Chapter 20: The Circulatory System: Blood Vessels and Circulationary
1/42
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
43 Terms
arteriole
small artery
what arteries do?
carry blood away from the heart
What do veins do?
carry blood toward the heart
What are capillaries?
microscopic, thin-walled vessels that connect the smallest arteries to the smallest veins
What do capillaries do?
the site of the transfer of materials into and out of tissues
venule
small vein
Exchange of materials (gases, nutrients, wastes,
hormones, etc.) with the tissues occurs only in
capillaries and in some venules
No cell in the body is more than about five cell
widths away from a _blank_ (except in ligaments, tendons, cartilage, cornea, and the lens).
capillaries
capillary exchange
passage of materials across the walls of capillaries
what are the three routes of capillary exchange?
Through the endothelial cells, spaces between the endothelial cells, and the filtration pores of fenestrated
capillaries
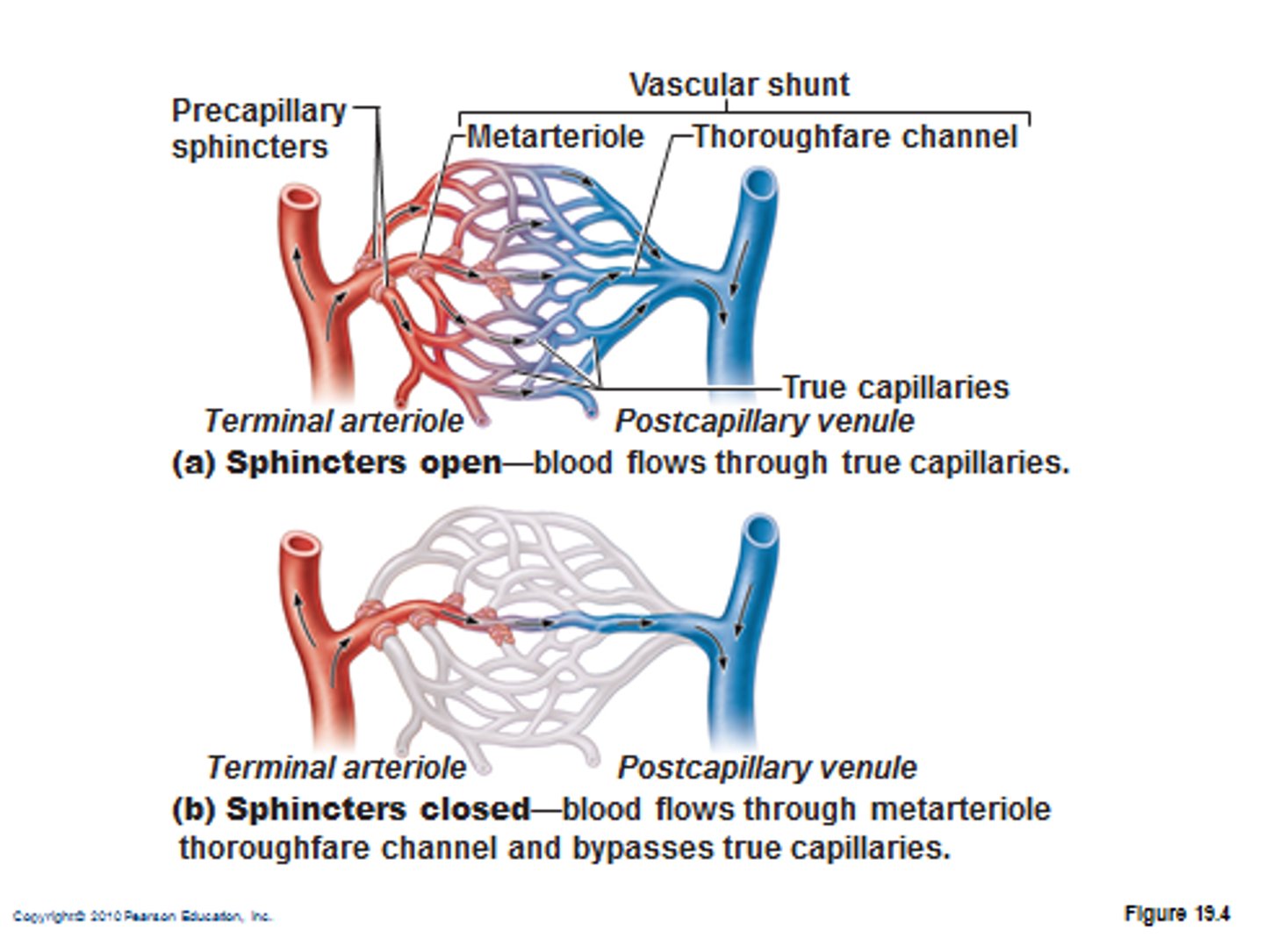
capillary beds
arrangement of capillaries in web-like networks
how can flow to particular capillaries be regulated?
