Lab Dx Exam 9 (Rheumatology and MSS Labs)
1/126
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
127 Terms
What is uric acid?
Nitrogenous compound and product of purine catabolism
Majority excreted by the kidneys
What are some causes of elevated uric acid?
- Overproduction or decreased excretion by the kidneys (e.g., renal failure)
- Foods high in purine (ex: red meats)
If uric acid is saturated in the urine, what can this cause?
crystals (body increases pH, uric acid is less saturated in alkaline --> prevents crystallization/stone formation)
What is the difference between hyperuricemia and uricosuria?
Hyperuricemia: elevated uric acid in serum (blood)
Uricosuria: elevated uric acid in the urine (has increased risk for kidney stones)
When do we check uric acid levels?
In patients with monoarticular arthritis
If the uric acid level is high and pt is susceptible, uric acid crystals will form in tissue and joints and provoke a severe inflammatory response
What is uric acid clinically associated with?
- gout, but not all gout pts have very high levels
- some pts with very high levels don't develop gout
What causes increased serum levels of uric acid?
- Gout
- Alcoholism
- Aspirin
- Caffeine
- Leukemia
- Metastatic cancer
- Multiple myeloma
- Renal failure
- Diuretic therapy (HCTZ)
- Idiopathic
What causes decreased serum levels of uric acid?
- Lead poisoning (not seen a lot, can be seen in children)
- Wilson disease
- ALS
What is Sjogren syndrome?
Autoimmune disease characterized by progressive destruction of the lacrimal and salivary glands, leading to mucosal and conjunctival dryness
Can occur by itself or in conjunction with other autoimmune disorders such as SLE, RA, scleroderma
What antibodies do we see in patients with Sjogren syndrome?
- Anti-SSA (anti-RO)
- Anti-SSB (anti-LA)
- Anti-SSC
These are all subtypes of antinuclear antibodies (ANAs)
What percentage of patients with Sjogren have either anti-SSA or anti-SSB antibodies?
- Anti-SSA --> ~70% of patients, can also be found in 25% of pts with SLE
- Anti-SSB --> 1/2 of pts with Sjogren, rarely present in pts with SLE
When do we usually see anti-SSC positive?
Positive in 75% of pts with RA or in pts with RA and secondary Sjogrens
What is scleroderma?
Multi-system autoimmune disorder that is characterized by inflammation with fibrosis of the small blood vessels in the skin, heart, lungs, kidneys, and GI tract (aka affects pretty much all organs)
What antibody do we commonly see in scleroderma?
Anti-scleroderma antibody (Scl-70 antibody) --> an antinuclear antibody
Used to dx scleroderma, found in 45% of pts with scleroderma
What is another name for scleroderma?
Progressive systemic sclerosis (PSS)
What is the anti-centromere antibody?
Present in ~57% of patients with limited scleroderma (previously called CREST syndrome)
Rarely found in patients with other connective tissue diseases or in healthy patients
What is CREST syndrome?
Limited cutaneous systemic sclerosis or limited scleroderma
Consists of:
- Calcinosis
- Raynauds
- Esophageal deformity
- Sclerodactyly
- Telangiectasias
What is osteoporosis?
Skeletal disorder characterized by compromised bone strength predisposing to an increased risk for fracture
Associated with thin and weak bones that are prone to fracture
What is a DEXA scan?
Bone densitometry, used to determine bone mineral content (BMC) and density (BMD)
Used to dx osteoporosis and osteopenia as well as monitor effectiveness of therapy
What does a DEXA scan evaluate?
- Lumbar spine (cancellous bone)
- Hip (mixed bone)
- Radius (cortical bone)
How often is a DEXA scan recommended to be repeated for screening and monitoring of osteoporosis?
Every 2 years
When does the USPSTF recommend screening for osteoporosis?
In women over 65 OR postmenopausal women younger than 65 at increased risk of osteoporosis
What is a T-score?
