Unit 3: Imaging of the Thorax
1/65
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
66 Terms
what do we need to remember when thinking about imaging in relation to PT?
imaging should be used in conjunction with examination, imaging may validate PT plan of care, systematic, and fractures may be hidden due to edema, etc
what are some common thoracic imaging?
plain film radiographs (CXR) heart and lung
echocardiography/cardiac ultrasound (TTE and TEE)
myocardial perfusion imaging (MPI): rest and exercise
cardiovascular magnetic resonance imaging (Cardiac MRI)
high resolution CT scams (HRCT)
CT pulmonary angiogram
cardiac catheterization/coronary angiography
describe the characteristics of chest radiograph (CXR)
is a standard screening diagnostic test, carries a dose of radiation, and screen both CV and pulmonary conditions. Can also be portable for the critically ill
what are the limitations of CXR?
patient conditions, and equipment requirements
what do portable CXRs evaluate?
may be routine daily ICU films, evaluate for support tubes and lines placement, fluid status, and presence of infection
how many dimensions would there be for CXR?
2, upright AP and Lateral (AP common in ICU), have to perform with good inspiratory hold (1 view is NEVER enough)
are CXRs more a screening tool or a diagnostic tool?
screening tool, the sensitivity and specificity is not as high as other imaging types
what are chest x rays particularly good at identifying?
pulmonary opacities
what can and cannot be imaged?
depends on the type of imaging done, and the structures being imaged
what might coloration of the different mediums be on a chest x ray?
air will be black (no density), soft tissue gray, and bone is white (most dense)
what is considered the highest quality projection for looking at the heart?
PA- with the patient standing and the x-ray plate in front of the patient, with the beam projected at the back
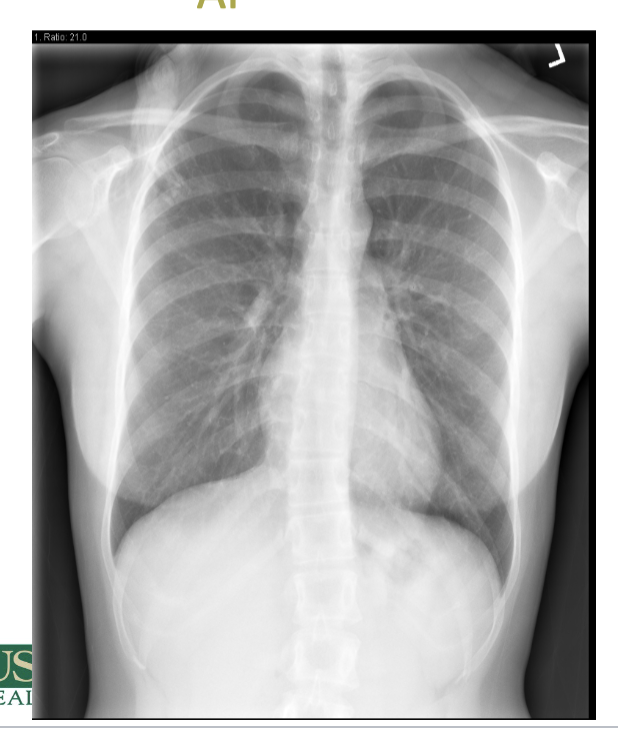
which type of projection is attached?
