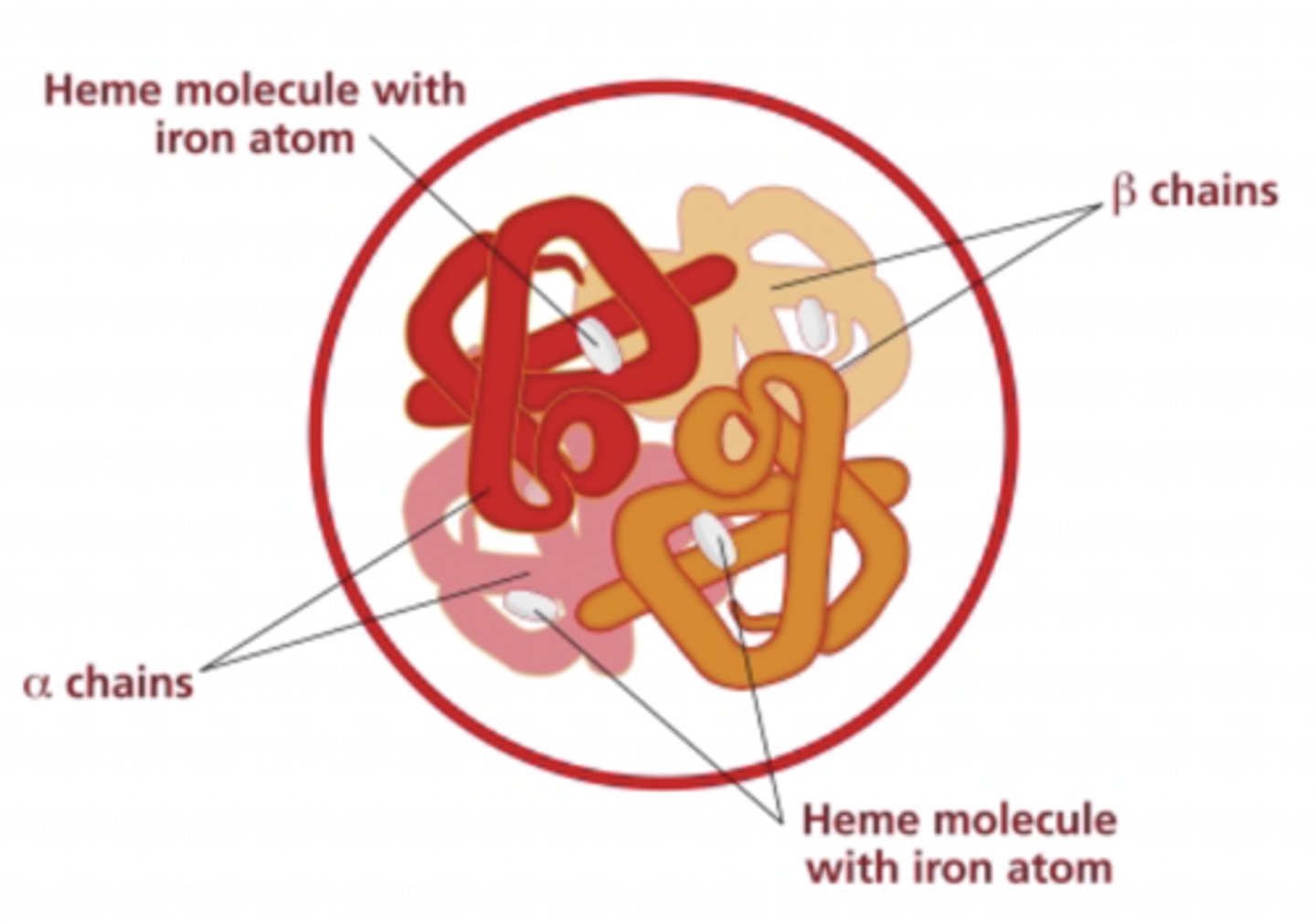
What is the structure of hemoglobin?
4 subunits (2 alpha globin and 2 beta globin chains matched together in a 1:1 ratio)
- each containing an iron atom bound to a heme group
What is fibrin? What does it do?
Insoluble protein formed from fibrinogen during the clotting of blood
Forms a fibrous mesh that impedes the flow of blood
What are neutrophils? What kind of infections are they involved in?
First line of defense (first cells to the site of infection to begin killing the invading microbes)
Involved in bacterial infections, rheumatologic inflammation
Deficiencies in neutrophils increase the risk of....
bacterial infections!
What are eosinophils? What kind of infections are they involved in?
Implicated in numerous inflammatory processes, especially allergic
Associated with parasitic infections
What kind of WBC do we see with bacterial infections?
Neutrophils
What kind of WBC do we see with parasitic infections?
Eosinophils
What are basophils? What kind of inflammation are they involved in?
Cause allergic symptoms by release of heparin and histamine (promotes blood flow to tissues)
Can also be seen with malignant disorders
What kind of WBCs do we see with allergies?
Eosinophils and basophils
What kind of WBC do we see with malignant disorders?
Basophils
What are monocytes? What is their function?
