Part 5: Water and Ion Balance
1/9
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
10 Terms
How much water is there inside the body
How is the water distributed?
Intracellular fluid
Extracellular fluid
What contributes to the water in the body? - what does it average out to?
Gains: 2 ways
Also state volume of water for each
Loss: 5 ways
Also state volume of water for each
about 55% of the body is composed of water
Water distribution
Intracellular: 2/3
Extracellular fluid: 1/3
75% of that interstitial fluid
25% of that is in plasma
Contributions
Gain
through drinking or eating 2.2 L/day
Byproducts of metabolic products 0.3 L/day
Loss
Urine 1.5 L/day
0.9 L/day
Skin (sweat)
Lungs (breathing)
Feces: 0.1 L/day
Gains and losses will be balanced to 0 L/day
Water Homeostasis
What happens when there is too much water loss?
Diseases
What happens inside the body + symptoms
What happens when there is too much water intake?
Where does the water go?
Symptoms
Water loss
Diseases: hypotension/shock
Process: water loss → less extracellular fluid → lowered blood pressure
Symptoms: confused, chest pain, low blood pressure, no urine
Too much water intake
Goes into the lungs, legs, abdomen
Difficulty breathing, walking, running etc
How is urine formed?
which organ involved
Explain process in the kidneys
Explain process of the main pathway of urine being formed
How much blood into the kidneys
How much waste is produced in the body
How much urine produced a day
Based on the process, what does it tell us about the the kidneys filtering process?
Kidney is involved
Blood —> kidney —> nephrons (where the blood plasma gets filtered) —> filter into ureter —> bladder —> urethra
1584 L into the kidneys
180 L filtrate formed a day
1.8 L of urine secreted/day
Not all filtrate gets secreted
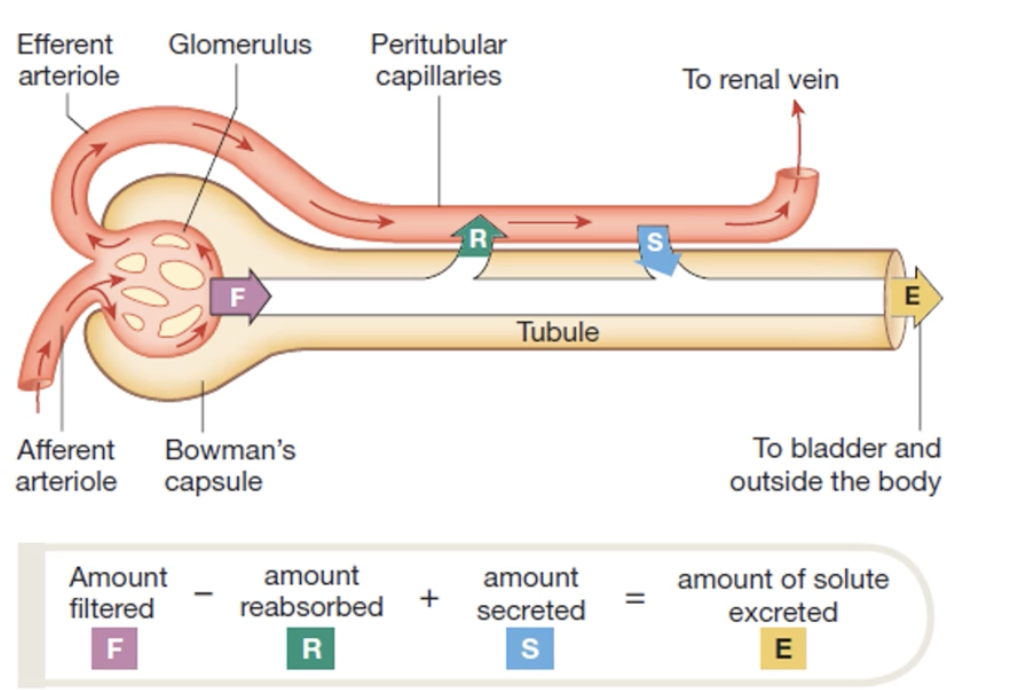