AP
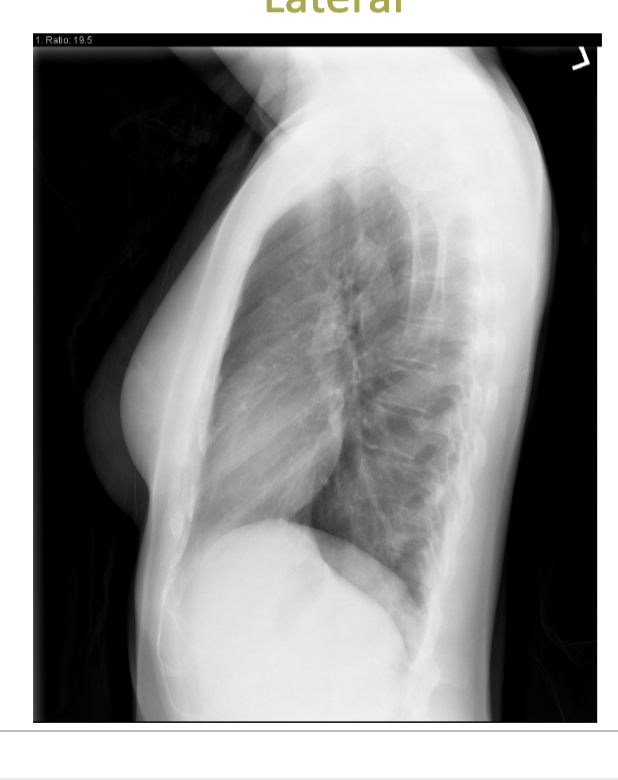
which type of projection is attached?
lateral
why might AP views not be as ideal for chest x rays?
AP views can distort heart size and shape due to magnification. They may also obscure some lung structures. also doesn’t show all of the thoracic structures
what are the ABCDEs of CXRs?
The ABCDEs of CXRs are Airway, Breathing, Circulation, Disability, and Everything else. This mnemonic helps to systematically evaluate chest X-rays for pathologies.
what parts of the airways can be seen in a CXR?
trachea to the carina, and the main bronchi (see if the carina too wide- greater than 100 degrees, or if the bronchial narrowing or dilation)
what can be look at to assess breathing in CXRs?
lung expansion/volume (should count 10 rubs posterior rib bilaterally), if one lung is larger than the other and are there areas of density, look at the crisp costophrenic angles - trace the lateral margins of lung to costophrenic angle. should look at the hemidiaphragms, and the cardiac borders (should be able to clearly see the L and R heart borders)
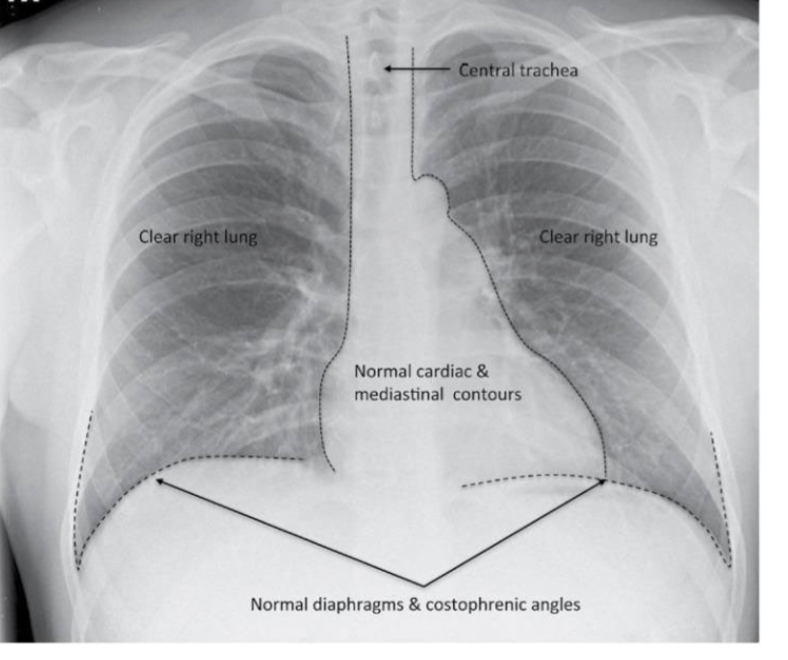
what type of view is shown?