Compares the bone mineral density (BMD) of the pts results to a young healthy adult (30 years old)
Positive T score indicates normal BMD
Negative T score indicates reduced BMD
What are the different values of a T score and what do they correspond to?
Normal: T-score greater than -1
Osteopenia: T-score between -1 and -2.4
Osteoporosis: T-score equal to or less than -2.5
What is a Z-score?
Compares the patient's results to a group of age-matched controls --> looks at where the patient is compared to "normal"
Helps us look for any secondary issues that may be causing the osteoporosis/penia
A score of -2 or lower indicates a secondary cause
What is a fracture risk assessment (FRAX)?
Estimates 10 year fracture risk from femoral neck bone density and clinical risk factors
What are bone turnover markers (BTMs)?
Used to monitor osteoporosis, can identify significant improvement in a few months after starting therapy (within 3-6 months)
Used to determine effectiveness and compliance of tx comparing BTMs with pre-tx levels
What are the different types of BTMs?
- N-telopeptide
- C-telopeptide
- Amnia-terminal propertied of type 1 procollagen
- Osteocalcin
- Pyridium
What are N-telopeptide (NTx) and C-telopeptide (CTx)?
Protein fragments that are seen in the bloodstream and excreted in the urine when the bone breaks down
NTx used to monitor successful therapy
What do elevated levels of N-telopeptide (NTx) indicate?
An increase in bone resorption (breakdown)
Can be seen with: osteoporosis, Paget disease, bone tumors/metastasis, hyperparathyroidism
NTx levels decline with:
Effective use of treatment
A reduction of what percent or more of NTx after 6 months of treatment indicates a satisfactory response to therapy?
50% or more
What is granulomatosis with polyangiitis (Wegener's granulomatosis)?
Rare autoimmune disease associated with systemic vasculitis in which the small and medium arteries of the kidneys, lungs, and upper respiratory tract are damaged by a granulomatous inflammation
Definitive dx is made by biopsy of the affected tissues
What antibody is used to assist in the dx of Wegener's granulomatosis?
Antineutrophil cytoplasmic antibody (ANCAs, c-ANCA and p-ANCA)
What is antineutrophil cytoplasmic antibody?
Used to assist in dx of Wegener's granulomatosis
Tracks the course of the disease, monitors the response to therapy, provides early detection of relapse
What are the 2 major patterns of staining of anti-neutrophil cytoplasmic antibody?
- c-ANCA
- p-ANCA
What is cytoplasmic ANCA (c-ANCA)?
Coarse granular staining of the cytoplasm
Main antigen is proteinase-3 (PR3), seen in ~90% of WG
What is perinuclear ANCA (p-ANCA)?
Staining of the nucleus and perinuclear area, leaving cytoplasm clear
Main antigen is myeloperoxidase (MPO), seen in ~50% of WG but also seen in pts with IBD such as UC (50-70%) and Crohn's (20%)
What is multiple myeloma?
Malignancy that is part of a spectrum of diseases ranging from monoclonal gammopathy to plasma cell leukemia
What are presenting symptoms of multiple myeloma?
- Bone pain
- Pathologic fractures
- Weakness, Malaise
- Hypercalcemia
- Renal failure
- Neuropathies (numbness/tingling)
How do we diagnose multiple myeloma?
- 24-hour urine collection for quantification of the Bence Jones protein (i.e., lambda light chains)
- M-spike at the beta or gamma globulin zone in SPEP
What is serum protein electrophoresis (SPEP)?
Separates the various components of protein into bands or zones according to their electrical charge
Can demonstrate polyclonal or monoclonal spikes
What are polyclonal spikes on SPEP? Monoclonal spikes?
Polyclonal: associated with infectious or inflammatory disease
Monoclonal: often neoplastic
If a patient has a monoclonal spike (M-spike) in the beta or gamma globulin zone on SPEP, what does this indicate?
Associated with multiple myeloma
What is useful for determining the type of renal damage in a patient if present, when suspecting multiple myeloma?
Urine protein electrophoresis
What is Bence Jones protein?
