Unit 9 - Physiology
1/142
There's no tags or description
Looks like no tags are added yet.
Name | Mastery | Learn | Test | Matching | Spaced | Call with Kai |
|---|
No analytics yet
Send a link to your students to track their progress
143 Terms
System integration
Integrated activity of all the organ systems
Emergent properties
Describes properties which emerge in a complex system, which are not seen in the individual components making up the system
permeable
thin tissue layer
moisture
large SA:V
concentration gradient
Properties of gas exchange surfaces (5)
dense network of blood vessels
continuous blood flow
ventilation
separation oxygenated/deoxygenated blood
Maintenance of concentration gradients in animals (4)
Pharynx
A
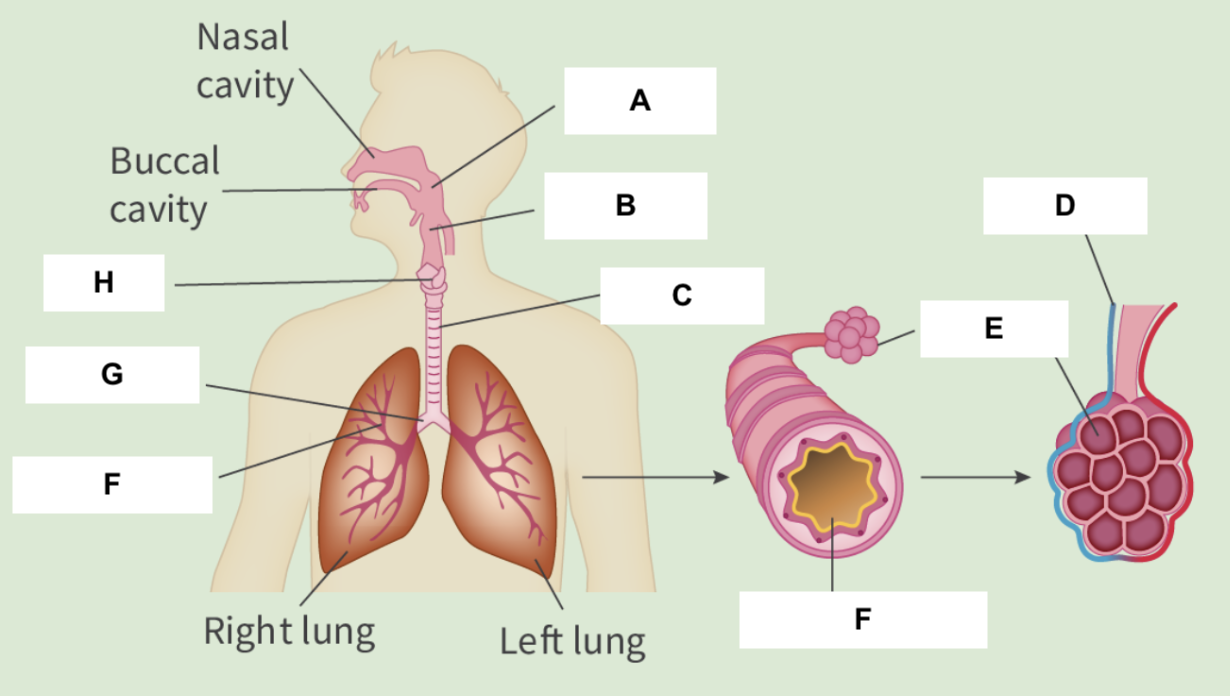
Epiglottis
B