PA view
what can be seen in relation to circulation on the CXRs?
can check cardiac position, assess cardiac size (cardio width should be less than 50% of the thoracic width) check the position and size of the aortic arch, check the width of the upper mediastinum, and look at the hilar vessels
what are the components of disability in CXR review?
trave the ribs to assess for fracture, assess the clavicle, the humerus, the glenoid bone health, and assess the vertebral bodies (similar height and shape, 2 pedicles/body, evidence of disc space)
what falls into the everything else category when doing CXR review?
looking at the pneumoperitoneum- free gas under the diaphragms, presence of hiatal hernia, and absent breast shadow
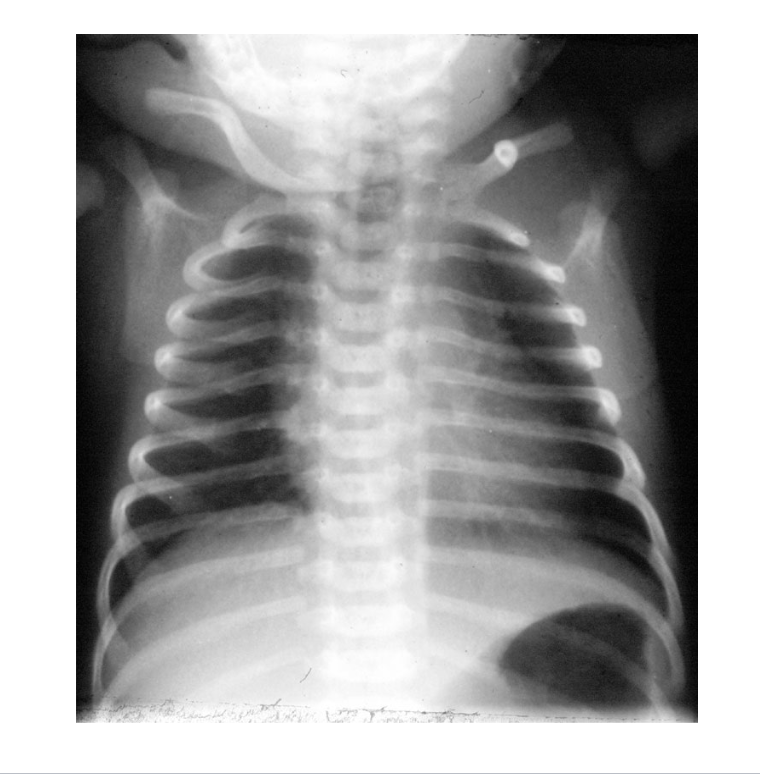
what kind of plain film is attached?
a neonatal AP plain film
what is atelectasis and how can it be assessed on a CXR?
defines as a loss volume from airspaces, can look for by comparing the R to teh L, identifying the border, and any loss of structures
how can pneumonia be identified in CXRs?
can be identified on CXRs by observing areas of opacification, since fluid obscures the structures (need to know anatomy to know what is missing)- should take 2 views to assess
true of false: pneumonia causes volume loss of collapse of the affected lung parenchyma
false, fluid fills up the space and generally doesn’t cause a collapse
true or false: a pneumothroax is best demonstrated by an upright expiratory chest x-ray
true, need person to be upright and look at the structures
what are some space occupying lesions?
pneumothorax, hemothorax, and pleural effusions
what does a pneumothorax look like?
