A&P I ch. 25
1/136
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
137 Terms
What is the primary function of the kidneys?
To maintain the body's internal environment by regulating water volume, solute concentration, ion concentrations, acid-base balance, and excreting metabolic wastes.
What hormone do kidneys produce that regulates blood pressure?
Erythropoietin
What is the role of renin produced by the kidneys?
To regulate red blood cell production.
What are the three main components of the urinary system?
Ureters, urinary bladder, and urethra.
Where are the kidneys located?
Retroperitoneal, in the superior lumbar region between T12 and L5.
Why is the right kidney lower than the left?
Because it is crowded by the liver.
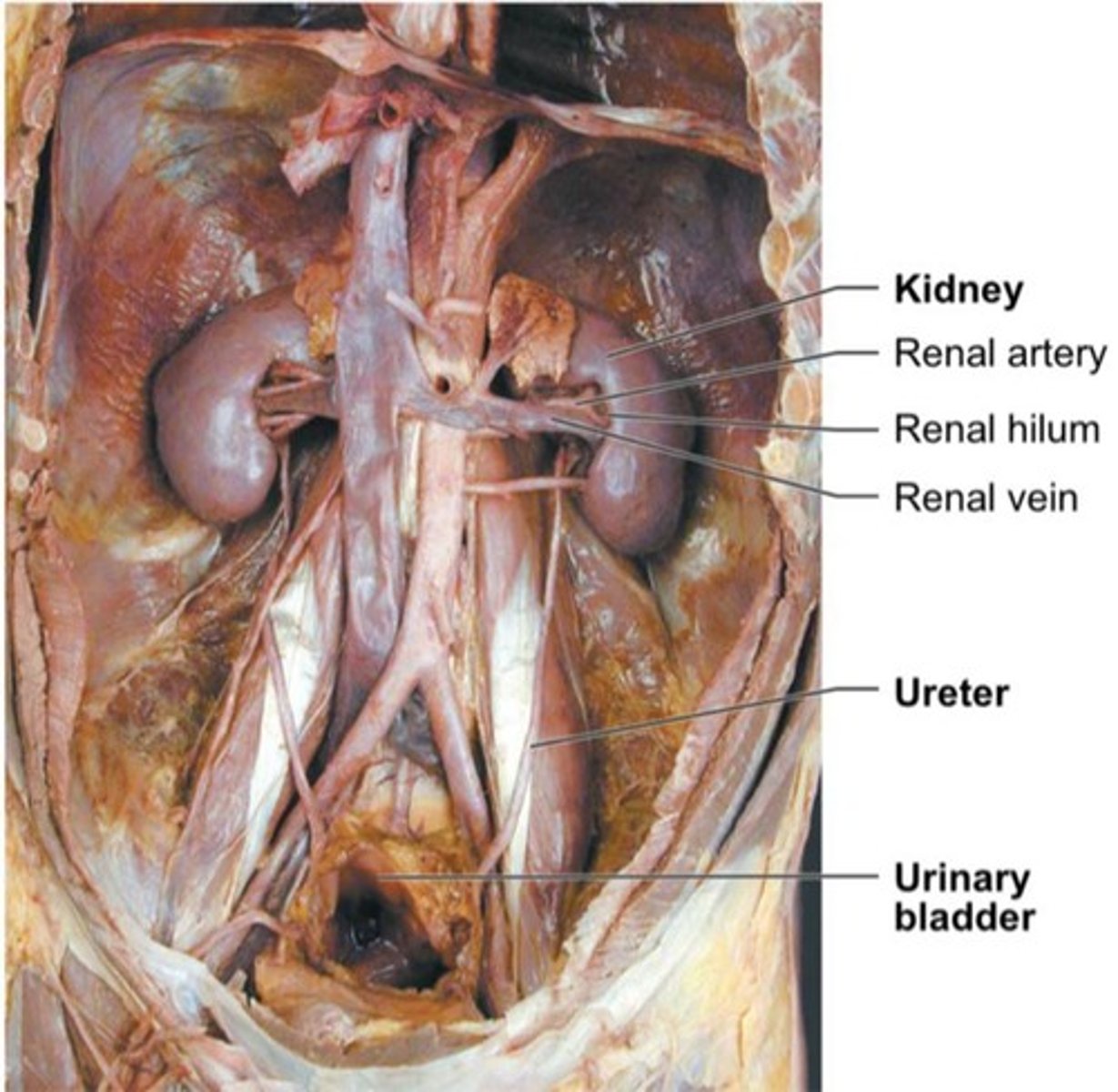
What is the renal hilum?