Immature macrophages that fight off bacteria, viruses, and fungi
Once infection occurs, will mature into macrophage to help eliminate the infection
What are monocytes used for in oncology?
monitor bone marrow response
What are lymphocytes? What kind of infection are they involved in?
Type of WBC that eliminates antigens by releasing antibodies (B cells), cytotoxic granules (T cells) or signaling to other cells (helper T cells)
Associated with viral infections
What kind of WBC do we see in viral infections?
Lymphocytes
What is the difference between B and T lymphocytes?
B lymphocytes produce antibodies
T lymphocytes can either be cytotoxic or signaling cells
B lymphocytes mature in the bone marrow
T lymphocytes mature in the thymus
What are blood cell disorders?
Hematologic conditions in which there's a problem with RBCs, WBCs, or platelets
Can either be benign or malignant (cancerous)
What are the two different RBC disorders?
- Anemia (low level of RBCs)
- Polycythemia (high level of RBCs)
What are the two different platelet disorders?
- Thrombocytopenia (low level of platelets)
- Thrombocytosis (high level of platelets)
What are the two different WBC disorders?
- Leukopenia (low level of WBCs)
- Leukocytosis (high level of WBCs)
What is the most common blood disorder worldwide?
Anemia
Affects about 1/3 of the global population
What is the incidence of iron-deficiency anemia?
About 1 billion people
Anemia is more common in which populations?
- Women (menstruation)
- During pregnancy
- Children as they are developing
- Elderly (poor nutrition)
Which population has the highest incidence of iron-deficiency anemia and why?
Women in menstrual years
Due to menstruation
How does anemia affect the healthcare system and workforce?
Increases costs of medical care