since there is air in the pleural space, see a collapsed lung and increased radiolucency on the affected side of the chest x-ray- structures will be pushed away from the affected side and a shift of the mediastinum
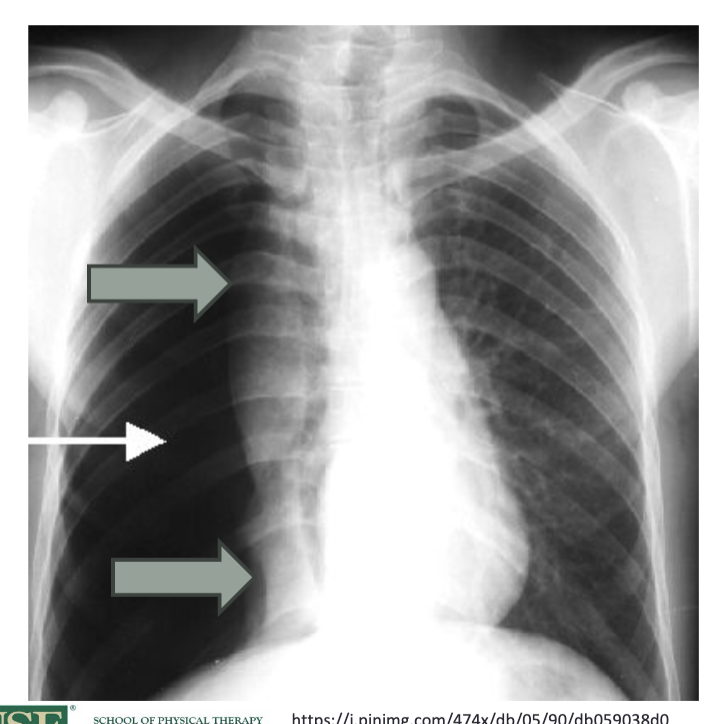
what does hemothorax look like in an CXR?
since there is blood in the thorax that may be from trauma, see a density increase on the affected side of the chest x-ray, often appearing as a concave upper border of the fluid level. might be due to chest tubes
what does pleural effusion look like on CXR?
since there is fluid outside the lungs, see increased opacities on the affected side.
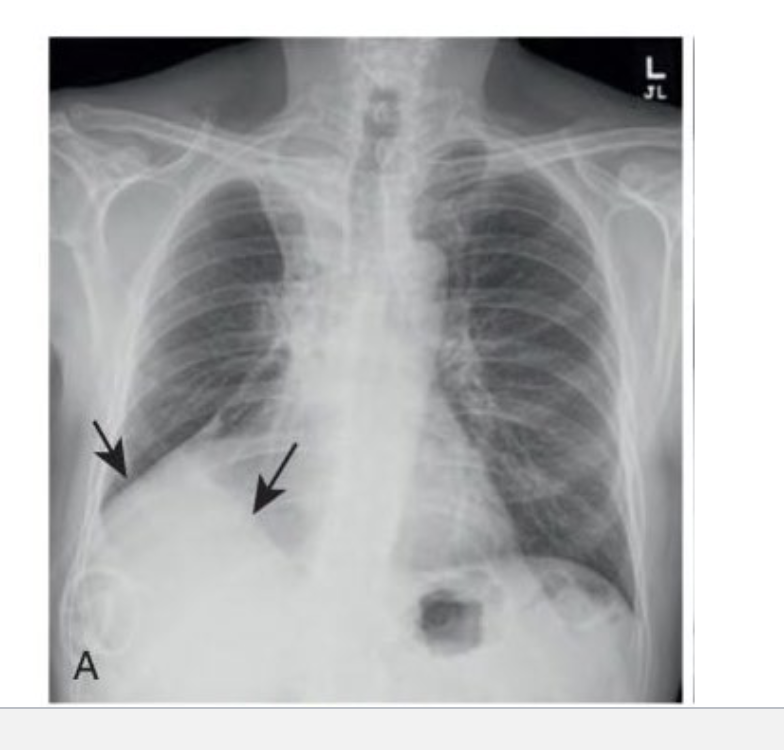
why might you see edema on the CXR?
either due to cardiogenic reasons like congestive heart failure, or due to non-cardiogenic causes like shock, trauma, renal failure, or drug overdose
when we find a fracture of ribs on the chest x-ray, what do we need to do as PTs?