The concave medial surface of the kidney where ureters, renal blood vessels, lymphatics, and nerves enter and exit.
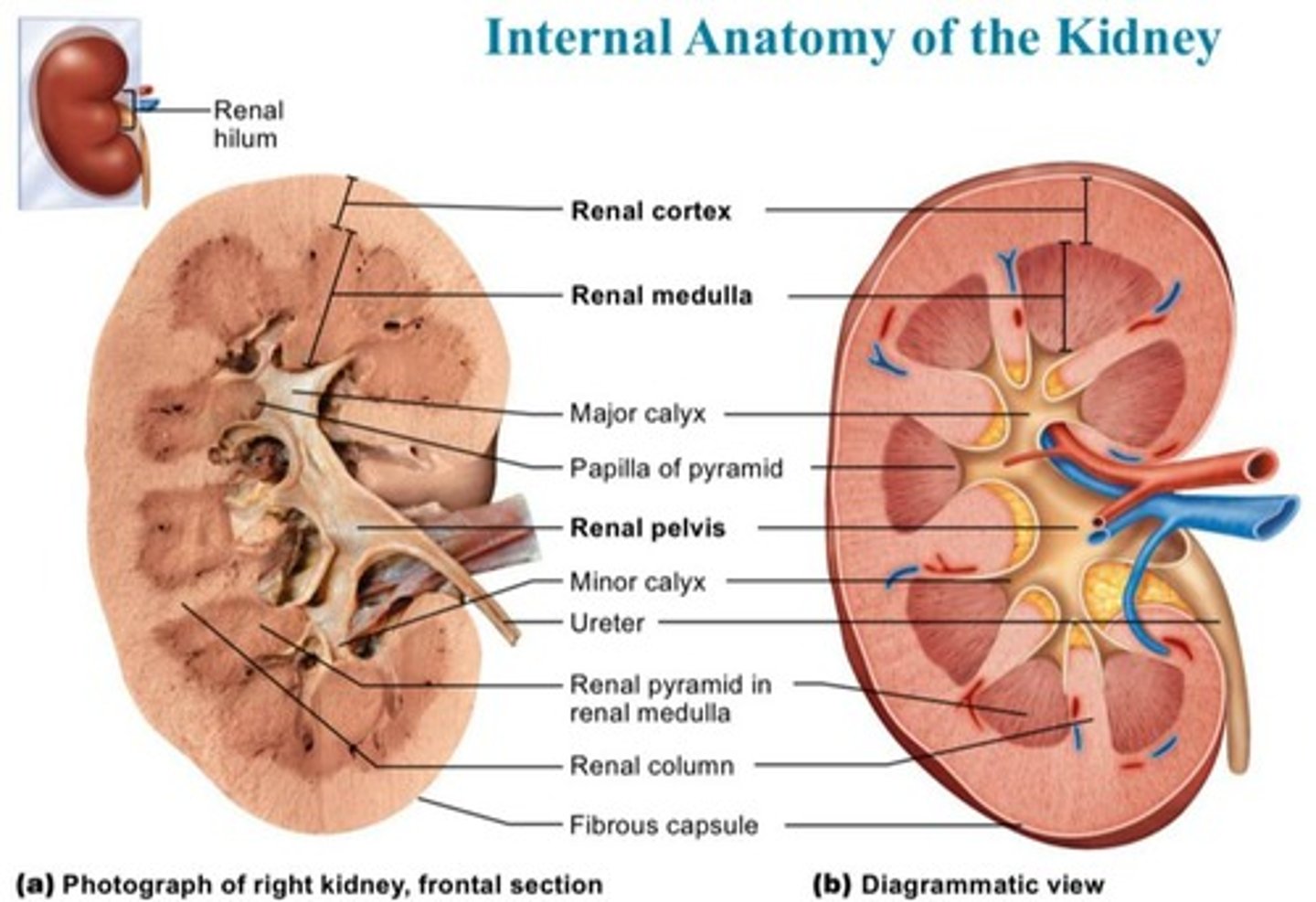
What are the three distinct regions of the internal kidney?
