Bio Unit B Flashcards
1/103
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
104 Terms
Testes
Male gonads, or primary reproductive organs; male sex hormones and sperm are produced in these
Ovary
Female gonad, or reproductive organ; female sex hormones and egg cells are produced here
Fertilization
Fusion of a male and a female sex cell
Zygote
The cell resulting from the union of a male and female sex cell. It contains 23 chromosomes from the sperm cell and 23 from the oocyte.
Embryo
The early stages of an animal’s development
Fetus
The later stages of an unborn offspring’s development
Scrotum
Sac that contains the testes. It is slightly colder than the abdominal cavity, as sperm cannot develop at body temperature.
Vas deferens
Tube that conducts sperm toward the urethra. Connects the testes to the bladder area.
Ejaculatory duct
A tubule formed at the union of the vasa deferentia and the seminal vesicle ducts and opening into the urethra. Semen is propelled into the urethra through here. The two vas deferenses connect here.
Semen (seminal fluid)
A secretion of the male reproductive organs that is composed of sperm and fluids
Vasectomy
Cutting the vas deferens so that sperm cannot go past the ejaculatory duct.
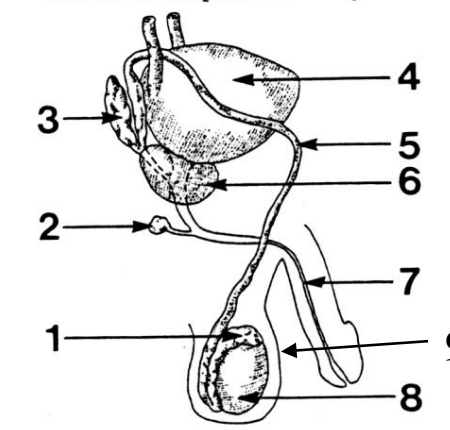
1
Epididymis
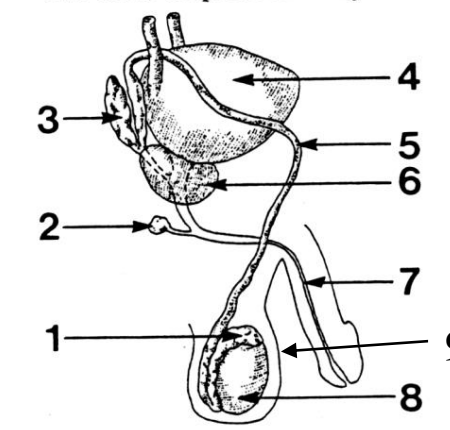
2
Cowper’s (bulbourethral) gland
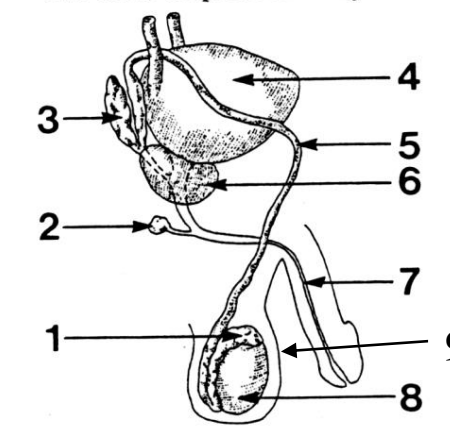
