Psychiatry Matrix
1/70
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
71 Terms
Psychosis
Impaired perception of reality through one or more of:
Hallucinations (sensory abnormalities w no stimuli)
Delusions (fixed false beliefs inconsistent to cultural/social norms)
Disorganised thinking, speech or behaviour
Primary Psychosis: results from psychiatric disorder (e.g. Schizophrenia)
Secondary Psychosis: results from general medical condition and/or the effect of a substance (inf., endocrine, neurological = stroke/tumour, autoimmune = SLE, B12 def.)
Psychotic Disorder: disease/condition producing psychosis
Schizophrenia Dx (R1)
Pos, Neg and Cognitive signs/sx of Psychosis persist for >6m, PLUS Social and Functional decline:
A) 2+ for >1m of: 1) Delusions, 2) Hallucinations, 3) Disorganised Speech, PLUS 4) Grossly Disorganised or Catatonic Behaviour, 5) Neg. Sx (dec. emotions)
B) Severe impact on function ability (work, care etc)
C) Duration persists >6m (Criteria A = >1m)
D) Ruled out Schizoaffective, Depressive or Bipolar
E) Ruled out attribution to effects of substances
RF: Genetics, Substances, Environmental/Psychosocial
Men = 18-25
Women = 25-35 (menarch) + >40 (menopause)
Late Onset Schizophrenia: >40-60, W>M, fewer neg. sx
Screening Tools:
PANSS (Pos + Neg Sx Scale)
BPRS (Bried Psychiatric Rating Scale)
Screen for organic cause (CRP, TSH, Urine)
MSE: A/B: poor, disorganised; M: abnorm; S: abnorm, delusions; C: low/distracted; R: __; I: impaired; J: impaired; P: hallucinations
Substance‑Induced Psychosis (R1)
Psychosis must be a direct consequence of substance USE or WITHDRAWAL
Sx development is related to the time the substance was last ingested, and sx duration is usually brief
Causes:
1. Recreational: Alcohol, Hallucinogens, Cocaine, Cannabis, Amphetamines
2. Medications: Analgesics (Opioids), Antihistamines, Sedatives/Hypnotics, Antidepressants (SSRIs), Benzo, Antiparkinsons (dopaminergics), Corticosteroids
Substance-Induced Psychotic Disorder: when sx outlast expected intoxication/withdrawal duration (however, >4wks indicates other psychotic disorders)
Schizoaffective Disorder (R2)
Mix of Schizophrenia and Bipolar Disorder (Psychosis AND Mania) for >2wks
A) Period of either: 1) Major Depressive Eps, 2) Manic Ep, 3) Mixed Ep with Schizophrenia sx of Criteria A
B) Delusions or Hallucinations for >2wks in SAME period of illness as Criteria A WITHOUT Mood Sx
C) Sx of Mood Ep. for majority of illness period
D) Ruled out attribution to effects of substances
Schizophreniform Disorder (R2)
Schizophrenic sx for a shorter duration of 1-6m
2/3 Pts develop Schizophrenia or Schizoaffective dis.
Criteria:
A) 2+ for >1m of: 1) Delusions, 2) Hallucinations, 3) Disorganised Speech, PLUS 4) Grossly Disorganised or Catatonic Behaviour, 5) Neg. Sx (dec. emotions)
B) Severe impact on function ability (work, care etc)
C) Duration persists 1-6m
D) Ruled out Schizoaffective, Depressive or Bipolar
E) Ruled out attribution to effects of substances
Delusional Disorder (R3)
At least 1 delusion
No other prominent psychotic sx (hallucinations, disorganised speech, negative sx)
A) Nonbizarre delusions >1m (i.e., involving situations that occur in real life, such as being followed, poisoned, infected, loved at a distance, or deceived by spouse or lover, or having a disease)
B) Criterion A for Schizophrenia has never been met
C) Functioning/Behaviour not impaired apart from the ramifications of the particular delusion
D) Any assoc. Mood Eps. have been comparatively brief
E) Ruled out attribution to effects of substances
Nonbizzare Del: can be true +/or consistent w cultural/social norms
Bizzarre Del: canNOT be true +/or inconsistent w cultural/social norms
Grandiose Del: insists special powers/importance
Brief Psychotic Disorder (R3)
A) Presence of >1 of: 1) Delusions, 2) Hallucinations, 3) Disorganised Speech, 4) Disorganised/Catatonic Behaviour
B) Duration is >1d BUT <1m with FULL functional return
C) Have Ruled out Mood Disorder With Psychotic Features, Schizoaffective Disorder, Schizophrenia or Substance Effects
RF: Stressful life event
Psychotic Disorders Mx
Screen for: past Dx of Psychosis, onset (sudden = 2°), head trauma, meds/drug hx, PMHx (Cushings, autoim, THYROID DISEASE!), Life Stressors, FHx
Ix: TFT, BMP, CBC, LFTs, ESR, ANA, Vit B12, Thiamine, HIV/Syphilis, Preg., Urine Tox, MRI/CT Head, EEG
Mx:
Psychosocial Intervs: better for neg/cog sx (CBTp)
Antipsychotic Medications:
*1st Line = Aripiprazole, Risperidone, Olanzapine, Quetiapine (SGAs); Haloperidol, Chlorpromazine (FGAs)
*Tx Resistant = Clozapine following failure of TWO different antipsychotics each for ≥ 6wks (requires CBC for neutropenia risk monitoring, AEs = constipation, myocard.)