Renal cortex, renal medulla, and renal pelvis.
What is the function of the renal pelvis?
It is a funnel-shaped tube that collects urine and is continuous with the ureter.
What are minor and major calyces?
Minor calyces collect urine from renal pyramids, while major calyces collect urine from minor calyces and empty it into the renal pelvis.
What is pyelitis?
An infection of the renal pelvis and calyces.
What is pyelonephritis?
An infection or inflammation of the entire kidney.
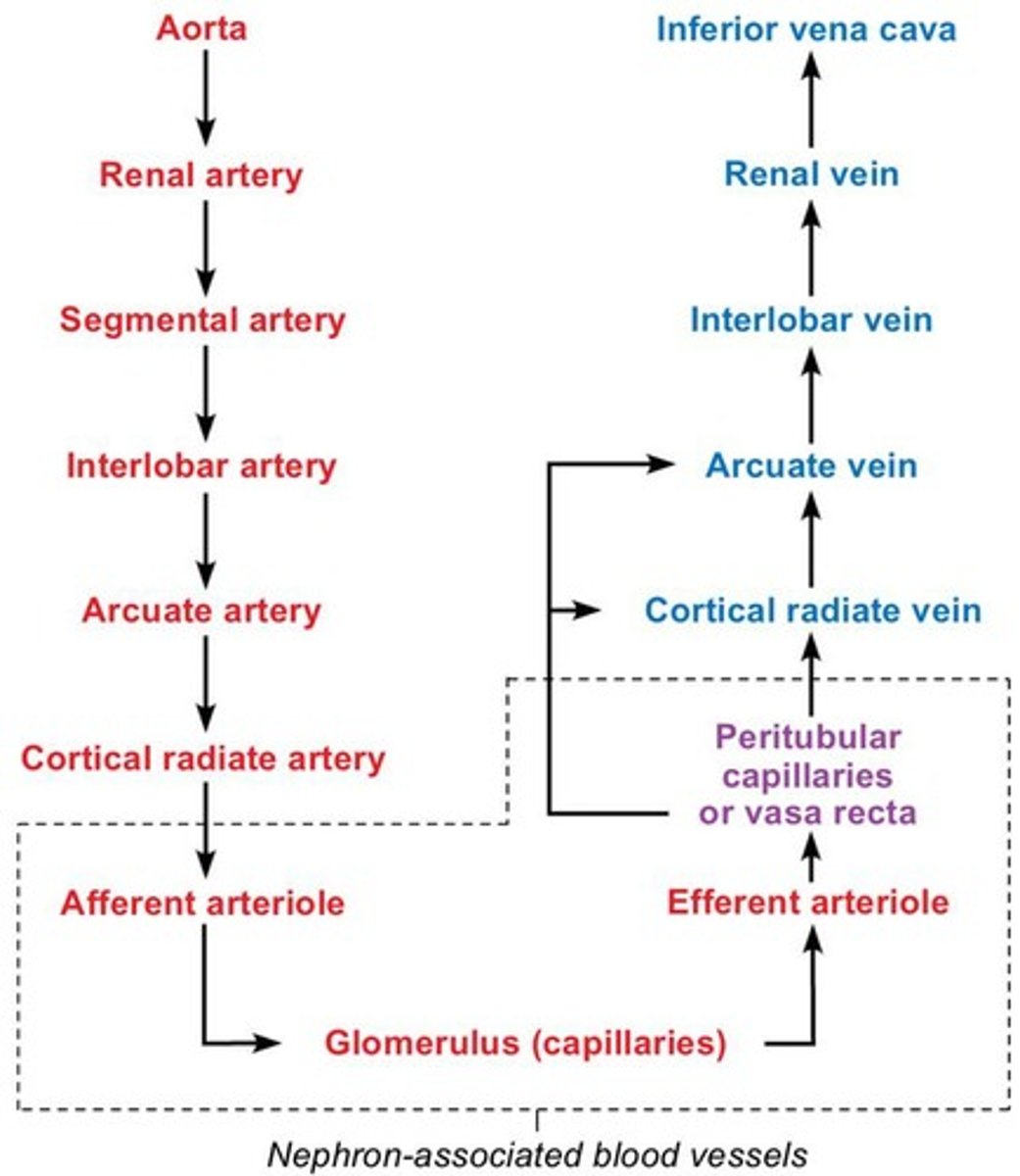
What is the blood supply to the kidneys?