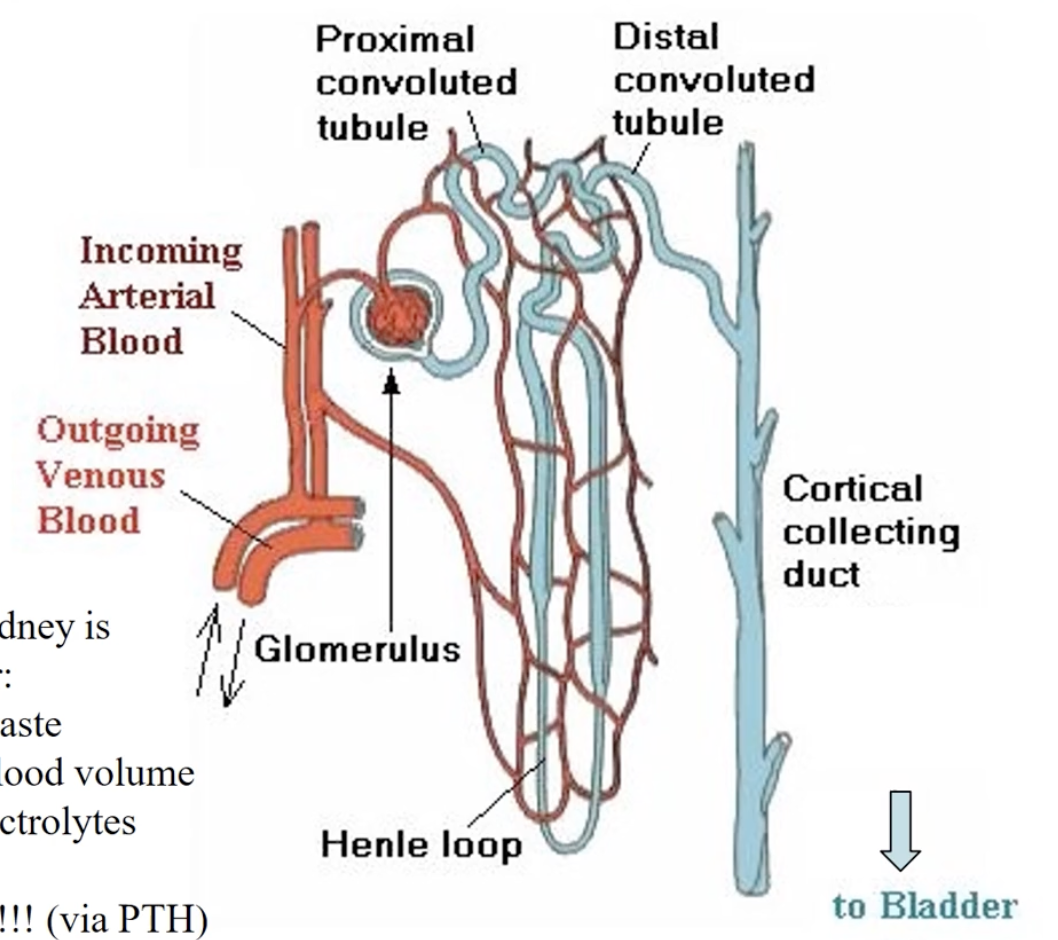
Nephron
Explain the where the blood meets up with the nephron
Why is the nephron so important?
5 factors
Explain the parts involved in blood filtration in the nephron
Arterial blood → glomerulus (where it meets up with the nephron)
Importance
Excreting waste
Regulates blood volume
Controls electrolytes
Blood pH
Vitamin D!!!!! (via PTH)
Process
(filtrate from blood) → proximal tubule (osmolarity: 300) —> loop of henle (reabsorption) —> distal convolted tubule —> collecting duct portion
What three hormones regulate water, Na+, and K+ balance
Just list them and how is water and/or Na+ and/or K+ affected by the hormone
Vasopressin
up water reabsorption
Aldosterone
up Na+ reabsorption
K+ secretion
has a very close relation with renin
Atrial natriuretic peptide
Na+ and water reabsorption
K+ reabsorption
Vasopressin
Another name for it
Primary function (based on name)
Purpose of function
Secondary function
Where is it synthesized
Where is it secreted
How is it regulated (the secretion)
2 main factors
How it works (for both; but initally two slightly different pathway)
How does the hormone work at the kidney
Explain the process and specifically where at the nephron (which part of it)
A.k.a antiduiretic hormone or ADH
Primary anti = prevent urination = prevent water reabsorption
Purpose
Conserve body water
Water balance and fluid homeostasis
Increases blood volume and blood pressure
Secondary function: regulating permeability of cells in the kidney
Purpose: to ensure reabsorption and low urine output
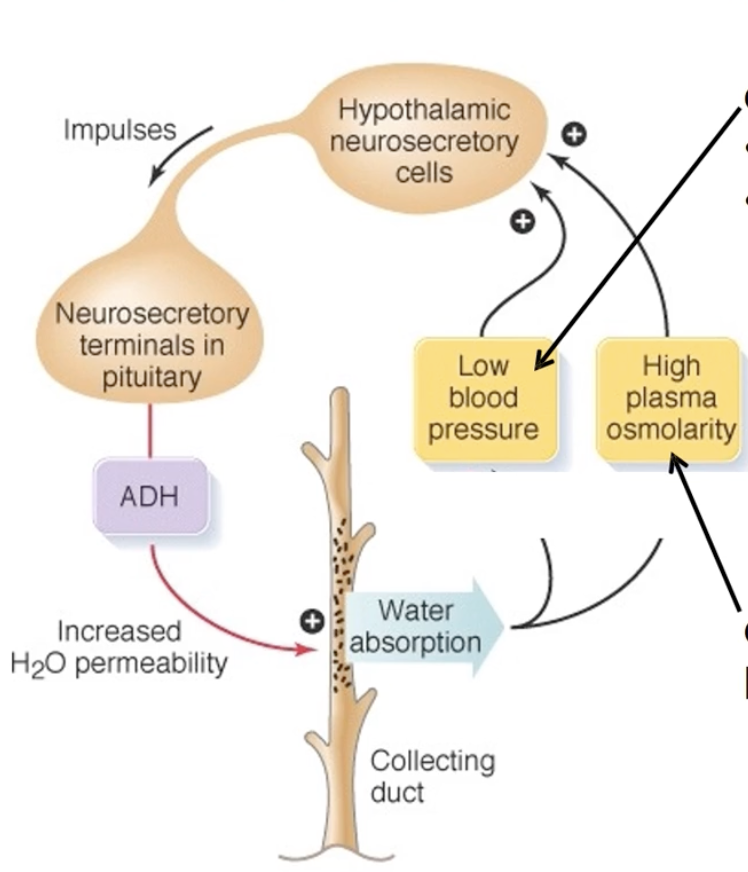
Synthesized in the hypothalamus
Secreted from the posterior pituitary
But does not make the hormone
Regulation
Main factor: high plasma osmolarity (increase salt/ion)
Need to dilute = reserve water
