ANHB2212 - Cardiovascular System Development
1/147
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
148 Terms
Where does formation of the blood vessels begin?
in extraembryonic mesoderm of the yolk sac (umbilical vesicle), connecting stalk, and chorion
When are the blood vessels formed?
week 3
What are the 2 steps of blood vessel formation?
vasculogenesis
angiogenesis
Vasculogenesis
Mesenchymal cells differentiate into angioblasts that aggregate to form blood islands.
Cavities appear within the blood islands.
Angioblasts flatten to form endothelial cells, forming the primordial endothelium.
The endothelium-lined cavities fuse to form networks of endothelial channels
Angiogenesis
Vessels sprout by endothelial budding into adjacent nonvascularized areas and fuse with other vessels forming communicating channels.
How do blood cells develop?
Develop from hematopoietic stem cells, hemangiogenic endothelium or blood vessels. Blood formation occurs the liver, and later in the spleen, bone marrow, and lymph nodes
When does the cardiac crescent develop?
week 3
Development of the cardiac crescent
During gastrulation: migration of heart forming epiblast cells through the primitive streak produces the first recognizable precardiac mesoderm, a crescent-shaped zone of thickened mesoderm, the cardiac crescent (primary/first heart field)
Second cardiogenic region becomes established behind the first heart field = secondary heart field
Where are the cardiogenic areas originally situated?
in front of the neural plate (developing brain)
What 4 things do the cardiogenic mesoderm (heart fields) form?
ventricular, atrial and outflow tract myocardium
contributes cells to endocardium, conduction system and aortic/pulmonary cushions
What 5 things does the proepicardium form?
epicardium
Interstitial fibroblasts in the myocardium
vascular smooth muscle cells
endothelial cells of coronary vessels
myocytes (mainly in AV system)
What 4 things do cardiac neural crest cells form?
Distal smooth muscle cells of the outflow tract & aorticopulmonary ridge.
Autonomic innervation of the heart.
Cardiac valve development
Septation of the heart
Development of the endocardial tube
Blood-forming cavities (blood islands) develop in splanchnic lateral plate mesoderm in the cranial end of the embryo (cardiac crescent/field), forming a horseshoe-shaped structure around the cranial and lateral portions of the neural plate.
The intra-embryonic coelom overlies this
The blood-forming cavities coalesce to form a horseshoe-shaped endocardial tube, lined by endothelial cells.
This tube becomes surrounded by myoblasts (from the mesenchyme) to form the myocardium.
On the surface of the myocardium the visceral mesoderm of the pericardial cavity forms the epicardium.
When does the heart reposition into the thorax?
week 4
Repositioning of the heart into the future thorax
Cranial-caudal folding brings the developing heart ventral to the developing foregut and caudal to the developing mouth (into the future thoracic region).
Lateral folding brings the endocardial tubes together in the midline fusing to form a primitive single tubular heart (primary heart tube) ultimately becoming the inner lining of the heart with adjacent mesoderm differentiating into cardiomyocytes.
Development of the Dorsal Aortae
With the cranio-caudal folding of the embryo, the cardiac tube is brought caudo-ventrally. The developing dorsal aortae approach the cardiogenic tube.
The cardiogenic tube is brought to a position ventral to the dorsal aortae and the vitelline veins approach the cardiogenic tube.
The caudal portion of the cardiogenic tube fuses with the cranial portion of the vitelline veins.
The caudal portions of the dorsal aortae fuse and the two sides of the cardiac tube fuse .
The dorsal and ventral aortae have formed, and the developing heart has formed the bulbus cordis , primordial ventricle and primordial atrium.
How does the primary heart tube form?
Lateral folding brings together the endocardial tubes which fuse to form the primary heart tube
What 4 things does the primary heart tube consist of?
endocardium (inner lining of heart)
cardiac jelly (acellular extracellular matrix)
myocardium (cardiac muscle)
epicardium (visceral pericardium)
How is endocardium formed?
fusion of endocardial tubes
How is cardiac jelly formed?
deposited by the developing myocardium, separating it from the endocardial tube
How is myocardium formed?
splanchnic mesoderm myocardial progenitors aggregate around the fused endocardial tubes
How is epicardium formed?
formed by splanchnic mesodermal cells which migrate onto the outer surface of the myocardium.
Development of pericardium
The portion of the intraembryonic coelom that surrounds the heart tube is the future pericardial cavity .
The pericardial cavity and myocardium gradually extend around the forming endocardial tube, leaving the dorsal mesocardium as a transient connection between the forming heart tube and the dorsal pericardial wall.