Renal arteries deliver about one-fourth of cardiac output to the kidneys each minute.
What are the two main parts of a nephron?
Renal corpuscle and renal tubule.
What is the glomerulus?
A tuft of capillaries in the renal corpuscle that allows for efficient filtrate formation.
What is Bowman's capsule?
A cup-shaped structure surrounding the glomerulus, consisting of parietal and visceral layers.
What are the three major parts of the renal tubule?
Proximal convoluted tubule, nephron loop, and distal convoluted tubule.
What is the function of the proximal convoluted tubule (PCT)?
It functions in reabsorption and secretion and is lined with cuboidal cells with dense microvilli.
What is the nephron loop also known as?
Loop of Henle.
What type of epithelium lines the descending limb of the nephron loop?
Simple squamous epithelium.
What type of cells are found in the thick ascending limb of the nephron loop?
Cuboidal or columnar cells.
What type of cells are found in the distal convoluted tubule (DCT)?
Cuboidal cells with very few microvilli
What is the primary function of the distal convoluted tubule?
Secretion rather than reabsorption
Where is the distal convoluted tubule confined?
To the cortex of the kidney
What are the two cell types found in the collecting ducts?
Principal cells and Intercalated cells
What is the function of principal cells in the collecting ducts?
Maintain water and Na+ balance
What do intercalated cells in the collecting ducts help maintain?
Acid-base balance of blood
What is the appearance of the medullary pyramids due to the collecting ducts?
They give the pyramids a striped appearance
What percentage of nephrons are cortical nephrons?
85%
What is the significance of juxtamedullary nephrons?
They are important in the production of concentrated urine
What are the two capillary beds associated with renal tubules?
Glomerulus and Peritubular capillaries
What is unique about the glomerulus compared to other capillary beds?
It is specialized for filtration and is fed and drained by arterioles
What is the normal glomerular filtration rate (GFR)?
120-125 ml/min
What is the primary force pushing water and solutes out of the blood in the glomerulus?
Hydrostatic pressure in glomerular capillaries (HPgc)
What is the net filtration pressure (NFP) in the glomerulus?
10 mm Hg, calculated as 55 mm Hg outward minus 45 mm Hg inward
What does GFR depend on?
Net filtration pressure, total surface area available for filtration, and filtration membrane permeability
What are the two types of renal autoregulation mechanisms?
Myogenic mechanism and Tubuloglomerular feedback mechanism
What does the myogenic mechanism do in response to increased blood pressure?
Contracts local smooth muscle to restrict blood flow into the glomerulus
What triggers the tubuloglomerular feedback mechanism?
Changes in filtrate NaCl concentration detected by macula densa cells
What happens to GFR during sympathetic nervous system activation?
Constriction of afferent arterioles decreases GFR
What is the role of the renin-angiotensin-aldosterone mechanism?
To increase blood pressure
How much fluid do the kidneys process daily?
180 L of fluid
What percentage of the processed fluid becomes urine?