Lowers a person's productivity through a decreased ability to work
What is anemia? How is it diagnosed?
Reduced circulating erythrocyte mass, diagnosed as low Hgb/Hct
What are some causes of anemia?
- Blood loss (hemorrhage)
- Increased destruction (hemolysis)
- Decreased production of RBCs
- Ineffective hematopoiesis
What are some causes of blood loss, and thus anemia?
- Menstruation
- GI bleed
- Surgical hemorrhage
- Postpartum hemorrhage
What happens with chronic anemia
The patient is able to accommodate due to the body adjusting --> do not have anemia symptoms
What are some causes of increased destruction/hemolysis that lead to anemia?
External triggers like the immune system
What are some causes of decreased production of RBCs that lead to anemia?
Issue within the bone marrow, not making as much RBCs are we should
EX. lymphomas, myeloproliferative diseases
What are some causes of ineffective hematopoiesis that lead to anemia?
Some defect within the cell/bone marrow itself, makes it unable to leave bone marrow appropriately
EX. B12 deficiency
Anemia can lead to:
Tissue hypoxia
We are not circulating oxygen to perfuse our organs like we should be
If people are living with anemia and are not hypoxic/super symptomatic, it is because of:
Adaptive measures by the body
EX. Increasing CO, respirations, etc.
What is erythropoietin? What does it stimulate
Hormone secreted by the kidney in response to hypoxia
Stimulates RBC production in the bone marrow
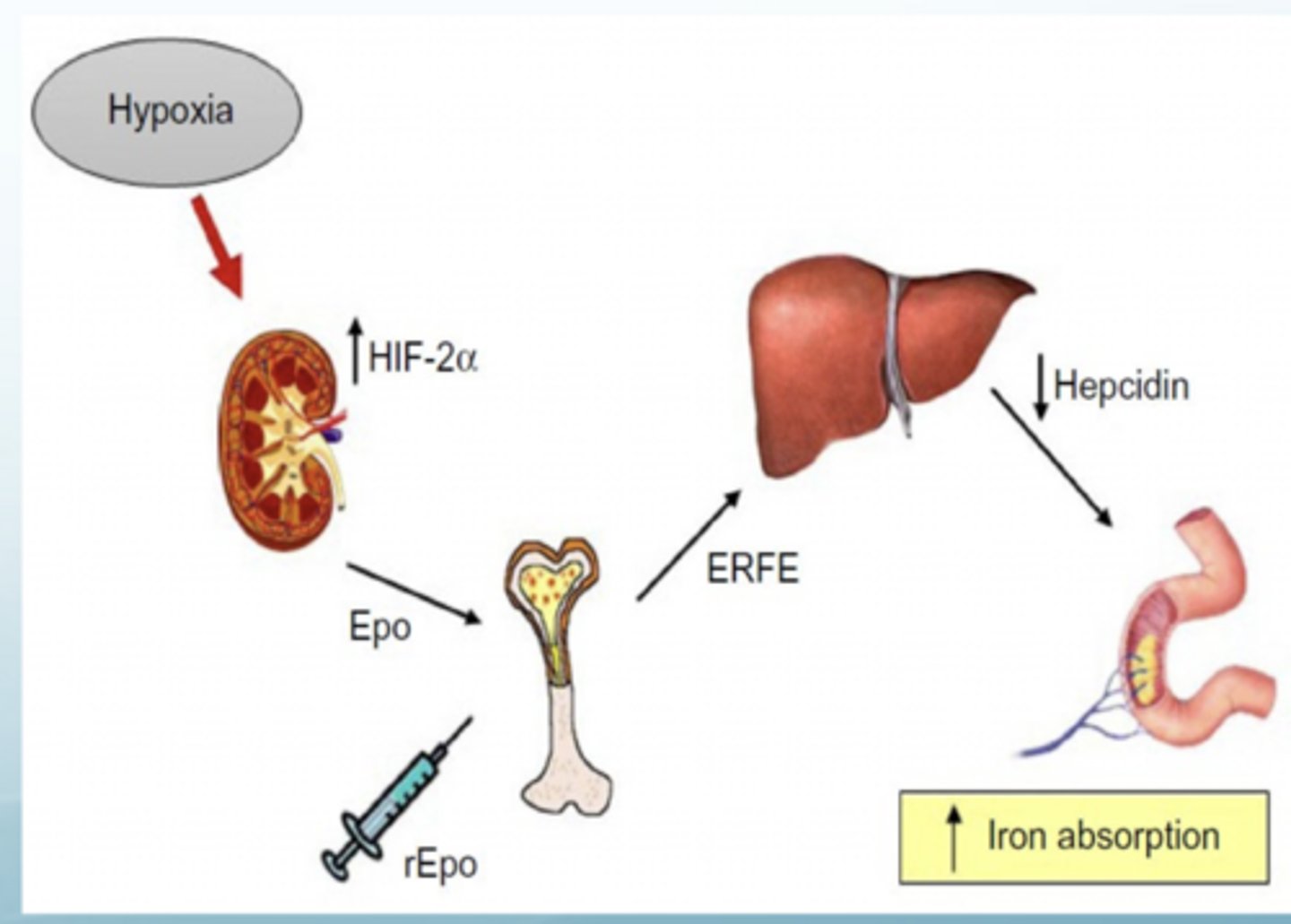
What is hypoxia inducible factor? What does it do?
HIF-2 is a transcription factor that regulates EPO synthesis in the kidney and liver
Plays a critical role in the regulation of intestinal iron uptake
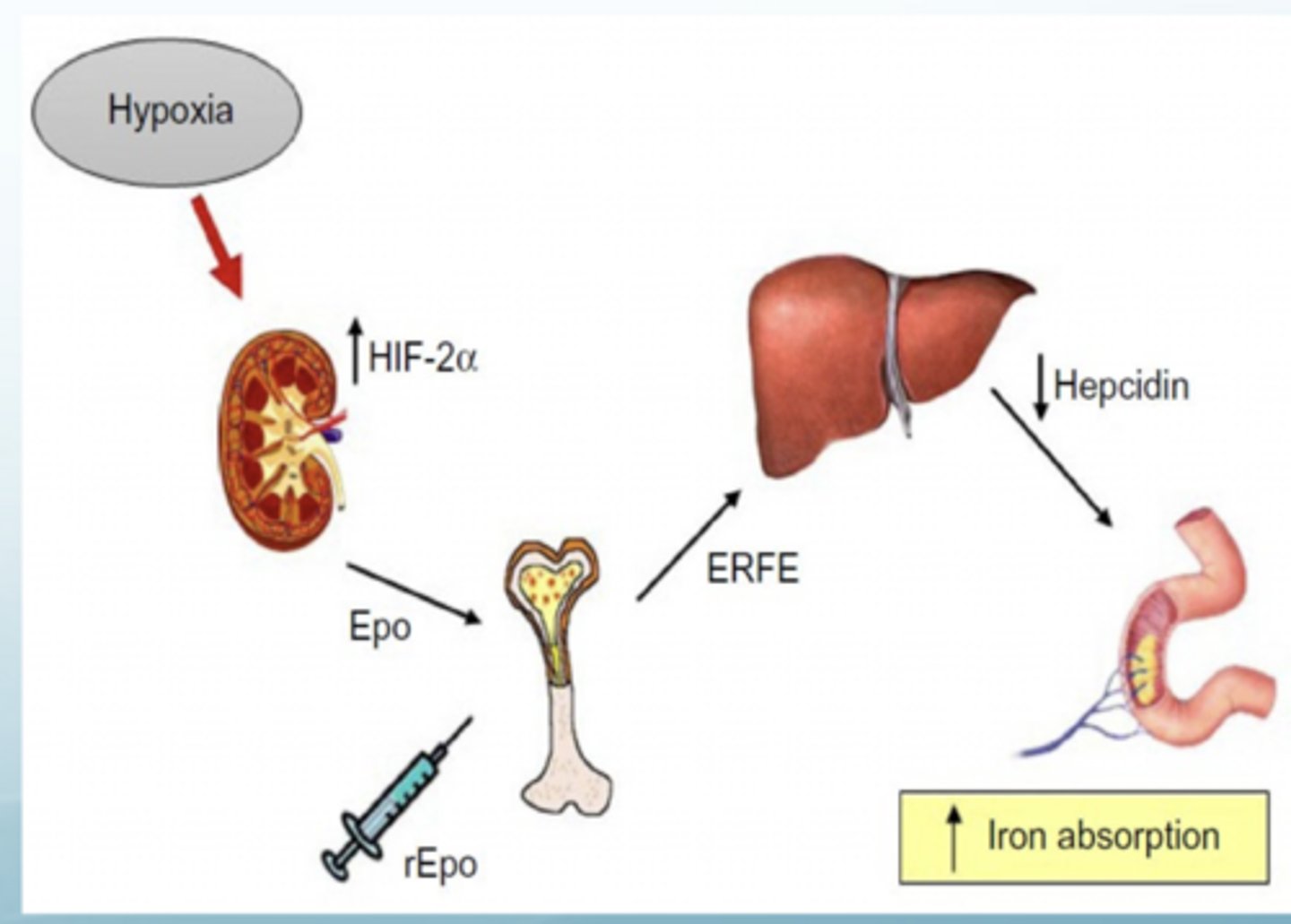
What is hepcidin?What does it do?
