Blood Banking Rotation Week 2 Exam
1/87
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
88 Terms
What testing is done on a cord blood specimen
ABO (Forwad type)
Rh
DAT(Direct Antiglobulin Test)
Why is it so important to wash a cord blood sample prior to testing?
Cord bloods contain Whartons jelly, which can cause a false positive in testing.
Cord bloods must be washed how many times?
4-6times
Babies don't develop their own antibodies until
4-6 months of age.
In addition to wartons jelly, a cord blood must be washed prior to testing due to the ________. Just like with with "Adult" DATs, washing removes __________________________
DAT test
any unbound antibody
When performing the direct anti-globulin test, we are only concerned with identifying the _____________________
the antibody that is bound to the cells
Why don't we test the reverse type on a cord specimen
The reverse type would be testing mothers plasma
Babies don't develop their own antibodies until 4-6 months of age.
What is a DAT?
Direct Anti-globulin Test
The DAT tests the paitents red cells to determine if they are coated with antibodies
indirect anti-globulin test (IAT)
IAT tests the patient plasma against known antigens to determine if patient has allo-antibody. The IAT also has an incubation period to allow the antibody (if present) to bind to the cells.
What can cause a positive DAT on a cord blood specimen
ABO incompatibility with mom OR mother has an antibody to another antigen (Example: K, Duffy, Kidd) that the baby possesses
DAT is seen in cord blood when
Maternal antibody coating baby's cells
DAT is seen in adult specimens when
Paitent recently transfused
Medications
Autoimmune Hemolytic Anemias
Unknown reasons
A positive DAT can occur in cord bloods and adult specimens for different reasons
1. Cord bloods- maternal antibody coating baby's cells
2. Adult specimens- patient recently transfused, medications, autoimmune hemolytic anemia's and unknown reasons
What is the most common ABO incompatibility that occurs with moms and babies
O mother and A babies
Mom has anti-A,B that can cross placenta
When testing for the D antigen, why is the tube with a negative reaction spun a second time?
When a patient has a negative test with Anti-D reagent at immediate Spin, a second drop should be added to the tube and the tube re-spun. This ensures that the test was truly negative and not falsely negative due to the lack of reagent added.
FYI: This is Mercy specific and may not be true at other institutions where you work
When testing for the D antigen, why is the tube with a negative reaction spun a second time?
When a patient has a negative test with Anti-D reagent at Immediate Spin, a second drop should be added to the tube and the tube respun. This ensures that the test was truly negative and not falsely negative due to the lack of reagent added. (FYI: This is Mercy specific and may not be true at other institutions where you work.)
If still negative, why do we perform the weak D test?
The weak D test is an extension of the RH typing that is performed daily in Blood bank to determine if a patient if a patient is Rh positive or negative. The D antigen can have weakened expression so in certain patient, the test is extended and is called the weak D test.
Tests that include the weak D test is carried through to _______ testing is done with a control tube and steps include _________, __________, _________, ________ and ____________
AHG
Immediate spin
Incubate
Wash
add AHG
Check cells of needed and interperation
When we are dealing with weak D test during the incubation period how many minutes are we going to incubate our specimen?
15-60
Do we add Liss on anti D? Why or why not?
We do not add Liss because anti-D has a Liss in it
Describe how to perform the weak D test
The weak D test is performed at all three phases IS, Incubation at 37 (15-60min) and AHG
We do not add liss since the anti-D reagent contains albumin
After incubation, the test does not need to be spun and read
Test should be read after adding AHG and reactions recorded
Check cells must be added to negative tubes
Describe when to perform the weak D test
The Weak D test should be performed when the patient:
· Has an anti-D identified in the antibody panel (the Weak D is the antigen screen).
· Cord Blood (first time we are testing them for D antigen)
· Is a female in childbearing years (<50 J).