Less than 1% of the original filtrate
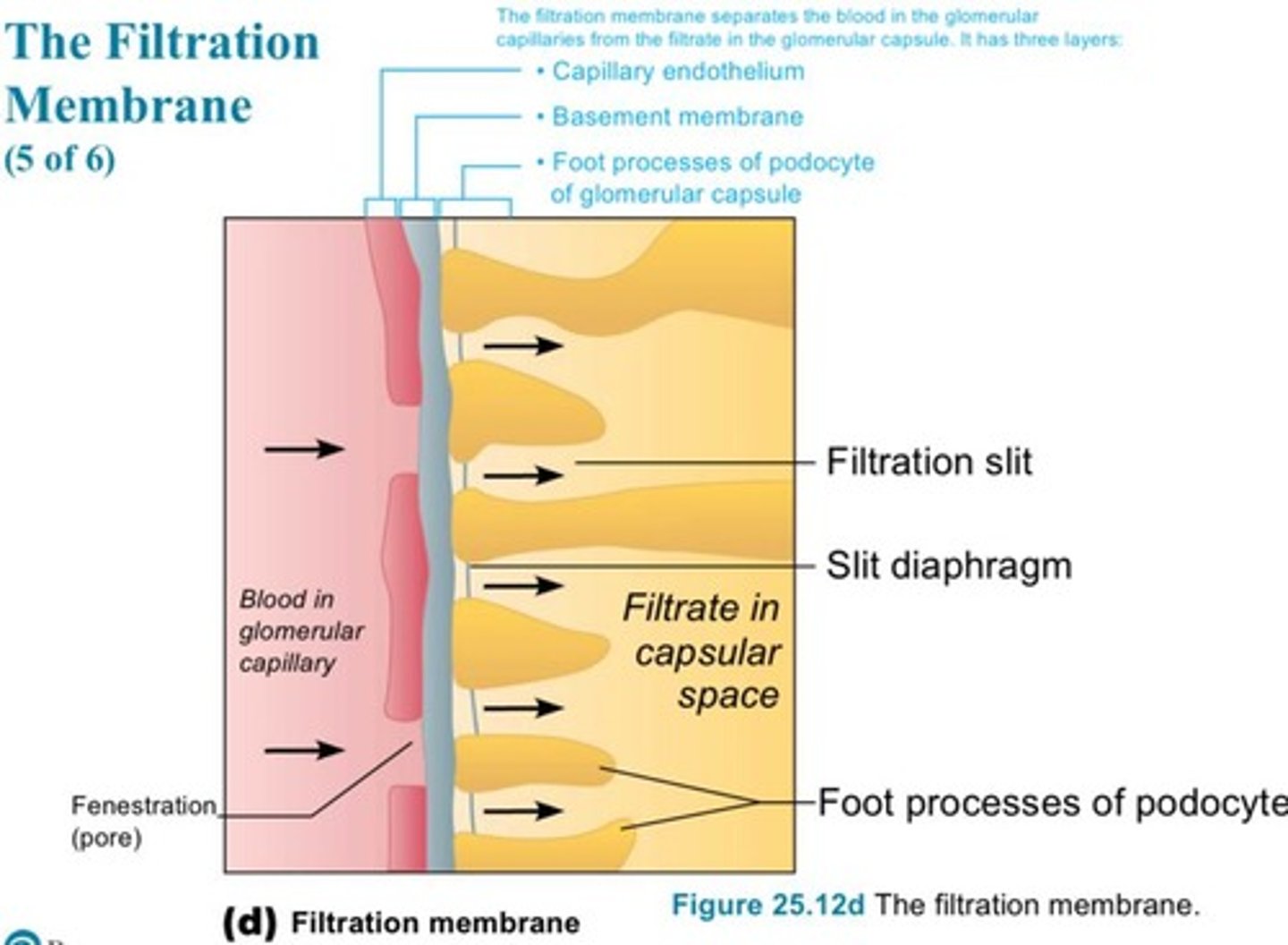
What is the filtration membrane composed of?
Fenestrated endothelium, basement membrane, and foot processes of podocytes
What is the function of vasa recta?
To function in the formation of concentrated urine
What is the significance of the high blood pressure in the glomerulus?
It facilitates the filtration process
What are the inward pressures that inhibit filtrate formation?
Hydrostatic pressure in capsular space and colloid osmotic pressure in capillaries
What is the effect of increased GFR on urine output?
Increased urine output, which lowers blood pressure
What are some chemicals released by renal cells that affect GFR?
Adenosine and Prostaglandin E2
What is the role of locally acting angiotensin II in the kidneys?
It reinforces the effects of hormonal angiotensin II.
What is anuria?
An abnormally low urinary output of less than 50 ml/day.
What may indicate that glomerular blood pressure is too low?
Anuria, as it suggests insufficient pressure to cause filtration.
What are some conditions that can lead to renal failure and anuria?
Acute nephritis, transfusion reactions, and crush injuries.