1st Gens (FGA) = dopamine receptors (muscular sx)
2nd Gens (SGA) = dopamine + serotonin (metabolic sx => monitor lipids, weight and BGLs) - SGA > FGA
Ari = young pts/ASD, acathesia (restlessness)
Risp = young pts/ASD, hyperprolactinaemia/galactorrhea
Olanz = weight gain/metabolic issues (O = wide)
Quet = sedating (Quet = Quiet)
Halo = Dystonia + NMS risk, EPSEs, hyperprolact., QT risk
Chlor = anticholinergic effects, photosens., HYPOtension
Bipolar I Disorder (R1)
Manic episodes >1wk OR causing hospitalisation NOT due to an organic/substance related cause
RF = FHx!!!, Age (18-30)
VERY High Risk of Suicide - Do Risk Assessment
Manic Eps = distinct periods of abnormally and persistently elevated, expansive, or irritable mood, PLUS abnormally and persistently increased energy or activity
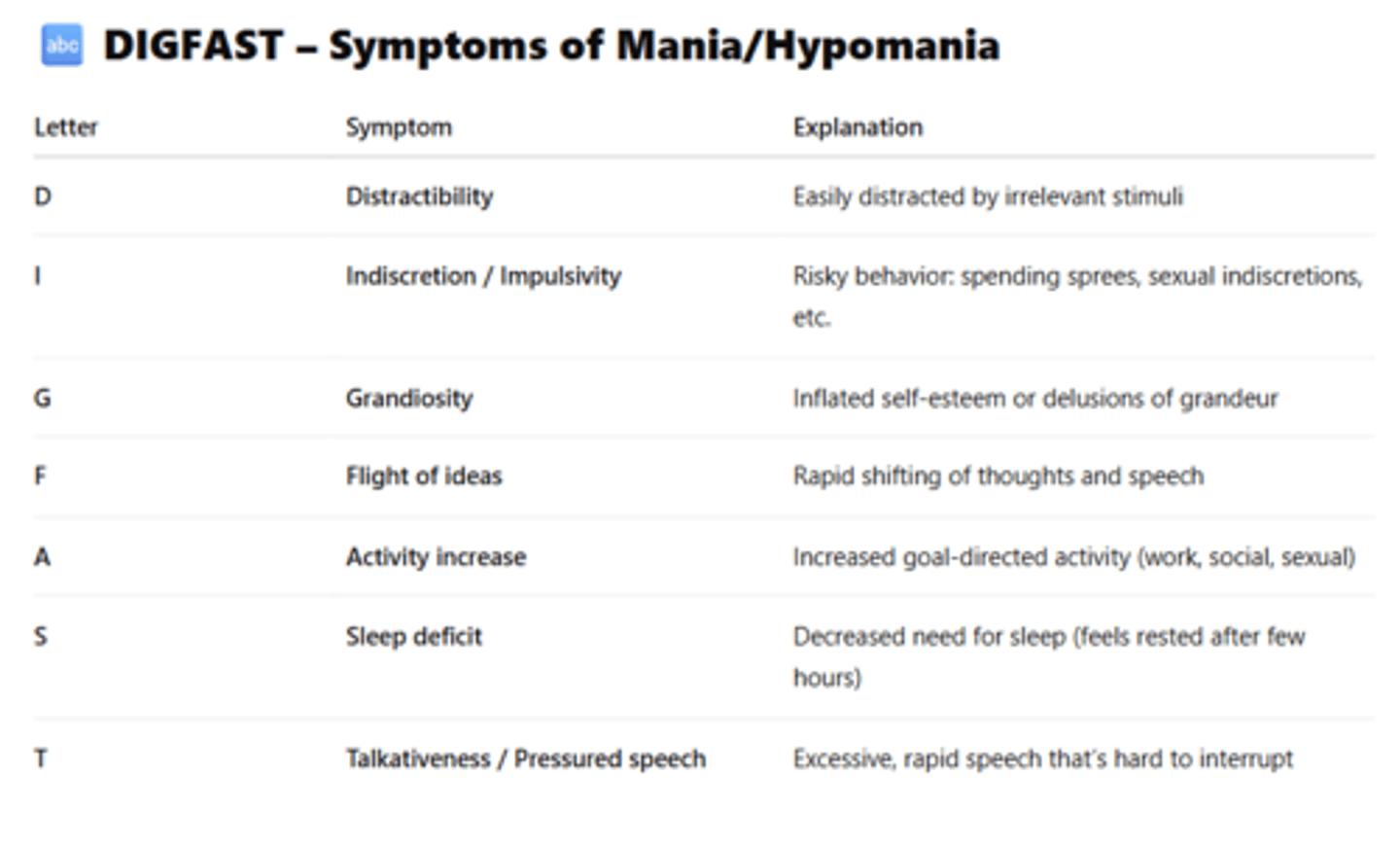
3+ sx of DIGFAST:
1) Distractibility: attention draws easily to irrelevant stimuli
2) Impulsivity/High-Risk Behavior: excessive activities with painful consequences (e.g., buying sprees, sexual indiscretions)
3) Grandiosity: Inflated self-esteem
4) Flight of Ideas/Racing Thoughts
5) Activity Increase/Goal-Directed Activity: increased energy at work, school, or socially, +/- psychomotor agitation
6) Sleep Def/Decreased Sleep: feeling rested after only a few hours
7) Talkativeness: pressured speec
Bipolar II Disorder (R2)
Hypomanic (low levels of mania) >4d
PLUS
Major Depressive episode >2wks
WITHOUT
Full manic episode/Major functional impairment

Drug‑Induced Mania (R3)
Mania distinct from a primary (non-substance-induced) bipolar disorder
Sx preceding the substance use, or persisting for a SIGNIFICANT TIME (>1m) after cessation
Substance Abuse: Usually cocaine and amphetamines, can be caused by ETOH, cannabis, opioids etc
Medications: antiparkinsonian drugs, corticosteroids, thyroxine
Suspicious for pts with mania age >35yrs
Cyclothymic Disorder (R3)
Episodes of hypomania and depression that:
1) Do not meet the full DSM‑5 diagnostic criteria for hypomania or major depressive disorder
2) Present at least half the time during a 2‑year period with ≤ 2 months of symptom remission
Bipolar and Related Disorders Mx
Consider ceasing antidepressants which can cause mania, should only use (SSRIs preferred) WITH Mood Stabilisers
Address triggers (sleep dep,. substance use)
Electroconvulsive Therapy (ECT) for sev./med intolerant
Medications: Combination Therapy (1 + 2) for Mod-Sev.