Trachea
C

Capillary
D

Alveoli
E

Bronchioles
F

Bronchus
G

Larynx
H

presence of surfactant
branched bronchiole network
extensive capillary beds
high surface area
thin membrane
Alveoli adaptations (5)
flattening of cells
microvilli
invagination
Adaptations to increase SA:V ratio (3)
Relaxed
A
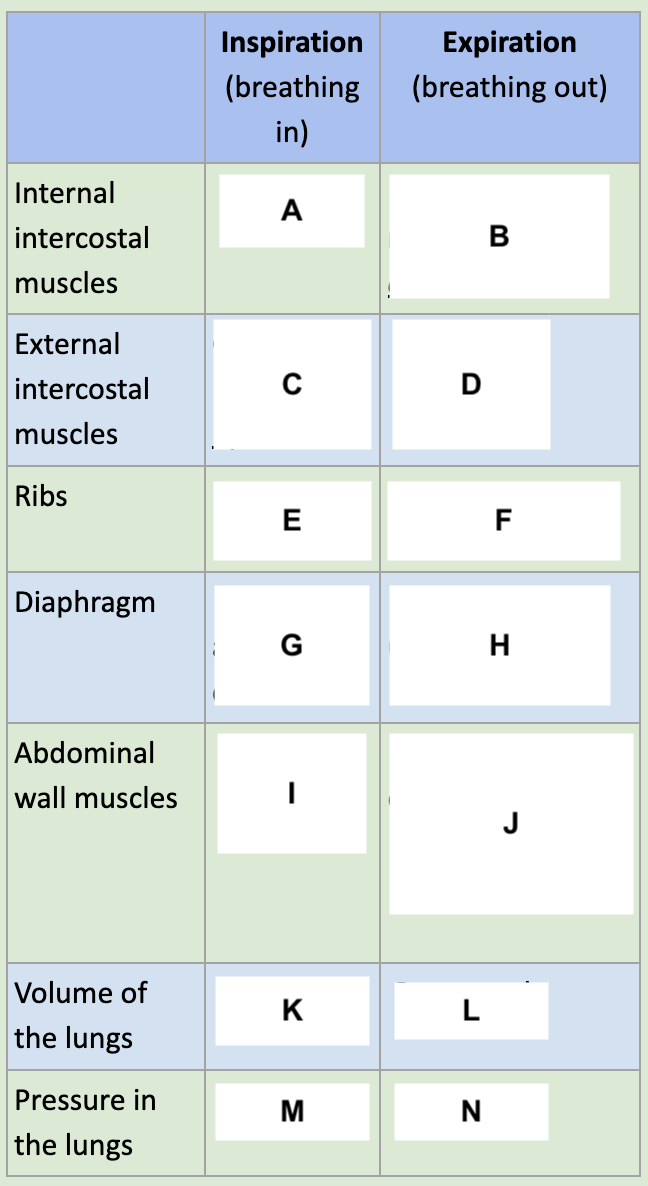
Contract to pull rib cage in and down
B

Contract to lift rib cage up and out
C

Relaxed
D

Expand
E

Move back in and down
F

Contracts and pulls down
G

Relax, arch back up
H

Relaxed
I

Used if forced breathing, relaxed otherwise
J

Increased
K

Decreased
L

Decreased
M

Increased
N

Inspiratory reserve volume
A
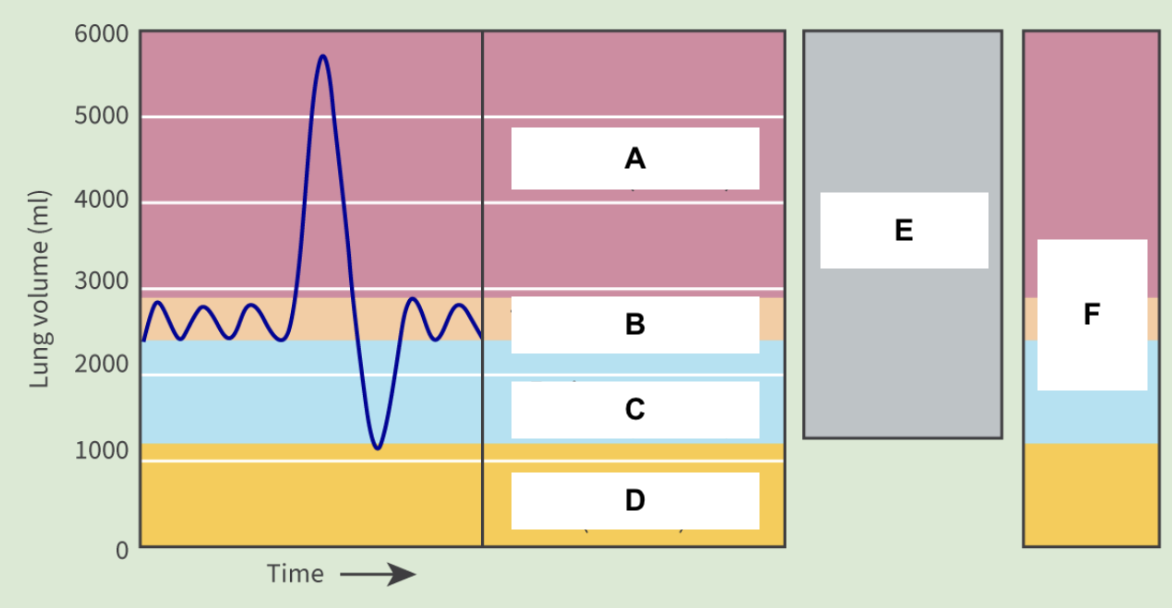
Tidal volume
B