splinting, education of other HC providers and of the patient in how to move to minimize additional damage
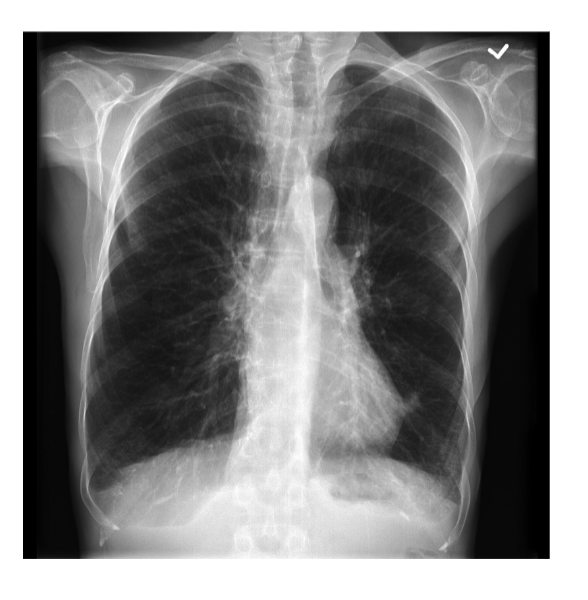
what is pictured/what is occurring with the lungs in the image attached?
hyperinflation of the lungs
how might COPD present on CXRs?
see hyperexpansion (more than 10 ribs seen, barrel chest), flattened diaphragm, cardiomegaly, cystic changes, irregular air pockets, costophrenic angle changes
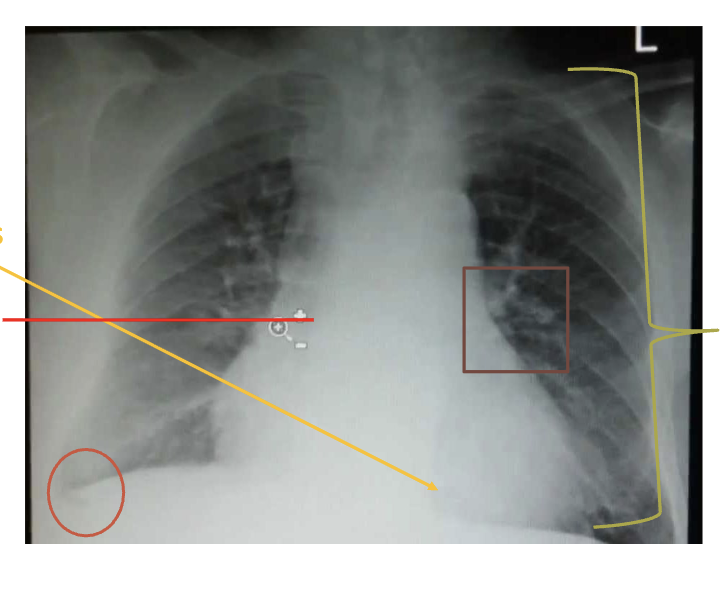
what are potential support lines or tubes that you might see in cxr?
NG (nasogastric) tube, feeding tube. potential complications caused from the position in the airway, or pneumothorax
how can ultrasound be used for thoracic imaging?
there is limited use for pulm thoracic imaging, can look at pleural effusion well though/overlying strucutres filled with gas and fluid, mostly used fro CV imaging. can also help see superficial chest wall masses or fluid. also non-invasive and safer since no radiation!
what is intravascular ultrasound (IVUS) used for?
used to visualize the interior of blood vessels, aiding in the assessment of atherosclerosis, vascular lesions, and the anatomy of coronary arteries. It provides real-time imaging during procedures, helping guide interventions and evaluate stent placements.
what is an echocardiography?
A non-invasive imaging technique that uses ultrasound waves to create images of the heart's structure and function and blood flow, allowing assessment of cardiac size, shape, and blood flow. provides real time images of the beating heart. important tool in the assessment and management of pts with thoracic trauma
different types of cardiac echos?
doppler, transthoracic, transesophageal, stress echomyocardial contrast echocardiography, 3D echocardiography, contrast echo
what is a transesophageal echocardiography?