1) Mood Stabilisers: Lithium (1st), Valproate (Avoid in Preg.), Lamotrigine (ONLY for depressive eps/depres-prominent)*
2) Antipsychotics: SGAs preferred (Aripip, Risp, Olanz, Quet)
3) Benzodiazepines: Lorazepam (for SHORT TERM and SEVERE: agitation, insomnia, behavioural disturbances)
Bipolar Depression: Quetiapine monotherapy, Lithium, Lamotrigine (more for prevention, slower onset), Lurasidone (often with lithium or valproate)
*Do NOT give high dose of Lamotrigine or Lam + Val due to high risk of SJS/TENS (skin burns)
Major Depressive Disorder (R1)
>5 sx from the 9 Sx Domains for >2wks including at least one of:
1) Depressed mood
2) Loss of interest or pleasure (anhedonia)
PLUS Functional Impact/Distress (Social, Occup. etc)
NOT attributable to a substance or medical condition
NO Hx of Mania/Hypomania Eps (rule out Bipolar)
The 9 symptom domains:
1) Depressed mood most of the day, nearly every day
2) Markedly reduced interest or pleasure in most activities
3) Significant weight loss or gain, or appetite change
4) Insomnia or hypersomnia
5) Psychomotor agitation or retardation (observable by others)
6) Fatigue or loss of energy
7) Feel worthless or excessive/inappropriate guilt
8) Reduced concentration or indecisiveness
9) Recurrent thoughts of death, suicidal ideation, or suicide attempt
Substance‑Induced Depressive Disorder (R3)
Clinically significant depressive syndrome that:
1) Develops during or soon after substance intoxication, withdrawal, or medication exposure
2) Is attributable to that substance
3) Is not better explained by a primary depressive disorder
Substance/Med is capable of causing depressive sx
E.g. ETOH, Opioids, Sedatives/Hypnotics, Stimulant Withdrawal, Other Prescribed Meds
Persistent Depressive Disorder/Dysthymia (R3)
Chronic depressive condition characterised by:
1) Depressed mood for most days for >2yrs (>1yr for children/adolescents: will be irritable > sad)
2) >2 additional depressive sx
3) No prolonged symptom‑free periods (not >2m)
4) No history of mania or hypomania
Disruptive Mood Dysregulation Disorder/DMDD (R3)
Childhood disorder characterised by severe, chronic irritability, rather than episodic mood elevation
A) Frequent Severe Temper Outbursts (Verbal/Behav)
B) Persistent Irritable Mood/Anger (close to 24/7)
C) Frequency of Temper Outbursts >3 times/wk
D) Duration >12m, No sx-free period >3m (consec.)
E) Sx in >2 settings (sev. in >1): home, school, w peers
F) Dx age only bw 6-18yrs (onset sx before 10yrs)
G) Exclusion of Mania/Not Better Explained by Another Dx/Disorder or Substances/Med. Condition
Disruptive mood dysregulation disorder is a childhood condition characterised by severe, recurrent temper outbursts and persistent irritability lasting at least 12 months across multiple settings, with onset before age 10 and no history of manic or hypomanic episodes
Depressive/Mood Disorders Mx
Antidepressants:
1) SSRIs
2) SNRIs/Other ()
SSRIs:
Sertriline: all-rounder, 1st line, min AEs,
Fluoxetine: min AEs, more activating than Sert (gives energy)
Generalised Anxiety Disorder/GAD (R1)
>6m of Excessive Worry about Everyday Issues that:
1) Is disproportionate to any inherent risk
2) Causes distress or impairment
3) Is hard to control
>3 sx are present most of the time:
1) Restlessness or nervousness
2) Being easily fatigued
3) Poor concentration
4) Irritability
5) Muscle tension
6) Sleep disturbance
Panic Disorder (R2)
Recurring unexpected panic attacks over >1m
Patient remains persistently concerned/anxious about having another attack
Not Due to Subs/Med Conds/Other Mental Disorders
At least one panic attack is followed by ≥1 month of one or both of:
1) Persistent concern/worry about panic attacks or their consequences
2) Persistent concern or worry about
Panic Attacks: sudden onset of intense physical and cognitive symptoms of anxiety that may be triggered by specific cues or occur unexpectedly
Agoraphobia (R2)
A = Marked fear or anxiety for >6m regarding >2 of:
1) Using public transport (e.g. buses, trains, planes)
2) Being in open spaces (e.g. car parks, marketplaces)
3) Being in enclosed spaces (e.g. shops, cinemas)
4) Standing in line or being in a crowd
5) Being outside the home alone
B = Reason for fear is hard to escape/get help
C = Situations are avoided/endured w distress/need a companion due to provoking fear/anxiety
D = Fear is out of proportion to posed danger
E = Functional Impairment (social, occupational etc)
F = Not better explained by another disorder
Can be diagnosed with/without panic disorder
Specific Phobias (R2)
intense fears of SPECIFIC OBJECTS or SITUATIONS persistent for >6m that are triggered upon actual or anticipated exposure to phobic stimuli
Exposure to the phobic stimulus almost always provokes immediate fear or anxiety
Situations w phobic cues are avoided/endured with intense anxiety
Excessive fears can cause functional impairments or lifestyle disruptions and is out of proportion
Mx = Exposure Therapy/CBT, Benzos for infrequent sx
Anxiety Disorders Mx
Obsessive‑Compulsive Disorder (R1)
Presence of one or both of:
A) Obsessions: recurrent/persistent thoughts, urges or images that are intrusive/unwanted causing anxiety or distress (attempt to ignore/neutralise)
B) Compulsions: repetitive behaviours/mental acts in response to an obsession aiming to prevent/reduce anxiety or distress that pt feels driven to perform
Obsessions/Compulsions are Time Consuming (>1hr/d) or cause distress/impaired functioning
Not better explained by sub./condition/disorder
Mx = Pharm + CBT/ERP
Body Dysmorphic Disorder/BDD (R3)
A) Preoccupation with appearance: >1 perceived flaws or defects not observable/apparent to others
B) Repetitive Behaviours/Mental Acts (skin pick etc)
C) Clinically Significant Distress or Impairment