The dorsal mesocardium partially breaks down, creating the transverse sinus of the pericardium
Persisting dorsal mesocardium at the venous pole forms the site of development of pulmonary veins
Describe the passage of the transverse sinus of pericardium
passage posterior to the aorta and pulmonary trunk and anterior to the superior vena cava
When do the vasculature circuits form?
week 4
What are the 3 vasculature circuits?
1 intraembryonic circuit and 2 extraembryonic circuits (vitelline arc and umbilical vessels)
Intraembryonic circulatory arc
A ventral aortic outflow tract from the heart splits into a series of aortic arches passing around the pharynx through the pharyngeal arches and then collecting into paired dorsal aortae that distribute blood throughout the body.
A system of cardinal veins collects the blood and returns it to the heart via a common inflow tract.
What happens to the intraembryonic portions of the extraembryonic circulatory arcs after birth?
After birth the intraembryonic portions of these arcs are retained as vessels or ligaments in the adult body.
What are the 7 segments of the cardiac tube from arterial to venous end?
truncus arteriosus
bulbus cordis
bulboventricular sulcus
primitive ventricle
atrioventricular canal
primitive atrium
sinus venosus
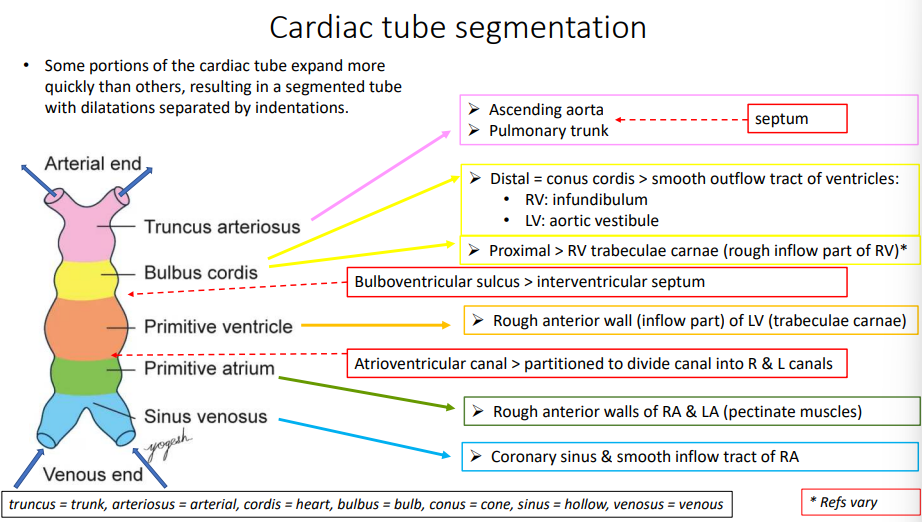
What causes the cardiac tube to become segmented?
Some portions of the cardiac tube expand more quickly than others, resulting in a segmented tube with dilatations separated by indentations.
What 2 things does the truncus arteriosus form?
ascending aorta
pulmonary trunk
What 3 things does the bulbus cordis form (distal and proximal ends)?
distal = conus cordis that becomes smooth outflow tract of right ventricle (infundibulum) and left ventricle (aortic vestibule)
proximal - right ventricle trabeculae carnae (rough inflow of RV)
What does the bulboventricular sulcus form?
interventricular septum
What does the primitive ventricle form?
rough anterior wall (inflow) of left ventricle (trabeculae carnae)
What does the atrioventricular canal form?
divides into right and left canals
what does the primitive atrium form?
rough anterior walls of right and left ventricle (pectinate muscles)
What 2 things does the sinus venosus form?
coronary sinus
smooth inflow tract of right atrium
When does cardiac looping occur?
week 4 when the heart tubes fuse
Cardiac Looping
Midsection of heart tube loops ventrally, caudally and to the right.
Primitive ventricle & bulbus cordis move ventral to the primitive atrium and sinus venosus.
Bulbus cordis moves to right of ventricle.
Inflow tract migrates towards the back and upwards.
Sinus venosus is now at the level of the ventricle and covered by part of the ventricle.
The atria now enclose the outflow tract on the left and right.
Sinus venosus & the atria are enveloped by the pericardium
Ventricles are mostly ventral & caudal to the atria
Outflow vessels (truncus arteriosus) remain in the midline.