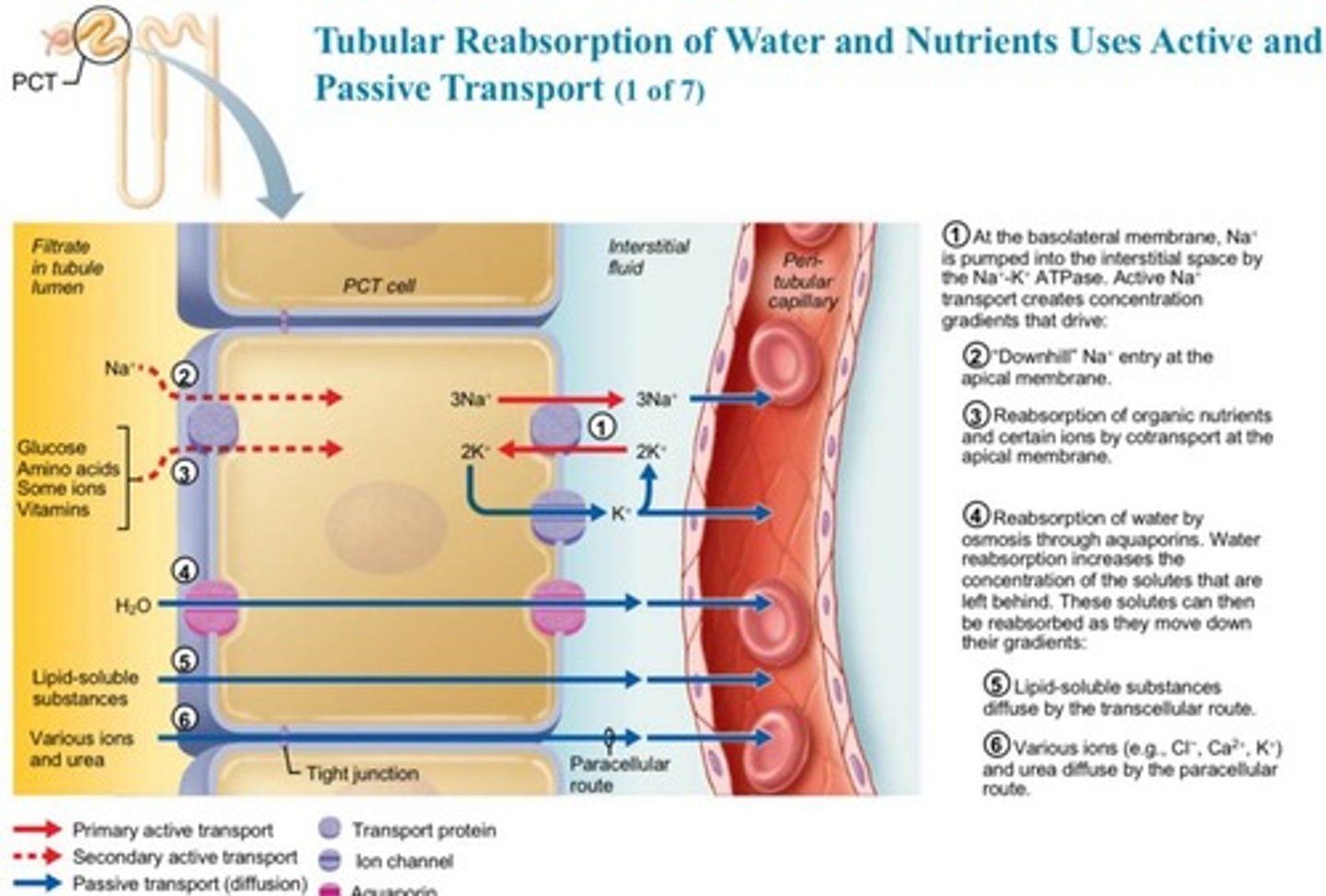
What is the transcellular route in tubular reabsorption?
Solute enters the apical membrane of tubule cells, travels through the cytosol, exits the basolateral membrane, and enters blood through the endothelium of peritubular capillaries.
What is the paracellular route in the nephron?
The paracellular route is the movement of substances between tubule cells, limited by tight junctions but leaky in the proximal nephron.
What substances move via the paracellular route in the proximal convoluted tubule (PCT)?
Water, Ca2+, Mg2+, K+, and some Na+.
How is sodium transported across the basolateral membrane of tubule cells?
Sodium is transported via primary active transport through Na+−K+ ATPase pumps.
What happens to Na+ after it is pumped into the interstitial space?
Na+ is swept by bulk flow into peritubular capillaries.
How does Na+ enter the tubule cell at the apical surface?
Na+ enters via secondary active transport (cotransport) or facilitated diffusion through channels.
What creates the electrochemical gradient within the tubule cell?
Active pumping of Na+ at the basolateral membrane results in low intracellular Na+ levels.
What is the role of Na+ reabsorption in tubular reabsorption?