D) Not Better Explained by an Eating Disorder
Muscle Dysmorphia Specifier: Preoccupation that the body is too small or insufficiently muscular (M > F)
Mx = Pharm + ERP
Hoarding Disorder (R3)
A) Persistent Difficulty Discarding Possessions (value regardless, perceived need to save items)
B) Accumulation/Clutter due to difficulty discarding
C) Clinically Significant Distress or Impairment
D) Not better explained by sub./condition/disorder
Mx = CBT
Trichotillomania (R3)
A) Recurrent pulling out of hair, resulting in hair loss
B) Repeated Attempts to Stop
C) Clinically Significant Distress or Impairment
D) Not better explained by sub./condition/disorder
Mx = HRT
Excoriation Disorder (R3)
A) Recurrent skin picking, resulting in skin lesions
B) Repeated Attempts to Stop
C) Clinically Significant Distress or Impairment
D) Not better explained by sub./condition/disorder
Mx = Pharm + HRT
Obsessive‑Compulsive & Related Disorders Mx
Non-Pharm: CBT/ERP!/HRT
Pharm: SSRIs +/- Tricyclic Antis (Clomipramine)
Do not give citalopram to BDD
ERP (Exp + Response Prev): systematic exposure to feared stimuli while preventing compulsive behaviours to reduce anxiety
HRT (Habit Revers Train): identifies triggers and substitutes behaviors
Clomipramine: Seratonin-Specific, Less Tolerated than SSRIs
Post Traumatic Stress Disorder - PTSD (R1)
All 4 Groups of sx for >1m following exp. to trauma:
1) Intrusion symptoms ≥1 (memories, reactions, etc)
2) Avoidance ≥1 (memories, reminders/places etc)
3) Negative alterations in cognition and mood ≥2 (e.g. inhibited memory, blame, neg. beliefs/emotions)
4) Alterations in arousal and reactivity ≥2 (irritable, reckless, sleep disturbance, dec. concentration etc)
Sx cause functional impairment
Trauma = actual/threatened death, serious injury, or sexual violence through direct experience, witnessing, of learning of from close family/friend
Acute Stress Disorder (R2)
Sx for 3d-1m, within 4wks following exp. to trauma
1) Intrusion symptoms ≥1 (memories, reactions, etc)
2) Avoidance ≥1 (memories, reminders/places etc)
3) Negative alterations in cognition and mood ≥2 (e.g. inhibited memory, blame, neg. beliefs/emotions)
4) Alterations in arousal and reactivity ≥2 (irritable, reckless, sleep disturbance, dec. concentration etc)
Sx cause functional impairment
Adjustment Disorders (R2)
A) Emotional or behavioural sx within 3m of an identifiable stressor
B) Causes disproportionate distress or functional impairment
C) Not better explained by sub./condition/disorder
D) Resolves within 6m of the stressor ending
Trauma & Stress‑Related Disorders Mx
Mild/Mod Sx <3m: active monitoring, supportive
Severe <3m or Sx ≥3: Psych Therapy, Pharm
Trauma-focused cognitive behavioural therapy (TFCBT)
Eye movement desensitisation and reprocessing (EMDR)
Pharm: 1st = SSRIs, SNRIs (Venlafaxine, monitor BP), Mirtazapine (for insomnia), Prazosin (nightmares)
Dissociative Identity Disorder (R3)
A) Presence of >2 distinct identities (alters) that control a person's behavior, often caused by severe, chronic childhood trauma
B) Causes recurrent amnesia/gaps in recall
C) Clinically Significant Distress or Impairment
D) Not a Normal Cultural or Religious Practice
E) Not Due to Substances or Medical Conditions
Dissociative Amnesia (R3)
A) Inability to Recall Important Information, usually following trauma/stress and is inconsistent with ordinary forgetting
B) Clinically Significant Distress or Impairment
C) Not better explained by sub./condition/disorder
Depersonalisation/Derealisation Disorder (R3)
A) Persistent or Recurrent Experiences of one or Both of: 1) Depersonalisation (robotic), 2) Derealisation (detachment)
B) Reality Testing Remains Intact
C) Clinically Significant Distress or Impairment
D) Not better explained by sub./condition/disorder
Dissociative Disorder Mx
Psychotherapy, CBT
Psychoeducation
Borderline Personality Disorder/BPD (R1) - Cluster B
Personality and Emotional Regulation Disorder
Pervasive pattern of instability in affect, self‑image, and interpersonal relationships with marked impulsivity
>5 of IMPULSIVE:
1) Impulsivity in >2 potentially self‑damaging areas (e.g. sex, money, substances)
2) Moodiness
3) Paranoia: Transient, stress‑related paranoid ideation or severe dissociative symptoms
4) Unstable self image/Identity disturbance
5) Labile intensive relationships: Unstable and intense interpersonal relationships
6) Suicidal: Recurrent suicidal behaviour, gestures, threats, or self‑mutilating behaviour
7) Inappropriate/intense anger or difficulty controlling anger
8) Vulnerability or abandonment
9) Emptiness: Chronic feelings of emptiness
Mood fluctuations over the course of the DAY/short periods (Bipolar = over longer periods/episodic/wks)
Feel unsafe in relationships, threat of abandonment
RF = genetics, trauma, difficult relationships
Usually emerges in adolescence or early adulthood
Is REVERSIBLE with Mx
Antisocial Personality Disorder (R2) - Cluster B
Pervasive pattern of disregard for and violation of the rights of others
Sx occur since age 15yrs, with dx made in adulthood
A) Pervasive Pattern of Antisocial Behaviour (failure to conform, impulsive, deceitful, reckless)
B) Age Requirement >18rs (must be an adult)
C) Evidence of Conduct Disorder Before Age 15
D) Exclusion Criteria: Antisocial behaviour does not occur exclusively during schizo/bipolar/mania
Narcissistic Personality Disorder (R2) - Cluster B
Pervasive pattern of grandiosity, need for admiration, and lack of empathy, beginning by early adulthood
>5 of:
1) Grandiose sense of self‑importance
2) Preoccupation with fantasies (success, power etc)
3) Belief of being "special" and unique
4) Requires excessive admiration
5) Sense of entitlement
6) Interpersonally exploitative behaviour
7) Lack of empathy
8) Envy of others/belief others envy them