Systemic iron-regulatory hormone, key regulator of the entry of iron into the circulation
HUGE factor of anemia regulation (high hepcidin --> lower ability our body has to absorb iron)
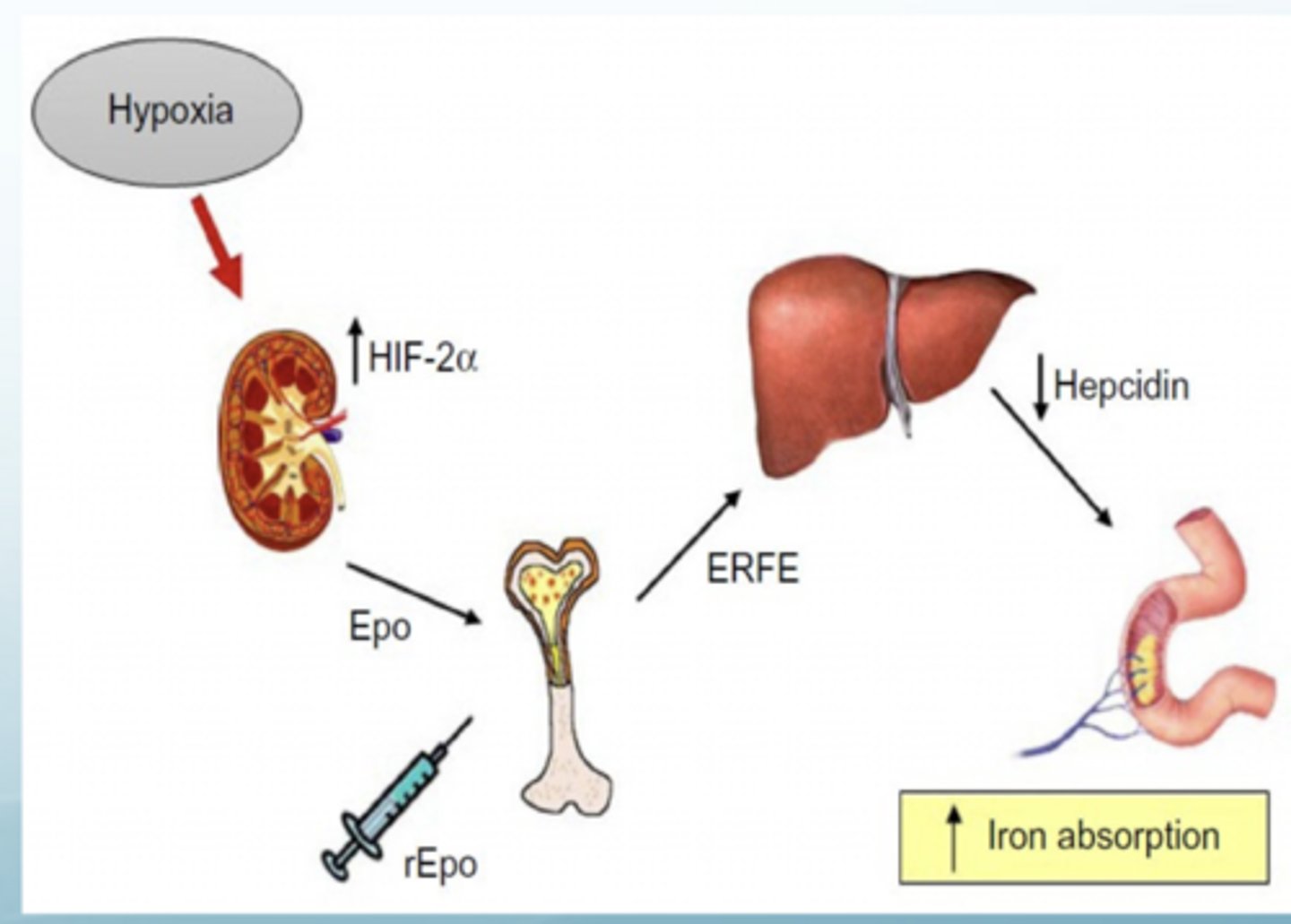
What upregulates hepcidin?