Express the answers for the given table
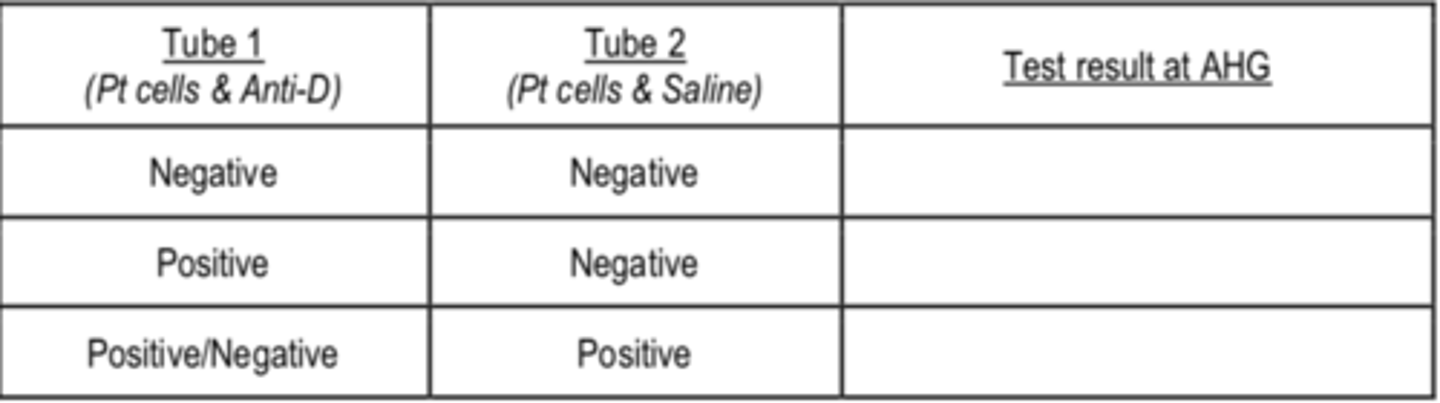
The answers for the previous question is
Weak D negative
Weak D positive
Test is Invalid
When we have an invalid result for a weak D test that means
Chloroquine treat the patient cells to disassociate the antibodies from the red blood cell antigens without destroying the antigens. Wash cells and repeat the Weak D test.
When is the next step when an invalid result is obtained in testing
Chloroquine treat the patient cells to disassociate the antibodies from the red blood cell antigens without destroying the antigens. Wash cells and repeat the Weak D test.
What does the Rh negative sticker on a cord blood specimen mean?
It means that the mothers blood is negative
During your testing if you determine the baby is Rh positive and the cord specimen was labeled with an Rh negative sticker what would you do?
In the computer, on the Mom's financial number, order a Postpartum workup. This will generate an order on the mom to be drawn for the Fetal Bleed Screen.
Note: (Order it in EN, uncollected status, and take label to phlebotomy to draw)
During your testing if you determine the baby is Rh positive and the cord specimen was labeled with an Rh negative sticker what would you do?
In the computer, on moms financial number, order .a postpartum workup. This will generate an order on the mom to be drawn for the fetal bleed screen
Order it in EN, uncollected status, and take label to phlebotomy to draw
During your testing if you determine the baby is Rh Positive and the cord blood specimen was labeled with an Rh negative sticker, what is your next step?
In the computer, on the Mom’s financial number, order a Postpartum workup. This will generate an order on the mom to be drawn for the Fetal Bleed Screen.
Note: (Order it in EN, uncollected status, and take label to phlebotomy to draw)
Is mom eligible for Rhogam?
Mother is eligible for atleast one vial of Rhogam
Mom needs to have a Fetal Bleed Screen done to determine if she needs
More than one vial of Rhogam
When is Rhogam is given?
Rhogam is given routinely to all Rh negative women at 28 weeks into the pregnancy. (It is also given when bleeding or a miscarriage has occurred.)
Rh negative women are alsoeligible for Rhogam after delivery of an Rh positive baby.
How does it work?
Rhogam is manufactured Anti-D. The intention is that the Rhogam Anti-D will bind to all of the baby's D positive cells in the maternal circulation. By removing the Rh positive cells, Rhogam suppresses the immune response of Rh negative individuals to Rh positive RBC's.
What is the Fetal Bleed Screen?
Fetal Bleed Screen is a qualtitative screening test of mom's blood to see if there are any Rh positive (babys) RBC's in mom system. The test differentiates based on Rh positive (baby) vs Rh negative (mom) cells
What is the Fetal Bleed Screen (FBS)?
Fetal Bleed Screen (FBS) is a qualitative screening test of mom’s blood to see if there are any Rh positive (baby’s) RBC’s in mom’s system. The test differentiates based on Rh positive (baby) vs. Rh negative (Mom) cells.
Why do we perform this test?
We perform the FBS to see if there was a bleed before or during the delivery
If FBS is negative, the Rh negative female is eligable for ________________
Only one vial of Rhogam
If FBS is positive, the ___________ or _________ should be performed
Fetal Cell Stain or Kleihauer-betke
What is the modified Kleihauer-betke (ir fetal cell stain)?
Kleihauer-Betke is a quantitative test using acid elution and a staining procedure which identifies fetal RBC’s (containing hemoglobin HgbF) in maternal adult (containing Hgb A) blood.