A specialized echocardiogram where an ultrasound probe is inserted into the esophagus to obtain detailed images of the heart. This method provides clearer images than transthoracic echocardiography, especially for structural heart disease and assessing valvular function.
what is a bronchoscopy?
A procedure that allows doctors to visualize the airways and lungs using a thin, flexible tube called a bronchoscope. may be used diagnostically or therapeutically, secretions may be removed for eval or treatment, particularly important in the diagnosis of bronchogenic carcinoma
what is a thoracentesis?
diagnostic test in which needle is inserted into the pleural space to obtain fluid or cultures
what is thoracoscopy?
diagnostic test in which small incision into the chest wall with a fiber optic scope is inserted to view the pleural cavity, may remove fluid or secretions
how are MRI images created?
uses nuclear magnetic resonance to build tissue images, nuclei are made to resonate in a magnetic field, causes hydrogen (also carbon 13, flroine 19 and sodium 23) nuclei to align with a magnetic field
what are the advantages of MRi?
non-ionizing radiofrequency, better distinction of abnormalities, better visualization, multi-plane imaging, no radiation and dynamic imaging capabilities.
what are the disadvantages of MRI?
difficulty using patient with metal implants, pacemakers or claustrophobia, expensive, extensive time requires, movement artefact possible
what can MRI be used to assess?
can be used to get images of the heart in real time to be used alongside EKGs, vascular imaging, mediastinal masses, chest wall masses, spine and neurogenic masses, valvular function (qualitative and quantitative), myocarditis, cardiomyopathies, congenital heart disease
why might MRIs be challenging to get pulmonary images?
Factors such as respiratory motion, difficulty in obtaining static images due to the need for breath-holding (movement of thoracic spine during exam)
what are some pulmonary indications for MRIs?
cystic fibrosis, lung cancer staging, lung nodule characterization, pulmonary hypertension
what is computed tomography?
A medical imaging technique that uses X-rays to create detailed cross-sectional images of the body, useful for diagnosing various conditions, including those in the thorax. an iodine based dye injected intravenously can enhance CT images. used to identify masses in the CV system or detect aortic aneurysms or pericardial thickening. LOTS of radiation- a typical chest CT will expose a pt to the radiation of 50 to 450 equivalent chest radiographs
what is high resolution CT used for?
a non invasive technique best used for imaging tissues with significant differences in density (vasculature, airways, chest wall/skeleton), also good for eval of nodules and masses, fluid collections, aortic aneurysms or pericardial thickening
what are the indications of CT scans?
assess mediastinum (lymph nodes, infection), assess chest wall, presence of cancer or pleural thickening, lung pathology, biopsy
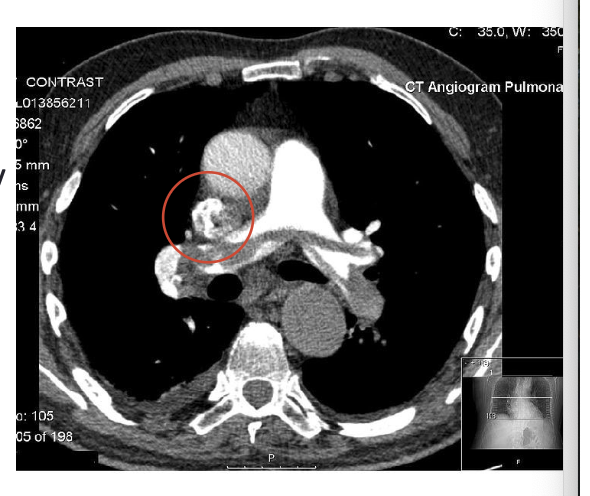
what is depicted in the image?