Inflammation
More inflammatory entities --> less iron absorption
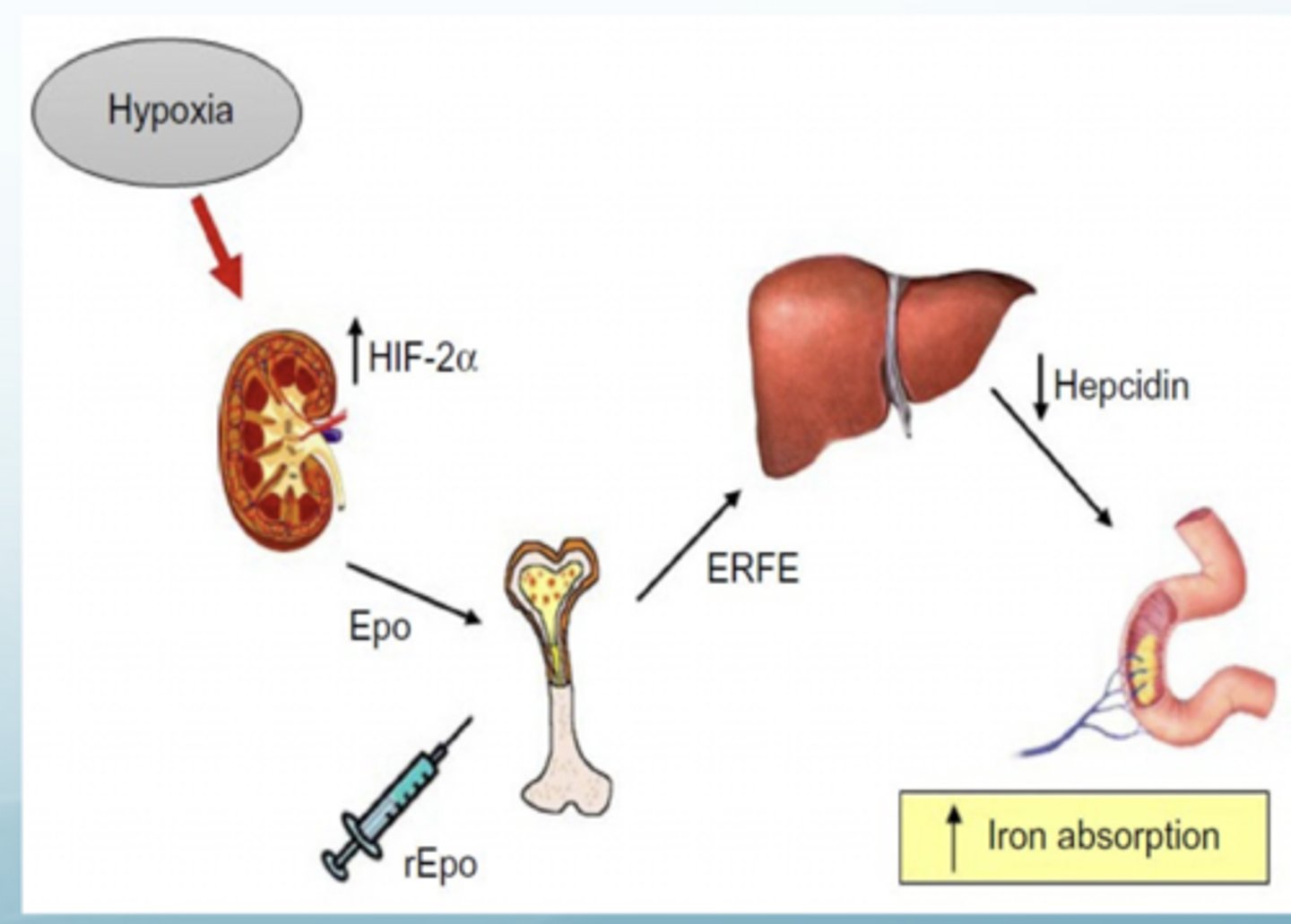
What is ERFE? What does it do?