What is the modified Kleihauer-Betke (or Fetal Cell Stain)?
Kleihauer-Betke is a quantitative test using acid elution and a staining procedure which identifies fetal RBC’s (containing hemoglobin HgbF) in maternal adult (containing Hgb A) blood.
Why do we perform this test?
To quantitate the fetal bleed and determine the aount of rhogam to give
What is the modified Kleihauer-Betke (or Fetal Cell Stain)?
Kleihauer-Betke is a quantitative test using acid elution and a staining procedure which identifies fetal RBC’s (containing hemoglobin HgbF) in maternal adult (containing Hgb A) blood.
Why do we perform this test?
To quantitate the fetal bleed and determine the amount of Rhogam to give.
What is the calculation that is done to determine the number of vials of Rhogam that the patient will need?
· Step 1. # of fetal cells X 100 = %
# of maternal cells
· Step 2. % X 50 = mls of fetal bleed
· Step 3. mls of fetal bleed = vials of RhoGAM needed*
30 *Round number up if >0.5,round down if <0.5.
· Step 4 Always add one to the number you get because this calculation is an estimate!!
Why is an Rh negative mother with an immune anti-D not eligible for Rhogam?
Mom has already made an Anti-D, which is what Rhogam is used to prevent.
Given the following situations, determine if the mother is eligible for Rh Immune Globulin
Answer below
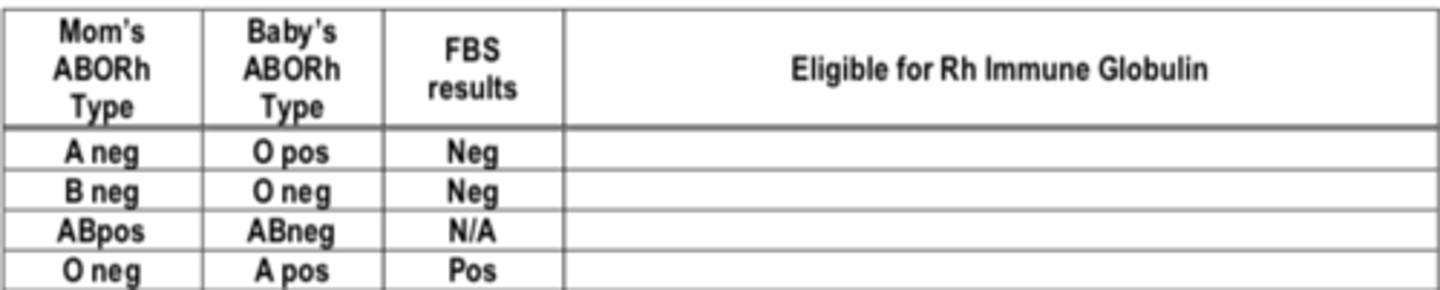
Answer

Interperate the following results for cord blood testing
Answer below
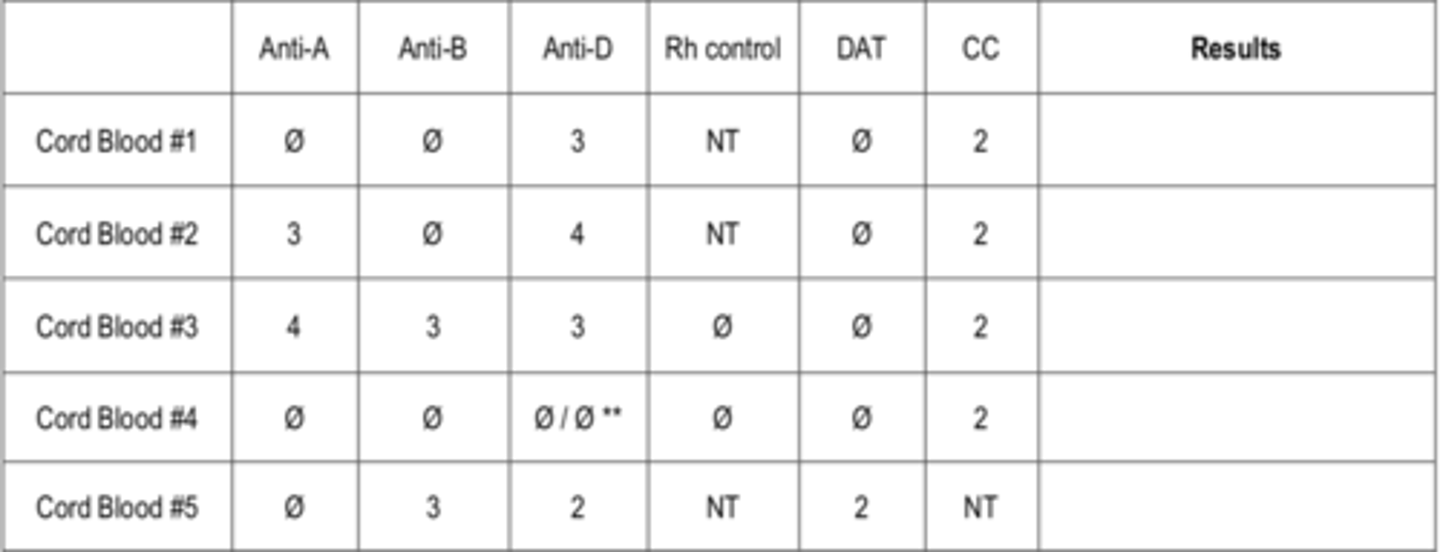