Detected by the osmoreceptors in the hypothamus
Second factor: low blood pressure
Detected by the reduced stretch of the walls of the atria of the heart and aortic and carotid arteries
Both same pathway
Detected by the hypthamalic neurosecretory cells to secrete ADH into the posterior pituitary
The posterior pituitary will secreted the ADH
Result: increased water permeability in the nephrons
Process
the vasopression goes to the kidney through the arteries and reaches thedistal convolted tubule and collecting duct, where the hormone binds to the receptors in these locations
Results in signal cascade (for metabotropic pathway)
aquaporin-2 water pores will be exocytosis to the apcical membrane (inside the tubule)
the water pores allows the water to goes through the collecting duct cells, through the interstitial fluid and to the blood stream
Aldosterone
what is it
Where is it made in
Main function
In what area in the nephron does it affect
What is it’s stimulus (2 kinds)
What type of feedback pathway does it follow
Types of it
What stimulus inhibits it?
A steroid
Synthesized in the adrenal cortex (located right above the kidneys)
Function: regulates sodium levels
Na+ reabsorption + retain water
K+ secretion
Affects the distal tubule and the collecting duct
Stimulus
high potassium concentration
Angiotensin 2 (blood pressure)
Pathway: negative feedback
Simple (K+ concentrations)
Complex (renin-angiotensin 2) (blood pressure)
Inhibitory
high osmolarity in the extracellular fluid
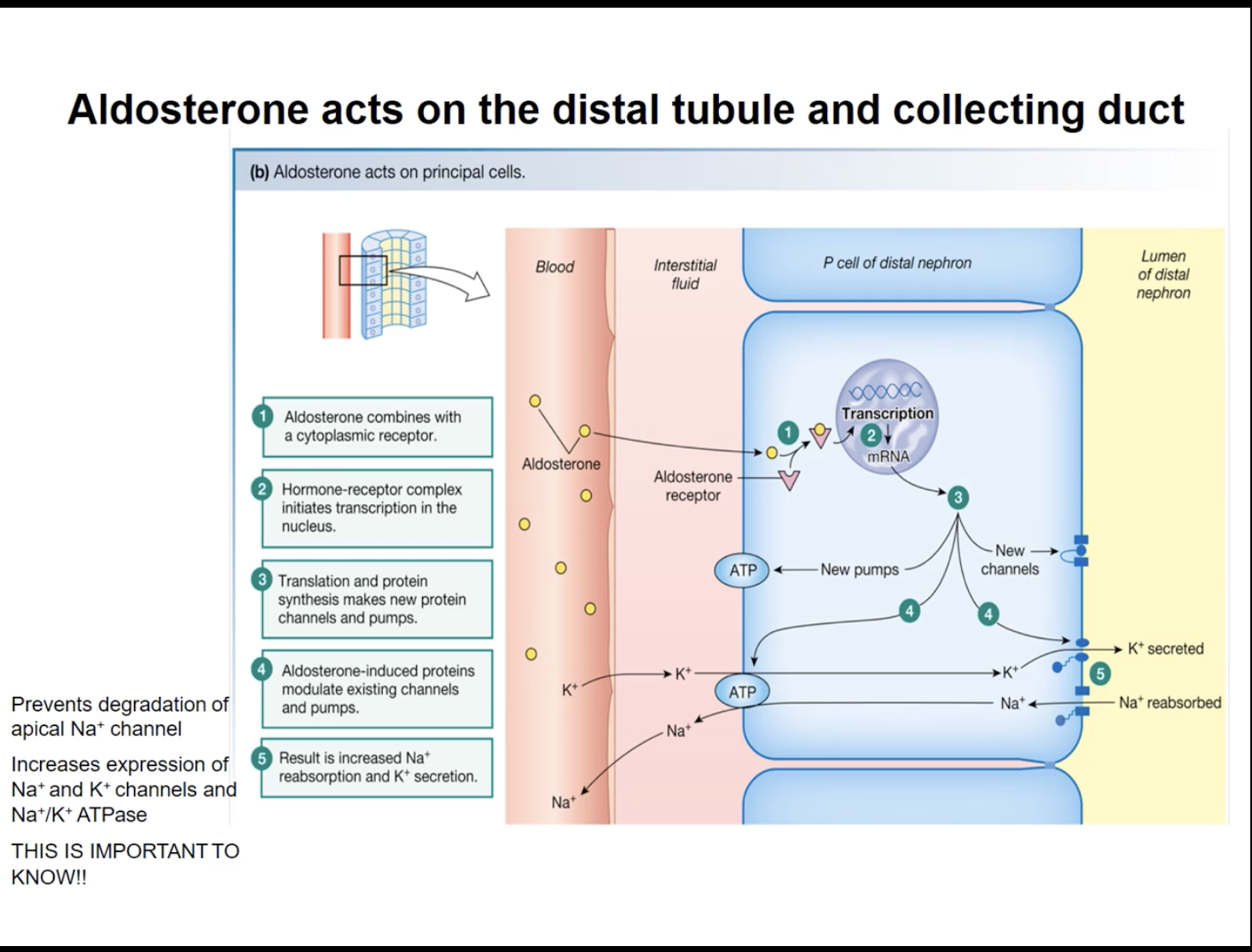
Process for simple aldosterone pathways with high potassium concentration
Process
Hormones in the blood stream reaches the kidneys
Goes through the blood, through the interstitial fluid, and into the distal collecting duct cells to bind with the cytoplasmic receptor