Expiratory reserve volume
C

Residual volume
D

Vital capacity
E

Total lung capacity
F

Reduced diffusion distance
A
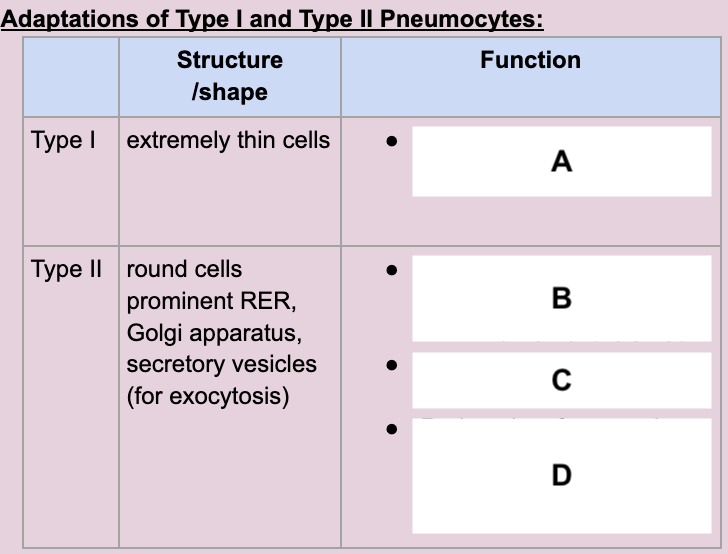
secreting surfactant
medium that gases can dissolve
reduced surface tension
B, C, D