9) Arrogant, haughty behaviours or attitudes
Traits are Pervasive, Inflexible, Maladaptive
Not better explained by Mood disorders (e.g. mania), Substance use or Cultural/Occupational norms
Obsessive‑Compulsive Personality Disorder (R2) - Cluster C
Pervasive pattern of preoccupation with orderliness, perfectionism, and control
>4 of:
1) Preoccupation with details, rules, lists, order, organisation, or schedules
2) Perfectionism that interferes with task completion
3) Excessive devotion to work and productivity (not explained by financial necessity)
4) Overconscientiousness, scrupulousness, and inflexibility about morality, ethics, or values
5) Inability to discard worn‑out/worthless objects, even with no sentimental value
6) Reluctance to delegate tasks or work with others
7) Miserly spending style toward self/others (hoards)
8) Rigidity and Stubbornness
Diagnosed in adulthood
Personality trait rather than anxiety disorder (OCD)
Limited insight but usually no obsession/compulsions
Paranoid Personality Disorder (R3) - Cluster A
Pervasive pattern of distrust and suspicion of others
>4 of:
1) Suspects, without sufficient basis, that others are exploiting, harming, or deceiving them
2) Preoccupied with unjustified doubts about the loyalty or trustworthiness of friends or associates
3) Reluctant to confide in others
4) Reads hidden demeaning or threatening meanings into benign remarks or events
5) Persistently bears grudges (unforgiving of insults, injuries, slights)
6) Perceives attacks on character or reputation
7) Recurrent suspicions, without justification, of the fidelity of a spouse/sexual partner
Disturbance does not occur exclusively during: Schizophrenia, Bipolar/Mania, Other Psych Disorder
Schizoid Personality Disorder (R3) - Cluster A
Pervasive pattern of detachment from social relationships and a restricted range of emotional expression
> 4 of:
1) Neither desires nor enjoys close relationships, including being part of a family
2) Almost always chooses solitary activities
3) Min-No interest in sexual experiences with another
4) Takes pleasure in few/any activities
5) Lacks close friends/confidants, except 1st‑degree relatives
6) Appears indifferent to praise/criticism from others
7) Shows emotional coldness, detachment, or flattened affectivity
Disturbance does not occur exclusively during: Schizophrenia, Bipolar/Mania, Other Psych Disorder
NOT Attributable to ASD or Medical/Neuro Condition
Schizotypal Personality Disorder (R3) - Cluster A
Pervasive pattern of social and interpersonal deficits, marked by: acute discomfort with close relationships, cognitive/perceptual distortions, eccentric behaviour
> 5 of:
1) Ideas of reference (exclude fixed delusions)
2) Odd beliefs or magical thinking (e.g. superstitions, clairvoyance, belief in special powers)
3) Unusual perceptual exp. (incl. bodily illusions)
4) Odd thinking/speech (e.g. vague, circumstantial, metaphorical, or over‑elaborate)
5) Suspiciousness or paranoid ideation
6) Inappropriate or constricted affect
7) Behaviour/appearance that is odd, eccentric, or peculiar
8) Lacks close friends/confidants, except 1st‑degree relatives
9) Excessive social anxiety (familiarity does not dec.)
Disturbance does not occur exclusively during: Schizophrenia, Bipolar/Mania, Other Psych Disorder
NOT Attributable to ASD or Medical/Neuro Condition
Histrionic Personality Disorder (R3) - Cluster B
Pervasive pattern of excessive emotionality and attention‑seeking
> 5 of:
1) Uncomfortable when not the centre of attention
2) Interactive behaviour with others is often inappropriate, sexually seductive or provocative
3) Rapidly shifting/shallow expression of emotions
4) Consistently uses physical appearance to draw attention to self
5) Style of speech is excessively impressionistic and lacking in detail
6) Self‑dramatisation, theatricality, and exaggerated expression of emotion
7) Suggestibility: easily influenced by others or circumstances
8) Considers relationships to be more intimate than they actually are
Traits must not occur exclusively during: Mood Disorders (e.g. mania) or Substance Intoxication
Must be pervasive and enduring, not situational
Avoidant Personality Disorder (R3) - Cluster C
Pervasive pattern of social inhibition, feelings of inadequacy, and hypersensitivity to negative evaluation
> 4 of:
1) Avoids occupational activities that involve significant interpersonal contact (due to fears of criticism, disapproval, or rejection)
2) Unwilling to get involved with people
3) Shows restraint within intimate relationships
4) Preoccupied with being criticised or rejected in social situations
5) Inhibited in new interpersonal situations
6) Views self as socially inept, personally unappealing, or inferior to others
7) Unusually reluctant to take personal risks/engage in new activities
Must not be better explained by: Social anxiety disorder alone, ASD, Mood disorders
Must be pervasive and enduring, not situational
Dependent Personality Disorder (R3) - Cluster C
Pervasive and excessive need to be taken care of, leading to submissive and clinging behaviour and fears of separation
> 5 of:
1) Difficulty making everyday decisions without excessive advice and reassurance from others
2) Needs others to assume responsibility
3) Difficulty expressing disagreement
4) Difficulty initiating projects or doing things independently
5) Goes to excessive lengths to obtain nurturance and support
6) Feels uncomfortable or helpless when alone
7) Urgently seeks another relationship when one ends
8) Unrealistic preoccupation with fears of being left to take care of themselves
Traits must not be better explained by: Major depressive dis, Anxiety dis, Medical illness
Must be pervasive and enduring, not situational
Personality Disorder Mx
Psychotherapy = 1st line!