Interperate the following results for cord blood testing
Answer below
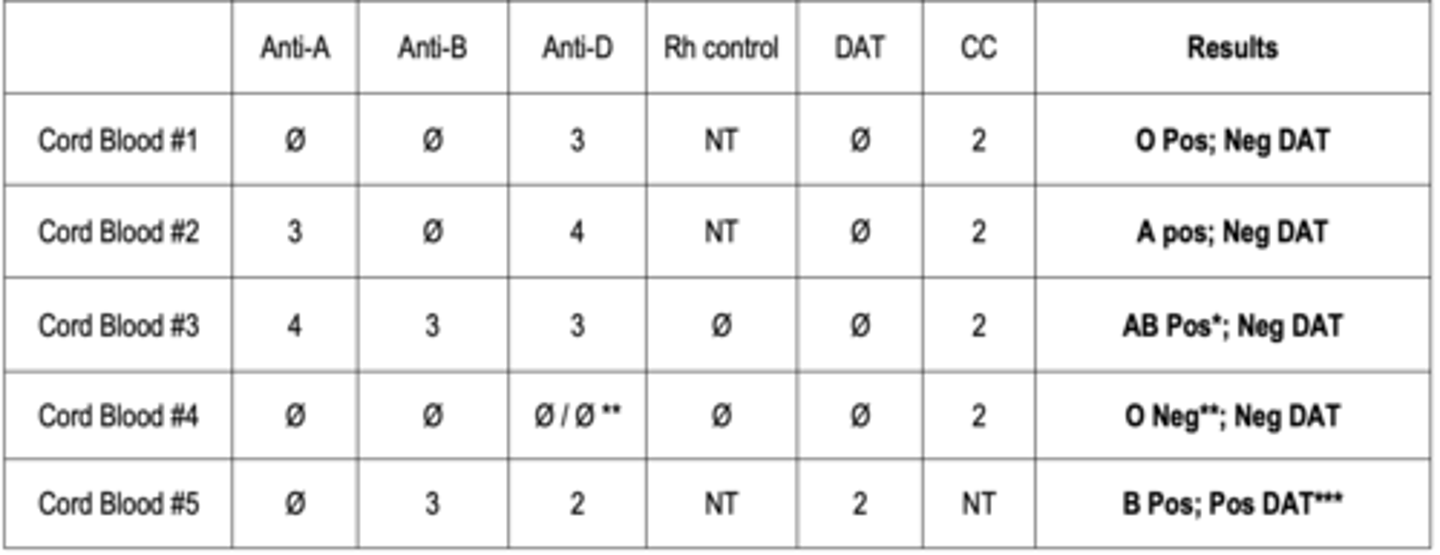
Rh control must be performed whenever you have a positive with all cells tested as happens with __________ patiient
AB Pos
What does the Rh Control process that
The reagent are causing the agglutination and not the patients cells
When the immediate spin Anti-D tube is negative what do we do?
Do another drop Anti-D and respun and read the second time
This is ensures anti-D was truley added to prevent a false negative due to lack of reagent
When the immediate spin Anti-D tube is negative, another drop of Anti-D should be added and tube respun and read a second time (this ensures anti-D was truly added to prevent a false-negative due to lack of reagent
Weak D test will need to be performed on this Cord Blood.
When you have a positive DAT on a cord blood, the mother's ABORh and ABSC needs to be tested. This will determine
· If mom and baby are ABO compatible
· If mother has an alloantibody that is possibly coating the baby's cells
Natural Antibodies
are antibodies occur prior stimulation
Eg: Anti-A and Anti-B
Passive Antibodies
are antibodies that are acquired through immunization or passed from mother to baby
Eg: Vaccination
Alloantibody
developed in response to pregancy or transfusion; to form the alloantibody the paitent must lack the antigen (test negative for the antigen)
Eg: Anti-K, Anti-Fya
What specific disease does the colld agglutination test for?