Alveolus
A
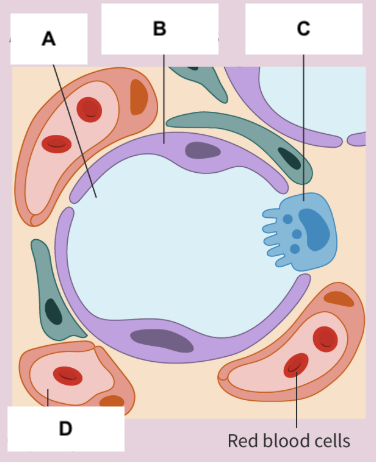
Type I pneumocytes
B

Type II pneumocytes
C

Capillary
D

walls are 1 cell thick
lumen is 1 blood cell wide
fenestrations
Adaptations of capillaries (3)
Thick tunica media to help artery recover when stretched and withstand high pressure
Muscle within tunica media pushes blood
Smaller lumen than veins to maintain blood pressure
Adaptations of arteries (3)
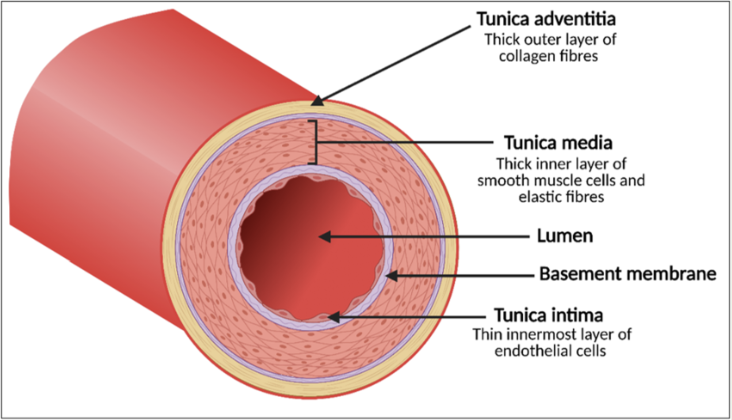
thinner tunica media
flexible wall
large lumen
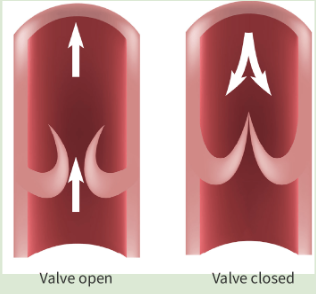
valves
Adaptations of veins (4)
Atherosclerosis
hardening and narrowing of the arteries due to the deposition of cholesterol
Tissue fluid
Formed when blood plasma is pushed out of the capillary walls into the surrounding tissue aka interstitial fluid.
Lymph
colorless fluid containing excess tissue fluid/white blood cells/proteins. Functions to help transport immune cells + remove foreign particles/toxins
Atrial systole
ventricular systole
diastole
3 stages in cardiac cycle
Superior vena cava
A
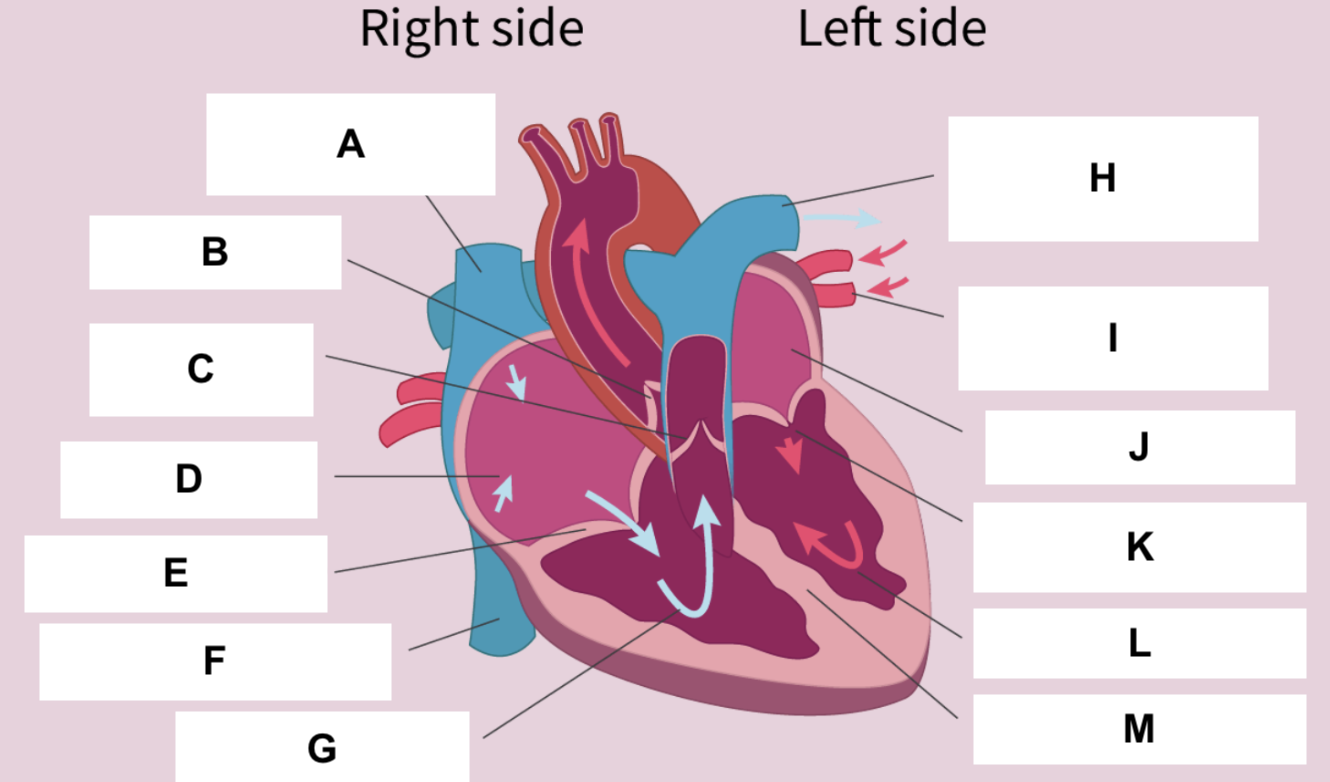
Aortic valve
B