Na+ reabsorption provides energy and means for reabsorbing almost every other substance.
What is secondary active transport in the context of tubular reabsorption?
It is when the electrochemical gradient created by pumps at the basolateral surface pushes the transport of other solutes.
What substances are cotransported with Na+ during reabsorption?
Glucose, amino acids, some ions, and vitamins.
How is water reabsorbed in the nephron?
Water is reabsorbed by osmosis, aided by aquaporins.
What is obligatory water reabsorption?
Water reabsorption that occurs through aquaporins that are always present in the PCT.
What is facultative water reabsorption?
Water reabsorption that occurs when aquaporins are inserted in collecting ducts only if ADH is present.
What happens to solute concentration in filtrate as water is reabsorbed?
Solute concentration increases, creating gradients that drive solutes into tubule cells and peritubular capillaries.
What is the primary site of reabsorption in the nephron?
The proximal convoluted tubule (PCT).
What percentage of Na+ and water is reabsorbed in the PCT?
65% of Na+ and water.
What occurs in the descending limb of the nephron loop?
H2O can leave, but solutes cannot.
What occurs in the ascending limb of the nephron loop?
H2O cannot leave, but solutes can.
What hormones regulate reabsorption in the distal convoluted tubule and collecting duct?
Antidiuretic hormone (ADH) and aldosterone.
What is the function of ADH?
ADH causes principal cells of collecting ducts to insert aquaporins, increasing water reabsorption.
What is the role of aldosterone in the nephron?
Aldosterone promotes synthesis of Na+ and K+ channels and Na+−K+ ATPases for Na+ reabsorption.
What is the effect of atrial natriuretic peptide?
It reduces blood Na+, resulting in decreased blood volume and pressure.
What does parathyroid hormone do in the nephron?
It acts on the distal convoluted tubule to increase Ca2+ reabsorption.
What is tubular secretion?
It is the process of moving selected substances from peritubular capillaries through tubule cells into the filtrate.
What substances are commonly secreted during tubular secretion?
K+, H+, NH4+, creatinine, organic acids and bases.
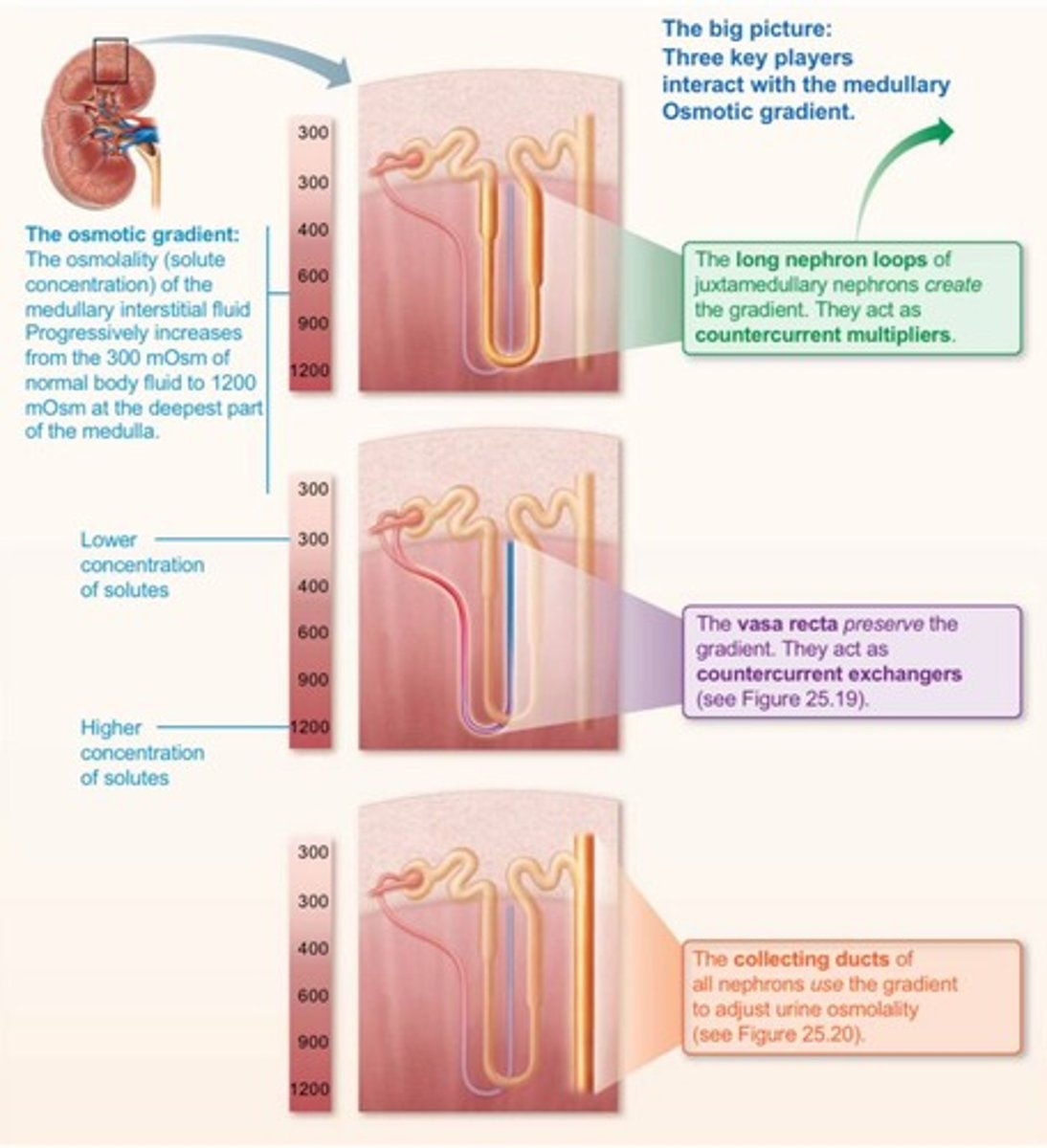
What is the main function of the kidneys regarding body fluid osmotic concentration?
To maintain body fluid osmotic concentration at around 300 mOsm.
What is the countercurrent mechanism in the kidneys?
It involves fluid flowing in opposite directions in two adjacent segments of the same tube with a hairpin turn.