Iron-regulatory hormone that acts as an erythroid regulator after hemorrhage
Produced by erythroblasts following blood loss, mediates suppression of hepcidin (allows our body to take up more iron)
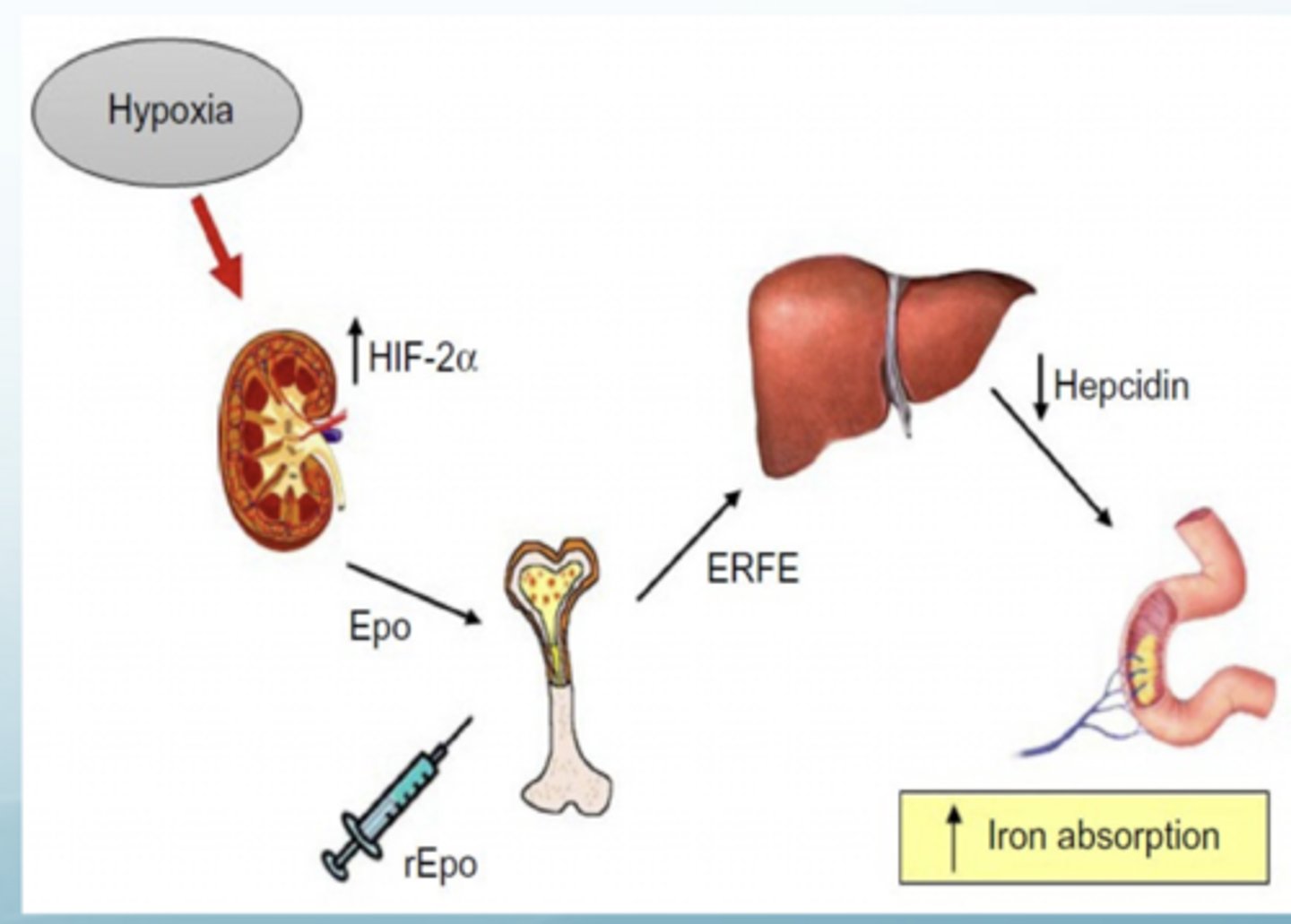
What is ERFE produced by and when?
Produced by erythroblasts following blood loss
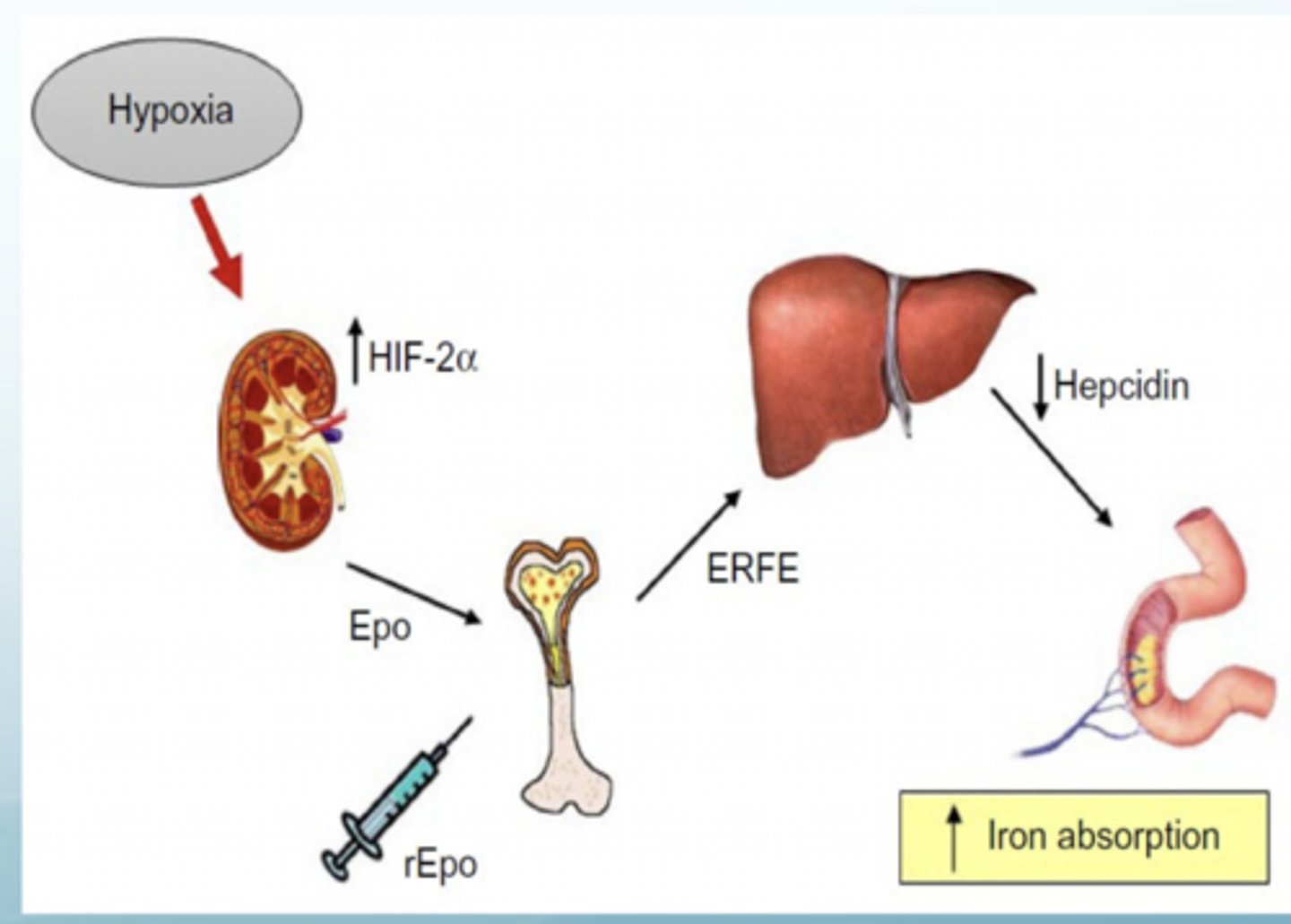
What is RBC morphology?