The complex initiates transcription in the nucleus (translocates there) to make new protein channels on the apical membrane (side facing towards the lumen of the nephron) and pumps on the basal membrane (facing towards blood)
Channels in charge of the secretion and reabsorption
ATPase pumps are in charge of the transportation of ions in between the
The new proteins will also modulate the existing ones
***by prevent degradation of the apical Na+ channel and the increase expression of the Na+ and K+ channels on the apical membrane and the ATPase pump Na+/K+ on the basal membrane
Process for complex aldosterone negative feedback pathway
state stimulus
than process
then three affects
The renal juxtaglomerular cells located on the arterioles near the glomerulus secrete enzyme renin with blood pressure falls
Kidney secreted renin
Liver produces precursor angiotensinogen which renin cleaves to angiotensin I
Lungs have ACE which cuts the precursor to angiotensin II
Affects
Hypothalamus: Thirst and drinking
Blood vessels: Vasoconstriction
Adrenal cortex produce aldosterone secretion → kidney undergoes salt and water retention
Results: increase in blood pressure
Natriuretic peptides
main function
What produces them
3 types
Their own functions
Where is it secreted from
main function: decrease water retention
Produced by secondary endocrine glands (have secondary function)
e.g
ANP: sense the stretch of the heart = high pressure = must dilate them and secrete fluids
Secreted by Atria (myocardia cells) and neurons
BNP
secreted by the ventricles myocardial cells and neurons
CNP
Secreted by the brain, pituitary glands, vessels, and kidneys
Main process
hypothalamus secreted less vasopressin
Kidney secretes less renin and increase globular filtrate rate
Adrenal cortex secreted less aldosterone
Medulla oblongata have decreased sympathetic output