Primary Atypical Pneumonia
Why does the specimen need to be kept warm from the time it is collected from the paitent until the testing is performed?
Because if it allowed to reach room temperature, the antibodies will bind to the red blood cells resulting in a false negative when the cold agglutinin titer is performed.
If the cold agglutinin is positive, the antibody usually shows a specificity to:
The antibodies tend to demonstrate specificity for Anti-I (which will react to most RBC's since 99% of people over the age of 2 have the I antigen.
What is the purpose of the control tube in the cold agglutinin test?
The control tube determines that the patient is reacting to the cold temperature and not the cells used in the testing system. (Typically the patient's own cells are used and then if the control tube is positive, the test is resetup using screening cells.)
Describe the steps in the cold agglutinin titer:
Testing is described in the Cold Agglutinin Procedure.
Laboratory testing is typically performed at ____________
Room temperature
20-24C
In Blood bank, testing is also performed at ________________
Body temperature
Cold agglutinins are antibodies that are typically react at _______
4 degree C
Some of these cold antibodies have a large __________
Thermal amplitude
What tube is for cold agglutination?
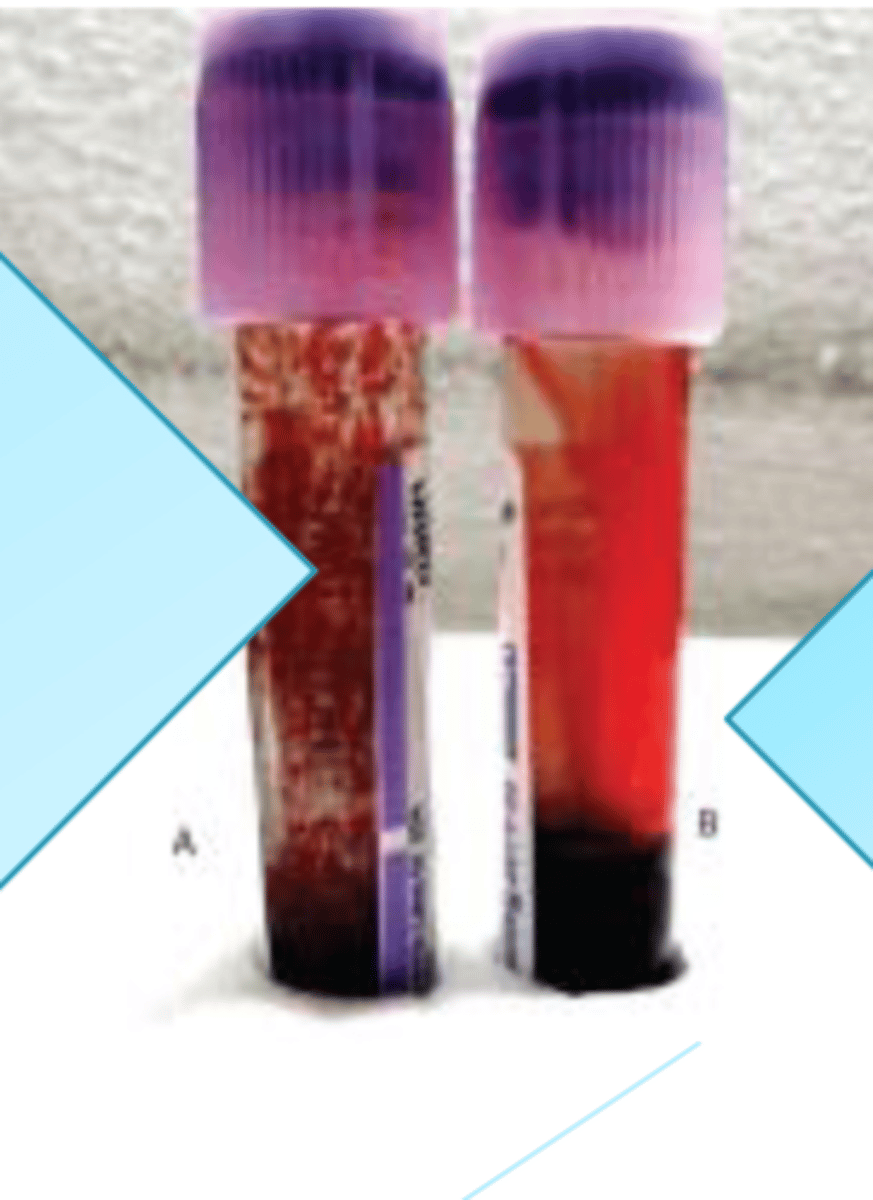
What tube is for cold agglutination?