3
Seminal vesicle
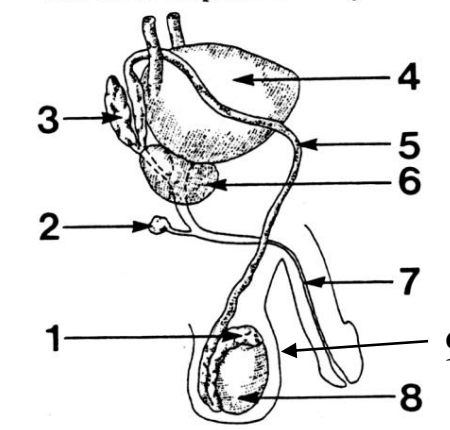
4
Bladder
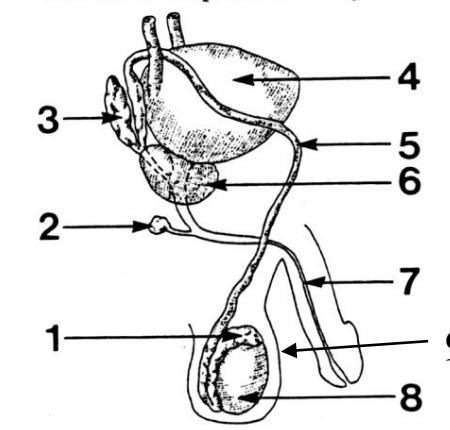
5
Vas deferens
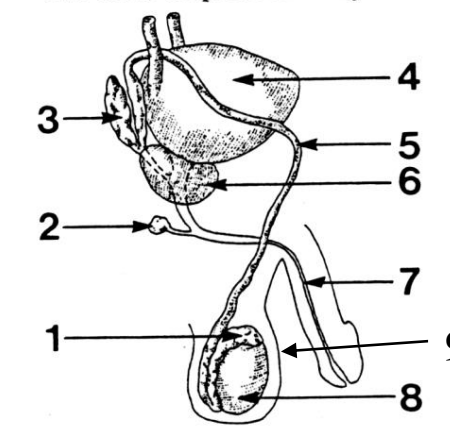
6
Prostate gland
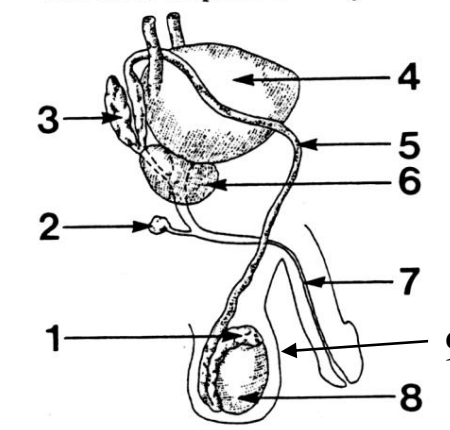
7
Urethra
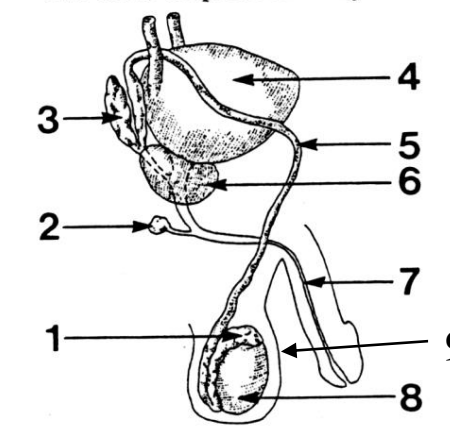
8
Testes
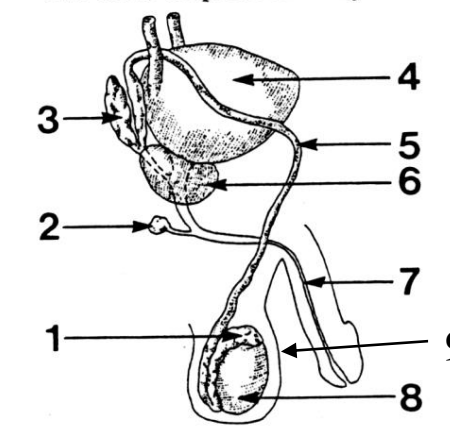
9
Scrotum
Semineferous tubules
Coiled ducts found within testes, where immature sperm cells divide and differentiate. Stimulated by FSH.
Spermatogenesis
Process by which spermatogonia divide and differentiate into mature sperm cells
Spermatogonia
Sperm-producing cells found in the seminiferous tubules (duplicated, diploid)
Spermatocyte
A cell that arises from division of spermatogonia during spermatogenesis (duplicated, haploid)
Spermatid (sperm cell)
An immature sperm cell that arises from division of a spermatocyte (unduplicated, haploid)
Somatic cell
Any cell in a multicellular organism that is not a reproductive cell; diploid
Seratoli cell
A cell that provides metabolic and mechanical support to developing sperm cells. Located in the seminiferous tubules. Acts as a barrier between blood and the testes, protecting sperm from hormones and blood.
Epididymus
Structure located along the posterior border of the testis, consisting of coiled tubules that store sperm cells. Sperm cells mature here and develop their swimming motion.