Detected in urine using urine protein electrophoresis
Monoclonal light-chain portions of immunoglobulin found in 75% of patients with MM
What is creatine kinase (CK)?
Found predominantly in the heart muscle, skeletal muscle, and brain
Elevated during a muscle or nerve injury, rises within 6 hours after damage --> if damage is not persistent, will return to normal within 2-3 days
What is CK used to support the diagnosis of?
- Myocardial muscle injury (infarction)
- Neurologic disease
- Skeletal muscle disease
What are the different creatine kinase isoenzymes?
- CK-MB
- CK-BB
- CK-MM
What is CK-MB?
Rises with heart damage
Examples: MI, PE, CHF
What is CK-BB?
Found predominantly in the brain and lung injury
Examples: CVA and PE
What is CK-MM?
Rises with injury to or disease of the skeletal muscle
Examples: rhabdomyolysis, vigorous exercise, electroconvulsive therapy, crush injury, recent surgery
CK-MM varies on patient's muscle mass --> muscular patients may have elevated CK
CK-MM varies on:
Patient's muscle mass --> muscular patients may have elevated CK
What are the isoforms of CK-MM?
MM1 and MM3
Useful for detecting cardiac disease (heart attack)
MM3/MM1 ratio over 1 suggests:
Acute myocardial injury
What could cause increased levels of CK-MM isoenzymes?
- Rhabdomyolysis
- Muscular dystrophy
- Myositis
- Recent surgery
- Multiple IM injections
- Crush injuries
- Delirium tremors
- Recent convulsions
- Electroconvulsive therapy
- Shock
- Hypokalemia
- Hypothyroidism
- Trauma
What is aldolase?
Enzyme used in glycolysis
Used to aid in the dx and surveillance of skeletal muscle or hepatic disease
Very high levels of aldolase are seen in pts with:
- Muscular dystrophy
- Dermatomyositis
- Polymyositis
- Muscular trauma
Elevated levels (not super high) can also be seen in pts with chronic hepatitis and liver cirrhosis
What can cause increased levels of aldolase?
- Hepatocellular disease (ex. hepatitis)
- Muscular disease (ex. muscular dystrophy, dermatomyositis, polymyositis)
- Muscular trauma (ex. severe crush injury)
- Muscular infections (ex. trichinosis)
- Gangrenous processes (ex. gangrene of the bowel)
- MI
What can cause decreased levels of aldolase?
- Hereditary fructose intolerance
- Muscle-wasting disease (ex. ALS)
What are complement assays?
Screening test that is used to dx hereditary and acquired deficiencies
Looks at the complement system of inflammation to determine if there are any abnormalities
What is the complement system?
Part of the innate immune system
Plays a critical role in the defense against infections, promotes inflammatory response, eliminates pathogens, and enhances the immune response
What can complement assays monitor the activity of?
Infectious or autoimmune disease
EX. Hereditary angioedema, SLE, infectious endocarditis, vasculitis, glomerulonephritis
What are the different serum complements?
- group of 31 proteins that act as enzymes, cofactors, inhibitors
- labeled C1-C9 (diff dz are associated w/different complement deficiencies)
What is arthrocentesis?
Aspiration of fluid from a joint
Can also be used to deliver medications into a joint space (intra-articular injection)
What is arthrocentesis used for?
To rule out:
- Infection
- Arthritis
- Crystal-induced arthritis (gout vs. pseudogout)
- Synovitis
- Neoplasms of the joint
What is the technique for an arthrocentesis?
Insert sterile needle into joint space to obtain synovial fluid
What are the major joints within which we can do an arthrocentesis?
- Knee
- Shoulder
- Hip
- Elbow
- Wrist
- Ankle
Why is a hip arthrocentesis not usually done in the office?
Lots of blood vessels in the area, needs to be done with imaging
What should the normal color of synovial fluid be?
Clear, straw colored, no blood
If a patient's synovial fluid has low glucose, what can this indicate?
- Inflammation
- Septic arthritis
- RA
If a patient's synovial fluid has increased uric acid, what can this indicate?