A
A
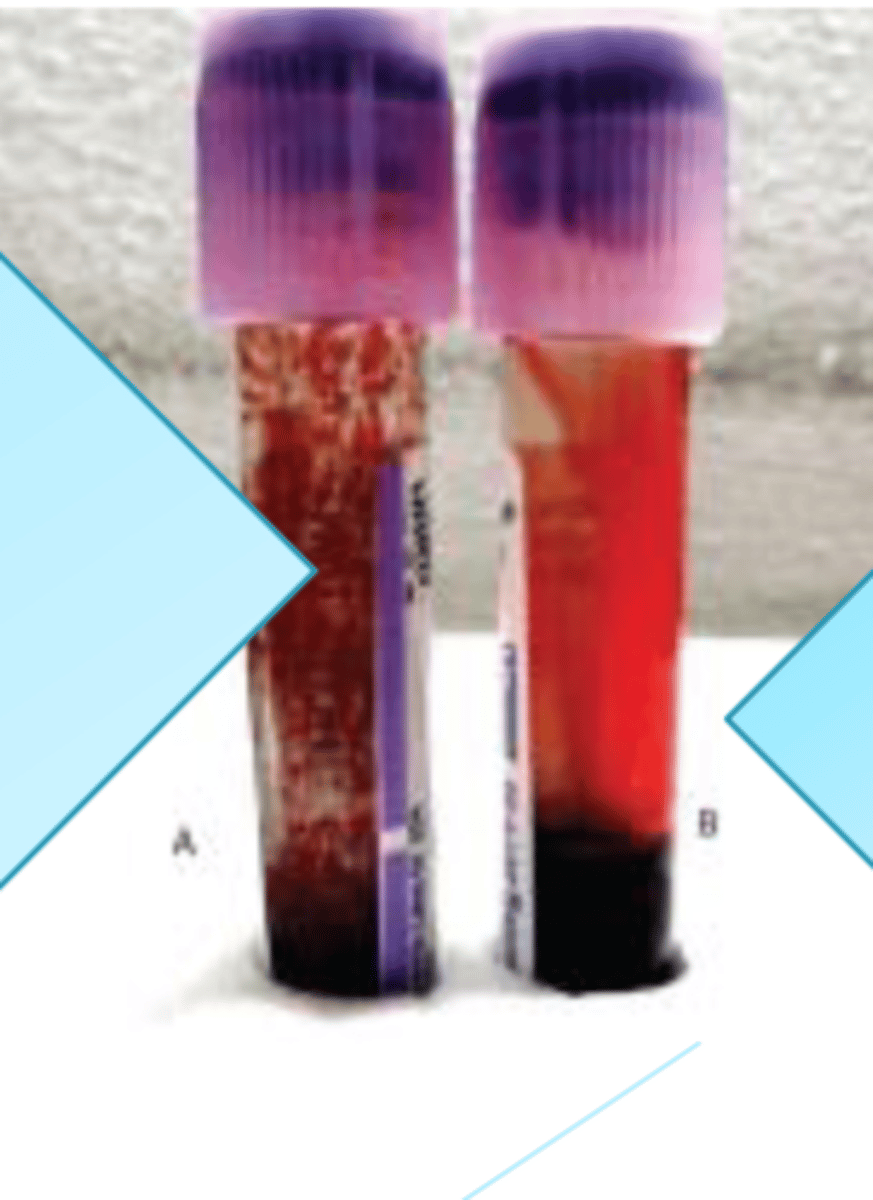
Why is tube A considered to be strong cold agglutination?
it is considered to be strong because it has a large thermal amplitude and it reacts at temperatures from 4c to 30c.