Create Crisis/Risk Management Plan
Adjunct Pharmacotherapy for Comorbidites (SSRIs for Depression/Anxiety etc)
Cluster A: odd or eccentric
Cluster B: dramatic, emotional and erratic
Cluster C: anxious or fearful
Anorexia Nervosa (R1)
Restriction of caloric intake relative to requirements leading to:
1) Low body weight for age, height, gender and developmental status
2) An intense fear of gaining weight
3) A body image disturbance/Overvaluation of weight or shape as an expression of self-worth
Two Subtypes:
1) Restrictive: no binging, limiting food intake, compulsive exercise
2) Binge Eating and Purging: recurrent episodes of binge eating (uncontrolled overeating) and purging (eg self-induced vomiting, laxative or diuretic misuse)
Often have medical and psychological comorbidities (eg osteopenia, pancreatitis, depression, anxiety)
Hospitalise when BMI <15, BP <80 systolic, dec. vitals
Life-threatening Weight Loss: BMI <15 in adults, <75% of median BMI for age + sex in children/adolescents
Precipitous Weight Loss: LOW >1kg for two consecutive weeks
Bulimia Nervosa (R1)
Severe preoccupation about weight and body shape
1) Recurrent episodes of binge eating, loss of control over eating
2) Compensatory mechanisms to prevent weight gain (self-induced vomiting, fasting, excessive exercise)
3) Body weight in the adequate to obese range
Binge eating and compensatory behaviours occur at least once weekly for >3m
RF: women in 20s/30s, trauma hx
Common Signs: Parotid Hypertrophy, Tooth Erosion
Feeding & Eating Disorder Mx
CBT/Psychotherapy
Nutritional replenishment/Re-feeding
Dietitian Referral
Pharm:
AN: No evidence for pharmacological mx
BN: SSRIs (1st = Fluoxetine, Citalopram, Fluvoxamine, Sertraline) - for young adults
Mx comorbidities (depression etc) and beware of pregnancy
Alzheimer's Disease (R1)
Chronic, progressive neurodegenerative disorder with global, non-reversible impairment in cerebral functioning
A) Neurocognitive Decline + Memory Impairment
B) Insidious onset with gradual, steady decline
Deteriorating course over up to 8-10yrs
Brain lesions: neurofibrillary tangles, senile plaques, neuronal loss, brain atrophy, acetylcholine synth defects
Most common dementia but can coexist with others
RF = Age, FHx, Genetics, Down's Syn., Hyperlipidaemia, Cerebrovascular disease, Drugs, Unfinished School
Vascular Dementia (R1)
Chronic progressive impairment of cognitive function caused by loss of brain parenchyma
Predominantly from cerebrovascular causes (infarction, haemorrhage, small-vessel changes)
Damage to grey and white matter
Signs:
Loss of Executive Functions (planning etc) > Memory
Motor and mood changes are often seen early
RF: age >60, obesity, HTN, smoking, DM
IX: MRI Brain, Ix causes of cog decline (UEC, BGL, B12)
Treat early and aggressively to prevent further cerebrovascular disease/address causes
Frontotemporal Dementia (R2)
Neurodegenerative Dementia causing disruption in personality and social conduct ± primary language disorder (2nd most common after AD)
Sx: Parkinsonism (50% of pts), Language Impairment, Personality/Social Behaviour Decline, Altered Eating Habits, Inattentiveness, Impulsivity
Note: does not usually present w memory loss
RF: Age 45-65 (mid-life), FHx, Genetics
Lewy Body Dementia (R2)
Neurodegenerative disorder with Lewy Bodies characterised by:
Parkinsonism (Bradykinesia, Tremor, Rigidity)
Progressive cognitive decline (with fluctuations)
Prominent executive dysfunction
Behavioural and sleep disturbances (REM disorder)
Visuospatial impairment
Ix: Pathology shows presence of Lewy Bodies (Autopsy?), CT/MRI Head, Screening
Mx:
Behavioural = Cholinesterase Inhibitors (Donepezil and Rivastigmine are best for behavioural sx without motor sx exacerbation)
REM Disorder = Clonazepam/Melatonin
Motor Sx = Levodopa/Carbidopa
Lewy Bodies: toxic clumps formed by damaged alpha-synuclein proteins folding into irregular shapes (linked to progressive dopamine loss in the brain)
Dementia due to Parkinson's Disease (R3)
Significant cognitive decline after >1yr of motor sx due to Parkinson’s Disease
Often overlap with Lewy Body Dementia (cognitive decline and motor sx begin and progress together)
Dementia due to Prion Disease (R3)
Very rapidly progressive fatal dementias due to prions
Disease is spontaneous, genetic or acquired