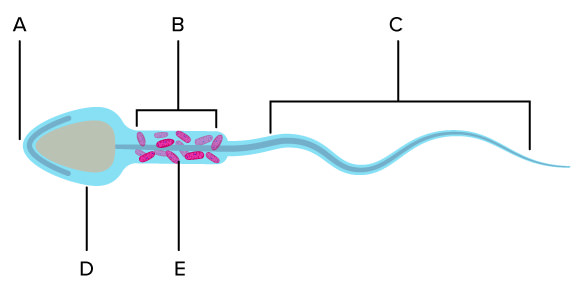
A
Acrosome
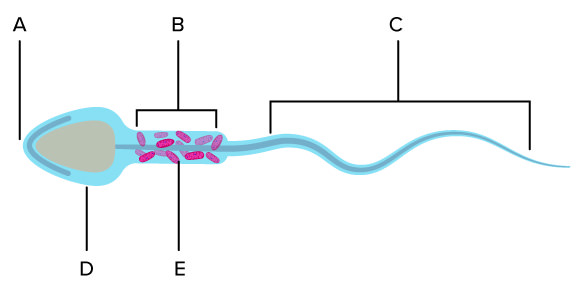
B
Midpiece
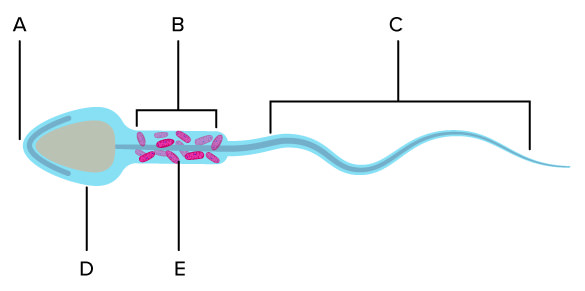
C
Hindpiece/flagellum
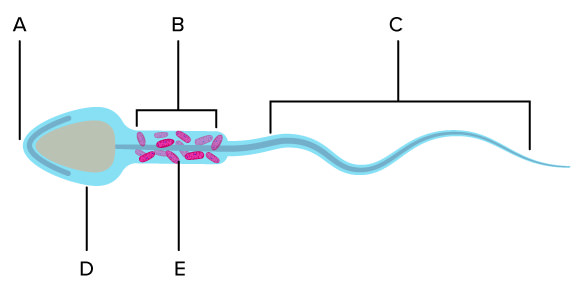
D
Head
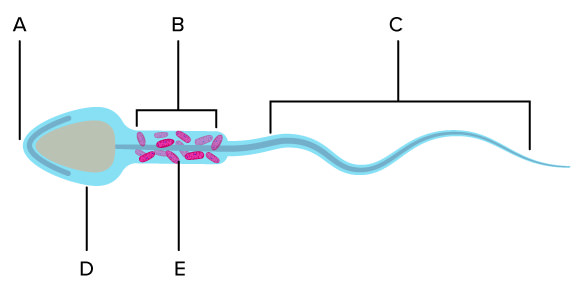
E
Mitochondria
Seminal fluid
Fluid part of semen, which is secreted by three glands
Seminal vesicle
Structure that contributes to the seminal fluid (semen), a secretion that contains fructose and prostaglandins
Prostate gland
Structure that contributes to the seminal fluid (semen), a secretion containing buffers that protect sperm cells from the acidic environment of the vagina
Cowper’s (bulbourethral) gland
Structure that contributes a mucus-rich fluid to the seminal fluid
Primary sexual characteristics
Physical characteristics of an organism that are directly involved in reproduction
Secondary sexual characteristics
External features of an organism that are indicative of its gender (male or female), but are not the reproductive organs themselves. Think, puberty
Testosterone
Male sex hormone produced by the interstitial cells of the testes
Gonadotropic hormones (gonadotropins)
Hormones produced by the pituitary gland that regulate the functions of the testes in males and the ovaries in females. Include FSH and LH.