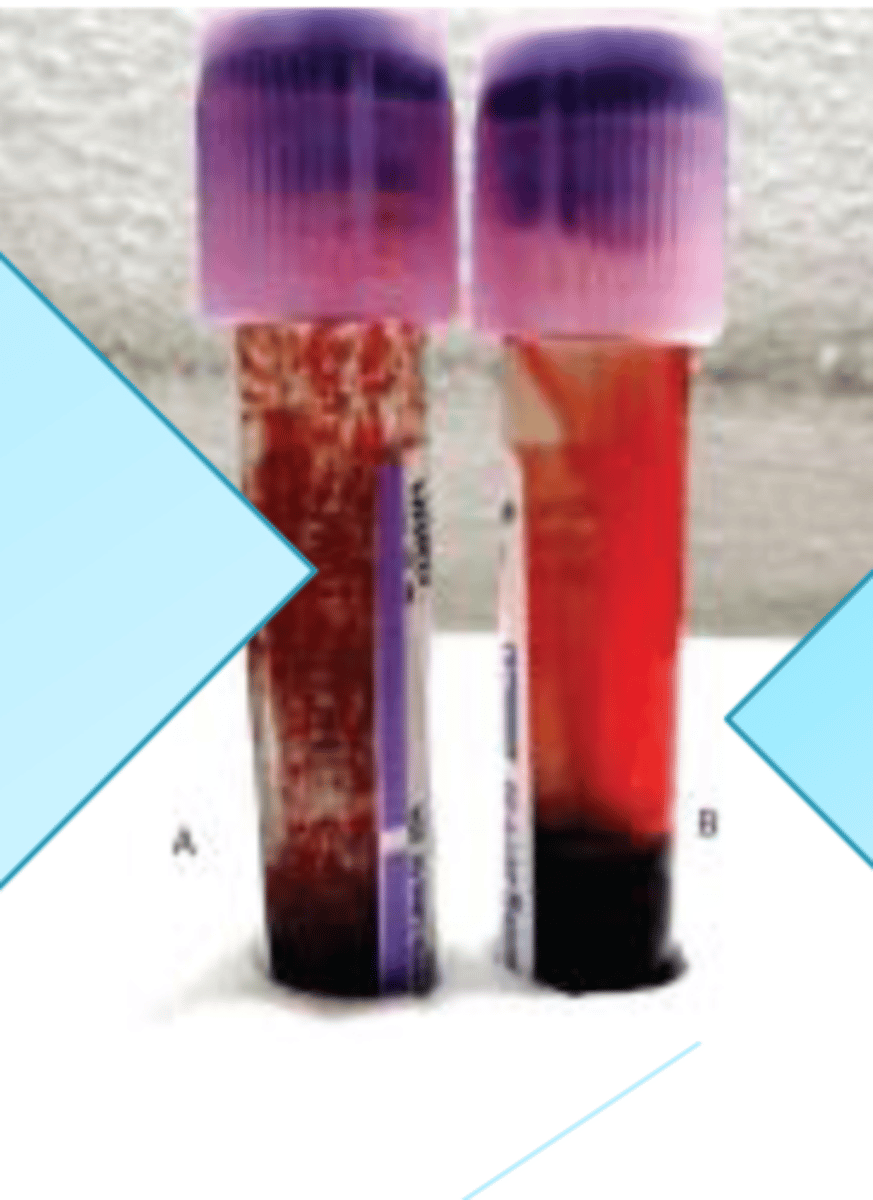
In the picture above, the specimen was intended for ________ but will have to be __________________
CBC
Warmed to 37c prior to running it on Sysmex
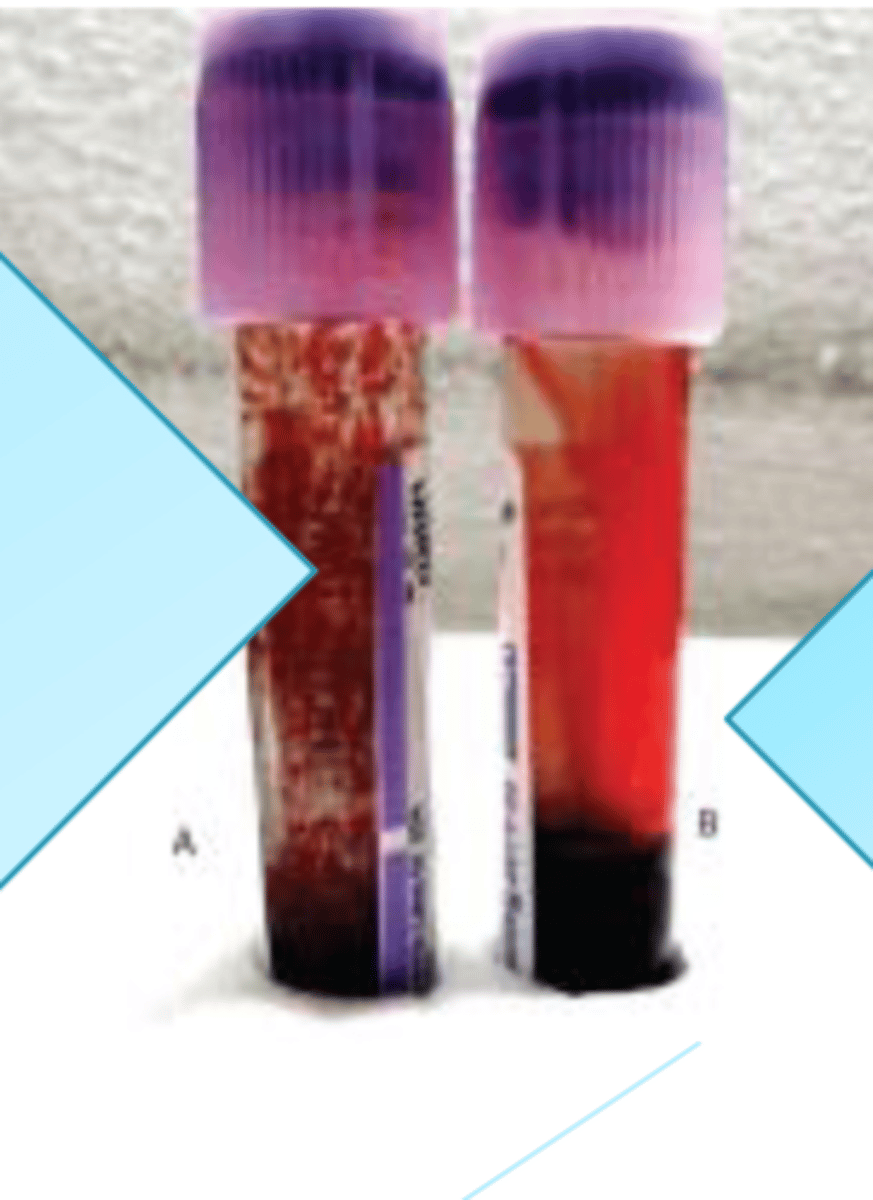
Benign cold autoantibodies
They are autoantibody shows when testing is performed at 4c
Typically it does not cause RBC destruction
can be present normal and healthy individuals
Pathologic Cold autoantibodies
autonomies shows when testing is performed at >30c
Typically does cause destruction
Three examples OF pathologic cold autoantibodies
Chornic, idiopathic
Acute, transient Disorder
Paroxysmal cold Hemogloburnia
All of the cold antibodies are __________________
Autoantibodies
Autoantibodies
Are formed to self antigens
Alloantibodies
Are formed to foreign antigen
So which one is going to be harmful Bengign cold autoantibodies or pathologic cold autoantibodies
Pathologic cold autoantibodies
Autoantibody shows when testing is performed
at 4c
Thermal range of benign cold autoantibodies are
20C-24C
When cold agglutinin interferes with testing, ___________________ is helpful
prewarming the specimen prior to testing
Why does Benign cold autoantibodies typically does not cause RBC destruction?
These autoantibodies are IgM ad can activate complement but destruction is not usually significant to patient
How come benign cold autoantibodies be present normal, healthy individuals
Any patients sample placed at 4c for a period of time would probably demonstrate a cold autoantibody. If tested, the specificity of the autoantibody is Anti-I
This autoantibody is a concern when the patient has symptoms How come benign cold autoantibodies be present normal, healthy individuals