Sx: Behavioural/psychiatric changes, memory impairment, visual disturbances, myoclonus, ataxia, language/hearing issues, movement dysfunction
RF: genetics, prion-contaminated surgical instruments, blood products/transfusions, UK Beef 1980-1996
Ix: pathology = definitive, MRI B
No cure - only palliative management (mortality = 1yr)
Dementia due to Huntington's Disease (R3)
Autosomal dominant slow-progressing neurodegenerative disorder often presenting mid-life
Sx: chorea, incoordination, cognitive decline, personality changes, psychiatric sx (resulting in immobility, mutism, and inanition)
Prognosis: 20yrs from dx
RF: genetics/FHx (pre-test genetic counselling/testing is recommended)
Dementia due to HIV (R3)
HIV-Associated Neurocognitive Disorder (HAND)
Rare neurodegenerative disorder resulting from HIV infection (virus attacks brain cells causing inflammation and damage)
Does not directly infect neurons but indirectly causes cognitive damage → subcortical dementia
More common in the later stages of HIV infection (7% of pts), but rare due to antiviral treatments (ART)
Severity levels:
Asymptomatic Neurocognitive Impairment (ANI)
Mild Neurocognitive Disorder (MND)
HIV‑Associated Dementia (HAD) = severe form
Signs and Sx:
Cognitive Features
Bradyphrenia (slowed thinking), Impaired attention/concentration, Executive dysfunction (planning/decisions), Memory retrieval problems (rather than storage)
Motor Features
Gait instability, Poor coordination, Slowed movements, Tremor
Behavioral / Psychiatric Features
Apathy, Depression, Irritability, Social withdrawal
Unlike Alzheimer’s disease, language and visuospatial skills are preserved
Neurocognitive Disorder Mx (Dementia)
Supportive: Exercise/Physical Activity, Memory Aids, CBT
End of life care
Pharmacological:
Acetylcholinesterase Inhibitors: (Donepezil, Galantamine Rivastigmine)
Transdermal patch > oral
Improve/stabilise cognition, alertness and function (Good for Mild to Severe)
AEs: GIT sx, Brady, Neuro/Insomnia/Vivid dreams
NMDA Receptor Antagonists: (Memantine)
SHORT-TERM improve/stabilisation in cognition/function
Good for Moderate to Severe
Supportive Pharm:
SSRIs: comorbid depression, agitation/aggression
Trazodone/Melatonin: insomnia
Vascular Prevention: Antiplatelets (Aspirin), Anticoagulants (Apixiban, Rivaroxaban)
Lewy Body Motor Sx = Levodopa/Carbidopa
Antipsychotics for acute mx of behavioural disturbance in dementia should be avoided increased risk of AEs/mortality
Delirium (R1)
Disturbance in attention and awareness developing over a short period of time, is a change from baseline and fluctuates throughout the day (
Acute deterioration of mental state characterised by fluctuating sx of impaired attention, cognition and consciousness, typically developing over hours to days
Three Main Types:
Hyperactive (agitation, restless, delusions, hallucinations)
Hypoactive (quiet, withdrawn) - most common
Mixed (alternates b/w hyper and hypo)
Ix: identify cause (bloods, BGL, ECG, temp, urine)
Mx: reverse causes, low stimuli environment
Avoid physical/chemical restraints (meds can worsen delirium)
IV Thiamine 3-5d if alcohol withdrawal
Antipsychotics if severe distress/hyperactive
Haloperidol, Olanzapine, Risperidol = Non Parkinson’s/Lewy Body Dementia
Quetiapine = Parkinson’s/LB Dementia
Demoralisation (R1)
Clinical/dysphoric state of existential distress characterized by:
Helplessness
± Hopelessness
± Subjective incompetence/Loss of meaning or purpose
Often arising from chronic illness, severe stress, or perceived failure to cope
Unlike depression, focus is on subjective incompetence rather than anhedonia (pervasive loss of interest)
Mx: psychotherapy, supportive care
Suicidality/Suicide Attempt (R1)
Two Types:
Impulsive: short time between idea and action
Planned: long time between idea and action (stages include idea, plan/research, prep etc)
RF: static (fixed, historic), dynamic (fluctuates in duration and intensity)
Mx: safety planning, psycotherapy, verbal de-escalation, consider involuntary tx, limit access to toxic drugs (overdose)
Somatic Symptom Disorder (R2)
Neuropsychiatric condition causing somatic sx associated with significant distress or impairment
Distressing physical sx (pain, fatigue, GI symptoms, etc.) that disrupt daily life, with/out medical explanation
Excessive and persistent psychological responses
Sx for >6m
Underlying cause not understood, psychological stressors may be a RF