Pulmonary valve
C

Right atrium
D

Tricuspid valve
E

Inferior vena cava
F

Right ventricle
G

Left pulmonary artery
H

Left pulmonary veins
I

Left atrium
J

Bicuspid valve
K

Left ventricle
L

Septum
M

Myogenic
The ability of cardiac muscle to beat without external stimulation.
Sarcomeres
The basic contractile unit of a muscle, containing actin and myosin. Gives muscle striated appearance
Synovial joint
Joints that are enclosed in a joint capsule, where bones are separated by a fluid-filled cavity, allowing free movement between the bones.
Neuronal synapses
A small gap at the end of a neuron that allows a signal to pass from one neuron to the next.
Neuromuscular junction
A specialised synapse that connects a motor neuron to a muscle fibre
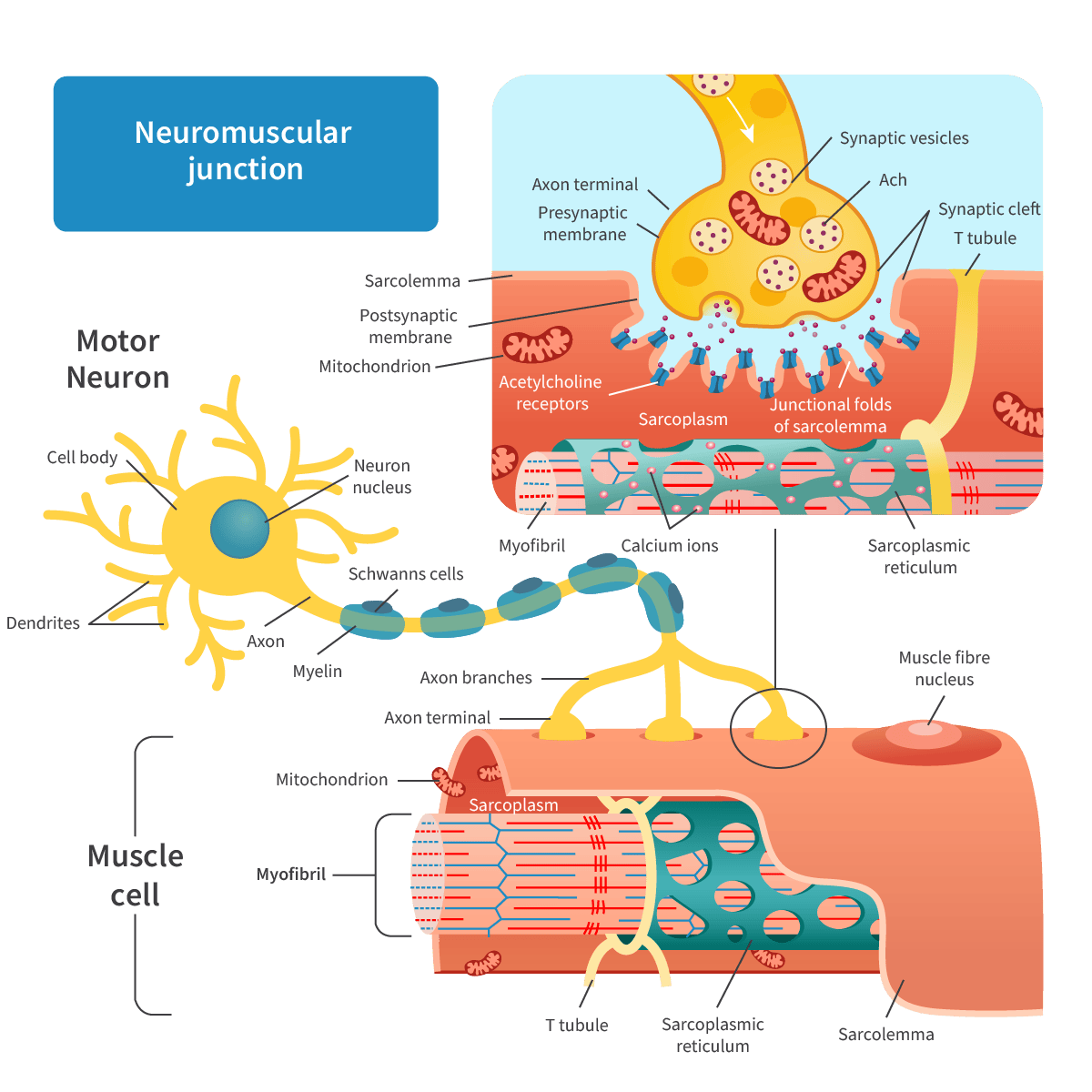
Neuroglandular junction
A small gap between a neuron and a gland.
Failed initiations
Not enough Na+ influx into post-synaptic neuron, cannot generate action potential
Threshold potential
The critical level to which a membrane potential must be depolarised to initiate an action potential
Saltatory conduction
The skipping motion of the action potential from one node of a myelinated axon to another.
Hyperpolarization
A change in the cell’s membrane potential that makes it more negative.
Summation
combined effect of the excitatory and inhibitory stimuli that are received from a number of presynaptic neurons and transmitted to the axon hillock (a specialized part of the cell body (soma) of a neuron that connects to the axon) of the postsynaptic neuron
All or nothing principle
This states that a stimulated nerve fibre either fires at full strength or does not fire at all
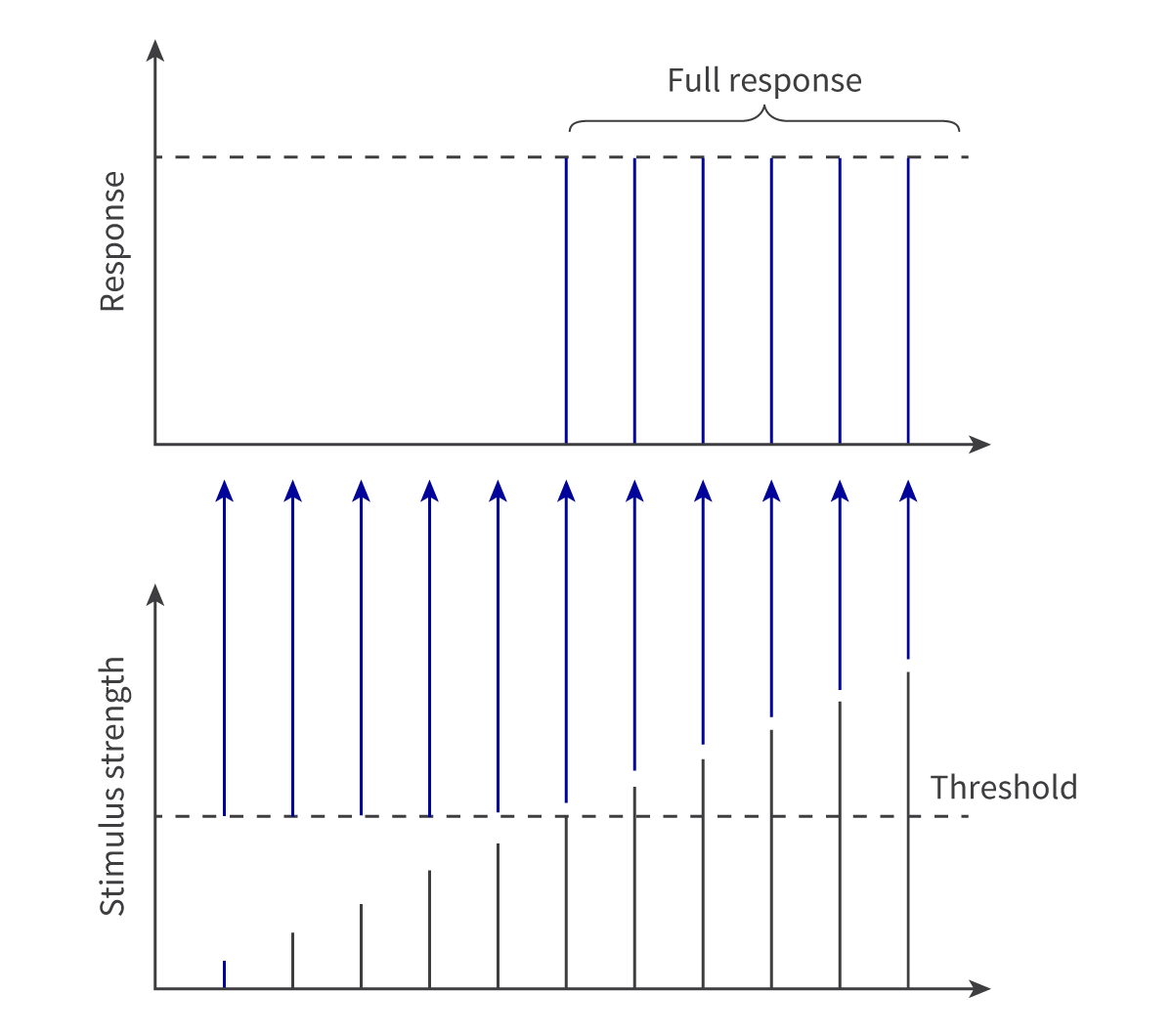
Epidermis
Outermost layer of skin. Protective barrier against external factors
Dermis
Contains blood vessels, hair follicles, sweat glands, sensory receptors
Thermoreceptors
Responsible for detecting change in temp
Meissner’s corpuscles
Detect light touch/low frequency vibrations
Nociceptors
Detect pain
Pacinian corpuscles
Detect deep pressure/high frequency vibrations
Ruffini endings
Detect skin stretch and continuous pressure
Free nerve endings
Detect pain/temp/itching