Any patients sample placed at 4c for a period of time would probably demonstrate a cold autoantibody. If tested, the specificity of the autoantibody is Anti-I
This autoantibody is a concern when the patient has symptoms such as
Hematuria (blood in urine) after being outside in the cold
Interestingly, the treatment would be to tell the patient to avoid the cold
Benign cold autoantibodies show a specificity to the ___________
I antigen
I antigen even though this is an autoantibody,
It still can show specifically to a certain antigen
In the I antigen, there are how many antigens?
I, I they are not antithetical
This means you either have Little I and Big I
At birth, all RBCs have the ________
At 18 month they start converting to ____ this completion is going to happen by age of ________
i antigen
I
2 years
Pathologic cold Autoantibody shows when testing is performed at _______
>30c they have broad thermal range
Why do the pathologic cold autoantibody cause destruction?
Paitents can have hemolytic anemia that range from mild to life threatening intravascular hemolysis
What are the three examples of pathologic cold autoantibodies
Chronic idiopathic
Acute Transient disorder
Paroxysmal Cold hemogloburenmia
Chornic idiopathic it is also called
Cold agglutination syndrome or idiopathic cold auto immune hemolytic anemia
It has no identifiable cause
Acute transient Disorder it is also called
Secondary cold auto immune hemolytic Anemia
Acute transient disorder is also associated with an ________________-
Infection from Mycoplasma p=pnuemonia or infectious mononucleosis