Gout
If a patient's synovial fluid has increased protein and lactate levels, what can this indicate?
Bacterial infection, inflammation
If a patient's synovial fluid has high WBCs with neutrophils, what can this indicate?
Acute bacterial infection
If a patient's synovial fluid has high WBCs with lymphocytosis or monocytosis, what can this indicate?
Gout or RA
If a patient's synovial fluid has decreased complement (protein) levels, what can this indicate?
- SLE
- RA
- Other immunologic arthritis
If a patient's synovial fluid has cloudy color, what can this indicate?
Infection
If a patient's synovial fluid has low viscosity, what can this indicate?
Inflammation
What is a gram stain?
- Test to determine if a bacteria is gram + or gram -
- Can describe shape (rods, cocci, diplococci in clusters, etc.)
- Must be ordered in addition to arthrocentesis
If a patient's arthrocentesis gram stain comes back + for calcium crystals, what does this indicate?
Pseudogout
If a patient's arthrocentesis gram stain comes back + for cholesterol crystals, what does this indicate?
RA
If a gram stain is purple small spheres, what kind of bacteria is it?
Staphylococci (gram +)
If a gram stain shows needle shaped crystals, what does this indicate?
- Uric acid crystals
- Negative bifringement, GOUT
- Yellow when parallel to compensator ray

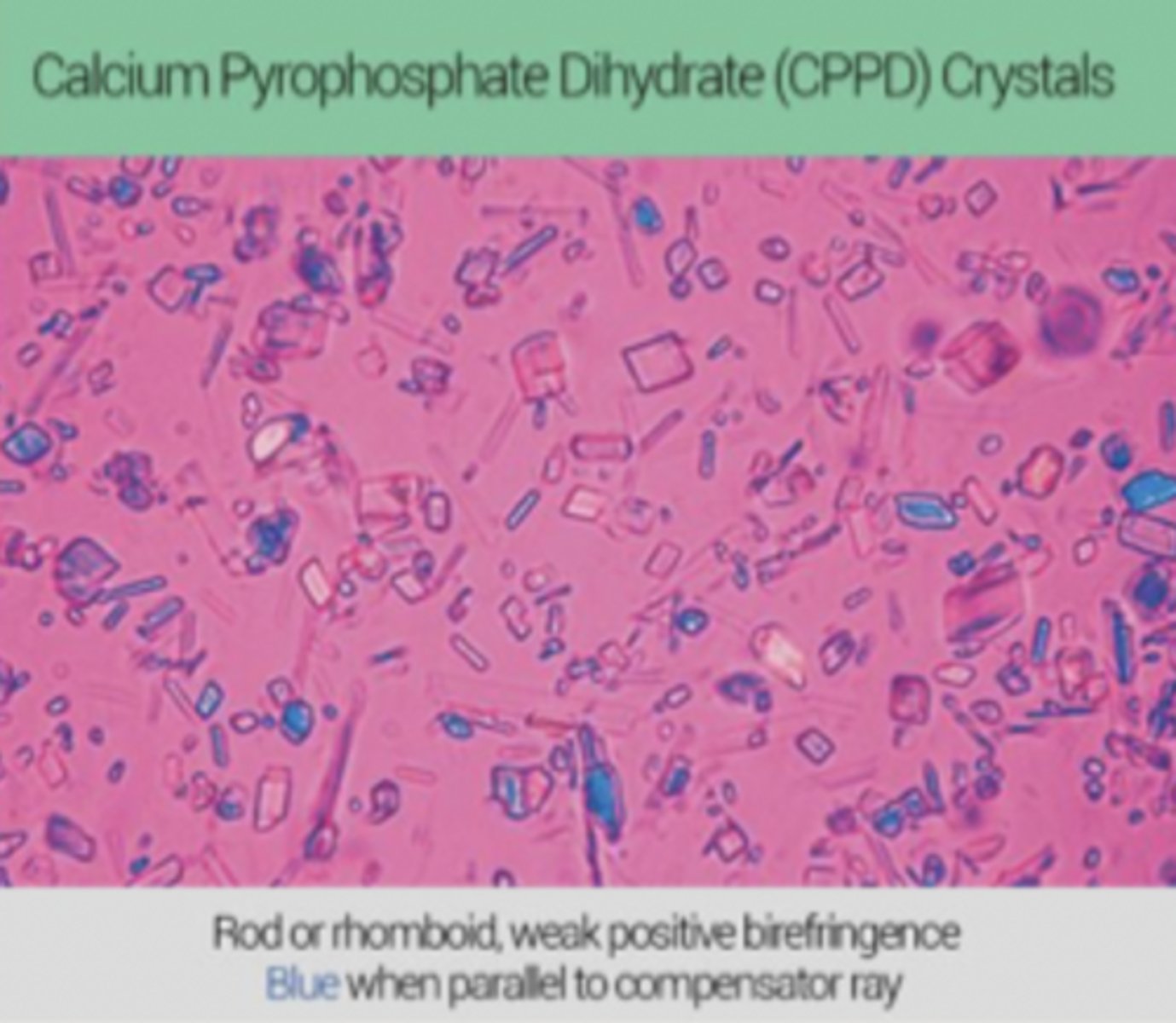
If a gram stain shows rhomboid shaped crystals, what does this indicate?
- Calcium crystals
- Positive bifringement, PSEUDOGOUT
- Blue when parallel to compensator ray
What are antinuclear antibodies (ANAs)?
Group of antinuclear antibodies used to diagnose SLE and other autoimmune diseases
Some of them are specific for SLE, some are associated with other rheumatological diagnoses (SLE, scleroderma, Sjogren's, CREST)
How many SLE patients have positive ANAs?
~95%
Since almost all patients with SLE develop ANAs, a negative ANA excludes the diagnosis
When should we check ANA levels?