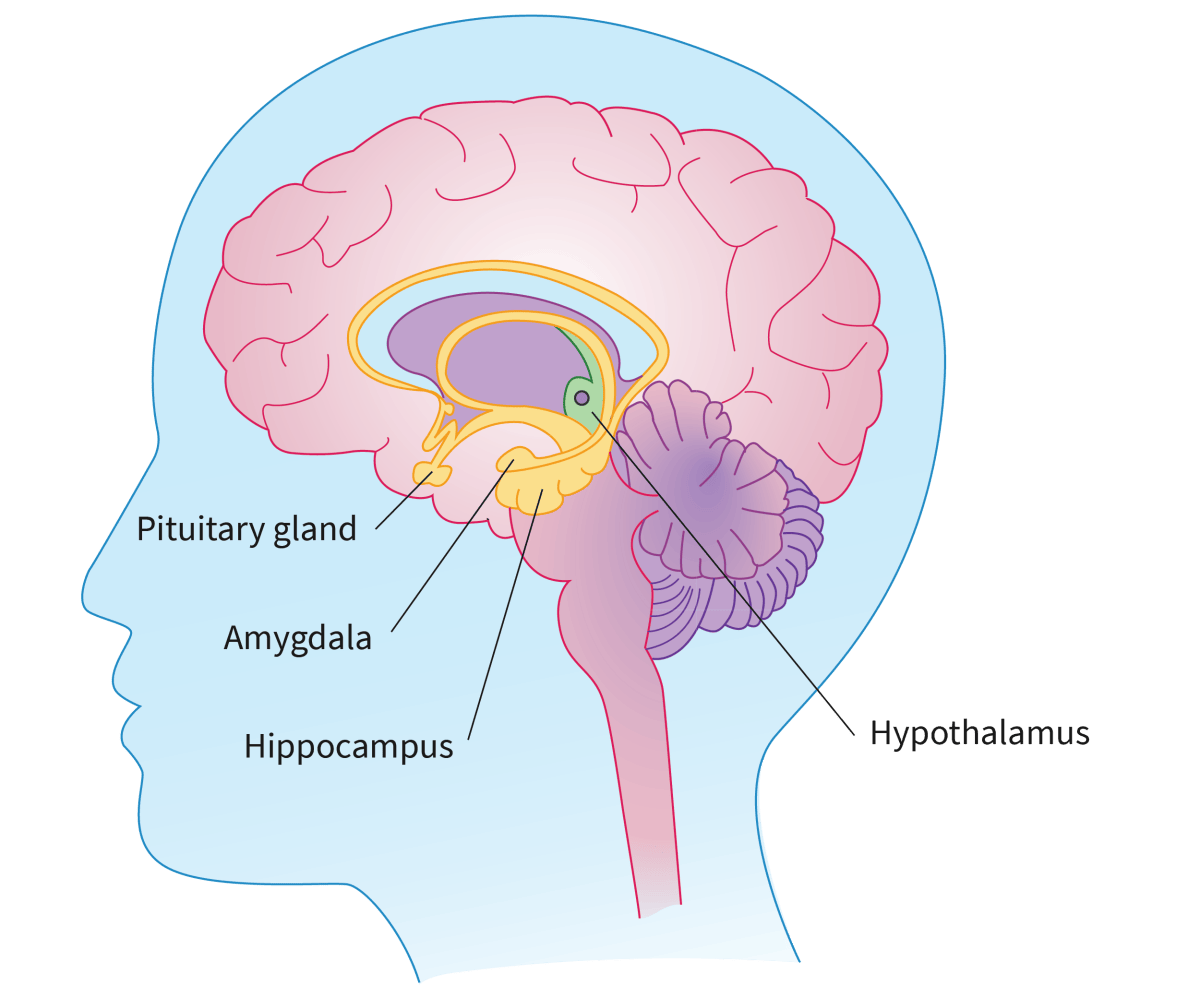
Cerebrum
Largest part of brain
Controls vision/hearing/touch/speech/thinking
Initiates and coordinates movement
Divided into 2 cerebral hemispheres
Each divided into 4 lobes:
Frontal lobe
Parietal lobe
Occipital lobe
Temporal lobe
Cerebellum
Back of head
Voluntary muscular movements + balance + coordination
2 hemispheres
Brainstem
Consists of midbrain + pons + medulla oblongata
_____
Largest part of brain
Controls vision/hearing/touch/speech/thinking
Initiates and coordinates movement
Divided into 2 cerebral hemispheres
Each divided into 4 lobes:
Frontal lobe
Parietal lobe
Occipital lobe
Temporal lobe
______
Back of head
Voluntary muscular movements + balance + coordination
2 hemispheres
_______
Consists of midbrain + pons + medulla oblongata
Reflex arc
Pathway followed by reflex action.
3 roles of cerebellum:
Coordination of voluntary muscle movements
Timing + force of contraction of muscle groups
Maintenance of balance + posture
Uses inputs from proprioceptors + other receptors to bring in shifts inn body position
Motor learning
Ex. Playing cricket
3 roles of cerebellum:
Coordination of ______ _______ _________
Timing + force of contraction of muscle groups
Maintenance of _____ + ______
Uses inputs from proprioceptors + other receptors to bring in shifts inn body position
____ learning
Ex. Playing cricket
peristalsis
movement of food down tract due to rhythmic contractions of muscles in waves
Quorum sensing
The regulation of gene expression in response to fluctuations in cell-population density.
Hormones, neurotransmitters, cytokines, calcium ions
4 types of signalling chemicals
Transmembrane receptors:
Binding of signalling chemical to outer side of transmembrane receptor → causes reversible changes to structure
Signal is amplified by triggering activation of protein kinases that phosphorylate many downstream proteins, causing chain reaction
Inner side (in contact with cytoplasm) becomes catalytically active + makes secondary messenger within cell (Ex. Cyclic AMP)
Protein kinases activated, that can phosphorylate proteins
Conveys signal to effectors within cell carrying responses
Transmembrane receptors:
Binding of signalling chemical to ____ side of transmembrane receptor → causes _____ changes to structure
Signal is _____ by triggering activation of ______ ______ that _________ many downstream proteins, causing chain reaction
Inner side (in contact with cytoplasm) becomes ______ active + makes ______ ________ within cell (Ex. Cyclic AMP)
Protein kinases activated, that can phosphorylate proteins
Conveys signal to _________ within cell carrying responses
Intracellular receptors:
Ligand passes through plasma membrane
Ligand binds to intracellular receptor
Active ligand-receptor complex
Complex can regulate gene expression
Intracellular receptors:
Ligand passes through plasma membrane
Ligand binds to intracellular receptor
Active _____-____ _______
Complex can regulate gene expression
Signal transduction cascade
Series of biochemical reactions that occur inside a cell in response to binding of a signalling molecule (like hormones/neurotransmitters) to its receptor on the cell surface
Insulin
Example of negative feedback mechanism
Blood clotting
Example of positive feedback mechanism
skin and mucous membranes
2 primary defence mechanisms against pathogens
Blood clotting process:
Activation + accumulation of platelets at site of injury
Platelets form a plug, sealing injury
Platelets + injured tissues release clotting factors (including Ca+)
When activated, clotting factors interact in cascade of chemical reactions
Ex. Clotting factor "thromboplastin" + calcium ions convert prothrombin to its active state, thrombin
Thrombin converts fibrinogen, a blood clotting factor normally dissolved in blood, to INSOLUBLE fibrin
Fibrin forms mesh over wound, trapping more platelets + red blood cells
Clot dries and shrinks over time, forming scab
Blood clotting process:
Activation + accumulation of _____ at site of injury
____ form a ____, sealing injury
_____ + injured tissues release _____ ______ (including Ca+)
When activated, clotting factors interact in _____ of chemical reactions
Ex. Clotting factor "_______" + _____ ions convert _______ to its active state, _______
______ converts ______, a blood clotting factor normally dissolved in blood, to INSOLUBLE _______
______ forms ______ over wound, trapping more platelets + red blood cells
Clot dries and shrinks over time, forming scab