Describe blood through in a single heart tube
Inflow tract (sinus venosus) contains blood from the vitelline veins (from yolk sac) and oxygen-rich blood from the umbilical veins.
Blood from the sinus venosus enters the primordial atrium.
Then through the atrioventricular canal into the primordial ventricle.
When the ventricle contracts, blood is pumped through the bulbus cordis and truncus arteriosus into the aortic sac
to the pharyngeal arch arteries
to the dorsal aortae for distribution to the embryo, yolk sac (umbilical vesicle), and placenta
When does the heart begin to beat?
day 28
When does partitioning occur?
week 4 to 8
What are the 4 steps of partitioning?
atrioventricular canal (develops AV cushions)
primordial atrium (septation of the atria)
primordial ventricle (interventricular septum separates primordial ventricle into 2 chambers)
outflow tract (partitioning of bulbus cordis and truncus arteriosus)
Partitioning the atrioventricular canal
Atrioventricular endocardial cushions form on the dorsal and ventral walls of the AV canal from a specialized extracellular matrix related to the myocardium (cardiac jelly) and neural crest cells.
Cushions approach each other and fuse, dividing the AV canal into right and left AV canals.
Partially separates the primordial atrium from the primordial ventricle to function as primitive AV valves.
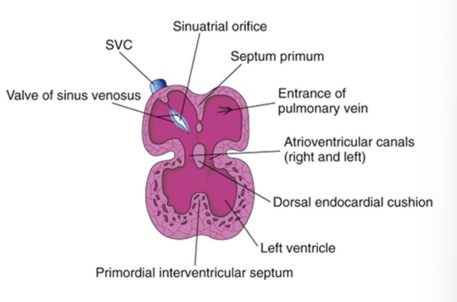
When does partitioning the atrioventricular canal occur?
day 26
When does partitioning of the primordial atrium occur?
day 30
Partitioning of the primordial atrium
Septum primum (first septum) grows downward from the roof of the atrium toward the endocardial cushions.
An opening remains (between the septum primum & endocardial cushions) called the foramen primum
Septum premium and endocardial cushions fuse forming the primordial AV septum which divides the atrioventricular canal into right and left segments.
Perforations (via apoptosis) appear in the septum primum called the foramen secundum which allows fetal venous return to the R atrium to pass across to the L atrium
Septum secundum (second septum) grows downward to the right of the septum primum overlapping the foramen secundum forming an incomplete partition called the foramen ovale
Cranial part of septum primum disappears and the remaining part of the septum, attached to the endocardial cushions, forms the valve of the foramen ovale, allowing fetal blood to pass from the R atrium to the L atrium
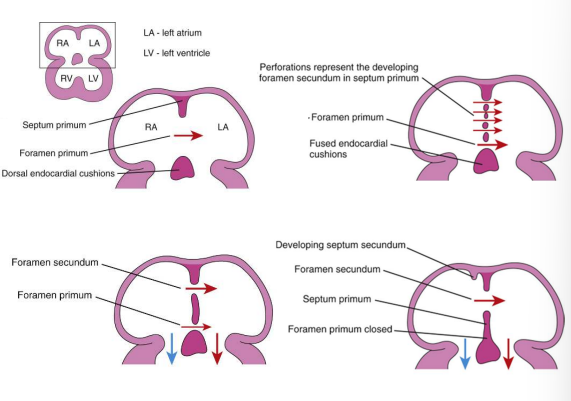
When does partitioning of the ventricles occur?
day 25
Partitioning the ventricles
Protrusions of endocardium from the floor of the primordial ventricle extend toward the inferior endocardial cushion and form the muscular part of interventricular (IV) septum.
Ventricular myocytes also contribute to the IV septum.
IV foramen forms between the free edge of the IV septum and the fused endocardial cushions to permit blood flow between ventricles.
Week 7: IV foramen closes with formation of membranous part of IV septum
Cavitation of the ventricular walls forms a spongelike mass of muscular bundles, the trabeculae carneae, papillary muscles and chordae tendineae.