Mx: CBT, Physiotherapy
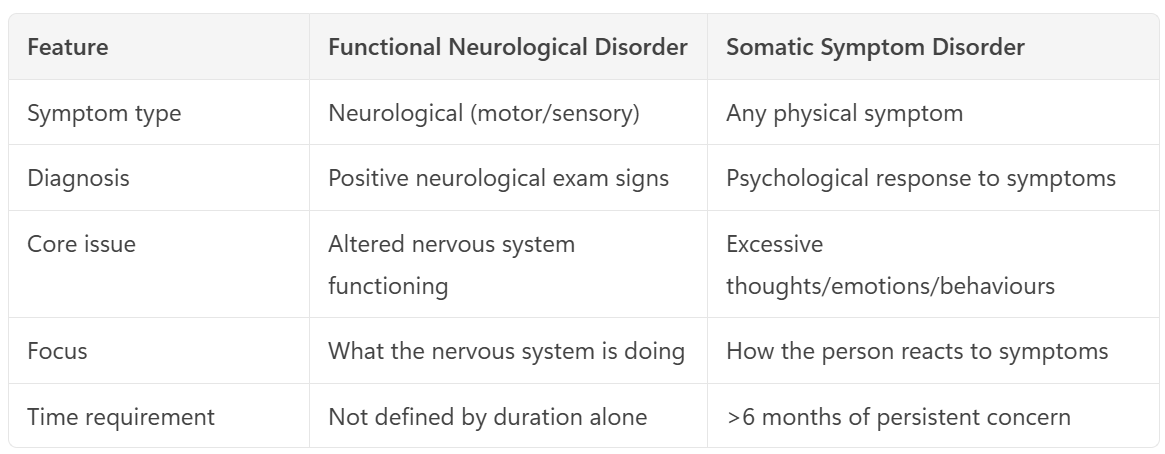
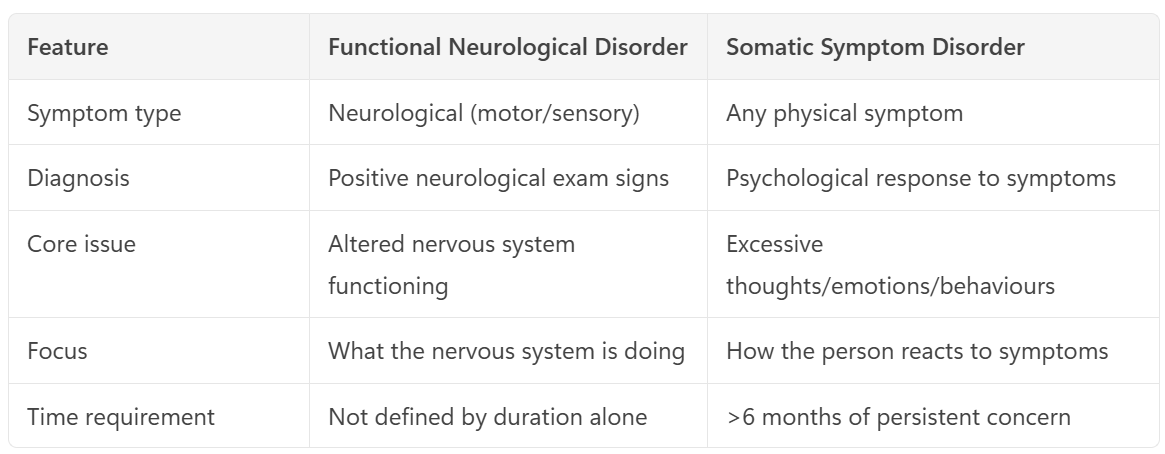
Functional Neurological/Conversion Disorder (R2)
Neuropsychiatric condition causing somatic sx associated with significant distress or impairment
Specific neurological (motor/sensory) signs and functional impairment
Problems with movement or sensation (e.g. weakness, tremor, numbness, non‑epileptic seizures, speech/gait problems) that look like neurological disease (inconsistent findings)
Underlying cause not understood, psychological stressors may be a RF
Dx: ‘rule in’ features on neuro exam
Sx improve with distraction
Inconsistency on exam
Patterns not matching known neuroanatomy
Mx: CBT, Physiotherapy, SSRIs etc (comorbid anx/dep)
Illness Anxiety Disorder (R2)
Disorder of health-related fear
Persistent fear/belief of having/developing a serious illness
Excessive fear of illness with minimal to no physical/somatic sx
Preoccupation with illness lasts ≥ 6m
Behaviours include: Repeated reassurance-seeking, Excessive internet searching, Frequent doctor visits or avoidance of medical care
Mx: CBT, Anxiety Mx (SSRIs etc)
Psychological Factors Affecting Medical Conditions (R2)
A) Medical condition/symptom is present
B) Psychological/behavioural factors adversely affect the medical condition in one of:
Influence the course of medical illness (e.g. cause exacerbation or trigger)
Interfere with tx (e.g. poor adherence)
Factors constitute additional well established health risks for the individual
Influence the underlying pathophysiology, precipitating or exacerbating sx
C) Not better explained by another mental disorder
Factitious Disorder (R3)
Patient consciously pretends to have physical sx without a clear secondary gain
A) Falscification of physical or psychological signs/sx or induction of injury or disease, associated with identified deception
B) The individual presents themself as unwell, injured or impaired
C) The deceptive behaviour is evident even in the absence of obvious external rewards
D) The behaviour is not better explained by another mental disorder e.g. delusional disorder
Can be Factitious disorder imposed on another (by proxy)
Malingering (R3)
Patient consciously pretends to have physical sx with a clear secondary gain
A) Falscification of physical or psychological signs/sx or induction of injury or disease, associated with identified deception
B) The individual presents themself as unwell, injured or impaired
C) The deceptive behaviour is evident even in the presence of obvious external rewards
D) The behaviour is not better explained by another mental disorder e.g. delusional disorder
Can be Factitious disorder imposed on another (by proxy)
Medication‑Induced Symptoms (R1)
Corticosteroids:
Psychiatric AEs = euphoria, hypomania, depression, disturbances of mood, cognition, sleep and behaviour
Delirium/psychosis are less common
Yasmin (OCP), Beta Blockers:
Increased risk of depression
Ketamine
Dissociation associated with confusion, fear or euphoria
Levodopa (Dopamine Agonist):
AEs = depression, psychotic sx, impulse control disorders (e.g. gambling, hyper-sexuality, overspending, binge eating, inappropriate internet use)
Isotretinoin (Roaccutane - Acne):
Dry skin & mucus membranes, depression
Levetiracetam (Keppra - Anticonvulsant):
Behavioural changes (e.g. agitation, irritability, depressed mood, anxiety)
Endocrine‑Induced Symptoms (R1)
Pheochromocytoma:
Classic triad of episodic headaches, tachycardia and sweating
Can cause anxiety symptoms (e.g. panic attacks)
Cushing's Syndrome:
Central obesity, proximal muscle wasting & hypertension
Can cause depression, mania and psychosis
Polycycstic Ovarian Syndrome:
Dx requires >2 of: Oligo/anovulation, Clinical or biochemical evidence of hyperandrogenism & polycystic ovaries
Hyperparathyroidism
‘Bones, stones, abdominal moans and psychic groans’
Sx: renal stones and decreased bone density, fatigue, depressed mood, psychosis, cognitive dysfunction
Hyperthyroidism:
Palpitations, heat intolerance, weight loss & sweating
Anxiety, insomnia, depression, mania, psychosis
Hypothyroidism:
Bradycardia, weight gain, cold intolerance, hair loss, fatigue, depression
Addison’s Disease:
Fatigue, weight loss, salt craving, hyperpigmentation & hypotension
Depression, psychosis, anxiety, mania (less common)