constriction or dilation of upstream arterioles or by precapillary sphincters
what is blood flow?
the amount of blood flowing through an organ, tissue, or blood vessel in a given amount of time (mL/min)
How is pressure and resistance related to blood flow?
blood flow=
Difference in Pressure/Resistance
what is blood pressure?
the force that blood exerts against the wall of a vessel
how can blood pressure be measured directly?
by inserting a catheter or needle connected to an external manometer
How is blood pressure typically measured?
we take blood pressure from the brachial artery as an approximation using a sphygmomanometer to measure it.
systolic pressure
the peak pressure recorded during ventricular systole

diastolic pressure
the minimum arterial pressure, measured during ventricular diastole.
what is pulse pressure?
The difference between the systolic and diastolic pressure
what is mean arterial pressure?
average pressure in the arteries
how can mean arterial pressure be calculated?
MAP=1/3 systolic pressure + 2/3 diastolic
How can gravity affect mean arterial pressure?
in a standing person,MAP is about 62 mm Hg in arteries of the head and about 180 mm Hg in arteries of the ankle
What is hypotension?
chronic low blood pressure
what is hypertension?
a chronic resting blood pressure higher than 140/90.
what are the health complications of long-term hypertension?
Heart Attack - due to atherosclerosis
Stroke - due to atherosclerosis
Heart Failure
Aneurysm
Metabolic Syndrome - high "bad" cholesterol,
low "good" cholesterol, high tryglycerides,
high insulin levels, extra body weight. Can
lead to heart disease, stroke, and diabetes
mellitus.
how does arteriosclerosis affect blood pressure?
Blood pressure increases with age as the arteries become less distensible
what is atherosclerosis?
The growth of lipid deposits in the walls of the arteries that can calcify and cause rigidity. High blood pressure.
what is blood pressured determined by?
cardiac output, blood volume, and resistance to flow
what are the three factors upon which peripheral resistance depends?
Blood viscosity, vessel length, Vessel Radius (can be altered via vasoconstriction and vasodilation)
what are bareoreflexes?
Neural Control
what structures are involved in baroreflexes?
Baroreceptors can be found in the aortic arch
and in the carotid sinuses (at base of internal
carotid artery).
What happens to baroreflexes if blood pressure is high?
this causes decreases in heart
rate/cardiac output and vasodilation in general.
This is regulated through the autonomic nervous
system.
what are chemoreflexes?
Neural Control
what structures are involved with chemoreflexes?
Chemoreceptors for oxygen, carbon dioxide,
and pH are found in the aortic arch and in the
carotid bodies (at base of external carotid
artery)
what happens to chemoreflexes if oxygen levels are low or if carbon dioxide or acidity levels are high?
cause widespread vasoconstriction. This increases overall BP, increasing blood flow to the lungs to promote
gas exchange. Respiration rate is also
increased.
aldostereone
promotes sodium and water retention in the kidneys
Angiotensin II
causes vasoconstriction
Antidiuretic hormone
promotes water retention, but it will also cause vasoconstriction.
Epinephrine/Norepinephrine
cause vasoconstriction in most blood vessels to increase blood pressure in the main arteries. This allows for increased blood flow to the brain, heart, and skeletal muscles.
what is Venous Return?
The flow of blood back to the heart
what are the five mechanisms that assist with Venous Return?
1.Pressure Gradient - Pressure falls as we
move from venules to the venae cavae.
This promotes flow toward the heart.
2.Gravity - At least from the head and neck.
3. The Skeletal Muscle Pump - Contractions of
muscles and presence of valves pushes blood
in one direction.
4. The Thoracic Pump - When you inhale, the
thoracic cavity expands and thoracic pressure
drops, while at the same time the diaphragm
moves downward to increase abdominal
pressure. This moves blood toward the thoracic
cavity.
5. Cardiac Suction - Suction from the empty atria
draws blood in.