FSH (males)
In males, a hormone that increases sperm production
LH (males)
In males, hormone that regulates the production of testosterone
GnRH
Chemical messenger from the hypothalamus that stimulates secretions of FSH and LH from the pituitary
Inhibin
A hormone produced by the Sertoli cells that inhibits production of FSH
Ovum
Egg cell
Oocyte
Immature ovum/egg cell
Uterus (womb)
The hollow, pear-shaped organ located between the bladder and the anus in females
Endometrium
The glandular inner lining of the uterus
Fallopian tube (oviduct)
One of the two tubes that connect the ovaries to the uterus
Fibrium
A fingerlike projection at the end of the Fallopian tube
Vagina
The muscular canal extending from the cervix to the outer environment; the birth canal
Cervix
A muscular band that separates the vagina from the uterus
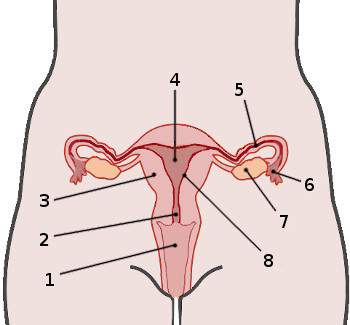
1
Vagina
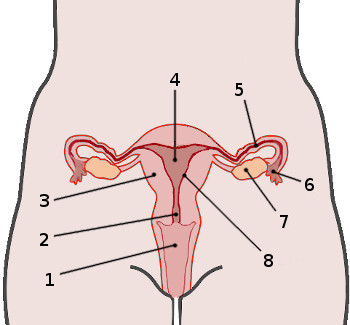
2
Cervix
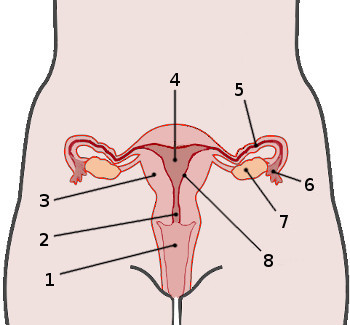
4
Uterus
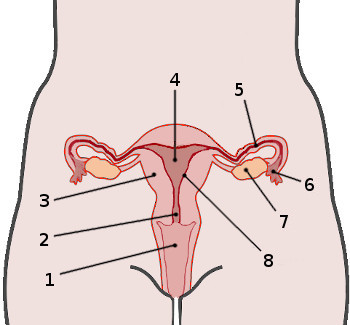
5
Fallopian tube
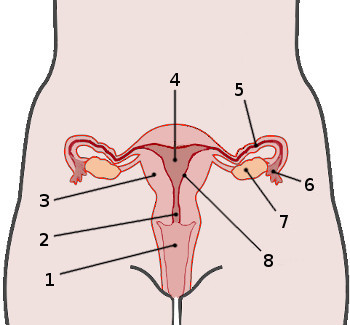
6
Fimbria
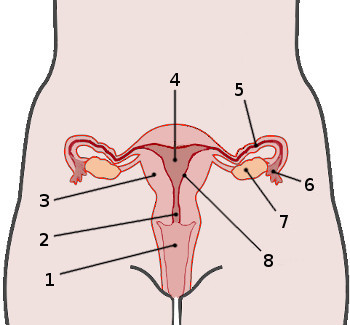
7
Ovary
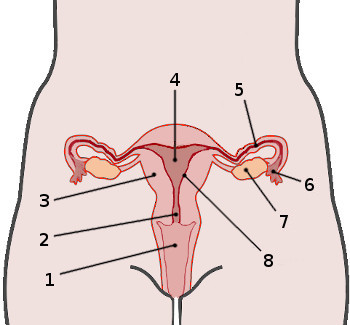
8
Endometrium
Oogenesis
Formation and development of mature ova
Follicle
Structure in the ovary that contains the oocyte
Primary oocyte
The diploid cell that divides to become the egg cell
Granulosa
Layer of small cells that forms the wall of a follicle
Ovulation
Release of the secondary oocyte from the follicle held within the ovary
Corpus luteum
Mass of follicle cells that forms within the ovary after ovulation; secretes estrogen and progesterone.
Secondary oocyte
Formed from the 1st meiotic division of the primary oocyte, and is the cell which retains the majority of the cytoplasm. It travels along the Fallopian tube and will undergo Meiosis 2 once it is fertilized.
Menstruation (flow) phase
The shedding of the endometrium during the menstrual cycle. Involves the release of oxytocin when progesterone levels fall. All hormones are at low levels during this phase, except oxytocin.