What are the two types of countercurrent mechanisms?
Countercurrent multiplier and countercurrent exchanger.
What does the collecting duct use to vary urine concentration?
The established medullary osmotic gradient.
What happens to urine concentration during dehydration?
Maximal ADH is released, producing concentrated urine (~1200 mOsm).
What are diuretics?
Chemicals that enhance urinary output by inhibiting reabsorption of Na+ and water.
What is the chemical composition of urine?
95% water and 5% solutes, including nitrogenous wastes like urea, uric acid, and creatinine.
What does a urinalysis examine?
Urine for signs of disease and can be used to test for illegal substances.
What defines chronic renal disease?
A GFR < 60 ml/min for 3 months.
What are the symptoms of renal failure?
Fatigue, anorexia, nausea, mental changes, and cramps.
What is GFR?
Glomerular Filtration Rate, a measure of how well the kidneys filter blood.
What factors can affect GFR?
Renal cells release chemicals such as adenosine and prostaglandin E2 that act on renal arterioles.
What conditions can lead to anuria?
Conditions such as acute nephritis, transfusion reactions, and crush injuries.
What are the two routes of tubular reabsorption?
Transcellular route and paracellular route.
Describe the transcellular route.
Solutes enter the apical membrane of tubule cells, travel through cytosol, exit the basolateral membrane, and enter blood.
What solutes typically move via the paracellular route?
Water, Ca2+, Mg2+, K+, and some Na+ in the proximal convoluted tubule (PCT).
How is sodium reabsorbed in the renal tubules?
Sodium is reabsorbed via primary active transport across the basolateral membrane by Na+−K+ ATPase.
What hormone regulates water reabsorption in the collecting ducts?
Antidiuretic hormone (ADH) increases water reabsorption by inserting aquaporins in the apical membranes.
What is the function of aldosterone in the kidneys?
Aldosterone promotes Na+ reabsorption and K+ secretion in the distal convoluted tubule and collecting ducts.
What is the primary function of the kidneys regarding urine concentration?
To maintain body fluid osmotic concentration around 300 mOsm.
What is the countercurrent mechanism?
A process where fluid flows in opposite directions in adjacent segments of the nephron to establish a medullary osmotic gradient.
What is the difference between dilute and concentrated urine formation?
Dilute urine is produced with low ADH levels, while concentrated urine is produced with high ADH levels.