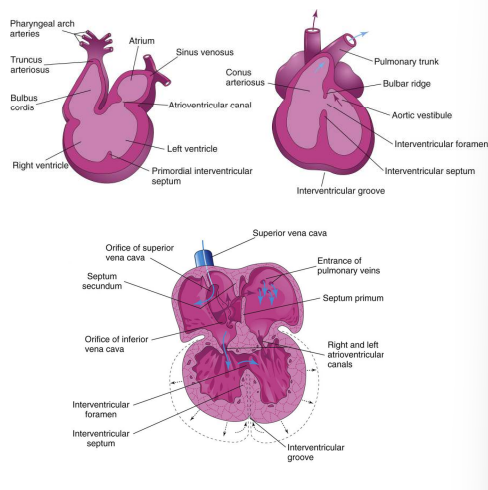
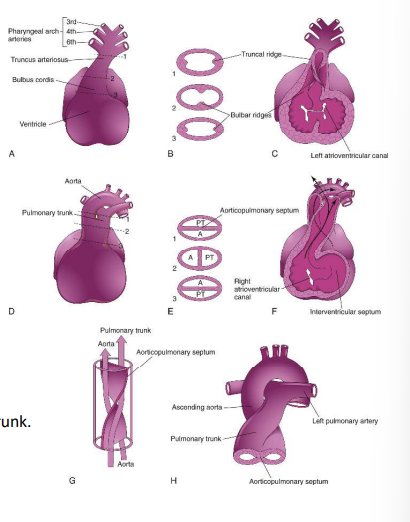
Partitioning of the outflow tract
Conotruncal septum (aorticopulmonary septum) develops from ridges that form in the bulbus cordis and truncus arteriosus (bulbar/truncal ridges)
Ridges fuse to form a spiral septum that divides the bulbus cordis and the truncus arteriosus into 2 arterial channels: aorta & pulmonary trunk
Spiralling > pulmonary trunk twists around the ascending aorta
Brings the future pulmonary trunk into communication with the R ventricle and the future aorta into communication with the L ventricle.
The distal bulbus cordis becomes incorporated into the walls of the definitive ventricles: R ventricle: infundibulum, which gives origin to the pulmonary trunk. L ventricle: walls of the aortic vestibule, the part of the ventricle inferior to the aortic valve
How does the semilunar valve develop?
Semilunar valves develop from three swellings of subendocardial tissue around the orifices of the aorta and pulmonary trunk.
Cardiac precursors, from neural crest cells, also contribute to this formation.
These swellings are hollowed out and reshaped to form three thin-walled cusps
How does the atrioventricular valve develop?
Atrioventricular valves develop from localized proliferations of tissue around the AV canals
What 5 things make up the intraembryonic circulatory arc?
aortic arches and dorsal aorta vessels'
cardinal veins
pulmonary system
coronary vessels
lymphatic system
How is the descending aorta formed?
Heart tube outflow tract bifurcates into the right and left 1st aortic arches, which join the paired dorsal aortae. The 2 dorsal aortae fuse to form the descending aorta.
When do the pharyngeal arches develop?
week 4
What are pharyngeal arches supplied by?
bilateral pharyngeal arch arteries from the aortic sac that enter the dorsal aorta on the same side.
How many pairs of aortic arches (pharyngeal arch arteries) develop?
6
What happens to the 1st pair of aortic arches?
mostly regress (remnants form maxillary arteries, may also contribute to external carotid arteries)
What happens to the 2nd pair of aortic arches?
mostly regress (remnants form hyoid arteries and stapedial arteries of middle ear)
What happens to the 3rd pair of aortic arches?
form common carotid arteries
What happens to the left 4th aortic arch?
forms aortic arch. Remains connected to L dorsal aorta (forms descending aorta)
What happens to the right 4th aortic arch?
adjoining R dorsal aorta and R 7th intersegmental artery form R subclavian artery (rest of R dorsal aorta degenerates)
L subclavian artery: (not derived from a pharyngeal arch artery) forms from the L 7th intersegmental artery.
Origin of R common carotid moves onto R subclavian to form brachiocephalic trunk
What happens to the 5th pair of aortic arches?
do not form in higher vertebrates
What happens to the 6th pair of aortic arches?
The proximal (ventral) portions remain on both sides and form the pulmonary arteries.
What happens to the right 6th aortic arch?
Proximal part persists as the proximal part of the R pulmonary artery.
Distal part degenerates
What happens to the left 6th aortic arch?
proximal part persists as the proximal part of the L pulmonary artery.
distal part passes from the L pulmonary artery to the dorsal aorta forming the ductus arteriosus (fetal shunt).
What is the 6th aortic arch (pulmonary arch) and what is it supplied by?
an asymmetrical capillary plexus associated with the developing trachea and lung buds supplied by ventral segmental arteries that arise from paired dorsal aortae.
How do the 6th pulmonary artieries form?
While the respiratory diverticulum and early lung buds elongate, the pulmonary capillary network forms a pair of discrete pulmonary arteries that connect to the 6th arch.