Useful diagnostic information regarding the underlying cause of anemia
Can be broken down into 3 main categories:
- Microcytic
- Macrocytic
- Normocytic/abnormal shapes
What characterizes microcytic anemia?
LOW MCV
Mean Corpuscular Volume (MCV)
What characterizes macrocytic anemia?
HIGH MCV
Causes enlarged RBCs, changes the border of RBCs and affects the cytoskeleton
What anemias are microcytic?
- Iron deficiency
- Thalassemia
- Sideroblastic (associated with lead poisoning)
What anemias are macrocytic?
- Folate or B12 deficiency
- Chronic liver disease (ex. cirrhosis)
- Alcohol use
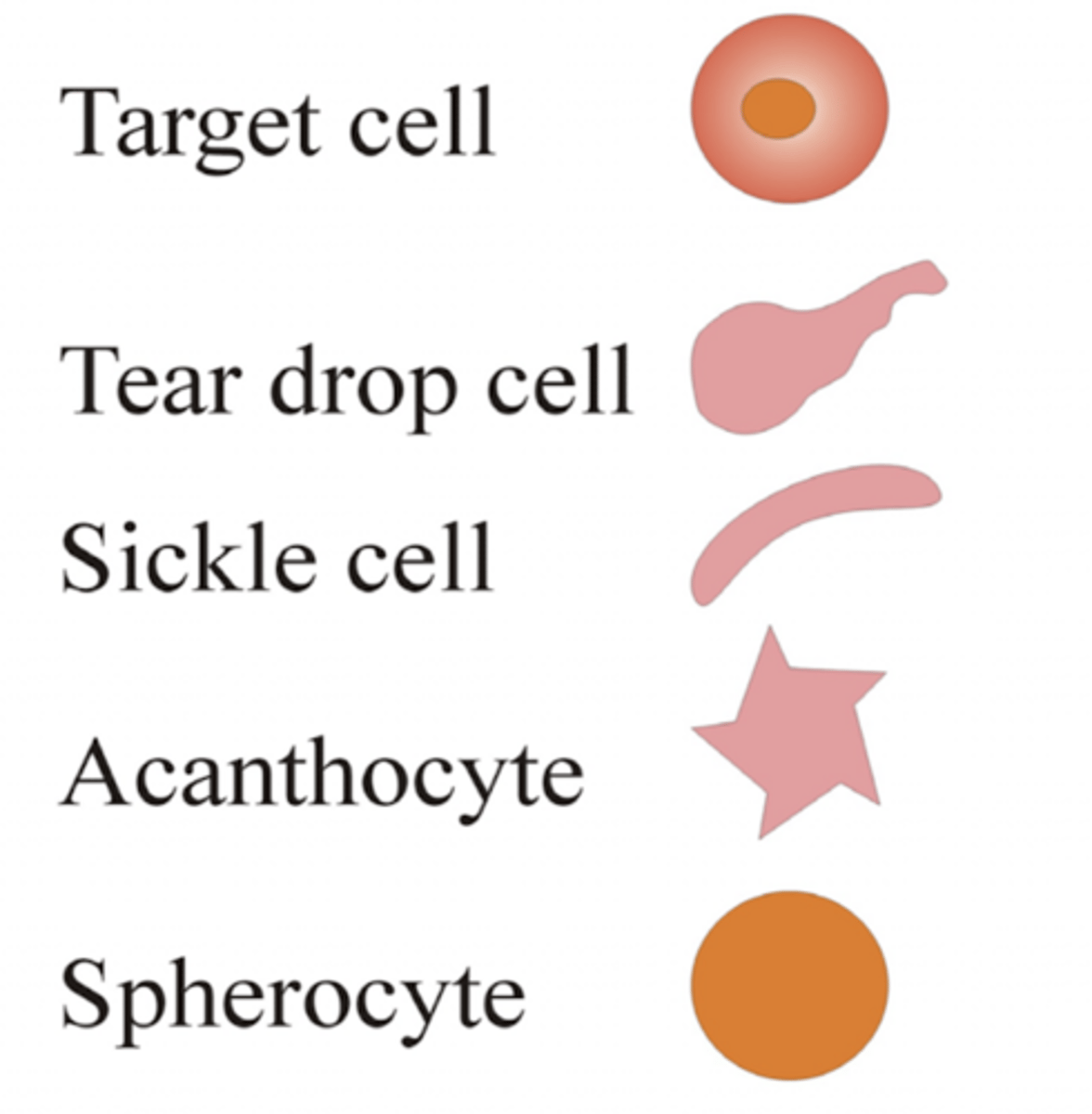
What anemias are normocytic/have abnormal shapes?