In patients with high suspicion of autoimmune disease (ex. young pts complaining of fatigue, joint pain, rash, fever)
ANA titers less than 1:40 are:
Negative (not significant)
ANA titers more than 1:160 are:
Significantly positive
Low-level ANA titers can be seen in:
Elderly or some healthy people
Why do we need to order more tests if a patient's ANA results come back positive?
A lot of rheumatological disorders will have a positive ANA --> in order to determine which the patient has, need additional testing
How are titers expressed?
- in terms of the way in which they are made
- dilution 1 in 8 is made by mixing 1 volume of serum w/7 volumes of diluents (normal saline)
If you see an anti-centromere ANA pattern, what does this indicate?
PSS (CREST)
look at ANA pattersn slide
What is lupus?
- autoimmune dz that can damage any part of your body
- chronic, waxes and wanes
What are anti-DNA antibodies?
Used to diagnose lupus
2 kinds:
- Anti single stranded DNA (anti-ssDNA)
- Anti double stranded DNA (anti-dsDNA)
What is anti single stranded DNA (anti-ssDNA)?
Anti-DNA antibody that can indicate SLE
Less sensitive and specific --> not in clinical use
What is anti double stranded DNA (anti-dsDNA)?
Anti-DNA antibody that is 95% specific and 70% sensitive for SLE --> supports dx of SLE
Occasionally found in other conditions such as RA, drug-induced lupus, autoimmune hepatitis
Higher levels of anti-dsDNA is predictive of:
Renal problem (nephritis) due to immune complex deposition
What is anti-smith (Sm) and anti-ribonucleoprotein antibody (anti-RNP)?
- Anti-Sm found in 10-40% of pts with SLE, but very infrequent with other conditions --> if negative, does not exclude SLE dx
- Anti-RNP found in 40-60% of pts with SLE, but not specific for SLE
Both titers do not correlate significantly with any clinical activity of the disease --> not usually ordered
What is rheumatoid arthritis (RA)?
- autoimmune dz that attacks tissues near joints and other body party
- sx: chronic swelling and pain
- usually affects joints symmetrically --> most frequently in the hand