How do the pulmonary veins develop?
Venous drainage channels arise from each lung to form a single large common pulmonary vein that drains into the left atrium of the heart.
LA expands and the common pulmonary vein becomes incorporated into its wall.
Absorption of the vessel continues passed the first and second branch points of the original pulmonary veins.
4 independent pulmonary veins enter into the left atrium.
Why does the location of the left and right recurrent laryngeal nerves differ?
These nerves supply the sixth pair of arches and hook around the sixth pair of arteries on their way to the developing larynx.
Because the distal part of the R 6th arch degenerates, the R recurrent laryngeal nerve moves superiorly and hooks around the proximal part of the right subclavian artery (derivative of the 4th arch)
L recurrent laryngeal nerve hooks around the ductus arteriosus (formed by the distal part of the 6th artery) and remains around the ligamentum arteriosum (remnant of DA) and the arch of the aorta
What are the 3 branches of the dorsal aorta?
posterolateral/dorsolateral branches
lateral branches
ventral branches
Where do the posterolateral branches arise from and connect to?
Arise between the somites and connect with dorsal aorta.
What are the 3 posterolateral branches of the dorsal aorta and what do they supply?
intersegmental arteries (supply body walls and limbs)
dorsal branch (supply neural tub, epimere and skin)
ventral branch (supply hypomere and skin)
What do the lateral branches of the dorsal aortae supply?
Supply organs derived from intermediate mesoderm (urinary & genital systems)
What are the 3 lateral branches of the dorsal aorta?
suprarenal, gonadal and renal arteries
What are the 2 ventral branches of the dorsal aorta and what do they supply?
vitelline arteries (supply the gastrointestinal tract)
umbilical arteries (carry deoxygenated blood from body to placenta)
Where does the dorsal aorta end?
median sacral artery
What are the 2 cardinal veins?
anterior (superior) and posterior (inferior) cardinal veins
Where does the anterior cardinal vein drain from?
head region
Where does the posterior cardinal vein drain from?
lower half of the body
Where do the cardinal veins drain into?
left and right common cardinal vein to the sinus venosus into the atrium
Describe the subcardinal veins?
Subcardinal veins appear on both sides with the formation of the urogenital system
Anastomoses arise between the L & R subcardinal vein.
What does the right subcardinal vein do?
join vessels of the liver to form a hepatocardiac canal
Where do the subcardinal veins drain from?
arms and legs as limb buds develop
Describe the supracardinal veins
an additional paired longitudinal system with a close relationship with the sympathetic trunk.
where does the sacrocardinal plexus form?
in the sacral region
Where does the brachiocephalic anastomosis form?
between superior cardinal veins
How does the cardinal system develop?
anterior and posterior cardinal veins form
left and right subcardinal veins form
hepatocardiac canal forms from the right subcardinal vein joining liver vessels
supracardinal veins form
posterior cardinal veins atrophy
sacrocardinal plexus forms
connection between right supracardinal vein and right subcardinal vein forms
left sinus horn and left vitelline vein atrophy
brachiocephalic anastomosis forms
venous blood moved towards right side
posterior cardinal veins now only exist near heart and sacral region
intersubcardinal anastomosis forms
abdominal veins form
sacral veins form
inferior vena cava forms
anastomisis forms below liver between supracardinal veins
What are 3 abdominal veins?
suprarenal, renal and gonadal veins
What are the 4 sacral veins?
sacral plexus forms a median sacral vein, common iliac vein and the internal & external iliac vein
How does the inferior vena cava form?
Inferior vena cava is made from several sections of various vein systems: R supra- and subcardinal vein as well as the liver veins, that form the hepato-cardiac channel (R. vitelline vein)
What does the hemiazygos vein arise from?
Anastomosis below the liver between the supracardinal veins
Where do vessels of the vitelline system arise from?
yolk sac wall (eventually lose their connection to the sac)
How do vitelline arteries form?
form as paired ventral vessels from abdominal dorsal aorta
What connects the dorsal aorta with the future gut?
left and right vitelline plexuses
Describe the vitelline arteries cranial to the diaphragm
~ 5 pairs of arteries develop and anastomose with the dorsal aorta to supply the thoracic oesophagus
Describe the vitelline arteries caudal to the diaphragm.
coeliac trunk
superior and inferior mesenteric artery
What does the coeliac trunk supply?
foregut and outgrowths
What does the superior mesenteric artery supply?
midgut
What does the inferior mesenteric artery supply?
hindgut