- Hereditary spherocytosis
- Sickle cell disease
- Anemia of renal disease
- Hypothyroidism
- Anemia of chronic disease
What is hemoglobin concentration?
Measures the amount of the hemoglobin molecule in a volume of blood
What is hematocrit?
Measures the volume of RBC compared to the total blood volume (RBCs and plasma)
What is the mean corpuscular volume (MCV)?
A measure of the average volume of a RBC
What is the mean corpuscular hemoglobin (MCH)?
Content (weight) of Hb of the average RBC, a reflection of hemoglobin mass inside red cells
Low can be indicative of iron deficiency
What is the red blood cell count?
How many RBCs, an erythrocyte count
What is the reticulocyte index?
How many immature RBCs seen
Generally should see 1-2% circulating in peripheral blood smear
Reticulocyte index can be increased in conditions such as:
Hemolysis
Body is compensating for the RBCs being destroyed by creating more --> will have more immature cells
Reticulocyte index can be decreased in conditions such as:
Bone marrow disease
What 2 tests do we used to determine if someone anemia or not?
Hgb/Hct
What is iron and its role in anemia?
Essential element for blood production in hemoglobin
Needed to form hemoglobin and THUS transport oxygen throughout the body
The liver stores iron as:
Ferritin
What is ferritin?
Total iron storage
Stored in the liver for about 4-6 months
What is the biggest limitation of ferritin?
It is an acute phase reactant (responds to inflammation)
If someone is having some sort of inflammation, they may have a higher ferritin response
What are some testing used for the evaluation of the etiology of anemia?
- Serum iron (measures amount of circulating iron bound to transferrin)
- Serum iron-binding capacity (TIBC, measures the blood's capacity to bind iron with transferrin)
- Transferrin saturation (measures how much transferrin is actually occupied by iron)
- Serum ferritin
- Total body iron stores
What is a normal transferrin saturation?
30%
What transferrin saturation is indicative of iron deficiency anemia?
<20%
What is serum ferritin used to diagnose
iron def anemia
What are some common symptoms of anemia?
Vary depending on the cause, common sx include:
- Fatigue
- Weakness
- Pallor (pale skin)
- Tachycardia or irregular heartbeat
- Shortness of breath (dyspnea)
- Chest pain
- Restless legs
What is a major cause of anemia?
Decreased production of hemoglobin (commonly due to iron deficiency)
What are some causes of decreased production of hemoglobin, that can lead to anemia?
- Decreased hemoglobin synthesis due to iron deficiency
- Anemia of chronic disease (ex. renal failure)
- Stem cell failure (ex. aplastic anemia)
- Myelophthisic anemia
What is myelophthisic anemia? What does it lead to?
Infiltrative process of the bone marrow, typically malignant --> leads to leukoerythroblastosis
What are the examples of myelophthisic anemia
myelofibrosis
hematologic malignancies
metastatic cancer
granulomatous disease
What is leukoerythroblastosis and when can we see it?
Production of immature granulocytes and nucleated erythrocytes due to myelophthisic anemia
When does iron deficiency anemia arise?
When the balance of iron intake, iron stores, and the body's loss of iron are insufficient to fully support production of erythrocytes
Describe iron deficiency anemia based on its RBC morphology.
Microcytic, hypochromic anemia with anisocytosis and poikilocytosis
What is anisocytosis?
Variation in RBC size
What is poikilocytosis?
Variation in RBC shape
Does reticulocytosis occur in iron-deficiency anemia?
No, there is impaired RBC production due to lack of iron --> you don't have the ingredients to make RBCs anyway so cannot have reticulocytes
Iron deficiency has impaired RBC production which causes:
Marrow erythroid hyperplasia
What are some causes of iron-deficiency anemia?
- Increased iron needs (infancy, childhood, pregnancy, lactation)
- Menstrual losses in reproductive age
- In postmenopausal women and men --> tumor or vascular lesions causing blood loss
What are specific signs and sx of blood loss that may be contributing to anemia?
- Rapid blood loss --> fall in BP and dizziness
- Gradual blood loss --> tired, SOB, pale
Anemia due to excessive bleeding results when:
Loss of RBCs exceeds production of new RBCs
What may be needed to determine a non-obvious source of bleeding in a patient you suspect has hemorrhage-induced anemia?
Stool, urine, and imaging tests