Follicular phase
Phase marked by development of ovarian follicles before ovulation. FSH levels increase, and so do estrogen levels. This stimulates follicle development and secondary sexual characteristics.
Estrogen
Hormone that activates development of female secondary sexual characteristics, and increased thickening of the endometrium during the menstrual cycle
Ovulatory phase
Phase in which ovulation occurs. LH spikes here, which causes ovulation and the development of corpus luteum. Progesterone begins to rise, starting the thickening of the endometrium. FSH slightly increases because of the low levels of progesterone.
Luteal Phase
Phase of the menstrual cycle characterized by the formation of the corpus luteum following ovulation. Here, progesterone levels climb dramatically, as the endometrium also begins to develop in anticipation of ovum implantation in the uterus. LH levels plummet now that the corpus luteum and ovulation have occured. Estrogen levels decline after the ovulatory phase, but the corpus luteum secretes estrogen and progesterone to keep them stable.
Progesterone
Hormone produced primarily by the corpus luteum, that induces changes in the endometrium during the menstrual cycle. If a woman becomes pregnant, high progesterone levels keep oxytocin low, preventing a miscarriage.
Menopause
The termination of the female reproductive years
FSH (females)
A gonadotropin that promotes the development of follicles in the ovary
LH (females)
A gonadotropin that promotes ovulation and the formation of the corpus luteum.
Hormone levels after the luteal phase if fertilization occurs:
LH levels will remain low, since the corpus luteum has already formed
Estrogen levels will stay stable since the corpus luteum continues to produce estrogen
Progesterone levels will stay stable since the corpus luteum continues to produce estrogen
FSH levels will remain low since no new follicles need to be produced
``
Hormone levels if an egg remains unfertilized
The corpus luteum withers and dies, and the next menstrual cycle begins.
LH levels return to normal, low levels during the flow phase
Estrogen levels will decline since there is no corpus luteum to produce it
Progesterone levels will decline also because there is no corpus luteum to produce it
FSH levels will increase since the next follicle must begin development
Cleavage
Cell division of zygote, in which the number of cells increases without any change in the size of the zygote
Blastocyst
AN early stage of embryo development
Implantation
The attachment of the embryo to the endometrium
Chorion
The outer extraembryonic structure of a developing embryo that will contribute to the placenta
Amnion
A fluid-filled extraembryonic structure
hCG
An embryonic hormone that maintains the corpus luteum
Amnionic cavity
The fluid-filled cavity surrounding the developing embryo. Protects it from infection dehydration, impact, and changes in temperature.
Extraembryonic coelom
Body cavity between the amnion and the chorion
Yolk sac
A membranous sac that forms during embryo development of most vertebrates; in humans, it does not contain yolk. It is the site of early red blood cell formation and later contributes to the primitive digestive tract.
Placenta
The site for the exchange of nutrients and wastes between mother and fetus
Chorionic villi
Vascular projections of the chorion that secrete hCG
Allantois
Extraembryonic structure that contributes to the blood vessels of the placenta. Precursor of umbilical cord.
Umbillical cord
Structure that connects the fetus to the placenta
First trimester
The period during pregnancy from conception until the end of the third month. It extends from fertilization up until just before the placenta fully develops. It encapsulates fertilization, implantation, specialization/differentiation, gastrulation.
Gastrulation
Process by which a gastrula is formed. A two-layered flattened disk in the blastula forms a three-layered structure called the blastula.
Gastrula
Stage of embryonic development in which the embryo is composed of three layers; ectoderm, mesoderm, and endoderm.
Ectoderm
The outer layer off cells in an embryo. It eventually forms things like the skin, hair, outer eye structures, teeth, and nervous system
Mesoderm
Middle layer of cells in an embryo. it eventually forms things like muscles, blood, bones, and reproductive structures
Endoderm
The inner layer of cells in an embryo, It eventually forms digestive and respiratory organs.
Second trimester
The period during pregnancy from the fourth month to the end of the sixth month. The fetus begins to look like a human and most organs are mostly developed. Other characteristics like hair and eyelashes begin to form. Sex is differentiable here.
Third trimester
The period during pregnancy from the seventh month until birth. Rapid growth occurs here, and any finishing touches are added.
Teratogen
Any medication, chemical, infectious disease, or environmental agent that might interfere with the normal development of a fetus or embryo