Steps of phagocytosis:
Recognition of pathogen by phagocytes: receptor molecules on plasma membrane of phagocytes recognize + bind to pathogen, triggering formation of pseudopodia
Pseudopodia encircle target microorganism, then both protrusions seal --> resulting in formation of phagosome (vesicle)
Phagosome undergoes maturation
Phagosome fuses with lysosomes forming phagolysosomes that contain digestive enzymes originally present in lysosome
Enzymes digest microbial components, then released from cell
Thus, Phagocytosis is the non-specific secondary line of defense
Steps of phagocytosis:
______ of pathogen by phagocytes: receptor molecules on plasma membrane of phagocytes recognize + bind to pathogen, triggering formation of _______
________ encircle target microorganism, then both protrusions seal --> resulting in formation of _______ (vesicle)
______ undergoes maturation
______ fuses with _______ forming _________ that contain digestive enzymes originally present in lysosome
Enzymes digest microbial components, then released from cell
Thus, Phagocytosis is the non-specific secondary line of defense
Overprescribing antibiotics
Unfinished treatment
Overuse in livestock
Causes of antibiotic resistance (3)
Zoonosis
An infection that can be transmitted from non-human animals to humans.
Spillover
when pathogens originally present in animal species (reservoirs) cross species barrier + enter humans
Examples of zoonosis:
Tuberculosis = Bacteria → Cattle → Humans
Rabies = Virus → Animal → Bite humans
Japanese encephalitis = Virus → Pigs/Waterbirds → Mosquito → Humans
COVID-19 = Bats → Pangolins → Humans
Examples of zoonosis:
Tuberculosis = Bacteria → ______ → Humans
Rabies = ____ → Animal → Bite humans
Japanese encephalitis = Virus → ____/Waterbirds → _____ → Humans
COVID-19 = Bats → Pangolins → Humans
DNA vaccine
Use plasmids to introduce gene encoding an antigen from a specific pathogen
Herd immunity
Indirect immunity from an infectious disease which occurs when a large proportion of the population are immune to the infection either by vaccination or previous infection(s).