CT scan showing a pulmonary embolus- spans the R/L pulmonary artery and there is blocked blood flow (gray area within the artery), black areas are the lung fields
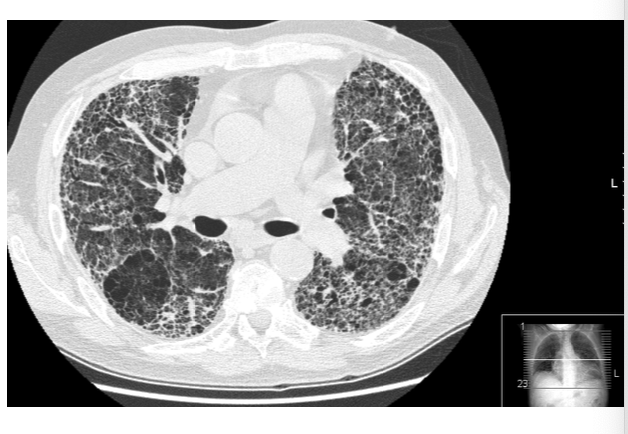
what is depicted in the image?
CT scan showing idiopathic pulmonary fibrosis, notice the diffuse interstitial pattern, the tissue vs open space, and the ground glass opacity
what is SPECT imaging?
single photon emission computed tomography- planar images are collected by rotating cameras- pt has to lie still 15 to 20 minutes
what is a VQ scan?
radionuclide ventilation-perfusion scan. this helps to detect the conditions that affect blood flow in the lung parenchyma, radioactive isotopes are injected into the bloodstream and inhaled in to the lungs. scanning for the location of these isotope is then able to determine the extent to which the lungs have been ventilated and perfused
what is positron emission tomography (PET)?
A type of imaging technique that uses positron-emitting radionuclides. used for visualization and direct measurement of metabolic function, gold standard for blood flow measurements, and provides info regarding cellular processes, delineates myocardial areas with reversible and irreversible injury, and can detect jeopardized but viable myocardium
what is myocardial perfusion imaging?
imaging that is used for diagnostic decisions, treatment decisions, and prognosis. important in the diagnosis of coronary artery disease
what are the different nuclear tests of the CV system?
first pass study (radiolabeled bolus of blood to ID cardiac chambers), gated equilibrium scans, exercise stress study (treadmill exercise test), pharmacologic stress studies
what is an angiography?
x-ray examination of the arterial system using an opaque contrast dye, cardiac imaging for cardiac catheterization, coronary arteriography, cardiac ventriculography, and pulmonary imaging for pulmonary angiography for diagnostic pulmonary embolism
what is a bronchography?
imaging technique used to visualize the bronchial tree and lungs by injecting a contrast medium into the airways, typically used to diagnose bronchial obstructions and other pulmonary conditions.
what is a coronary angiography?
commonly performed as diagnostic and therapeutic procedure, gold standard for dx coronary angiography to detect flow limiting lesions, diagnostic for ventricular and valvular function, therapeutic use for stent placement, biopsy, and ablation
what is ventriculography?
A diagnostic imaging procedure that involves the injection of a contrast dye into the ventricles of the heart, allowing for visualization of heart chamber size, shape, and function, typically used to assess ventricular performance and detect abnormalities.
what are indications for cardiac catherization?
cardiac arrest or ventricular fibrillation, pulmonary edema, intolerance of or noncompliamnce with medical therapy for angina. significant decrease in exercise duration. progressive decline in systolic BP to less than 100 mmHg to during exercise, evidence of symptomatic hypoperfusion during exercise, left ventricular ejection fraction less than 35%, and ventricular tachycardia with exercise
what is holter monitoring?
a noninvasive diagnostic test that allows for continuous 24 hour elecrtrocardiographic monitoring of the pts heart rhythm, used in diagnosis and management of cardiac arrythmias
what is the zio patch?
A portable, wearable device for continuous ECG monitoring over an extended period, typically up to 14 days, used to detect arrhythmias in patients. (can be used to replace the holter monitoring)